History of Colon Wound Management 43 rd Annual





















































- Slides: 73

History of Colon Wound Management 43 rd Annual Phoenix Surgical Symposium Scottsdale, AZ Elvis Presley Memorial Trauma Center UTHSC Department of Surgery Memphis, TN

I have no conflicts to disclose

History of Colon Wounds 1330 BC “And the hilt also went in after the blade; and the fat closed upon the blade, for he drew not the sword out of his belly; and the dirt came out. ” Judges 3: 21 -22

Civil War Experience • Penetrating colon wounds managed predominantly non-operatively • Staggering mortality rates (>90%) with most patients succumbing to infection and sepsis • Attempts at surgery led to mortality rates equivalent to non-operative management

World War I • Introduction of high-velocity missiles • Most destructive injuries • Early care consisted of expectant management • Later attempts were made at primary repair or diversion • Mortality 60 -75%

World War II • Mortality fell to 22 -35% • Advancements in - Triage - Aggressive resuscitation - Improved antibiotics - Blood banks • Exteriorization of ALL colon injuries

"The treatment of colon injuries is based on the known insecurity of suture and the dangers of leakage. Simple closure of a wound of the colon, however small, is unwarranted; men have survived such an operation, but others have died who would still be alive had they fallen into the hands of a surgeon with less optimism and more sense. Injured segments must either be exteriorized, or functionally excluded by a proximal colostomy. " W. H. Ogilvie 'Forward Surgery in Modern War', 1944

“The exteriorization of colon injuries, a step which I have repeatedly advocated since the outbreak of war is, perhaps the greatest single factor in the improved results we are able to record. ” Primary repair COURT MARTIAL W. H. Ogilvie ‘Abdominal Wounds in the Western Desert’, 1944

“At the Charity Hospital of Louisiana in New Orleans, 23 cases of colon injury were treated during the years 1945 and 1946. Primary suture was used in 15 of these cases, but during 1947 and 1948, the influences of war surgery became evident, because in 25 cases of colon injury, only five were treated with primary suture. Although exteriorization or proximal decompression proved valuable in the treatment of battle colon injuries, an evaluation of the results obtained in civilian practice is essential. ”

Ann Surg 1979

Criteria for Obligatory Colostomy 1. Preop shock (< 80 / 60) 2. Intraperitoneal hemorrhage > 1000 ml 3. > 2 intra-abdominal organ systems injured 4. Significant peritoneal contamination by feces 5. Injury to operation > 8 hours 6. Colon wound so destructive as to require resection 7. Abdominal wall major loss of substance / mesh replacement Stone HH, Fabian TC: Management of Perforating Colon Trauma. Ann Surg, Oct. 1979

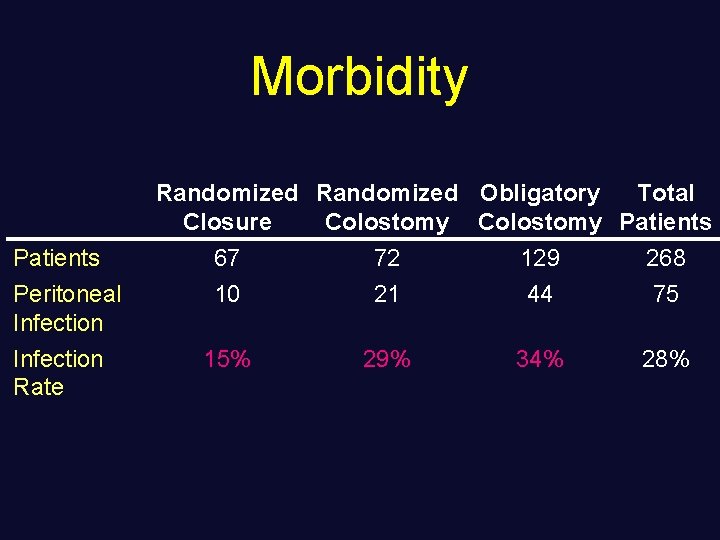
Morbidity Randomized Obligatory Total Closure Colostomy Patients 67 72 129 268 Peritoneal Infection 10 21 44 75 15% 29% 34% 28% Infection Rate

Conclusions • Confirmed the safety of primary closure for colon wounds in selected cases • But what qualifies a “high risk” patient?

• 102 pts with penetrating colon injuries • Pts managed regardless of shock, contamination, or associated injuries • Management - 83 primary repair → no leaks - 12 resection & anastomosis → 1 leak - 7 end colostomy Ann Surg 1989

Risk Factors • Risk factors for intra-abdominal sepsis or complication - Transfusion > 4 units - Significant contamination - Increased colon injury score • Concluded nearly all penetrating injuries can be repaired primarily or with resection & anastomosis

To Resect or Not Resect … • Chappuis et al. , Ann Surg 1991 - “…primary repair or resection & anastomosis should be considered for treatment of all patients” - Generalization was made from a relatively small number of pts (n=11) receiving resection & anastomosis • When is resection + anastomosis appropriate over diversion?


Destructive Colon Injuries • Wounds involving > 50% of colon wall circumference • Complete transection • Devascularized segments

Stewart et al - Memphis 1994 60 patients with destructive colon injuries Destructive Wounds + Co-morbidities / > 6 u PRBCs 42% suture line failure Destructive Wounds + No Co-morbidities / < 6 u PRBCs 3% suture line failure

Significant Co-morbidities • • • Cirrhosis Human Immunodeficiency Virus Severe Diabetes Congestive Heart Failure Chronic Renal Failure Patients on Chronic Steroids

Management Algorithm Full-thickness Colon Injuries Nondestructive Primary Repair Destructive +Comorbidity >6 units PRBCs -Comorbidity ≤ 6 units PRBCs Diversion Resection + Anastomosis

• Conclusions: “On the basis of these data and the relative infrequency of patients in prospective randomized trials with destructive colon injuries, we believe there is still room for consideration of fecal diversion in patients in high-risk categories with destructive colon injuries requiring resection”

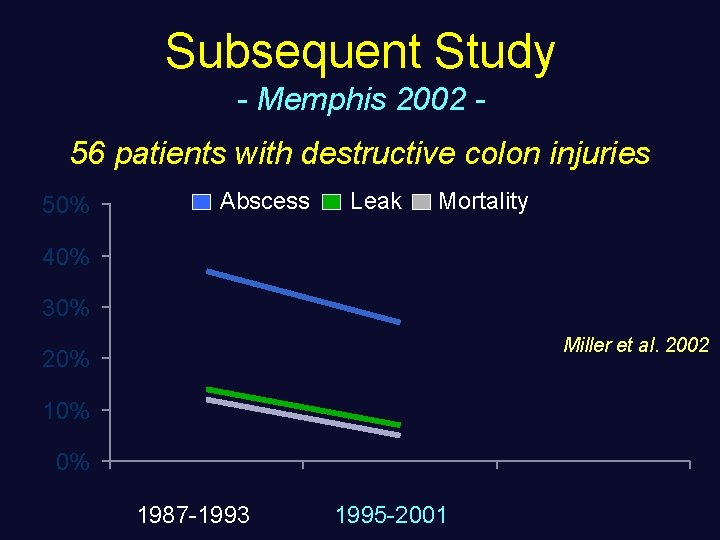
Subsequent Study - Memphis 2002 56 patients with destructive colon injuries 50% Abscess Leak Mortality 40% 30% Miller et al. 2002 20% 10% 0% 1987 -1993 1995 -2001

AAST Multi-institutional Study • 297 penetrating colon injuries requiring resection from 19 different centers • Regression analysis identified severe fecal contamination, transfusion > 4 u RBC, single agent abx prophylaxis as independent predictors of complication Demetriades et al. , J Trauma 2001

AAST Study Conclusions “In view of these findings, the reduced quality of life, and the need for subsequent operation in colostomy patients, primary anastomosis should be considered in all such patients” Demetriades et al. , J Trauma 2001

AAST Study Problems • Concluded # of transfusions as an independent predictor of complications - But not recommended to use for operative decisions • 19 different centers using 19 difference management schemes - No control for selection bias

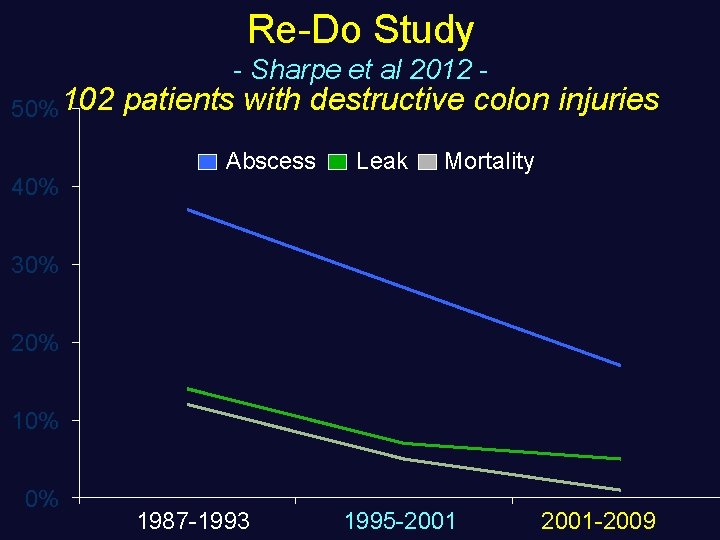
Re-Do Study 50% 102 40% - Sharpe et al 2012 - patients with destructive colon injuries Abscess Leak Mortality 30% 20% 10% 0% 1987 -1993 1995 -2001 -2009

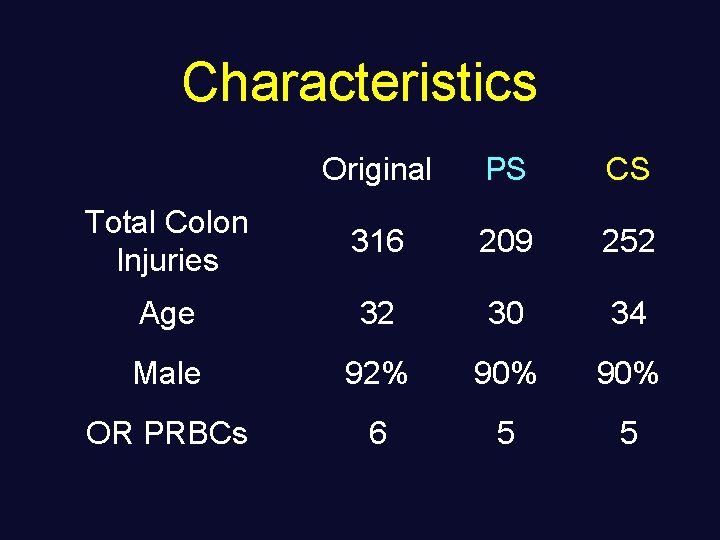
Characteristics Original PS CS Total Colon Injuries 316 209 252 Age 32 30 34 Male 92% 90% OR PRBCs 6 5 5

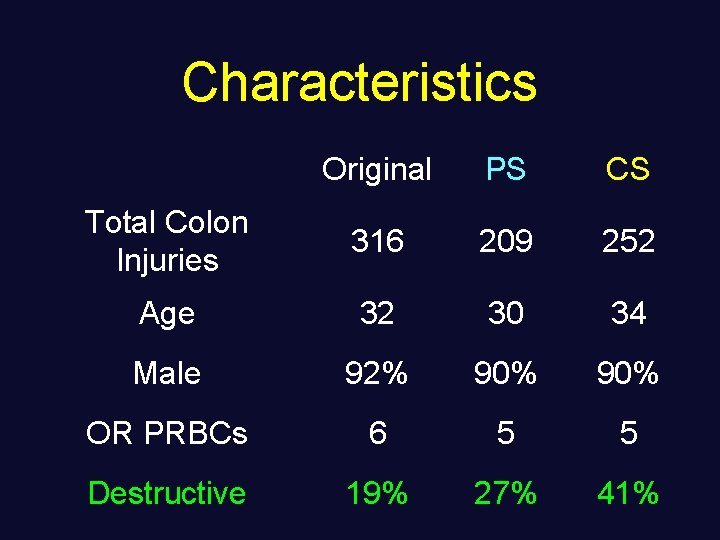
Characteristics Original PS CS Total Colon Injuries 316 209 252 Age 32 30 34 Male 92% 90% OR PRBCs 6 5 5 Destructive 19% 27% 41%

Algorithm Compliance – 90% 102 Destructive Injuries 92 Followed Pathway 69 R+A 10 Protocol Violations 3 Diversion 7 R+A 2 Leaks 2. 9% 29%

Left versus Right … • Controversy persists regarding the management of left-sided colon injuries • Is it safe to perform resection and anastomosis for destructive wounds to the left colon?

Anatomic Distinction • Historical perception of tenuous collaterals between the left colic artery and the middle colic artery • Most previous reports only focused on right vs left-sided injuries

Denver – 1981 • Review of 105 penetrating colon injuries over 5 years • No difference in rates of diversion, morbidity, and mortality between right & left-sided injuries Thompson et al. , Ann Surg 1981

Emory - 2005 - 217 Penetrating Injuries • Location subdivided into ascending, transverse, descending, & sigmoid • Baseline characteristics, injury severity, & management were similar • No comparison of outcomes between the anatomic locations • 7 suture line failures - 3 in distal transverse colon - 4 in splenic flexure Dente et al. , J Trauma 2005

Emory - 2005 - 217 Penetrating Injuries • Conclusions - “We feel, however, that a surgeon who is managing even what appears to be a simple wound to the splenic flexure should proceed with caution until better prospective data are available” • Data likely suffers from selection bias • Analysis should be obtained from an institution that manages all colon injuries the same, regardless of location Dente et al. , J Trauma 2005

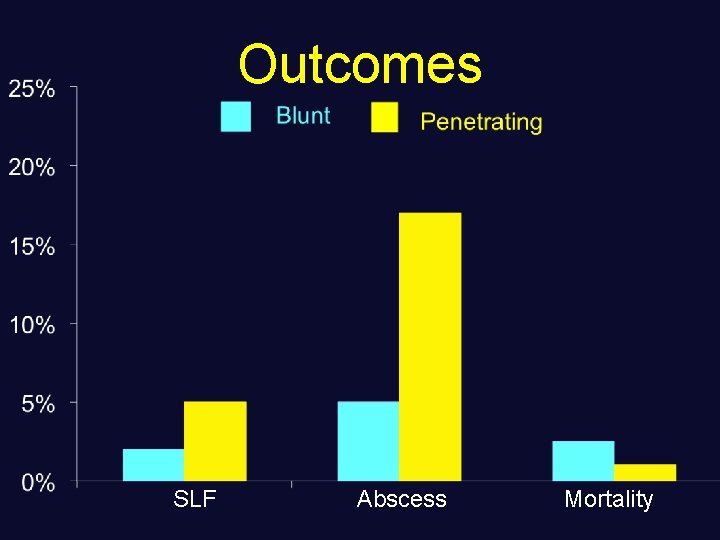
Patients • Penetrating colon injuries over a 13 year-period • Exclusions - Deaths within 24 hours - Rectal injuries - Partial thickness injuries Outcomes • Colon-related Morbidity - Suture line failure - Abscess • Colon-related Mortality Outcomes were compared between the different colon locations

469 Patients

469 Patients 33%

469 Patients 29%

469 Patients 14%

469 Patients 24%

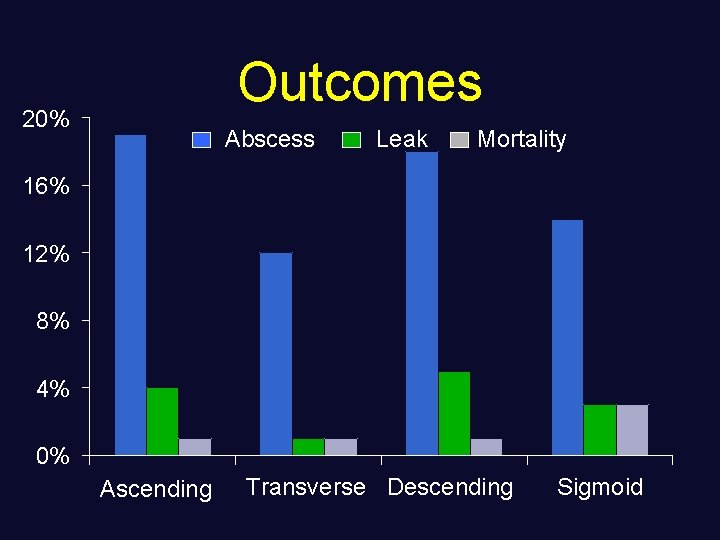
Outcomes 20% Abscess Leak Mortality 16% 12% 8% 4% 0% Ascending Transverse Descending Sigmoid

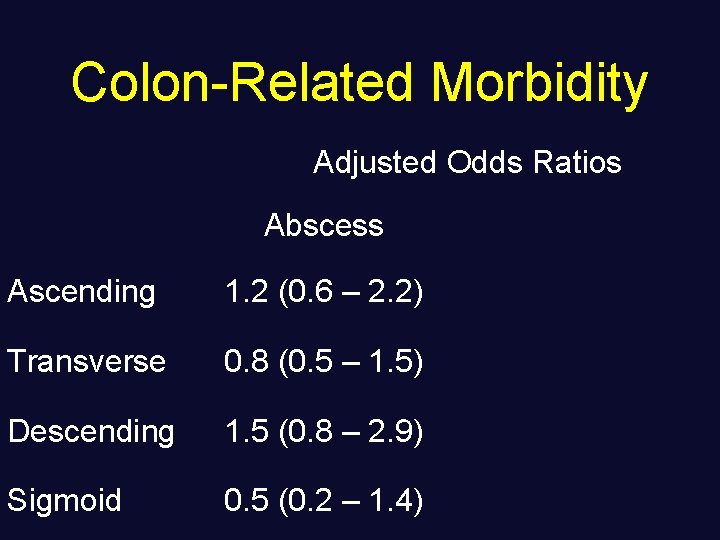
Colon-Related Morbidity Adjusted Odds Ratios Ascending Transverse Descending Sigmoid

Colon-Related Morbidity Adjusted Odds Ratios Abscess Ascending 1. 2 (0. 6 – 2. 2) Transverse 0. 8 (0. 5 – 1. 5) Descending 1. 5 (0. 8 – 2. 9) Sigmoid 0. 5 (0. 2 – 1. 4)

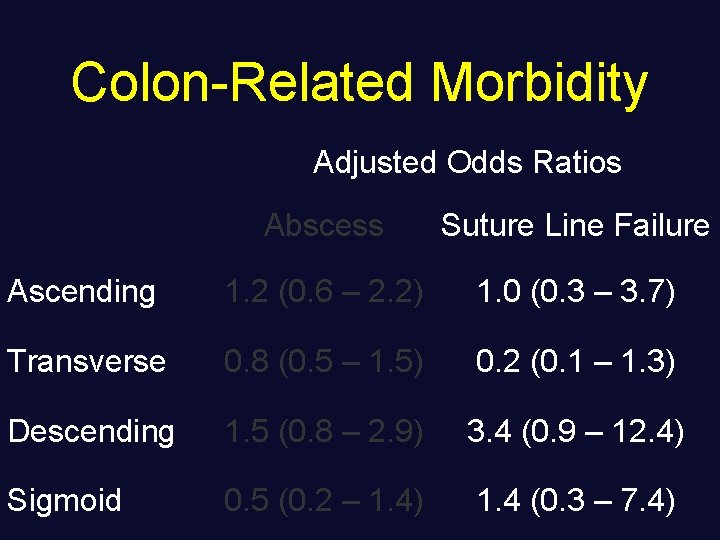
Colon-Related Morbidity Adjusted Odds Ratios Abscess Suture Line Failure Ascending 1. 2 (0. 6 – 2. 2) 1. 0 (0. 3 – 3. 7) Transverse 0. 8 (0. 5 – 1. 5) 0. 2 (0. 1 – 1. 3) Descending 1. 5 (0. 8 – 2. 9) 3. 4 (0. 9 – 12. 4) Sigmoid 0. 5 (0. 2 – 1. 4) 1. 4 (0. 3 – 7. 4)

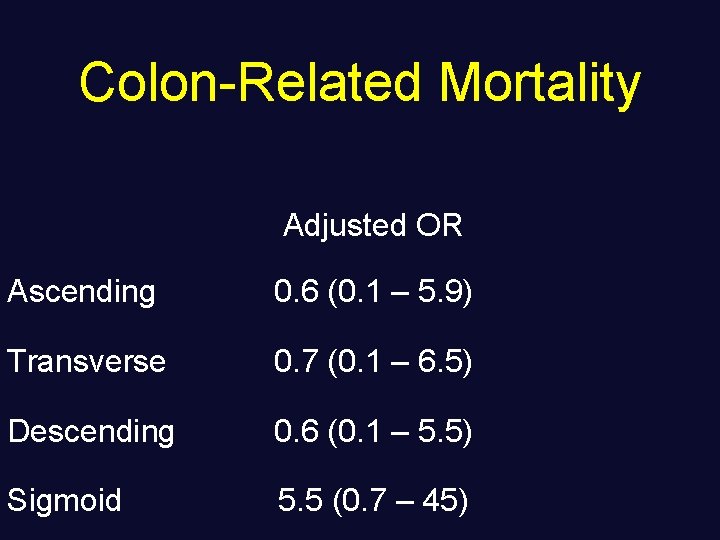
Colon-Related Mortality Adjusted OR Ascending 0. 6 (0. 1 – 5. 9) Transverse 0. 7 (0. 1 – 6. 5) Descending 0. 6 (0. 1 – 5. 5) Sigmoid 5. 5 (0. 7 – 45)

Conclusions • Injury location did not impact morbidity or mortality following penetrating colon injuries • Non-destructive injuries should be primarily repaired • For destructive injuries, operative decisions based on a defined algorithm rather than injury location achieves an acceptably low morbidity and mortality rate and simplifies management

What about Blunt Injuries? • Reported incidence 0. 1 – 0. 5% • Little research regarding management • Wounds prone to ischemia secondary to mesenteric compromise

Approach • Traditional management schemes for penetrating colon injuries may not apply to blunt injuries • Controversy persists regarding the optimal management of these difficult injuries

Study Design Patients • Blunt colon injuries over a 13 year-period • Exclusions - Deaths within 24 hours - Rectal injuries Outcomes • Colon-related Morbidity - Suture line failure - Abscess • Colon-related Mortality Outcomes were evaluated to determine if additional risk factors should be considered in the management of blunt colon injuries

Destructive Colon Injuries • Serosal wounds involving > 50% of colon wall circumference • Mesenteric devascularization • Full-thickness perforations

95% Algorithm Compliance 151 Blunt Colon Injuries 143 Followed Pathway 75 Reserosalization 44 R+A 2 Leaks 1. 7%

95% Algorithm Compliance 151 Blunt Colon Injuries 143 Followed Pathway 75 Reserosalization 44 R+A 8 Protocol Violations 5 R+A 3 Primary Repair/ Reserosalization 2 Leaks 1 Leak 1. 7% 12. 5%

Outcomes SLF Abscess Mortality

Conclusions • Adherence to a defined algorithm was efficacious for the management of blunt colon injuries

Conclusions • Adherence to a defined algorithm was efficacious for the management of blunt colon injuries Colon Injuries Nondestructive Primary Repair Destructive +Comorbidity >6 units PRBCs -Comorbidity ≤ 6 units PRBCs Diversion R+ A

What about this situation?

Wake Forest – 2007 - 22 pts with open abdomen • 11 patients underwent resection with delayed anastomosis (DA) • 0 leaks • “DA is safe in selected patients” Truth: Almost half (45%) of those 11 patients died prior to hospital discharge Miller et al, Am Surg 2007

Alabama – 2009 - 56 pts with open abdomen • 33 patients underwent resection with DA • 12% leak rate • Colon-related morbidity for DA was larger than for anastomosis in single laparotomy Anastomosis in the setting of an open abdomen is a “cautionary tale, ” and diversion may be a safer alternative Weinberg et al, J Trauma 2009

Denver – 2009 - 29 pts with open abdomen • 25 patients underwent resection with DA • 16% leak rate • Concluded DA was safe in most patients managed with an open abdomen Despite a larger suture line failure rate compared to Weinberg et al (16 vs 12%), authors have drawn different conclusions Kashuk, Moore, Surgery 2009

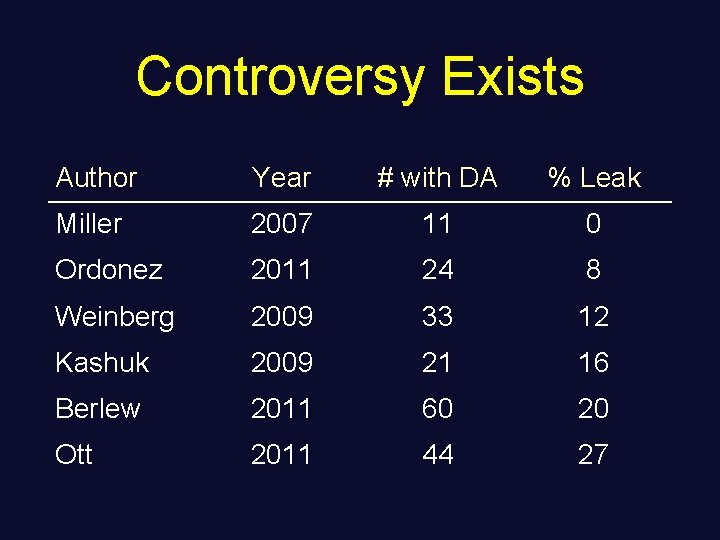
Controversy Exists Author Year # with DA % Leak Miller 2007 11 0 Ordonez 2011 24 8 Weinberg 2009 33 12 Kashuk 2009 21 16 Berlew 2011 60 20 Ott 2011 44 27

What about our algorithm? • Risk factors for colon injuries were defined prior to the widespread use of abbreviated laparotomy (AL) or open abdomen • Do not necessarily address the issue of performing delayed anastomosis • May place the patient at increased risk of suture line failure

Study Design Patients • Destructive colon injuries over a 17 year-period • Exclusions - Deaths within 24 hours - Rectal injuries - Single laparotomy Outcomes • Colon-related Morbidity - Suture line failure - Abscess • Colon-related Mortality Outcomes were evaluated to determine if additional risk factors should be considered in the management of destructive colon injuries following abbreviated laparotomy

Destructive Colon Injuries Penetrating • • Wound >50% of colon wall Complete transection Significant tissue loss Devacularized segments Blunt • Serosal tear >50% of colon wall • Full thickness perforation • Mesenteric devascularization

Study Population 149 Patients 117 Destructive 32 Nondestructive 42 DA 72 SD 2 Early deaths, 1 PR

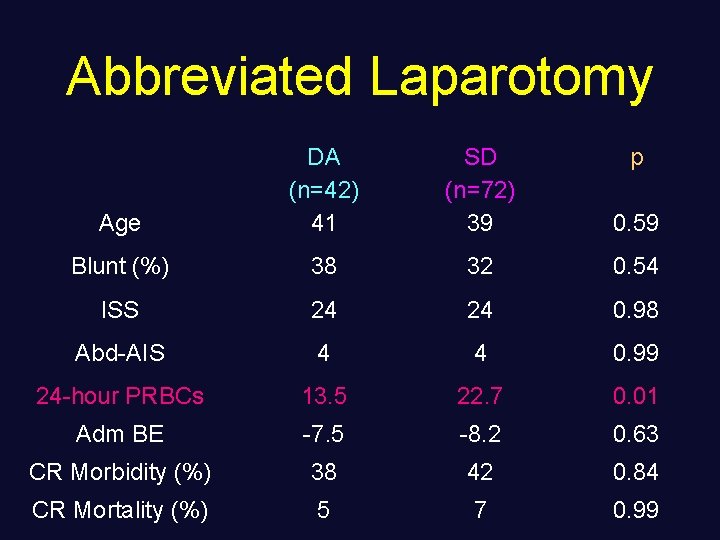
Abbreviated Laparotomy Age DA (n=42) 41 SD (n=72) 39 p 0. 59 Blunt (%) 38 32 0. 54 ISS 24 24 0. 98 Abd-AIS 4 4 0. 99 24 -hour PRBCs 13. 5 22. 7 0. 01 Adm BE -7. 5 -8. 2 0. 63 CR Morbidity (%) 38 42 0. 84 CR Mortality (%) 5 7 0. 99

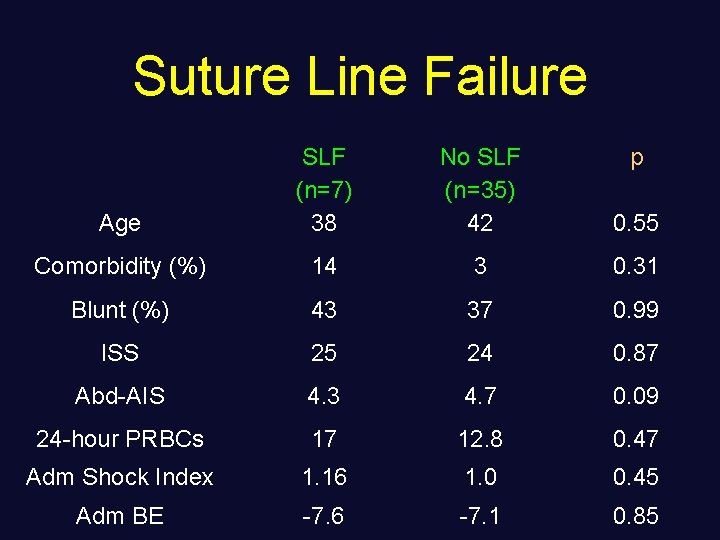
Suture Line Failure Age SLF (n=7) 38 No SLF (n=35) 42 p 0. 55 Comorbidity (%) 14 3 0. 31 Blunt (%) 43 37 0. 99 ISS 25 24 0. 87 Abd-AIS 4. 3 4. 7 0. 09 24 -hour PRBCs 17 12. 8 0. 47 Adm Shock Index 1. 16 1. 0 0. 45 Adm BE -7. 6 -7. 1 0. 85

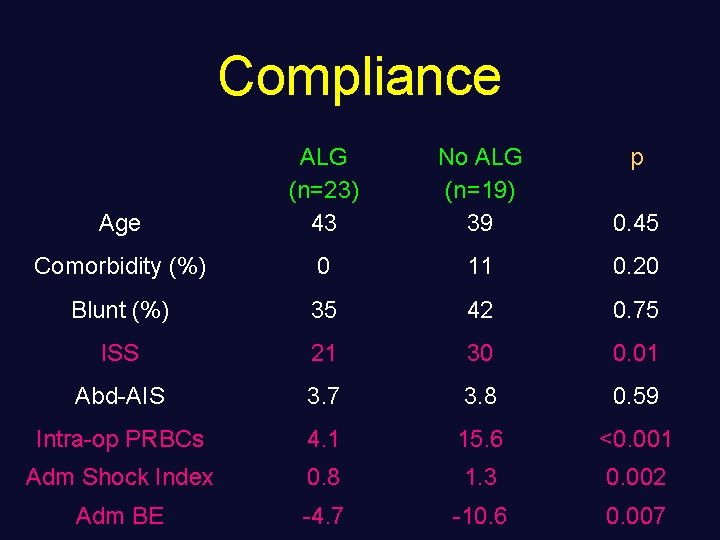
Compliance Age ALG (n=23) 43 No ALG (n=19) 39 p 0. 45 Comorbidity (%) 0 11 0. 20 Blunt (%) 35 42 0. 75 ISS 21 30 0. 01 Abd-AIS 3. 7 3. 8 0. 59 Intra-op PRBCs 4. 1 15. 6 <0. 001 Adm Shock Index 0. 8 1. 3 0. 002 Adm BE -4. 7 -10. 6 0. 007

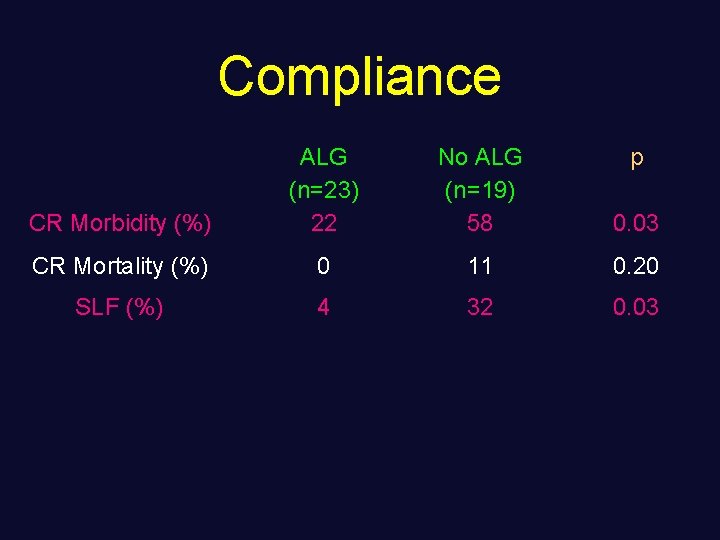
Compliance CR Morbidity (%) ALG (n=23) 22 No ALG (n=19) 58 p 0. 03 CR Mortality (%) 0 11 0. 20 SLF (%) 4 32 0. 03

Conclusions • The management of destructive colon injuries in the setting of AL is not straightforward • The decision-making process is multi-factorial, relying on both objective and subjective information • Adherence to an established algorithm, originally defined and validated for destructive colon injuries following single laparotomy was efficacious for the management of these injuries in the setting of AL

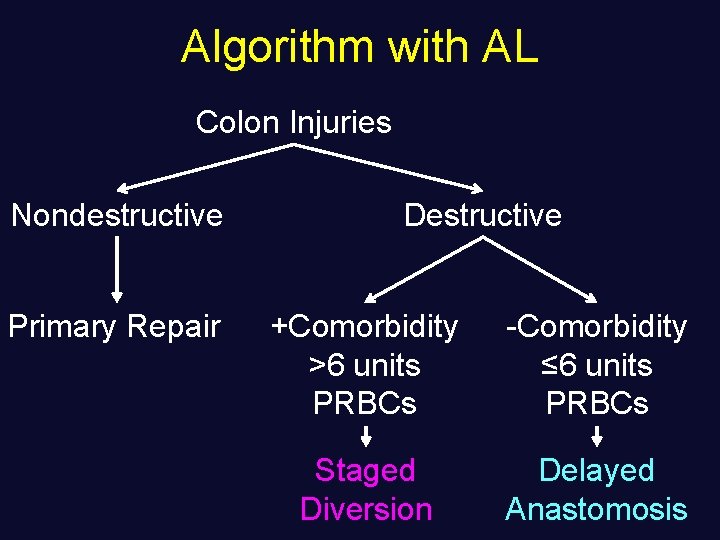
Algorithm with AL Colon Injuries Nondestructive Primary Repair Destructive +Comorbidity >6 units PRBCs -Comorbidity ≤ 6 units PRBCs Staged Diversion Delayed Anastomosis

Summary • Primary repair is the treatment of choice for nondestructive colon wounds • Resection & anastomosis is safe in selected patients • Adherence to a defined clinical pathway results in optimal outcomes - Destructive wounds - Blunt injury - Abbreviated laparotomy
