Homeostatic imbalances Pericarditis inflammation of the pericardium Endocarditis

Homeostatic imbalances • Pericarditis inflammation of the pericardium • Endocarditis bacterial infection of the endocardium can lead to valvular stenosis • Myocardial infarction heart attack/coronary • Heart block any damage to the AV node results in irregular beating of ventricles • Murmurs abnormal or unusual hearts sounds
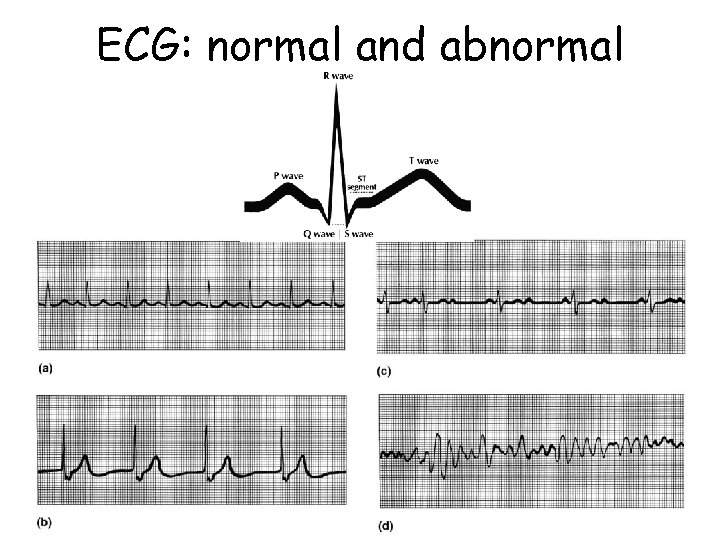
ECG: normal and abnormal

Alterations in Electrocardiogram Clinical Cardiology Concepts for Vets 20 -3

Cardiac Output • Cardiac Output - the amount of blood pumped by a ventricle per minute. Units may be in milliliters or Liters per minute. • Heart Rate - number of cardiac cycles per minute. Average for males = 64 -72/min. Average for females = 72 -80/min. • Stroke Volume - amount of blood pumped out of a ventricle each beat. Average resting stroke volume = 70 ml.

Cardiac Output • CO (m. L/min) =SV (70 m. L/beat) X HR (75 beat/min) – Cardiac output = stroke volume X heart rate = 5250 ml/min • SV= EDV - ESV – Stroke volume = end diastolic volume – end systolic volume • Cardiac reserve is the difference between a person’s maximum cardiac output and cardiac output at rest.

Frank Starling Law of the Heart • The more cardiac muscle is stretched within physiological limits, the more forcibly it will contract. • Rubber band analogy • Increasing volumes of blood in ventricles increase the stretch & thus the force generated by ventricular wall contraction. • Greater stretch means more blood volume is pumped out, up to physical limits.

Regulation of stroke volume • Preload is the degree of stretch on the heart. • Contractility is the force of ventricular contractions. • Afterload is the pressure that must be exceeded to eject blood from the ventricles. • The Frank-Starling law of the heart—preload is the critical factor controlling SV (stroke volume).

Regulation of heart rate • When blood volume drops or the heart is weakened, SV drops and the HR increases. – Positive chronotropic factors increase HR. – Negative chronotropic factors decrease HR. • Extrinsic regulation by the ANS – Sympathetic nervous system increases firing of the pacemaker and enhances Ca 2+ entry into heart cells. – Parasympathetic nervous system reduces heart rate through ACh which opens K+ channels. – Under resting conditions the PNS is dominant

Chemical Regulation • Hormones – Epinephrine enhances HR and contractility – Thyroxine enhances effects of Epi and NE and leads to slower more sustained increase in HR • Ions – Hypocalcemia (Ca 2+)depresses the heart; – Hypercalcemia prolongs the plateau phase and lead to heart irritability – Hyperkalemia (K+) may lead to heart block and cardiac arrest; hypokalemia leads to arrhythmia and weakened contractions. – Excess Na+ blocks Ca 2+ inflow, decreasing contractile strength

Other Factors • Exercise leads to a reduced HR when at rest. • Working large body muscles for at least 20 minutes elevates cardiac output and accelerates metabolism. – Athletes have a larger heart and a resting HR of 40 -60 beats per minute • Increased temperature increases heart rate; decreased temperatures reduce heart rate and oxygen needs.

Homeostatic imbalances • Congestive heart failure – Caused by Coronary artherosclerosis – Caused by Persistent high blood pressure – Caused by Multiple myocardial infarcts – Left side failure Pulmonary congestion – Rights side failure Peripheral congestion

Angina Pectoris • Medical term for chest pain due to coronary heart disease. • It occurs when the myocardium doesn’t get as much blood (Oxygen) as it needs. • Insufficient blood supply is called ischemia. • May initially occur during physical exercise, stress, or extreme temperatures. • It is a sign of increased risk of heart attack.

Cardiac Arrhythmias • Arrhythmias irregular heart rhythms that may lead to fibrillation • Tachycardia: Heart rate in excess of 100 bpm • Bradycardia: Heart rate less than 60 bpm • Sinus arrhythmia: Heart rate varies 5% during respiratory cycle and up to 30% during deep respiration • Premature atrial contractions: Occasional shortened intervals between one contraction and succeeding, frequently occurs in healthy people

Aneurysm • Weakness of the wall of an artery causing an abnormal enlargment or bulge. • The aorta or the arteries that supply the heart, brain, legs or kindeys are most commonly affected.

Atherosclerosis (Arteriosclerosis) • Narrowing and hardening of arteries and impairment of blood flow due to the deposition of fatty materials and calcium in their walls. • Risk factors include: – smoking – inactivity – diabetes – high blood cholesterol – personal or family history of heart disease – Atherosclerosis Animation

Resources • • Heart Sounds & Cardiac Arrhythmias Live Cardiac Exam Video Anatomy Links Cardiac Cycle Graphics Interactive Physiology Review AP II Notes Homepage

Conducting System of Heart
- Slides: 17