Hidradenitis Suppurativa Authors Saideep Bose 1 Preetha Madhukumar

Hidradenitis Suppurativa Author(s): Saideep, Bose 1 Preetha, Madhukumar 2 ; Jeremy Ng 2 Academic Affiliation(s) : 1 Duke-NUS Graduate Medical School, Medical Student 2 Singapore General Hospital, Consultant Level: Basic Version No: 1. 2 Submitted: March 2012 Editors’ Review: December 2014

2 Disclaimer/Liability • The information provided in the VAP is made available in good faith and is derived from sources believed to be reliable and accurate at the time of release. • The materials presented on the VAP may include links to external Internet sites. These external information sources are outside the control of Duke-NUS. The user of the Internet links is responsible for making his or her own decision about the accuracy, reliability and correctness of the information found. • In no event shall Duke-NUS be liable for any indirect, special, incidental, or consequential damages arising out of any use of reliance of any information contained in the VAP. Nor does Duke-NUS assume any responsibility for failure or delay in updating or removing the information contained in the VAP. • Moreover, information provided on the VAP does not constitute medical advice or treatment nor should it be considered as a replacement of the patient/physician relationship or a physician’s professional judgment. Duke-NUS expressly disclaims all liability for treatment, diagnosis, decisions and actions taken or not taken in reliance upon information contained in the VAP. This work is licensed under a Creative Commons Attribution-Non. Commercial-No. Derivs 3. 0 Unported License To view a copy of this license, visit [http: //creativecommons. org/licenses/by-nc-nd/3. 0/]

3 Financial Disclosures (past 3 years) No Disclosures

4 Learning Objectives • Understanding the pathophysiology of hidradenitis suppurativa (HS) • Recognizing the common symptoms of the disease • Learning how to manage a patient with HS

5 Outline • Epidemiology • Anatomy • Pathophysiology • Presentation • Laboratory findings • Management • Differential diagnosis

6 Clinical Scenario • A 32 -year-old man comes to the clinic complaining of painful swollen boils in both of his armpits and his groin. The have recurred countless times and he remembers first noticing them as a teenager. • On examination you notice painful, swollen, erythematous nodules, scarred skin, and draining sinus tracts in both regions. • He has been treated multiple times with incision and drainage and antibiotics with no relief. • What are the next steps to take in the management of this patient?

7 Epidemiology • Prevalence is 1% in the general population • More common in women • Average of onset of symptoms is 20– 30 • Can be extremely painful and disabling • Diagnosis often delayed • Frequently mistaken for a simple infection
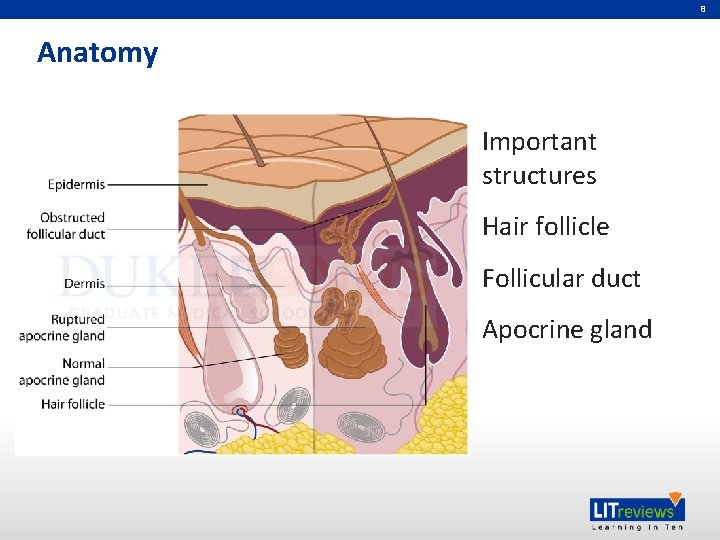
8 Anatomy Important structures Hair follicle Follicular duct Apocrine gland

9 Pathophysiology • Triggered by follicular obstruction • Allows bacterial proliferation and invasion • Follicle eventually ruptures • Bacteria, hair, and sebum spread to dermis • Immunologic response • Abscess and granuloma formation • Recurrence leads to scarring and sinus tract formation

10 Presentation • Mild symptoms during puberty • Tender subcutaneous nodules – Rounded and not pointed like boils • Average of two active lesions per month • Abscesses, rope like scars, and draining sinus tracts seen after repeated flares • Bilaterally affects axilla, inguinal, perianal, mammary, and pubic regions

11 Laboratory Findings • Cultures frequently negative • During a flare, normal skin flora usually found

12 Management • Diagnosis made clinically – Typical lesions: multiple, deep seated nodules – Typical locations: bilateral axillary, groin, or mammary involvement – History of relapses and ineffective treatment • Hurley’s clinical staging system
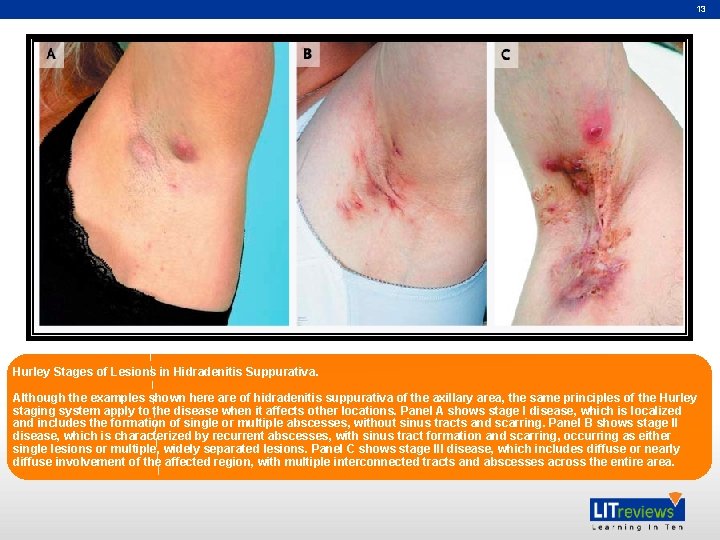
13 Hurley Stages of Lesions in Hidradenitis Suppurativa. Although the examples shown here are of hidradenitis suppurativa of the axillary area, the same principles of the Hurley staging system apply to the disease when it affects other locations. Panel A shows stage I disease, which is localized and includes the formation of single or multiple abscesses, without sinus tracts and scarring. Panel B shows stage II disease, which is characterized by recurrent abscesses, with sinus tract formation and scarring, occurring as either single lesions or multiple, widely separated lesions. Panel C shows stage III disease, which includes diffuse or nearly diffuse involvement of the affected region, with multiple interconnected tracts and abscesses across the entire area.

14 Management • Diagnosis made clinically • Hurley’s clinical staging system • Minimize Irritation • Drug therapy – Antibiotics: oral clindamycin + rifampicin – Hormonal manipulation therapy – TNF-alpha inhibitors: adalimumab • Surgery – Incision and drainage: only for symptomatic relief – Local unroofing – Excision: 1 cm margins, all the way to subcutaneous tissue, defect fixed with skin graft or local flap

15 Differential Diagnosis • Follicular pyoderma • Crohn’s disease • Acne

16 Summary • Results from the occlusion of a hair follicle, follicular rupture, and the subsequent inflammatory response • The diagnosis is made clinically • Stage I disease can be managed with drugs, Stage II with a combination of drugs and unroofing, and Stage III with unroofing or wide excision

17 References and Further Reading • Jemec GBE. Clinical practice. Hidradenitis suppurativa. N Engl J Med 2012; 366: 158– 164. • Margesson LJ and Danby FW. Treatment of hidradenitis suppurativa. Up. To. Date. October 12, 2011. • Margesson LJ and Danby FW. Pathogenesis, clinical features, and diagnosis of hidradenitis suppurativa. Up. To. Date. February 11, 2011. • Kathju S, Leslie-Ann L, and Post C. Hidradenitis suppurativa: A disease of apocrine gland physiology. Journal of the American Academy of Physician Assistants. November 1, 2008.

Partners in Academic Medicine
- Slides: 18