HLA Ab Donor Reactivity and Risk of Rejection

HLA Ab, Donor Reactivity and Risk of Rejection and Graft Loss Ronald H. Kerman, Ph. D The University of Texas Medical School ~ Houston, TX Division of Immunology and Organ Transplantation

Allograft Rejection Time: Mediated by: Hyperacute 0 -48 hrs Abs Accelerated 5 -7 days Abs/cells Early/delayed Cells/Abs >60 days Abs/cells/? Type: Acute Chronic

Responsibilities of the Histocompatibility Laboratory To identify clinically relevant recipient Ig. G HLA antibodies

Positive crossmatches, due to Abs or other factors not impacting on graft outcome, should not influence the donorrecipient pairing for transplantation.

Detection of Recipient Sensitization Screen sera for reactivity vs target cells by cytotoxicity/fluorescence readouts. Use the most informative sera when performing the recipient vs donor crossmatch (historically most reactive, current and pretransplant sera).

Detection of Immunoglobulin Reactivity • NIH-CDC • AHG-CDC • Flow cytometry Membrane-dependent assays
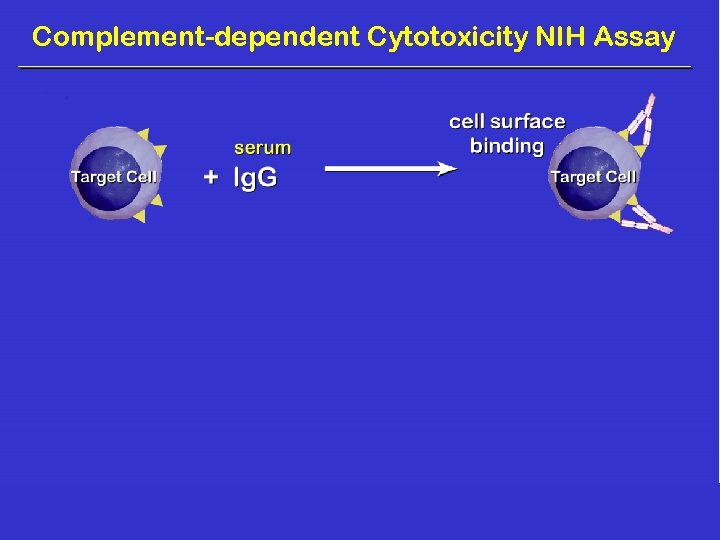
Complement-dependent Cytotoxicity NIH Assay
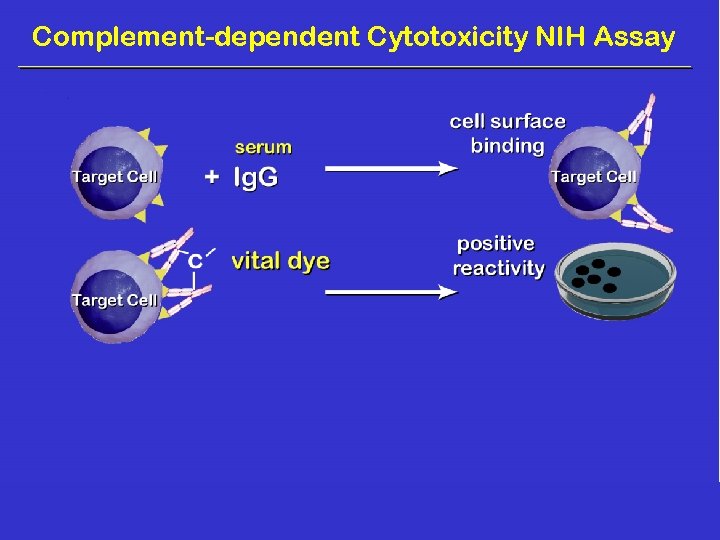
Complement-dependent Cytotoxicity NIH Assay
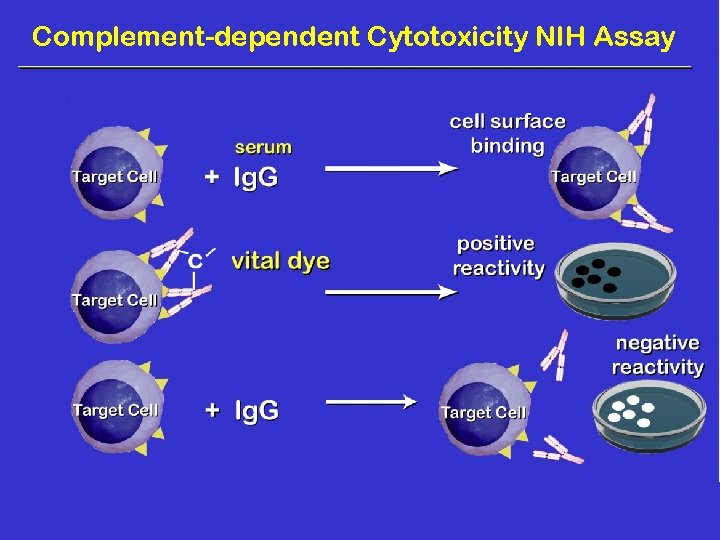
Complement-dependent Cytotoxicity NIH Assay
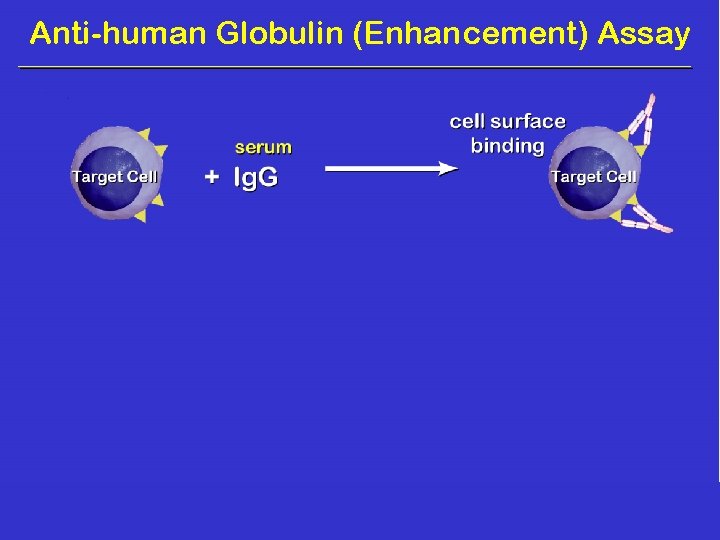
Anti-human Globulin (Enhancement) Assay
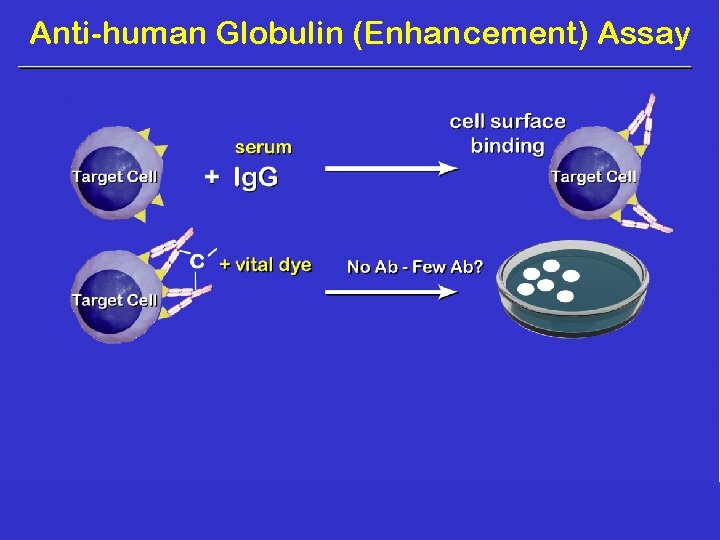
Anti-human Globulin (Enhancement) Assay
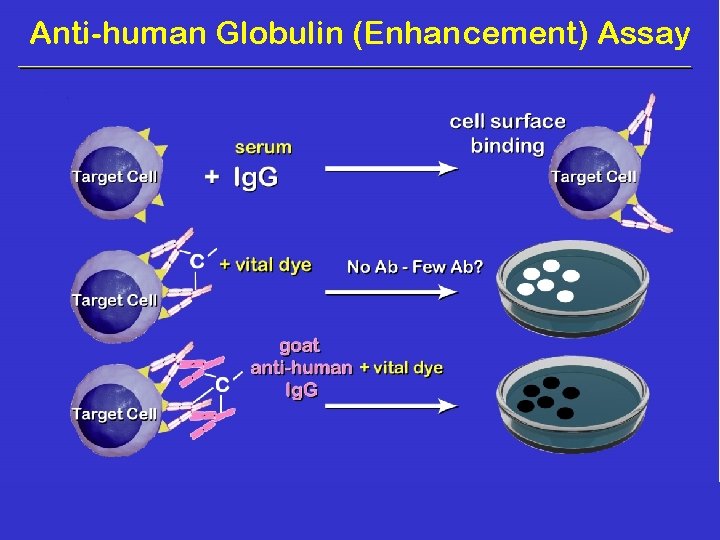
Anti-human Globulin (Enhancement) Assay
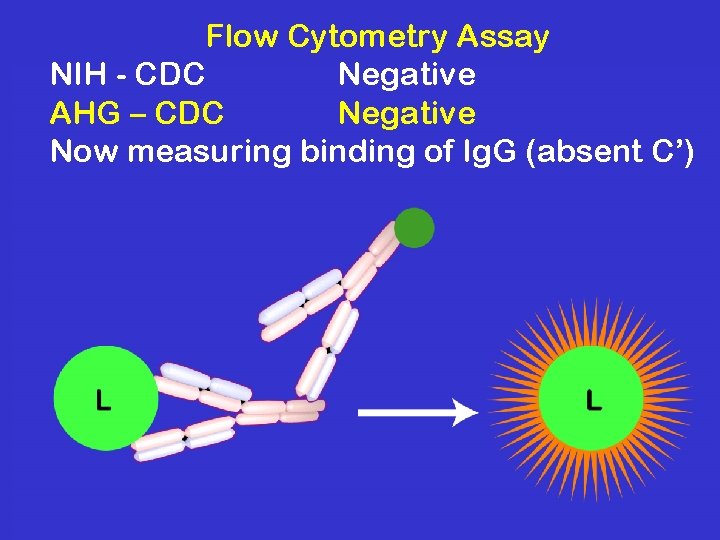
Flow Cytometry Assay NIH - CDC Negative AHG – CDC Negative Now measuring binding of Ig. G (absent C’)

Cadaveric Renal Allograft Survival Among 1 o Cs. A-Pred Recipients at 12 months NIH Neg. AHG Neg. Pos. n=166 n=151 n=15 81% 82% 67% (134/166) (124/151) (10/15) P<0. 01 Kerman et al, Transplantation; 51: 316, 1991
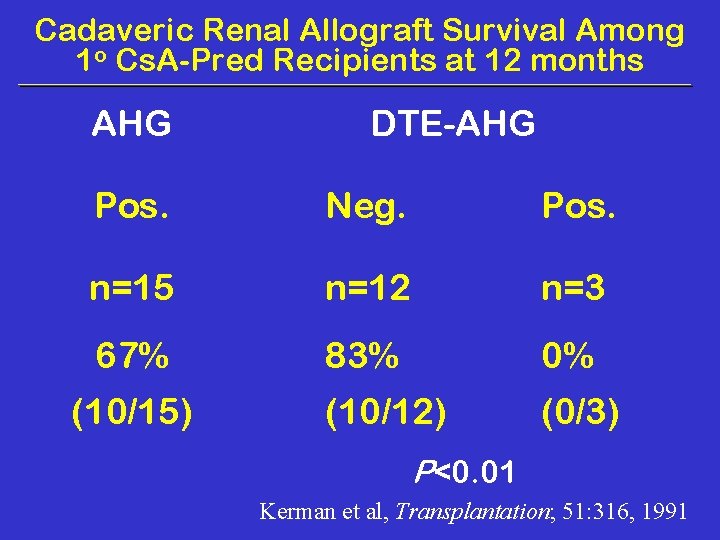
Cadaveric Renal Allograft Survival Among 1 o Cs. A-Pred Recipients at 12 months AHG DTE-AHG Pos. Neg. Pos. n=15 n=12 n=3 67% 83% 0% (10/12) (0/3) (10/15) P<0. 01 Kerman et al, Transplantation; 51: 316, 1991

Cadaveric Renal Allograft Survival Among 1 o Cs. A-Pred Recipients at 12 months FCXM DTE/AHG XM Neg. n=166 81% Neg. Pos. n=130 n=36 81% Kerman et al, Transplantation; 51: 316, 1991

Neg-NIH Extended XM: FCXM Study T-FCXM Pos. Neg. n=148 n=693 75% 82% P<0. 01 Ogura et al, Transplantation; 56: 294, 1993

Could Ron Kerman have been wrong about his crossmatch results and interpretation?
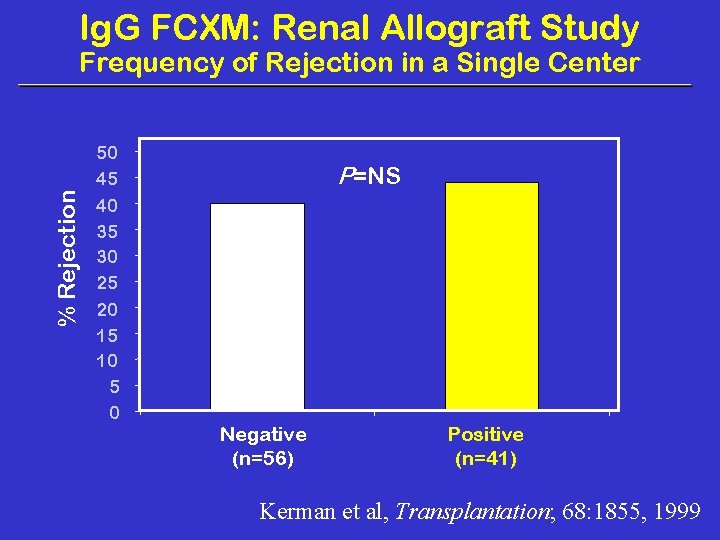
Ig. G FCXM: Renal Allograft Study % Rejection Frequency of Rejection in a Single Center 50 45 40 35 30 25 20 15 10 5 0 P=NS Negative (n=56) Positive (n=41) Kerman et al, Transplantation; 68: 1855, 1999

Could Ron Kerman have been wrong about his crossmatch results and interpretation? I don’t think so!
The Cell Surface Is a Jungle HLA

Membrane-dependent Assays • NIH-CDC • AHG-CDC • Flow cytometry Detection of membrane receptors may not be related to HLA!

Membrane-independent Assays ELISA-determined Ig. G HLA Abs vs MHC-I (pooled platelets) ELISA-determined Ig. G HLA Abs vs MHC-I/II (PBL cultures) Flow bead PRA-determined Ig. G HLA vs I/II (soluble HLA I/II antigens on microbeads measured by cytometry)
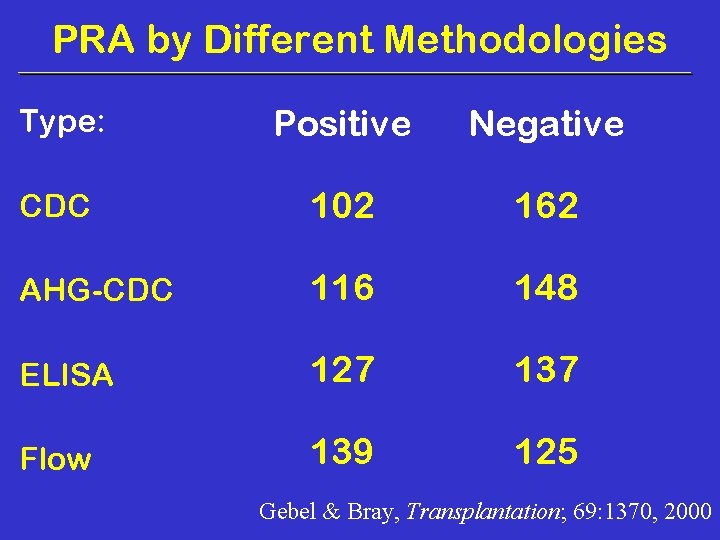

PRA by Different Methodologies Type: Positive Negative CDC 102 162 AHG-CDC 116 148 ELISA 127 137 Flow 139 125 Gebel & Bray, Transplantation; 69: 1370, 2000
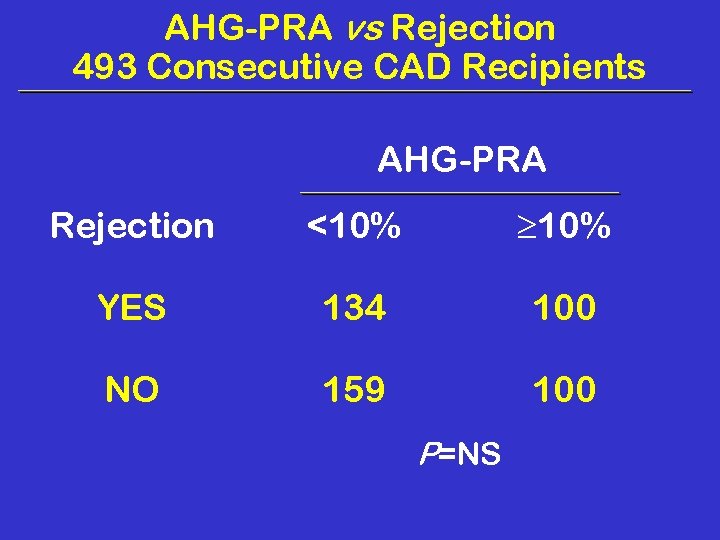

AHG-PRA vs Rejection 493 Consecutive CAD Recipients AHG-PRA Rejection <10% YES 134 100 NO 159 100 P=NS
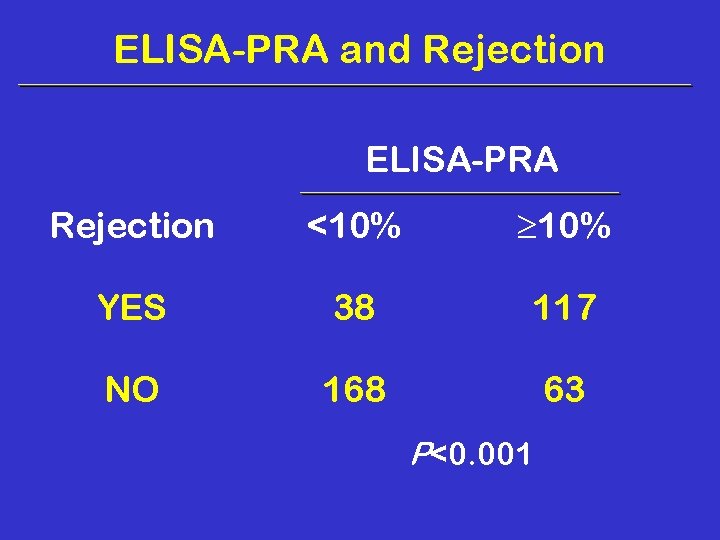
ELISA-PRA and Rejection ELISA-PRA Rejection <10% YES 38 117 NO 168 63 P<0. 001
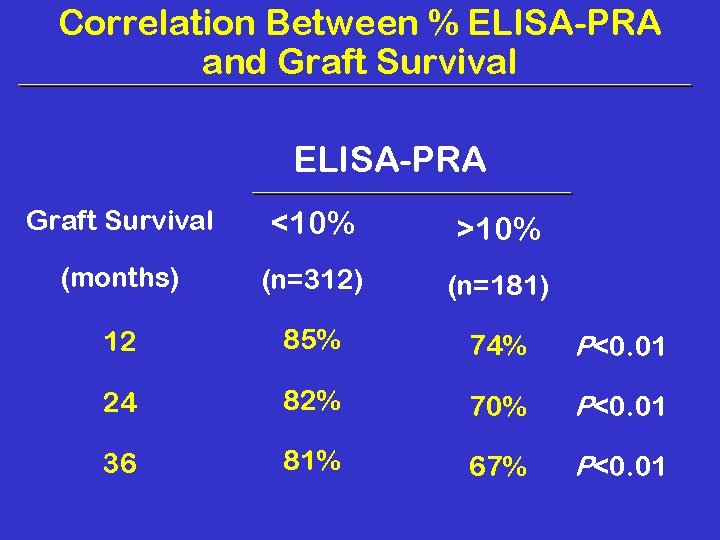
Correlation Between % ELISA-PRA and Graft Survival ELISA-PRA Graft Survival <10% >10% (months) (n=312) (n=181) 12 85% 74% P<0. 01 24 82% 70% P<0. 01 36 81% 67% P<0. 01

Sensitivity and sensitization, defining the unsensitized patient Gebel & Bray, Transplantation; 69: 1370, 2000 Application of membrane-independent assays to identify HLA antibodies
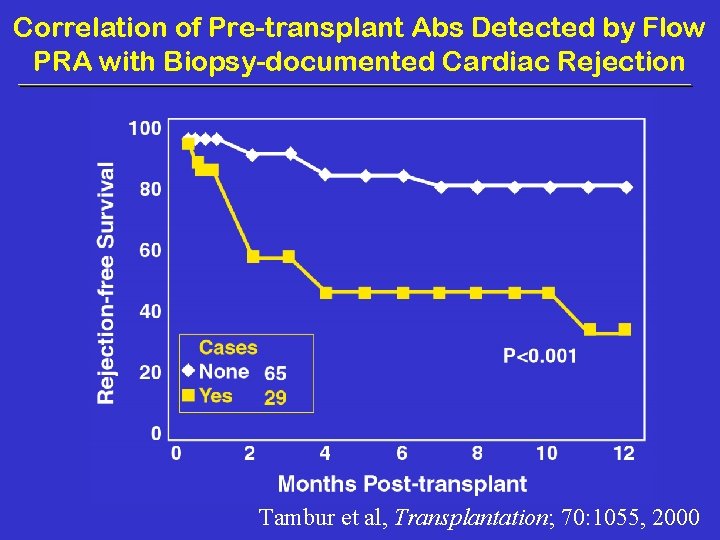
Correlation of Pre-transplant Abs Detected by Flow PRA with Biopsy-documented Cardiac Rejection Tambur et al, Transplantation; 70: 1055, 2000
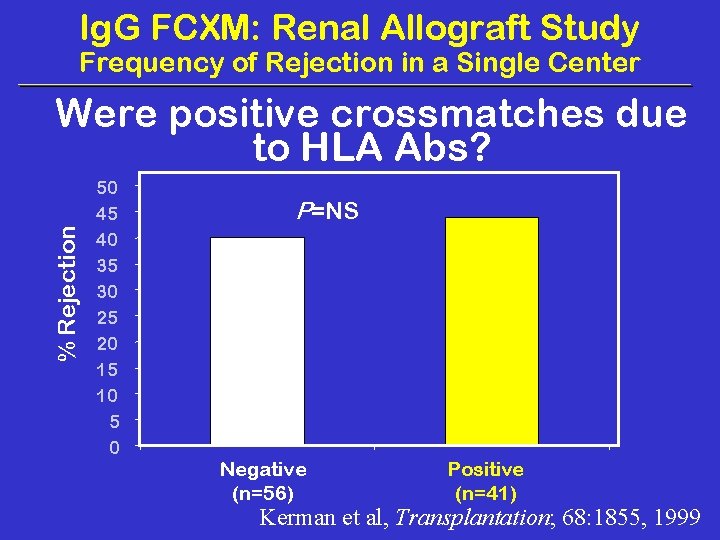
Ig. G FCXM: Renal Allograft Study Frequency of Rejection in a Single Center % Rejection Were positive crossmatches due to HLA Abs? 50 45 40 35 30 25 20 15 10 5 0 P=NS Negative (n=56) Positive (n=41) Kerman et al, Transplantation; 68: 1855, 1999

Immunosuppressive Menu: • Neoral - Cs. A • Steroids • Prograf - FK 506 • Cellcept - MMF • Rapamycin - Sirolimus • Thymoglobulin • OKT 3, anti-IL-2 R, FTY 720

If new immunosuppressive therapies reduce the incidence of acute rejection, are pre-Tx HLA antibodies clinically relevant?

RAPA-Cs. A-Pred treated primary recipients of CAD renal allografts experience fewer acute rejections vs Cs. A -Pred recipients. We therefore tested their pre-Tx sera for the presence of HLA Abs and correlated the results to the occurrence of rejection during the first 12 months post-transplant.

147 RAPA-Cs. A-Pred recipients were studied 48 patients were chosen specifically because they had a rejection episode. 99 patients were chosen because they had not experienced a rejection episode during the first year post-transplant.

PRA Testing Anti-human globulin (AHG) ELISA (One Lambda, Inc. LAT) Flow PRA (One Lambda, Inc. )

Results: AHG-PRA detected 18 reactive sera ELISA-PRA detected 25 reactive sera (11 vs HLA class I, 3 vs II, 11 vs I/II) Flow PRA detected 59 reactive sera (31 vs HLA class I, 9 vs II, 19 vs I/II)
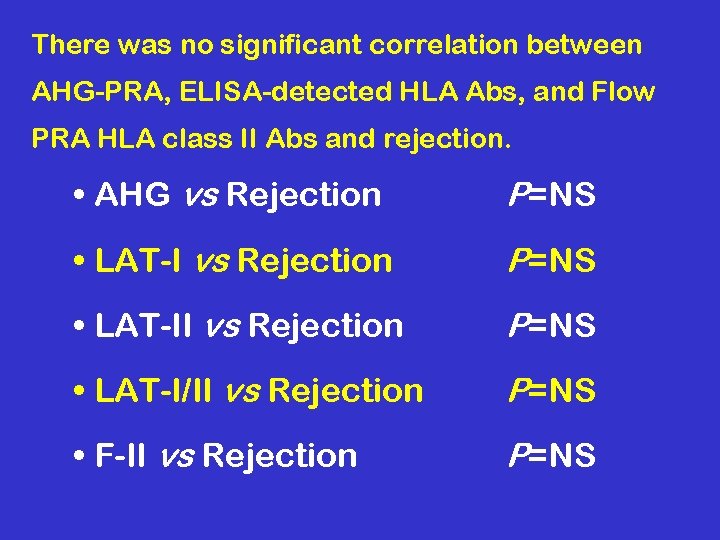

There was no significant correlation between AHG-PRA, ELISA-detected HLA Abs, and Flow PRA HLA class II Abs and rejection. • AHG vs Rejection P=NS • LAT-II vs Rejection P=NS • LAT-I/II vs Rejection P=NS • F-II vs Rejection P=NS
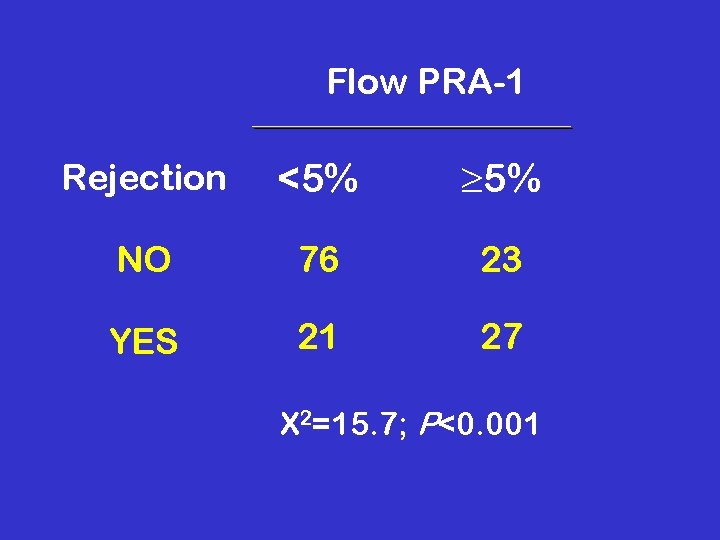
Flow PRA-1 Rejection <5% 5% NO 76 23 YES 21 27 X 2=15. 7; P<0. 001

FCXM Flow PRA Day of 1 st Rejection Pos. Neg. 0% 57 ± 34 2 8 No grafts lost (+) FCXM vs non-HLA Ab

Flow PRA Day of 1 st Rejection 13 ± 9% 55 ± 31 No grafts lost. FCXM Pos. - Neg. 30
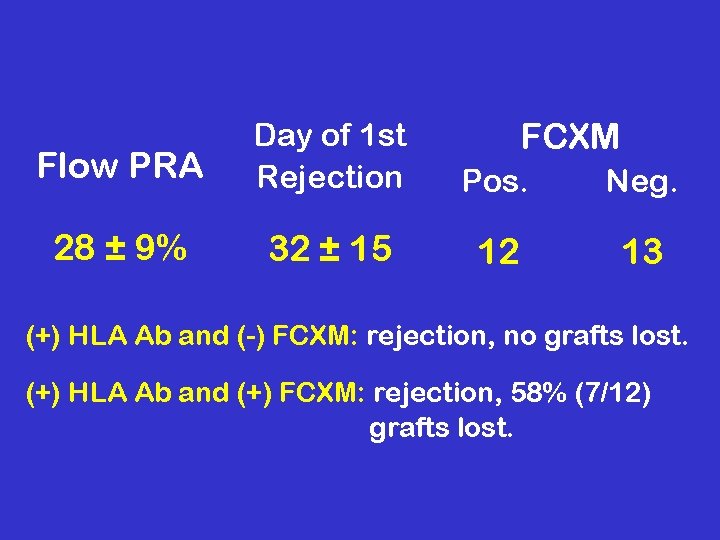

FCXM Flow PRA Day of 1 st Rejection Pos. Neg. 28 ± 9% 32 ± 15 12 13 (+) HLA Ab and (-) FCXM: rejection, no grafts lost. (+) HLA Ab and (+) FCXM: rejection, 58% (7/12) grafts lost.

FCXM Flow PRA Day of 1 st Rejection Pos. Neg. 48 ± 31% 17 ± 12 8 7 (+) HLA Ab and (-) FCXM: rejection, no grafts lost. (+) HLA Ab and (+) FCXM: rejection, 63% (5/8) lost to AMR.
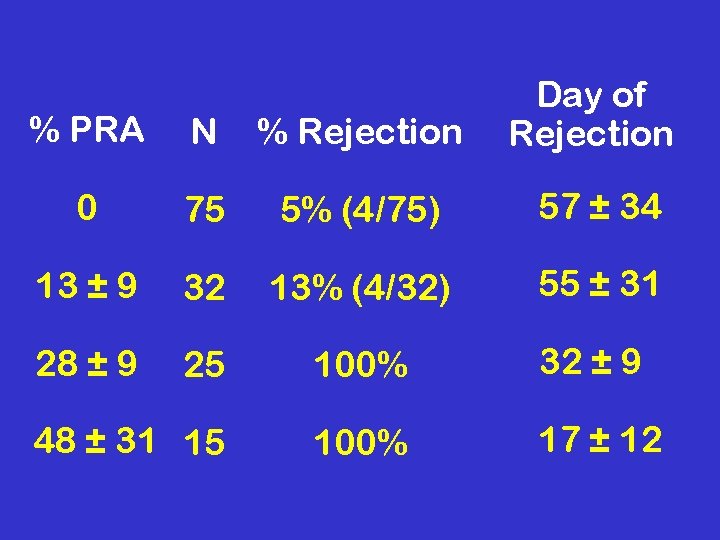
% PRA N % Rejection Day of Rejection 0 75 5% (4/75) 57 ± 34 13 ± 9 32 13% (4/32) 55 ± 31 28 ± 9 25 100% 32 ± 9 48 ± 31 15 100% 17 ± 12

1. Assays that measure binding of immunoglobulin to targets may not represent HLA Ab reactivity. 2. The AHG-XM protects RAPA-Cs. A-Pred recipients from hyperacute rejection. 3. The Flow PRA assay detects clinically relevant HLA Abs associated with rejection and/or graft loss.

4. How many antibodies are present may be clinically relevant. 5. The antibody titer may also be important. 6. Patients with pre-Tx (+) HLA Abs and (+) donor reactivity (+ FCXM) are at risk for graft rejection and loss.

We have performed heart transplantation following a negative AHG-XM. We evaluated the clinical relevance of FCXM for heart recipients.
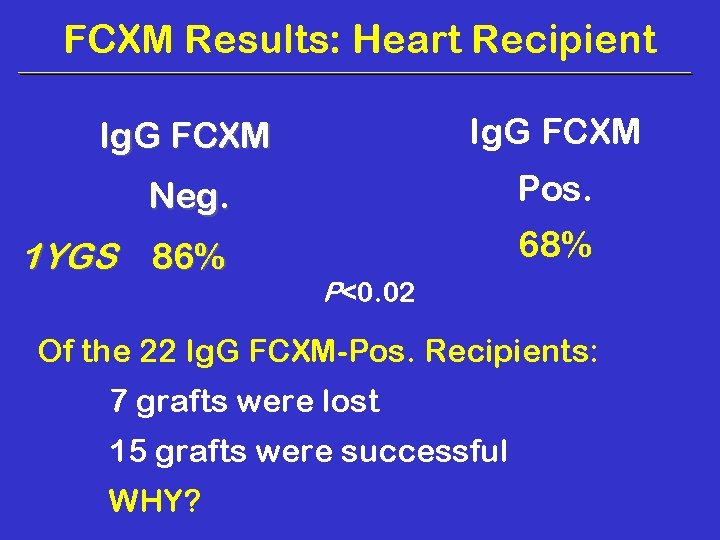
FCXM Results: Heart Recipient Ig. G FCXM Neg. Pos. 1 YGS 86% 68% P<0. 02 Of the 22 Ig. G FCXM-Pos. Recipients: 7 grafts were lost 15 grafts were successful WHY?

We Flow PRA Tested the Ig. G FCXM-Pos. Sera 5 sera tested from lost grafts All 5 sera were Flow PRA reactive vs MHC I (Flow PRAs of 36%, 52%, 68%, 50% and 49%) 11 sera tested from successful recipients All 11 sera were Flow PRA non-reactive
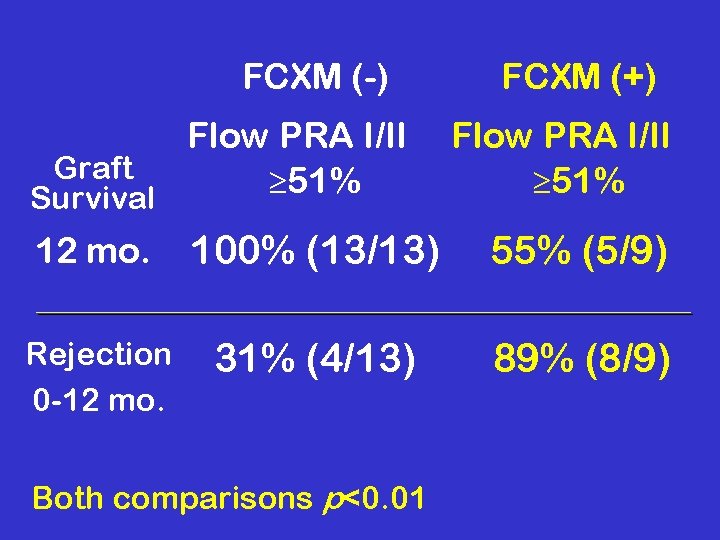
FCXM (-) FCXM (+) Flow PRA I/II Graft 51% Survival 12 mo. 100% (13/13) 55% (5/9) Rejection 0 -12 mo. 31% (4/13) Both comparisons p<0. 01 89% (8/9)

HLA Ab and Donor Specific Reactivity Rank Order of Risk 1. HLA Ab negative, FCXM negative (at risk for reversible, cellular rejection) 2. HLA Ab negative, FCXM positive (non-HLA allo-Ab - at risk for reversible, cellular rejection)

HLA Ab and Donor Specific Reactivity Rank Order of Risk 3. HLA Ab positive, FCXM negative (at risk for reversible, cellular, +/- HLA Ab, rejection) 4. HLA Ab positive, FCXM positive (at risk for humoral/cellular rejection and graft loss)

To transplant or not to transplant, that is the question! Whether it is nobler in the minds of transplant surgeons to treat with thymoglobulin, OKT 3, Plasmapheresis, IVIg, or the kitchen sink!

Applications 1. Pre-transplant identification of immunologically high risk patients. Consideration of induction and/or maintenance immunosuppression. 2. Clarify the role of HLA antibody in rejection episodes (including the role of C 4 d ).

Applications 3. Transplantation of highly sensitized and/or positive crossmatch recipients. 4. Long term monitoring of the presence of HLA antibody and graft outcome.

“I have never let my schooling interfere with my education. ” -Mark Twain
- Slides: 55