High Risk Newborn Part II Resuscitation n Asphyxia

High Risk Newborn: Part II

Resuscitation n Asphyxia leads to tissue damage n Oxygen saturation 93 -97% Airway -- establish patent airway n Suction mouth and nose n Prone in sniffing position Breathing – Rate of 40 -60 bpm n Initiate breathing n Tactile stimulation while drying n Mask fits over nose and mouth n 100% oxygen

Resuscitation n n Circulation n Assess pulse by palpating umbilical cord or auscultate apical pulse n If pulse < 60 bpm, begin compressions Drugs – administer medications n Initiate IV of 10% dextrose (D 10 W) n Epinephrine for bradycardia n Naloxone Hydrochloride (Narcan) to reverse narcotic depression

Respiratory Distress n Assessment n Tachypnea n Retractions n Expiratory grunt n Nasal flaring n Cyanosis n Decreased breath sounds Breath sounds wet n Decreased p. H, decreased p. O 2, increased p. CO 2 Causes n Cold stress n Sepsis n Respiratory distress syndrome n n

Respiratory Distress n Interventions n Monitor color, rate, and effort of breathing n Monitor oxygenation n Airway clearance n Support respirations as prescribed n O 2 at lowest concentration needed n Nasal cannula or Oxyhood n Positive pressure or High frequency ventilator n Liquid ventilation or Nitric oxide

Transient Tachypnea of the Newborn n n Begins after birth and lasts about 2 days Delayed absorption of fetal lung fluid n Common in babies from cesarean delivery n Smoking during pregnancy n Neonates of diabetic mothers n Small for gestational age n Percipitous delivery – no thoracic squeeze

Transient Tachypnea of the Newborn n n Assessment – respiratory distress Intervention n Oxygen administration n Monitor oxygen level n Neutral thermal environment n Maintenance of acid-base balance n Nutrition

Respiratory Distress Syndrome n Deficiency in surfactant production resulting in atelectasis, hypoxia, and acidosis n n n n With atelectasis, lungs are less compliant Leads to vasoconstriction and increased pulmonary vascular resistance Decreases blood flow to lungs Leads to hypoxia and increased CO 2 Leads to acidosis Leads to increased vasoconstriction Which further impairs surfactant production

Respiratory Distress Syndrome n n (cont) n Alveoli can become necrotic and capillaries are damaged n Ischemia allows fluid to leak into the interstitial and alveolar space n Forms a hyaline membrane n Hyaline membrane hinders respiratory function by decreasing lung compliance n Poor lung compliance leads to right to left shunting of blood through foramen ovale and ductus arteriosus Associated with high risk of long-term respiratory and neurologic complications

Respiratory Distress Syndrome n Assessment n n n n Tachypnea Labored breathing Retractions and nasal flaring Crackles Cyanosis Expiratory grunting Hypoxemia, hypercapnia, aciodosis X-ray has diffuse granular pattern

Respiratory Distress Syndrome n Intervention n n n n Administer surfactant replacement Administer glucocorticosteroids Thermoregulation Oxygen and mechanical ventilation Monitor blood oxygen level Correct acidosis Parenteral feedings Decrease stresss

Persistent Pulmonary Hypertension (PPHN) n n n High pulmonary vascular resistance n Unoxygenated blood shunting through ductus arterosa Assessment n Respiratory distress and tachycardia n Murmur n Fluctuating PO 2 levels Interventions n Administer O 2 and nitric oxide n Decrease stress

Bronchopulmonary Displasia n n n Chronic disease as complication of RDS n Ventilator - alveoli over inflate and rupture n Inflammatory changes lead to scarring Assessment n Abnormal alveoli on x-ray n Signs of respiratory distress Interventions n Low ventilator pressure to maintain O 2 level n Theophylline to increase lung compliance n Diuretics to decrease interstitial fluid n Long hospitalization and maybe home on O 2

Meconium Aspiration Syndrome n n Fetal hypoxia, relaxing anal sphincter, passes meconium in amniotic fluid Meconium inhaled into lungs while in utero or with first breaths n Adheres to airway and alveoli n Meconium creates ball-valve effect n Hyperinflation, hypoxemia, and acidosis causes increased peripheral vascular resistance

Meconium Aspiration Syndrome n n Assessment n Dark green staining of amniotic fluid n Green staining of vernix, skin, and nails n Respiratory distress with course crackles Interventions n Suction airway before shoulders are delivered and before first breath taken n Suction trachea until clear n Administer oxygen and ventilation n Extracorporeal membrane oxygenation

Thermoregulation: Cold stress n n Maintain neutral thermal environment to ensure metabolic homeostasis n Temperature at which the infant’s metabolic rate and oxygen consumption is at a minimum Influencing factors n Characteristics of baby n Environment: sources of heat loss n Stimulation of non-shivering thermogenisis

Thermoregulation: Cold stress n Signs of cold stress n Decreased skin temperature n Mottling, acrocyansis, and pallor n Respiratory distress n Lethargy, decreased muscle tone, poor feeding n Decreased oxygen to tissues n Hypoglycemia n Acidosis
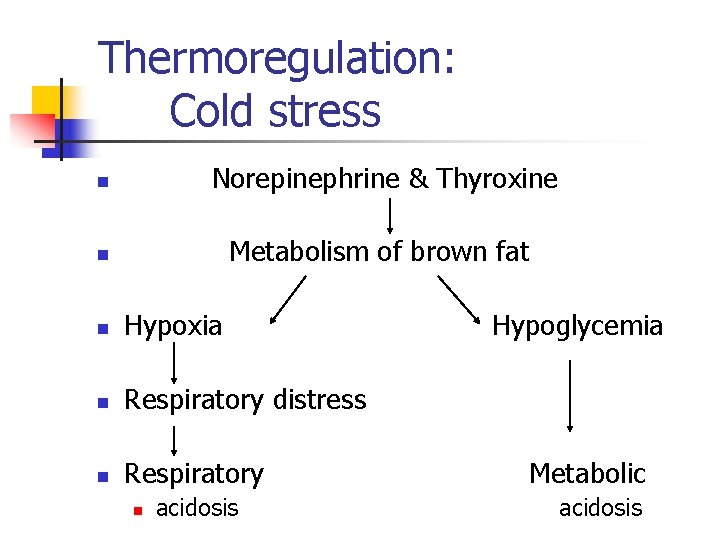
Thermoregulation: Cold stress Norepinephrine & Thyroxine n Metabolism of brown fat n n Hypoxia n Respiratory distress n Respiratory n acidosis Hypoglycemia Metabolic acidosis

Thermoregulation: Cold stress n Intervention n Reduce heat loss -- Conduction, convection, radiation, evaporation n Gradually warm baby n Monitor vital signs n Monitor for and treat hypoglycemia n Monitor for and treat hypoxemia n Evaluate for underlying problems

Sepsis n Assessment n Behavioral changes n Temperature instability n Changes in feeding n Apnea n Mottling, pallor, and cyanosis Hyperbilirubinemia n Abdominal distention Intervention n Obtain cultures n Antibiotics n Neutral thermal environment n Supportive care n n

Hypoglycemia n n Factors n Decreased availability of glucose and fat n Increased utilization of glucose Signs n Jittery and twitching - Poor suck n Unstable temperature - Seizures n Apnea - Hypotonia n Lethargy - Weak cry n Hypoglycemia: < 40 mg/dl

Hypoglycemia n Interventions n Monitor at-risk population n Decrease glucose requirements n Provide glucose n Entera: Oral and Gavage n Parenteral: IV

Pain Relief n n Pain medications Sucrose elevates the pain threshold through an opioid release in the CNS n Use for heel sticks, suctioning, venipuncture, circumcision n 0. 5 to 2 ml via syringe or nipple n Monitor for hyperglycemia

Hyperbilirubinemia n n n Bilirubin - red blood cells are broken down n Unconjugated cannot be excreted n Liver enzymes transform into conjugated n Conjugated bilirubin excreted in stools and kidneys Jaundice - yellow pigment in tissue Kernicterus - Serum level over 20 mg/d. L n Unconjugated bilirubin is toxic and crosses blood-brain barrier n Results in permanent neurological damage

Hyperbilirubinemia n Intervention n Phototherapy n Florescent light alters structure of bilirubin to water soluble for excretion n Expose as much skin as possible n Shield eyes n Monitor temperature and increase fluids n Fiberoptic blanket n Home phototherapy n Frequent feeding for hydration and excretion n Administer albumin and phenobarbital

Hyperbilirubinemia: Pathologic jaundice or hemolytic disease n n Rh and ABO blood type incompatibility n Antigens from baby’s blood enter mom’s bloodstream n Antibodies are formed by mom n Future pregnancies the antibodies cross the placenta n Antibodies hemolize fetal RBCs ABO more common but less threatening than Rh n ABO - Type O mom with Type A or B fetus n Rh – negative moms with positive baby

Hyperbilirubinemia: Pathologic jaundice or hemolytic disease n n Assessment n Hyperbilirubinemia rapidly after birth n Edema and anemia Intervention n Exchange transfusion after birth or intrauterine n Indicated for positive direct Coombs’ and elevated bilirubin levels n Removes sensitized RBC and treats anemia n Rho(D) immune globulin (Rho. GAM) within 72 hours of delivery or procedures

Neonatal Developmental Care n n n Decrease noxious stimulation n Lights and noise Read the baby’s behavioral cues n Stress n Self-comforting Care techniques n Containment n Nesting n Kangaroo care n Co-bedding

Psychosocial Needs: Facilitate family coping n n Explain equipment simply and slowly n No technical jargon n Focus on the baby not on the equipment Don’t make promises you cannot keep Do not give unrealistic reassurance or take away all their hope Allow parents to touch and talk to baby n Don’t insist that they touch if they are uncomfortable n Show baby is responding to them

Psychosocial Needs: Facilitate family coping n n n Refer to child by name Parents need to understand be understood Allow to voice concerns and feelings Allow to help with THEIR child’s care Allow to voice concerns and feelings n Keep communication open. Telephone calls. n “You must be wondering what caused this” “Are you wondering how you are going to manage? ”

Anticipatory Grief n Attachment n n Loss of the perfect child n n Parents go home without baby (loneliness), bring in toys and pictures, marital problems Guilt (what did I do wrong? ), may withdraw physically or emotionally, be realistic and honest with child’s outcome, must grieve for loss of perfect child before attaching to this one, demands from abnormal child inhibit grief recovery Neonatal death n Pictures, lock of hair, foot prints, hold baby

ECMO n Extra Corporeal Membrane Oxygenation

References n n n Hogan, M. A. , & Glazebrook, R. S. (2003). Maternalnewborn nursing: Reviews & rationales. Upper Saddle River, NJ: Prentice Hall. Ladewig, P. A, London, M. L. , & Davidson, M. R. (2006). Contempary maternal-newborn nursing care (6 th ed. ). Upper Saddle River, NJ: Prentice Hall. Littleton, L. Y. , & Engebretson, J. C. (2005). Maternity nursing care. Clifton Park, NY: Thomson Delmar Learning. Olds, S. B. , London, M. L. , Ladewig, P. A. , & Davidson, M. R. ( 2004). Maternal-newborn nursing & women’s health care (7 th ed. ). Upper Saddle River, NJ: Prentice Hall. Silvestri, L. A. (2002). Saunders comprehensive review for NCLEX-RN (2 nd ed. ). Philadelphia: W. B. Sanders. Straight A’s in maternal-neonatal nursing. (2004). Philadelphia: Lippincott Williams & Wilkins.
- Slides: 33