Hospital Discharge Camden Partnership Rough Sleepers CPRS Debra

Hospital Discharge Camden Partnership – Rough Sleepers (CP-RS) Debra Holt: AD Integrated Commissioning Camden CCG/LA Clare Mc. Ginley: Integrated Care Clinical Operations Manager & HCPC Reg Occupational Therapist UCLH
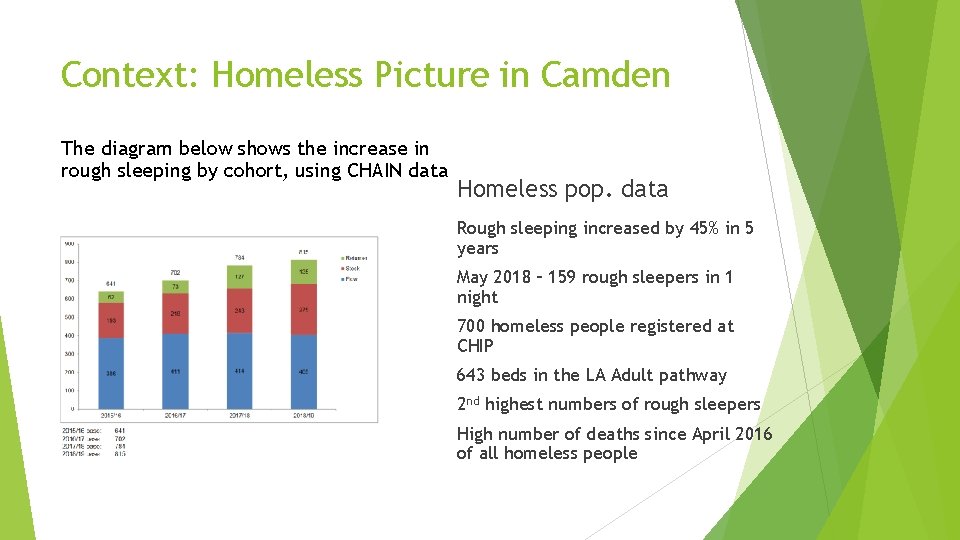
Context: Homeless Picture in Camden The diagram below shows the increase in rough sleeping by cohort, using CHAIN data Homeless pop. data Rough sleeping increased by 45% in 5 years May 2018 – 159 rough sleepers in 1 night 700 homeless people registered at CHIP 643 beds in the LA Adult pathway 2 nd highest numbers of rough sleepers High number of deaths since April 2016 of all homeless people
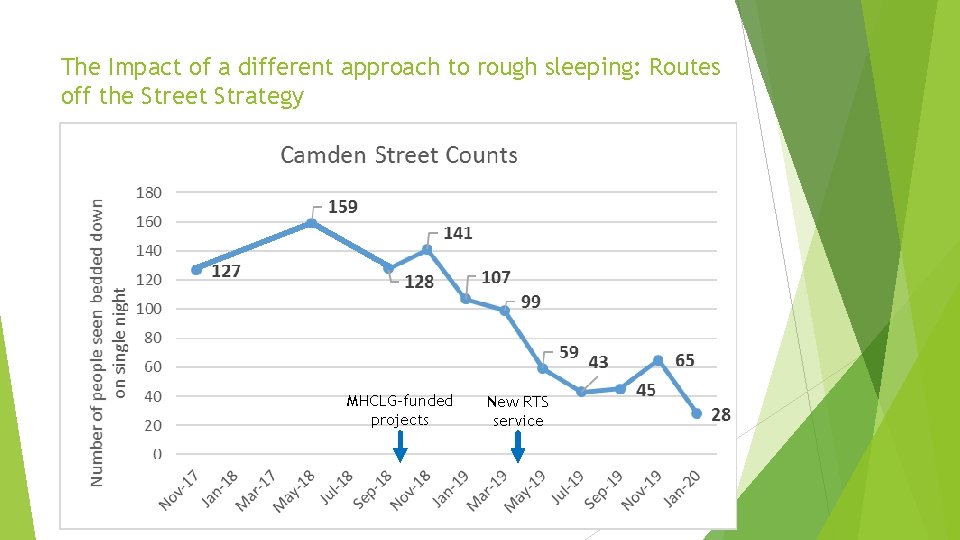
The Impact of a different approach to rough sleeping: Routes off the Street Strategy MHCLG-funded projects New RTS service
Original Focus of our Bid Support rough sleepers who are either Medically optimized with no discharge destination Discharged safely as part of the hospital at home model Identified High Intensity Users with complex needs
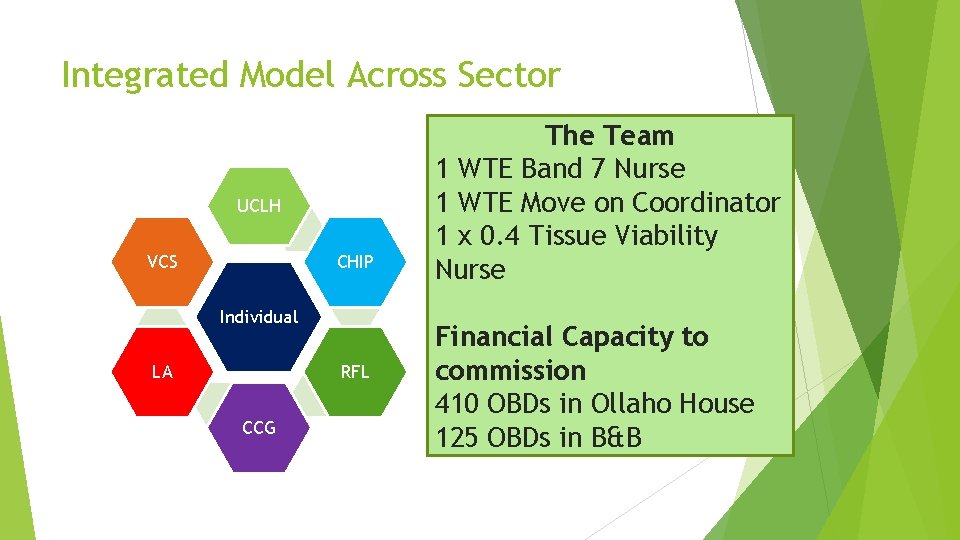
Integrated Model Across Sector UCLH VCS CHIP Individual RFL LA CCG The Team 1 WTE Band 7 Nurse 1 WTE Move on Coordinator 1 x 0. 4 Tissue Viability Nurse Financial Capacity to commission 410 OBDs in Ollaho House 125 OBDs in B&B

Where are service users identified? Emergency Departments (ED) Routes off the Street (RTS) Camden Health Improvement Practice(CHIP)

What is CP-RS doing… Patients can be discharged to Olallo House hostel or B&B with a wrap around services on discharge from ED Jointly the Rough Sleepers CNS, MOC, GP & RTS Hu. B Manage health and psychosocial needs Prevent a return to the streets Reduce frequency of attendances of HIU’s patients at ED Rough Sleepers CNS provides general nursing care, GP registration, coordination into service, follow ups, in & outreaching with ED, Psychosocial support MOC works jointly with the nurse with the reconnections and connections in & out of Camden and to move on from Olallo when deemed medically fit RTS is the cornerstone of the project as the outreach clinics are ran from there Direct referral into TVN specialist wound care clinic based at CHIP This an innovative integrated partnership in which a gap has been identified which cannot be left unturned
GP Registration Wound Care General Health Check up Support to Access other health services Women’s Health Nurse lead ‘drop in’ Clinic Running for the next 7 weeks only When…… Register at RTS reception to see the Nurse Sibo…. Tues Morning - Women Only 0930 -1230* Tues Afternoon 1400 -1630* Friday Lunch time (Hot food served while you wait) 1130 -1630* *last appointment must be registered 20 mins before

Consultant Nurse Wound Clinic • Specialist Compression Therapy • Prevention focused • Specialist approach to engage complex patients • Wound related complications managed outside of hospital • Non- wound related co-morbidities identified and ref for treatment to correct services • Funded to be delivered Mon&Fri CP-RS • Additional appointments bookable on Wed • Linking in & Joint working • Sign posting from other service • Increasing awareness jemellgeraghty@nhs. net
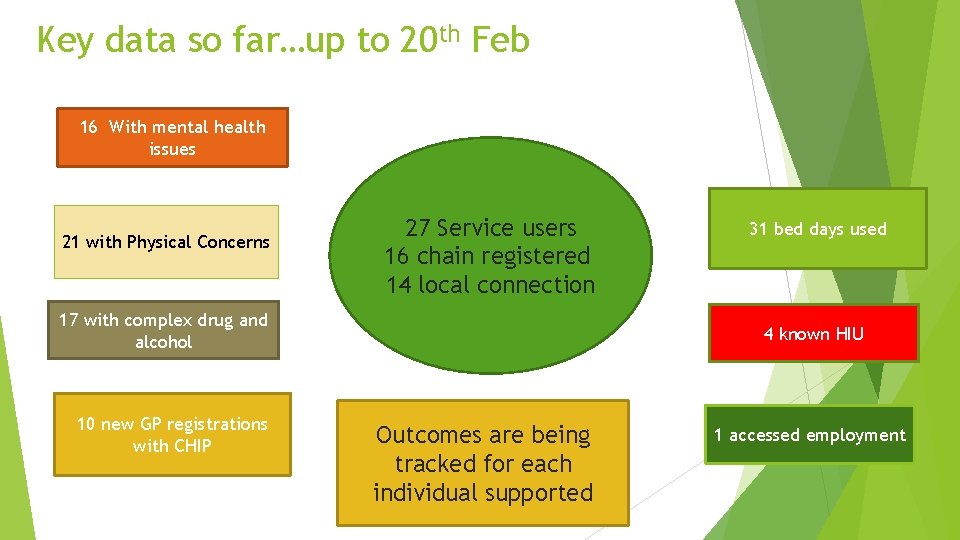
Key data so far…up to 20 th Feb 16 With mental health issues 21 with Physical Concerns 27 Service users 16 chain registered 14 local connection 17 with complex drug and alcohol 10 new GP registrations with CHIP 31 bed days used 4 known HIU Outcomes are being tracked for each individual supported 1 accessed employment

35 yr old Male ‘Joe’ Outreach team found on the streets chain registered-advised to see the nurse in RTS whilst at the HUB Seen by the Rough Sleepers CNS full history gathered and Recent UCLH activity reviewed Identified as having 9 ED attendances since Dec 2019 -Feb 2020 relating to wound needs & medication ED-notes reveal he was oversubscribing on anticoagulation medication, this was increasing the bleeding & wounds were not improving and had a significant risk of infection as remained sleeping on the streets and injecting daily CNS Input: • Referred into Hostel • Registered with CHIP • Referred to the TVN bilateral leg wound clinic • Monitoring his anticoags • Referred to addiction services • Reduced ED admission, • Attended all appointments made –but does continue to use MOC Input: • Supported into Olallo • As medical care is being provided supporting to access services for longer term Outcome: ED attendances reduced-not been there since 22 nd! Engaging with RTS & CHIP services Joined up working to supporting to connect into health/mental health/social services

43 yrs. old male ‘Ernest’ Moved from Camden to Surrey approx. 3 yrs ago to live with his girlfriend, approx 3 wks ago they had a fight in which she stabbed him 9 times- police involved, advised man to leave and not returned to Surrey, complied but had no belongings or ID. Attended RTS following outreach input on the streets, identified as having stitches which were overdue for removal in the stabbed wounds and was very low in mood History of drug & Alcohol intake Reported prior to his addiction he was in FT employment as an IT worker and he was married. Marriage broken down as wife had Post Natal depression, divorced several years ago and no contact but they are Camden based. Reported his mother also Camden based, however, she has a diagnosis of bipolar and they have a complex relationship due to her MH needs and feels risk associated if he returned. CNS Input: • Removed stitches and dressed/cleaned wounds • Registered with Camden GP • Referred to ICAS-Alcohol Service • Referred to psyc in CHIP • Set up GP appointment for f/up • Hypertension identified and BP plan put in place MOC Input: • Supported into Olallo • Contacted police to obtain Breach of peace appointment to obtain ID as in Surrey • Identified a case worker in Camden to support with long term support needs Outcome Remains in Olalla (Day 17) Breach of peace appointment will take place on 27/2/20. Passport is obtained, a copy will be given to allocated worker and he can then be progress into long term accommodation support on Friday. Continues to see CHIP GP & Psyc with groundswell support and is doing really well

43 yrs. old Male ‘Lukaz’ Polish speaking –no English Arrived into this country approx. 3 mths ago to join his girlfriend, approx. 1 mth after arrival she committed suicide at this time he was working in a vegetable factory in south London, he had worked for 22 days without any payment. Advised when asked regarding payment it would go to his friend-this never happened and then he was informed he is working in ‘blackmarket’ –therefore left, was unable to keep up with his rent so began sleeping on the streets. When attended RTS he reports had been living on the streets in Camden for approx 3 wks. Attended RTS had visible injuries to both eyes swollen , bruised and bloodshot following a fight on the streets and was anxious. CNS Input: • Head injury assessment completed • Cleaned eye wounds • Supported to get GP registration • Accessed interrupter services to get full history • F/up completed for wounds and head • Ref to GP & Psyc service • Health promotion provided • Ref for bed in Olallo MOC Input: • Supported into Olallo • Supported to contact the polish embassy • Support to gain ID • Support to connect to appropriate housing support • Referred to another hostel place to stay LT until situation has been outcome Outcome: Spent 10 days in Olallo Transferred to hostel for long term planning

53 yr old ‘Paddy’ Came into ED by Ambulance, picked up from the streets following a alcohol related fall had sustained a head injury. Intoxicated and drowsy on arrival into ED. Had been rough sleeping in Camden for approx 2 wks following the breakdown in a relationship in kent where he had moved to from Camden 3 yrs ago. Reported return to the Camden area as felt safer rough sleeping her than in Kent. CNS Input: • Assessed in ED jointly with the alcohol nurse • Referred to RTS for follow up the next day • Reviewed wounds & head injury • Registered with GP • Ref to ICAS • Ref to Olallo hostel • Diabetic • Identified allergic to metformin on alternative meds • Appointment made to see psychologist at CHIP • Referred to groundswell MOC Input: • Liaised with Kent council, initially declined as patient was in London • Persistent with the referral as patient had only been in Camden for 2 wks. • Kent Council refused to accept unless presented to them in person • Supported given to get to local council • Update received as accepted and rehoused in Kent Outcome: Returned to previous locality after 5 days of wrap around input. Patient contacted MOC and reported rehoused and settled on 18 th Feb Contacted GP in Kent and handed over needs and outcomes of initial assessments and bloods results.

Lessons to date Partnership working and a centralised HUB has provided opportunity to reach and support more people Created transparency, quick collaboration, system benefits, person centred care, reduced duplication for patients and is more up to date accurate info Flexing the model as it evolves, adding a significant prevention opportunity HUB provides alternative place to attend to primary care level needs outside of ED and is engage the ‘missed gaps’ and the difficult to engage IT is key to partnership working and has proved the biggest challenge! Wound care needs are prevalent +++ Physical/MH/Addiction coexisting is prevalent+++ Move on support within Olallo, ED & RTS has been invaluable to promoting healing and holistic care provision Clinic access has increased provision of holistic and system partner orientated care CHIP relationship has been pivotal to success Presence and repeated education is essential across all and jointly Incidences have identified gaps and learning opportunities for future proofing a longer term service CHAIN registration in ED can prove a challenge 15 flexibility is driving output and success thus far Human factors and

Timeline & key Milestones Project live date 2 nd January 2020 – focused on developing process and engaging wider partners All staff in post mid January Bi-Weekly MDTS all partners Education & promotional material across sector February – services ramps up March – exit strategy April - soft evaluation based on achievement of individual outcomes and system impact Make the case for change for sustainability
- Slides: 16