Histopathological diagnosis Pathology Irreversible loss of functioning hepatocyte
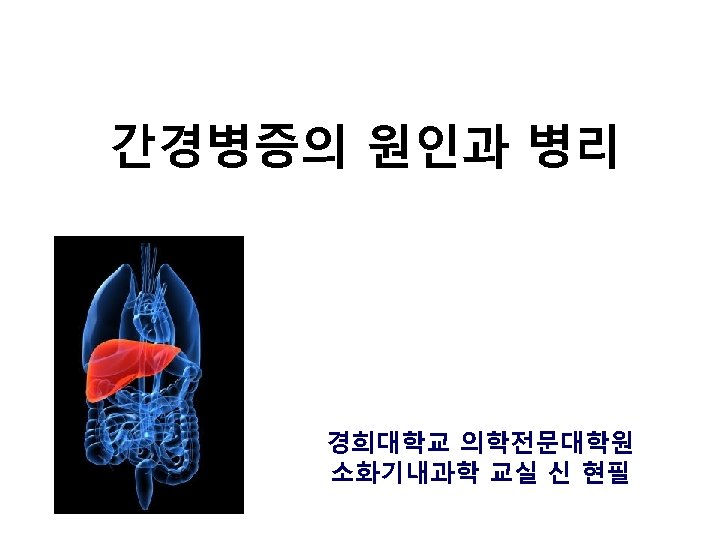

Histopathological diagnosis • Pathology 특징 · Irreversible loss of functioning hepatocyte · Extensive fibrosis · Formation of regenerative nodule • Irreversible? reversal of fibrosis 일부 가능. • Fibrosis 발달되어 architectural distortion + regenerative nodules 형성할 정도. hepatocellular mass와 function 저하, blood flow 변화 유도.
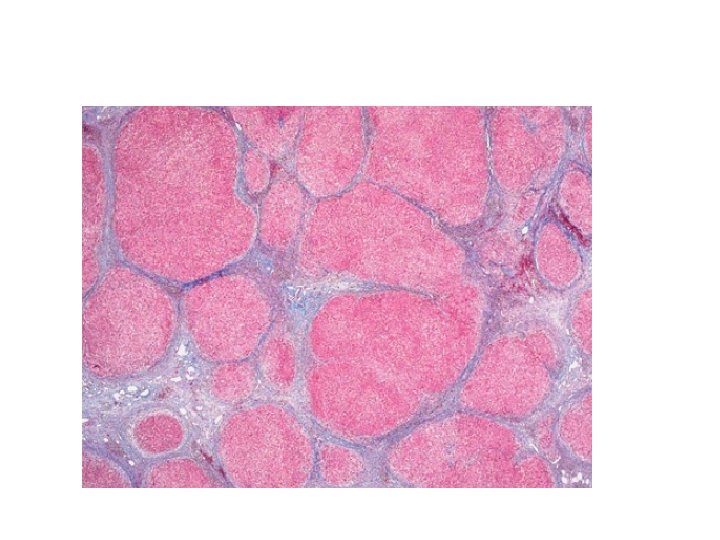

Fiborsis • • Hepatic stellate cells activation : fibrosis induction collagen과 다른 extracellular matrix 양 증가. 임상적 특성: pathologic changes의 결과로 간질환 정도 반영 Pathologic grading and staging (Advanced fibrosis) Bridging fibrosis with nodularity : stage 3 Cirrhosis : stage 4. Hepatocellular function 상실의 결과: jaundice, coagulation disorders, hypoalbuminemia, portosystemic encephalopathy.

Causes of Cirrhosis

Portal Hypertension The portal venous system : blood from the stomach, intestines, spleen, pancreas, and GB portal vein : confluence of the superior mesenteric and splenic veins hepatic venous pressure gradient (HVPG) to >5 mm. Hg 상승 두 가지 hemodynamic processes (1) increased intrahepatic resistance to the passage of blood flow by cirrhosis and regenerative nodules (2) increased splanchnic blood flow secondary to vasodilation within the splanchnic vascular bed 2 major complications of cirrhosis (1) variceal hemorrhage life-threatening 20– 30% mortality (each) (2) ascites

Portal HTN 원인분류 Prehepatic Portal vein thrombosis Splenic vein thrombosis Massive splenomegaly (Banti's syndrome) Hepatic Presinusoidal Schistosomiasis Congenital hepatic fibrosis Sinusoidal Cirrhosis—many causes Alcoholic hepatitis Postsinusoidal Hepatic sinusoidal obstruction (venoocclusive syndrome) Posthepatic Budd-Chiari syndrome Inferior vena caval webs Cardiac causes Restrictive cardiomyopathy Constrictive pericarditis Severe congestive heart failure
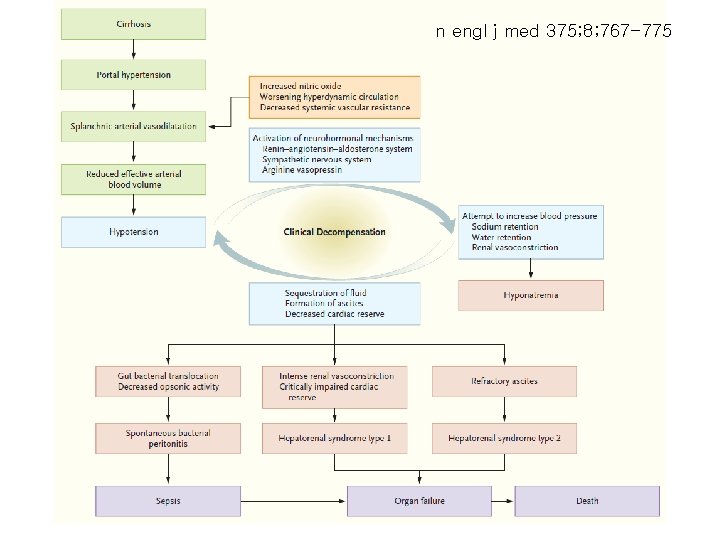
n engl j med 375; 8; 767 -775
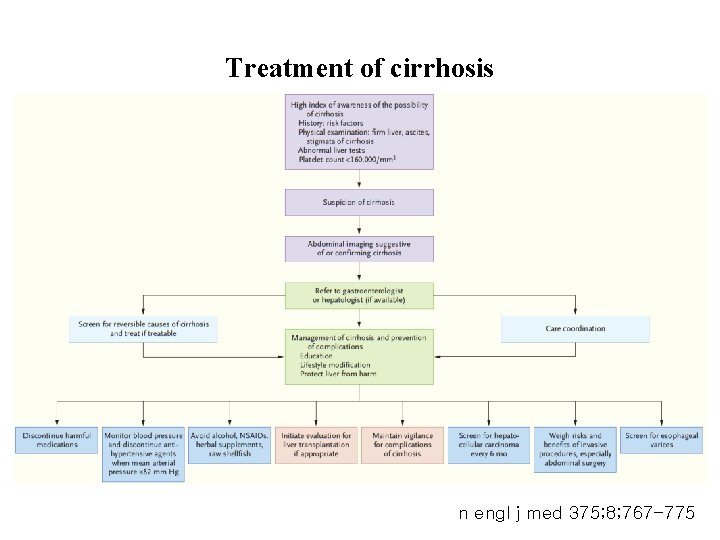
Treatment of cirrhosis n engl j med 375; 8; 767 -775

Complications of Cirrhosis
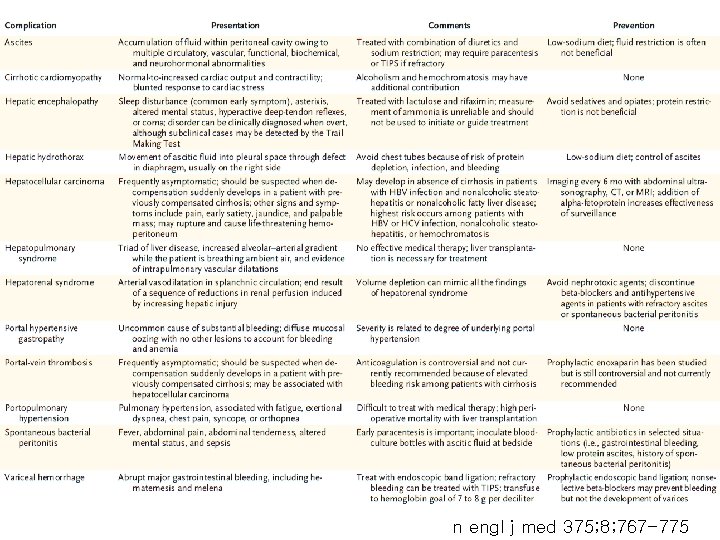

n engl j med 375; 8; 767 -775

Alcoholic cirrhosis • Excessive chronic alcohol use • Alcoholic fatty liver, hepatitis, cirrhosis. • 동반시 liver damage 증가 : hepatitis C, hemochromatosis, fatty liver disease (obesity) • Chronic alcohol use can produce fibrosis (동반된 inflammation 이나 necrosis 없이). • Fibrosis : centrilobular, pericellular, periportal 모두 가능함 • Fibrosis 일정수준 : normal liver architecture 파괴 + liver cells의 regenerative nodules로 • Micronodular. : cessation • mixed micronodular and macronodular cirrhosis
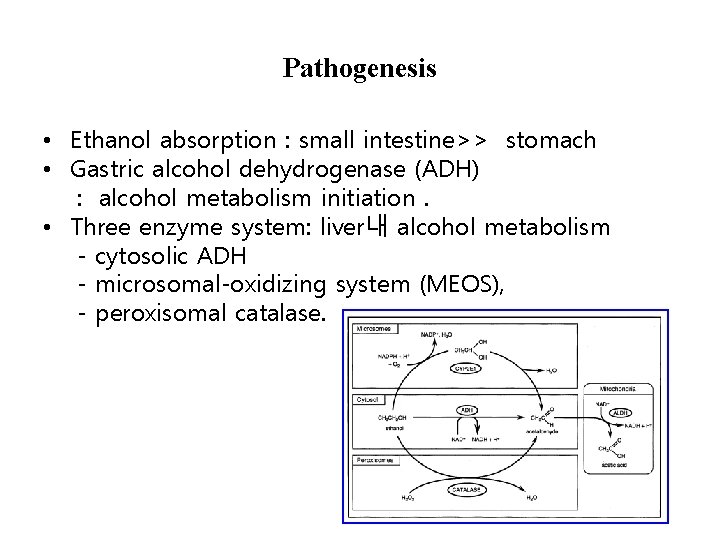
Pathogenesis • Ethanol absorption : small intestine>> stomach • Gastric alcohol dehydrogenase (ADH) : alcohol metabolism initiation. • Three enzyme system: liver내 alcohol metabolism - cytosolic ADH - microsomal-oxidizing system (MEOS), - peroxisomal catalase.
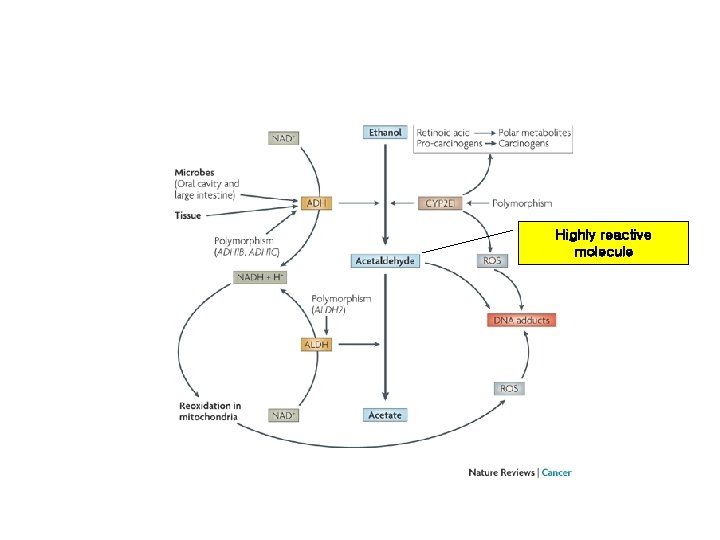
Highly reactive molecule

Effect of ethanol • Ethanol 섭취: 세포 내 triglycerides 증가시킴 (fatty acid uptake 증가, fatty acid oxidation 과 lipoprotein secretion 감소) • Oxidative damage to hepatocyte membranes by formation of reactive oxygen species; - Acetaldehyde : highly reactive molecule protein-acetaldehyde adducts형성. 특정 enzyme activities방해
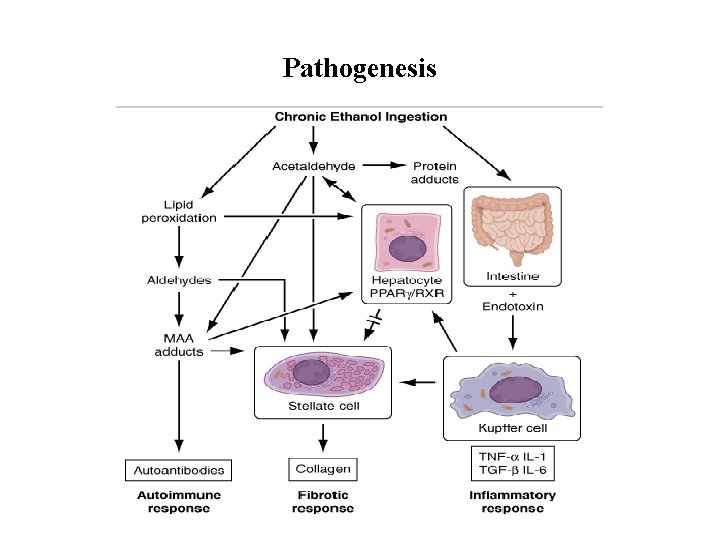
Pathogenesis

• Acetaldehyde-mediated hepatocyte damage + certain reactive oxygen species Kupffer cell activation (profibrogenic cytokine 생산) stellate cell activation Production of excess collagen and ECM Connective tissue 가 periportal and pericentral zones 모두에서 regenerative nodule 1. Hepatocyte loss 2. Increased collagen production and deposition 3. Continuing hepatocyte destruction
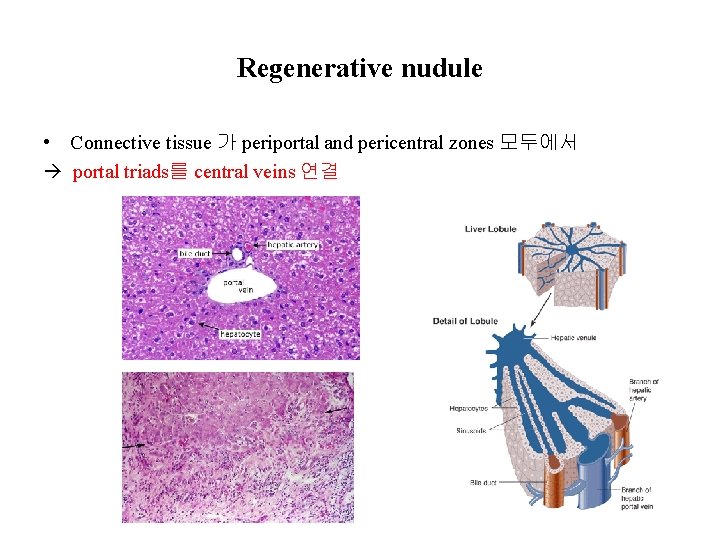
Regenerative nudule • Connective tissue 가 periportal and pericentral zones 모두에서 portal triads를 central veins 연결
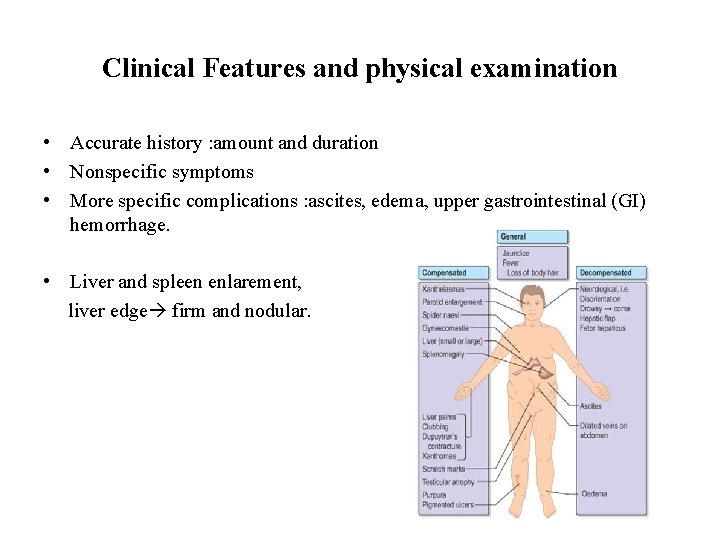
Clinical Features and physical examination • Accurate history : amount and duration • Nonspecific symptoms • More specific complications : ascites, edema, upper gastrointestinal (GI) hemorrhage. • Liver and spleen enlarement, liver edge firm and nodular.

Laboratory • Normal : early compensated alcoholic cirrhosis. • Anemia : chronic GI blood loss, nutritional deficiencies, hypersplenism related to portal hypertension, BM suppression • Hemolytic anemia (with spur cells and acanthocytes) Zieve's syndrome : severe alcoholic hepatitis. • Thrombocytopenia • Serum bilirubin 초기 정상 • Prothrombin times, parenteral vitamin K response 반응안해 • Hyponatremia: ascites 동반시 • Serum aminotransferases (ALT, AST) : > 2: 1 ratio.

Diagnosis • 과거력: alcohol. + other forms of chronic liver disease (e. g. , chronic viral hepatitis, metabolic or autoimmune liver diseases). • Liver biopsy 6개월 정도 금주 잔존 기능, 가역성 판단가능 • LC with complication + alcohol 지속 <50% 5 -year survival.

Treatment • Abstinence • Good nutrition • Glucocorticoids : severe alcoholic hepatitis in the absence of infection Discriminant function (DF) value of >32. improved survival at 28 days • Pentoxifylline: TNF alpha and other proinflammatory cytokines 감소. Glucocorticoid 보다 투여 쉽고 적은side effects. • nutritional therapies 효과 ? • infliximab or etanercept로 TNF –Alpha 감소

Cirrhosis Due to Chronic Viral Hepatitis B or C • HCV exposure 80% develop chronic hepatitis C 20– 30% cirrhosis over 20– 30 years. concomitant alcohol use: only HCV ? HCV is a noncytopathic virus, probably immune-mediated. HCV genotype 3, steatosis is often present. • HBV exposed adult 5% develop chronic hepatitis B 20 -25% cirrhosis. • Chronic hepatitis C 간질환 악화의 특징: Portal-based fibrosis with bridging fibrosis and nodularity cirrhosis. • Mixed micro- and macronodular cirrhosis : Bx

Clinical Features, Diagnosis, Treatment • Symptoms and signs of chronic liver disease. • Diagnosis - Quantitative HCV RNA testing, HCV genotype, - Hepatitis B serologies : HBs. Ag, anti-HBs, HBe. Ag, anti-HBe, and quantitative HBV DNA levels • Treatment : underlying, complication - Specific therapy for treatment of whatever complications occur (esophageal variceal hemorrhage, development of ascites and edema, encephalopathy). - Antiviral therapy
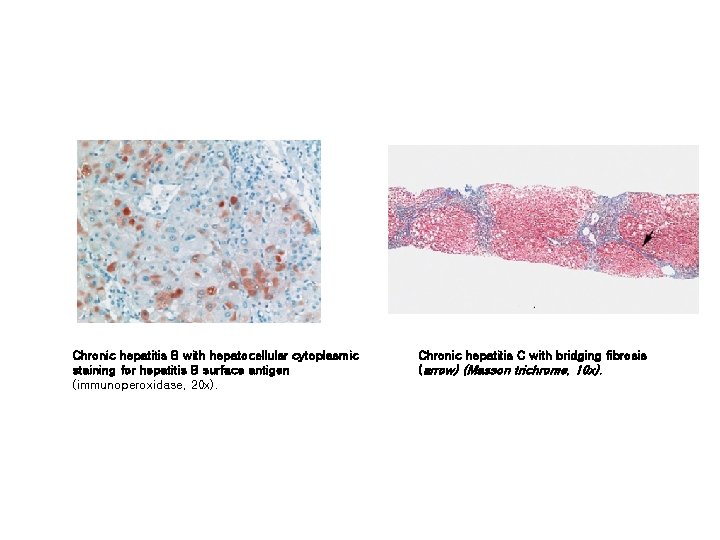
Chronic hepatitis B with hepatocellular cytoplasmic staining for hepatitis B surface antigen (immunoperoxidase, 20 x). Chronic hepatitis C with bridging fibrosis (arrow) (Masson trichrome, 10 x).
Cirrhosis from Autoimmune Hepatitis and Nonalcoholic Fatty Liver Disease • Autoimmune hepatitis (AIH) present with cirrhosis - No benefit from immunosuppressive therapy (glucocorticoids or azathioprine) - Liver biopsy : no significant inflammatory infiltration • Diagnosis : (+) autoimmune markers : ANA or ASMA • Active inflammation + elevated liver enzymes considerable benefit from the use of immunosuppressive therapy. • Nonalcoholic steatohepatitis 에서 cirrhosis 증가. - obesity - cryptogenic cirrhosis

Biliary Cirrhosis - Different from either alcoholic or posthepatitic cirrhosis - Manifestations of end-stage liver disease : same • Cholestatic liver disease 가능요인 - necroinflammatory lesions - congenital or metabolic processes - external bile duct compression • Anatomic sites of abnormal bile retention - Extrahepatic obstruction : surgical or endoscopic biliary tract decompression - Intrahepatic cholestatic processes : interventions ?

Chronic cholestatic syndromes • - Major causes primary biliary cirrhosis (cholangitis) (PBC) autoimmune cholangitis primary sclerosing cholangitis (PSC) idiopathic adulthood ductopenia. • DDx by antibody testing, cholangiographic findings, clinical presentation - 비슷한 histopathologic features : cholate stasis, copper deposition, xanthomatous transformation of hepatocytes, irregular so-called biliary fibrosis.

Primary Biliary Cholangitis (구 Primary Biliary Cirrhosis) - 여성에서 호발 9: 1, 진단 시 평균 50세. - 원인 미상 • 병리 특징 - Portal inflammation, necrosis of cholangiocytes in small and medium-sized bile ducts. • Cholestatic features and biliary cirrhosis : elevated bilirubin level and progressive liver failure. • Antimitochondrial antibodies (AMA) : 약 90%. intermitochondrial membrane proteins을 인식 AMA : not pathogenic, useful markers for diagnosis

Pathology • 가장 초기소견: chronic nonsuppurative destructive cholangitis : necrotizing inflammatory process of the portal tract - Medium and small bile ducts: lymphocyte infiltration - 경도의 fibrosis 와 간혹 bile stasis 관찰 • 진행: inflammatory infiltration은 감소하면서 bile duct 수 감소 더 작은 bile ductules proliferation • Fibrosis 증가하다가 cirrhosis (micronodular or macronodular) • Liver biopsy: stage 확인
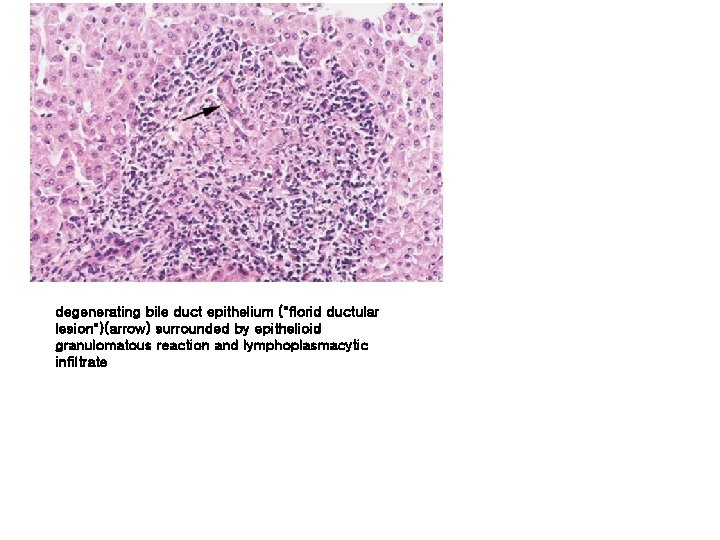
degenerating bile duct epithelium ("florid ductular lesion")(arrow) surrounded by epithelioid granulomatous reaction and lymphoplasmacytic infiltrate

Clinical Features - 대부분 end-stage manifestations 전에 진단 - 무증상 많다 - Pruritus : 진단 시 약 50%, 간헐적이고 저녁 - Jaundice 발생 전 pruritus : severe disease and poor prognosis - Physical examination : jaundice and other complications of chronic liver disease - Unique to PBC : hyperpigmentation, xanthelasma, and xanthomata (altered cholesterol metabolism) - Hyperpigmentation : 몸통이나 각질부. - Bone pain : osteopenia or osteoporosis

Laboratory Findings - cholestatic liver enzyme 상승 : gamma-glutamyl transpeptidase, ALP - Ig. M 상승 전형. - Hyperbilirubinemia : cirrhosis 진행 후. - Liver biopsy - PBC 환자 10%에서 AIH 특성 : "overlap" syndrome. PBC환자처럼 치료 받다가 cirrhosis 진행 가능

Diagnosis • AMA (titer 1: 40이상) 90% • Cholestatic liver enzymes 상승 • Liver biopsy 합당한 소견


Treatment • Obeticholic acid : UDCA와 구조적으로 비슷하나 훨씬 저용량 selective farnesoid X receptor (FXR) agonist중의 하나 Bile acid chenodeoxycholic acid: endogenous FXR ligand서 유래하며 FXR 활성화하는데 chenodeoxycholic acid 100배 Pruritus 흔한 부작용 • FXR: 간과 장에 분포하는 bile acid receptor의 다른 이름 chenodeoxycholic acid, 다른 bile acid 등: FXR의 ligand Bile acid 합성을 negative feedback으로 억제하고 Bile acid transporter를 up regulation하여 choleresis (담즙분비) 자극 • LT : decompensated cirrhosis

Treatment • Fatigue, pruritis 증상에 대한 치료 (UDCA 효과 없어) - 피로에 낮잠? - antihistamines, naltrexone, rifampin. - Cholestyramine (UDCA와 병용시 투여시간 4시간 이상 차이 두어야) • Osteopenia and osteoporosis : bisphonate
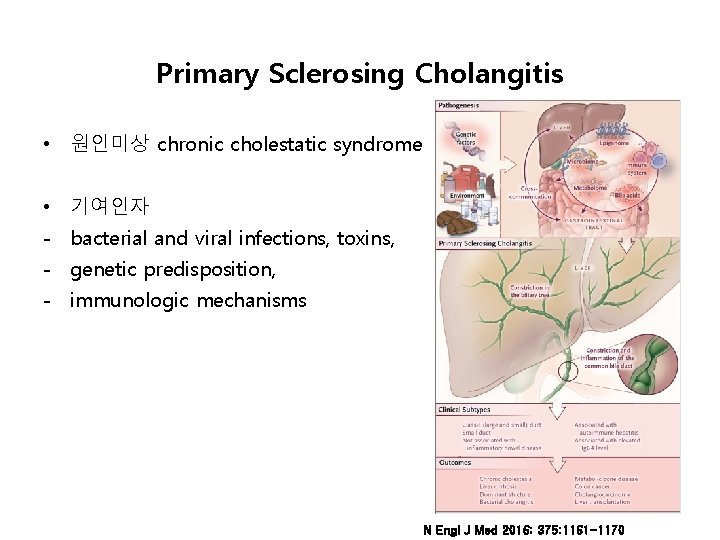
Primary Sclerosing Cholangitis • 원인미상 chronic cholestatic syndrome • 기여인자 - bacterial and viral infections, toxins, - genetic predisposition, - immunologic mechanisms N Engl J Med 2016; 375: 1161 -1170

Primary Sclerosing Cholangitis • 특징: diffuse inflammation fibrosis (전체 biliary tree) chronic cholestasis유발 intra- and extrahepatic biliary tree obliteration biliary cirrhosis, portal HTN, and liver failure. • Pathologic changes : - bile duct proliferation, ductopenia and fibrous cholangitis (pericholangitis). • Liver biopsy 서 periductal fibrosis가 진단에 부분적 도움 biliary tree imaging 중요.
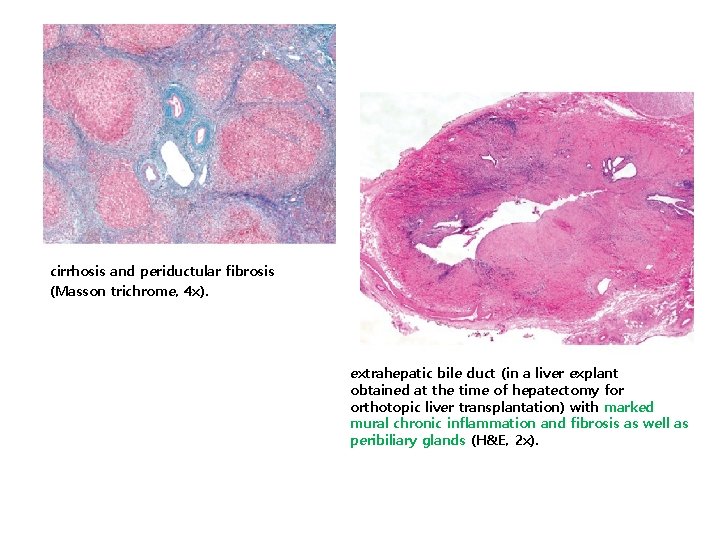
cirrhosis and periductular fibrosis (Masson trichrome, 4 x). extrahepatic bile duct (in a liver explant obtained at the time of hepatectomy for orthotopic liver transplantation) with marked mural chronic inflammation and fibrosis as well as peribiliary glands (H&E, 2 x).

Clinical Features - 진단시 Hepatomegaly 44%, splenomegaly 39% - 증상이 있다면 복통, 가려움증 황달 등 - 일반적인 cholestatic liver disease 특징들: fatigue, pruritus, steatorrhea, fat-soluble vitamins 부족 등 - Pruritus가 cholestasis 관련되어 나타나지만 질병 중등도와 비례 안 해 - Metabolic bone disease가 PBC처럼 가능

Laboratory Findings - ALP 두 배 이상 상승, aminotransferases 가능 - Albumin levels 저하, prothrombin times 증가 - Aminotransferase elevations 5배 이상 증가시 조직검사서 AIH 소견 보이기도. overlap syndrome between PSC and AIH. - Overlap syndrome -autoantibodies (+) 많다 - PSC 단독시는 p-ANCA 외 음성 - P-ANCA(+): 약 65% - Ulcerative colitis (UC) 동반 : 약 50% colonoscopy
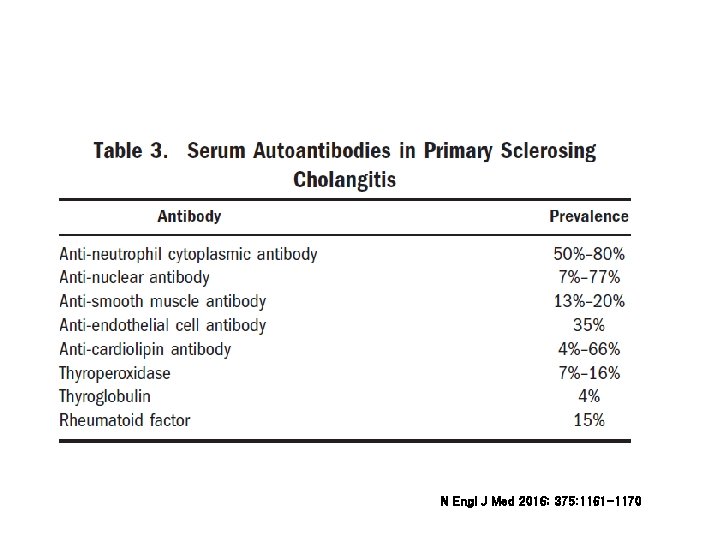
N Engl J Med 2016; 375: 1161 -1170
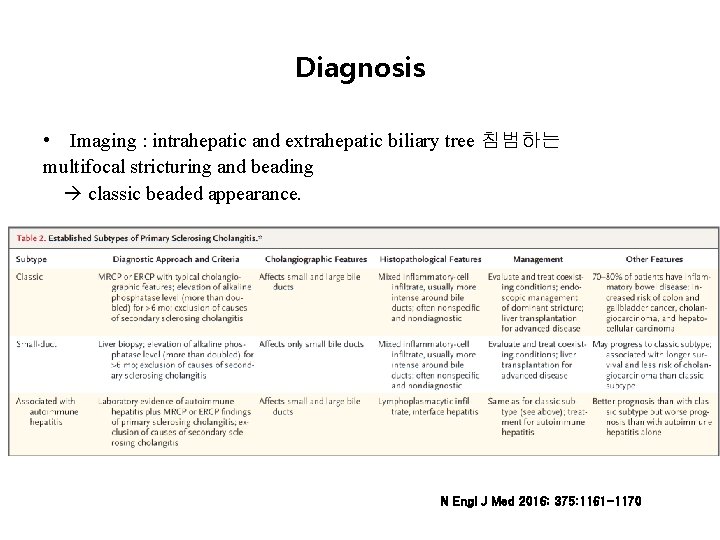
Diagnosis • Imaging : intrahepatic and extrahepatic biliary tree 침범하는 multifocal stricturing and beading classic beaded appearance. N Engl J Med 2016; 375: 1161 -1170
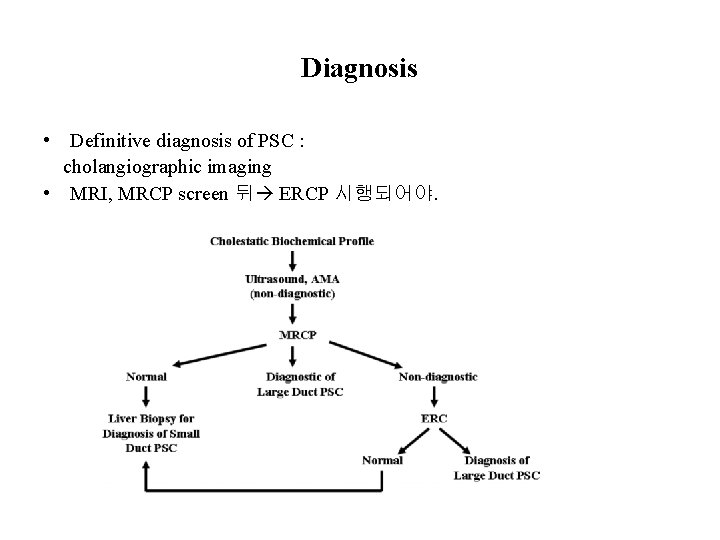
Diagnosis • Definitive diagnosis of PSC : cholangiographic imaging • MRI, MRCP screen 뒤 ERCP 시행되어야.
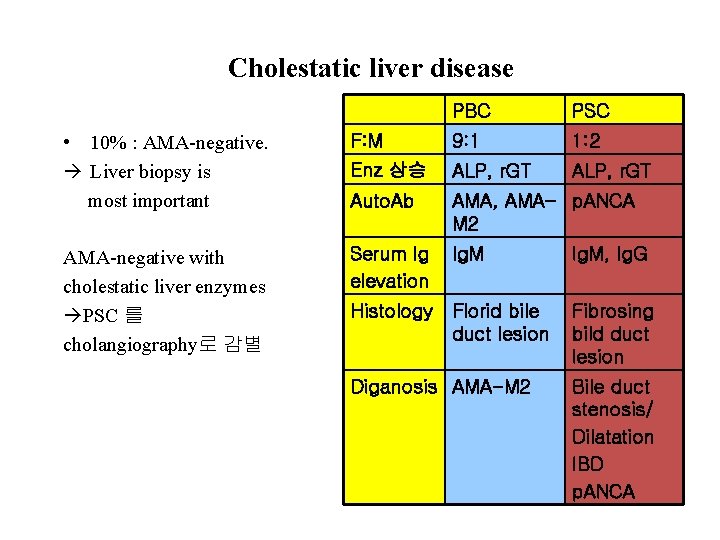
Cholestatic liver disease PBC PSC • 10% : AMA-negative. Liver biopsy is most important F: M 9: 1 1: 2 Enz 상승 ALP, r. GT Auto. Ab AMA, AMA- p. ANCA M 2 AMA-negative with cholestatic liver enzymes PSC 를 cholangiography로 감별 Serum Ig elevation Ig. M, Ig. G Histology Florid bile duct lesion Fibrosing bild duct lesion Diganosis AMA-M 2 Bile duct stenosis/ Dilatation IBD p. ANCA

Treatment and Prognosis • No specific proven treatment • UDCA? • Endoscopic dilatation : dominant strictures 에나 • The gallbladder and cystic duct : 약 15% 에서 침범. • High-grade, diffuse stricturing of the intrahepatic bile ducts : poor prognosis. • 결국 biliary cirrhosis • 결국 liver transplantation가 치료 • Cholangiocarcinoma serious Cx : relative contraindication to liver transplantation. • Pruritus : PBC에서와 같은 치료
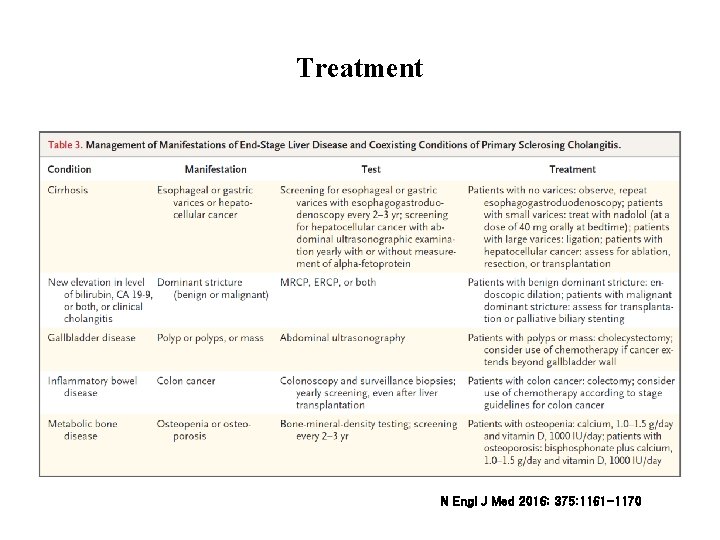
Treatment N Engl J Med 2016; 375: 1161 -1170

Cardiac Cirrhosis • 지속적인 right-sided congestive heart failure chronic liver injury유발. • 매우 드물다 • Etiology and Pathology 장기간 right-sided heart failure로 증가된 venous pressure 가inferior vena cava와 hepatic veins을 통해 liver sinusoids 로 전달됨 • Long-term passive congestion and relative ischemia, centrilobular hepatocytes가 necrotic pericentral fibrosis periphery 로 진행 cirrhosis

Clinical Features • Signs of congestive heart failure • Enlarged firm liver on physical examination. • ALP levels 특징적으로 증가 aminotransferases 정상이거나 다소 증가 AST > ALT많아. • Variceal hemorrhage or encephalopathy.

Diagnosis and Treatment • Clear-cut cardiac disease + elevated ALP + enlarged liver. • Liver biopsy : pattern of fibrosis 가 중요 • 감별진단 1. Budd-Chiari syndrome (BCS) : hepatic vein occlusion으로 extravasation of RBC. 2. Venoocclusive disease : hepatic outflow 영향 - liver내 small vein occlusion - BMT with radiation and chemotherapy • Treatment : underlying cardiac disease.
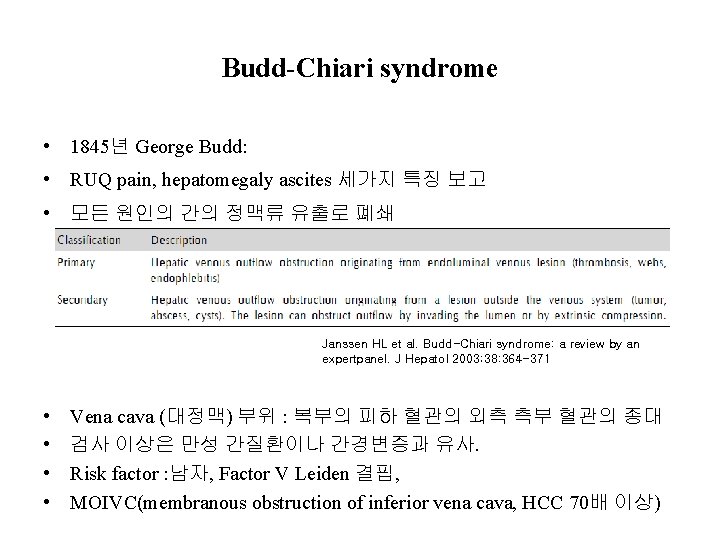

Budd-Chiari syndrome • 1845년 George Budd: • RUQ pain, hepatomegaly ascites 세가지 특징 보고 • 모든 원인의 간의 정맥류 유출로 폐쇄 Janssen HL et al. Budd-Chiari syndrome: a review by an expertpanel. J Hepatol 2003; 38: 364 -371 • • Vena cava (대정맥) 부위 : 복부의 피하 혈관의 외측 측부 혈관의 종대 검사 이상은 만성 간질환이나 간경변증과 유사. Risk factor : 남자, Factor V Leiden 결핍, MOIVC(membranous obstruction of inferior vena cava, HCC 70배 이상)
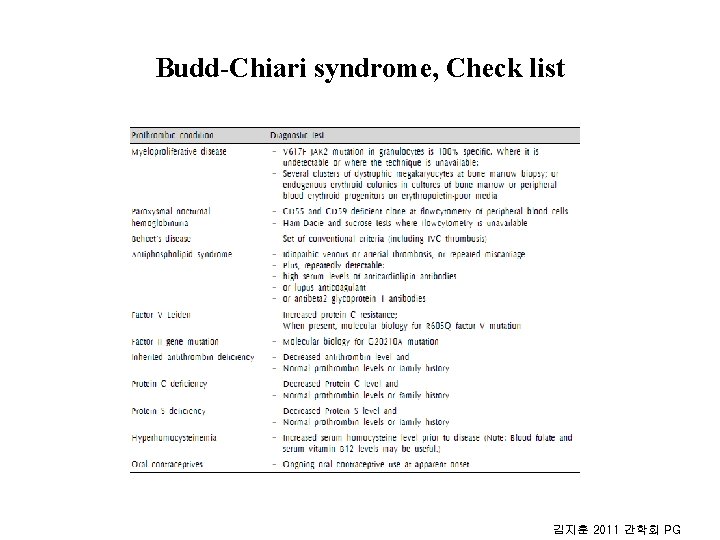
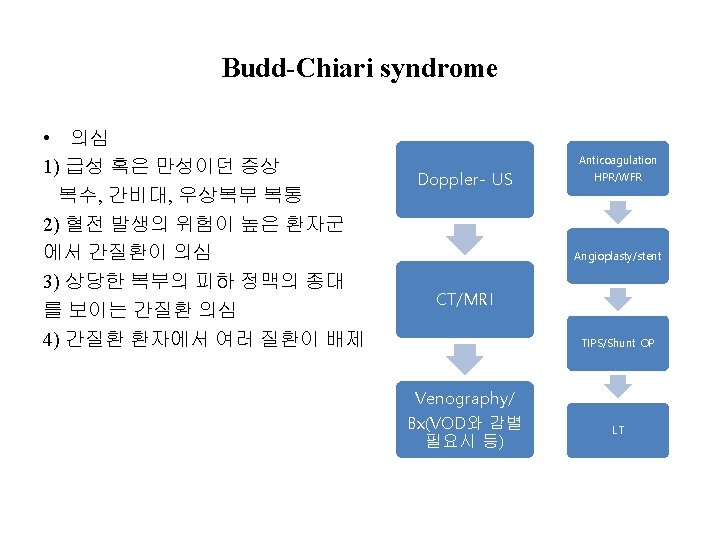

Budd-Chiari syndrome, Check list 김지훈 2011 간학회 PG

Budd-Chiari syndrome treatment 김지훈 2011 간학회 PG
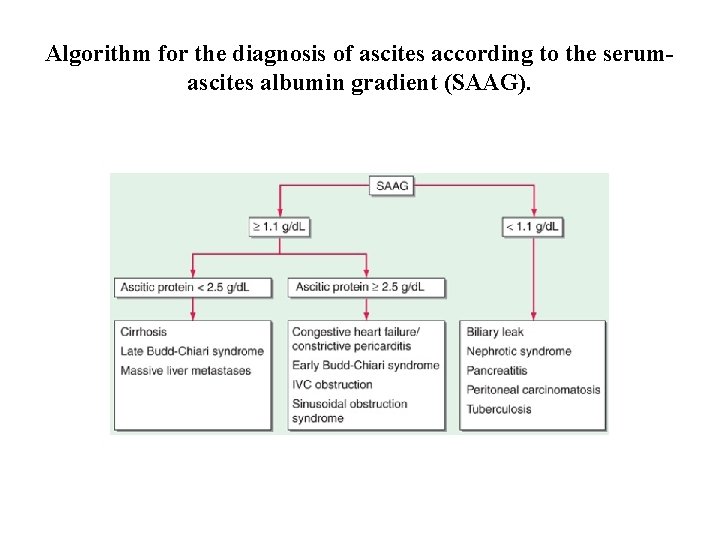
Algorithm for the diagnosis of ascites according to the serumascites albumin gradient (SAAG).
- Slides: 56