Hepatic Encephalopathy Maybe Case Conference February 19 th

Hepatic Encephalopathy… Maybe? Case Conference February 19 th, 2013 Scott Laura

Chief Complaint • Confusion and worsening back pain for 2 weeks

HPI • 55 y. o. male with hx of HIV (CD 4 count 01/10 was 23: Below 200 since 2005), emphysema, Hep B and C, depression, Ao. CD, GERD, chronic back pain, who presents with confusion and back pain x 2 weeks that has progressively worsened. • Pt presented to ED under his own volition, with complaint of pain in his “bones and back” • Also reported minimal weakness.

HPI • Patient stated he had been confused since a female acquaintance stole his home prescription of morphine. – On chronic pain meds for LBP. • Unsure of cause • No previous mention in chart review – He was slow to answer questions and perseverating during exam. • Patient was noted to be removing IV access and agitated

Past Medical History • HIV with CD 4 of 23 and % of 4. 8 (1/10) • Pulmonary MAC – Diagnosed in 4/2010 treated with Clarithromycin, Ethambutol and Rifampin. • Smear negative 1/2011 x 1 – Followed by NO/AIDS and pulmonary (1 visit in 1/11) • • • Hep B and Hep C Emphysema Anemia of Chronic Disease Chronic low back pain Depression Poly-substance abuse

Past Surgical History • No Known Surgical Procedures – Per chart review

Medications • Morphine of unknown dosage/prescriber • Per Chart review Jan 2011 – – – Azithromycin 1200 mg weekly Bactrim DS 1 tab daily Ethambutol 400 mg 2. 5 tabs daily Clarithromycin 500 mg 2 tabs daily Rifabutin 150 mg 3 tabs daily Raltegravir 400 mg BID Abacavir/Lamivudine 600/300 mg daily Albuterol HFA 2 puffs q 4 -6 hours PRN: SOB/wheezing Tiatropium 18 mcg daily Fluoxetine 20 mg daily Ibuprofen 200 mg 1 -2 tabs q 8 hours PRN: pain Lansoprazole 30 mg daily

Allergies • IV Contrast: Anaphylaxis • Penicillins: Throat Swelling

Family History • Father passed away from unknown causes at 34 y/o. • Maternal grandfather died of mesothelioma at unknown age. • Mother unknown.

Social History • Per Chart Review – 80 year tobacco history – Denied current alcohol use – History of Heroin Use – unknown quantity/duration • • Heterosexual Incarcerated 3 years prior Has lived in homeless shelters in past Worked as a “boiler-maker” for ~10 yrs.

Health Maintenance • PCP with NO AIDS task force. • Unknown Flu, pneumo, tetanus. • No colonoscopy per records.

ROS Limited • Gen: No weight changes, fever or chills • HEENT: No visual changes, sore throat, rhinorrhea but + conjunctival erythema • CV: No chest pain, palpitations, SOB, DOE, orthopnea or PND • RESP: No cough, SOB • GI: No N/V/Diarrhea/melena/BRBPR, – + constipation • • Skin: No new rashes GU: Denied Dysuria or change in frequency Neuro: + for dizziness Musculoskeletal: Low back pain x 1 year acutely exacerbated 2 weeks prior

Physical Exam • Vitals – Triage • T 99. 1 BP 134/82 P 105 RR 19 O 2 100% on RA • 6’ 68 kg BMI 20 – Exam • T 98. 3 BP 121/68 P 90 RR 28 O 2 100% on RA

Physical Exam • GENERAL: – Thin, cachectic & dishelved. – Altered with slurred speech and difficult to understand. – Uncooperative with exam • HEENT: – – Normocephalic, atraumatic. MMM with no dentition. PERRL, EOMI, unable to assess optic nerve. No scleral icterus No obviously elevated JVP. • CARDIOVASCULAR: – Regular rate and rhythm. No murmurs, S 3 or S 4 noted • RESPIRATORY: – CTA however patient uncooperative with deep inspiration and palpation

Physical Exam • ABDOMEN: – Bowel sounds present. – Soft. Nontender. Nondistended. No organomegaly. – No rebound, guarding , shifting dullness, fluid wave, or caput medusa appreciated. • EXTREMITIES: – No clubbing, cyanosis, or edema. • Back: – Uncooperative with straight leg raise or range of motion. – Lumbar paraspinal muscle TTP • Skin: – Multiple tattoos • Some professional and multiple homemade. – No signs of telangiectasias

Physical Exam • NEUROLOGIC: – Mental: Oriented to self and place, not to time (day, month or year) – Sensation intact to light touch. – Reflexes unable to assess – Strength is 5/5 bilaterally in the upper and lower extremities. – Cerebellar function: Patient seen standing and ambulating on exam – CN II-XII: EOMI intact, PERRLA, sensation intact to light touch, raises eyebrows, closes eyes tight, symmetric faces

Physical Exam • NEUROLOGIC: – CN II • Not assessed – CNIII, IV, VI • EOMI intact and PERRLA B/L – CN V • Sensation intact to light touch B/L – CN VII • Raises eyebrows & closes eyes tight symmetrical B/L – CN VIII • Gross hearing intact – CN IX, X • Phonation and swallowing intact – CN XI • Not assessed secondary to being un-cooperative but moving shoulders and neck – CN XII • Tongue appeared mid-line
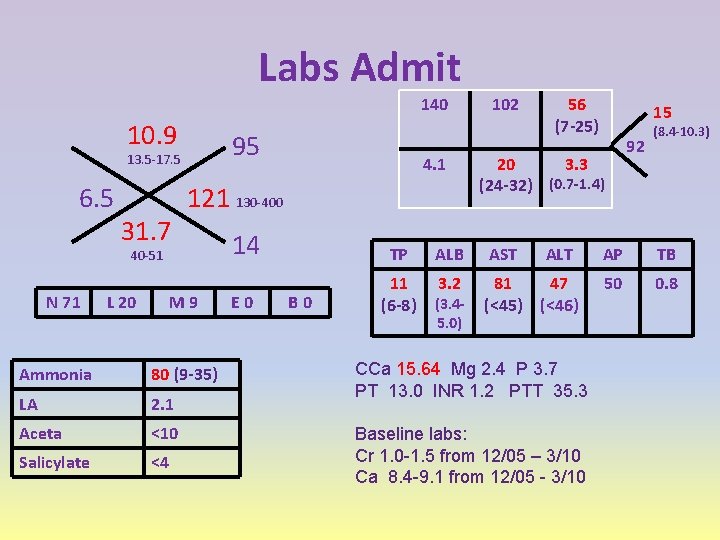
Labs Admit 140 10. 9 95 13. 5 -17. 5 6. 5 31. 7 121 130 -400 40 -51 N 71 L 20 4. 1 M 9 Ammonia 80 (9 -35) LA 2. 1 Aceta <10 Salicylate <4 102 56 (7 -25) 20 3. 3 (24 -32) (0. 7 -1. 4) 14 TP ALB AST E 0 11 (6 -8) 3. 2 81 47 (<45) (<46) B 0 (3. 45. 0) 15 ALT CCa 15. 64 Mg 2. 4 P 3. 7 PT 13. 0 INR 1. 2 PTT 35. 3 Baseline labs: Cr 1. 0 -1. 5 from 12/05 – 3/10 Ca 8. 4 -9. 1 from 12/05 - 3/10 92 (8. 4 -10. 3) AP TB 50 0. 8
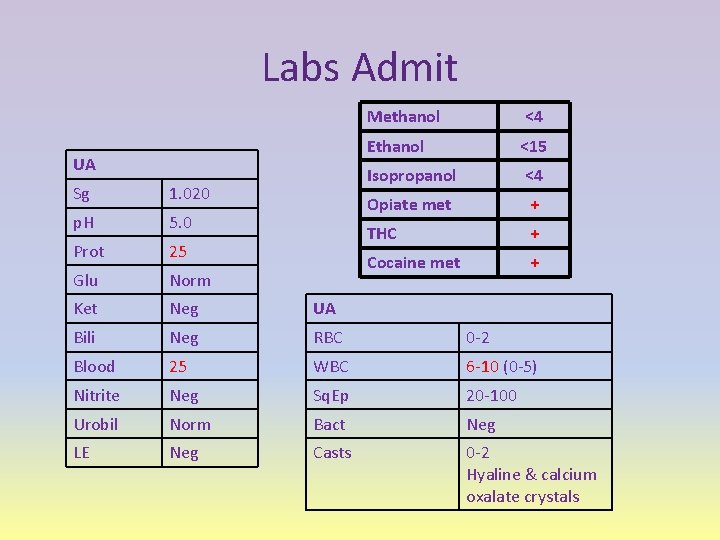
Labs Admit UA Methanol <4 Ethanol <15 Isopropanol <4 Opiate met + THC + Cocaine met + Sg 1. 020 p. H 5. 0 Prot 25 Glu Norm Ket Neg UA Bili Neg RBC 0 -2 Blood 25 WBC 6 -10 (0 -5) Nitrite Neg Sq. Ep 20 -100 Urobil Norm Bact Neg LE Neg Casts 0 -2 Hyaline & calcium oxalate crystals
CXR No acute abnormality identified

Hospital Coarse • Overnight/Day 1 – Underwent CT head W/O contrast – Patient received Ativan 2 mg for LP around midnight – Did not receive Lactulose – X ray of lumber spine • Multilevel degenerative changes in the spine with no significant interval change. – Urine: No organisms on smear – Upep/Spep Pending
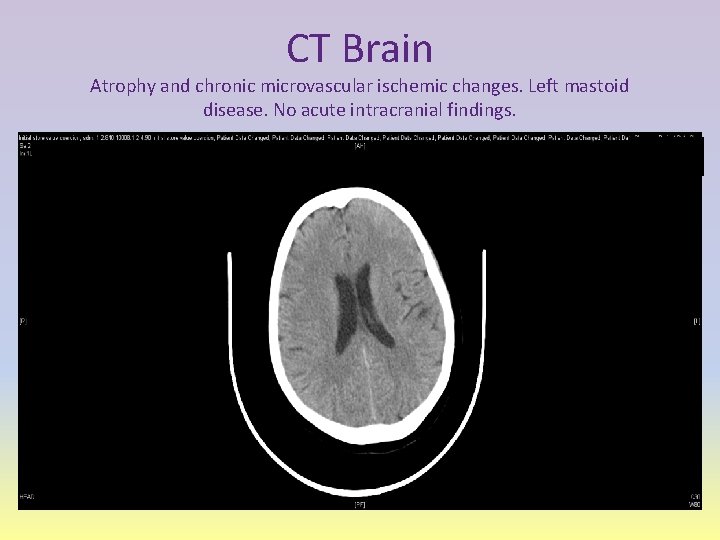
CT Brain Atrophy and chronic microvascular ischemic changes. Left mastoid disease. No acute intracranial findings.

Labs • LP (Tube 4) – CSF Clear – WBC 4 (differential not performed for <6) – RBC 12 (0 -5) – LDH 23 – Glucose 55 (40 -70) – Total Protein 40. 2 (15 -45) – Crypto Antigen Negative • Gram Stain: – No Organisms
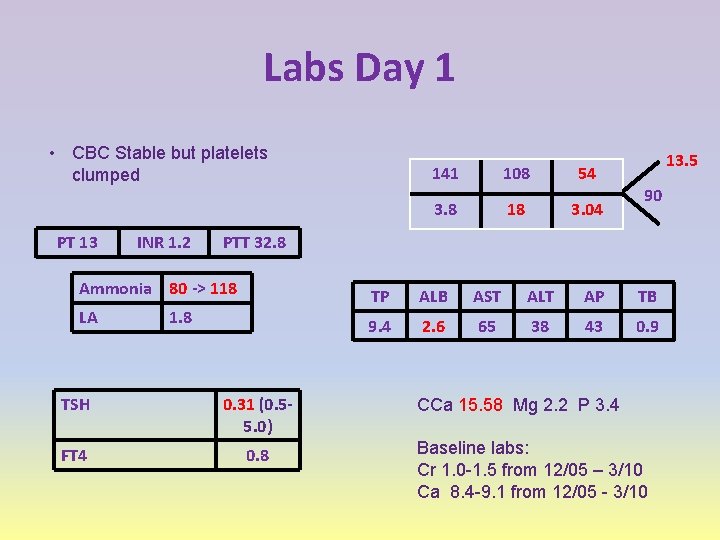
Labs Day 1 • CBC Stable but platelets clumped PT 13 INR 1. 2 108 54 3. 8 18 3. 04 13. 5 90 PTT 32. 8 Ammonia 80 -> 118 LA 141 1. 8 TSH 0. 31 (0. 55. 0) FT 4 0. 8 TP ALB AST ALT AP TB 9. 4 2. 6 65 38 43 0. 9 CCa 15. 58 Mg 2. 2 P 3. 4 Baseline labs: Cr 1. 0 -1. 5 from 12/05 – 3/10 Ca 8. 4 -9. 1 from 12/05 - 3/10
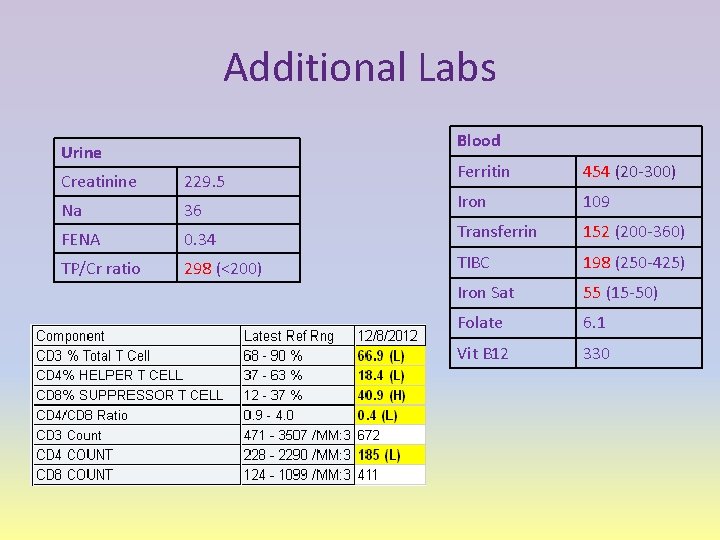
Additional Labs Blood Urine Ferritin 454 (20 -300) Iron 109 0. 34 Transferrin 152 (200 -360) 298 (<200) TIBC 198 (250 -425) Iron Sat 55 (15 -50) Folate 6. 1 Vit B 12 330 Creatinine 229. 5 Na 36 FENA TP/Cr ratio

Hospital Coarse • Day 2 – Transferred to floor overnight – Received 1 -2 doses of Lactulose – Began vomiting, no hematemesis noted Ammonia 80 > 118 > 125 > 95 BUN 56 > 54 > 50 Creatinine 3. 3 > 3. 04 > 2. 97 Calcium 15 > 13. 7 > 14. 2

• Day 3: Hospital Coarse – Patient received Ativan 2 mg overnight for “excessive restlessness” – Mental status waxing and waning, AM of Day 3 he was able to answer questions but still with slurred speech and confusion – Outputs unrecorded – Calcium still elevated with only slight improvement in renal function • Calcitonin 250 U Q 12 started with considerable increase in IVFs PTH 9 (12 -65) Ammonia 80 > 118 > 125 > 95 > 112 BUN 56 > 54 > 50 > 51 Creatinine 3. 3 > 3. 04 > 2. 97 > 2. 75 Calcium 15 > 13. 7 > 14. 2 > 12. 9

Hospital Coarse • Late that afternoon (Day 3) Large Monoclonal Band in Beta Region Adequate amount of normal serum immunoglobulin present Ig. M KAPPA specificity UPEP: Extra Band in the mid Gamma Region Immunofixation: Free Kappa Light Chains Heme-Onc consulted

Hospital Coarse • Day 4: – Mental status still waxing and waning, he was able to answer questions but still with slurred speech and confusion – Received Lactulose as scheduled – Net negative 10 Liters from admission • 4. 7 Liters in past 24 hrs Ammonia 80 > 118 > 125 > 95 > 112 > cancelled BUN 56 > 54 > 50 > 49 > 60 Creatinine 3. 3 > 3. 04 > 2. 97 > 2. 91 > 2. 24 Calcium 15 > 13. 7 > 14. 2 > 12. 9 > 12. 6

Hospital Coarse • Day 4: – Heme/Onc: • Kappa/lamba ratio, Ig. M, Ig. G, Ig. D, and beta-2 microglobulin ordered • Bone Marrow Biopsy pending • Decadron 40 mg IV Q 24 • Pamindronate 60 IV – X-ray Bone survey completed and compared with completed CT of Head (Day 1). – CT chest/abdomen/pelvis
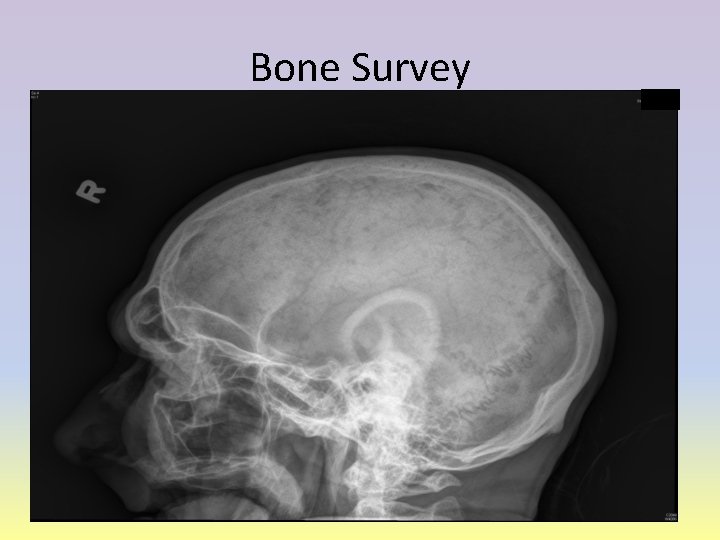
Bone Survey
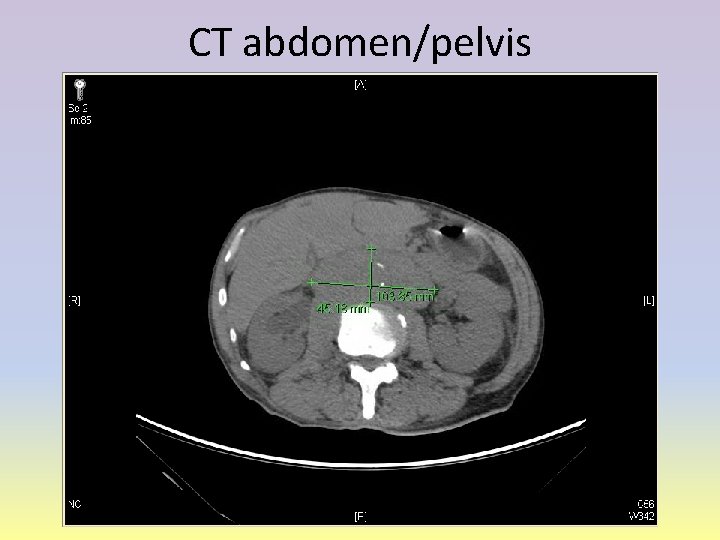
CT abdomen/pelvis
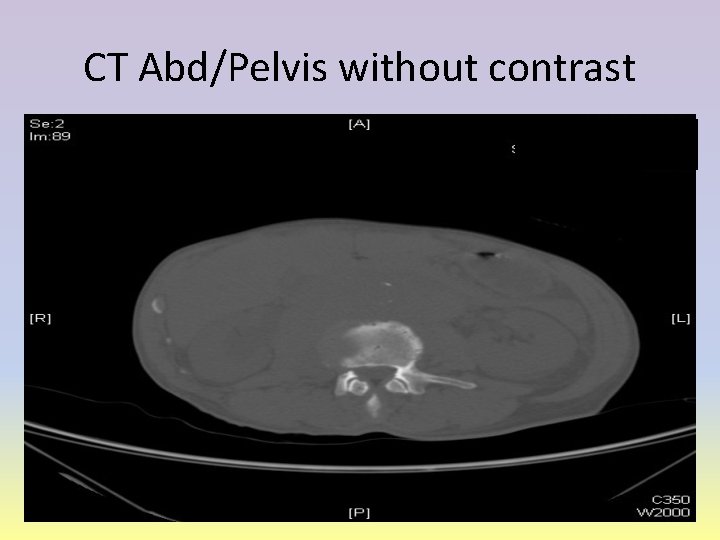
CT Abd/Pelvis without contrast
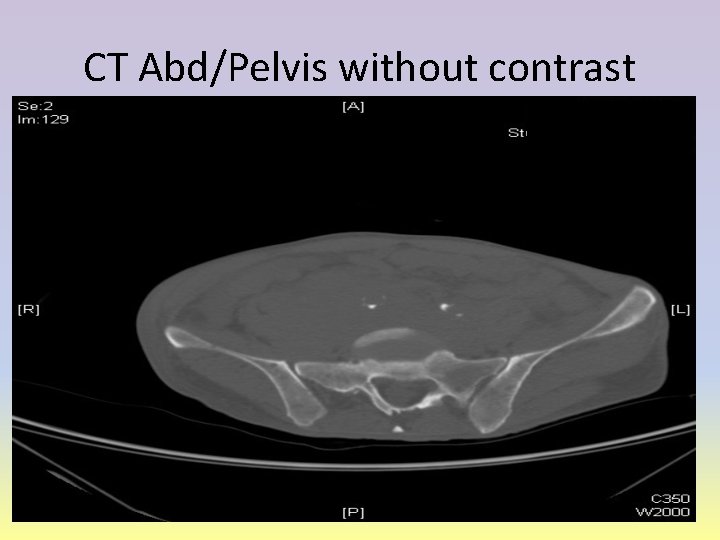
CT Abd/Pelvis without contrast
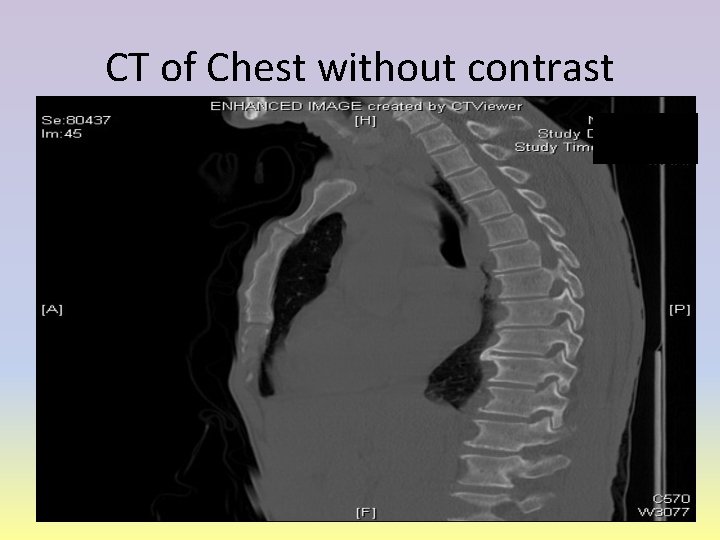
CT of Chest without contrast
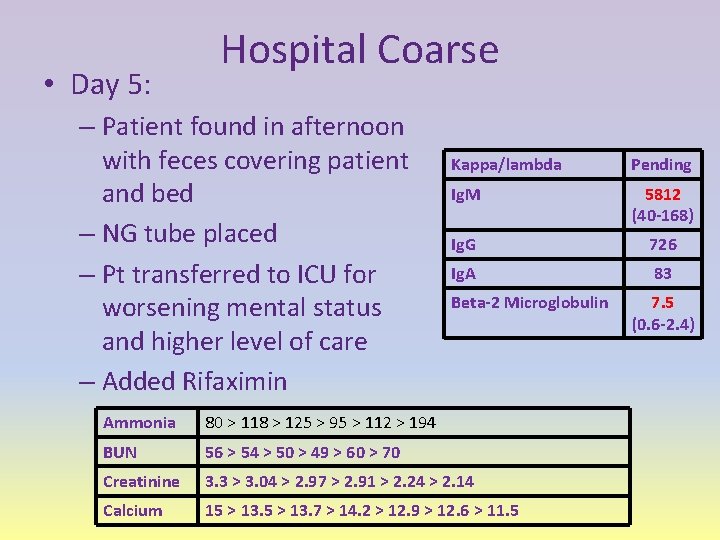

• Day 5: Hospital Coarse – Patient found in afternoon with feces covering patient and bed – NG tube placed – Pt transferred to ICU for worsening mental status and higher level of care – Added Rifaximin Kappa/lambda Pending Ig. M 5812 (40 -168) Ig. G 726 Ig. A 83 Beta-2 Microglobulin Ammonia 80 > 118 > 125 > 95 > 112 > 194 BUN 56 > 54 > 50 > 49 > 60 > 70 Creatinine 3. 3 > 3. 04 > 2. 97 > 2. 91 > 2. 24 > 2. 14 Calcium 15 > 13. 7 > 14. 2 > 12. 9 > 12. 6 > 11. 5 7. 5 (0. 6 -2. 4)
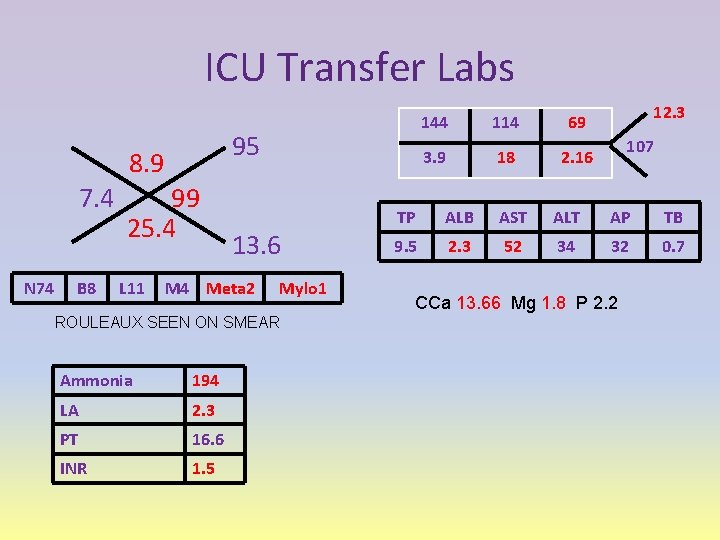
ICU Transfer Labs 95 8. 9 7. 4 N 74 B 8 99 25. 4 L 11 13. 6 M 4 Meta 2 Mylo 1 ROULEAUX SEEN ON SMEAR Ammonia 194 LA 2. 3 PT 16. 6 INR 1. 5 144 114 69 3. 9 18 2. 16 12. 3 107 TP ALB AST ALT AP TB 9. 5 2. 3 52 34 32 0. 7 CCa 13. 66 Mg 1. 8 P 2. 2
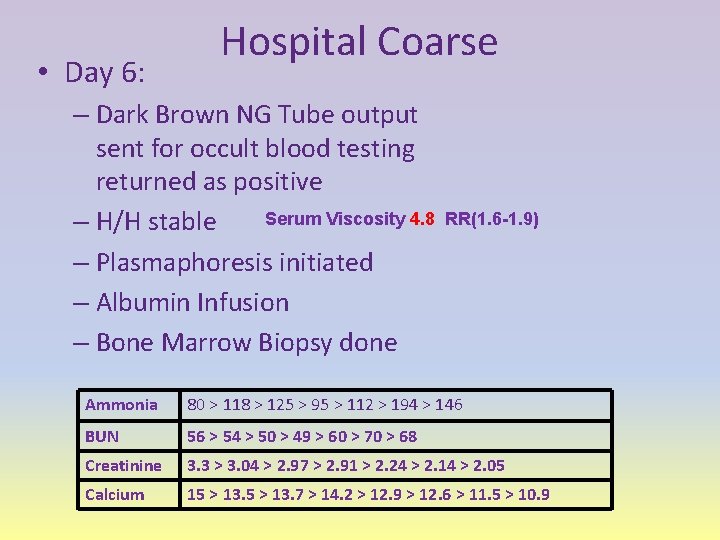
• Day 6: Hospital Coarse – Dark Brown NG Tube output sent for occult blood testing returned as positive Serum Viscosity 4. 8 – H/H stable – Plasmaphoresis initiated – Albumin Infusion – Bone Marrow Biopsy done RR(1. 6 -1. 9) Ammonia 80 > 118 > 125 > 95 > 112 > 194 > 146 BUN 56 > 54 > 50 > 49 > 60 > 70 > 68 Creatinine 3. 3 > 3. 04 > 2. 97 > 2. 91 > 2. 24 > 2. 14 > 2. 05 Calcium 15 > 13. 7 > 14. 2 > 12. 9 > 12. 6 > 11. 5 > 10. 9
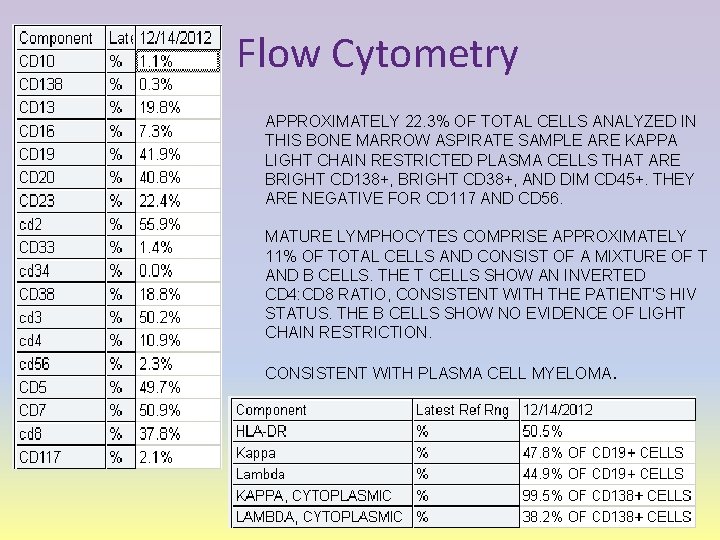
Flow Cytometry APPROXIMATELY 22. 3% OF TOTAL CELLS ANALYZED IN THIS BONE MARROW ASPIRATE SAMPLE ARE KAPPA LIGHT CHAIN RESTRICTED PLASMA CELLS THAT ARE BRIGHT CD 138+, BRIGHT CD 38+, AND DIM CD 45+. THEY ARE NEGATIVE FOR CD 117 AND CD 56. MATURE LYMPHOCYTES COMPRISE APPROXIMATELY 11% OF TOTAL CELLS AND CONSIST OF A MIXTURE OF T AND B CELLS. THE T CELLS SHOW AN INVERTED CD 4: CD 8 RATIO, CONSISTENT WITH THE PATIENT'S HIV STATUS. THE B CELLS SHOW NO EVIDENCE OF LIGHT CHAIN RESTRICTION. CONSISTENT WITH PLASMA CELL MYELOMA.
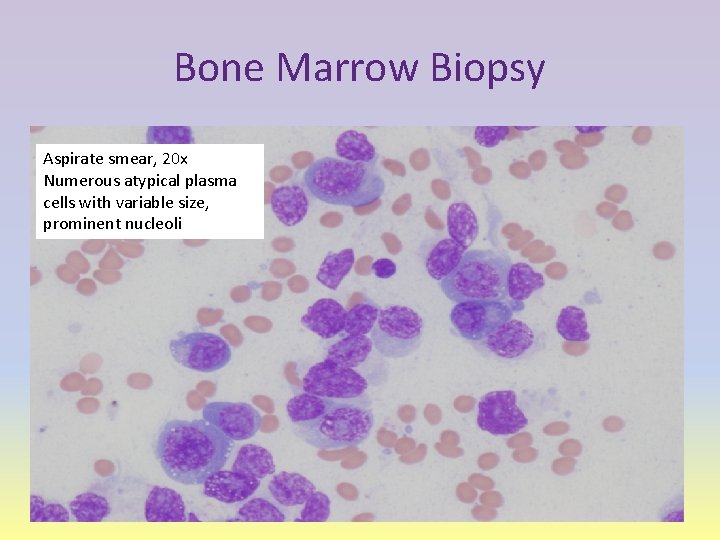
Bone Marrow Biopsy Aspirate smear, 20 x Numerous atypical plasma cells with variable size, prominent nucleoli
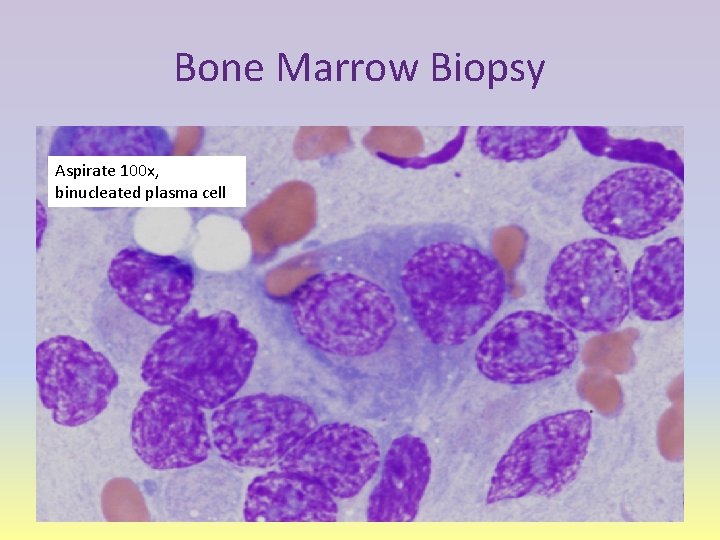
Bone Marrow Biopsy Aspirate 100 x, binucleated plasma cell
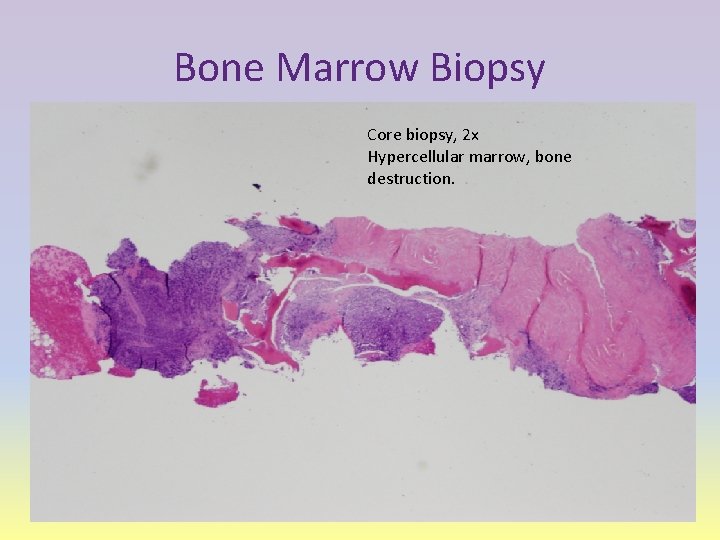
Bone Marrow Biopsy Core biopsy, 2 x Hypercellular marrow, bone destruction.
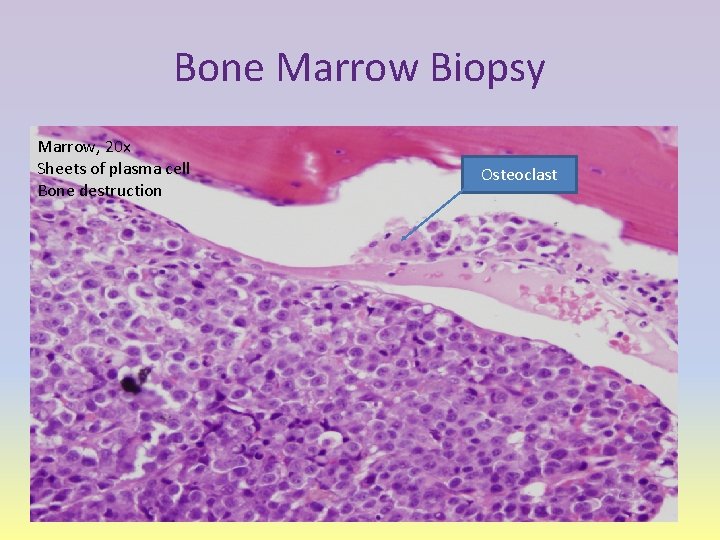
Bone Marrow Biopsy Marrow, 20 x Sheets of plasma cell Bone destruction Osteoclast
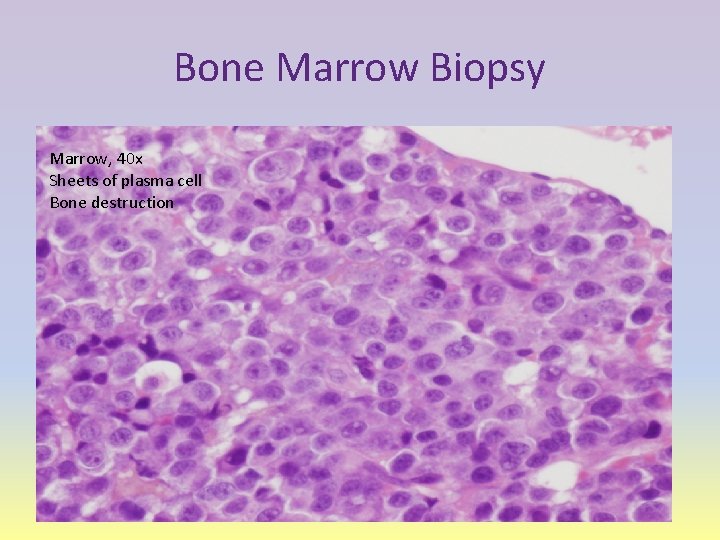
Bone Marrow Biopsy Marrow, 40 x Sheets of plasma cell Bone destruction
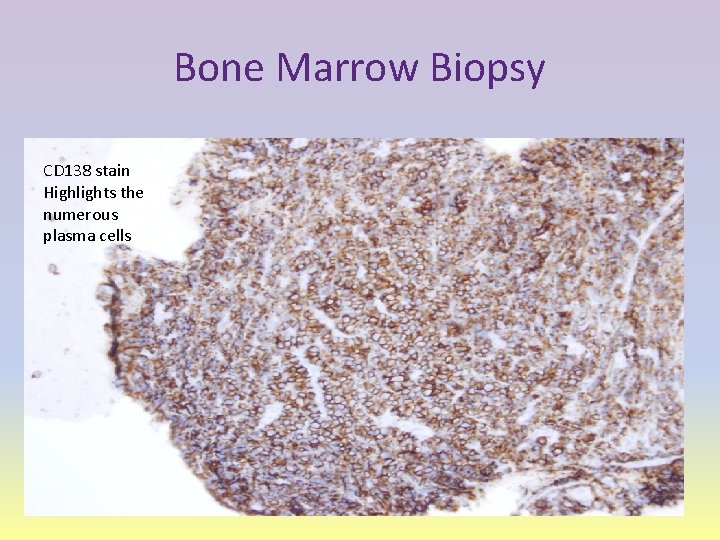
Bone Marrow Biopsy CD 138 stain Highlights the numerous plasma cells
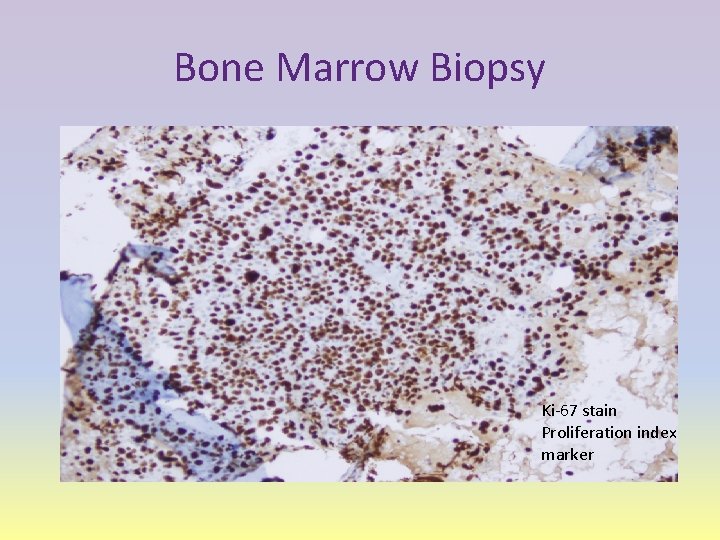
Bone Marrow Biopsy Ki-67 stain Proliferation index marker

Hospital Coarse • Day 7: – Multiple BMs overnight – Improving Mental Status – Started Feeds Per NGT – Consulted Urology for hyrdonephrosis • Deferred to IR – IVF and lasix discontinued • Calcitonin continued Ammonia 80 > 118 > 125 > 95 > 112 > 194 > 146 > 159 BUN 56 > 54 > 50 > 49 > 60 > 70 > 68 > 54 Creatinine 3. 3 > 3. 04 > 2. 97 > 2. 91 > 2. 24 > 2. 14 > 2. 05 > 1. 75 Calcium 15 > 13. 7 > 14. 2 > 12. 9 > 12. 6 > 11. 5 > 10. 9 > 8. 5

Hospital Coarse • Day 8: – Continued multiple BMs overnight – Mental Status still improving – Calcitonin discontinued – IR consult for biopsy of retroperitoneal mass and access for chemo Ammonia 80 > 118 > 125 > 95 > 112 > 194 > 146 > 159 BUN 56 > 54 > 50 > 49 > 60 > 70 > 68 > 54 > 51 Creatinine 3. 3 > 3. 04 > 2. 97 > 2. 91 > 2. 24 > 2. 14 > 2. 05 > 1. 71 Calcium 15 > 13. 7 > 14. 2 > 12. 9 > 12. 6 > 11. 5 > 10. 9 > 8. 5 > 8
Hospital Coarse – Day 9: Ativan given for agitation • Worsening mental status – Day 10: IR placed nephrostomy tube and performed biopsy of retroperitoneal mass. • Anaplastic appearing cells, many with plasmacytoid features. • The malignant cells stain with CD 138 and are negative for CD 3, CD 20, and CD 56. Ki-67 stains approximately 90% of cells. • Findings most consistent with diagnosis of a plasma cell neoplasm, most likely plasma cell myeloma – CT head (no changes)

Hospital Coarse – Day 11: Corrected Sodium, but physically abusive to staff. • • No family/contacts could be reached. Patients mental status improved. Ethics and Palliative care consult placed. Patient had coherent conversation with Oncology team – Understood disease process – Wished to not pursue further treatment.

Hospital Coarse – Day 12: Two of patient’s friends were located, meeting with ethics committee. • They stated prior to presentation, patient was usual self [walking, riding bikes, buses etc]. – Patient has made comments in recent past of “ready to go. ” – Estranged son in FL [unk name or contact info]. – Patient status changed to DNR/DNI – Transfer to Hospice

Thank You
- Slides: 52