Hmmm A B C D 1 1 1

Hmmm A B C D 1$ 1$ 1$ 2$ 2$ 2$ 3$ 3$ 3$ 4$ 4$ 4$ Final Jeopardy 5$ 5$

C 1 $100 Which of the following acute-phase protein levels is/are increased in human plasma after acute inflammation? A. C-reactive protein B. HSP Fo C. Chaperonics D. Fibrinogen E. Albumin F. a, b, c, and d only G. all of the above

C 1 $100 Which of the following acute-phase protein levels is/are increased in human plasma after acute inflammation? A. C-reactive protein B. HSP Fo C. Chaperonics D. Fibrinogen E. Albumin F. a, b, c, and d only G. all of the above
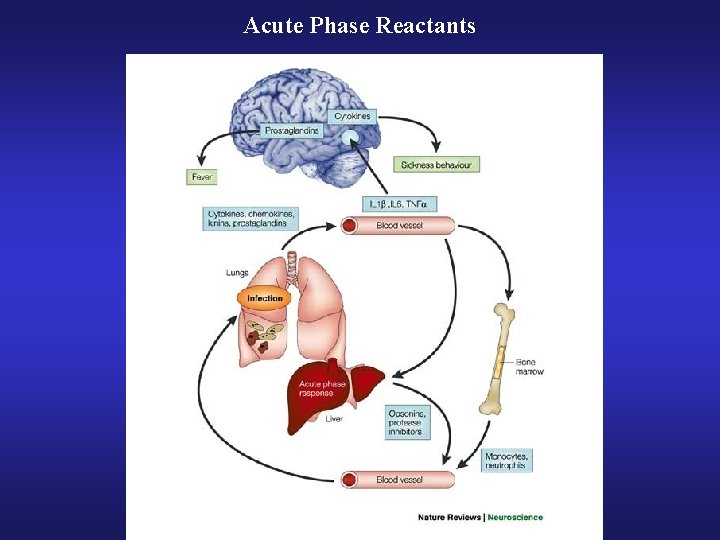
Acute Phase Reactants
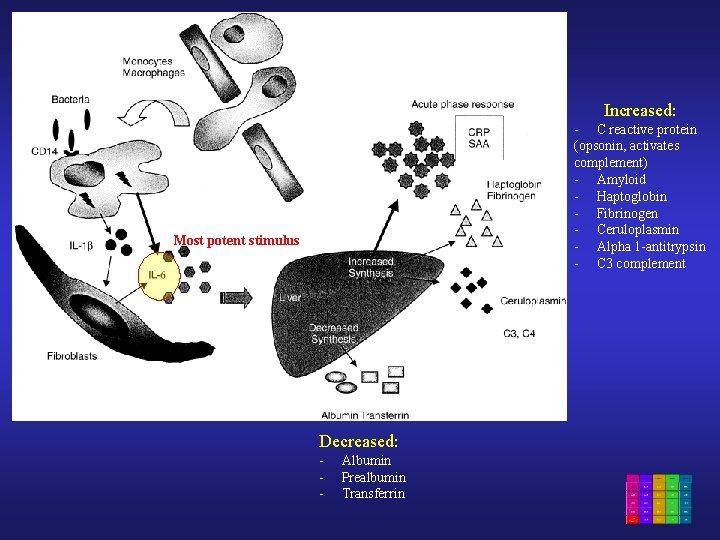
Increased: - C reactive protein (opsonin, activates complement) - Amyloid - Haptoglobin - Fibrinogen - Ceruloplasmin - Alpha 1 -antitrypsin - C 3 complement Most potent stimulus Decreased: - Albumin Prealbumin Transferrin

C 1 $200 Neutrophils are attracted to areas of inflammation and injury. Homing to areas of injury requires the neutrophils to adhere to endothelium in the affected area. This process is mediated by which of the following molecules? A. TNF B. L-selectin C. IL-2 D. NO

C 1 $200 Neutrophils are attracted to areas of inflammation and injury. Homing to areas of injury requires the neutrophils to adhere to endothelium in the affected area. This process is mediated by which of the following molecules? A. TNF B. L-selectin C. IL-2 D. NO
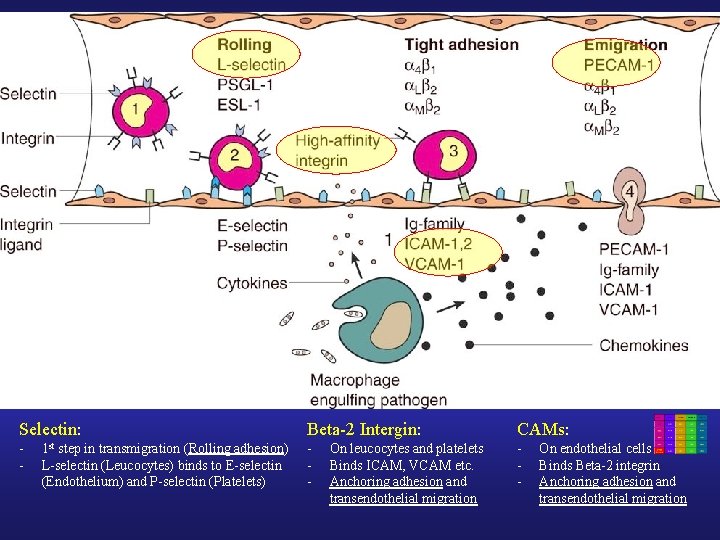
Selectin: Beta-2 Intergin: CAMs: - - - 1 st step in transmigration (Rolling adhesion) L-selectin (Leucocytes) binds to E-selectin (Endothelium) and P-selectin (Platelets) On leucocytes and platelets Binds ICAM, VCAM etc. Anchoring adhesion and transendothelial migration On endothelial cells Binds Beta-2 integrin Anchoring adhesion and transendothelial migration

C 1 $300 Natural Killer cells: A. Are restricted by MHC B. Require previous exposure to antigens C. Require antigen presentation by APCs D. Recognize cells that lack self-MHC E. Are not a part of the body’s natural immune-surveillance for cancer F. Are a type of T cell

C 1 $300 Natural Killer cells: A. Are restricted by MHC B. Require previous exposure to antigens C. Require antigen presentation by APCs D. Recognize cells that lack self-MHC E. Are not a part of the body’s natural immune-surveillance for cancer F. Are a type of T cell

Natural Killer Cells (NK Cells) • Activated by IL-2 • NOT involved in T cell receptor & antigen-MHC recognition • Attack cells with low expression of MHC (missing self) : Viral infections? • Attack cells with bound antibody (Have Fc receptor)

C 1 $400 Which of the following is NOT an oxidant generated in inflammation: A. Superoxide anion radical (O 2 -) B. C. Hydrogen Peroxide (H 2 O 2) Hydroxyl radical (-OH) D. Hypochlorous acid (HOCL-) E. Superoxide dismutase and Catalase

C 1 $400 Which of the following is NOT an oxidant generated in inflammation: A. Superoxide anion radical (O 2 -) B. C. Hydrogen Peroxide (H 2 O 2) Hydroxyl radical (-OH) D. Hypochlorous acid (HOCL-) E. Superoxide dismutase and Catalase
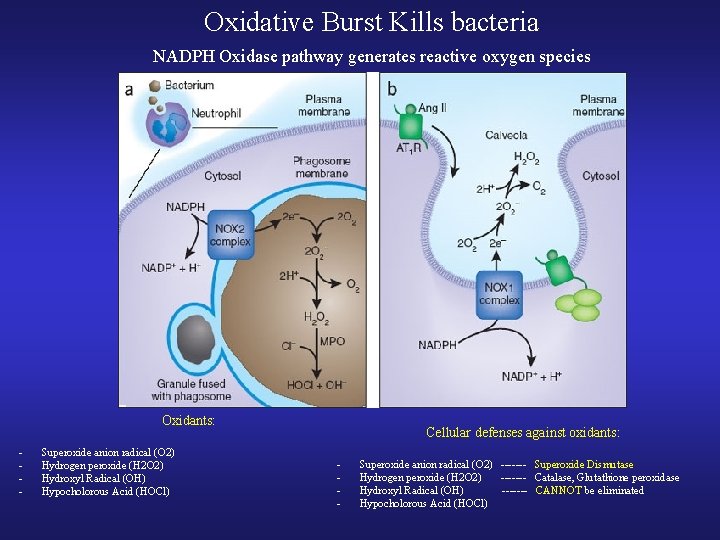
Oxidative Burst Kills bacteria NADPH Oxidase pathway generates reactive oxygen species Oxidants: - Superoxide anion radical (O 2) Hydrogen peroxide (H 2 O 2) Hydroxyl Radical (OH) Hypocholorous Acid (HOCl) Cellular defenses against oxidants: - Superoxide anion radical (O 2) ------- Superoxide Dismutase Hydrogen peroxide (H 2 O 2) ------- Catalase, Glutathione peroxidase Hydroxyl Radical (OH) ------- CANNOT be eliminated Hypocholorous Acid (HOCl)

- Primary mechanism of injury for O 2 radicals: - DNA damage - RBCs: - Have antioxidant properties - Have Superoxide dismutase and Catalase - Chronic Granulomatous Disease: - Enzyme defect in PMNs and macrophages - Leads to decreased superoxide radical formation

C 1 final Steve is on the million dollar question in “Who wants to be a Millionare’. He is phoning a friend and its you…… Guess the correct mechanism of action for the drug below? A. Glucocorticoids stimulate phospholipase and prostaglandin synthesis B. ASA reversibly and non-selectively inhibits COX and inhibits prostaglandin synthesis C. Celebrex is a selective COX 2 inhibitor which only acts at inflamed tissues and decreases incidence of ulcers (But causes increased incidence of CVS S/E) D. NSAIDs are nonreversible COX inhibitors that are both nonselective (Ibuprofen, Naproxen) and selective (Celebrex) E. I quit this residency %&%$#$ Timer

C 1 final Steve is on the million dollar question in “Who wants to be a Millionare’. He is phoning a friend and its you…… Guess the correct mechanism of action for the drug below? A. Glucocorticoids stimulate phospholipase and prostaglandin synthesis B. ASA reversibly and non-selectively inhibits COX and inhibits prostaglandin synthesis C. Celebrex is a selective COX 2 inhibitor which only acts at inflamed tissues and decreases incidence of ulcers (But causes increased incidence of CVS S/E) D. NSAIDs are nonreversible COX inhibitors that are both nonselective (Ibuprofen, Naproxen) and selective (Celebrex) E. I quit this residency %&%$#$
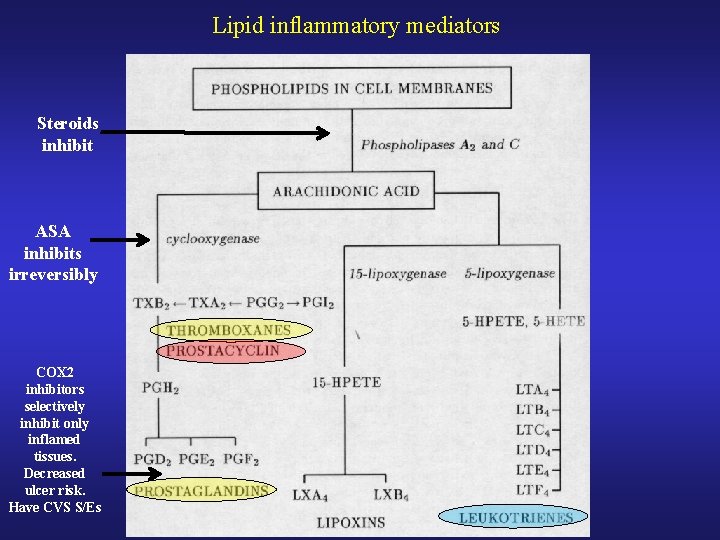
Lipid inflammatory mediators Steroids inhibit ASA inhibits irreversibly COX 2 inhibitors selectively inhibit only inflamed tissues. Decreased ulcer risk. Have CVS S/Es
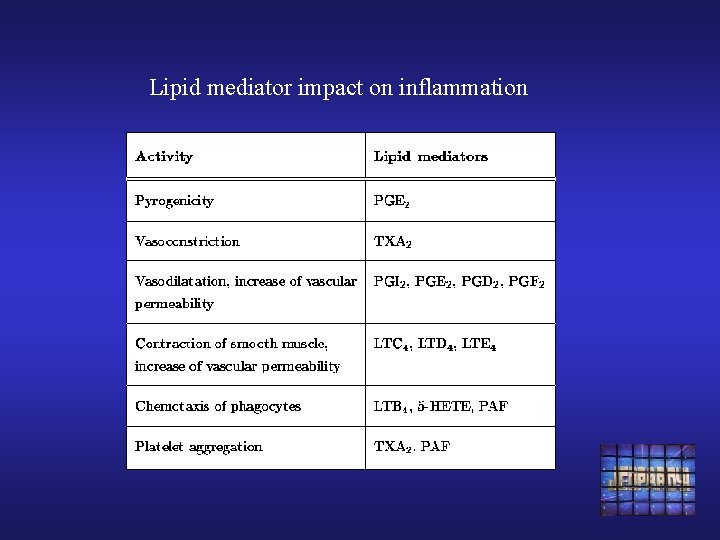
Lipid mediator impact on inflammation

C 2 $100 T cells recognize only those antigens associated with surface major histocompatibility complex molecules by specialized antigen-presenting cells. Antigen presenting cells do NOT include: A. Dendritic cells B. B cells C. Endothelial cells D. Macrophages E. I give up

C 2 $100 T cells recognize only those antigens associated with surface major histocompatibility complex molecules by specialized antigen-presenting cells. Antigen presenting cells do NOT include: A. Dendritic cells B. B cells C. Endothelial cells D. Macrophages E. I give up

C 2 $200 MHC complex: A. Class I activates CD 8 cells B. Class II activates CD 4 cells C. Class I is present on all nucleated cells while Class II only on B cells and APC D. Class I activates cytotoxic T cells while Class II stimulates antibody formation E. All of the above

C 2 $200 MHC complex: A. Class I activates CD 8 cells B. Class II activates CD 4 cells C. Class I is present on all nucleated cells while Class II only on B cells and APC D. Class I activates cytotoxic T cells while Class II stimulates antibody formation E. All of the above

C 2 $300 Which activation sequence is completely TRUE? A. Viral protein bound to class I MHC cell surface recognized by CD 4 T cells B. Bacteria endocytosed bound to class I MHC cell surface recognized by CD 4 T cell and B cells Activation of B cells into plasma cells and memory B cells C. Macrophage (APC) Helper T cell Killer T cell, NK cells, memory T cell, cytotoxic T cell D. Macrophage (APC) B cells forms memory B cells (actively releases antibody) and plasma cells (for future response)

C 2 $300 Which activation sequence is completely TRUE? A. Viral protein bound to class I MHC cell surface recognized by CD 4 T cells B. Bacteria endocytosed bound to class I MHC cell surface recognized by CD 4 T cell and B cells Activation of B cells into plasma cells and memory B cells C. Macrophage (APC) Helper T cell Killer T cell, NK cells, memory T cell, cytotoxic T cell D. Macrophage (APC) B cells forms memory B cells (actively releases antibody) and plasma cells (for future response)

C 2 $400 Which of the following IS true? 2 -4 a (Type a clue in the form of a statement) A. Supressor T cells (CD 8) have no role in regulating CD 4 and CD 8 cells B. Cytotoxic T cells (CD 8) recognize and attack non-self antigens attached to MHC class II receptors C. Defect in cell mediated immunity leads to infection with intracellular pathogens (TB, viruses) D. Intradermal skin test (TB skin test) is used to test antibody-mediated immunity

C 2 $400 Which of the following IS true? A. Supressor T cells (CD 8) have no role in regulating CD 4 and CD 8 cells B. Cytotoxic T cells (CD 8) recognize and attack non-self antigens attached to MHC class II receptors C. Defect in cell mediated immunity leads to infection with intracellular pathogens (TB, viruses) D. Intradermal skin test (TB skin test) is used to test antibody-mediated immunity

C 2 $500 Which of the following is NOT true? A. Helper T cells (CD 4) release IL 2 which causes B cells to mature into plasma cells B. Helper T cells (CD 4) release IL 4 which causes cytotoxic T cell maturation C. Th 1 and Th 2 helper cells both predominantly release proinflammatory cytokines D. Helper T cells (CD 4) are involved in delayed type hypersensitivity (by attracting inflammatory cells by chemokine secretion)

C 2 $500 Which of the following is NOT true? A. Helper T cells (CD 4) release IL 2 which causes B cells to mature into plasma cells B. Helper T cells (CD 4) release IL 4 which causes cytotoxic T cell maturation C. Th 1 and Th 2 helper cells both predominantly release proinflammatory cytokines D. Helper T cells (CD 4) are involved in delayed type hypersensitivity (by attracting inflammatory cells by chemokine secretion)
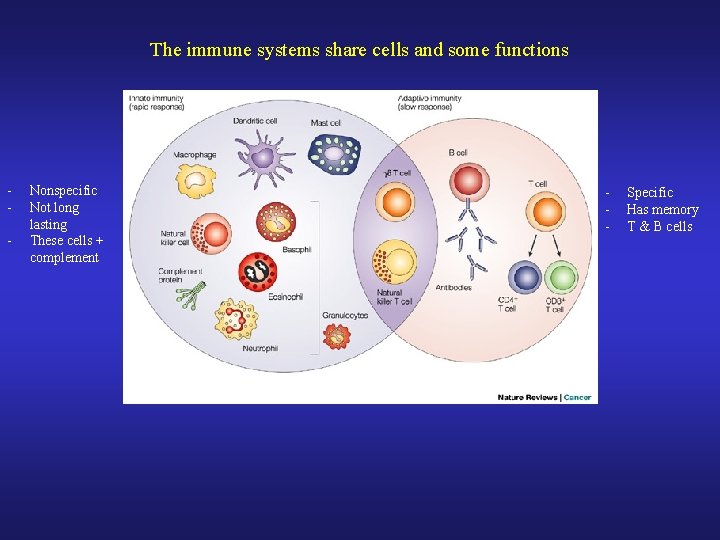
The immune systems share cells and some functions - Nonspecific Not long lasting These cells + complement - Specific Has memory T & B cells
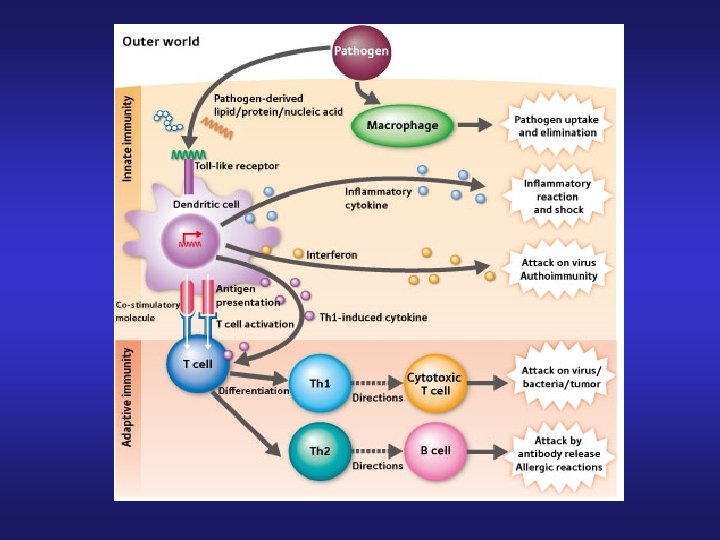

T Cells • Helper T cells (CD 4): • Releases: • IL-2 Activated cytotoxic T cells and NK cells (Th 1) • IL-4 Activates B cells into plasma and memory cells (Th 2) • IFN-gamma Potentiates macrophage bactericidal property • Cytotoxic T cells (CD 8): • Attacks cells damaged, infected or dysfunctional • T cell receptor attaches to MHC Class I with bound antigen releases perforin + granulysin (pores in cell membrane and lysis) + releases granzymes (causes apoptosis)
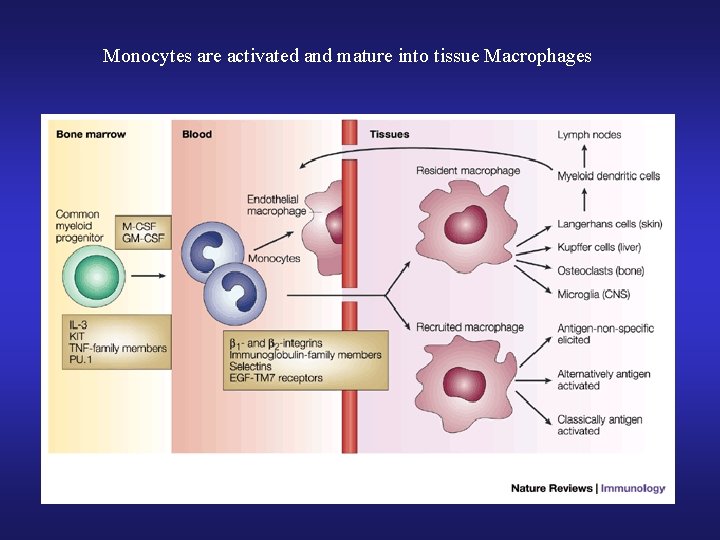
Monocytes are activated and mature into tissue Macrophages
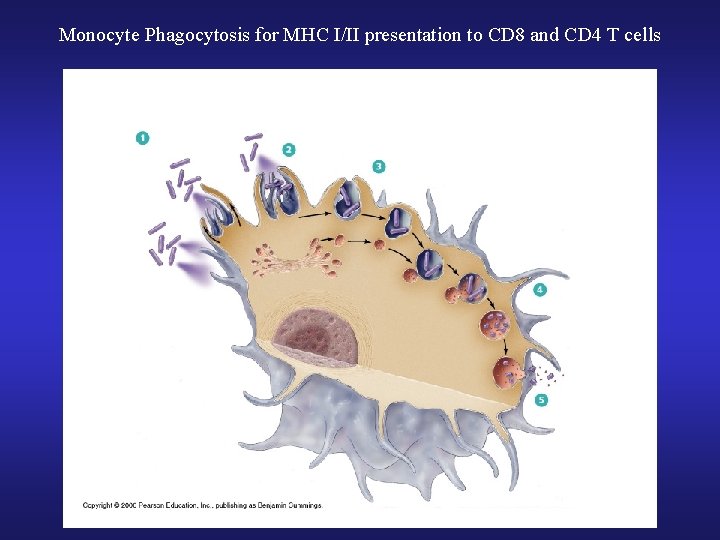
Monocyte Phagocytosis for MHC I/II presentation to CD 8 and CD 4 T cells
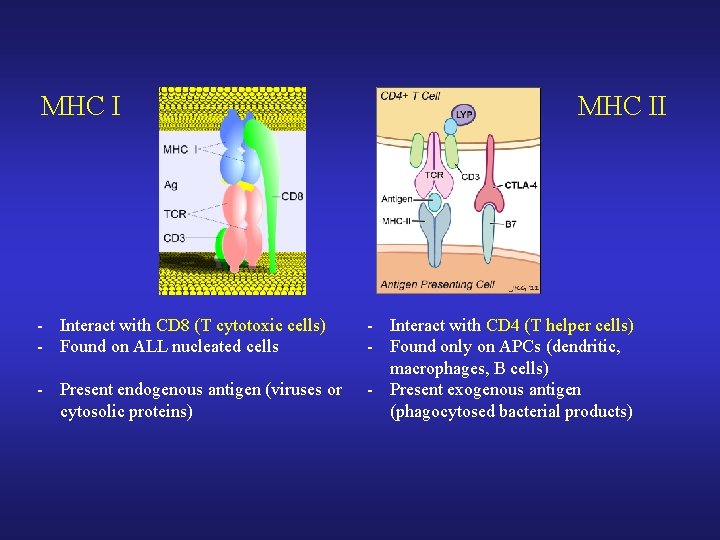
MHC I - Interact with CD 8 (T cytotoxic cells) - Found on ALL nucleated cells - Present endogenous antigen (viruses or cytosolic proteins) MHC II - Interact with CD 4 (T helper cells) - Found only on APCs (dendritic, macrophages, B cells) - Present exogenous antigen (phagocytosed bacterial products)
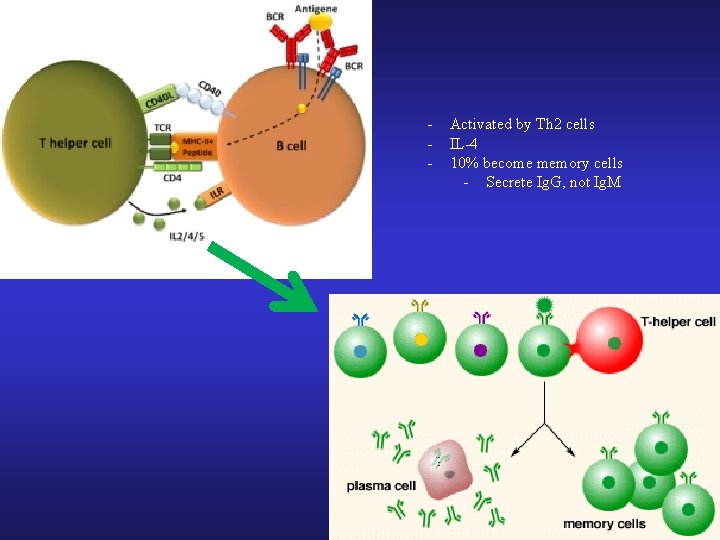
- Activated by Th 2 cells IL-4 10% become memory cells - Secrete Ig. G, not Ig. M
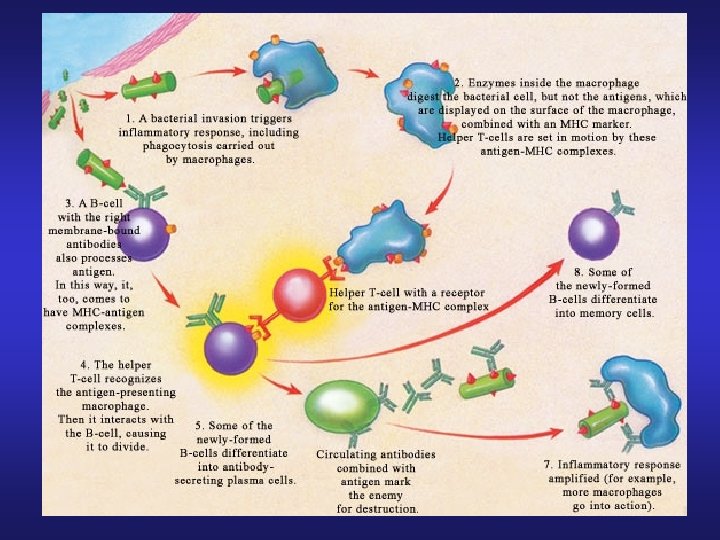
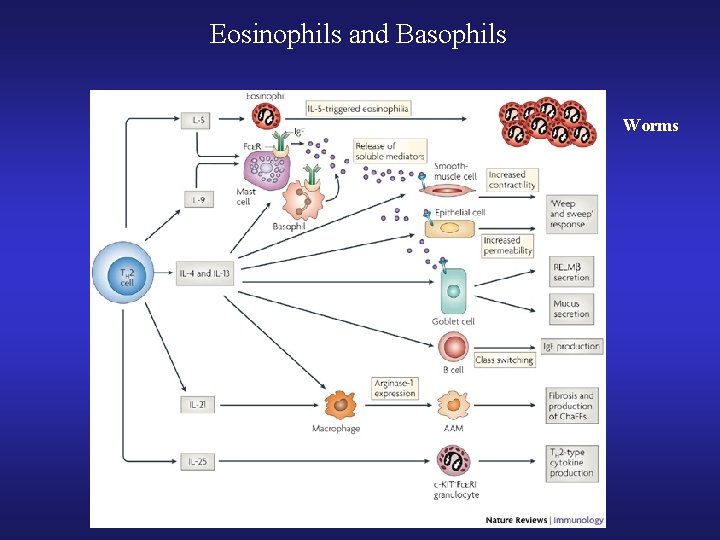
Eosinophils and Basophils Worms

C 3 $100 Activation of the classical complement pathway is caused by which of the following stimuli? A. Mannose B. Microbial cell surfaces C. Interleukin-2 D. Antigen-antibody complexes

C 3 $100 Activation of the classical complement pathway is caused by which of the following stimuli? A. Mannose B. Microbial cell surfaces C. Interleukin-2 D. Antigen-antibody complexes

C 3 $200 Which of the following regarding complement activation is NOT true: A. Alternate pathway is activated by antigen-antibody complex B. Classic pathway is activated by direct binding of pathogen to C 1 C. Factors C 1, C 2 and C 3 are found only in the classic pathway D. Endotoxin and bacteria activate the alternate pathway leading to C 3 activation E. Factors B, D and P are found only in the alternate pathway

C 3 $200 Which of the following regarding complement activation is NOT true: A. Alternate pathway is activated by antigen-antibody complex B. Classic pathway is activated by direct binding of pathogen to C 1 C. Factors C 1, C 2 and C 3 are found only in the classic pathway D. Endotoxin and bacteria activate the alternate pathway leading to C 3 activation E. Factors B, D and P are found only in the alternate pathway
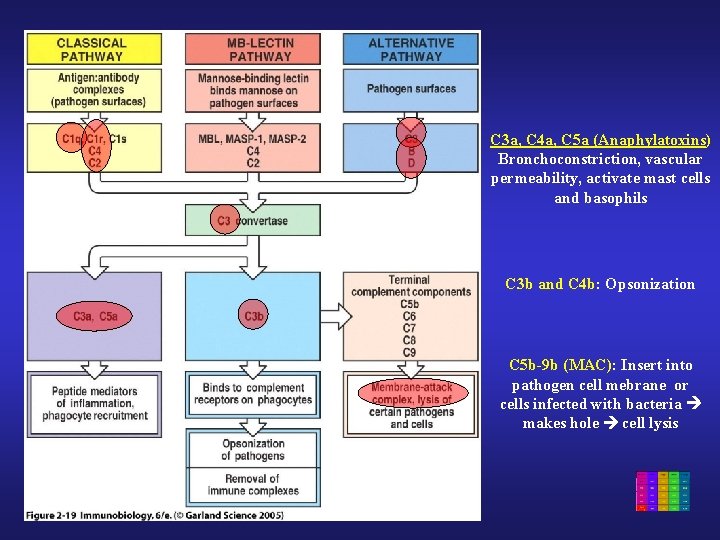
C 3 a, C 4 a, C 5 a (Anaphylatoxins) Bronchoconstriction, vascular permeability, activate mast cells and basophils C 3 b and C 4 b: Opsonization C 5 b-9 b (MAC): Insert into pathogen cell mebrane or cells infected with bacteria makes hole cell lysis

C 3 $300 Antibody functions include: A. Ig. A and Ig. D fix complement B. Ig. A and Ig. G are opsonins C. All have a variable region recognized by only viruses D. All have a constant region recognized by PMNs and macrophages

C 3 $300 Antibody functions include: A. Ig. A and Ig. D fix complement B. Ig. A and Ig. G are opsonins C. All have a variable region recognized by only viruses D. All have a constant region recognized by PMNs and macrophages

C 3 $400 Which of the following is TRUE regarding antibodies: A. Ig. M is the initial antibody produced after exposure to antigen B. Ig. G is the most abundant antibody in the body, can cross placenta and protects the newborn C. Ig. A is found in secretions, Peyers patches in gut, breast milk and helps prevent microbial adherence and invasion in gut D. Ig. E is involved in allergic reactions, parasitic infections E. Ig. D is a membrane bound receptor on T cells F. A, B, C and D ONLY

C 3 $400 Which of the following is TRUE regarding antibodies: A. Ig. M is the initial antibody produced after exposure to antigen B. Ig. G is the most abundant antibody in the body, can cross placenta and protects the newborn C. Ig. A is found in secretions, Peyers patches in gut, breast milk and helps prevent microbial adherence and invasion in gut D. Ig. E is involved in allergic reactions, parasitic infections E. Ig. D is a membrane bound receptor on T cells F. A, B, C and D ONLY
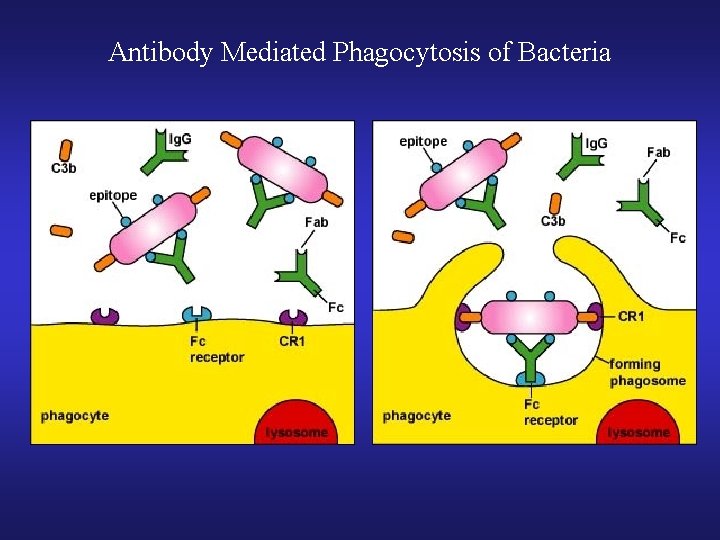
Antibody Mediated Phagocytosis of Bacteria

• Ig. M: • Primary immune response (first antibody made) • Activates complement AND opsonin for phagocytosis • Does NOT cross placenta • Lack of Ig. M after splenectomy leads to OPSS • Ig. G: • Most common Ab overall • Secondary immune response • Activates complement AND opsonin for phagocytosis • Crosses placenta (protection in newborn) • Type II and III Hypersensitivity reaction • Ig. E: • Type I Hypersensitivity reaction and parasitic infection • Ig. A: • Mucosal immunity (Found in secretions) • Plasma cells release Ig. A Taken up by epithelial cells and released on mucosal luminal surface Ig. A bids to pathogen to prevent its adherence to mucosal cells
C 3 $500 Match the 2 columns below for the type of hypersensitivity reaction: A. Type I SLE B. Type II Asthma, allergic reactions C. Type III ITP, acute hemolytic reactions D. Type IV Graft versus host disease
C 3 $500 Match the 2 columns below for the type of hypersensitivity reaction: A. Type I Asthma, allergic reactions B. Type II ITP, acute hemolytic reactions C. Type III SLE D. Type IV Graft versus host disease

• Type I: • Asthma, allergic reactions (lymphazurin blue), anaphylaxis • Requires re-exposure • Ig. E mediated (Antigen interacts with Ig. E bound to mast cells and basophils) • Histamine mediated response, Bradykinin causes pain • Type II: • ITP, acute hemolytic reactions, hyperacute rejection • Ig. G or Ig. M mediated (activates either cell mediated immunity OR activates complement) • Type III: • SLE, serum sickness (anivenom) • Antigen-antibody complexes (Ig. G mediated) deposit in vessel walls and induce inflammation (Antibodies NOT bound to cell surface as in Type II) • Type IV: • Graft versus host disease, chronic rejection, PPD test, contact dermatitis • T cell mediated response (Antibody independent), takes 2 -3 days

C 4 $100 Apoptosis is characterized by which of the following? A. loss of cell membrane integrity B. Inflammation C. DNA fragmentation D. cytokine production

C 4 $100 Apoptosis is characterized by which of the following? A. loss of cell membrane integrity B. Inflammation C. DNA fragmentation D. cytokine production

C 4 $200 Cellular injury from oxidants may be manifested by which of the following? A. Cell membrane lipid peroxidation B. DNA strand breaks C. Cytoskeletal disassembly D. Depletion of adenosine triphosphate E. a, b, and c only F. all of the above

C 4 $200 Cellular injury from oxidants may be manifested by which of the following? A. Cell membrane lipid peroxidation B. DNA strand breaks C. Cytoskeletal disassembly D. Depletion of adenosine triphosphate E. a, b, and c only F. all of the above
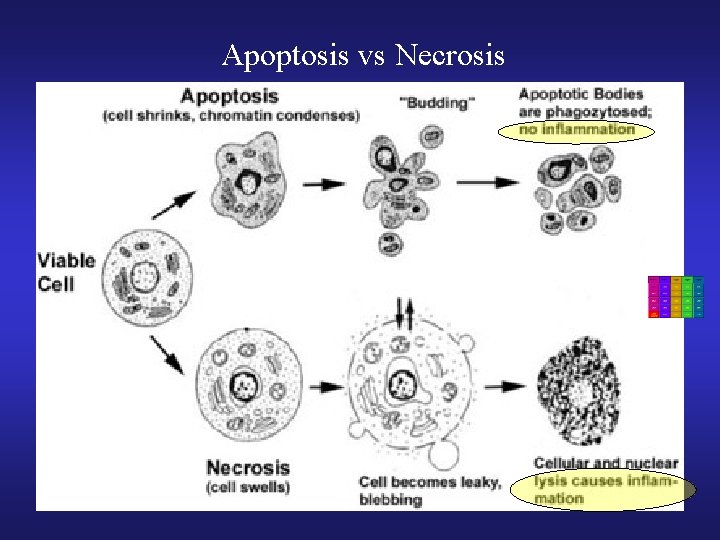
Apoptosis vs Necrosis

C 4 $300 You are participating in a race……. . You overtake the second person What position are you in?

C 4 $300 2 nd place

C 4 $400 Match the 2 columns below for the predominant cell type by day s/p injury: A. 1 st hour Macrophages B. Days 0 -2 Fibroblasts C. Days 3 -4 Platelets D. Days 5 and on PMNs

C 4 $400 Match the 2 columns below for the predominant cell type by day s/p injury: A. 1 st hour Platelets B. Days 0 -2 PMNs C. Days 3 -4 Macrophages D. Days 5 and on Fibroblasts

C 4 $500 Which of the following is the KEY cell and the KEY factor in wound healing? A. Macrophage, PDGF (Platelet derived Growth Factor) B. Platelet, PDGF C. Macrophage, PAF (Platelet Activating Factor) D. Fibroblast, FGF (Fibroblast Growth Factor) E. PMNs, EGF (Epidermal Growth Factor) F. Macrophage, TGF-B

C 4 $500 Which of the following is the KEY cell and the KEY factor in wound healing? A. Macrophage, PDGF (Platelet derived Growth Factor) B. Platelet, PDGF C. Macrophage, PAF (Platelet Activating Factor) D. Fibroblast, FGF (Fibroblast Growth Factor) E. PMNs, EGF (Epidermal Growth Factor) F. Macrophage, TGF-B

Wound Healing • Predominant cell: • Macrophage • Predominant growth factor: • PDGF • Predominant cytokines: • IL-1 and TNF alpha • Order of cell arrival in wound: • Platelets PMNs (day 0 -2) Macrophages (day 3 -4) Fibroblasts (day 5 on)

C 5 $100 Aspirin and non-steroidal anti-inflammatory drugs interfere with platelet function via their activity against which enzyme? A. Thromboxane synthase B. Nitric oxide synthase C. Phospholipase C D. Mitogen-activated protein kinase

C 5 $100 Aspirin and non-steroidal anti-inflammatory drugs interfere with platelet function via their activity against which enzyme? A. Thromboxane synthase B. Nitric oxide synthase C. Phospholipase C D. Mitogen-activated protein kinase

C 5 $200 Platelets have a wide array of functions in inflammation. Which of the following is/are among these? A. Synthesis and release of vasoactive eicosanoids B. Release of chemotactic factors C. Adherence to and coating of bacterial and tumor cells D. Increase of vascular permeability E. Phagocytosis of bacteria F. a, b, c, and d only G. all of the above

C 5 $200 Platelets have a wide array of functions in inflammation. Which of the following is/are among these? A. Synthesis and release of vasoactive eicosanoids B. Release of chemotactic factors C. Adherence to and coating of bacterial and tumor cells D. Increase of vascular permeability E. Phagocytosis of bacteria F. a, b, c, and d only G. all of the above

Platelets • Tissue Injury exposed collagen • PAF released from endothelium recruits platelets, leucocytes PDGF released by platelets PMN and macrophage recruitment • Tissue factor released from endothelium activates clotting cascade fibrin crosslinks platelets Platelet plug formed • vasoconstriction from platelet and endothelial TXA 2 • Platelets release histamine vasodilation (late) Edema and leucocyte migration • PDGF: KEY growth factor in wound healing • Chemotactic • Activates inflammatory cells and fibroblasts • Angiogenesis and accelerates wound healing • TGF-beta: Immunosupressive
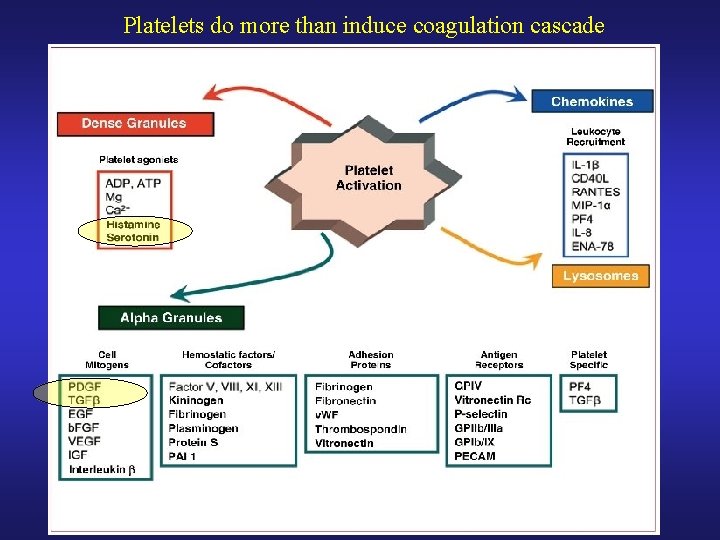
Platelets do more than induce coagulation cascade
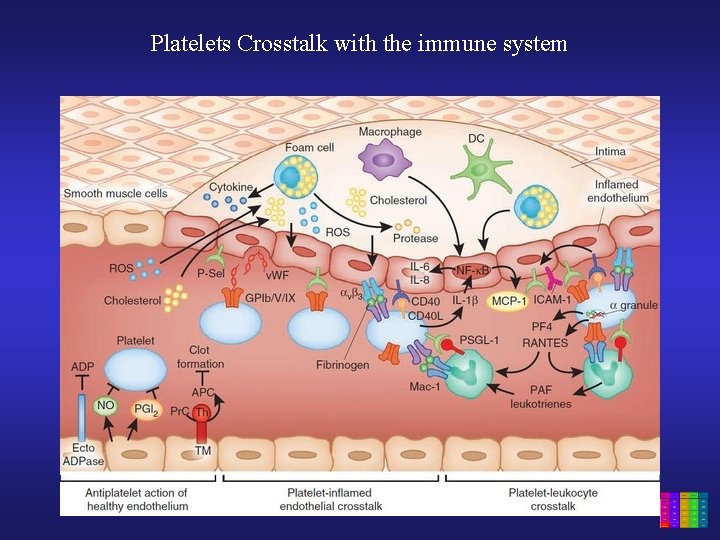
Platelets Crosstalk with the immune system

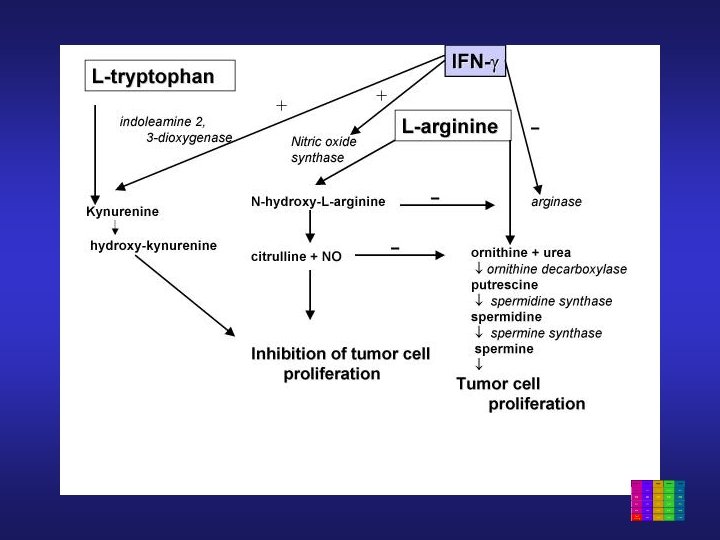
C 5 $300 Nitric oxide is ubiquitous signaling molecule, active in many aspects of inflammation. The effects of NO are transient, in part because of rapid inactivation. Which of the following molecules is involved in inactivation of NO? A. Copper B. Hemoglobin C. L-arginine D. Citrulline

C 5 $300 Nitric oxide is ubiquitous signaling molecule, active in many aspects of inflammation. The effects of NO are transient, in part because of rapid inactivation. Which of the following molecules is involved in inactivation of NO? A. Copper B. Hemoglobin C. L-arginine D. Citrulline

C 5 $400 TNF alpha is responsible for all the following except: A. Principally produced by macrophages B. Increases cell adhesion molecules (ICAM, selectins) C. Is a procoagulant D. Causes cachexia in cancer patients E. Causes myocardial excitement in high concentrations F. Activated PMNs and other macrophages Growth factor production cell recruitment

C 5 $400 TNF alpha is responsible for all the following except: A. Principally produced by macrophages B. Increases cell adhesion molecules (ICAM, selectins) C. Is a procoagulant D. Causes cachexia in cancer patients E. Causes myocardial excitement in high concentrations F. Activated PMNs and other macrophages Growth factor production cell recruitment

C 5 $500 Match the following: A. IL-1 Increases hepatic acute phase proteins B. IL-6 Chemotaxis of PMNs and angiogenesis C. IL-8 Released by alveolar macrophages in atelectasis causes fever (PGE 2 mediated) A. IL-10 Down regulation of immune response

C 5 $500 Match the following: A. IL-1 Released by alveolar macrophages in atelectasis causes fever (PGE 2 mediated) B. IL-6 Increases hepatic acute phase proteins C. IL-8 Chemotaxis of PMNs and angiogenesis D. IL-10 Down regulation of immune response
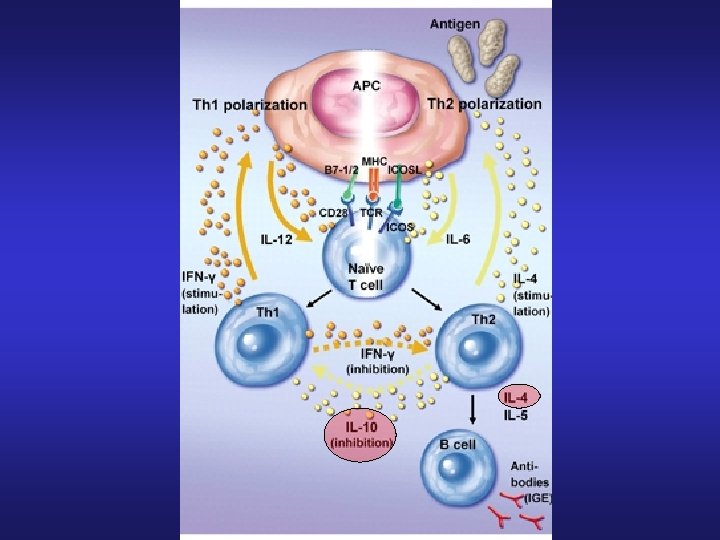
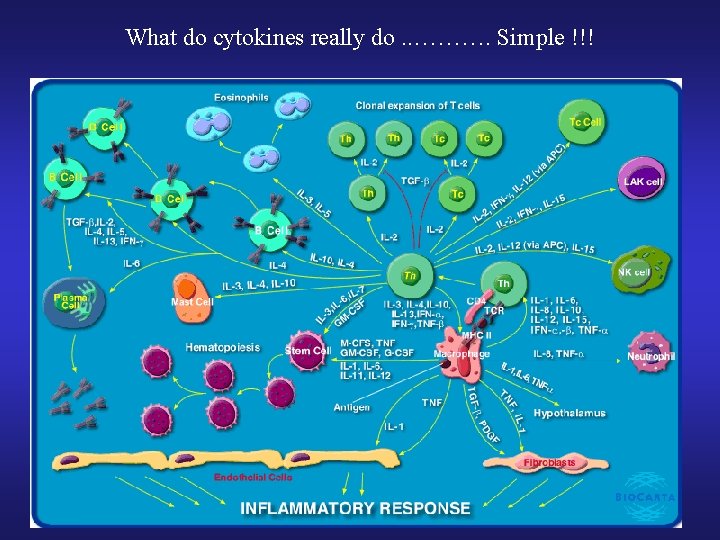
What do cytokines really do. . ………. Simple !!!

Cytokines • Most produced by Macrophages • Major cytokine for inflammation IL-1 and TNF • TNF alpha: • Procoagulant • Low concentration Myocardial excitement • High concentration Myocardial depression, MOF • Cachexia in cancer patients • IL-1: • Induces fever (PGE 2 mediated) • NSAIDs Reduce fever by reducing PGE 2 production • Atelectasis Fever by release of IL-1 from alveolar macrophages • IL-6: Hepatic acute phase protein production • IL-10: Downregulates immune response • IL-15: Activates NK cells in response to viral infection

Interferons • Released by Lymphocytes and NK cells in response to viral infection • Activates cell mediated immunity • Upregulates MHC expression • Inhibits viral replication

Questions 1 -5 TNF alpha is responsible for all the following except: A. Principally produced by macrophages B. Increases cell adhesion molecules (ICAM, selectins) C. Is a procoagulant D. Causes cachexia in cancer patients E. Causes myocardial excitement in high concentrations F. Activated PMNs and other macrophages Growth factor production cell recruitment

TNF alpha is responsible for all the following except: A. Principally produced by macrophages B. Increases cell adhesion molecules (ICAM, selectins) C. Is a procoagulant D. Causes cachexia in cancer patients E. Causes myocardial excitement in high concentrations F. Activated PMNs and other macrophages Growth factor production cell recruitment

Neutrophils are attracted to areas of inflammation and injury. Homing to areas of injury requires the neutrophils to adhere to endothelium in the affected area. This process is mediated by which of the following molecules? A. TNF B. L-selectin C. IL-2 D. NO

Neutrophils are attracted to areas of inflammation and injury. Homing to areas of injury requires the neutrophils to adhere to endothelium in the affected area. This process is mediated by which of the following molecules? A. TNF B. L-selectin C. IL-2 D. NO

Which of the following is NOT an oxidant generated in inflammation: A. Superoxide anion radical (O 2 -) B. C. Hydrogen Peroxide (H 2 O 2) Hydroxyl radical (-OH) D. Hypochlorous acid (HOCL-) E. Superoxide dismutase and Catalase

Which of the following is NOT an oxidant generated in inflammation: A. Superoxide anion radical (O 2 -) B. C. Hydrogen Peroxide (H 2 O 2) Hydroxyl radical (-OH) D. Hypochlorous acid (HOCL-) E. Superoxide dismutase and Catalase

Apoptosis is characterized by which of the following? A. loss of cell membrane integrity B. Inflammation C. DNA fragmentation D. cytokine production

Apoptosis is characterized by which of the following? A. loss of cell membrane integrity B. Inflammation C. DNA fragmentation D. cytokine production

Aspirin and non-steroidal anti-inflammatory drugs interfere with platelet function via their activity against which enzyme? A. Thromboxane synthase B. Nitric oxide synthase C. Phospholipase C D. Mitogen-activated protein kinase

Aspirin and non-steroidal anti-inflammatory drugs interfere with platelet function via their activity against which enzyme? A. Thromboxane synthase B. Nitric oxide synthase C. Phospholipase C D. Mitogen-activated protein kinase
- Slides: 93