HIGH RISCK NEW BORN BABY PRETERM NEW BORN
HIGH RISCK NEW BORN BABY PRETERM NEW BORN

PRETERM NEW BORN Definition: Preterm new born is a baby with: ØGA < 37 weeks, Ø Wb < 2500 g, Ø Hb < 47 cm. Preterm new born has the adequate weight for the gestational age.

Prematurity degrees International Clasification Diseases (ICD) New born Gestational Age Birth Weight Low birth weight (LBW) Very low birth weight (VLBW) GA < 37 w. Wb = 2499 g – 1500 g GA < 32 săpt. Wb =1499 g – 1000 g Extremely low birth weight (ELBW) GA < 28 săpt. Wb < 1 000 g

PRETERM NEW BORN Causes of prematurity: Maternal causes: Ø mother’s age < 14 years and > 35 years; Ø mother’s height (<1, 50 m); Ø mother’s weight (< 45 kg); Ø Obstetrical causes: - uterine: infantile uterus, uterine malformations, tumors, chronic endometritis, uterine fibromatosis, incompetence cervicoisthmic;

PRETERM NEW BORN Maternal causes: - placenta: retroplacentare hemorrhage, early detachments of placenta, placenta praevia; - premature rupture of membranes, repeated abortions, narrow pool, oligo / polihidramnios, multiparous; - acute diseases: influenza, pneumonia, hepatitis; - chronic diseases: diabetes, feto - maternal isoimmunization, thyroid disease, kidney or heart disease, syphilis, tuberculosis;

PRETERM NEW BORN Maternal causes: - vascular-kidney syndrome; - chronic poisoning: smoking, alcoholism, drugs - self-intoxications: pregnant toxemia; - history of infertility; - pregnancies occurred in a too short time; - hormonal imbalances.

PRETERM NEW BORN Fetal Causes: - twins; - fetal chromosomal diseases; - fetal malformations; - erythroblastosis; - Intrauterine Growth Retardation - IUGR; - fetal chronic infections (TORCH).

PRETERM NEW BORN Social causes: - low socio-economic status; - low education; - poor diet; - physical trauma and / or psychological; - excessive effort; - failure to comply with hygiene rules. Cause unknown ~ 30% of premature births.

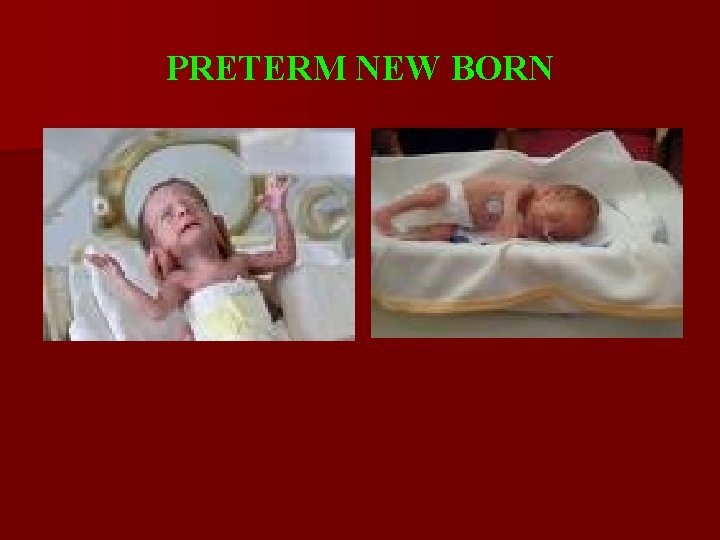
Clinical Features of premature new born Clinical features - specific for duration of gestation. HEAD: - large dehiscence sutures, fontanelles wide open, hair rarely - face - small, triangular, senile aspect, large mouth, sharp chin, - ears – low position, stuck to his head, with poor development of cartilage. The neck is thin.

Clinical Features of premature new born Chest: narrow, poorly mineralized, the ribs are horizontal. Abdomen: - voluminous and flattened on the sides (large volume of liver and muscle hypotonicity) - frequently → dehiscence of rectus abdominis, umbilical and inguinal hernia. The legs are short and thin.
PRETERM NEW BORN

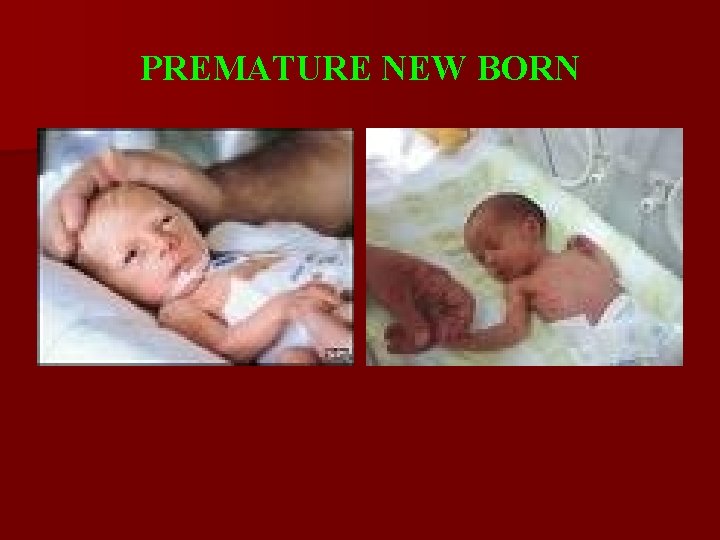
Clinical Features of premature new born Skin: - thin, red at birth, become pale after a week; - lanugo: abundant on the face, limbs, back trunk; - vernix caseosa: small quantity / missing; - physiological desquamation: prolonged, furfuraceous or lamellar; - hangs in folds.

Clinical Features of premature new born Nails: - soft, weak, lacking longitudinal ribs, do not touch fingertips. Subcutaneous tissue: - diminished; - turgor is flaccid. Muscle: - hypotonic.

Clinical Features of premature new born Skeletal system: poorly mineralized. External genitalia: poor developed; ♂: - testis are not present in the scrotum (80%) - scrotum is small, without pleats and poorly pigmented. ♀ - vulva wide open - labia majora, underdeveloped - do not cover labia minora and clitoris. - genital crisis is absent / appears later.
PREMATURE NEW BORN

Deficiency of the Respiratory Function: - trachea and bronchisoles are narrow; - lung elasticity is low; - poor mineralization of the ribs, muscle hypotonia and high position of lungs and diaphragm limites lungs expansion and favors indrawing; - qualitative and quantitative deficiency of surfactant maintains high superficial tension and promote the collapse of the alveoli;
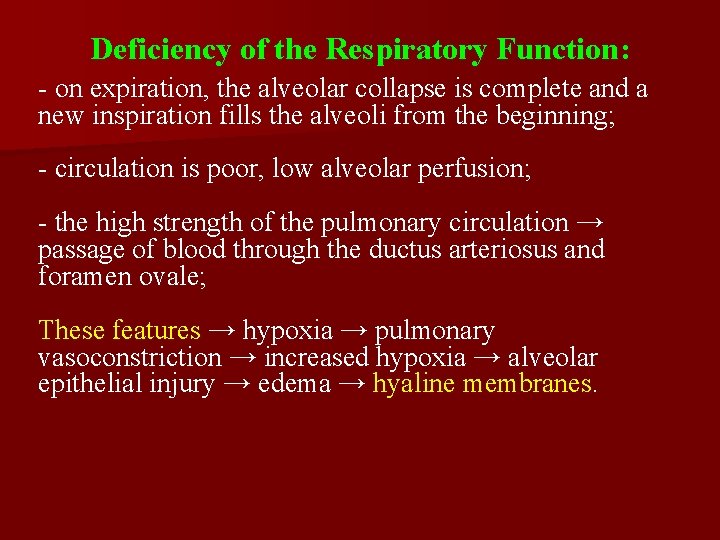
Deficiency of the Respiratory Function: - on expiration, the alveolar collapse is complete and a new inspiration fills the alveoli from the beginning; - circulation is poor, low alveolar perfusion; - the high strength of the pulmonary circulation → passage of blood through the ductus arteriosus and foramen ovale; These features → hypoxia → pulmonary vasoconstriction → increased hypoxia → alveolar epithelial injury → edema → hyaline membranes.

Deficiency of the Respiratory Function: Respiratory center → three centers: - apneustic - on the superior part of the medulla oblongata; - pneumotaxic – in pons; - gasping - at the inferior part of the medulla oblongata. Apneustic center → tonic contraction of respiratory muscles → inspiration. His action is discontinuous interrupted by pneumotaxic center → expiration.

Deficiency of the Respiratory Function: Hypoxia → apneustic center stops working → automatism of gasping center → rudimentary respiration, with sudden inspiration, jerky, spasmodic movements of the mouth and jaw, followed by long pauses in breathing. Imperfection of the superior respiratory centers and the automatism of the inferior respiratory centers = apneic attack of the premature baby.
Deficiency of the Respiratory Function: Apnea of the premature baby = cease breathing ~ 20 seconds, accompanied by bradycardia (HR<80 beats / min) and cyanosis. Types: - Central apnea: cessation of breathing movements and nasal airflow, favored by diaphragmatic fatigue and impaired neurotransmission; - Obstructive apnea: cessation of nasal airflow, maintaining respiratory movements secondary airway obstruction; - Mixed apnea (the most common): combination of central and obstructive apnea.

The deficiencies of respiratory → respiratory distress Clinic: - tachypnea (up to 100 – 120 breath/min) - functional respiratory syndrome (expiratory moaning, intercostal indrawing, thoraco-abdominal swing) - cyanosis. To reduce its severity i. m. corticosteroid (Betamethasone) are recomanded to all pregnant women with imminent premature delivery.

Cardio-vascular characteristics of premature new born Hypoxia → pulmonary vasoconstriction → high resistance in the pulmonary circulation→ increase volume of the right ventricle (EKG: the heart's electrical axis deviation to right). Hypoxia and metabolic acidosis → Botal's hole permeability and persistence of the ductus arteriosus (clinical: the corresponding murmurs). Low oxygenation of the myocardium and depletion of small quantity of glycogen → heart failure.
PREMATURE NEW BORN

Haemodynamic Features in new born baby Blood pressure: low (45 -70 mm. Hg/30 -45 mm. Hg) → peripheral irrigation is reduced and slow. Cerebral arteries conjunctivo - elastic tunic is weak, fragile → bleeding. High permeability of capillaries + hypoproteinemia → edema. n

Haemodynamic Features in new born baby Hemoglobin: 90 -100% fetal hemoglobin, persist for a long time. Leukocytes: - 8. 000 -10. 000/mm 3 birth, predominantly neutrophils, - lymphocytes predominate after 2 -3 weeks. Platelets: 150000 - 200000/mm 3. Clotting factors: low levels + capillary fragility → bleeding (in the brain and adrenal) between the 3 rd and 7 th day after birth.

Deficiency of Digestive Function Sucking reflex: - absent in children GA<32 -33 weeks. Swallowing reflex: - absent in most children with Wb <2000 g. In these children liquids are administered by gavage feeding. Reduced salivary secretion, dry and permeable oral mucous membrane → stomatitis. Salivary amylase is present at birth.

Deficiency of Digestive Function Stomach: - low capacity - mucosa has few folds, - glands and muscle fibers are less developed, - evacuation is delayed, - hydrochloric acid secretion is good, - rennin, pepsin and gastric lipase are present at birth.

Deficiency of Digestive Function Intestine: - hypotonic musculature, → slow peristaltic movements - bloating and constipation, - much increased mucosal permeability, - disaccharidases (invertase, maltase and lactase) activity are normal at birth. Pancreas: - pancreatic amylase missing - lipase activity is low - trypsin activity is normal.

Deficiency of Digestive Function Liver: - embryonic-type structure, with haematopoietic centers, - immature liver function: → jaundice more frequently, earlier, prolonged and intense (bilirubin can reach 150 mg / l) as function of conjugation is deficient; phototherapy and exchange transfusion rarely required; → hypoalbuminaemia which favors the occurrence of edema; → vascular fragility ↑ + hypoprotrombinemie → bleeding tendency; → hypoglycemia due to inappropriate storage of glycogen in the liver.

Deficiency of Digestive Function Digestion and absorption of milk proteins is the same as that of full term new born. Digestion and absorption of lipids in human milk is made effective due to the existing milk lipases. Carbohydrate digestion and absorption is satisfactory. Pre term newborn can use the lactose in milk, despite having a transient lactase deficiency in the first week of life.

PRETERM NEW BORN

Deficiency of Urinary System Kidneys → embryonar lobulated. → irrigation is low. - glomerular filtration is deficient. - dilution capacity and concentration are poor → tendency to hyper / hyponatremia and the occurrence of edema. - increased glomerular permeability in the first days of life → albuminuria. - renal immaturity → imbalance in removing urea, chlorides, phosphates.

Particularities of Hydro-mineral metabolism - increased body fluid content (75 -82%); - predominates extracellular fluids; - hydrolability slightly higher due to mobilization of extracellular fluid; - retention tendency for Na with edema appearance; - tendency to hypocalcemia (Ca reserves are low due to a short gestation, food intake does not cover high needs of the premature baby).

Deficiency of Immune System Nonspecific immunity: Mechanical barrier: - skin does not act as a barrier (lack of both stratum corneum and skin acidity created by sudoriparous glands). - mucous: has no secretory Ig A. Cellular Immunity: is poor because of weak leukocyte chemotactic response. Characteristics of serious infections: - develops without an increase in the number of white blood cells, sometimes with leukopenia, - have non-specific clinical aspects, difficult to recognize.

Deficiency of Immune System Non-specific humoral immunity (opsonins, complement, properdin, Lysozyme) is also low. Specific immunity: specific humoral immunity is very diminished (Ig. G from mother to fetus passes in the last months of pregnancy). Personal immunogenesis - Ig. M and Ig. A – is deficient.

Cerebral Deficiency Brain: - convolution and grooves: only sketched; - distinguish between white and gray matter is hardly seen; - cortical and subcortical low vascularization is a little higher in periventricles region and for gray nuclei. Nervous cerebral cells are less developed.

Cerebral Deficiency Myelination process is almost absent (only the spinal cord and medulla oblongata have a beginning of myelination). CML(cerebromedullary liquid): -xanthochromic; -albuminorrhachia, glycorrhachia and cellularity are increased. Primitive reflexes are barely sketched / missing in most premature.

Deficiency of the Termoregulator Function - tendency to hypothermia - thermolysis → increased (subcutaneous tissue is reduced) - thermogenesis → deficient, is achieved primarily by chemical mechanisms. Maintaining body temperature at 36. 5 ° to 37 ° C is absolutely required to reduce energy costs and nutrient intake.

Deficiency of the Termoregulator Function Hypothermia: → vascular collapse, → diffuse capillary bleeding, → hypoglycemia → severe kidney disorders, → sclerema (irreversible waxy induration of the skin and subcutaneous tissue). The point of thermic neutrality at which the infant has a minimum oxygen consumption is the temperature of 32º C.

Preterm new born

Evolution and Prognosis of Preterm New Born Depends on: - degree of prematurity; - hypoxia at birth; - the underlying cause of premature birth; - nursing conditions and subsequent morbidity. Immediate complications: - intraventricular hemorrhage; - ulcerative-necrotic enterocolitis; - hyaline membrane disease; - cholestatic liver; - nutritional deficiencies; - severe infections.

Evolution and Prognosis of Preterm New Born Late complications: - Eye (premature n. b. retinopathy, strabismus, myopia); - Auditory (hearing loss, deafness); - Neurologycal (motor disability, mental retardation, speech, learning, memory, attention and behavior disorders); - Lung (broncho-pulmonary dysplasia, chronic lung disease) - Deficiencies (anemia, rickets, malnutrition).

Premature New Born Care v Prevention of premature delivery: tocolytic medication in pregnant women. v In the delivery room: Controlling respiratory deficit: - gentle suction airways and mouth for improving the breath; - laterally recumbent position and head upper; - in gastric stasis – suction of gastric content to make easier the diaphragmatic movements; - heated, humidified, discontinuous oxygen, 2 -4 l / min by nasal cannula, CPAP (Continuous Positive Airway Pressure), tracheal intubation;
Premature New Born Care

Premature New Born Care Thermoregulation Deficiency Control: - delivery room`s temperature of 26° C; - swaddling with warm clothes; - ward`s temperature of 26 – 28° C; - premature infants with W. b → T = 34° C; for each additional 250 g T→ minus 1° C; per 250 g minus T is increased by 1° C.
Premature New Born Care

Premature New Born Care Acidosis control: - glucose solution + oxygen + 5% sodium bicarbonate for mother during delivery and then for new born, during the first days, depending on the values of Astrup. Hemorrhage tendency control: - smooth gestures; - avoiding Trendelemburg position (increased risk of intracranial hemorrhage); - vitamins C and E (capillary - trophy); - vit. K during the first days.

Premature New Born Care Infections prophylaxis: - small wards with their own circuits; - access to foreign persons is forbidden; - limiting contact between sick and the healthy new born babies; - cyclic and curent disinfection of wards, cots, incubators; - humidifiers` liquid and oxygenators will be changed daily.

Premature New Born Care Infections prophylaxis: - prevention of air contamination in wards; - the staff will be regularly checked clinically and bacteriologically; - thorough washing of hands before handling each baby; - linens, dishes and medical instruments used will be sterilized before each use; - preventing contamination of milk.

Premature New Born Care Nutrition in premature new born babies : - individualized considering the degree of prematurity; - ideal food is human milk; - to premature Wb <1500 g human milk fortifiers will be added (eg FM 85, FMS); - in the absence of human milk will be used special milk formula (Humana 0, Aptamil Prematil, Pre. NAN).

Nutrition of Preterm New Born

Nutrition of Preterm New Born

Nutrition of Preterm New Born

Premature New Born Care Criteria for discharge of the premature new born: - receives all food ration (from bottle / breast); - shows a steady increase in weight and reached 2500 g; - is thermally stable outside the incubator; - does not show recent crises of apnea or bradycardia. We recommend periodic: ophthalmologic, acoustic haematologycal evaluation.

INTRAUTERINE GROWTH RETARDATION (IUGR)

IUGR NEW BORN IUGR new born baby is also known as: - dismature, - malnourished in utero, - small for gestational age (SGA). Definition: IUGR new born baby is the child who`s W. b is below the 10 th percentile on standard intrauterine growth or less than 2 SD from the average over the appropriate weight for GA.

IUGR NEW BORN

IUGR NEW BORN Maternal factors: - ↓ uteroplacentate flow (preexisting / pregnancyinduced hypertension, preeclampsia, diabetes, chronic disease, reno -vascular, collagen disease); - hypoxemia (severe anemia, chronic lung disease, cyanogen heart disease, hemoglobinopathyes, high altitude);

IUGR NEW BORN Maternal factors: - malnutrition (poor diet, low maternal H and W, anorexia nervosa); - multiple pregnancy (inadequate prenatal nutrition); - tobacco, alcohol, drugs; - drugs (anticonvulsants, anticoagulants, etc. )

IUGR NEW BORN Placental Causes: - perfusion disorders; - anatomical abnormalities (placental detachment, heart attacks, cancer, abnormal cord insertion, umbilical vessel thrombosis); - inflammation (bacterial, viral, parasitic).

IUGR NEW BORN Fetal Causes: -chromosomal abnormalities (trisomy 13, 18, 21, Turner syndrome, etc. ); -intrauterine infection (TORCH, syphilis); -malformations (anencephaly, gastrointestinal atresia, cardiovascular anomalies except for tetralogy of Fallot, transposition of great vasals).

IUGR NEW BORN Classification: Symmetric IUGR (harmonic, hypoplasia): W, H, HC equally affected; Asymmetric IUGR (disharmonic, hypotrophyc): H, HC relatively normal, low abdominal circumference.

IUGR NEW BORN Symmetric IUGR: microcephaly and elements suggesting genetic abnormalities (dysmorphic features), intrauterine infection (jaundice, petechiae, liver splenomegaly, abnormal eye).

IUGR NEW BORN Asymmetric IUGR: - n. b is thin, long, with a big head in contrast to the rest of the body; - the face is small, triangular, forehead is wrinkled; - the skin is thin, wrinkled, sometimes translucent and often persistent skin fold. - subcutaneous tissue: diminished.

IUGR NEW BORN Asymmetric IUGR: - muscle mass: diminished, showing hypertonia. - behavior: alert. - archaic reflexes: exaggerated. - ± tremor of the extremities. - appetite: generally good.

IUGR NEW BORN Complications: Intrauterine death by: - placental insufficiency; - malformations incompatible with life; - severe infections.

IUGR NEW BORN Complications Perinatal asphyxia and its sequelae: - hypoxic-ischemic encephalopathy, - meconium syndrome aspiration, - persistent fetal circulation syndrome, - respiratory distress syndrome, - heart failure - renal failure.

IUGR NEW BORN Complications Hypothermia secondary to disorders of thermogenesis and increased heat loss. Metabolic: disturbance of metabolism - of glucose (hypo / hyperglycemia); - of lipid (oxidation and diminished use of free fatty acids and triglycerides); - of protides (reduced absorption and increased loss of protein).

IUGR NEW BORN Complications Polycythemia secondary to chronic fetal hypoxia. Reduced immunological respondence and increased infectious risk. IUGR new born have higher risk of: - Ulcerative-necrotic enterocolitis; - Gastrointestinal perforations; - Sudden death.

IUGR NEW BORN Prognosis and evolution: Symmetrical IUGR will have a more reserved prognosis in terms of growth and neurological development compared with asymmetrical IUGR. Evolving → frequently neurological disturbances such as: cerebral palsy; low IQ; cognitive deficit; behavioral problems.

IUGR NEW BORN Prophylactic treatment: - monitoring of pregnancy (clinical examination, ultrasound screening for infections) - low dose aspirin therapy (prevents utero-placental thrombosis and infarction of the placenta) - caesarean section birth (natural birth would result in additional stress and aggravate pre-existing hypoxia).

IUGR NEW BORN IUGR newborn care In the delivery room: - hypothermia and hypoxia control (the same as premature); - 26 ° C temperature in wards; - gentle suction of upper airways - of mucus, amniotic fluid, meconium; - clamping and cutting immediately the umbilical cord - concedering polycythemia; - rebalancing via umbilical cord; - careful clinical examination → congenital malformations.

IUGR NEW BORN In neonatal unit care: correcting - hypothermia: thermal neutrality (32 ° C); - acidosis: solution of sodium bicarbonate; - hypoglycemia: glucose solution 10% - cerebral edema: mannitol in slow intravenous infusion - polycythemia: liquid in intravenous infusion / exchange transfusion with plasma according to Ht. Nutrition: the same principles as in the preterm new born, but has a better digestive tolerance.

POSTMATURE NEW BORN

POSTMATURE NEW BORN Definition: The newborn with GA > 42 weeks, regardless of W. b. Etiology: incompletely elucidated, more frequently in women with reproductive disorders and primiparous. Intrauterine evolution normal up to 42 weeks, but extended pregnancy lowers oxygen and nutrients → intrauterine death / acute fetal distress (Apgar often < 5 at 1 minutes).

POSTMATURE NEW BORN Clinic: - aspect of a 2 -3 weeks old child, thin, with wrinkled face, alert and eyes wide opened; - skin is pale, parchmenty, dry, cracked, sometimes greenish (impregnated with meconium); - lanugo and vernix caseosa missing; - hair is long and abundant; - nails are long; - subcutaneous tissue is diminished; - umbilical cord is impregnated with meconium.
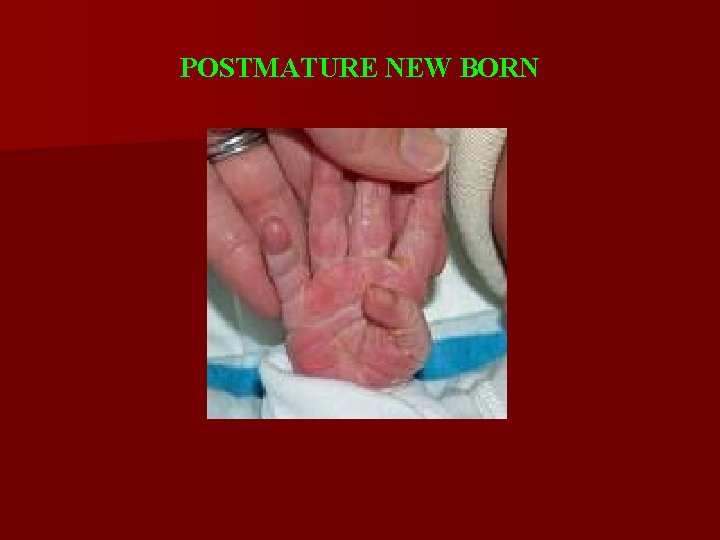
POSTMATURE NEW BORN

POSTMATURE NEW BORN Complications: - asphyxia at birth - meconium aspiration syndrome - persistent pulmonary hypertension - metabolic disorders (hypoglycemia, hypocalcemia) - mechanical trauma at birth.

POSTMATURE NEW BORN Postmature new born prognosis: reserved. Higher morbidity in the newborn period due to aspiration of amniotic fluid, meconium or central nervous system distress. Mortality can be reduced through appropriate obstetrical measures.

POSTMATURE NEW BORN Postmature new born care: Immediately after birth → fighting against: - aspiration syndrome of meconium and / or amniotic fluid; - hypoxia and acidosis.
- Slides: 80