Hernias of the anterolateral wall of the abdomen

Hernias of the anterolateral wall of the abdomen -particular forms-

Inguinal hernias

Anatomy briefing w Definition: hernias produced through a defect situated on the posterior wall of the inguinal canal w Inguinal canal: a space designed for the passage of – Testis – peritoneal diverticula present at birth – Round ligament – peritoneal diverticula present at birth (Nuck) w Major opening in the mucsculo-fascial structure of the abdominal wall
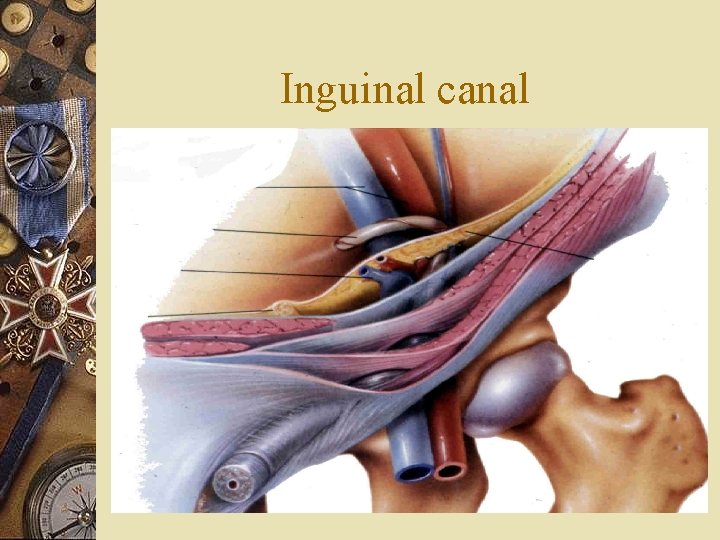
Inguinal canal

Inguinal canal - structure w Anatomic structures are dynamic – description represents a schematic view – 4 walls (anterior, posterior, superior and inferior) – 2 orifices: internal and external
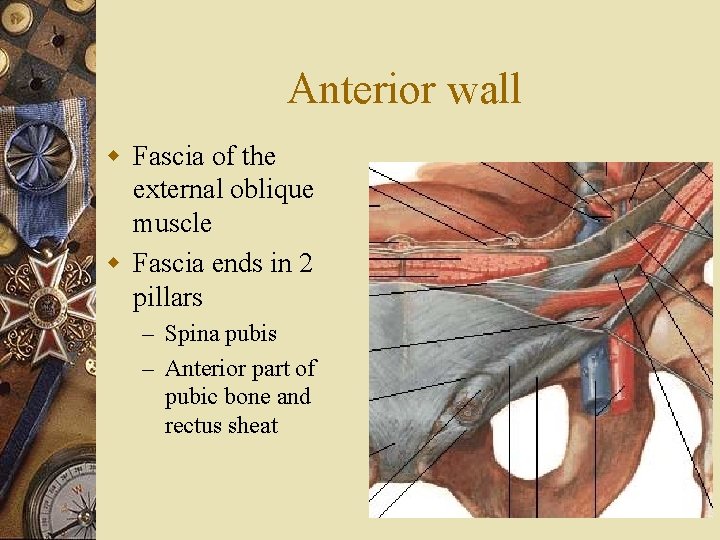
Anterior wall w Fascia of the external oblique muscle w Fascia ends in 2 pillars – Spina pubis – Anterior part of pubic bone and rectus sheat

Inferior wall w Inguinal ligament w Concavity opened above w Internally – it reflects fibers towards the pectineal ridge = the triangular ligament of Gimbernat and prolonges on the pubic branch of the iliac bone forming one body with the ligament of Cooper – solid strutcture
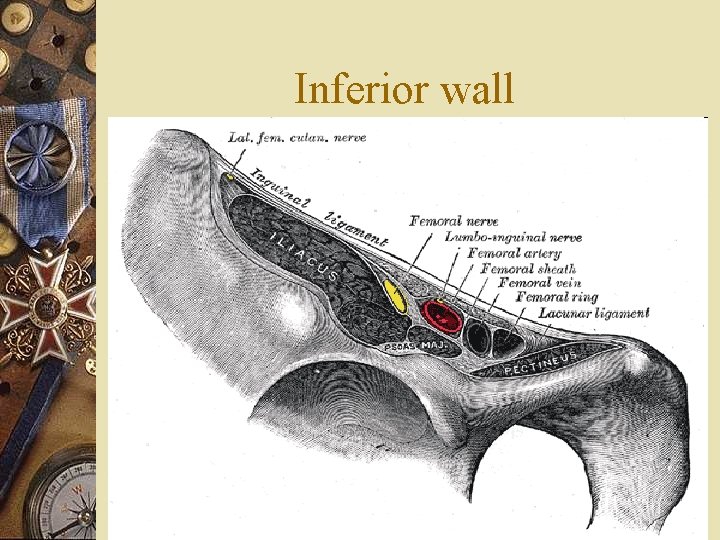
Inferior wall

Superior wall w Inferior border of internal oblique and transversus : the conjoined ligament w Fusion of the structures is NOT the rule w The resultant structure is not fibrotic and sometimes very friable – not suitable for suturing
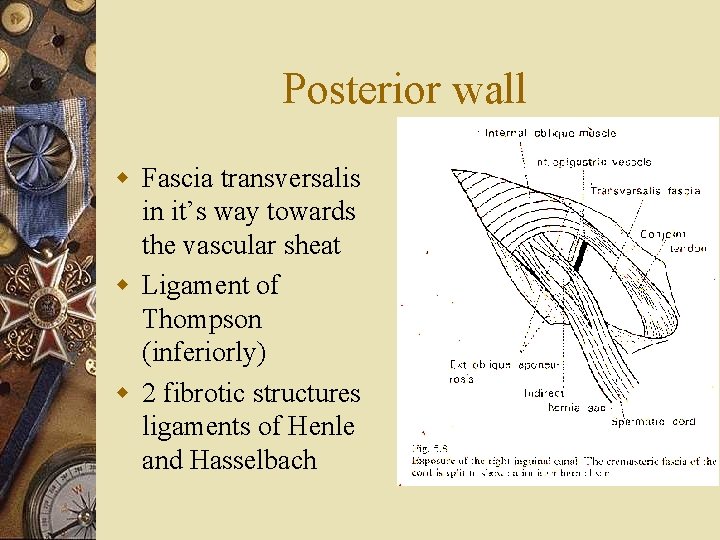
Posterior wall w Fascia transversalis in it’s way towards the vascular sheat w Ligament of Thompson (inferiorly) w 2 fibrotic structures ligaments of Henle and Hasselbach

Posterior wall w Weak anatomic region predisposed to hernia formation w Muscular structures are supposed to close the defect during effort w Inferior eipgastric vessels separate 3 parts – Profound inguinal orifice (external oblique hernia) – Middle part (medial to the epigastric vessels)– direct inguinal hernia – Internal part (medial to the umbilical artery) inetrnal oblique hernia

Orifices w Profund (lateral or internal) – Situated in fascia transversalis – the external part – A weak point of the abdominal wall w Superficial (medial or external) – Between the pillars of the fascia of the external oblique muscle – The place where a hernia engages towards the scrotum – Place to introduce finger for palpation

Content of the inguinal canal w Women: round ligament + vessels w Men: spermatic cord – – – cremaster vas deferens spermatic artery deferntial artery 2 venous plexuses Nervous branches (ilio-hipogastric, ilioininguinal, genital)

Shall we all develop hernia? w There is a content passing from the abdomen to scrotum w BUT – The trajectory is oblique through muscles and during effort the structures are compressed together – Oblique muscles work as a curtain and close the defect – Internal orrifice is strangulate during effort

External oblique inguinal hernia w Congenital: persistentce of the peritoneal diverticula through which the testis migrated in scrotum. Frequently associated with abnormal migration of the testis. – Complete form with totaland free comunication from the peritoneum till scrotum – Incomplete forms – vaginala testicularis is separeted +/- hydrocele or cystic remnants in the spermatic cord.
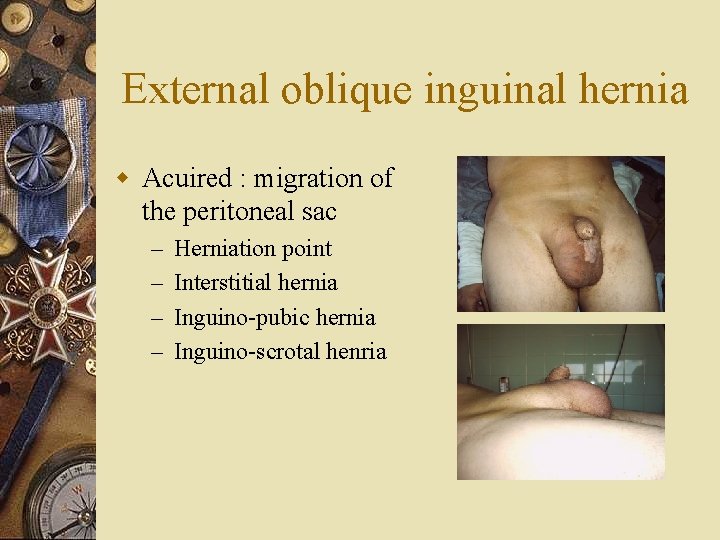
External oblique inguinal hernia w Acuired : migration of the peritoneal sac – – Herniation point Interstitial hernia Inguino-pubic hernia Inguino-scrotal henria

Clinical signs w Common signs for all hernia w Digital exploration through the superficial orifice – Evaluation of the defect – Relations with the epigastric vessels = variety of hernia

Differential diagnosis w Uncomplicated interstitial hernia – Ectopic testis – Cysts of the spermatic cord – Solid tumors w Uncomplicated inguino-pubic hernia – Crural hernia (line of Malgagine) – Lypoma of labia major – Cyst of the Nuck canal w Inguino-scrotal hernia – Hydrocel – Varicocel – Testicular tumors

Direct inguinal hernia w A weak point hernia w The area of weakness is the middle inguinal area (between the epigastric artery and remnant of the umbilical artery) w Sac is completely separated from the spermatic cord which is pushed away

Particularities w Frequently in older people, associated with other hernias w Frequently bilateral w Generally small and do not descend in the scrotum, trajectory being perpendicular on the inguinal ligament. w Defect is large – unlikely to produce comlications
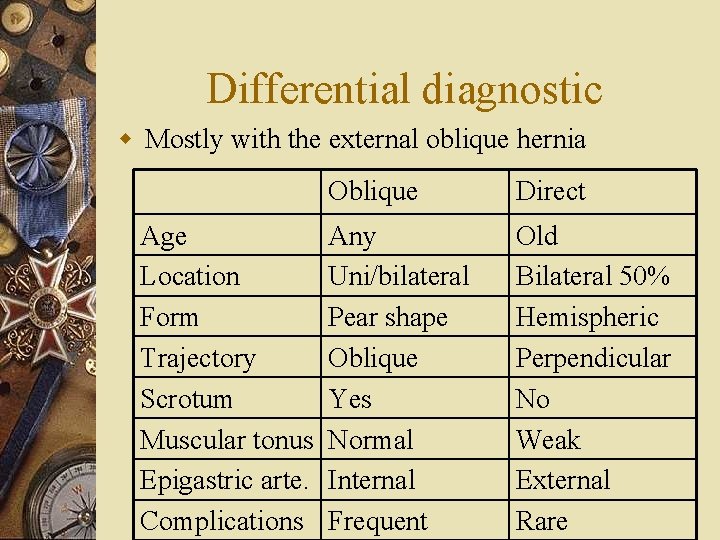
Differential diagnostic w Mostly with the external oblique hernia Age Location Form Trajectory Scrotum Muscular tonus Epigastric arte. Complications Oblique Direct Any Uni/bilateral Pear shape Oblique Yes Normal Internal Frequent Old Bilateral 50% Hemispheric Perpendicular No Weak External Rare

Treatment of Inguinal Hernia w Objectives: – Resection of the hernia sac – Treatment of the defect – a solid wall to prevent hernia recurrence LARGE VARIETY OF TECHNIQUES
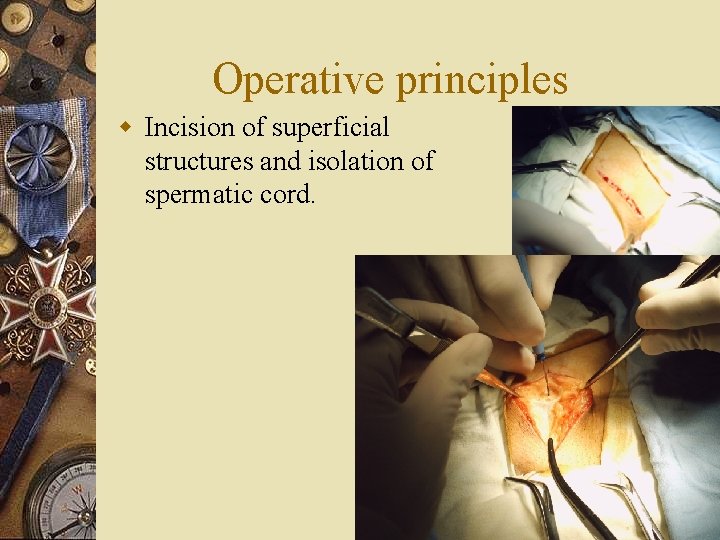
Operative principles w Incision of superficial structures and isolation of spermatic cord.
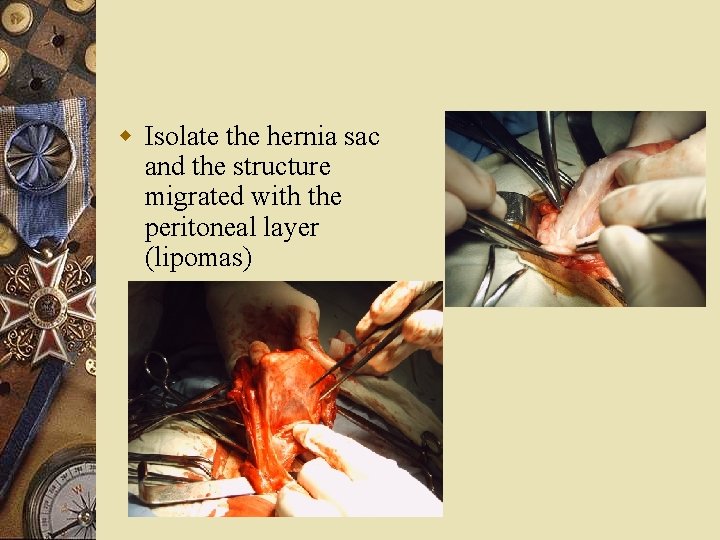
w Isolate the hernia sac and the structure migrated with the peritoneal layer (lipomas)
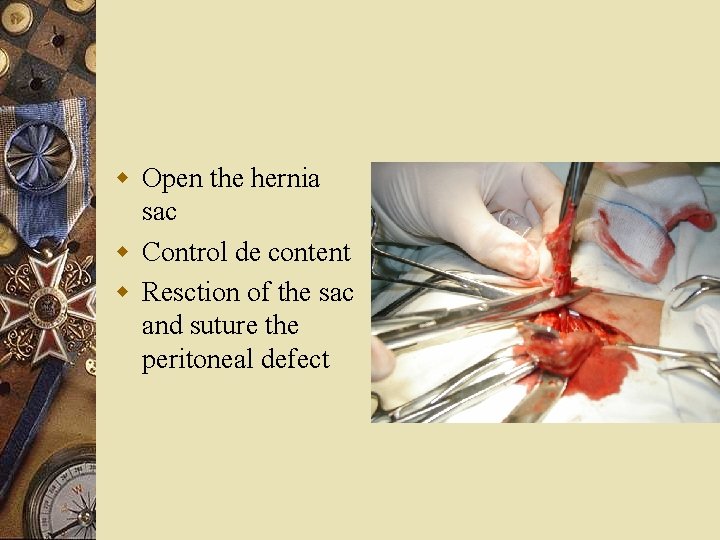
w Open the hernia sac w Control de content w Resction of the sac and suture the peritoneal defect

Posterior wall repair w GOAL – prevent recurrences w “Anatomical” procedures – Behind the spermatic cord (Bassini, Shouldice, Mc. Vay) – In front of the spermatic cord (Kimbarowski, Forgue) w Procedures that use a synthetic structure (mesh repair) – respect the principle of tension-free repair.
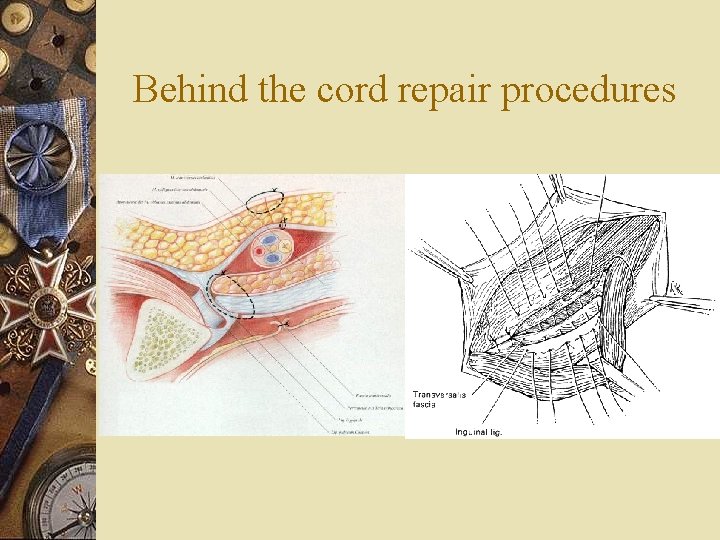
Behind the cord repair procedures
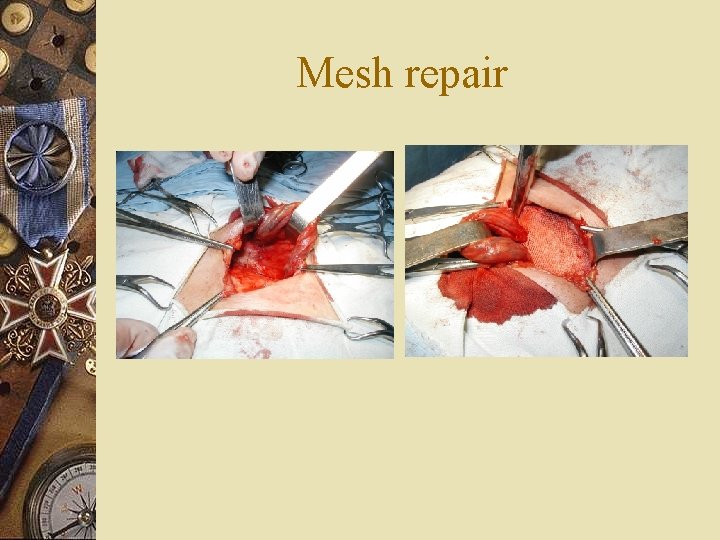
Mesh repair
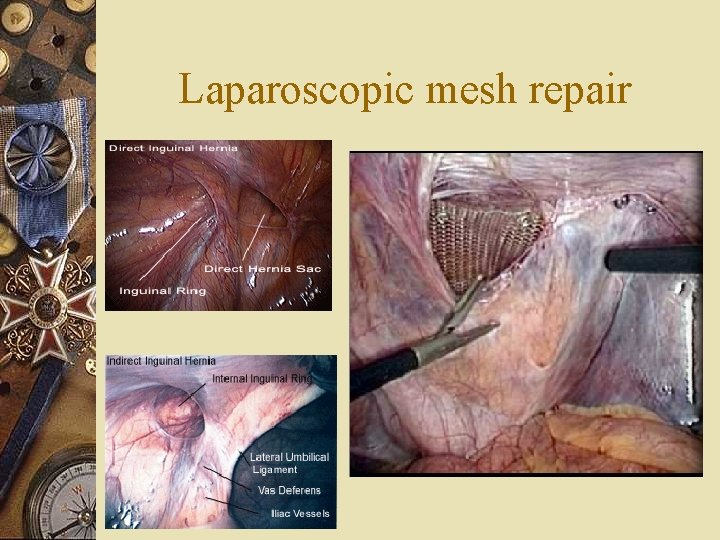
Laparoscopic mesh repair
Orthopedic treatment w ONLY when the patient refuses operations or major contraindication for surgical repair

Femoral hernia
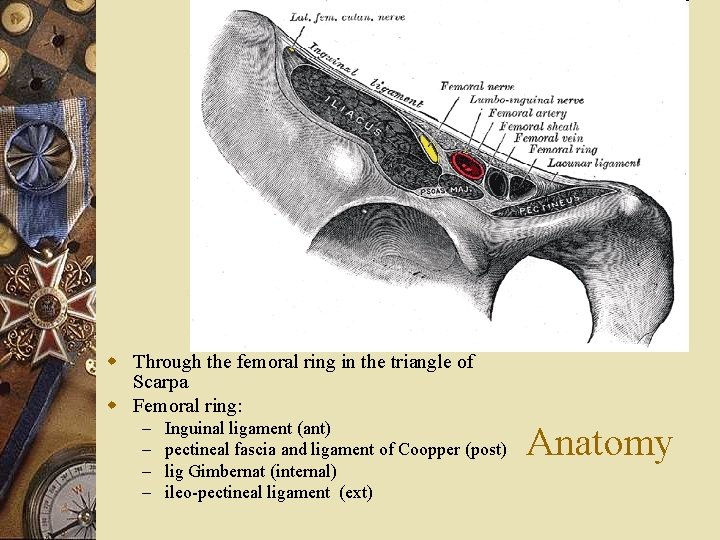
w Through the femoral ring in the triangle of Scarpa w Femoral ring: – – Inguinal ligament (ant) pectineal fascia and ligament of Coopper (post) lig Gimbernat (internal) ileo-pectineal ligament (ext) Anatomy

Variants – Herniation point – incomplete (under the cribriform fascia) – complete w Prevascular, retrovascular, external w Laugier (through the fibers of the ligament of Gimbernat) w Femuro-pectineal (under the pectineal fascia) w Multi-divericular w In combination with inguinal hernia – distension of the groin

Higher incidence in women w 4 x more frequent in women w Diameter of the pelvic girdle is larger w Accentuated lordosis in lumbar area w Pregnancies: weakens the abdominal wall + sustained increase in intraabdominal pressure
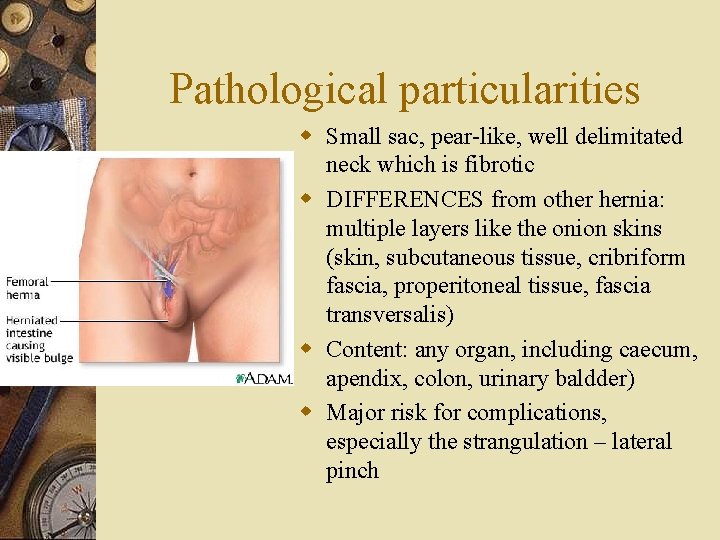
Pathological particularities w Small sac, pear-like, well delimitated neck which is fibrotic w DIFFERENCES from other hernia: multiple layers like the onion skins (skin, subcutaneous tissue, cribriform fascia, properitoneal tissue, fascia transversalis) w Content: any organ, including caecum, apendix, colon, urinary baldder) w Major risk for complications, especially the strangulation – lateral pinch

Clinical signs - particularities w Few or no functional signs: little pain or heaviness in the groin or during extension of the hip. w +/- digestive symptoms (colicky pain, urinary symptoms) more often believed to have another source TYPICALLY the signs indicate and abdominal suffering and the physician does not explore the groin

Clinical examination w Small pseudo-tumor in the Scarpa triangle , most typical medial to the femoral vessels. INCONSTANT w Round or oval shape w Prolonged under the inguinal ligament – if the tumor can be felt w Frequently obese patients with lare subcutaneous fat layer

Clinical examination w Consistency is elastic or granular – atypical for a hernia w IREDUCIBLE but not associated with a loud symptomatology in the groin w IMPULSION AND EXPANSION are either absent or faint w High percentage are complicated at presentation
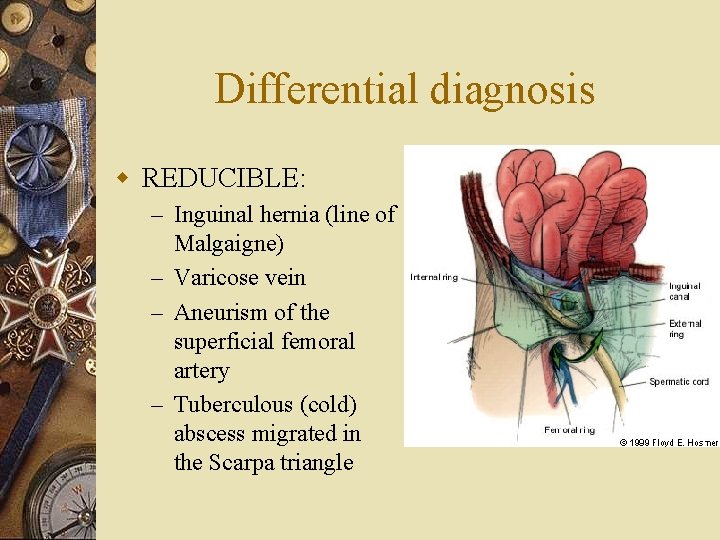
Differential diagnosis w REDUCIBLE: – Inguinal hernia (line of Malgaigne) – Varicose vein – Aneurism of the superficial femoral artery – Tuberculous (cold) abscess migrated in the Scarpa triangle
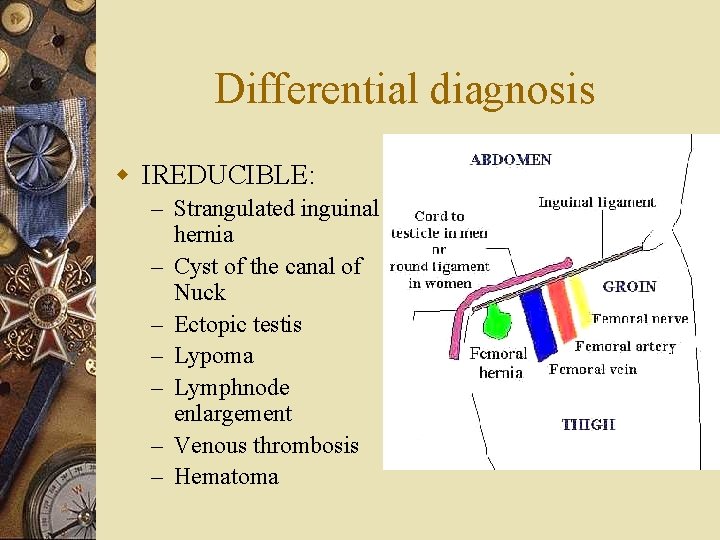
Differential diagnosis w IREDUCIBLE: – Strangulated inguinal hernia – Cyst of the canal of Nuck – Ectopic testis – Lypoma – Lymphnode enlargement – Venous thrombosis – Hematoma
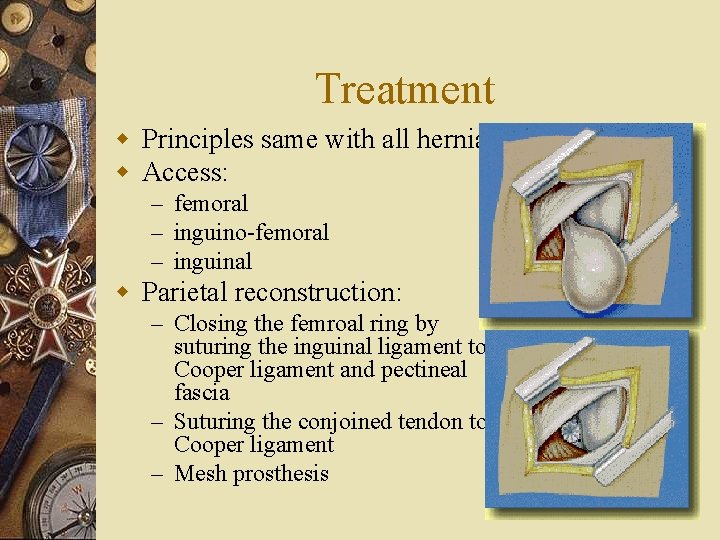
Treatment w Principles same with all hernia w Access: – femoral – inguino-femoral – inguinal w Parietal reconstruction: – Closing the femroal ring by suturing the inguinal ligament to Cooper ligament and pectineal fascia – Suturing the conjoined tendon to Cooper ligament – Mesh prosthesis
Umbilical hernia

A. Congenital w Failure in the development of the abdominal wall – Embryonic form (defect appears before the 3 rd month and organs are not covered by peritoneum – not real hernia – Fetal form – covered by peritoneum

Pathology w Translucent covering (displastic wall) without vessels and muscles w You can see abdominal viscera through the wall. Content can be as much as the whole abdominal content
Clinical aspects w Large ventral tumor, present at birth and surrounded by a skin ring w Transparent wall: abdominal viscera EVOLUTION: spontaneous rupture + death TRATAMENT: surgical - small defects: as in hernia - large defects: skin flaps +/- serial operations
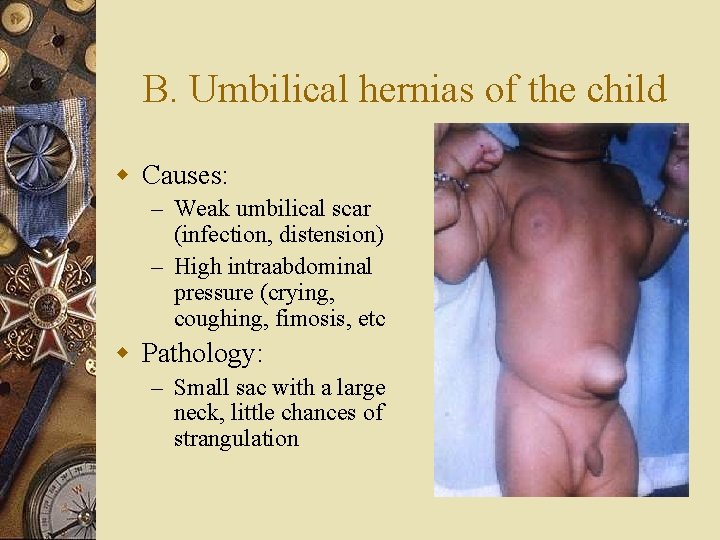
B. Umbilical hernias of the child w Causes: – Weak umbilical scar (infection, distension) – High intraabdominal pressure (crying, coughing, fimosis, etc w Pathology: – Small sac with a large neck, little chances of strangulation

Treatment w Conservative: if – Less then 2 years – Less then 2 cm diameter • Has to be maintained reduced via a skin fold until spontaneous closure w Surgical: – Resection of the sac – Parietal repair
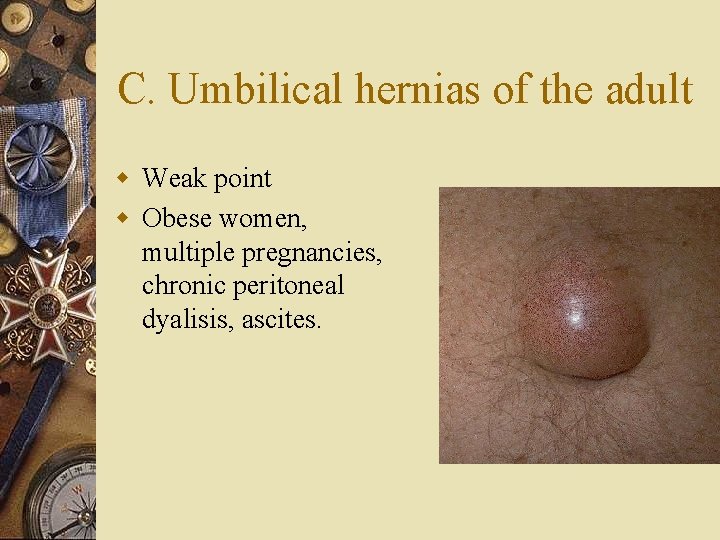
C. Umbilical hernias of the adult w Weak point w Obese women, multiple pregnancies, chronic peritoneal dyalisis, ascites.

Particularities w Direct herniation most typically (indirect machanism is possible if the ring is asymmetrically positioned) w Sac initially small may become multidiverticular + changes generated by the degenration of the sac by expnasion w Rigid neck – strangulation factor w Content: most frequent properitoneal fat, but viscus can migrate as well

Clinical signs w Pain on effort +/- digestive symptoms w Typical signs of hernia with a major tendency to become irreducible w If palpation of the ring is possible – large, round, rigid defect

Complications w Strangulation (rigid ring, with rapid progression to necrosis) w Progressive enlargement – irreducible and loosing the right to stay in the abdominal cavity

Treatment w Surgical: – Omfalectomy and treatment of hernia – Techniques that conserve the umbilical scar (subcutaneous dissection) – Plastic surgery
Epigastric hernias

Particularities w Supraumbilical median line w Frequent multiple hernias w At the crossing of fibers in the linea alba w Small, irreducible and containing mostly properitoneal fat w One particular form – diastases of the rectus sheat w Symptomatic hernia require treatment

Ventro-lateral hernia Spiegel

Particularities w Anatomic: defect in the ventro-lateral abdominal wall where vessels pass subctaneous. (lateral to the rectus sheat) w Hernia pushes the fascia of the external oblique muscle (interstitial form) or overpasses is (complete form)

Particularities w Clinical: pain + abdominal deformity w Dg: in interstitial forms sometimes no signs. Positive dg by US scan w Rsik of becoming irreducible or strangulated w Surgical treatment like any hernia

UNUSUAL HERNIA

Lumbar hernia w Pposterior wall (triangle of J. L. Petit – G. oblique, G. dorsal, iliac bone) or Grynfeld qudrate space (C 12 with small dentate muscle, paravertebral muscles, small oblique and lumbar quadrat) – extraperitoneal – paraperitoneal – peritoneal

Other forms w Obturator w Perineal w Hiatus w Internal w Ischiatic

Postoperative hernia

Generalities w HERNIAS = peritoneal diverticulum under the skin + defect developed postraumatic w EVISCERATIONS = posttraumatic wall defect without a peritoneal covering

Ethiology w Posttraumatic or postoperative w Causes that favor postoperative hernia Old age – scaring abnormalities Co-morbidities (liver cirrhosis, cancer diabetes) Obesity Type of incision Postoperative infection Increased intraabdominal pressure developed postoperative – Not adequate suture material – – –
Pathology w Abdominal wall defect – variable in diameter, frequently multiple, situated under the skin scar w Hernia sac: thickened peritoneum, multidiverticular, frequently under the skin in contact with it w Visceral content

Clinical examination w Pseudo-tumor with all characters of hernia w Related with the scar w Diemension and number of parietal defects w Reducible or irreducible w Skin overlaying the hernia

Treatment w Evisceration: urgent, viscus should be placed back in the abdomen and skin should be closed w Postoperative hernia: complex treatment preferably elective
- Slides: 66