HISTORY TAKING GENERAL EXAMINATION By Dr Zahoor 1

HISTORY TAKING & GENERAL EXAMINATION By Dr. Zahoor 1

History Taking Important Points �Look confident �Welcome the patient saying Asalam O Alaikum �Shake hand with patient �Introduce yourself – I am so and so medical student 2

Important Points �Explain that you wish to ask some questions to find out what happened �Make sure patient is comfortable and curtains are in place �Confirm patient’s name, age, occupation 3

Importance of History �Ask principal symptoms and allow the patient to describe �Inquire about the sequence of symptoms and events �Don’t ask leading questions in the beginning 4

Usual Sequence of History 1. Chief complaint with duration 2. History of present illness 3. Past history e. g. past illness, admission in hospital, surgery 4. Family history 5. Personal and social history – smoker/not, travel, pet, animal contact Drug history including allergies 5

1. Chief complaint with duration �Patient c/o chest pain – 2 months 2. History of present illness �Ask when he was completely well? Then what happened and then describe symptoms in chronological order of onset �Obtain detailed description of each symptom 6

2. History of Present Illness �With all symptoms obtain details eg if pain - Duration - One set – acute or gradual - Constant or periodic - Frequency, radiation - Precipitating or relieving factors - Associated symptoms 7

Example 1 �Chest pain – 2 months Ask Ø Site of pain Ø Character – feeling pressure, dull, stabbing, shooting Ø Radiation 8

Example 1 (cont) Ø Severity – interfere with work or sleep Ø H/O this pain before Ø Pain associated with nausea, sweating e. g. angina Note – When patient is unable to give history, then get necessary information from friends, relative 9

Example 2 �If patient c/o cough with sputum – 10 days Ask about cough �When he was well, how it started �When do you have cough, how long it lasts �Can he sleep well �Precipitating factors, relieving factors Sputum �Color, how much amount do you cough up, smell, any blood in the sputum 10

3. Past history Ask for �Previous illness, hospital admission �Any operations (if yes, when it was done and what was the problem) �Medicines 11

4. Family History Ask about �Parents – father and mother are alright �Any history of hypertension, diabetes mellitus �If history of death – what was the cause of death �How many brothers and sisters you have? They are alright. 12

5. Personal and social history �Ask about job. �Are you married? �How many children do you have? Their age? They are fine? �Ask about, smoker/not, travel, pet, animal contact, any medicine he’s taking and allergy �If patient is old – ask about where he lives e. g. ground floor or upstairs �Any difficulties regarding toilet, cooking, shopping? 13

Specimen History � Mr. Ahmed � Age: 50 years, machine operator � C/O severe chest pain – 2 hours � But gives H/O chest pain since 6 months Date - _____ History of present illness � Perfectly well until 6 months ago, began to notice central dull chest pain occasionally radiating to the jaw, coming when he walks about 1 km, worse when going up hill and in cold weather, when he stops the pain goes away after 2 mins � GTN sublingual relieved pain 14

Specimen History �Last month, pain came on less exercise after 100 yards �Today at 10 am, while sitting at work, chest pain started suddenly. It was worse pain he had experienced. The pain was central crushing in nature radiating to the left arm and neck with feeling of nausea and sweating �The patient was rushed to hospital where he received IV Diamorphine and ECG was done which showed ANTERIOR MI and he was given IV Streptokinase 15

Specimen History �After history of present illness, you will take past history, family history, personal and social history 16

Usual Sequence of Events in Patient Care �History �Examination – General Examination – Systemic Examination �Problem list �Differential diagnosis and most likely diagnosis �Investigations �Diagnosis confirmed �Treatment 17

General Examination 18

General Examination �General Examination includes - General appearance - Alertness, mood, general behavior - Hands and nails - Radial pulse and blood pressure - Lymph node – Cervical , Axillary - Face, eyes, tongue - Peripheral oedema 19

General Examination General appearance �Does the patient look ill ? �Alert, confused, drowsy �Co-operative, happy, sad �Obese, muscular, wasted �In pain or distressed 20

General Examination Hands and nails Hands � Unduly cold, warm, cold and sweaty (anxiety, sympathetic over activity) � Peripheral cyanosis � Nicotine staining � Raynaud’s � Palms – palmer Erythema may be normal, also occurs with chronic liver disease, pregnancy � Dupuytren’s contracture – thickened palmer skin to the flexor tendons of fingers (fourth finger) 21

General Examination Nails Clubbing � The tissue at the base of nail are thickened � The angle between the base of nail and adjacent skin of finger is lost � Nails become convex both transversely and longitudinally Causes - heart – infective endocarditis - lung – carcinoma bronchus, Bronchiectasis, fibrosing alveolitis - liver cirrhosis - Crohn’s disease 22

General Examination Nails (Cont) �Koilonychia – Concave nail (iron deficiency anemia) �Leukonychia – white nails (cirrhosis liver) �Splinter hemorrhages - Infective endocarditis � Pitting – psoriasis �Onycholysis – separation of nail from nail bed Psoriasis, Throtoxicosis 23

Finger clubbing 24
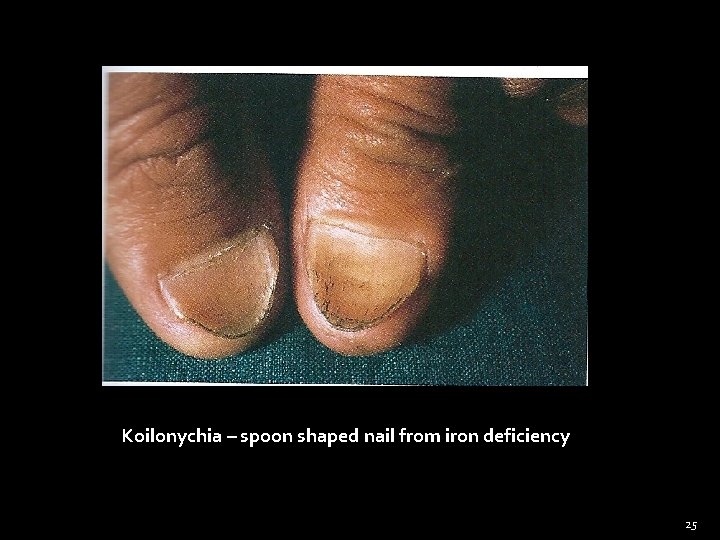
Koilonychia – spoon shaped nail from iron deficiency 25
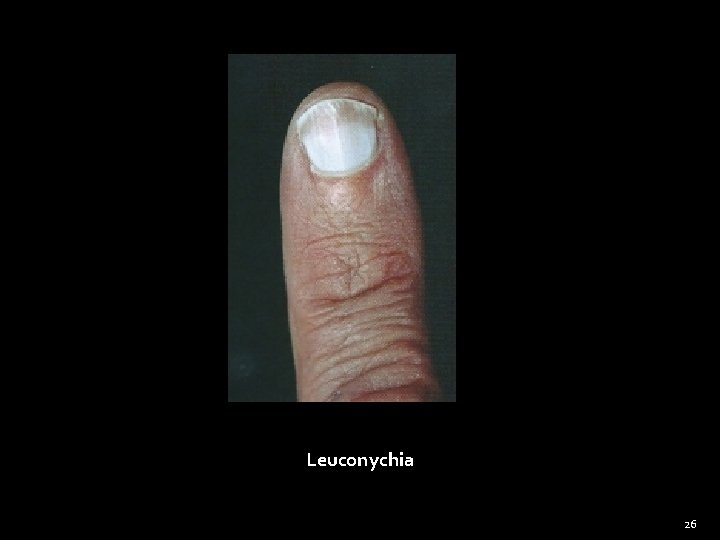
Leuconychia 26
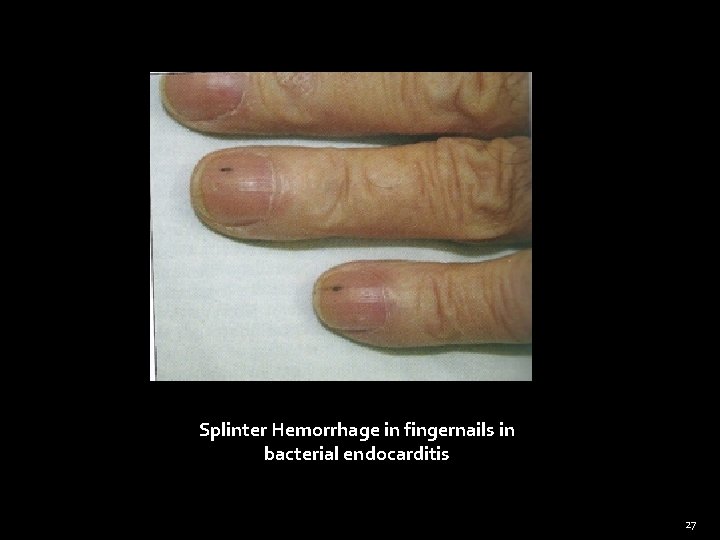
Splinter Hemorrhage in fingernails in bacterial endocarditis 27
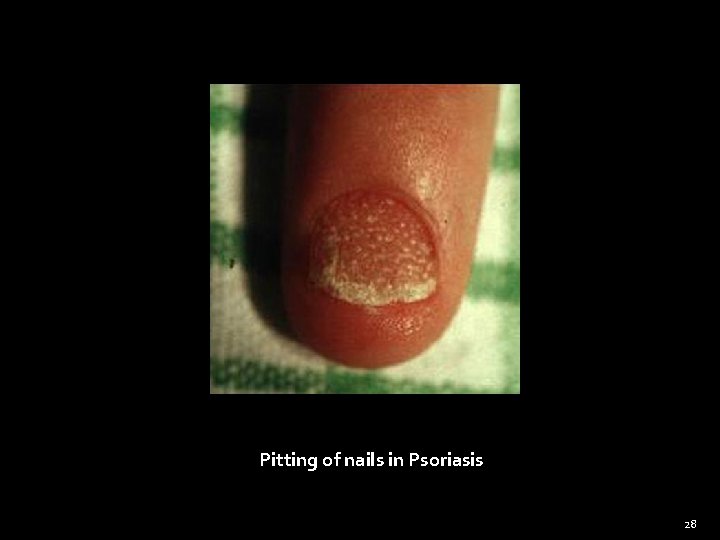
Pitting of nails in Psoriasis 28
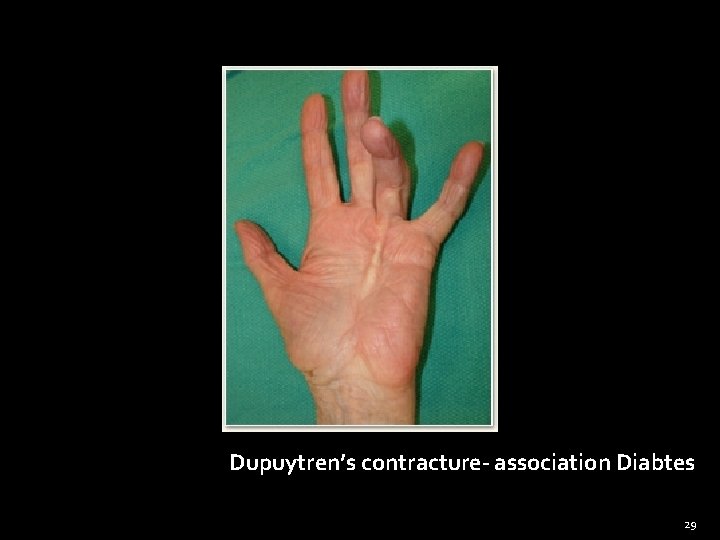
Dupuytren’s contracture- association Diabtes 29

General Examination Face, eyes, tongue �Mouth – look at the tongue moist or dry - Cyanosed (central) �Central cyanosis – blue tongue Cause: - Congenital heart disease e. g. fallot’s tetralogy - Lung disease e. g. obstructive airway disease �Peripheral cyanosis – blue fingers denotes inadequate peripheral circulation, tongue will be pink 30

General Examination Face, eyes, tongue (cont) Mouth �Look at the teeth – dental hygiene, caries �Look at the gums – bleeding, swollen �Smell patient’s breath - Ketosis – diabetes (sweet smelling breath) - Foetor – hepatic failure (musty smell) - Alcohol 31

General Examination Face, eyes, tongue (cont) Eyes �Look at the sclera – for jaundice (yellow sclera) �Look at lower lid conjunctiva – anemia (pale, mucous membrane of conjunctiva) �Eye lid – yellow deposit (Xanthelasma) �Puffy eyelid e. g. general oedema (Nephrotic syndrome) , thyroid eye disease (myxoedema) 32

General Examination Eyes (cont) �Red eye – Iritis, conjunctivitis, episcleritis �White line around cornea, Arcus senilis – suggest hyperlipidaemia in younger patient, but has little significance in elderly �White band keratopathy – hypercalcaemia - Sarcoid - Parathyroid – hyperplasia - Lung oat – cell tumor - Vitamin D excess intake 33
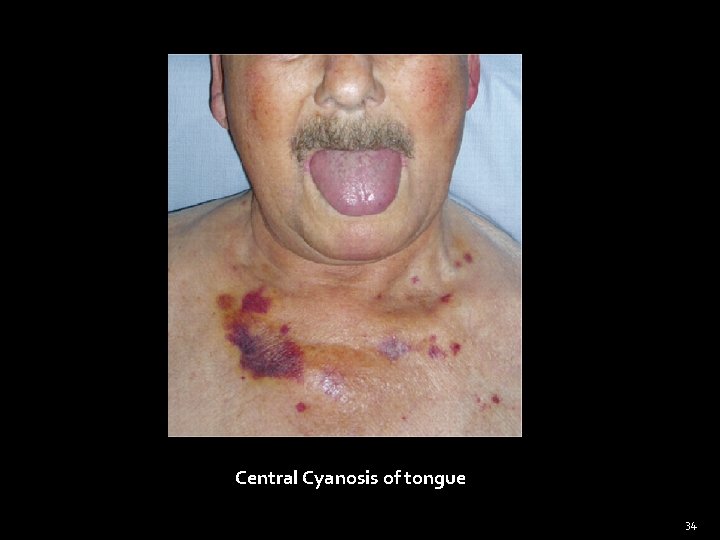
Central Cyanosis of tongue 34
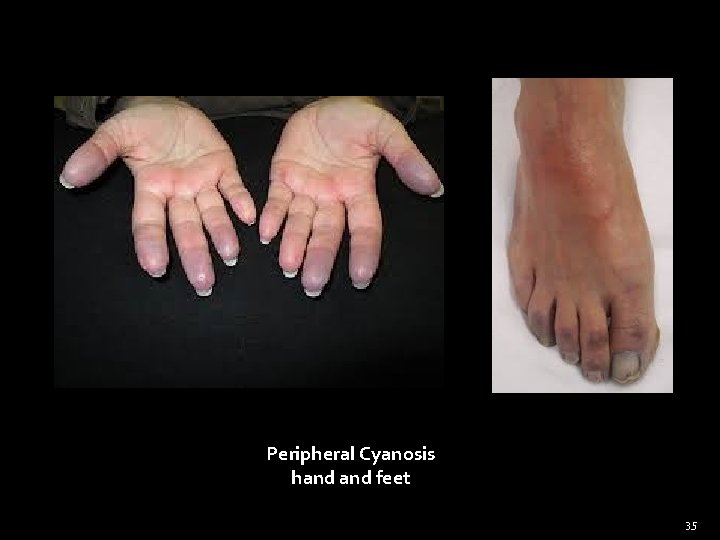
Peripheral Cyanosis hand feet 35
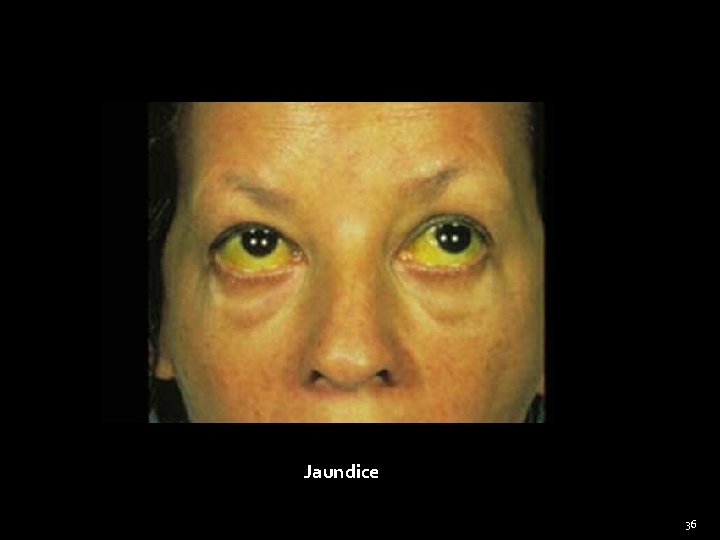
Jaundice 36
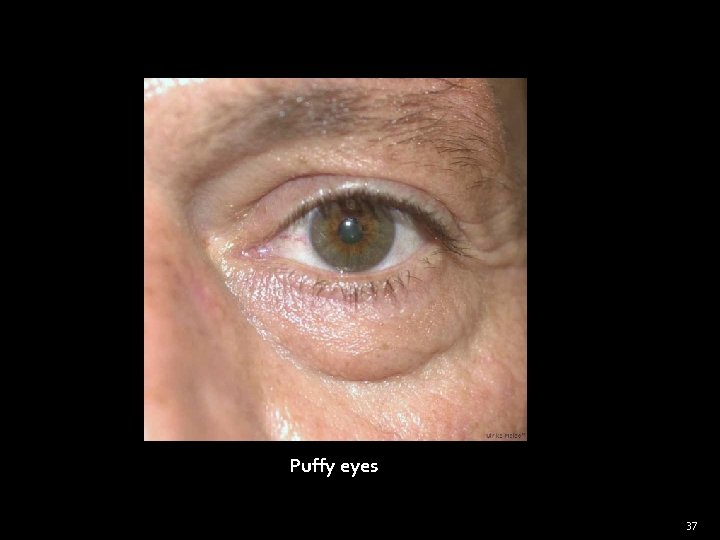
Puffy eyes 37
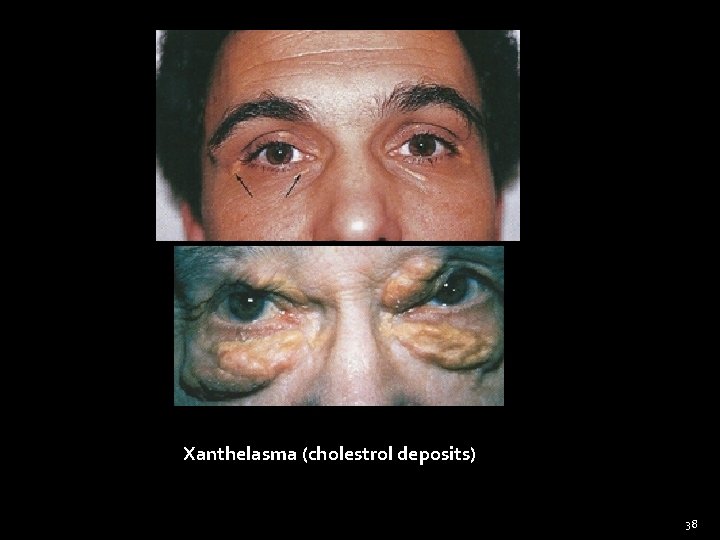
Xanthelasma (cholestrol deposits) 38
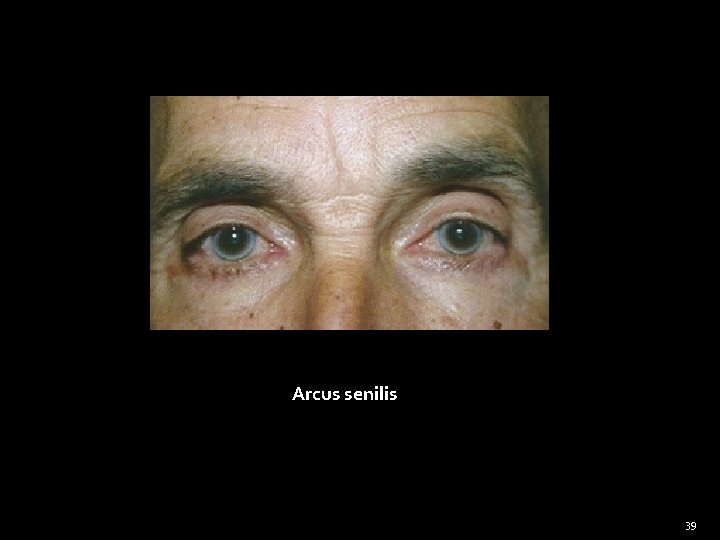
Arcus senilis 39
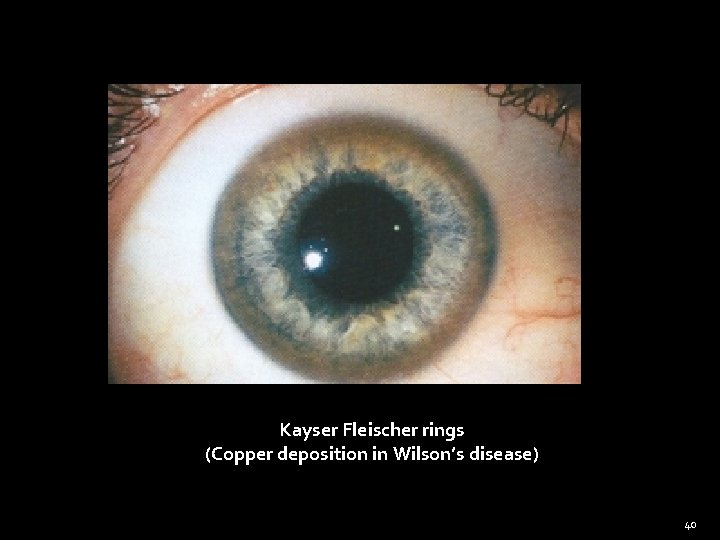
Kayser Fleischer rings (Copper deposition in Wilson’s disease) 40
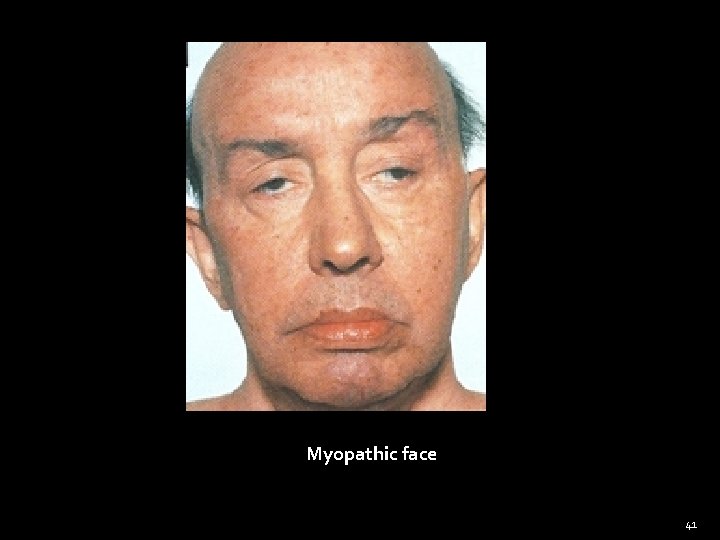
Myopathic face 41
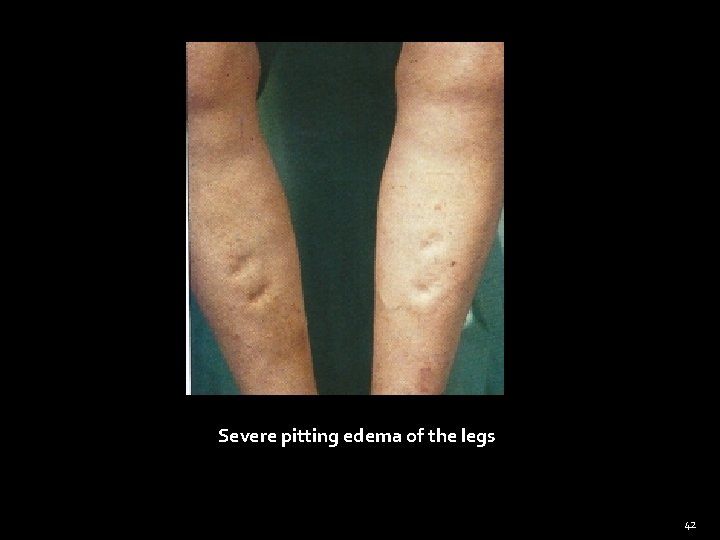
Severe pitting edema of the legs 42
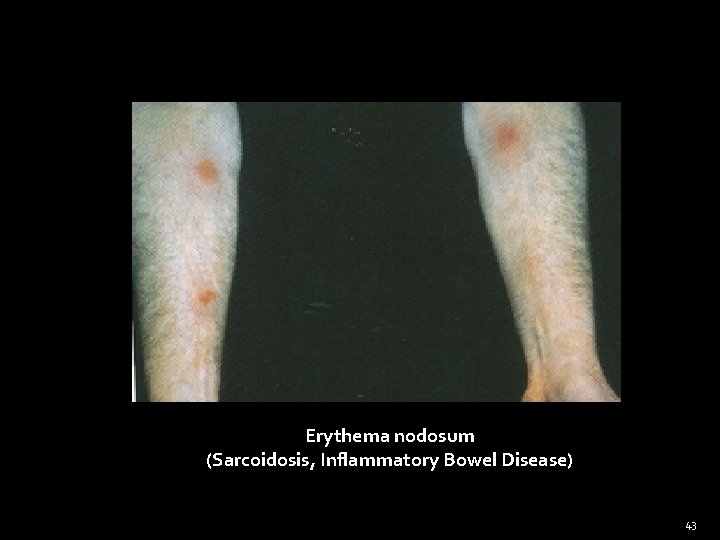
Erythema nodosum (Sarcoidosis, Inflammatory Bowel Disease) 43
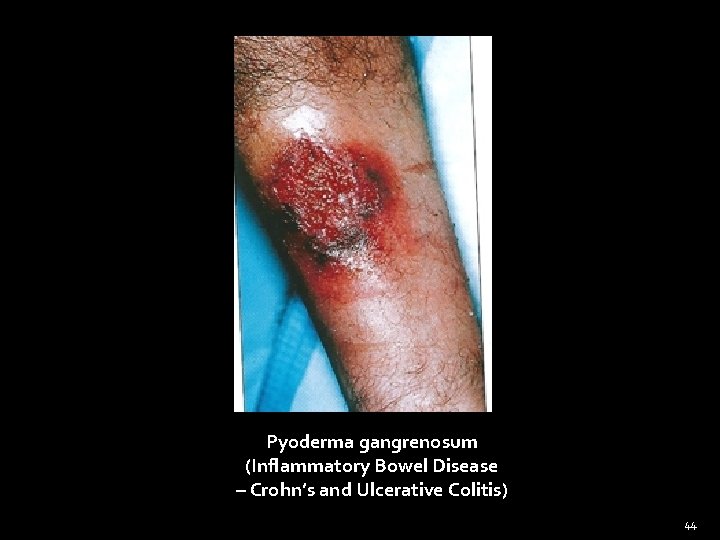
Pyoderma gangrenosum (Inflammatory Bowel Disease – Crohn’s and Ulcerative Colitis) 44

�In the end (after taking history and examination), ask him – Have you any questions. �Please remember to cover the patient and THANK him/ her at the end of examination. �Note : After history you should have ideas which system you wish to concentrate for examination. And after examination, you should put diagnosis/differential diagnosis 45

Thank you 46
- Slides: 46