HighGrade T 1 Bladder Cancer A Clinical Quandary

High-Grade T 1 Bladder Cancer: A Clinical Quandary Daniel Canter, M. D. Assistant Professor of Urology Emory University presentation created for:

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity/Mortality of Surgery Risk Stratification
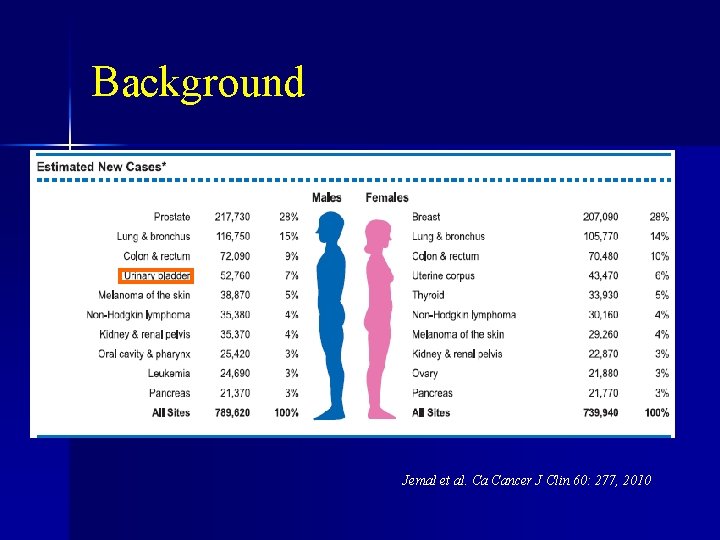
Background Jemal et al. Ca Cancer J Clin 60: 277, 2010
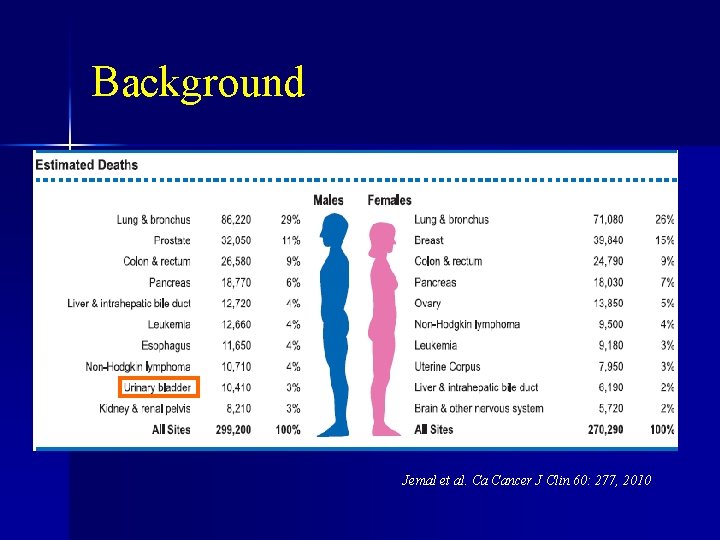
Background Jemal et al. Ca Cancer J Clin 60: 277, 2010

Background n n 70, 520 new cases of bladder cancer in 2010 14, 680 deaths attributable bladder cancer in 2010 Jemal et al. Ca Cancer J Clin 60: 277, 2010

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity of Surgery Risk Stratification

Incidence of High-Grade T 1 Disease n 25% of bladder cancer presents as muscle-invasive disease or greater 1 n n 17, 630 patients (expected) Approximately 25% of non-muscle-invasive bladder cancer presents as high-grade T 1 disease 2 n 13, 222 patients (expected) 1 Fedeli 2 Strope et al. , J. Urol, 185: 72, 2011 et al. , Cancer, 116: 2604, 2010
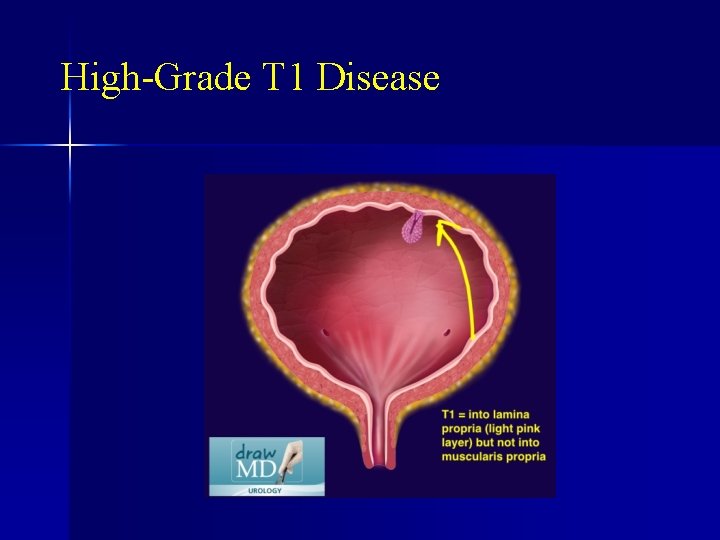
High-Grade T 1 Disease

Rule of 30%s 1 n 30% never recur n 30% require deferred cystectomy n 30% die of metastatic TCC 1 Cookson et al. , J Urol, 158: 1, 1997

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity of Surgery Risk Stratification
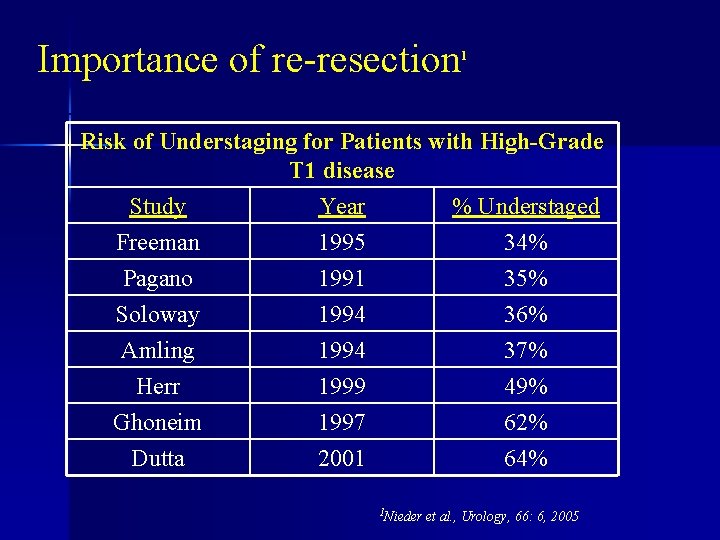

Importance of re-resection 1 Risk of Understaging for Patients with High-Grade T 1 disease Study Year % Understaged Freeman 1995 34% Pagano 1991 35% Soloway 1994 36% Amling 1994 37% Herr 1999 49% Ghoneim 1997 62% Dutta 2001 64% 1 Nieder et al. , Urology, 66: 6, 2005
Prognostic Importance of Reresection n 14% progression rate with less than T 1 disease n 76% progression rate with residual T 1 disease 1 Nepple et al. , Can J Urol, 3: 4, 2009

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity of Surgery Risk Stratification

Recurrence and Progression 1 n Probability of recurrence at 5 years: 50 -70% n Probability of progression to muscle invasion: moderate to high 1 NCCN Guidelines Version 2. 2011

Recurrence and Progression 1 n Predictive score based on – Number of tumors – Tumor size – Prior recurrence rate – T category – CIS – Grade 1 Sylvester et al. , Eur Urol, 49: 3, 2006

Progression 1 n Predictive score > 9 or presence of CIS – 2 -year progression rate approximately 30% 1 Sylvester et al. , Eur Urol, 49: 3, 2006

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity of Surgery Risk Stratification
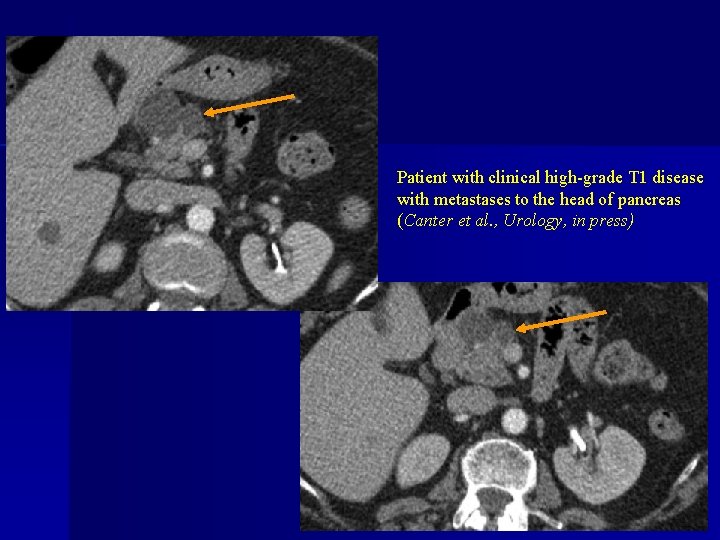
Patient with clinical high-grade T 1 disease with metastases to the head of pancreas (Canter et al. , Urology, in press)

Pathological Up-Staging at Time of Radical Cystectomy 1 n 51. 4% had p. T 2 disease or greater n 33. 4% had p. T 3 disease or greater n 16. 2% of patients had lymph node metastasis (range=9 -18% ) n 6. 3% of patients had positive surgical margins 2 1 Fritsche 2 Kulkarni et al. , Eur Urol, 57: 2, 2010 et al. , Eur Urol, 57: 1, 2010
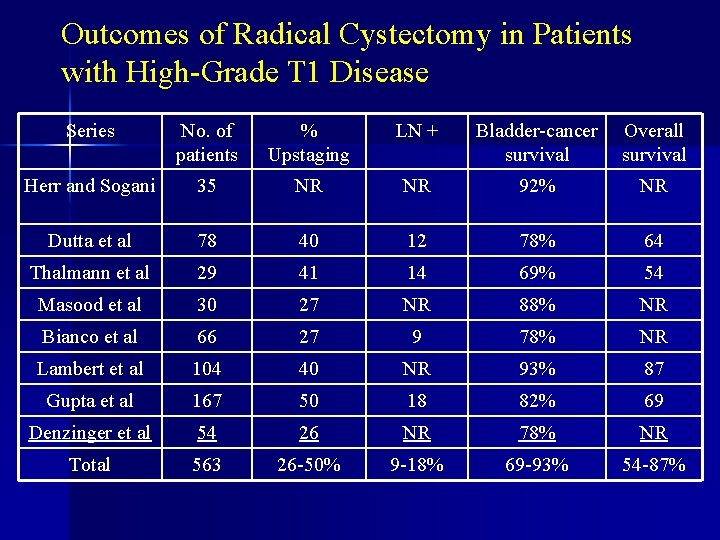
Outcomes of Radical Cystectomy in Patients with High-Grade T 1 Disease Series No. of patients % Upstaging LN + Bladder-cancer survival Overall survival Herr and Sogani 35 NR NR 92% NR Dutta et al 78 40 12 78% 64 Thalmann et al 29 41 14 69% 54 Masood et al 30 27 NR 88% NR Bianco et al 66 27 9 78% NR Lambert et al 104 40 NR 93% 87 Gupta et al 167 50 18 82% 69 Denzinger et al 54 26 NR 78% NR Total 563 26 -50% 9 -18% 69 -93% 54 -87%

Risk Stratification 1 n Low-risk T 1 – – n Unifocal disease No associated CIS Tumor accessible/resectable in full Residual disease <T 1 on restaging TURBt High-risk T 1 – – Multifocal disease Associated CIS Tumor hard to access/not resectable in full Residual disease >T 1 on restaging TURBT 1 Nieder et al. , Urology, 66: 6, 2005

1 Indications for Early Cystectomy n n Morphologic features – solid – large tumor size – multifocality Pathologic characteristics – depth of tumor invasion – associated CIS – presence of lymphovascular invasion Response to prior intravesical therapy Status of p 53, Ki 67, Cox-2, NMP-22 1 Bochner, Urol Oncol, 27, 2009

1 Indications for Early Cystectomy n n n Youth Extensive disease Incomplete resection Multiple, early recurrences T 1 with CIS High-risk histology (micropapillary, small cell, etc. ) 1 Montgomery et al. , Urol Oncol, 28, 2010

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity of Surgery Risk Stratification
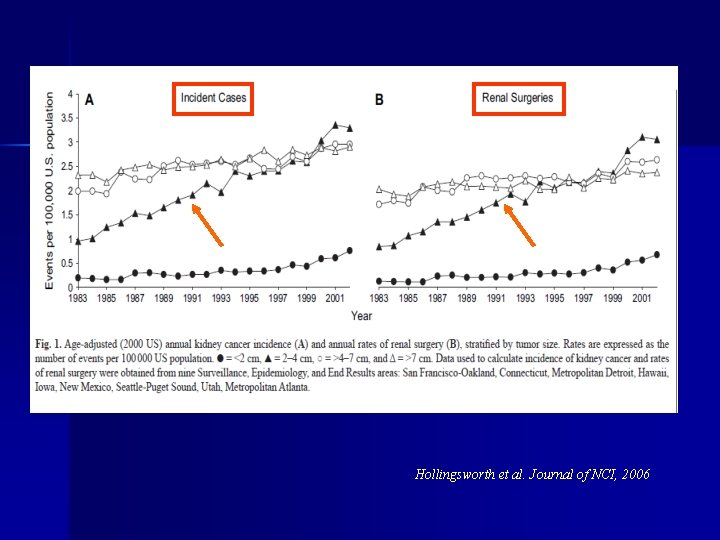
Hollingsworth et al. Journal of NCI, 2006
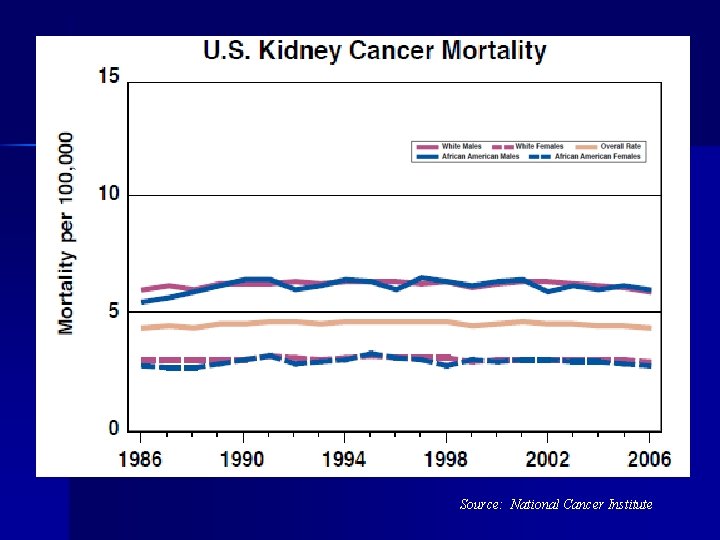
Source: National Cancer Institute
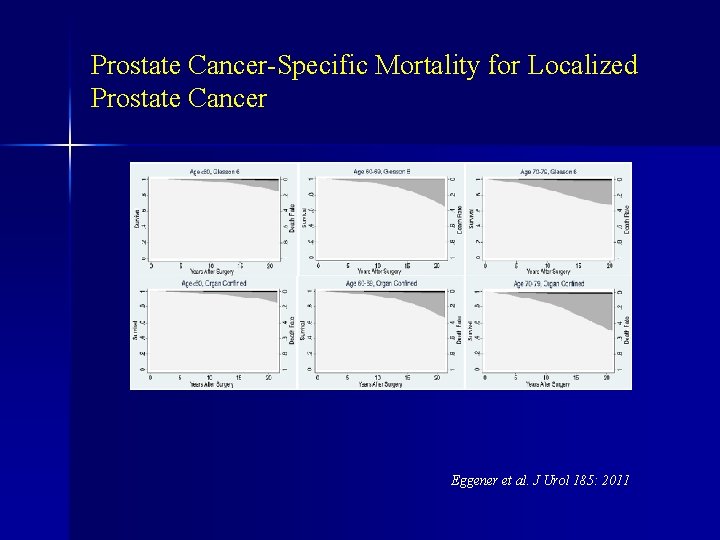
Prostate Cancer-Specific Mortality for Localized Prostate Cancer Eggener et al. J Urol 185: 2011

High-grade T 1 Disease n Why are more radical cystectomies not being done for high-grade T 1 disease?

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity of Surgery Risk Stratification

Risk Factors for Bladder Cancer n Age – Incidence increases with age – Median age=73 years n Gender – M: F=3: 1 n n History of cigarette smoking History of external beam radiation
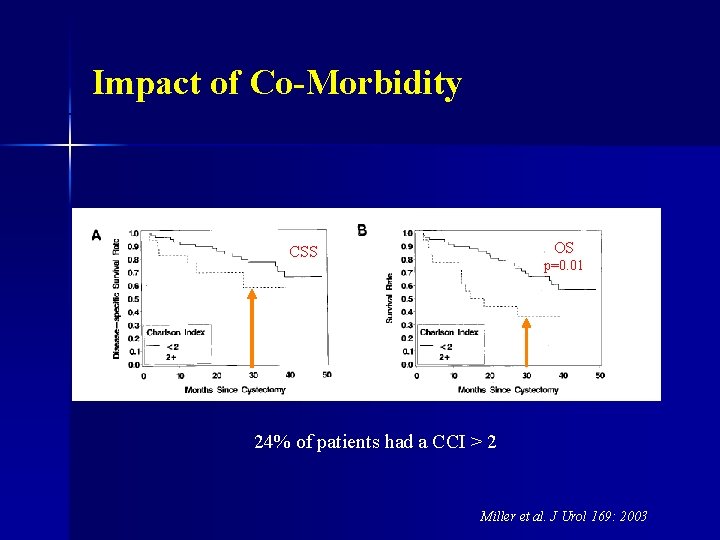
Impact of Co-Morbidity OS CSS p=0. 01 24% of patients had a CCI > 2 Miller et al. J Urol 169: 2003
90 -day Mortality Rate after Radical Cystectomy based on Hospital Discharge Status n Home without services = 4% n Home with services = 4. 8% n Transferred to facility = 20. 5% Aghazadeh et al. J Urol 185: 1, 2011

Early Complications n n n Examination of 1142 consecutive patients who underwent cystectomy at MSKCC Complications occurred in 64% of patients (735/1142) within 90 days of surgery Major complications (Clavien grade III-V) occurred in 13% of patients Shabsigh et al. Eur Urol, 55: 1, 2009

Early Complications n 6, 577 patients from NIS from 1998 to 2002 n 2. 57% in-hospital mortality rate n 28. 1% complication rate, digestive system most common (16. 1%) n Age and co-morbid conditions predictors of complications; high-volume centers and women were associated were lower risk of complications Konety et al. Urol, 68(1), 2006

Long-term Complications after Radical Cystectomy n 1, 057 patients n 1, 453 conduit-related complications in 643 (61%) patients n 2. 3 complications/patient Shimko et al. J Urol, 185: 2, 2011

High-grade T 1 Disease n How can we choose better?

Outline n n n n Background Incidence of High-grade T 1 Disease Importance of Re-resection Recurrence and Progression Clinical Understaging Patient Selection Morbidity of Surgery Risk Stratification

Charlson Co-Morbidity Index (CCI)

http: //www. medal. org/Online. Calculators/ch 1. 13/ch 1. 13. 01. p hp or www. urologymatch. com

Competing Risks Nomograms www. cancernomograms. com

www. cancernomograms. com

www. cancernomograms. com
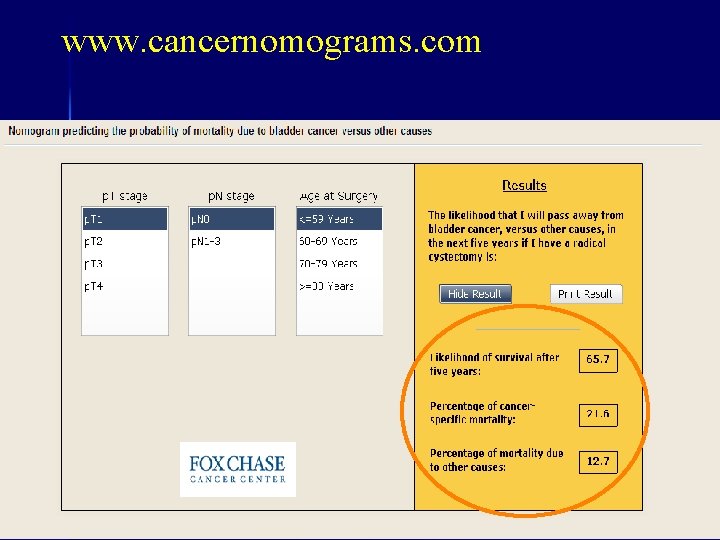
www. cancernomograms. com

Conclusions n High-grade T 1 bladder is a heterogeneous disease with an aggressive biologic behavior in the majority of patients n Radical cystectomy is not without risk, carrying a high amount of morbidity and mortality n Risk stratification is imperative n These tools exist and can help to objectify treatment decision-making (i. e, early cystectomy versus delayed cystectomy)

Conclusions n Considering the aggressive phenotype of highgrade T 1 bladder cancer and the fact that many patients will have extravesical/nodal disease at the time of “early cystectomy”, is it justified to defer early definitive treatment in this group of patients when medically fit?
- Slides: 45