HEPATITIS VIRUSES Part 2 Pathogenesis of HBV Infections

HEPATITIS VIRUSES Part 2

Pathogenesis of HBV Infections • HBV is transmitted only in blood and body fluids • Replication starts in the hepatocytes, “the only host cells” • HBs. Ag particles are liberated into blood stream, “they are not infective” • Dane particles “complete virion” are so numerous, up to 1010/ml, 0. 001 ml of blood can transmit infection • Incubation period 50 -180 days • Liver injury may be due to cellular immune response directed toward the new antigens deposited in the cell membrane of infected cells 2

Pathogenesis of HBV Infections 1. Acute Infection • Follows initial infection and is characterized by a high rate of viral replication. • Damage to liver cells which results in: • high blood concentration of liver enzymes • and the obstruction of small bile tubes due to inflammation leads to the development of jaundice. • In severe cases liver function may be so damaged that clotting is impaired or hepatic encephalopathy develops. This is referred to as acute fulminant hepatitis. 3

Pathogenesis of HBV Infections • Percentage of acute infection that will not be cleared and become chronic infection: • • • Between 1% and 4% of adults, about 70– 80% of infants and children, and 90% of neonates 40% of hemodialysis patients and up to 20% of patients with immune deficiencies. 4

Pathogenesis of HBV Infections 2. Chronic infections • Chronic HBV infection is defined as HBV infection lasting longer than 6 months. • It includes a spectrum from chronic asymptomatic carrier state to chronic active hepatitis with rapid progression to cirrhosis. a) Chronic persistent (carriers): • are often asymptomatic and may not be aware that they are infected; • they are capable of infecting others • no anti HBs. Ag “antibodies” • “mild degree of liver damage” 5

Pathogenesis of HBV Infections b) Chronic active hepatitis: • develops in more than 25% of carriers and often results in cirrhosis • Significant damage to the liver • Patients at risk may develop cirrhosis or hepatocellular carcinoma which arises as a result of integration of viral genome into the DNA of the hepatocytes. 6

Laboratory Diagnosis • HBV infection cannot be differentiated on the basis of clinical symptoms alone, and definitive diagnosis depends on the results of serologic testing • Serologic markers of HBV infection vary depending on whether the infection is acute or chronic. • Liver function tests, abnormally elevated “transaminases, bilirubin, alkaline phosphatase, LDH” • The presence of HBs. Ag confirms diagnosis, tested by ELISA, PCR, RIA • Liver biopsy 7

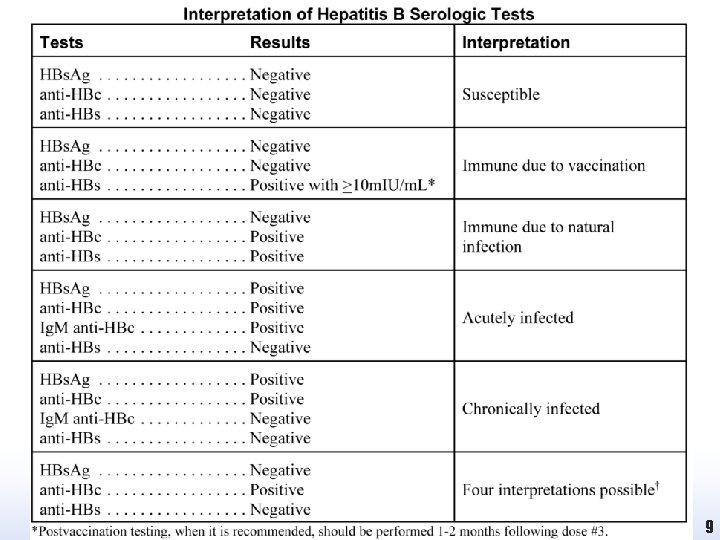
Laboratory Diagnosis • HBs. Ag is the most commonly used test for diagnosing acute HBV infections or detecting carriers. • HBs. Ag can be detected as early as 1 or 2 weeks and as late as 11 or 12 weeks after exposure to HBV when sensitive assays are used. • The presence of HBs. Ag indicates that a person is infectious, regardless of whether the infection is acute or chronic. 8
9

Laboratory Diagnosis 1. May be recovering from acute HBV infection 2. May be distantly immune and the test is not sensitive enough to detect a very low level of anti-HBs in serum 3. May be susceptible with a false positive anti-HBc 4. May be chronically infected and have an undetectable level of HBs. Ag present in the serum 10

Control of HBV Infections • Blocking of person-to-person transmission, prevent blood or body fluids of infected persons gaining access to the circulation of someone else. • Active immunization with HBs. Ag obtained by recombinant DNA technology (in yeast) for high-risk groups and infants or plasma derived vaccine. • Passive immunization: Human immunoglobulin with a high titer of anti-HBs (HBIg: hepatitis B immunoglobulin), which gives immediate passive protection, should be given with active vaccine. • HBIg is given for healthcare staff who suffer “needle-stick”. 11

Treatment • Two major groups of antiviral treatment have been licensed for the treatment of chronic HBV infection in many countries. • These include interferon alpha (IFNa, or PEG-IFNa) and nucleoside or nucleotide analogues such as lamivudine. 12

Hepatitis C • • It belongs to Flaviviridae family genus hepacivirus HCV diameter is 50 nm Icosahedral symmetry, Enveloped Positive single stranded RNA There are 6 major genotypes (1 -6) HCV has 2 envelope glycoproteins; E 1 and E 2, two transmembrane proteins; NS 1 and NS 2 in addition to RNA polymerase (NS 5 B) and interferon resistance protein(NS 5 A) • HCV has a high mutation rate • HCV has high rate of replication, one trillion particles per day • Transmission is similar to HBV 13

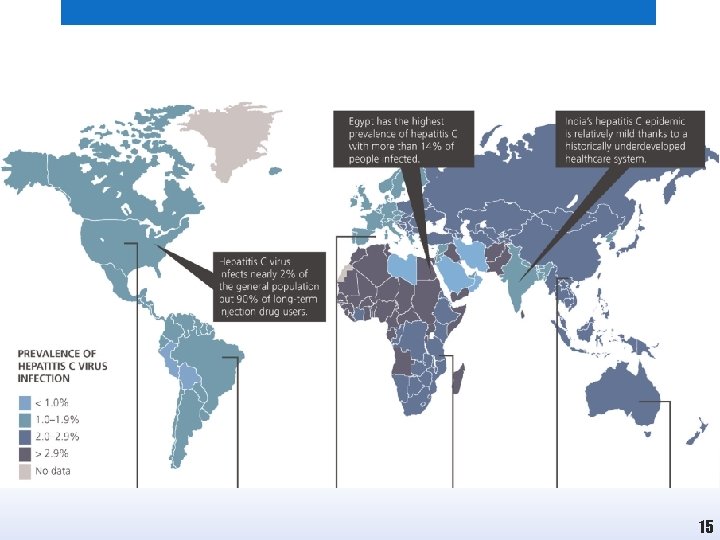
Epidemiology • Incubation period: 2 -26 weeks • An estimated 170 million people are infected worldwide with HCV. • About 2 -3 million people are infected per year • Co-infection with HIV is common • HCV is considered to be the most common cause of post - transfusion hepatitis. 14
15

Pathogenesis 1. Acute hepatitis C • It refers to the first 6 months after infection with HCV. • Between 60 -70% of infected people develop no symptoms during the acute phase. • Symptoms include decreased appetite, fatigue, abdominal pain, jaundice and itching. • HCV is detected in blood within 1 -3 weeks after infection using PCR technique. • Antibodies are detectable within 3 -15 weeks. • Viral clearance rates are highly variable, 10 -60% of infected persons clear the virus during the acute phase as shown by normal liver enzymes. • Most patients develop chronic infection lasting more than 6 months 16

Pathogenesis 2. Chronic hepatitis C • It is often asymptomatic. • One third of patients progress to liver cirrhosis in less than 20 years, others may develop liver cancer. 17

Treatment • IFN-α-2 a injection • Ribavirin tablets (a purine nucleoside analogue), it inhibits viral RNA polymerase, it may cause shift of TH 2 into TH 1. • Treatment may last for 24 -48 weeks depending on HCV genotype. • Vaccination against HAV and HBV is strongly recommended, as infection with a second virus could worsen their liver disease. • No vaccine against HCV is available. • Alcoholic beverages consumption accelerates HCV associated cirrhosis and makes liver cancer more likely. • Smoking may have the same effect. • Amantadine may be effective in combination with IFN-α and Ribavirin. • HCV resistant strains develop against IFN-α and/or Ribavirin 18

Laboratory Diagnosis • Liver enzymes increased (ALT in particular) • PCR • Used to diagnose HCV in the acute phase • To monitor the response to antiviral therapy • Anti HCV antibodies • Genotyping is recommended to determine the length and potential response to IFN-α. 19

Delta Agent (HDV) • • Incomplete RNA virus HBV-dependent “for replication” It may be transmitted along with HBV May be detected in hepatocyte nuclei of patients with chronic HBV infection • Its outer coat is formed from HBs. Ag • It uses HBV S antigen to provide the protein for its envelope and thus HDV can only replicate and spread within HBVinfected individuals. • Recovery is usually complete and development of chronic hepatitis D is rare (less than 5% of acute hepatitis). 20

Laboratory Diagnosis • Diagnosis of the active infection depends on detecting the delta antigen or its Ig. M antibody in the blood • Immunization against HBV also protects against infection with delta agent 21

Hepatitis E Virus “HEV” • • RNA(+), single stranded. Icosahedral symmetry, nonenveloped. Size: 27 -34 nm. HEV has one serotype and 4 genotypes. • Genotypes 1 and 2 are restricted to humans. • Genotypes 3 and 4 infect humans, pigs and other animal species. • In addition an avian virus has been described which causes hepatitisspleenomegaly syndrome in chickens. • • • Spread via fecal-oral route Clinically, it is comparable to HAV. HEV causes severe infection in pregnant women. Incubation-period 2 -7 weeks A vaccine has been developed recently which is based on recombinant viral proteins, (registered in China). 22

Laboratory Diagnosis • Definitive diagnosis of hepatitis E infection is usually based on the detection of specific Ig. M antibodies to the virus in a person’s blood; this is usually adequate in areas where disease is common. • Additional tests include reverse transcriptase polymerase chain reaction (RT-PCR) to detect the hepatitis E virus RNA in blood and/or stool. • This test is particularly needed in areas where hepatitis E is infrequent, and in cases with chronic HEV infection. 23
- Slides: 23