Hip Pelvis and Thigh Problems Anatomy Evaluation and

Hip, Pelvis and Thigh Problems: Anatomy, Evaluation and Management Kevin de. Weber, MD, FAAFP Director, Sports Medicine Fellowship USUHS Family Medicine (credits to LTC Erik A. Dahl MD for some slides)

Objectives § Review pertinent hip, pelvis and thigh anatomy § Describe clinical presentation of injuries § Review best examination techniques for the hip § Briefly outline treatment for common conditions

Hip Examination § Anatomy § History § Physical Examination § Radiology and Laboratory
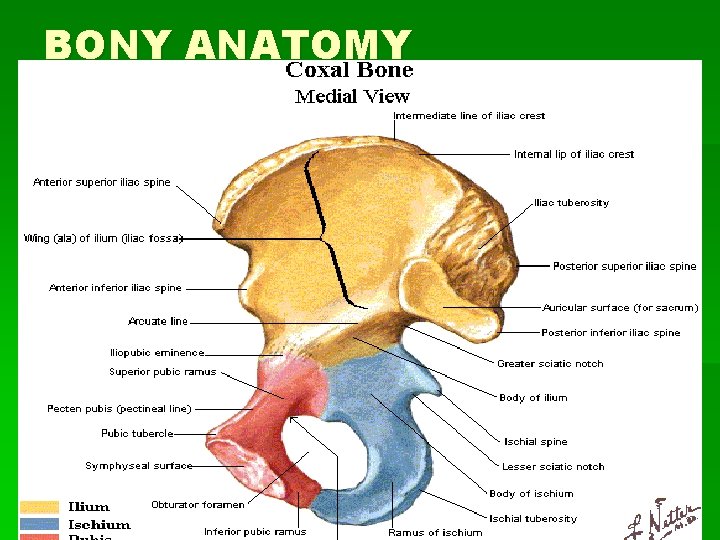
BONY ANATOMY
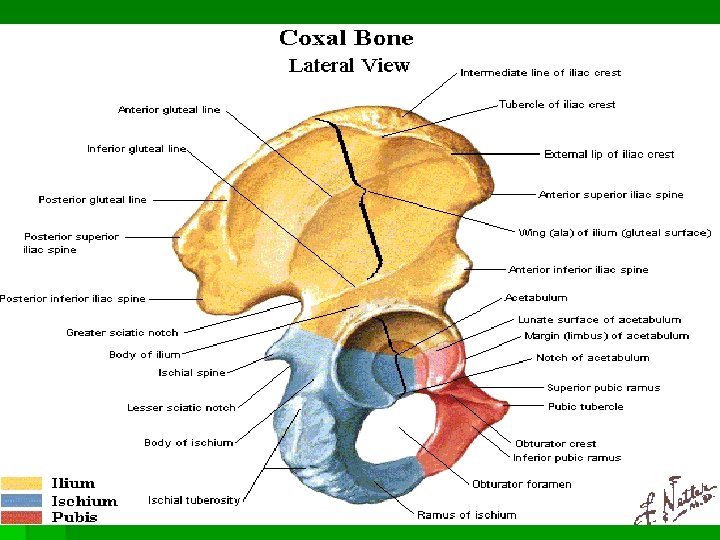
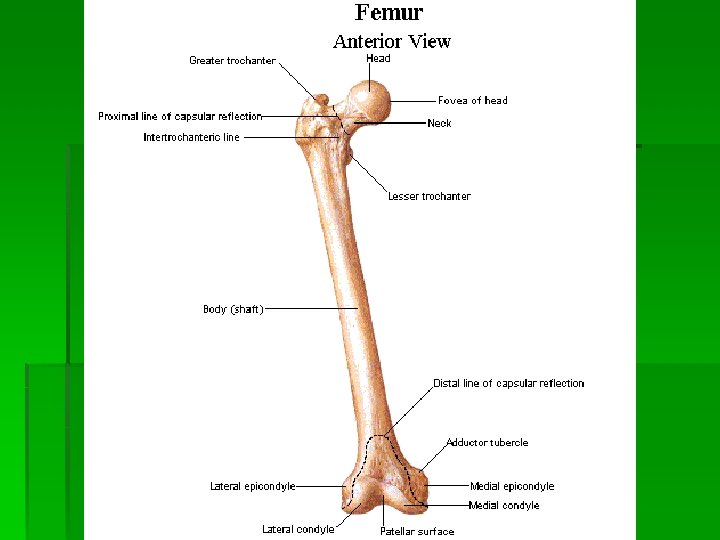
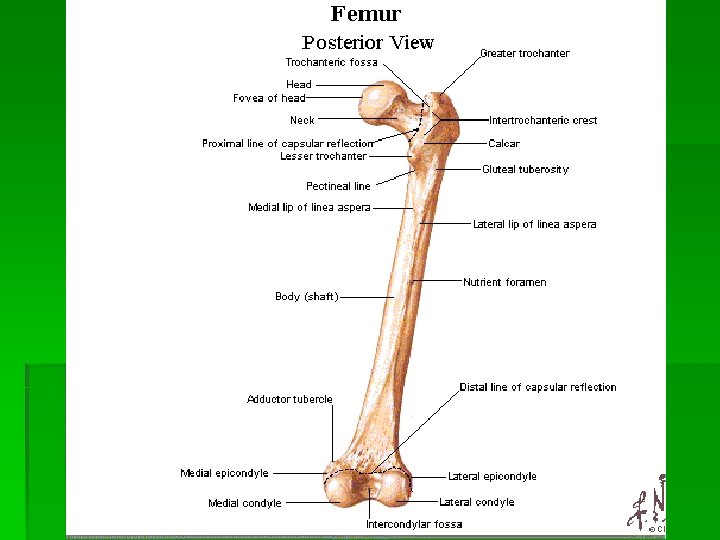
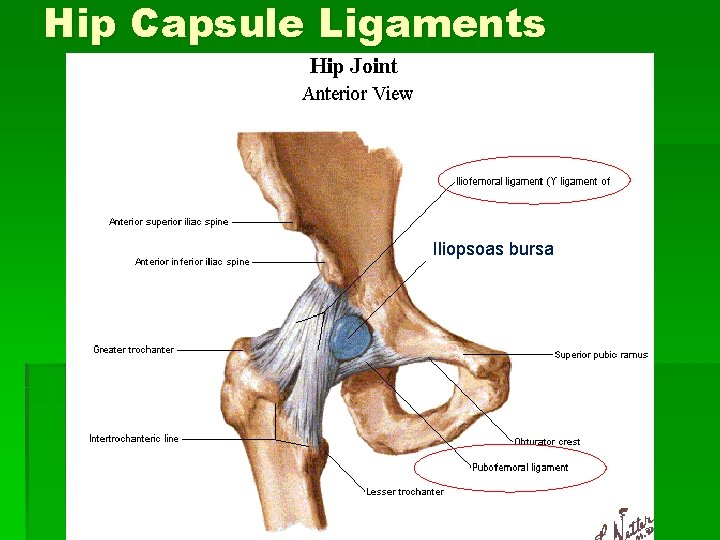
Hip Capsule Ligaments Iliopsoas bursa
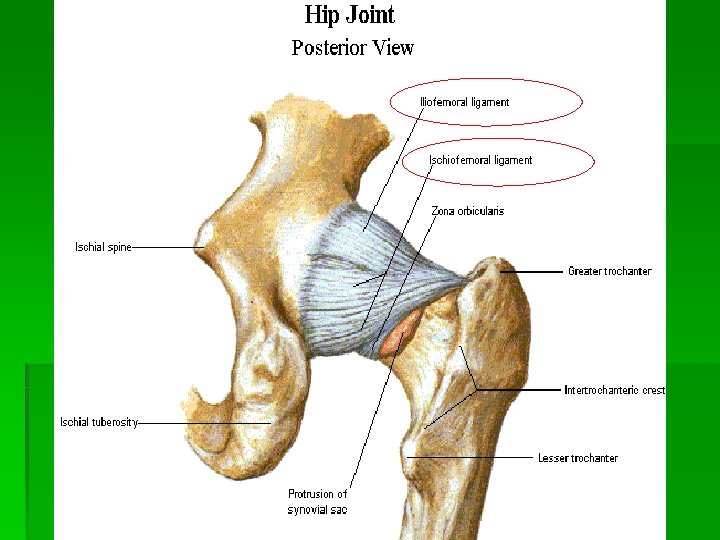
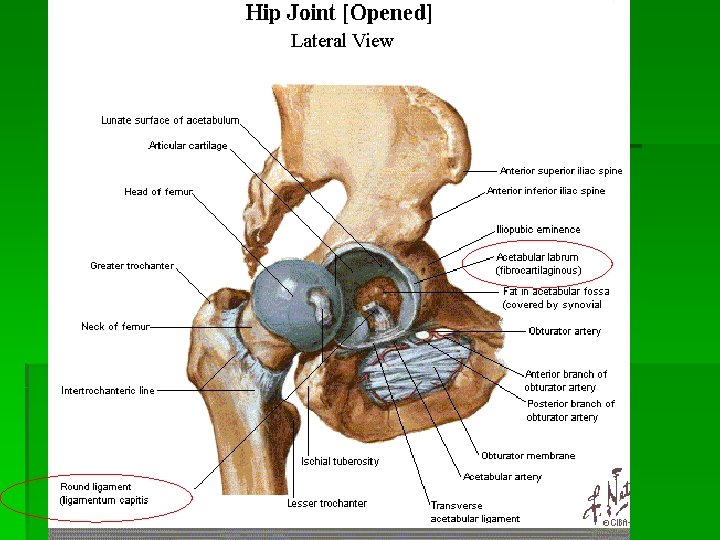
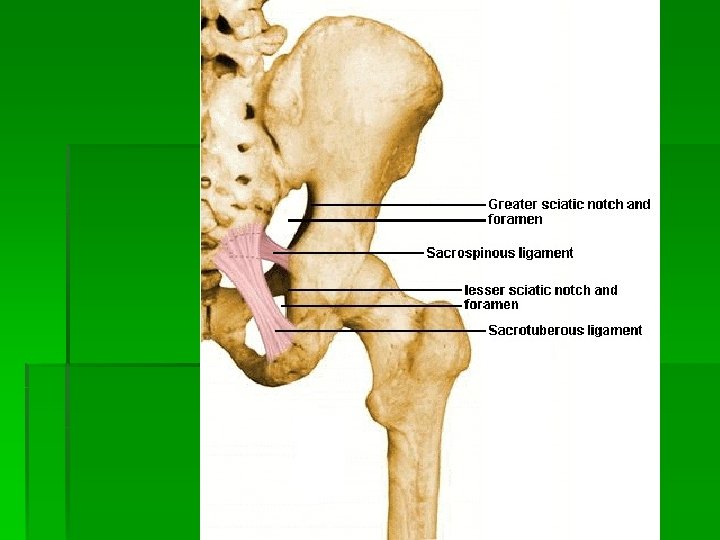
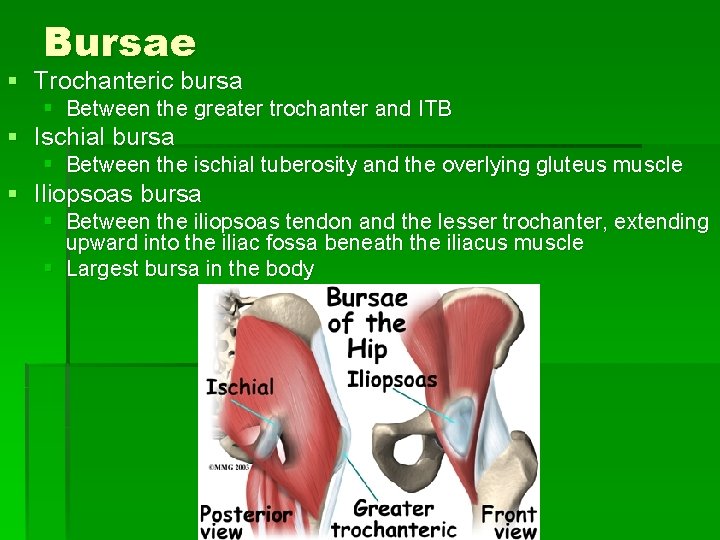
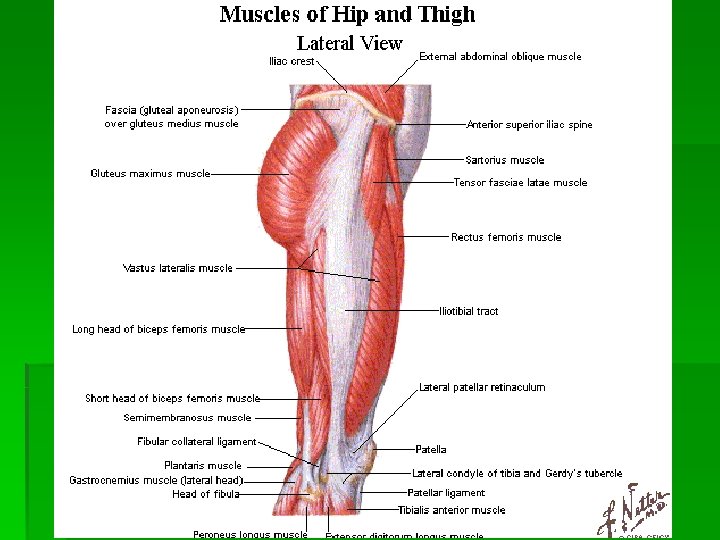
Bursae § Trochanteric bursa § Between the greater trochanter and ITB § Ischial bursa § Between the ischial tuberosity and the overlying gluteus muscle § Iliopsoas bursa § Between the iliopsoas tendon and the lesser trochanter, extending upward into the iliac fossa beneath the iliacus muscle § Largest bursa in the body
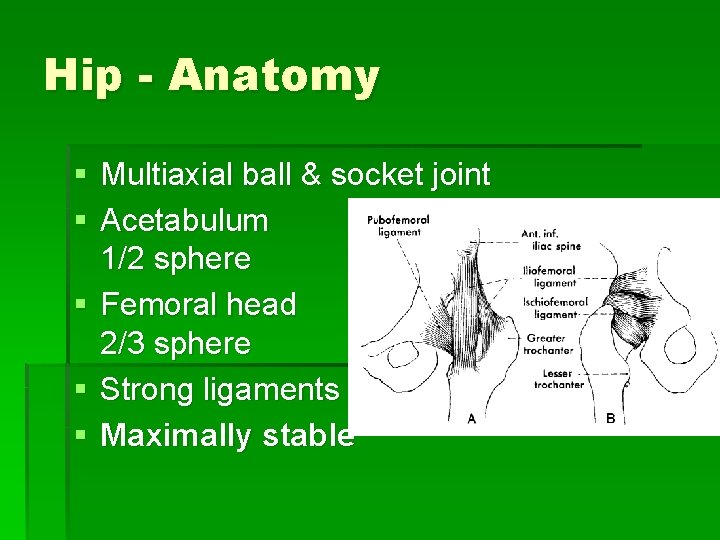
Hip - Anatomy § Multiaxial ball & socket joint § Acetabulum 1/2 sphere § Femoral head 2/3 sphere § Strong ligaments & capsule § Maximally stable
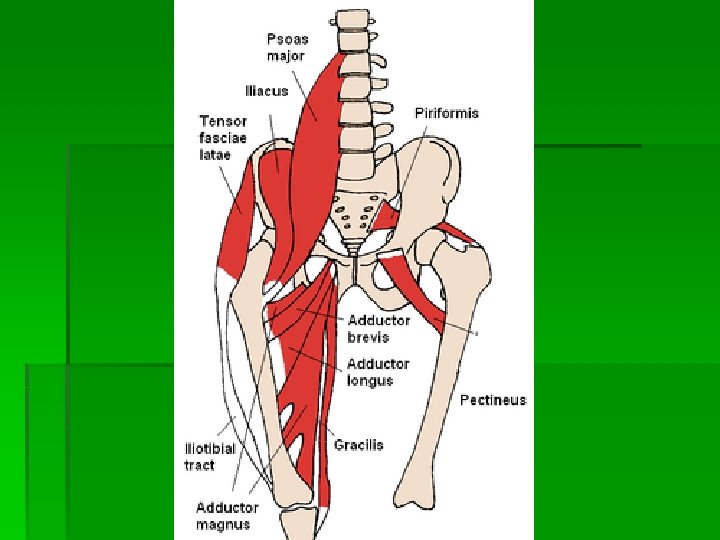
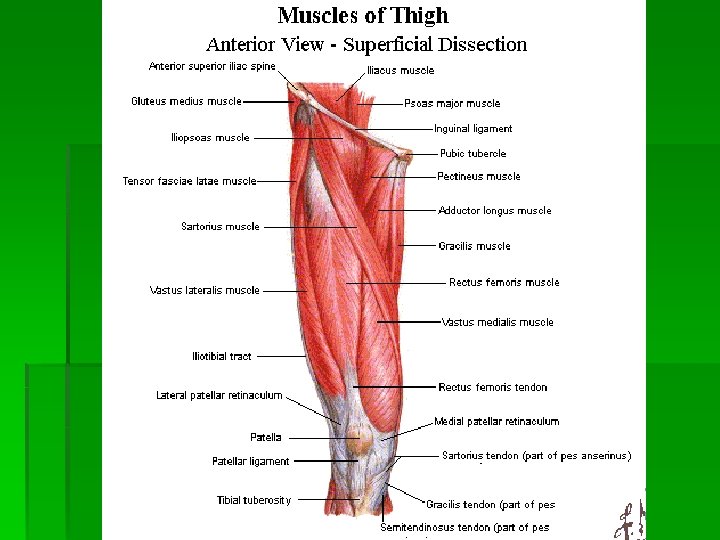

History § Age § infancy: congenital hip dysplasia § 3 -12 year old boys: Legg-Calve-Perthes, SCFE, acute synovitis § middle age & elderly: osteoarthritis § Mechanism of injury § land on outside hip § land on knee § repetitive loading

History § Pain details § location § snapping § progression of symptoms § exacerbating factors § alleviating factors § Weakness § Occupation, Sport

Observation § § Gait Posture Balance Limb position § shortened, adducted, medially rotated § abducted, laterally rotated § shortened, laterally rotated § Leg shortening

Inspection § § § Pelvic unleveling (iliac crest levels) Pelvic rotation (PSIS levels) If asymmetric, measure leg lengths
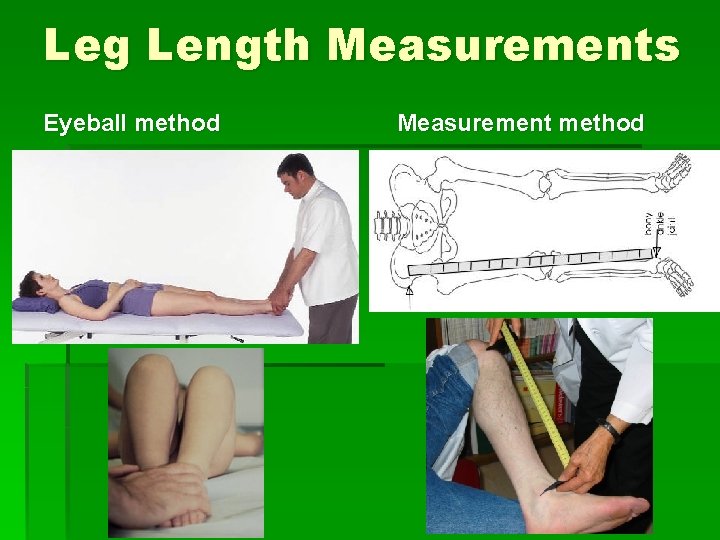
Leg Length Measurements Eyeball method Measurement method
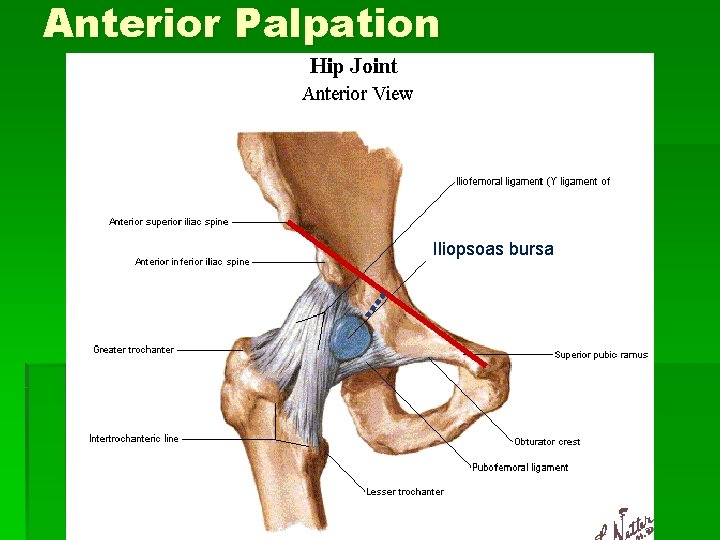
Anterior Palpation Iliopsoas bursa
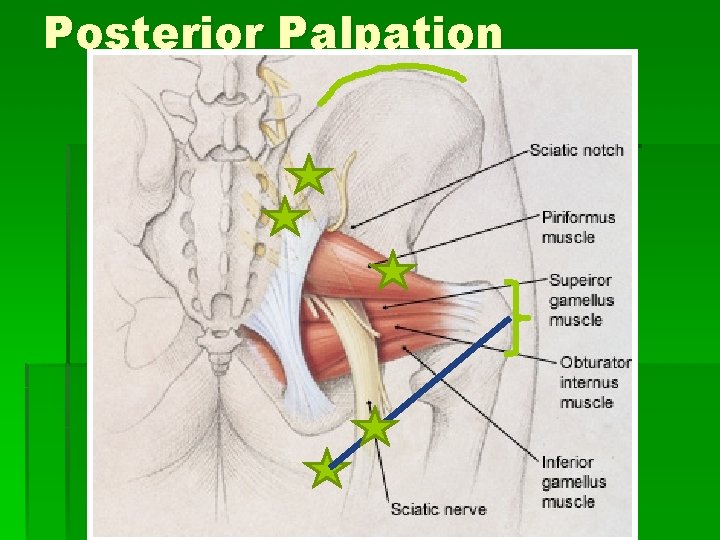
Posterior Palpation
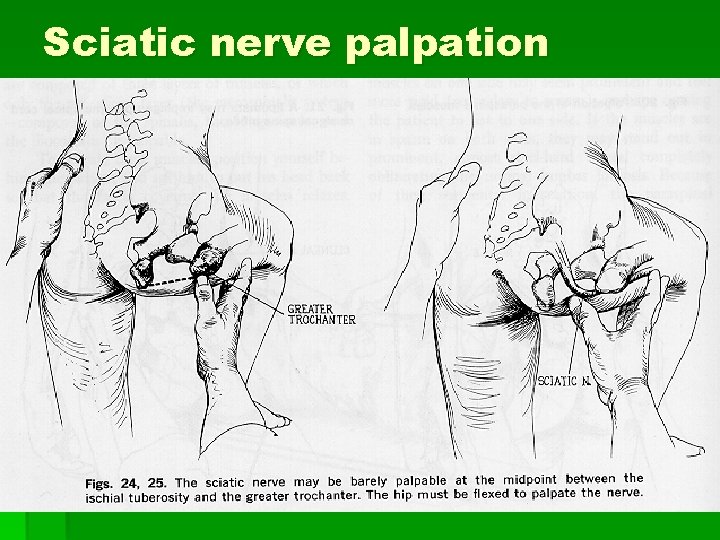
Sciatic nerve palpation

Range of Motion: pearls § Quick screen w/ Log-roll IR/ER: § pain may be from intra-articular fracture, synovitis, or infection § Decreased IR: § First plane to be painful in OA

Range of Motion § Flexion: 110 to 120 degrees § Extension: 10 to 15 degrees

§ Abduction: 30 to 50 degrees § Adduction: 30 degrees
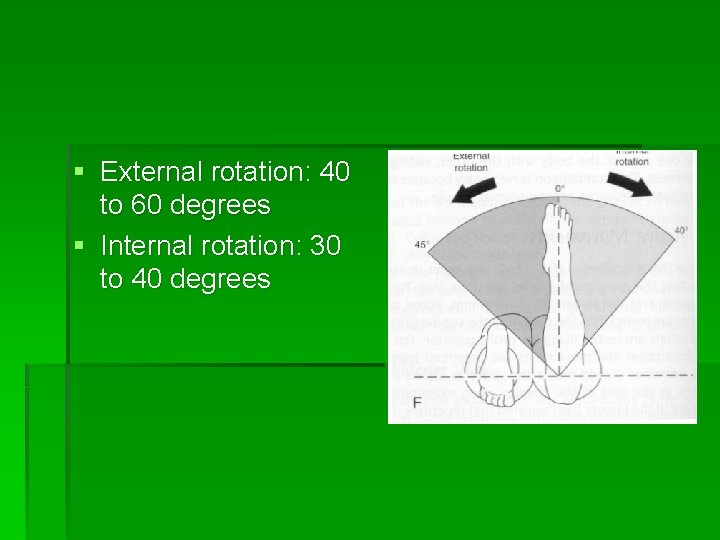
§ External rotation: 40 to 60 degrees § Internal rotation: 30 to 40 degrees
Examination § Strength testing § § isometric eccentric knee extension knee flexion
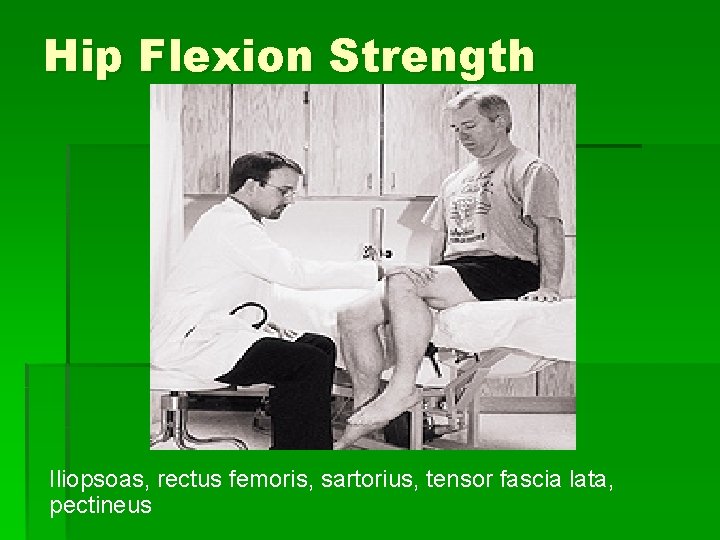
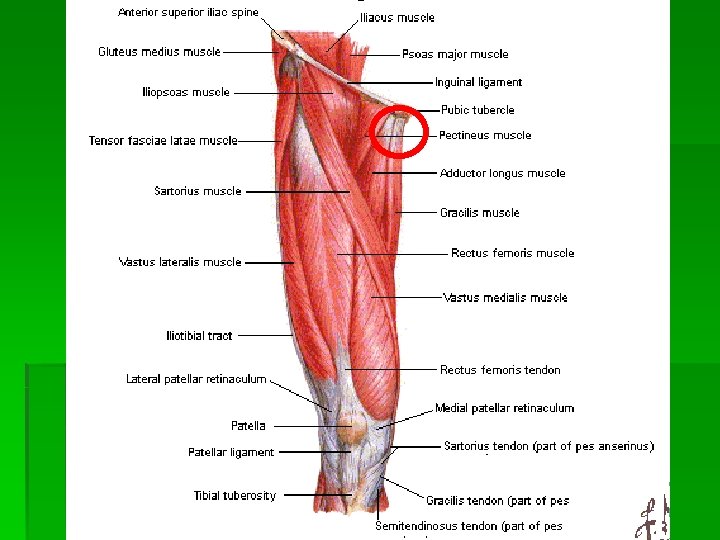
Hip Flexion Strength Iliopsoas, rectus femoris, sartorius, tensor fascia lata, pectineus
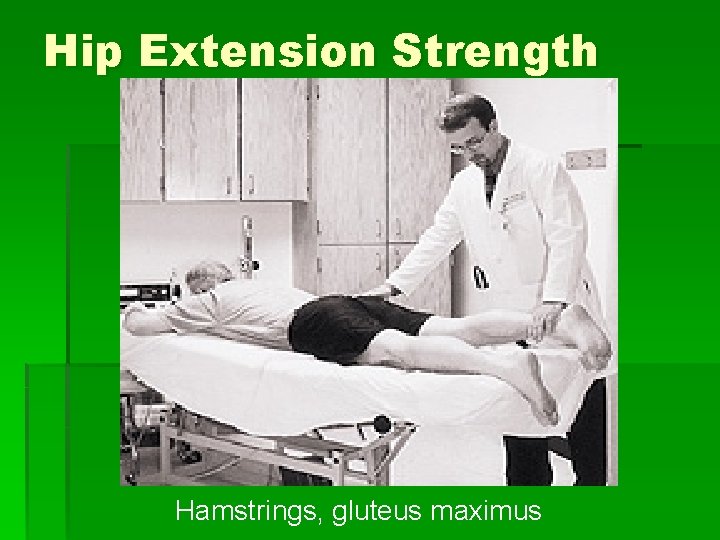
Hip Extension Strength Hamstrings, gluteus maximus
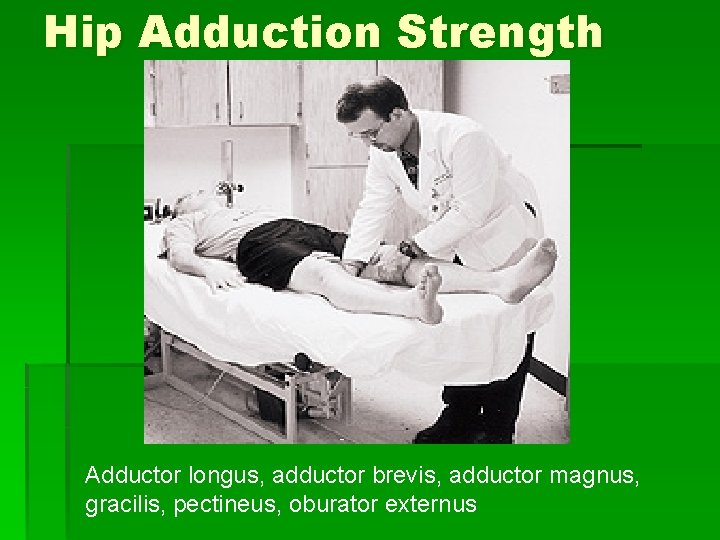
Hip Adduction Strength Adductor longus, adductor brevis, adductor magnus, gracilis, pectineus, oburator externus
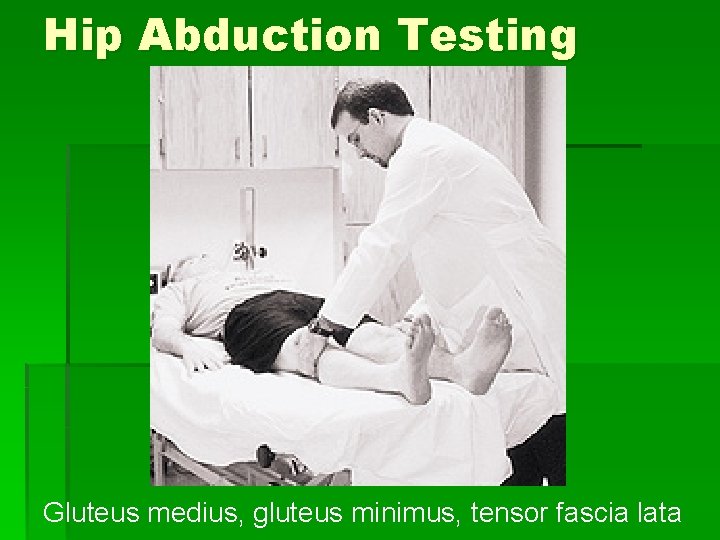
Hip Abduction Testing Gluteus medius, gluteus minimus, tensor fascia lata
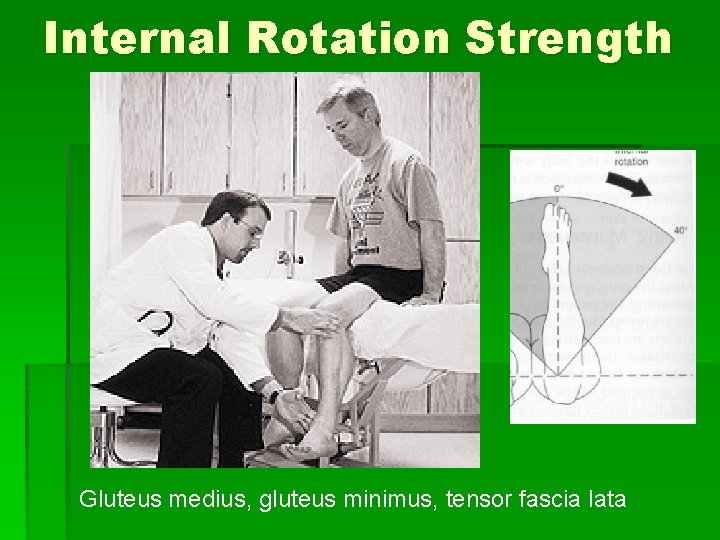
Internal Rotation Strength Gluteus medius, gluteus minimus, tensor fascia lata
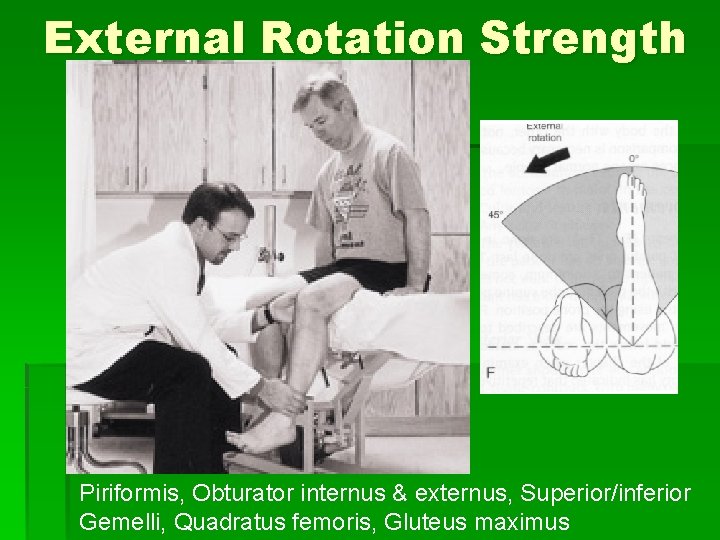
External Rotation Strength Piriformis, Obturator internus & externus, Superior/inferior Gemelli, Quadratus femoris, Gluteus maximus

Abdominal strength

Special Tests § Patrick’s Test (FAb. ER) § hip joint § SI joint
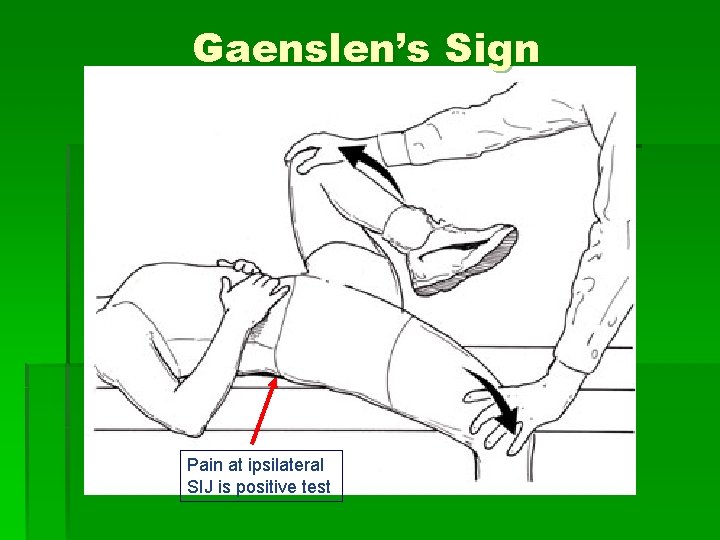
Gaenslen’s Sign Pain at ipsilateral SIJ is positive test

Special Tests § modified Thomas Test § hip flexor and quad flexibility

Special Tests § Ober Test § iliotibial band flexibility

Special Tests § Piriformis Test § Piriformis flexibility or pain

Special Tests § Popliteal Angle § Hamstring flexibilty

Special Tests § Labral Injury § FAd. Ax. L: flexion, Adduction, Axial Load + some IR/ER § pain +/- click

True Hip Pain Misdiagnosis Common § The patients studied by Lesher's team received hip injections for pain. Prior to hip injecton, patients told doctors where they felt pain: § Buttocks: 71% § Thigh: 57% § Groin: 55% § Lower leg: 22% § Foot: 6% § Knee: 2% SOURCE: John Lesher, M. D. 22 nd Annual Meeting of the American Academy of Pain Medicine, San Diego, Feb. 22 -25, 2006. News release, American Academy of Pain Medicine.

Think outside the pelvis! § § § Abdominal exam Obturator and Iliopsoas signs Back exam Pelvic exam in females Hip joint problems can radiate to KNEE
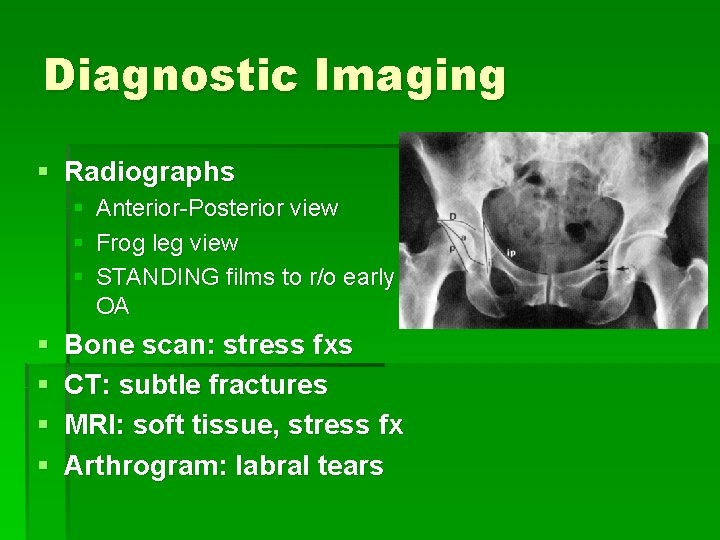
Diagnostic Imaging § Radiographs § Anterior-Posterior view § Frog leg view § STANDING films to r/o early OA § § Bone scan: stress fxs CT: subtle fractures MRI: soft tissue, stress fx Arthrogram: labral tears

Approach to hip problems § Better anatomy knowledge better diagnoses § Differentiate Anterior, Lateral, and Posterior Hip Pain § Develop an appropriate differential based on the location and the exam § Consider AGE in DDx
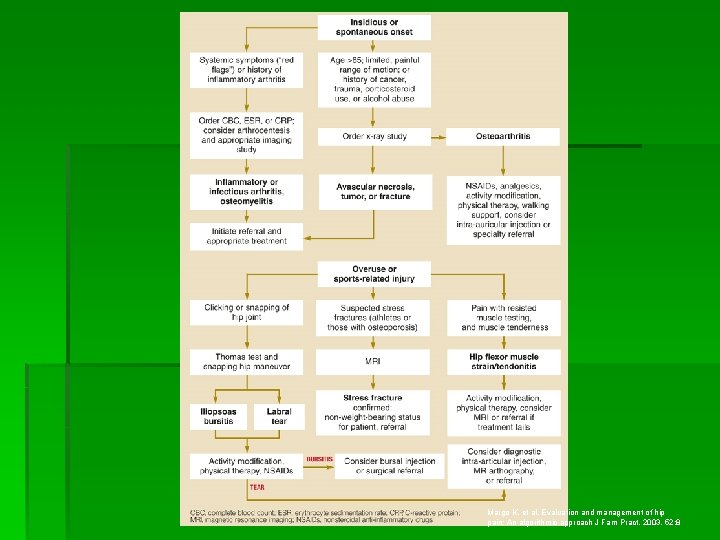
Margo K, et al. Evaluation and management of hip pain: An algorithmic approach J Fam Pract. 2003, 52: 8

Common Hip Problems by Age § Newborn – Congenital dislcation of hip § Age 2 -8 – AVN of hip (Legg-Calve. Perthes), sysnovitis § Age 10 -14 – Slipped Cap Fem Epiphysis § Age 14 -25 – Stress Fracture § Age 20 -40 – Labral Tear § Age >40 – Osteoarthritis
Anterior Hip Pain § Differential Dx § § § Osteoarthritis Muscle strains or tendinopathy Stress fracture (femoral neck, pubis) Sports “hernia” Osteitis pubis Acetabular labral tears Obturator or ilioinguinal nerve entrapment Meralgia paresthetica (may be lateral) Inflammatory arthritis Iliac crest apophysitis AVN of femoral head
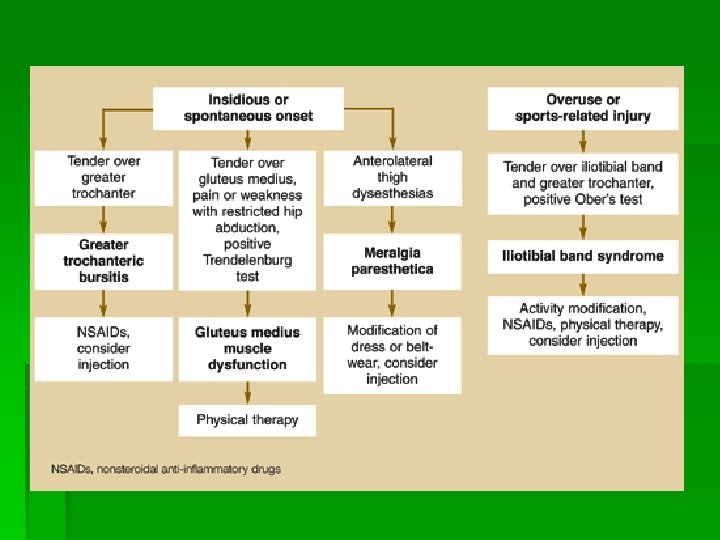
Lateral Hip Pain § Differential Dx § Greater trochanteric bursitis § ITB § Meralgia paresthetica § OA, labral tear, AVN § TFL or gluteus medius strain
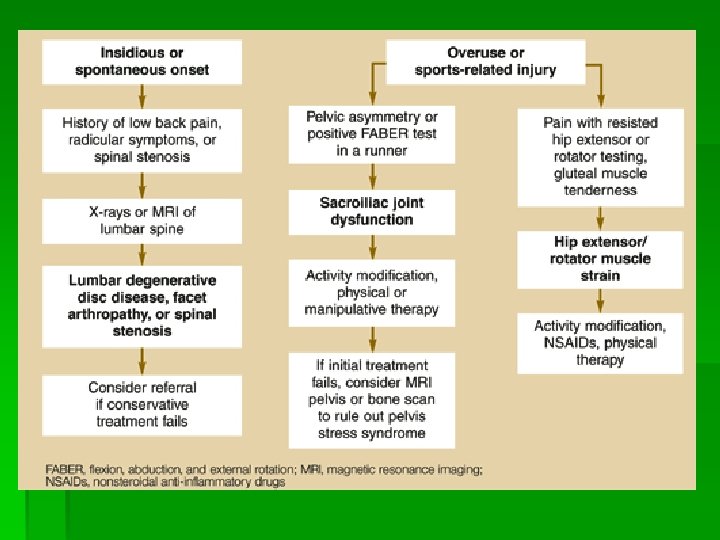
Posterior Hip Pain § Differential Dx § Lumbar spine disease and radicolopathy § Eval for “red flags” § Sacroiliac joint disorders § Hip extensor strain or tendinopathy § Glut max, hamstrings § External rotator strain § Piriformis strain or “syndrome” § Aortoiliac vascular occlusive disease (rare)

Specific Conditions
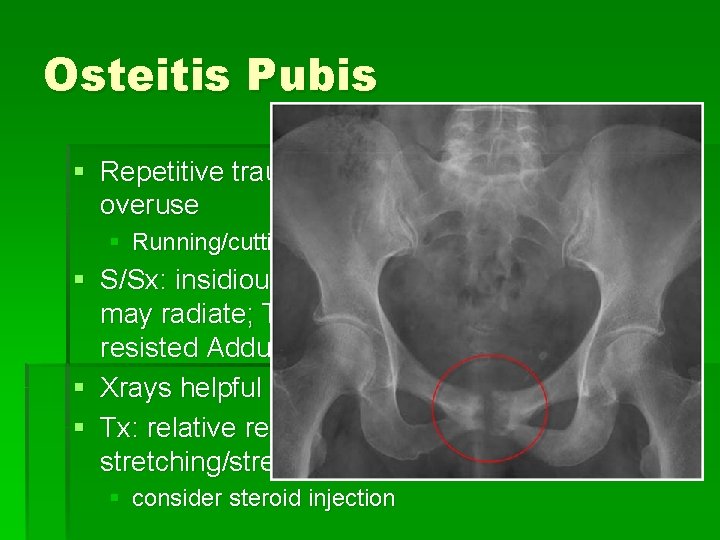
Osteitis Pubis § Repetitive trauma to pubic symphysis due to overuse § Running/cutting, esp soccer, football, basketball § S/Sx: insidious onset dull anterior groin pain; may radiate; TTP over PS; +/- pain w/ resisted Adduction or passive Abduction § Xrays helpful § Tx: relative rest, brief NSAID, cross-tng, stretching/strength rehab, § consider steroid injection
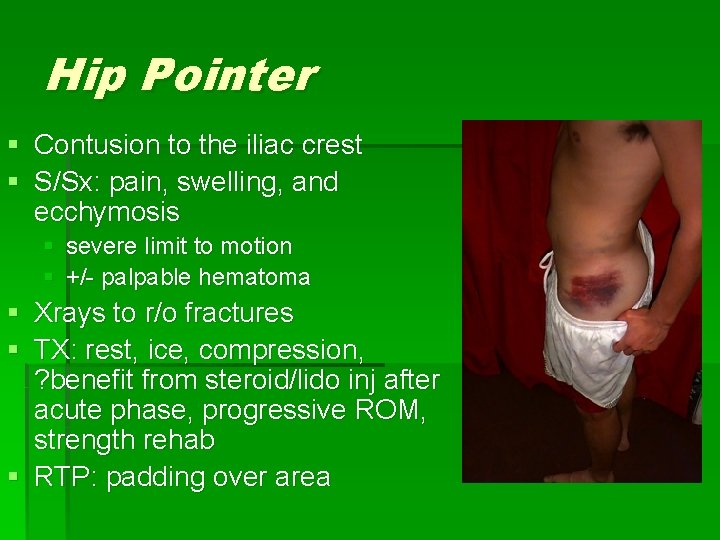
Hip Pointer § Contusion to the iliac crest § S/Sx: pain, swelling, and ecchymosis § severe limit to motion § +/- palpable hematoma § Xrays to r/o fractures § TX: rest, ice, compression, ? benefit from steroid/lido inj after acute phase, progressive ROM, strength rehab § RTP: padding over area
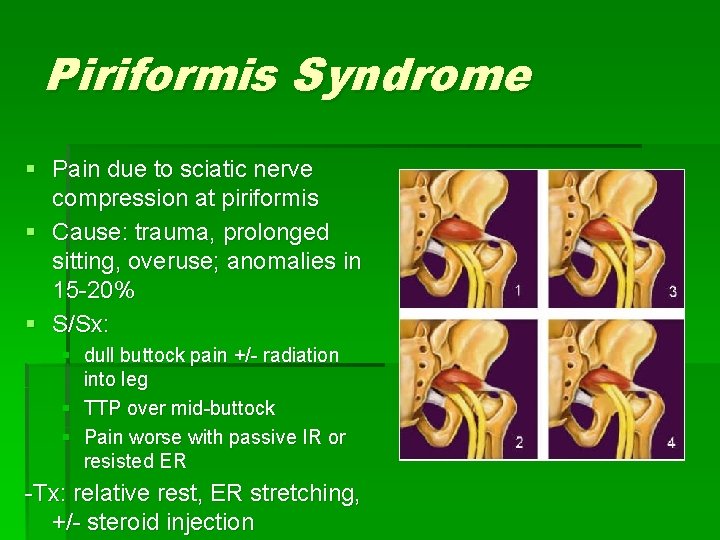
Piriformis Syndrome § Pain due to sciatic nerve compression at piriformis § Cause: trauma, prolonged sitting, overuse; anomalies in 15 -20% § S/Sx: § dull buttock pain +/- radiation into leg § TTP over mid-buttock § Pain worse with passive IR or resisted ER -Tx: relative rest, ER stretching, +/- steroid injection

Trochanteric bursitis § Causes: § friction between IT band, glut medius/minimus/max and greater trochanter; common in running w/ improper biomechanics and overtraining § direct blows § S/Sx: § local pain, tenderness over the greater trochanter § Eval for leg length discrep, adductor/abductor muscle imbalance, hyperpronation § Tx: relative rest, ice, brief NSAID, ITB stretching, +/- steroid injection § Address biomechanical defects above

Ischial bursitis § Cause: excessive friction over ischial tuberosity, or direct blow (hematoma, scarring) § S/Sx: pain with sitting, TTP over ischial tuberosity, pain w/ passive hip flexion and active/resistive hip extension § Xray to r/o fractures in traumatic hx § Tx: § Ice, padding, brief NSAID § Prolonged: steroid injection § Refractory: surgical excision

Iliopsoas bursitis § Cause: overuse of hip flexors § S/Sx: § § anterior hip pain, +/- snap preferred position of hip in flex/ER, TTP to deep palpation anteriorly, pain with passive hip extension § Tx: relative rest, ice, brief NSAID, stretching of iliopsoas, § +/- steroid injection (preferably w/ guidance)
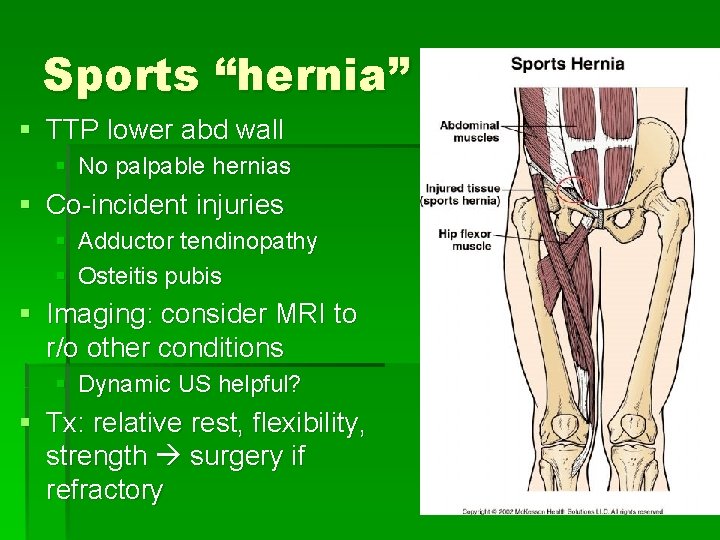
Sports “hernia” § TTP lower abd wall § No palpable hernias § Co-incident injuries § Adductor tendinopathy § Osteitis pubis § Imaging: consider MRI to r/o other conditions § Dynamic US helpful? § Tx: relative rest, flexibility, strength surgery if refractory

Muscle strains § Adductors, gluteals, quads, hamstring tears usually from overstretching during eccentric contraction, esp when muscle fatigued § Risk factors § Early in season § Muscle imbalance, inflexibility, inadequate warmup § S/Sx: localized pain and TTP, +/- swelling or ecchymosis , rarely palpable muscle defect, and decreased ROM § Graded I, III similar to sprains § Xrays to r/o avulsion fxs if near muscle origins; MRI if suspected complete tear § Tx: PRICEMM, Rehab (ROM strength cardio sport-specific tng)
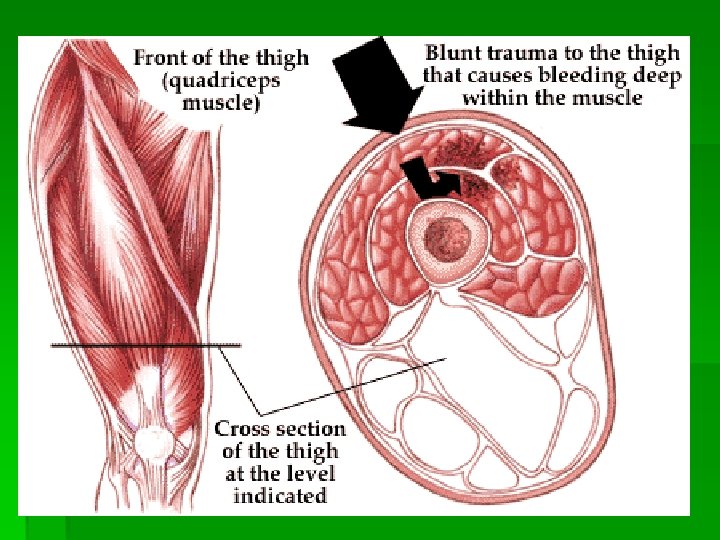

Quadriceps Contusions § Direct blow to muscle causes tissue damage § S/Sx: localized TTP, +/-ecchymosis § § § Grade I: knee flexion >90 Grade II: knee flexion 45 -90 Grade III: knee flexion <45 § Tx: PRICE; avoid NSAID 48 hrs § § § Max knee flexion, wrap in place 24 hrs Crutches, gradual WB, rehab (ROM strength) RTP when FROM, 90%+ strength, activity w/o pain § Complications: § Compartment syndrome (acute) § Myositis ossificans (chronic) § Slowly enlarging mass, redness, increasing pain § Xrays + 3 -4 weeks, BS/US sooner

Stress Fractures § Caused by repetitive overuse stresses § RF’s: training errors, females, inadequate footwear, intrinsic factors § Pelvic, femoral neck, femoral shaft § S/Sx: insidious pain w/ activity; +/- local TTP or pain w/ hop test, +/- decreased ROM § Xrays first, MRI or BS if neg but suspected § Tx § Femoral: immediate NWB, Ortho referral § Tension side surgery § Pelvic/femoral shaft: painless relative rest; graduated WB, strength/stretching rehab, address other RF’s
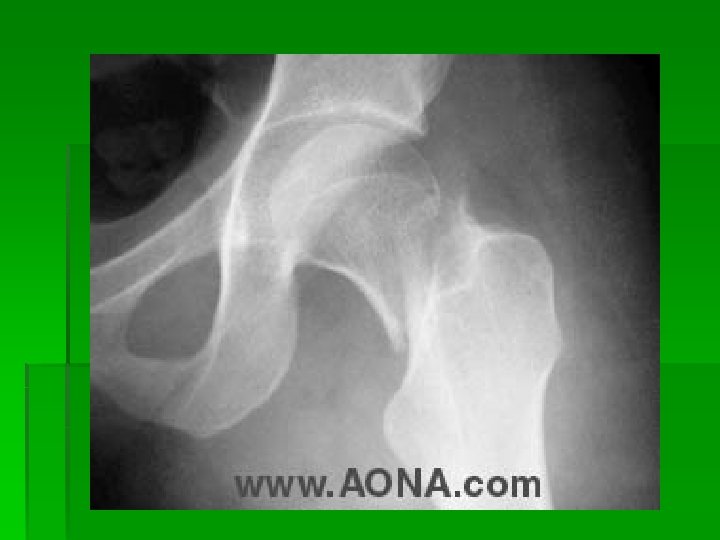
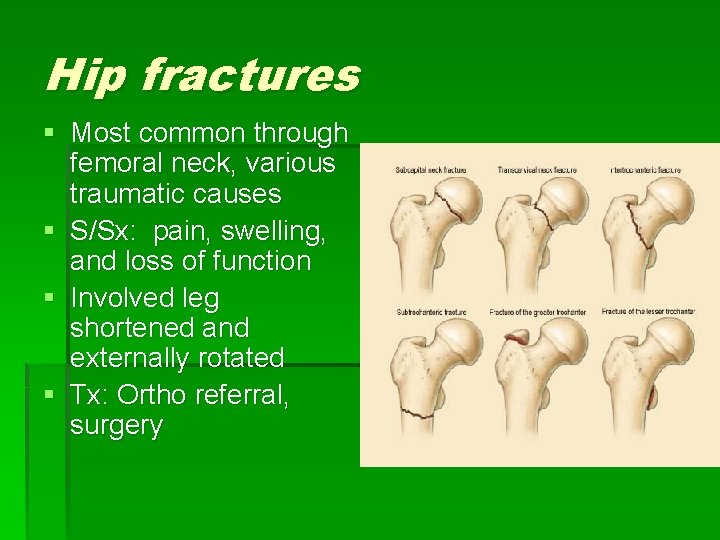
Hip fractures § Most common through femoral neck, various traumatic causes § S/Sx: pain, swelling, and loss of function § Involved leg shortened and externally rotated § Tx: Ortho referral, surgery
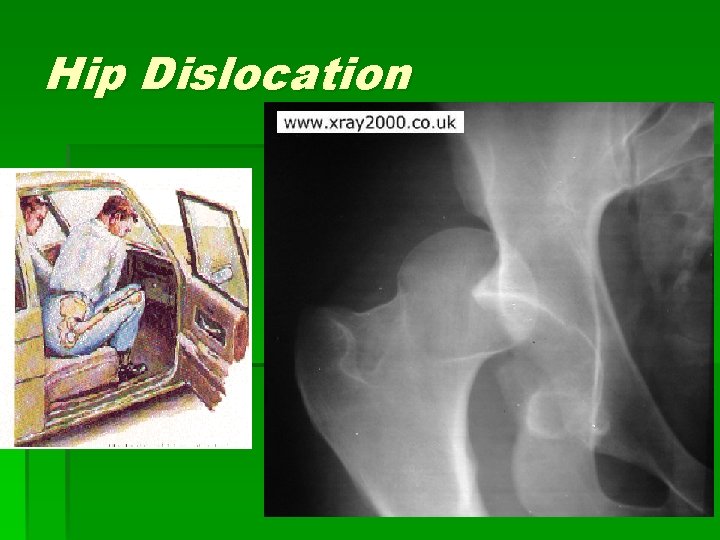
Hip Dislocation § Femoral head usually goes posteriorly § common mechanism: knee to dashboard during traffic collision § S/Sx: extreme pain, obvious deformity, unwilling to move the extremity; position typically flexion, adduction, and internal rotation (FAd. IR) § Tx: emergent reduction in ER under sedation (Ortho STAT!)
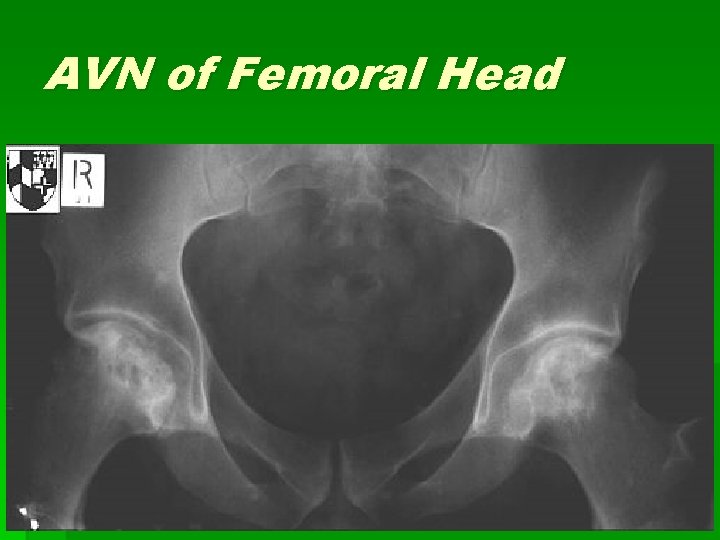
AVN of Femoral Head § Causes: § Trauma: fxs, hip dislocation, surgery § Medical conditions (numerous) § S/Sx: nonspecific hip pain, may radiate to knee; exam may be relatively unremarkable, with decr IR/ER as dz advances § Xrays usually diagnostic >3 mo duration; MRI or BS if normal § Tx: make pt NWB and refer to Ortho § Conservative tx vs hip replacement depending on severity

Conditions in adolescents and children
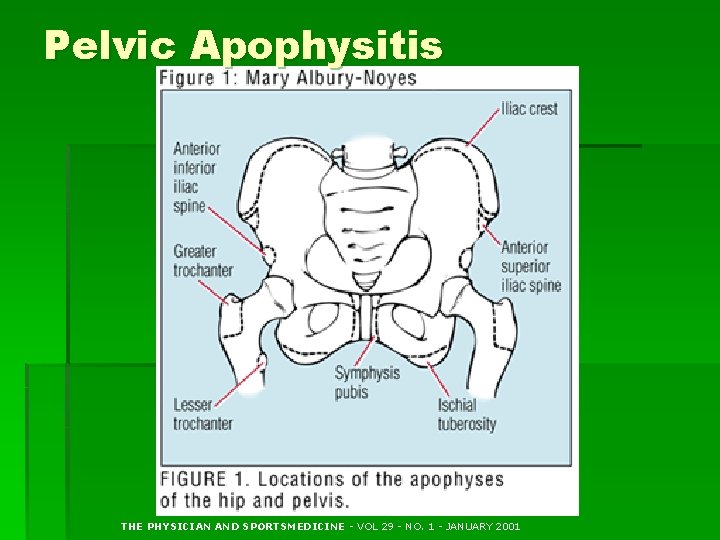
Pelvic Apophysitis THE PHYSICIAN AND SPORTSMEDICINE - VOL 29 - NO. 1 - JANUARY 2001

Pelvic Apophysitis § Cause: overuse at tendinous insertion at apophysis § Iliac crest > ASIS, AIIS, lesser troch, greater troch, ischial tuberosity § S/Sx: localized pain, TTP, pain w/ passive stretch of attached muscle § Xrays to r/o avulsion fxs § Tx: relative rest (rare crutches), ice, brief NSAID? , cross training, strength rehab, flexibility

Pelvic Avulsion Fractures § Caused by violent contraction of the attaching muscle in skeletally immature athlete § Sprint, jump, soccer, gymnast, dancer, football § Ischial tuberosity > AIIS > ASIS > iliac crest, lesser troch, greater troch § S/Sx: sudden pain +/- pop, poor ROM, local pain and TTP +/- muscle bulging away from the attachment § Xrays needed to eval size/displacement § Tx: PRICEMM, progressive rehab § Ortho referral if displacement >2 cm
Slipped Capital Femoral Epiphysis (SCFE) § Slippage of femoral epiphysis laterally off femoral head § Most prevalent ages 9 -15, esp overweight § Bilateral up to 50% § S/Sx: insidious poorly localized hip/groin pain +/- radiation to knee, worse w/ activ § May have limited IR § Xrays usually diagnostic; MRI early if neg but dz suspected § Tx: immed NWB, Ortho referral, surgery
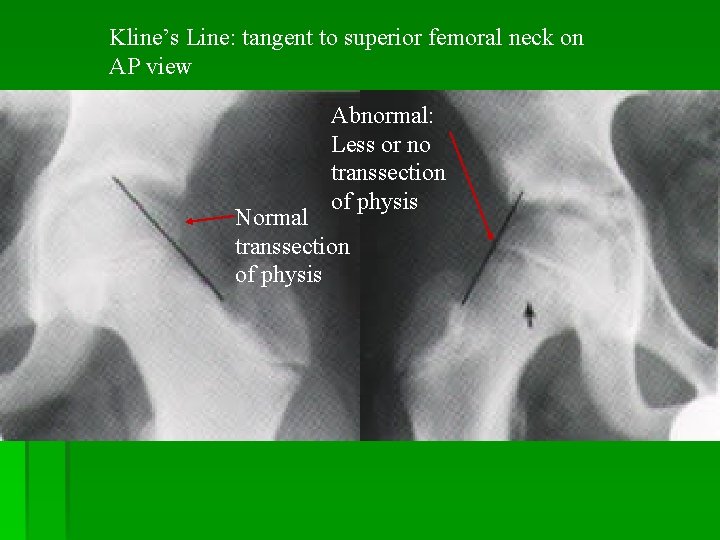
Kline’s Line: tangent to superior femoral neck on AP view Abnormal: Less or no transsection of physis Normal transsection of physis
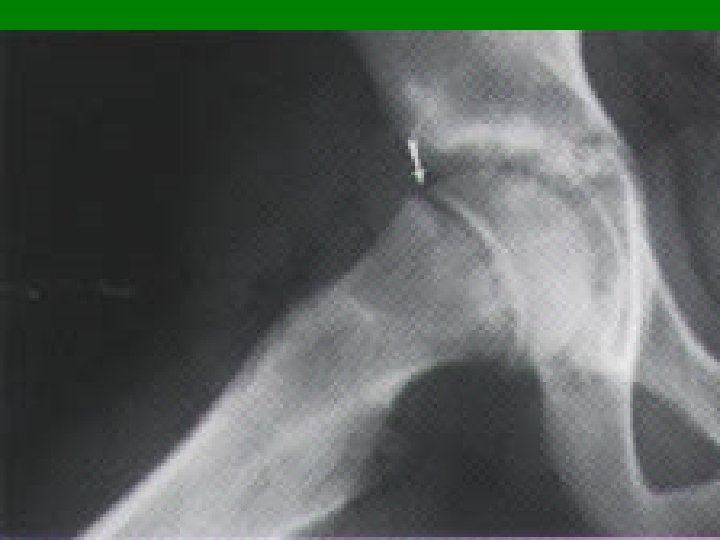
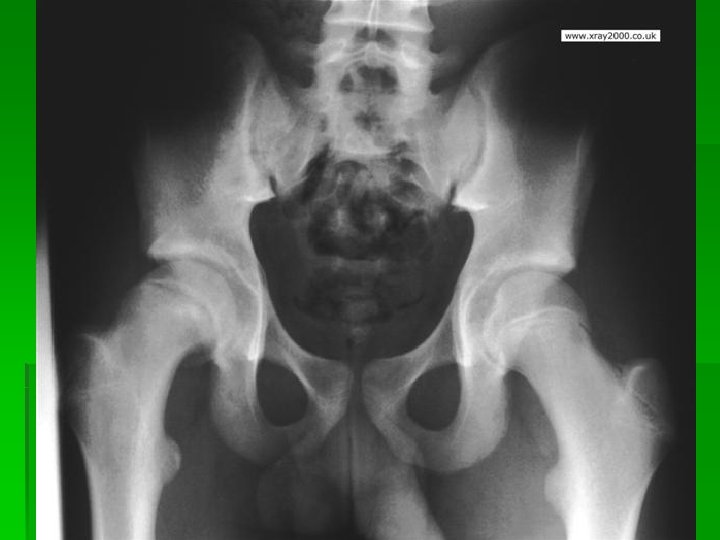

Legg-Calve-Perthes Dz § Avascular necrosis of proximal femoral epiphysis § Most prevalent ages 4 -9, males 4: 1 § Develops slowly § S/Sx: intermittent deep hip pain worse w/ activity, +/- radiating to groin, ant/med thigh, knee; § limping, decreased ROM, and hip flexor tightness may be noted § Xrays usually diagnostic: MRI or BS early if xray neg but AVN suspected § Tx: Ortho referral; crutches, pain meds

Acute Transient (“Toxic”) Synovitis § inflammatory process of hip w/ chronic irritation and excess secretion of synovial fluid within the capsule; ? cause § Most common dx in limping child <10, but it’s a Dx of exclusion; § § § r/o septic arthritis, SCFE, stress fx, etc. Xrays normal; MRI helpful ruling out other causes Labs: normal CBC, CRP § S/Sx: pain w/ walking, low-grade fever § Tx: relative rest, analgesics

Conclusion § Know your anatomy § Know why you’re doing an exam

References § Birrer R. and O’Connor F. Sports Medicine for the Primary Care Physician. Boca Raton: CRC Press, 2004. § Greene W. Essentials of Musculoskeletal Care. Rosemont: American Academy of Orthopaedic Surgeons, 2001. § Hoppenfeld S. Physical Examination of the Spine and Extremities. East Norwalk: Appleton-Century-Crofts, 1976; 5974. § Lillegard W. Evaluation of Knee Injuries. In W Lillegard (ed), Handbook of Sports Medicine. Boston: Butterworth-Heinemann, 1999: 233 -249. § Netter F. Atlas of Human Anatomy. West Caldwell: CIBAGeigy, 1989. § Tandeter H. et al. Acute Knee Injuries: Use of Decision Rules for Selective Radiograph Ordering. American Family Physician. Dec 1999; 60: 2599 -608. (For Radiograph Images)
- Slides: 84