Hodgkin Lymphoma Board Review Brad Kahl MD 111803

Hodgkin Lymphoma Board Review Brad Kahl, MD 11/18/03

Hodgkin Lymphoma · · Epidemiology Biology Classification Approach to the Patient

Hodgkin Lymphoma · Epidemiology – – – 14% of malignant lymphomas 0. 5% of all malignancies approximately 8000 new cases/yr in US approximately 1500 deaths/yr over past 30 years · age adjusted incidence rates declined appreciably · mortality rates declined substantially
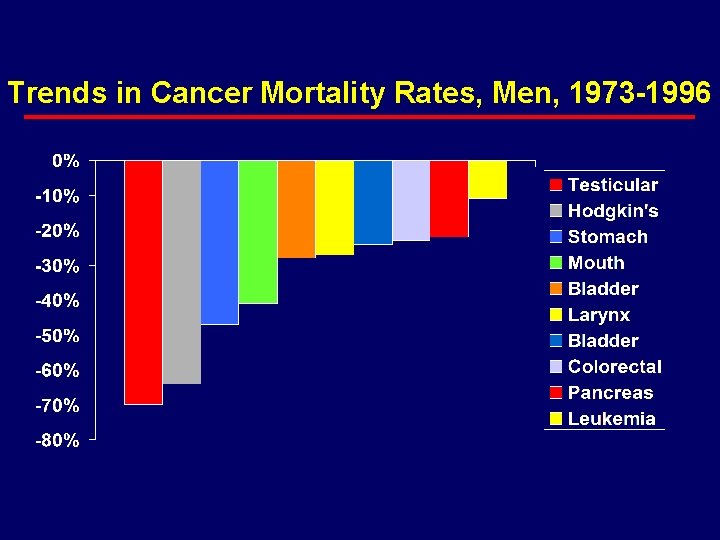
Trends in Cancer Mortality Rates, Men, 1973 -1996
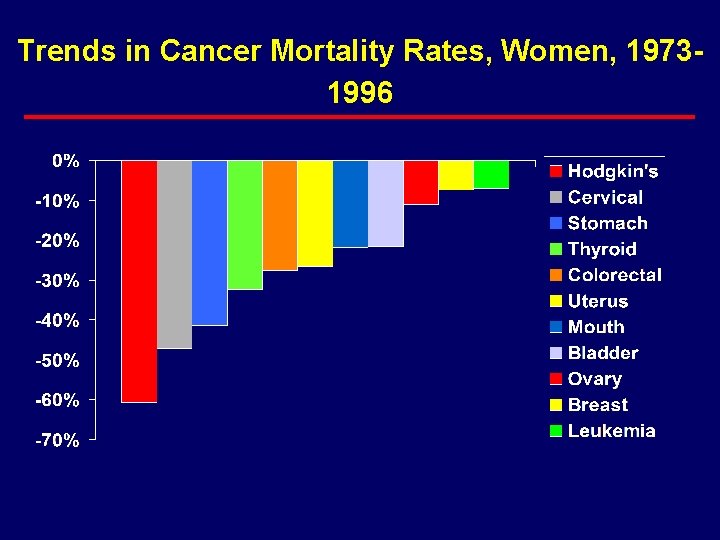
Trends in Cancer Mortality Rates, Women, 19731996

Hodgkin Lymphoma · Epidemiology – men > women – whites > blacks > Asians – no clear risk factors, several implicated · woodworking, farming · familial risk – Concordance for HD in twins ¡ 10/179 in monozygotic vs 0/187 in dizygotic twins (Mack et al, NEJM 1995)

Hodgkin Lymphoma · Risk Factors con’t – HIV · increases risk for HD 8 fold – HD not an AIDS defining illness · NHL 113 x · KS 310 x – Unclear why risk for NHL so much greater in HIV patients compared to HD

Hodgkin Lymphoma · Epstein Barr Virus – EBV DNA found in 50% RS cells – pathogen or passenger – Increased risk for HD after infectious mono (Hjalgrim et al, NEJM 2003) – Absolute risk 1/1000 – Median incubation time from mono to EBV+ HD 4. 1 years – No increased risk for EBV- HD after mono
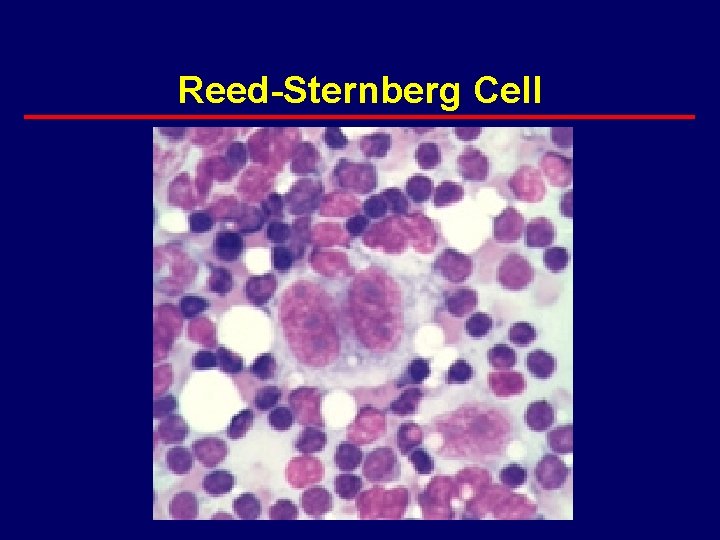
Reed-Sternberg Cell

Hodgkin Biology · Hodgkin’s Disease – Reed-Sternberg cell is the malignant cell · 1% of cells in a biopsy specimen · potent cytokine producing cell (at least 12 cytokines) · cytokines appear to drive the disease process – remainder of cells are background inflammatory cells · lymphocytes, plasma cells, macrophages, eosinophils – RS cell as the malignant cell · origin only worked out within the past 5 years

Hodgkin Biology · RS is a “crippled” germinal center B cell – does not have normal B cell surface antigens – micromanipulation of single RS followed by PCR demonstrates clonally rearranged, but non functional immunoglobulin genes · somatic mutations result in stop codon (no s. Ig) · no apoptotic death malignant transformation – unclear how this occurs; ? EBV – unclear how cells end up with RS phenotype

Hodgkin Lymphoma Classification · “Classic” Hodgkin’s Disease · nodular sclerosis · mixed cellularity · lymphocyte depleted (very rare) · classical lymphocyte rich – HRS cells CD 30 and CD 15 positive · nodular lymphocyte predominant – HRS cells (L&H cells) have B cell markers · CD 20 and surface Immunoglobulin

NLP Hodgkin Lymphoma · differs from classical HD clinically and histopathlogically – preference for peripheral nodal sites – early stage distribution – late median time to recurrence – late recurrences common – low mortality from HD – L&H cells · express CD 20 (B cell marker) · express surface Ig
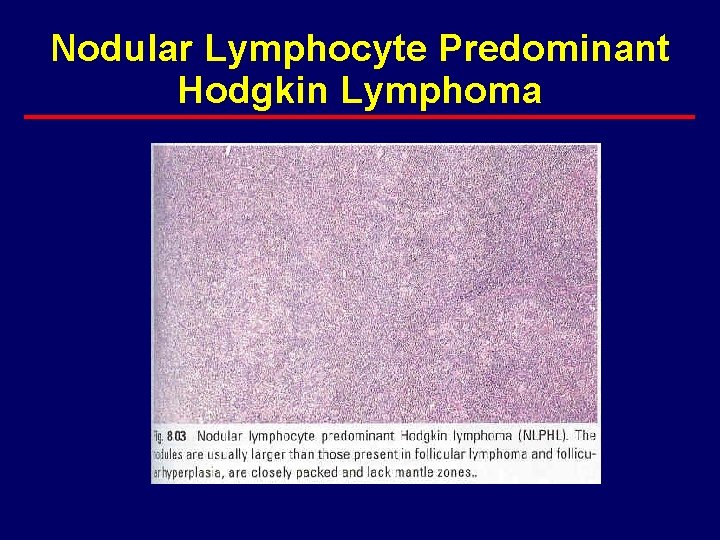
Nodular Lymphocyte Predominant Hodgkin Lymphoma
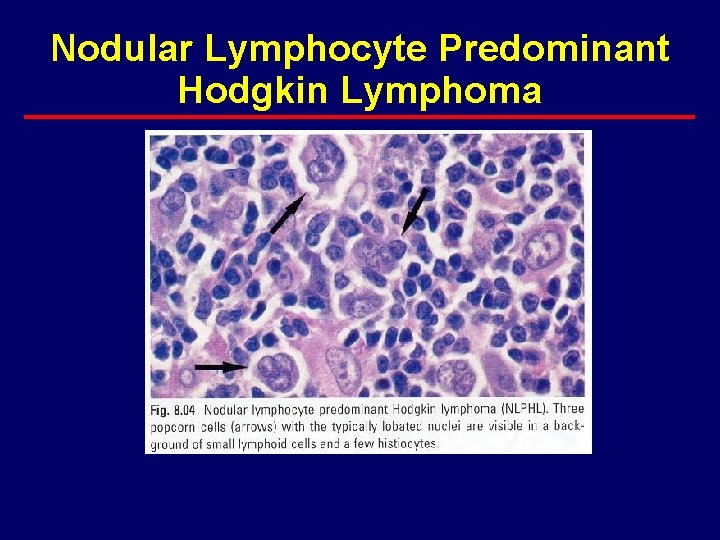
Nodular Lymphocyte Predominant Hodgkin Lymphoma
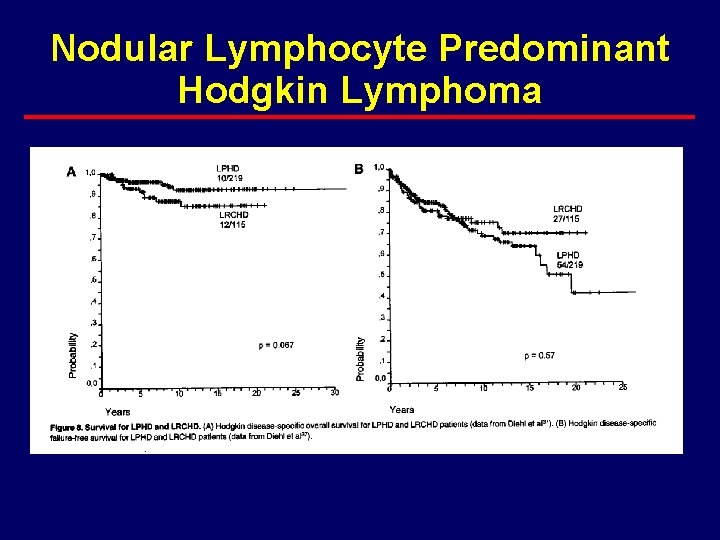
Nodular Lymphocyte Predominant Hodgkin Lymphoma

Nodular Lymphocyte Predominant Hodgkin Lymphoma · Management – No consensus · often treated like classical hodgkins · My view is “do not overtreat” as cure is unlikely and as many deaths from second malignancies as from LPHD (possible related to HD therapy) · I believe watch and wait is reasonable · Often can do IFRT to problem areas as they appear · Rituximab effective in relapse with ORR 85 -100%.
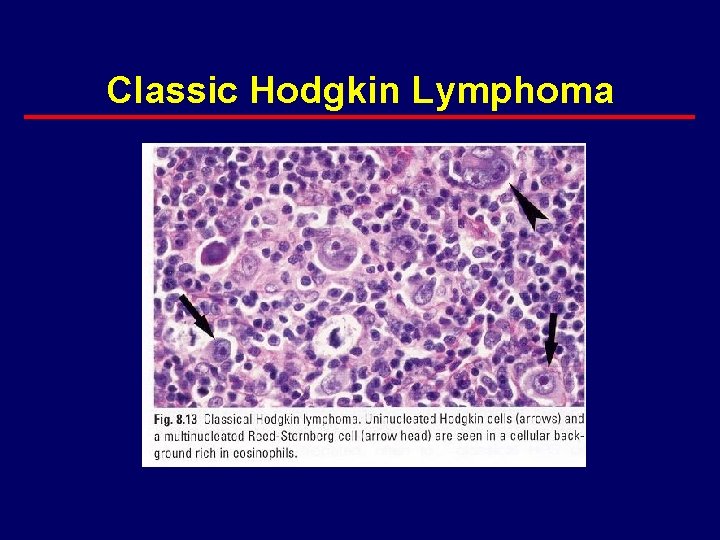
Classic Hodgkin Lymphoma
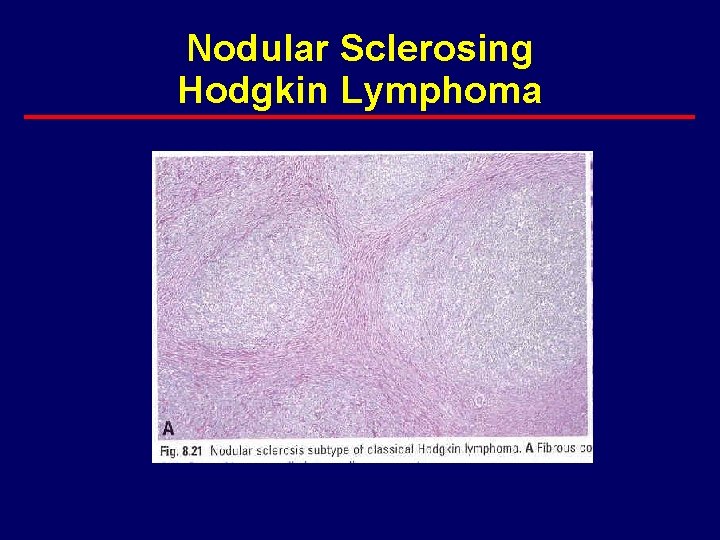
Nodular Sclerosing Hodgkin Lymphoma
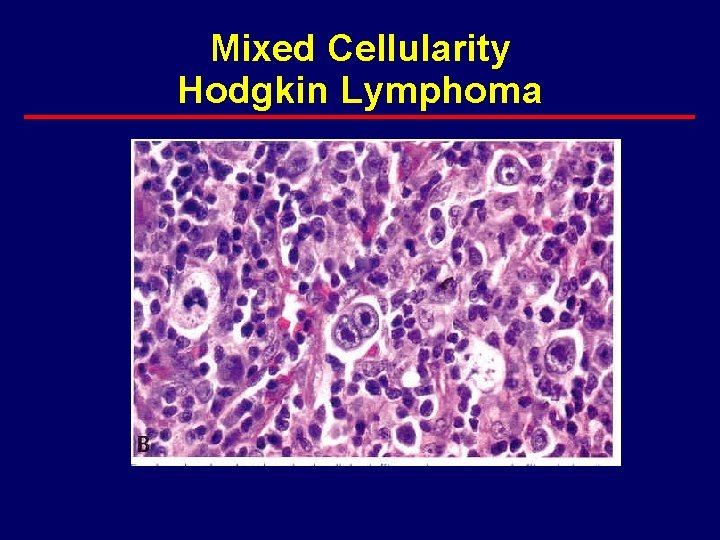
Mixed Cellularity Hodgkin Lymphoma
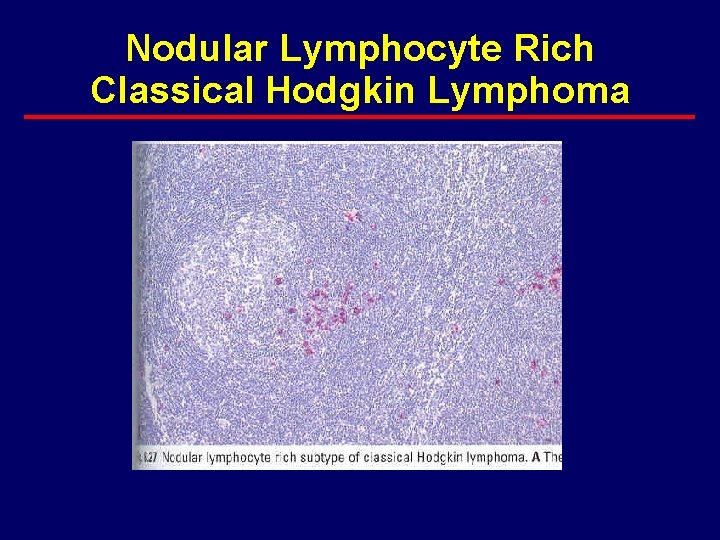
Nodular Lymphocyte Rich Classical Hodgkin Lymphoma
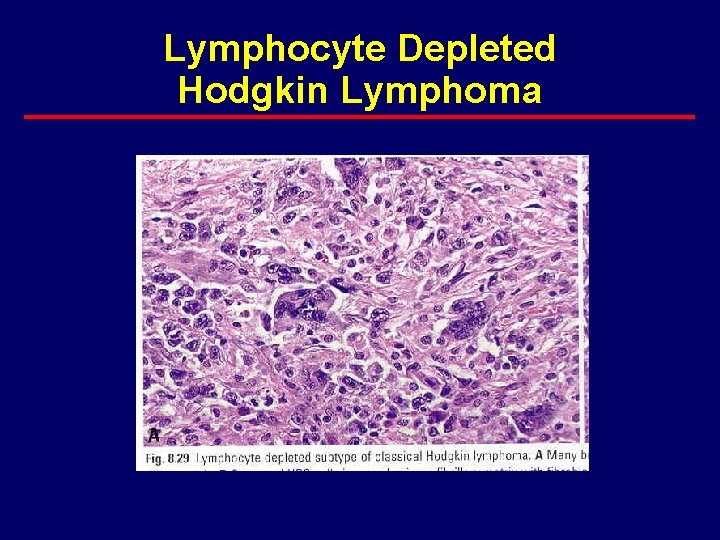
Lymphocyte Depleted Hodgkin Lymphoma

Hodgkin Lymphoma: approach to patient · staging evaluation ·H&P · CBC, diff, plts · ESR, LDH, albumin, LFT’s, Cr · CT scans chest/abd/pelvis, CXR · bone marrow evaluation (for stage IIB and higher) · PET scan may be helpful · PFTs, LVEF when clinically indicated · Fertility counseling · **lymphangiogram or laparotomy**

Modified Ann Arbor Staging Stage I Involvement of a single lymph node region Stage II Involvement of 2 lymph node regions on the same side of the diaphragm Stage III Involvement of lymph node regions on both sides of the diaphragm Stage IV Multifocal involvement of 1 extralymphatic sites ± associated lymph nodes or isolated extralymphatic organ involvement with distant nodal involvement Cancer. 1982; 49: 2112.
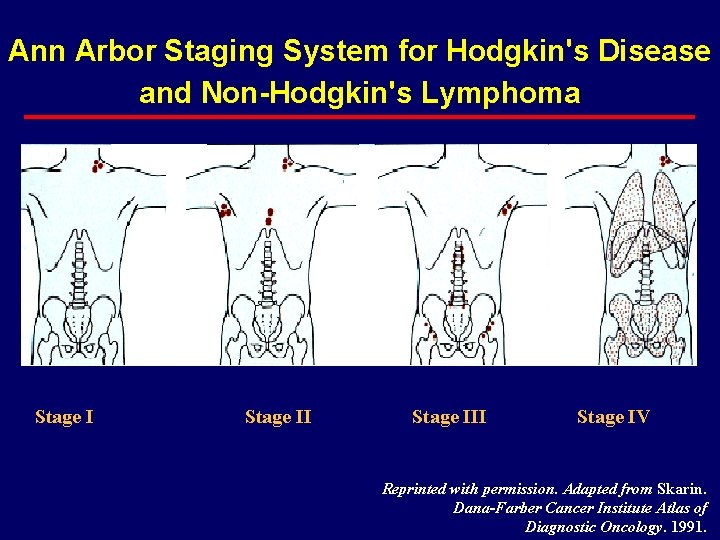
Ann Arbor Staging System for Hodgkin's Disease and Non-Hodgkin's Lymphoma Stage III Stage IV Reprinted with permission. Adapted from Skarin. Dana-Farber Cancer Institute Atlas of Diagnostic Oncology. 1991.
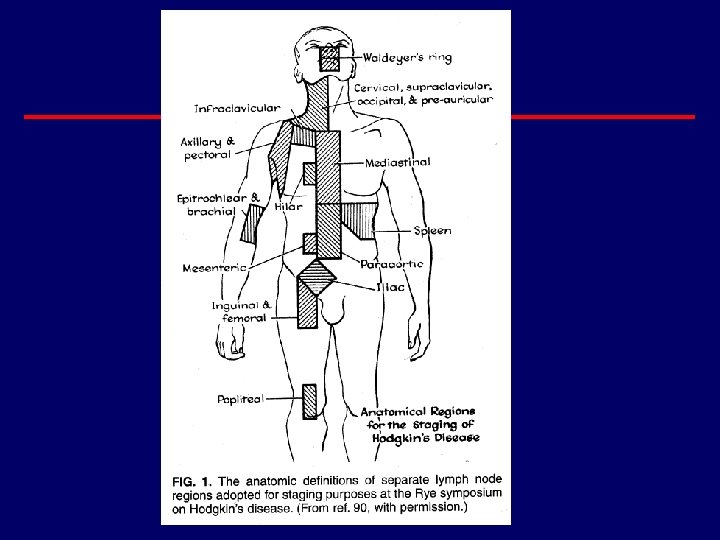

Modified Ann Arbor Staging · “E” designation for extranodal disease · B symptoms · recurrent drenching night sweats during previous month · unexplained, persistent, or recurrent fever with temps above 38 C during the previous month · unexplained weight loss of more than 10% of the body weight during the previous 6 months · Criteria for bulk – 10 cm nodal mass – mediastinal mass > 1/3 thorax diameter

Hodgkin Lymphoma: Prognostic Factors · Adverse prognostic features for stage I & II (EORTC data) · more than 3 nodal sites · bulky adenopathy · ESR > 50 · B symptoms · invasion into critical organs · male · age > 40 · MC or LD subtype – should probably not receive XRT alone if any of the above present (excessive relapse rate)

Hodgkin Lymphoma: Prognostic Factors · Independent adverse prognostic factors – advanced stage (III-IV) · male sex · age > 45 · albumin < 4 gm/dl · Hg. B < 10. 5 mg/dl · stage IV disease · WBC count > 15, 000/mm 3 · lymphocyte count < 600/mm 3 (Hasenclever et al, NEJM 339, 1506 -1514; 1998)
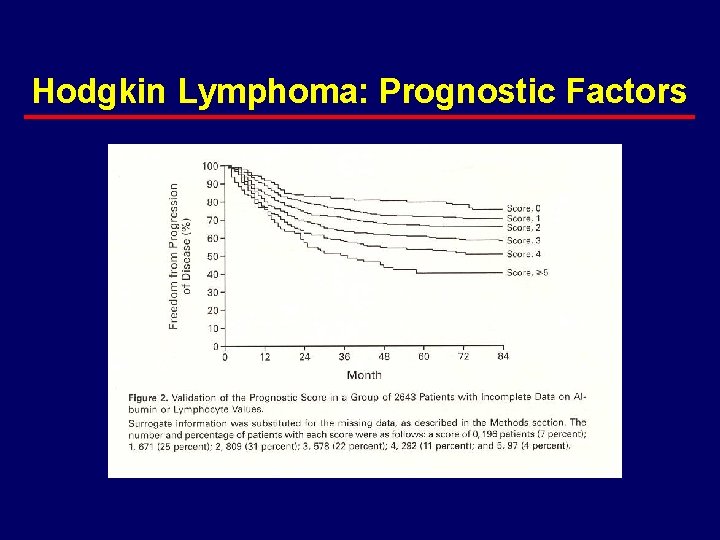
Hodgkin Lymphoma: Prognostic Factors

Hodgkin Lymphoma: Biologic Prognostic Factors · Favorable – EBV in tumor cells · Unfavorable – – – Tissue eosinophila (NSHD) Lymphocyte depletion (NSHD) RS atypia (NSHD) Bcl-2 overexpression P 53 High proliferative rate

Hodgkin Lymphoma · Treatment – approach depends upon stage, prognostic factors, and co-morbidities – Stage I-II · consider XRT, chemotherapy, or combined therapy – Bulky stage I-II · combined modality therapy, usually 6 cycles of chemotherapy – Stage III-IV · ABVD x 6 -8 cycles gold standard

Hodgkin Lymphoma · Results of Treatment stage 5 year overall survival –I 90% –III 80% –IV 65%

Hodgkin Lymphoma: Treatment of limited stage disease · Current general consensus is to administer CMT – ABVD x 4 (consider 6 cycles for bulk) – Followed by IFRT – Definite trend towards limiting the radiation field and possibly lowering the radiation dose due to concern over late effects – Data from 2 large trials · #1: Institute Nazionale Tumori – Enrolled patients with stage I, IIA bulky, and IIEA – Data presented at 2001 ASH meeting

Hodgkin Lymphoma: Treatment of limited stage disease

Hodgkin Lymphoma: Treatment of limited stage disease

Hodgkin Lymphoma: Treatment of limited stage disease · Study #2: Engart et al, JCO Oct 2003. – Included patients with limited stage HD and at least one risk factor · Bulky mediastinal disease · Extranodal disease · Massive splenic disease · ESR > 50 and no B symptoms · ESR > 30 and B symptoms · More that 2 lymph node regions
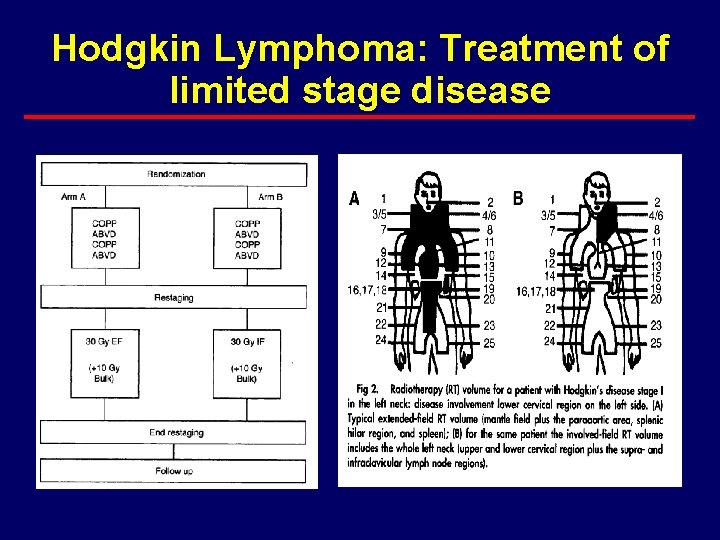
Hodgkin Lymphoma: Treatment of limited stage disease
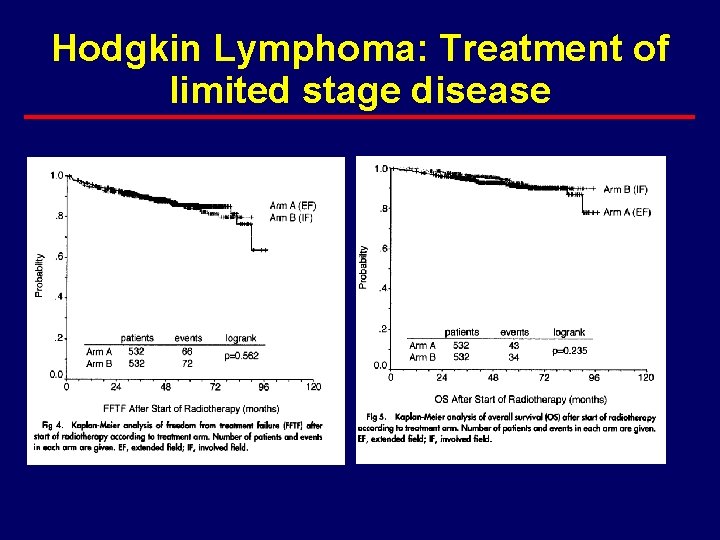
Hodgkin Lymphoma: Treatment of limited stage disease

Hodgkin Lymphoma: Treatment of limited stage disease · More acute toxicities in EFRT · Late toxicities (second CA, cardiac, pulmonary) not statistically different – Trend worse in EFRT arm – Longer follow up will needed · Conclusion from trials 1 and 2 – 4 cycles of chemotherapy plus IFRT equally effective to treatment plans including larger radiation fields

Hodgkin Lymphoma · Excess death rate (relative)* (SEER data) – – – 2 years: 5 years: 10 years: 15 years: 20 years: 5. 6% 8. 8% 14. 3% 19. 4% 23. 9% *compared to age and sex matched control (deaths other than from Hodgkins)

Hodgkin Lymphoma: Late Complications · Radiotherapy appears to confer the most late risk – Actuarial rate of second CA 1%/year with no plateau – In one study the 25 year cumulative risk of breast CA was 16. 3% · Current major focus of current clinical trials to to maintain high cure rate while minimizing late complication · shorter courses of chemotherapy with lower radiation doses in smaller fields · elimination of radiotherapy (some argue for this already)

Hodgkin Lymphoma · Current EORTC trial for stage I-II patients – EBVP x 6 + 36 Gy IF – EBVP x 6 + 20 Gy IF – EBVP x 6 (arm closed do to excessive relapse) · Current GHSG trial for stage I-II patients – – ABVD x 4 + 30 Gy IF ABVD x 4 + 20 GY IF ABVD x 2 + 30 Gy IF ABVD x 2 + 20 GY IF

Hodgkin Lymphoma: Late Complications · Other Late Complications – depends upon treatment modality utilized · XRT vs. MOPP vs. ABVD vs. CMT – issues depends upon the age of patient · relative risks higher in younger patients · absolute risks higher in older patients – Risks of leukemia and infertility appear substantially lower using ABVD rather than MOPP · Infertility 20% vs. 50 -70% – Pulmonary-Bleomycin, Cardiac-adriamycin

Hodgkin Lymphoma: Advanced Disease · More straightforward right now – ABVD is standard – Treat until CR + 2 cycles up to maximum of 8 – No role for routine XRT after chemo ¡(Aleman et al, NEJM June 2003) – Common practice is to administer consolidative XRT to bulky mediastinal disease after chemo · Stanford V, BEACOPP being compared to ABVD in prospective clinical trials currently

Hodgkin Lymphoma: Stem Cell Transplant · Reserved for patients who relapse after chemotherapy (autologous) – Superior to additional conventional chemotherapy in RCT ¡(Schmitz et al, Lancet 2002) · Upfront transplant for poor prognosis disease does not appear superior (2 trials) · Beneficial for the small group of patients with primary refractory HD
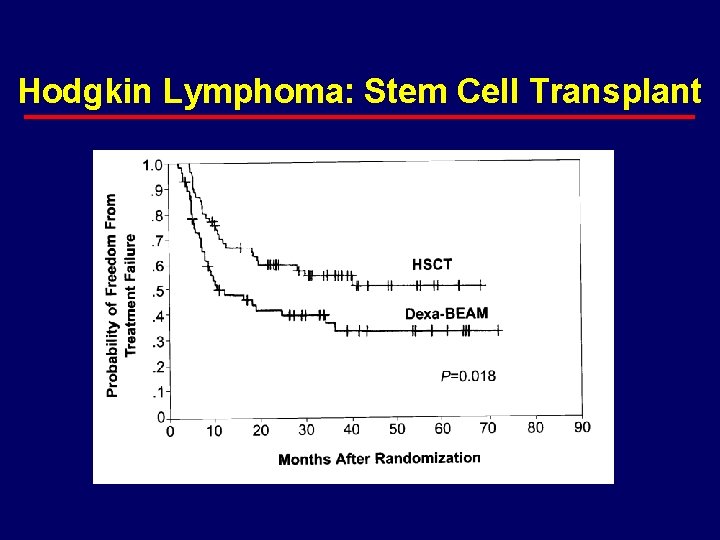
Hodgkin Lymphoma: Stem Cell Transplant

Lymphoma and Pregnancy · 4 th most common malignancy among pregnant females (breast > cervical > ovarian) · no good evidence that pregnancy has a prognostic influence on the lymphoma (except Burkitts) · Staging Issues – CT scans and radioisotope scans contraindicated – rely on PE, labs, CXR, US, MRI, and marrow

Lymphoma and Pregnancy · Therapy during pregnancy – choices will vary on case by case basis – type of lymphoma, gestational age, personal beliefs – therapeutic abortion vs watchful waiting vs limited XRT vs chemotherapy · Indolent NHL (rare) and some Hodgkins – will be able to defer therapy until after delivery

Lymphoma and Pregnancy · Aggressive NHL and Hodgkins requiring therapy – 2 nd and 3 rd trimester · data suggests can give combination chemotherapy with minimal risk to fetus (CHOP or ABVD) · need to plan delivery to avoid neutropenia and thrombocytopenia – 1 st trimester (most difficult situation) · consider therapeutic abortion · risk of fetal malformation with combination chemo approximately 20%

Lymphoma and Pregnancy · Things to avoid – excessive XRT · maximum acceptable dose to fetus 10 Gy – anti-metabolites · methotrexate – regimens heavy in alkylating agents · MOPP
- Slides: 51