Histology of blood cells Jeanne Adiwinata Pawitan Department

Histology of blood cells • Jeanne Adiwinata Pawitan • Department of Histology FMUI

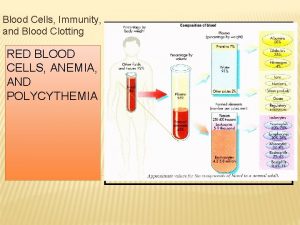
Blood – 5 lt • Specialized connective tissue – circulate – logistical support, communication • Component: ° Blood plasma - serum ° Cells • Erythrocytes (45%) • Leucocytes – (polymorphonuclear, mononuclear) ° Platelets 1%

Leukocytes • Polymorphonuclear (granular→ granulocyte) ° Basophilic leukocytes (basophils) ° Eosinophilic/acidophilic leukocytes (eosinophils) ° Neutrophilic/heterophilic /polymorphonuclear leukocytes (neutrophils, polys) • Mononuclear (agranular→ agranulocyte) ° Monocytes ° Lymphocytes • B lymphocytes • T lymphocytes

Leucocyte granules • Nonspecific (azurophilic) granules– 0. 5μm - all leucocytes • Specific granules – Giemsa/Wright ° Neutrophils • Small specific granules (0. 1 μm– light pink) • Tertiary granules ° Eosinophils – specific granules (oblong: 1 -1. 5 μm >< 1 μm ) - dark pink ° Basophils –specific granules (0. 5 μm-blueblack)-pressed to periphery →rough

Azurophilic granules • = lysosomes contain: ° ° Acid hydrolase Myeloperoxidase Lysozyme (antibacterial agent) Bactericidal permeability increasing (BPI) protein ° Cathepsin G ° Elastase, Nonspecific collagenase → extracellular matrix →tissue damage

Neutrophils • Most numerous → 60 -70 % total leuco • Ø 9 -12 μm (in blood smears) • Nucleus ° multilobes – chromatin threads, age ↑- lobe↑ ° ♀- drumstick/Barr body - condensed, inactive, 2 nd X chromosome • ↑- acute bacterial infection

Neutrophil’s specific granules • Small specific granules: ° Enzymes ° Pharmacological agent antimicrobial function facilitate migration • Tertiary granules-neutrophil chemotactic agent→release: ° Gelatinase-degrades basal lamina - facilitate migration ° Cathepsins ° Glycoproteins – inserted to plasmalemma – facilitate phagocytosis

Neutrophil’s function • Phagocytosis – microorganism → microphage • Kill bacteria by ° Enzymes ° Forming reactive Oxygen compounds → die → (dead leuco, bacteria, tissue fluid) • Synthesize leucotrienes (from arachidonic acid-in their cell membrane) – aid in initiation of inflamation

Phagocytosis ↓ phagosome (intracellular vacuole) → destroyed ingested microorganism ↑ Azurophilic granules (lysosome)

Reactive oxygen compounds • Superoxide - formed in respiratory burst (by NADPH oxidase) • Hydrogen peroxide formed from superoxide (by superoxide dismutase) • Hypochlorous acid (HOCP) formed from hydrogen peroxide and chloride ions (by myeloperoxidase)

• • < 4 % - total leucoØ 10 -14 μm Nucleus – bilobe Plasmalemma rec binds to ° Histamin ° Leucotrienes ° Eosinophil chemotactic factor release by mast cells, baso-, neutro- Eosinophils → Migrate to site of ° Allergic reaction ° Parasitic worm invasion ° Inflammatory reaction

Eosinophil’s specific granules • EM: ° center (=internum) – crystal like –electron dense – contains: • Major basic protrein form pores in • Eosinophilic cationic protein parasites’ pellicle • Eosinophil derived neurotoxin ° Externum – less electron dense- contains: • Histaminase • Peroxidase, & other enzymes

Eosinophil’s function • Kill parasites-by facilitating access of superoxide, hydrogen peroxide via pores in pellicles • Release histaminase & other substances → inactivate initiators of inflamation ° Histamine ° Leucotriene C • Engulf Ag-Ab complex → endosomal compartment → degradation of Ag-Ab complex

Basophils • < 1% total leuco • Ø 8 -10 μm • Nucleus – S shaped – masked by specific granules • Plasmalemma – surface receptors – e. g. Ig E receptors → binds Ig. E (from plasma cells)

Basophil’s specific granules • Specific granules contain: ° Heparin ° Histamine • Vasodilation • Smooth muscle contraction (in the bronchial tree) • Leakiness of blood vessels ° Eosinophil chemotactic factor ° Neutrophil chemotactic factor ° Peroxidase

Basophil’s functions • Ig. E – Ag → ° content of specific granules released ° Phospholipase - phospholipids (in plasmalemma) → arachidonic acids → leukotrienes C 4, D 4, E 4 (=slow reacting substance of anaphilaxis, SRS-A) → • similar effects with histamine, but the action is slower, and more persistent • Activate leuco- →migrate to site of Ag challenge

Lymphocyte • 20 -25% - total leuco • Blood smears ° Round, pleomorphic – conective tissue ° Nucleus • round –slightly indented – occupies most of the cell • acentrically located • dense- heterochromatin>>> ° Cytoplasm – light blue • azurophilic granules = lysosomes • Mitochondria-few, Golgi App- small, RER-few, ribosomes >>>

Lymphocyte Size • Small Ø 8 -10 μm • Medium Ø 12 -15μm less numerous • Large Ø 15 -18μm Type (functional) • B lymphocytes – 15 % - months immuno • T lymphocytes - 80 % - years cytochem • Null cells (surface markers)

Lymphocyte functions • In connective tissue (not in blood) ° Immune system • B lymphocyte – bone marrow • T lymphocyte – thymus (cortex) immunocompetent (maturation) →lymphoid system →mitosis →clone Ø Memory cells – ready for subsequent Ag chalenge Ø Effector cells → respond to Ag

Effector cells • B cells diff→ plasma cells - Ab • T cells – cellular immune system diff → ° Cytotoxic T cells (CTL, T killer cells) – contact – kill • Foreign cells • Virally altered cells ° T suppressor cells →signaling molecules ° T helper cells (cytokines, lymphokines) Suppression/→specific response of other cells in immnune system

Monocyte • 3 -8% -total leuco • 12 -15 μm • Circulation – few days → connective tissue macrophage • Nucleus- large, acentric, kidney shaped ° Chromatin network- coarse – 2 nucleoli →moth eaten/soap buble appearance • Cytoplasm – bluish gray ° Azurophilic granules ° Vacuole-like spaces

Monocyte ME • Cytoplasm ° Organels ° Periphery • • Microtubules Microfilaments Pinocytotic vesicles Filopodia

Monocyte-functions • →macrophage ° Phagocytosis - phagosome – enzymatic digestion, superoxide formation→ destruction • Cells (dead, defunct) • Ag • Foreign particulate matter (bacteria) ° APC – epitope (most Agnic) + class II HLA/MHC ° →foreign body giant cells – large foreign particle ° Cytokines • activate inflamatory response • → proliferation, maturation of other cells

Platelets/thrombocyte/thromboplastids • • • 250, 000 -400, 000/mm 3 blood Life span < 14 days Disk shaped - Ø 2 -4μm Cytoplasmic fragment–megakaryocyte-bone marrow LM ° Hyalomere – periphery - clear ° Granulomere - central – darker • Plasmalemma ° Glycocalyx (15 -20 nm) ° Receptor molecules

Platelets – EM - hyalomere • 10 -15 microtubules (MT)-parallel → a ring – diskoid morphology • Actin, myosin monomers – associated to MT – assembly →contractile apparatus • Tubular system • Surface opening (connecting) – molecule rapid uptake & release from activated platelets • Dense tubular system – sequester Ca? >< platelet stickiness?

Platelets – EM - granulomere • Few organels ° Mitochondria ° Peroxisomes • Glycogen deposits • Enzymes ° Catabolize glycogen ° Consume O 2 ° Generate ATP • Granules (α, δ, λ)

Platelets - granules • α granules – 300 -500 nm –contains ° ° ° Fibrinogen Platelet derived GF Platelet thromboplastin Thrombospondin Coagulation factors • α granules content → facilitate ° Vessel repair ° Platelet aggregation – blood coagulation

Platelets - granules • δ granules (dense bodies) – 250 -300 nm contains ° Ca, ADP, ATP ° Serotonin, histamine ° Pyrophosphatase platelet aggregation & adhesion, blood coagulation • λ granules (lysosomes) – 200 -250 nm – contains ° hydrolytic enzymes →clot resorption

Platelets - functions • Injury → limit hemorrhage ° Platelets → activated ° Tissue factors - plasma born factors – platelet derived factors → blood clot

Normal • Endothelium intact – inhibit platelet aggr. ° Prostacyclins ° NO 2 • Endothelium luminal plasmalemma – inactivate specific coagulation factor ° Thrombomodulin ° Heparin – like molecule Injury • Endothelium ° Stop producing inhibitors ° Von Willebrand factor →platelet activation ° Tissue thromboplastin ° Endothelin→vasoconstr • Endothelial disruption → platelet - collagen → platelet activated → → → blood clot

Platelet - activated • Content of granule – released ° ADP platelet - sticky ° thrombospondin →Platelet adhesion (to damaged vessel wall) →Platelet aggregation o Plug – block hemorrhage o Plasmalemma - platelet factor 3 = phospholipid surface – assembly of coagulation factors esp. thrombin • Arachidonic acid (plasmalemma)→ thromboxane A 2 ° Potent vasoconstrictor ° Platelet activator
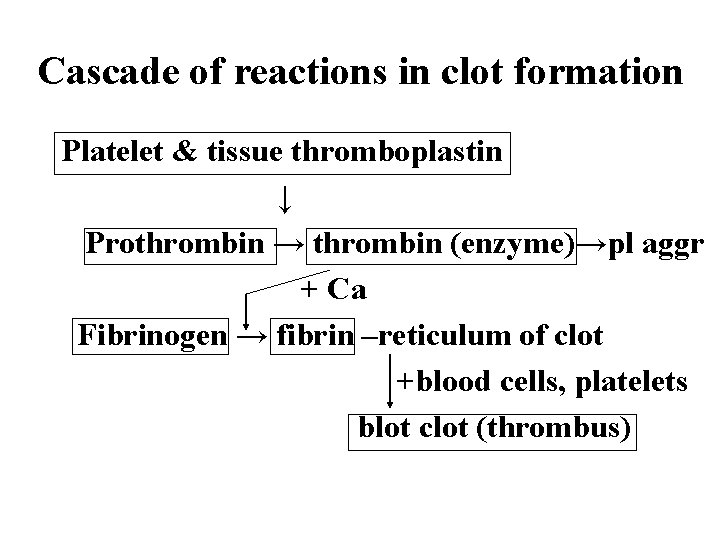
Cascade of reactions in clot formation Platelet & tissue thromboplastin ↓ Prothrombin → thrombin (enzyme)→pl aggr + Ca Fibrinogen → fibrin –reticulum of clot +blood cells, platelets blot clot (thrombus)

Thrombus (blot clot) formation • Erytrhrocytes – facilitate – platelet activation • Neutrophils limit platelet activation • Endothelium & thrombus size • After clot formation ° 1 hour → clot contraction – ½ size → pulling edges → minimize blood lost ° Repair of blood vessel → lysis of thrombus
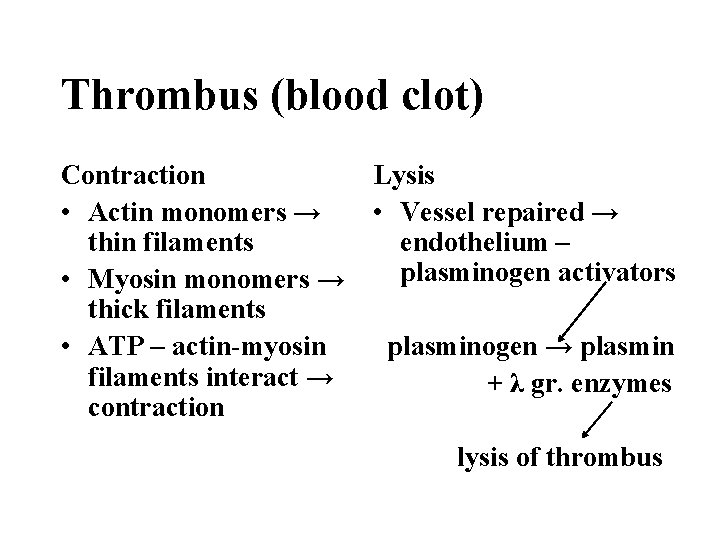
Thrombus (blood clot) Contraction • Actin monomers → thin filaments • Myosin monomers → thick filaments • ATP – actin-myosin filaments interact → contraction Lysis • Vessel repaired → endothelium – plasminogen activators plasminogen → plasmin + λ gr. enzymes lysis of thrombus
- Slides: 34