Hepatic Encephalopathy Presented by Mohannad A Almikhlafi Ahmed

Hepatic Encephalopathy Presented by: Mohannad A. Almikhlafi Ahmed M. Aljabri Supervised by: Prof. Dr. Mahmood Abdulmenem
Key Points • • Epidemiology & definition Etiology Pathogenesis Stages of H. E. Sign and Symptoms Diagnosis Ascites Case presentation
Epidemiology v. Cirrhosis affects 3. 6 per 1000 adults in the United States and is responsible for 26, 000 deaths per year. v. Chronic liver disease represents the fourth leading cause of deaths among all races and sexes in the 45 to 54 -year-old age group, exceeded only by malignancy, heart disease, and accidents.
Definition It is a neuropsychiatric disturbances caused by liver disease.
Pathogenesis • HE is due to cerebral intoxication by nitrogenous compounds produced by bacteria in GIT. • Several nitrogenous compounds have been implicated as causes of HE : they include ammonia , false transmitters & fatty acids.
Pathogenesis • In the presence of poor hepatocellular function , nitrogenous compound in the portal venous blood pass in to the systemic circulation with out being metabolized by the liver, & cross BBB.
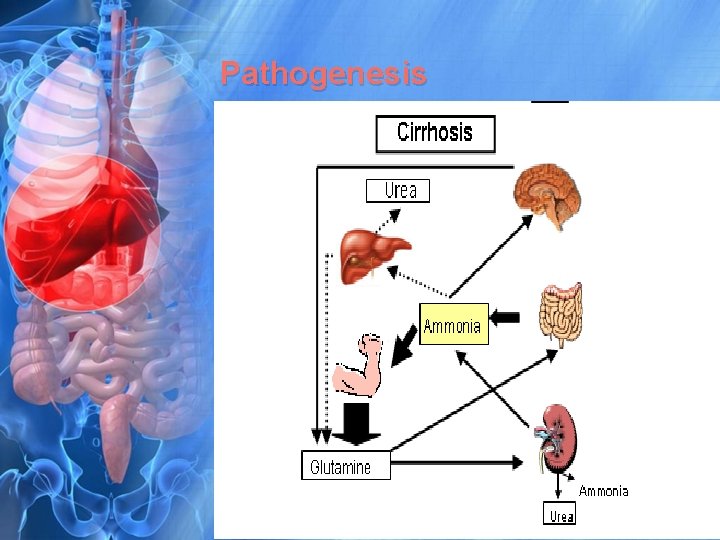
Pathogenesis

Precipitaiting factors § § § § Infections Constipation GIT bleeding Excess protein intake Hypokalemia, Metabolic-alkalosis (vomiting, diarrhea , dehydration) Azotemia Drugs ( Diuretic, sedative , hypnotic) Renal failure.
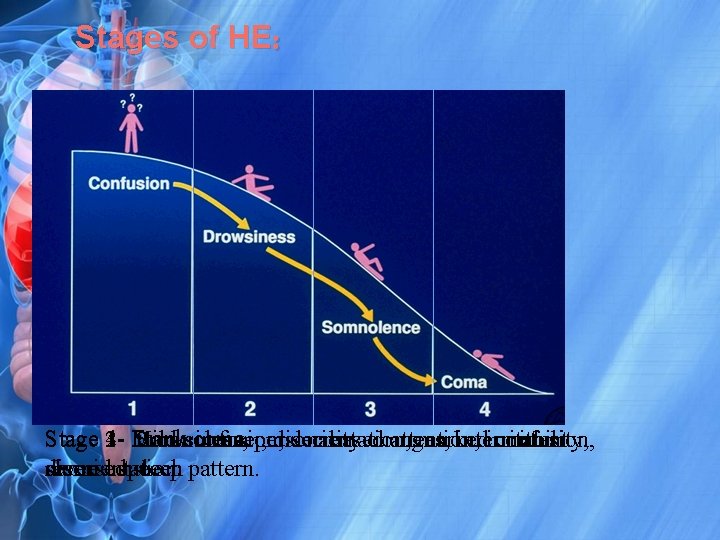
Stages of HE: Stage 4 coma personality 1 - Frank 23 Mild Drowsiness, Somnolence confusion, , disorientation, decreased changes, attention, marked intermittent irritability, confusion, reversedspeech disorientation slurred sleep pattern.
Sign and Symptom Some of the following signs and symptoms may occur in the presence of cirrhosis or as a result of the complications of cirrhosis: • Abdominal swelling. • Nausea , vomiting. • Dark urine. • Sleep disturbances.
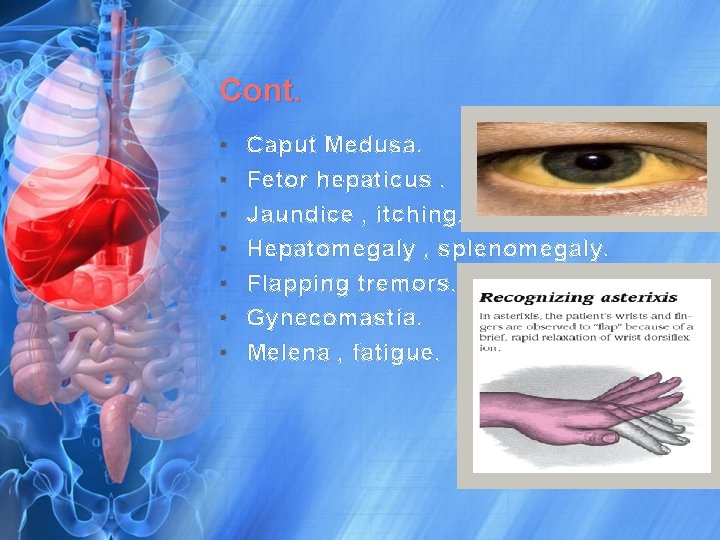
Cont. • • Caput Medusa. Fetor hepaticus. Jaundice , itching. Hepatomegaly , splenomegaly. Flapping tremors. Gynecomastia. Melena , fatigue.
Diagnosis • Laboratory: CBC, LFT, Kidney function, serum electrolyte. • Radiology. • Liver biopsy.
Laboratory tests 1 - Hypoalbuminemia 2 - Elevated prothrombin time 3 - Thrombocytopenia 4 - Elevated alkaline phosphates 5 - Elevated aspartate transaminase (AST) alanine transaminase (ALT) 6 - Elevated glutamyl transpeptidase (GGT)
• Radiology • X-ray , CT, US & radioisotope scan. • biopsy • Definitive diagnosis depend on biopsy & microscopic interpretation.
Ascites • Is the pathologic accumulation of lymph fluid within the peritoneal cavity. • It is one of the earliest and most common presentations of cirrhosis. • Spontaneous bacterial peritonitis (SBP) may occur & have a high mortality rate.
Cont. It is due to : • Portal hypertension. • Hypoalbuminemia (due to failure of liver to form plasma protein). • Hyperaldosteronism (due to failure of liver to inactivation of aldosterone).
Precipitating factors: • ↑Protein load in the intestine(↑protein intake, Constipation & GIT bleeding) • Electrolyte disturbance(hypokalemiametabolic alkalosis) • Dehydration • CNS depressant drugs(hypnotics , opioids &sedatives)
Management Of HE
Goal of therapy Ø To reduce nitrogen load in the GIT Ø To correct any metabolic or electrolyte disturbance that may arise.
1. Lactulose: o o o Inhibit intestinal bacteria absorption of nitrogenous waste product Laxative effect to remove nitrogenous wastes. Dose: 20 -60 ml 3 times/day, Titrated to achieve 2 -4 soft stools / day without diarrhea.
o Maximum laxative effect appear at 2 -4 days Enema should be used during the initial 2 days SE: Flatulence , Diarrhea , dehydration, Gaseous distention.
2. Antibiotics: • Neomycin – 1 g/6 hrs – SE: ototoxicity and nephrotoxicity • Metronidazole – 400 mg /6 hrs – SE: Headache, ataxia, pancreatitis.
Contraindicated Drugs • Execs diuretic • Sedative & hypnotic drugs • Drug have toxic effect on the liver
Parameters used to monitor Therapeutic effect: 1 -Biochemical parameters: Serum ammonia Serum electrolyte levels BUN 2 -Clinical parameters: Improvement of symptoms & physical signs of HE

Management Of Ascites
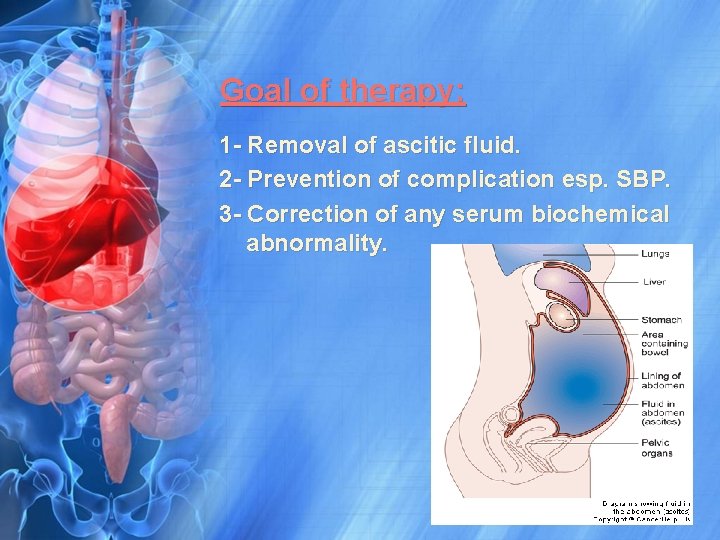
Goal of therapy: 1 - Removal of ascitic fluid. 2 - Prevention of complication esp. SBP. 3 - Correction of any serum biochemical abnormality.
Lines of Therapy A- Rest with restriction of sodium (only 2 g/d) - Serum biochemical analysis determine if fluid restriction is needed. - Restriction of water should be done if hyponatremia is present.

B- Diuretics: Diuresis should be gradual because hypokalemia or intravascular volume depletion caused by aggressive therapy compromised renal function, and hepatic encephalopathy.
Patients have increased serum aldosterone due to: -Increased production due to decreased intravascular volume and decreased renal perfusion Activation of RAAS. -Decreased excretion due to hepatic impairment decreased metabolism.
1 - Spironolactone: Block aldosterone redeptors. Indication: Diuretic of choice in treatment of ascites and edema due to liver cirrhosis. Dose: 100 -400 mg once daily. Dose Adjusted after 2 days at least because maximum effect is after 2 -4 days.
Adjusted according to: -Clinical parameters effective dose decreases weight by 0. 5 kg/d (if ascites) and 1 kg/d (if ascites and lower limb edema). -Biochemical parameters hyperkalemia, hyponatremia, urea and creatinine to avoid renal impairment
Precautions: • Hyperkalemia continuous serum potassium monitoring. • Urea and creatinine should be measured because spironolactone is contraindicated in renal failure.
2 - Furosemide: • If spironolactone was inadequate or no response or appearance of side effects, furosemide (20 -40 mg/d) is added. • We start with both in initial doses and increase dose by same rate.
C- Antibiotics: • Third generation cephalosporin e. g. cefotaxime 1 g/12 hr IV for 1 week. • Quinolones e. g. oral Ofloxacin or norfloxacin 400 mg BID for 1 week.
D- Paracentesis: • Which is removal of ascitis fluid (4 - 6 L) from the abdominal cavity with a needle or catheter. • Indicated in tense ascites. • Fluid is rich in albumin for every 1 L removed give 6 -8 g albumin.
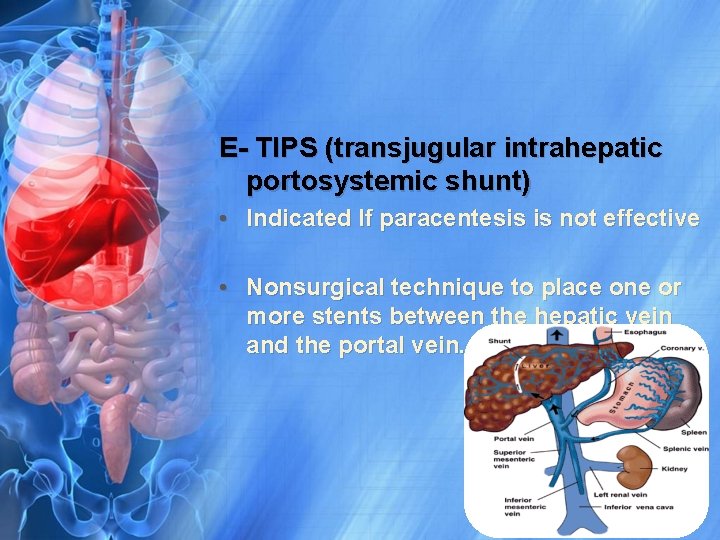
E- TIPS (transjugular intrahepatic portosystemic shunt) • Indicated If paracentesis is not effective • Nonsurgical technique to place one or more stents between the hepatic vein and the portal vein.
Case presentation

I. A. is a 62 years old Egyptian male admitted to ED of KAUH on 13 May, 2009. Confusion since today morning, disorientation, lethargy, abdominal pain, constipation.
• Past medical history: DM ( on OHG agent), CLD(LC, Hematemesis), HCV, HBV, Portal hypertension, post spleenoctomy, esophagitis. • Family history: No family history of similar condition.
• Home medications: o Glimepiride 3 mg PO OD o Metformin 500 mg PO BID Furosemide 40 mg PO OD Lactulose 30 m. L PO TID ( D/C 4 days before admission) • Diagnosis: Hepatic encephalopathy
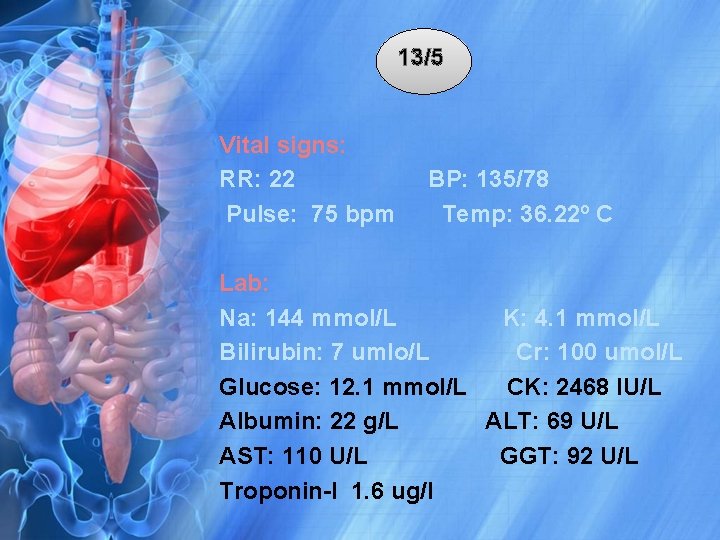
13/5 Vital signs: RR: 22 Pulse: 75 bpm BP: 135/78 Temp: 36. 22º C Lab: Na: 144 mmol/L K: 4. 1 mmol/L Bilirubin: 7 umlo/L Cr: 100 umol/L Glucose: 12. 1 mmol/L CK: 2468 IU/L Albumin: 22 g/L ALT: 69 U/L AST: 110 U/L GGT: 92 U/L Troponin-I 1. 6 ug/l
Examination: o General condition: Disorientation & Confusion o Skin: No jaundice, no skin rash o CVS: S 1 + S 2 + 0 o CNS: Normal reflexes, flapping tremors o Chest: Bilateral basal crepitation o Abdomen: Distended, soft, lax, hepatomegally, mild ascitits
PLAN Lab: CBC, LFT, PT, APTT, U&E, PCR HBV DNA & HCV RNA. Medications: Furosemide 40 IV BID Lactulose 30 m. L PO TID Lactulose enema 300 m. L PR OD Ceftriaxone 2 gm IV OD Insulin sliding scale S. C Q 6 hr Ornithine (hepamerz®)1 Sachet
14/5 • Currently ptn is conscious, oriented, free of pain, no abdominal pain, no tenderness, no melena, mild ascites. • Normal vital signs Propranolol 10 mg PO BID Albumin 100 m. L IV OD for 2 days Omeprazol 40 mg PO OD
16/5 Patient is stable, conscious, oriented. Plan: D/C Ceftriaxone, ISS Adjustment for Lactulose frequency TID QID & for Furosemide route of administration IV PO Glimepiride 3 mg PO OD Metformin 500 mg PO BID Discharge tomorrow
17/5 • Patient was discharged. • Discharge medications: o o o Omeprazole 20 mg PO OD Propranolol 20 mg BID Lactulose 30 m. L PO QID Glimepiride 3 mg PO OD Metformin 500 mg PO BID
Assessment o Furosemide is not prefer because of: Potent & rapid acting (ptn had mild ascites) hypovolemia aggravate HE SE: hypokalemia (metabolic alkalosis) • Spironolactone is the drug of choice for ascites (mild diuresis, antagonize aldosterone) starting with 100 mg OD titrated to 300 mg/day if no response.
• Norfloxacin is the prophylactic drug of choice for SBP. • Lactulose effect will start after 2 -3 days, so, giving lactulose enema is a good decision.
• Therapeutic dose of Lactulose is the dose that produce 4 soft stool without diarrhea. • The right Propranolol dose is the dose that decrease pulse baseline by 25% (but not ˂ 60 bpm).
• Diuretics and beta-blockers may increase the risk of hyperglycemia so, carful monitoring for blood sugar level. • Beta-blockers may mask symptoms of hypoglycemia such as tremors and tachycardia, other symptoms: headache, dizziness, drowsiness, nausea, hunger, and sweating may be unaffected.
• Laxatives can cause significant losses of fluid and electrolytes, including Na, K, Mg and zinc, that may be additive to those of diuretics, so carful monitoring for these parameters & any signs of fluid & electrolyte depletion. • Most complaints about lactulose are nausea (due to sweet taste of the drug), diarrhea, flatulence.
THANKS
Reference • http: //www. nlm. nih. gov/medlineplus/en cy/article/000302. htm • http: //emedicine. medscape. com/article/ 186101 -overview • http: //www. gastroresource. com/gitextb ook/en/chapter 14/14 -13. htm • http: //www. umm. edu/ency/article/00030 2. htm
- Slides: 53