HIV II Update on Opportunistic Infections Prevention and
























































- Slides: 76

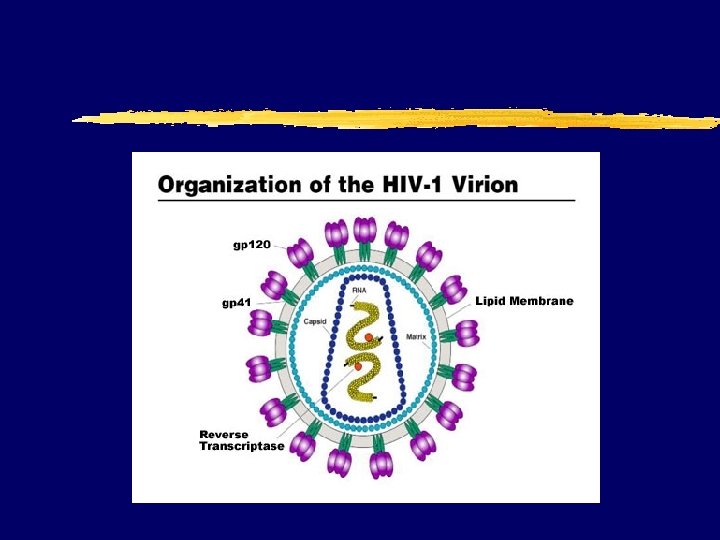
HIV II Update on Opportunistic Infections Prevention and Treatment


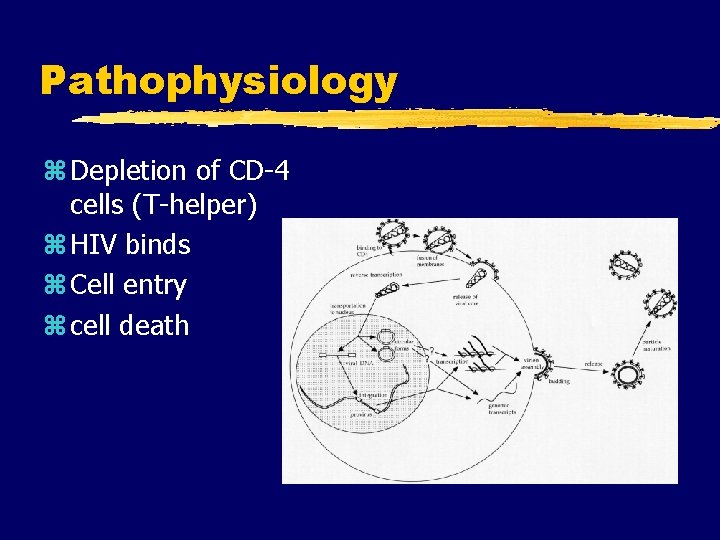
Pathophysiology z Depletion of CD-4 cells (T-helper) z HIV binds z Cell entry z cell death

CD 4 -deficiency z Direct mechanisms y Accumulation of unintegrated viral DNA y Interference with cellular RNA processing y Intracellular gp 120 -CD 4 autofusion events y Loss of plasma membrane integrity because of viral budding y Elimination of HIV-infected cells by virus-specific immune responses z Indirect mechanisms y Aberrant intracellular signaling events y Syncytium formation y Autoimmunity y Superantigenic stimulation y Innocent bystander killing of viral antigen-coated cells y Apoptosis y Inhibition of lymphopoiesis

CD 4 depletion syndromes z. HIV/AIDS zidiopathic CD 4+ T lymphocytopenia z. Iatrogenic y. Corticosteroids y. Immunosuppresants

Opportunistic infections z For patients taking potent combination antiretroviral therapy (ART), beginning in 1996, there has been a dramatic decline in the incidence of AIDS-related opportunistic infections (OIs) such as Pneumocystis carinii pneumonia (PCP), disseminated Mycobacterium avium complex (MAC), and invasive cytomegalovirus (CMV) disease

Treatment Guidelines z 2001 USPHS/IDSA Guidelines for the Prevention of Opportunistic Infections in Persons Infected with HIV z. Treatment of Tuberculosis - June 20, 2003

Rating Strength of the Recommendation A Both strong evidence for efficacy and substantial clinical benefit support recommendation for use. Should always be offered. D Moderate evidence for lack of efficacy or for adverse outcome supports a recommendation against use. Should generally not be offered. B Moderate evidence for efficacy -- or strong evidence for efficacy but only limited clinical benefit -- supports recommendation for use. Should generally be offered. E Good evidence for lack of efficacy or for adverse outcome supports a recommendation against use. Should never be offered. C Evidence for efficacy is insufficient to support a recommendation for or against use. Or evidence for efficacy might not outweigh adverse consequences (e. g. , drug toxicity, drug interactions) or cost of the chemoprophylaxis or alternative approaches. Optional. Gross PA, Barrett TL, Dellinger EP, et al. Purpose of quality standards for infectious diseases. Clin Infect Dis 1994; 18(3): 421.

Quality of evidence supporting the recommendation I Evidence from at least one properly randomized, controlled trial. II Evidence from at least one well-designed clinical trial without randomization, from cohort or case-controlled analytic studies (preferably from more than one center), or from multiple timeseries studies. Or dramatic results from uncontrolled experiments. III Evidence from opinions of respected authorities based on clinical experience, descriptive studies, or reports of expert committees.

HIV and fever z. Disseminated MAC ybefore HAART, most common cause of FUO in advanced AIDS. z. Disseminated histo zbartonellosis z. CMV zcryptococcosis

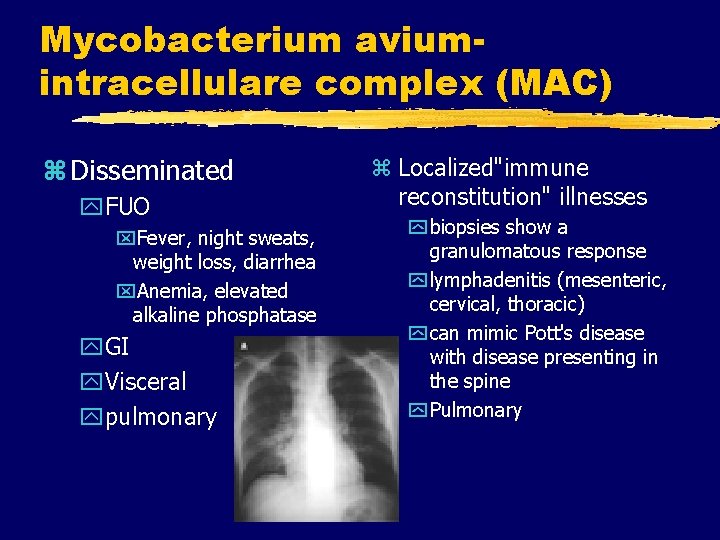
Mycobacterium aviumintracellulare complex (MAC) z Disseminated y. FUO x. Fever, night sweats, weight loss, diarrhea x. Anemia, elevated alkaline phosphatase y. GI y. Visceral ypulmonary z Localized"immune reconstitution" illnesses y biopsies show a granulomatous response y lymphadenitis (mesenteric, cervical, thoracic) y can mimic Pott's disease with disease presenting in the spine y Pulmonary

MAC z Findings y. Adenopathy y. Elevated alk phos yanemia z Diagnosis y. Blood culture y. Tissue culture y. Histopathology z Treatment y. Macrolide + ethambutol + rifabutin y. Amikacin yciprofloxacin

MAC z. Sources y. Food y. Water ysoil z. Screening not rec b/c no data for benefit, although predicts disease z. No recs for avoidance

MAC prophylaxis z Primary CD 4 < 50 until >100 3 mo. (AI) y. Clarithromycin y. Azithromycin y. Rifabutin (not combo-EI) x. Exclude TB x. DI’s z Secondary for 12 mo and until CD 4 no sx and CD 4 >100 6 mo (BCx neg) y. Macrolide + ethambutol, +/- rifabutin y. High dose clarithromycin asso. W/higher mortality (EI) y. Clofazimine too many ADR’s (DII) z Restart at CD 4 <50 -100

Drug Interactions z Azithromycin not affected by c P 450 z Protease inhibitors y. Increase clarithromycin levels y. Some contraindicated w/rifabutin z NNRTIs (efavirenz) y. Induce clarithromycin metabolism y. Some contraindicated w/rifabutin

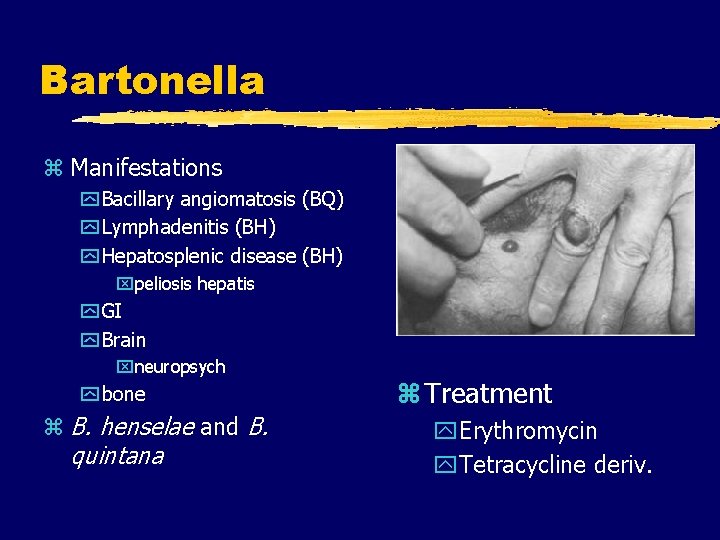
Bartonella z Manifestations y Bacillary angiomatosis (BQ) y Lymphadenitis (BH) y Hepatosplenic disease (BH) xpeliosis hepatis y GI y Brain xneuropsych y bone z B. henselae and B. quintana z Treatment y. Erythromycin y. Tetracycline deriv.

Bartonellosis z. HIV-higher incidence z. Older cats less likely to transmit z. Control fleas z. No rec for primary prophylaxis z. Consider long-term suppression (C-III)

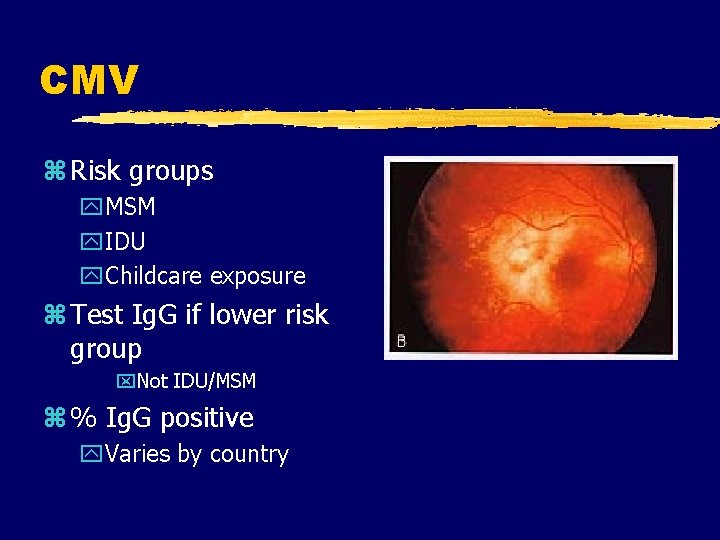
CMV z Risk groups y. MSM y. IDU y. Childcare exposure z Test Ig. G if lower risk group x. Not IDU/MSM z % Ig. G positive y. Varies by country

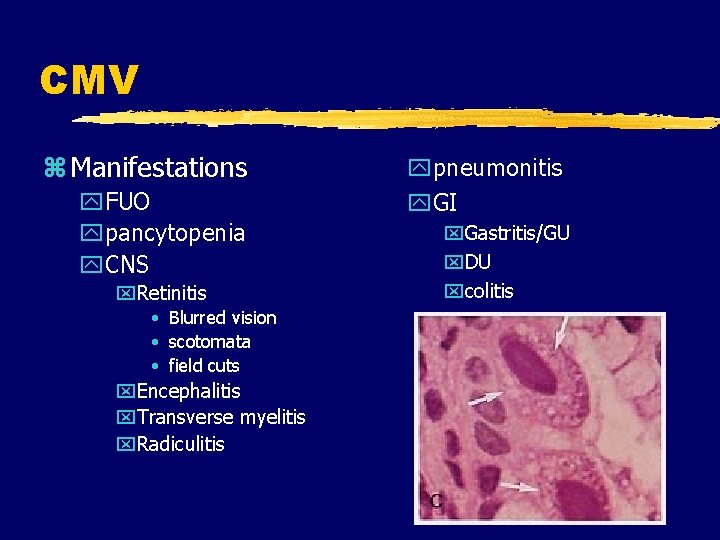
CMV z Manifestations y. FUO ypancytopenia y. CNS x. Retinitis • Blurred vision • scotomata • field cuts x. Encephalitis x. Transverse myelitis x. Radiculitis ypneumonitis y. GI x. Gastritis/GU x. DU xcolitis

CMV z Diagnosis y. Serology-not helpful y. Tissue histopathology y. Molecular diagnostics x. Antigen x. PCR z Treatment y. Valganciclovir y. Ganciclovir 5 mg/kg IV bid × 14 -21 days y. Foscarnet 60 mg/kg IV q 8 h or 90 mg/kg IV q 12 h × 14 -21 days y. Cidofovir 5 mg/kg IV weekly × 2 then every other week y. Implants

CMV prophylaxis z Primary y. Can consider if Ig. G (+) and CD 4 <50 y. Oral ganciclovir or valganciclovir y. Regular optho exams y. Discuss symptoms y. NOT acyclovir/valacyclovir z Secondary y. Intraocular alone not sufficient y. Valganciclovir y. Consider stopping when CD 4>100 -150 6 mo y. Continue regular f/u z CMV-neg or leukopoor irradiated blood if CMV (-)

HIV and diarrhea z Cryptosporidium z Microsporidiosis z Isospora z Giardia z bacterial enteric infections y. Salmonella y. Shigella ycampylobacter y. Listeria z CMV z Cdiff

HIV and diarrhea • Crampy abdominal pain, bloating, and nausea suggest small bowel • Cryptosporidia • Microsporidia • Isospora • Giardia • cyclospora) • MAC. • High-volume, watery diarrhea with weight loss and electrolyte disturbance is most characteristic of cryptosporidiosis • bloody stools with abdominal cramping and fever ( invasive bacterial pathogen) • Clostridium difficile • CMV colitis

HIV and diarrhea z Stool studies y O&P y Trichrome y AFB y Immunohisto y Cdiff z Thorough history z Medication review z Low threshold for flex sig z Given the availability of effective treatment; more aggressive evaluation that often includes endoscopy has replaced the less invasive approach. z Treatment y Antimotility agents x. Imodium, Lomotil x. Opium y Calcium y octreotide

Bacterial Enteric Infections Prevention z Seek vet care for animals with diarrhea z WASH HANDS z Travel precautions y Bottled beverages y Avoid fresh produce y Avoid ice y Consider prophylaxis or early empiric therapy x. Cipro 500 qd x. Bactrim z Avoid y Reptiles, chicks and ducklings y Raw eggs y Raw poultry, meat and seafood y Unpasteurized dairy products/juices y Raw seed sprouts y Soft cheeses y Deli counters unless can reheat y Refrigerated meat spreads

Cryptosporidium z coccidian protozoan (I. belli, C. cayetanensis, and Toxoplasma gondii) z 5%-10% of diarrhea in immunocompetent z Asymptomatic carriers z mammalian hosts-cattle, horses, rabbits, guinea pigs, mice. z transmission fecal-oral. z Waterborne outbreaks due to contamination of drinking water z thick-walled, highly resistant oocyst z excysts in stomach z sporozoites infect enterocytes and persist at the apical pole of intestinal epithelial cellsmicroscopic appearance of extracellular, adherent parasite

Cryptosporidiosis prevention z biopsy z fecal examination y Modifed AFB y Immunohisto stains z Treatment y Azithromycin y Paromomycin y Octreotide y nitazoxanide y HAART z Clarithromycin/rifabutin work, but no data. z Counsel regarding exposure-avoid feces y diapers y young animals (screen BIII) y water xboil water when suggested (AI) xfilters (CIII) xoysters xbottled (CIII)

Microsporidiosis z observed initially in intestinal biopsy specimens in 1982 z No disease in normal hosts z 2 types y Enterocytozoon bieneusi, reproduces within enterocytes y Encephalitozoon (Septata) intestinalis infects epithelial cells and stromal cells of the lamina propria and causes systemic infection z Diagnosis y Difficult to see by light microscopy-order trichrome stain z Treatment y Albendazole (for intestinalis) y Atovaquone y metronidazole. z No recs for prevention

Isospora zno other known host zendemic in Brazil, Colombia, Chile, and parts of equatorial Africa and southwest Asia. zseen rarely in normals zfecal-oral route

Isospora z Immunocompetent y watery diarrhea y usually clear the infection within about 2 weeks; y may persist z histologic sections y. Villus atrophy, eosinophil infiltrates, and disorganization of the epithelium z HIV-chronic high-volume watery diarrhea z shown better with z Detection in stool samples Giemsa on histo difficult, and concentration or flotation z Cipro better than methods. AFB + Bactrim

Cyclospora zfirst reported in the 1980 s zendemic in tropical countries and other areas w/poor standards of hygiene and water purification zseverity related to the degree of immunosuppression z. Rx Bactrim

Cyclospora z. Epidemics attributed to contamination of water supplies, fruits, and vegetables zsimilar to Cryptosporidium but larger (8 to 10 mum versus 4 to 5 mum) and AFB + zfecal-oral route zintermittent watery diarrhea for 3 > mo. zinfect enterocytes and proliferate within a supranuclear parasitophorous vacuole.


HIV and pneumonia z. PCP zhistoplasmosis zcryptococcosis zrhodococcus z. CMV z. Pneumococcus y 100 -fold risk z. Nontypable H. flu z. Pseudomonas y 40 -fold risk y. Lowest CD 4 z. HHV-8 z. Coccidiodomycosis


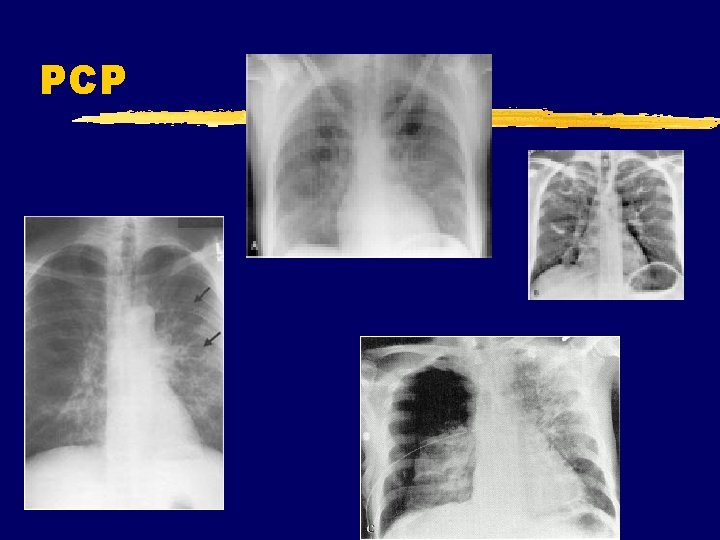
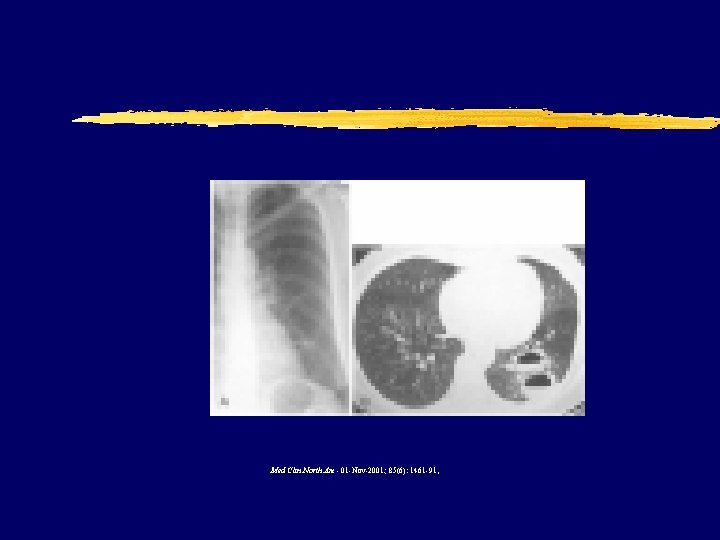
PCP

PCP z Symptoms y Incidious onset y SOB>cough y pneumothorax z Findings y diffuse infiltrates in a perihilar or bibasilar distribution and a reticular or reticulonodular pattern y No effusion y Elevated LDH y SX>>>CXR x. Normal in 26% z Diagnosis y. Sputum for DFA y. Sputum cytology y. BAL for same y. Histopathology/stains

PCP z TMP 15 mg/kg/d + SMX 75 mg/kg/d po or IV × 21 days in 3 -4 divided doses; for outpatient, 2 DS tablets po tid rash, fever, gastrointestinal symptoms, hepatitis, hyperkalemia, leukopenia, and hemolytic anemia y. Steroid (p. O 2 < 70 or A-a gradient > 35) y. TMP-dapsone y. Clinda/primaquine y. Atovaquone y. Trimetrexate/folinic acid y. Iv Pentam xnausea, infusion-related hypotension, hypoglycemia, hypocalcemia, renal failure, and pancreatitis

PCP prophylaxis z CD 4<200 or history of z Bactrim (AI) oral thrush (AII) y. DS daily (toxo, bacterial pathogens) z CD 4%<14 or other OI y. SS daily (BII) y. DS TIW (BII) yrechallenge if rash (desens) - 70% tolerate

PCP prophylaxis z Dapsone + pyrimethamine/leucov orin z aerosolized pentam (Respirgard II)pregnancy 1 st term z atovaquone All BI z Other aerosolized Pentam z parenteral pentam z oral pyrimethamine/ sulfadoxine z oral clinda/primaquine z trimetrexate All CIII

PCP prophylaxis z Stop when CD 4>200 for 3 mo. z Restart if CD 4<200 z Stop secondary prophylaxis if CD 4>200 unless PCP occurred at higher CD 4 z Children of HIV mothers need prophylaxis z Children with PCP can not stop secondary prophylaxis.

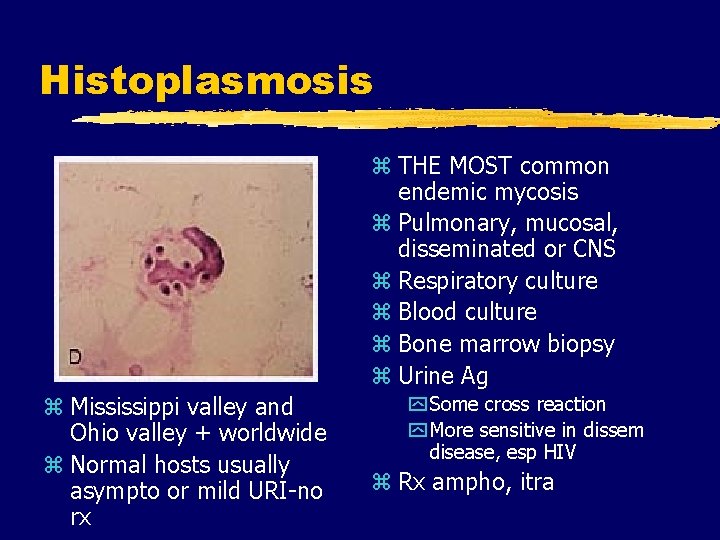
Histoplasmosis z THE MOST common endemic mycosis z Pulmonary, mucosal, disseminated or CNS z Respiratory culture z Blood culture z Bone marrow biopsy z Urine Ag z Mississippi valley and Ohio valley + worldwide z Normal hosts usually asympto or mild URI-no rx y Some cross reaction y More sensitive in dissem disease, esp HIV z Rx ampho, itra

Clin Chest Med - 01 -DEC-1996; 17(4): 725 -44

Histoplasmosis Prevention z Routine skin testing not predictive z Avoid y. Creating soil/old building dust y. Cleaning chicken coops y. Disturbing bird roosts y. Exploring caves z Secondary prophylaxis y. Itraconazole y. No data-no rec for stopping z Primary Prophylaxis y. No proven survival benefit y. Consider in high risk and CD 4<100

Typical CAP z Increased mortality z Maintain normal with Pneumococcal granulocyte count & z Increased incidence of Ig. G Pseudomonas z Prevention y. Pneumovax z Bactrim and macrolide x. BII rec if CD 4>200 prophylaxis prevent x. No data for CD 4<200 resp infections, but x. Repeat in 5 years not rec solely for this x. Repeat when CD 4 reason >200

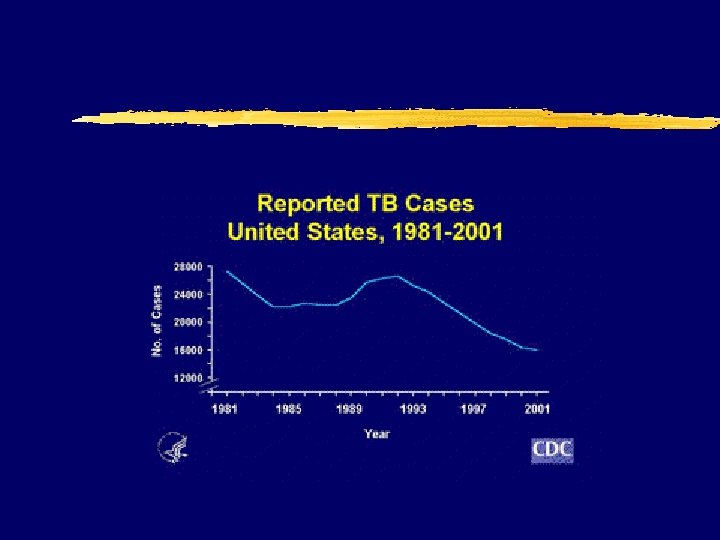
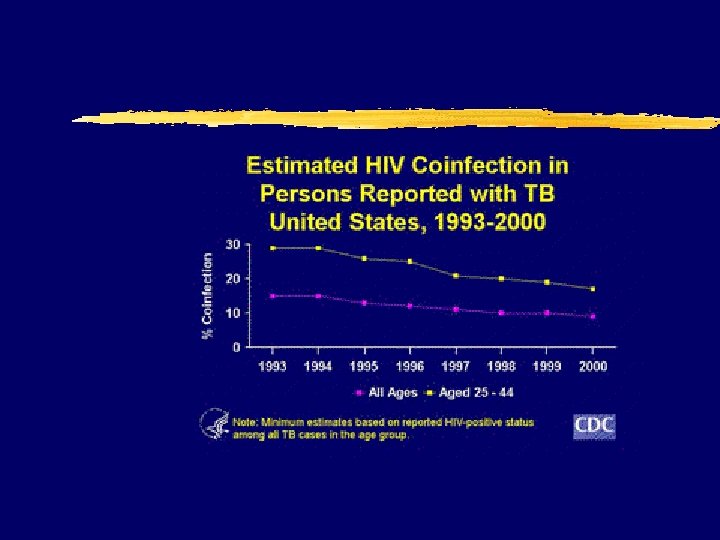
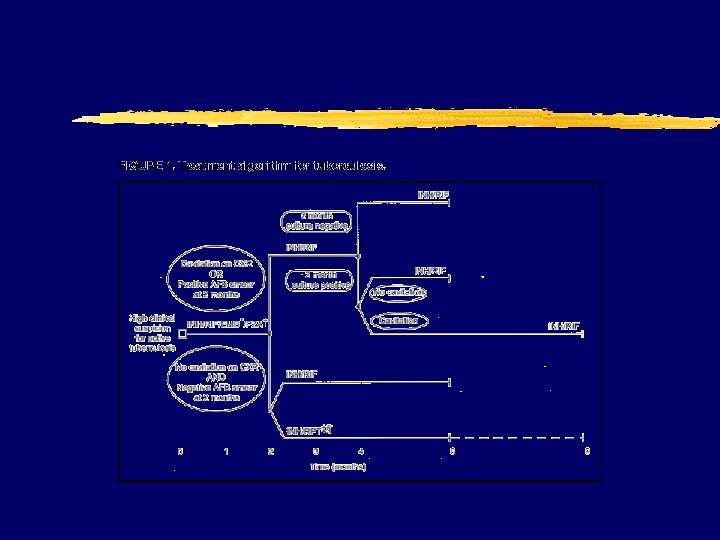
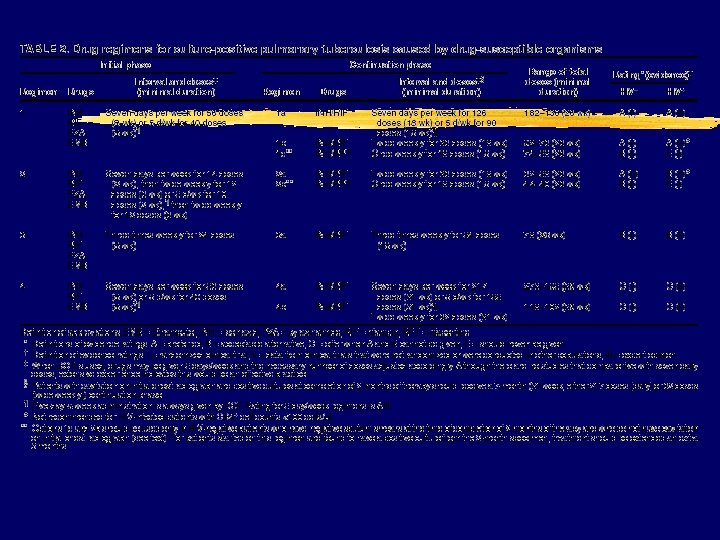
Tuberculosis z Low threshold of z 4 -drug therapy suspicion initially z Lower CD 4=atypical z Drug interactions presentation major issue z Higher mortality z Tuberculin skin testing (TST) negative in 40% of patients with disease



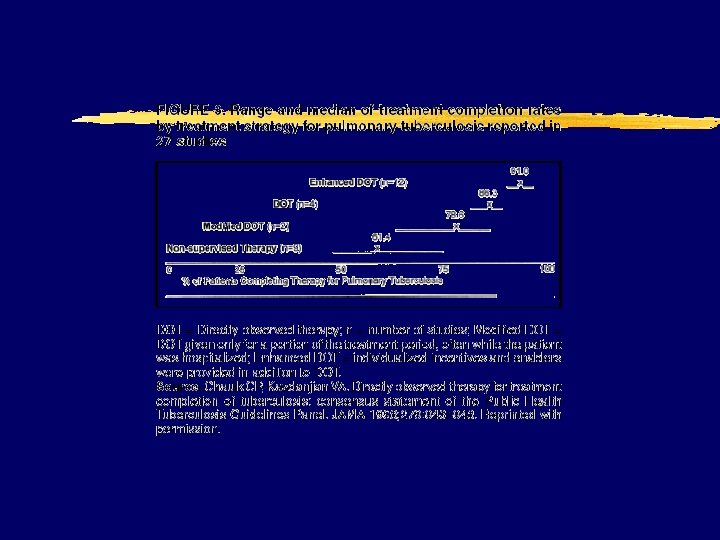
Tuberculosis z New guidelines y. Emphasize DOT and provider responsibility x. Louis Pasteur once said, "The microbe is nothing. . . the terrain everything" y. Reculture at 2 mo of trx x. Extend if still + and cavitary disease z INH--rifapentine once weekly continuation phase (Regimens 1 c and 2 b) is contraindicated z CD 4+ cell counts <100/µl should receive daily or three times weekly treatment z “paradoxical” flares occur y Associated w/HAART y Effusions, infiltrates, enlargement of CNS lesions, nodes, fever y Steroids used





Tuberculosis prevention z PPD on diagnosis of HIV (5 mm) z if positive treat z Close contacts should be treated if HIV+ z if exposed to MDR TB needs expert advice y. INH/B 6 9 months (AII) and PH yrifampin 4 months (BIII) z BCG contraindicated yrif/PZA for 2 months z Vague guidelines for xhepatic toxicity repeating PPD yrifabutin can be sub’d (less data) yyearly if “high risk” yrepeat when CD 4>200

Coccidiocomycosis z Growth is enhanced by bat and rodent droppings. z Exposure is heaviest in the late summer and fall z Acute pulm, chronic pulm, dissem, CNS z more severe in immunosuppressed individuals, African Americans, and Filipinos z 2/3 of immunosuppressed have disseminated disease z Avoid disturbing native soil z Diagnose by serology or biopsy z Blood cultures not usually positive z Skin test not predictive z Often refractory to treatement z Secondary prophylaxis lifelong, too little data for stopping (>100)

Med Clin North Am - 01 -Nov-2001; 85(6): 1461 -91,

HIV and rash z Molluscum z HHV-8 (KS) z HPV z VZV z HSV z cryptococcus z Bartonella z Syphilis z Candida z Seborrheic dermatitis z Folliculitis y. Eosinophilic ybacterial z Psoriasis z Onchomycosis z Prurigo nodularis z scabies

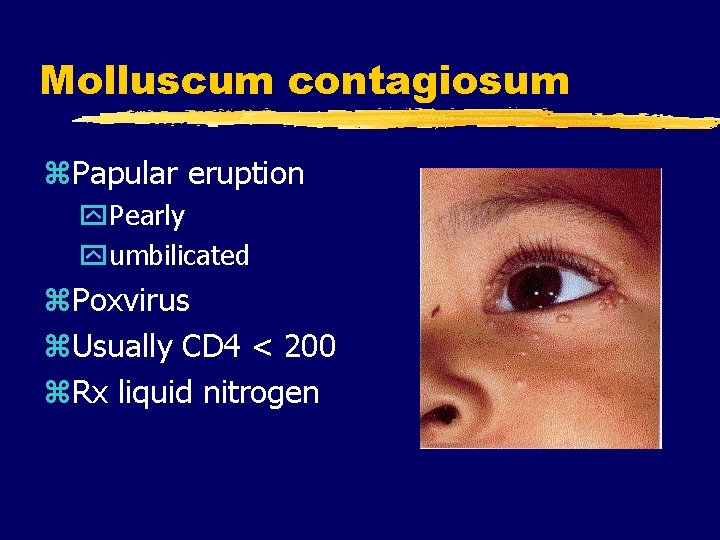
Molluscum contagiosum z. Papular eruption y. Pearly yumbilicated z. Poxvirus z. Usually CD 4 < 200 z. Rx liquid nitrogen

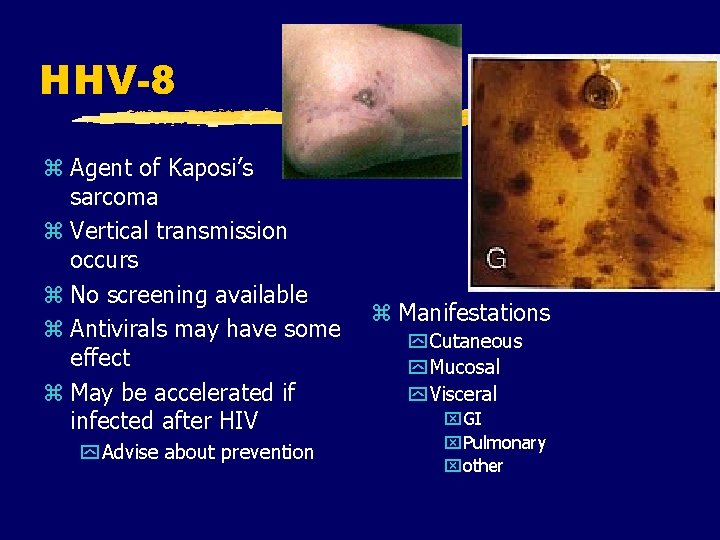
HHV-8 z Agent of Kaposi’s sarcoma z Vertical transmission occurs z No screening available z Manifestations z Antivirals may have some y Cutaneous effect y Mucosal z May be accelerated if y Visceral x. GI infected after HIV y Advise about prevention x. Pulmonary xother

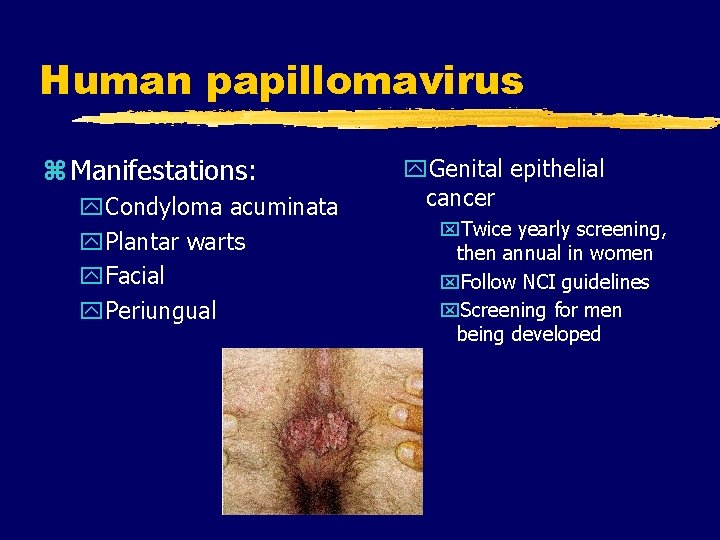
Human papillomavirus z Manifestations: y. Condyloma acuminata y. Plantar warts y. Facial y. Periungual y. Genital epithelial cancer x. Twice yearly screening, then annual in women x. Follow NCI guidelines x. Screening for men being developed

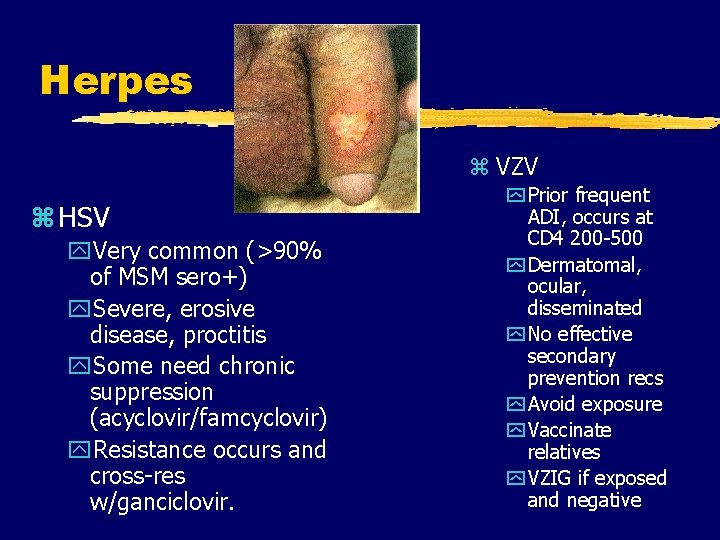
Herpes z VZV z HSV y. Very common (>90% of MSM sero+) y. Severe, erosive disease, proctitis y. Some need chronic suppression (acyclovir/famcyclovir) y. Resistance occurs and cross-res w/ganciclovir. y Prior frequent ADI, occurs at CD 4 200 -500 y Dermatomal, ocular, disseminated y No effective secondary prevention recs y Avoid exposure y Vaccinate relatives y VZIG if exposed and negative

Candida Infections z Manifestations y Oral thrush y Esophageal candidiasis y Candidal dermatitis y vulvovaginal z Treatment y fluconazole y Clotrimazole y Nystatin y Itraconazole y Amphotericin (po or iv) z Responds quickly to therapy z Primary prophylaxis not rec z Secondary is optional, prefer early empiric rx z Azole resistance is an issue

HIV and headache z. Cryptococcus-meningitis z. Toxoplasmosis-enhancing z. PML zlymphoma z. HIV z. CMV (perivent) z. EBV nonenhancing

Cryptococcus z Meningitis y Headache y subtle cognitive effects. y Occaasional meningeal signs and focal neurologic findings y nonspecific presentation is the norm z Pulmonary disease z Disseminated disease y FUO y Adenopathy y Skin nodules y Organ involvement z Diagnosis y. CSF Ag sens=100% y. Need opening pressure z Treatment y. Ampho + 5 FC (GI, hem toxicity) yfluconazole

Cryptococcal meningitis z. ICP management y>250 mm H 2 O was seen in 119 out of 221 patients xhigher titers of cryptococcal antigen xmore severe clinical manifestations • headache, meningismus, papilledema, hearing loss, and pathologic reflexes • shortened long-term survival y Desired OP < 200 mm H 2 O or 50% of the initial pressure y Daily lumbar punctures until the pressure is stable y Lumbar drain y Ventriculoperitoneal shunting y Corticosteroids are not recommended

Cryptococcus Prevention z. Primary prophylaxis effective but generally not rec z. Secondary until CD 4>100 -200 6 mo. and no sx (only CIII rec) y. Fluconazole (AI) y. Restart at <100 -200

Toxoplasmosis 1. Toxoplasmosis seronegative or toxoplasmosis prophylaxis or lesions atypical radiographically for toxoplasmosis (single, crosses midline, periventricular): CSF exam +/biopsy • + EBV PCR highly correlates with lymphoma • + JCV PCR c/w PML • + toxo PCR diagnostic 2. Toxo Ig. G + & no prophylaxis: Empiric Rx • Clinical response is usually seen within 7 days (and often sooner), and • radiographic response in 14 days.

Toxoplasmosis z. Encephalitis ysensorimotor deficits, seizure, confusion, ataxia. y. Fever, headache common. y. Multiple ring-enhancing lesions y. Almost always due to reactivation

Toxoplasma Treatment z Pyrimethamine 100200 mg then 50 -100 mg/d + folinic acid 10 mg/d + sulfadiazine 4 -8 g/d for at least 6 weeks z Or sub clinda, azithro, clarithro or atovaquone z Steroids if mass effect

Toxoplasma prophylaxis z. Screen for Ig. G (BIII) yif negative, aggressively counsel regarding avoidance of cat litter, raw meat (165 deg) ywash, wear gloves when gardening ywash vegetables ykeep cats indoors, avoid raw meat foods ygetting rid of or testing the cat is an EIII offense! z. CD 4 <100 if seropositive only

Toxoplasma primary prophylaxis z. Trim/sulfa DS qd (AII) zdapsone/pyrimethamine (BI) zatovaquone (CIII) zdapsone, macrolides, pyrimethamine don’t work (DII) z. Aerosolized pentam definitely doesn’t work (EII)

Toxoplasma primary prophylaxis z Stop primary px when CD 4 > 200 for 3 months z stop secondary z restart when CD 4 drops <100 again

Toxoplasma secondary prophylaxis z. After initial therapy completed z. Pyrimethamine plus sulfadiazine zpyrimethamine plus clinda (not for PCP) zstop when CD 4>200 for 6 months, no symptoms and initial therapy completed zrestart if drop below 200

What’s new?

What’s new? z. Drug interactions z. Immunization guidelines z. HHV-8 transmission zemphasized HCV screening

References z Opportunistic infections in HIV disease: down but not out. Sax PE - Infect Dis Clin North Am - 01 -JUN-2001; 15(2): 433 -55 z Graybill JR, Sobel J, Saag M, et al: Diagnosis and management of increased intracranial pressure in patients with AIDS and cryptococcal meningitis. The NIAID Mycoses Study Group and AIDS Cooperative Treatment Groups. Clin Infect Dis 30: 47, 2000 z Infectious diarrhea in human immunodeficiency virus. Cohen J - Gastroenterol Clin North Am - 01 -SEP-2001; 30(3): 637 -64 z AMERICAN GASTROENTEROLOGICAL ASSOCIATION PRACTICE GUIDELINES. AGA Technical Review: Malnutrition and Cachexia, Chronic Diarrhea, and Hepatobiliary Disease in Patients With Human Immunodeficiency Virus Infection. Volume Gastroenterology 111 • Number 6 • December 1, 1996 z State-of-the-art review of pulmonary fungal infections. Seminars in Respiratory Infections. Volume 17 • Number 2 • June 2002