HeparinInduced Thrombocytopenia HIT Pathophysiology Clinical Implications Therapy and

Heparin-Induced Thrombocytopenia (HIT): Pathophysiology, Clinical Implications, Therapy, and Cases Jerrold H Levy, MD Emory University School of Medicine Atlanta, Georgia ARG 266 R 0

HIT w Immune-mediated allergic reaction to heparin/platelet factor 4 complex w Thrombocytopenia – Platelet count <150, 000 thrombocytes/mc. L or a 30% to 50% drop from baseline during heparin exposure – Onset 5 to 14 days after initiating heparin but can be earlier or later w With or without thrombotic complications at presentation w Diagnosis is clinical w Any type of heparin or route of administration can lead to HIT Kelton. Semin Hematol. 1999; 36(suppl 1): 17 -21; Matthai. Semin Thromb Hemost. 1999; 25(suppl 1): 57 -60; Rice et al. Ann Intern Med. 2002; 136(3): 210 -215. Greinacher et al. Thrombosis Research. 2005 In Press. Slide 2

Incidence of HIT w HIT occurs in up to 5% of patients receiving unfractionated heparin (UFH) w Up to 1% incidence with low molecular weight heparin (LMWH) Gruel et al. Br J Haematol. 2003; 121; 786 -792; Warkentin. J Crit Illness. 2005: 20(1): 6 -13. Slide 3

Consequences of HIT w Thrombotic complications – Amputation: ~20% – Death: ~30% to 50% w If left untreated, the overall risk of thrombosis is 38% to 76% in HIT patients based on 3 studies (n=425) w Based on increased morbidity and mortality, heparin cessation alone is inadequate Hirsh et al. Arch Intern Med. 2004; 164: 361 -369; Warkentin. Semin Hematol. 1998; 35 (suppl 5): 9 -16. Slide 4
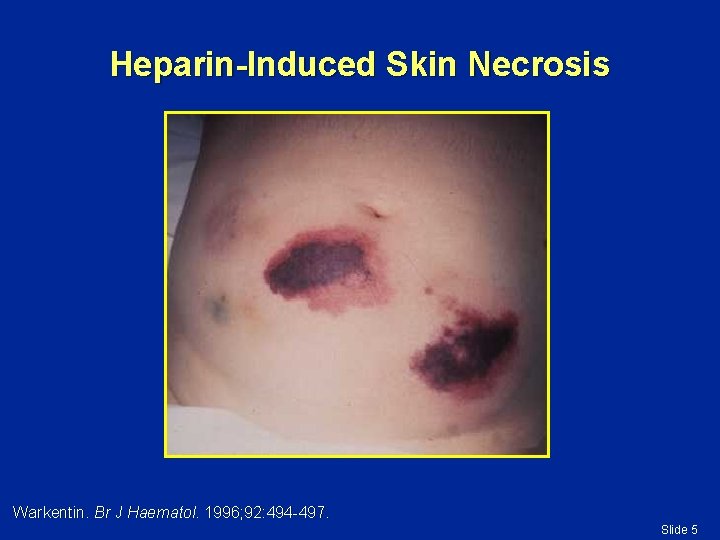
Heparin-Induced Skin Necrosis Warkentin. Br J Haematol. 1996; 92: 494 -497. Slide 5
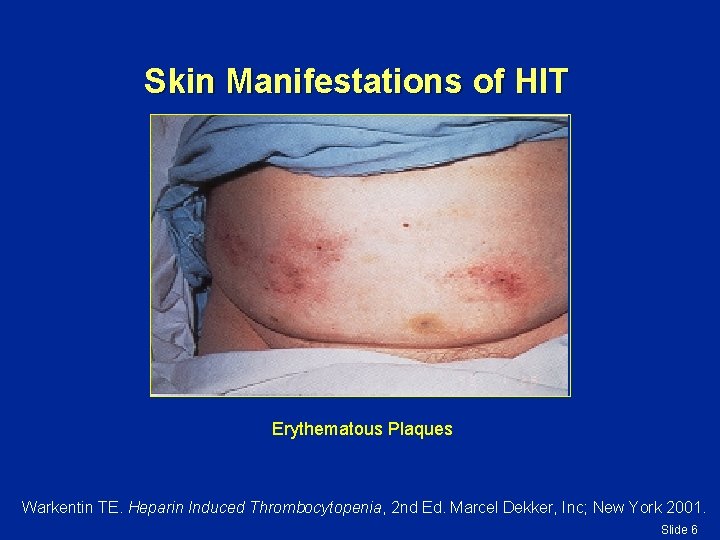
Skin Manifestations of HIT Erythematous Plaques Warkentin TE. Heparin Induced Thrombocytopenia, 2 nd Ed. Marcel Dekker, Inc; New York 2001. Slide 6
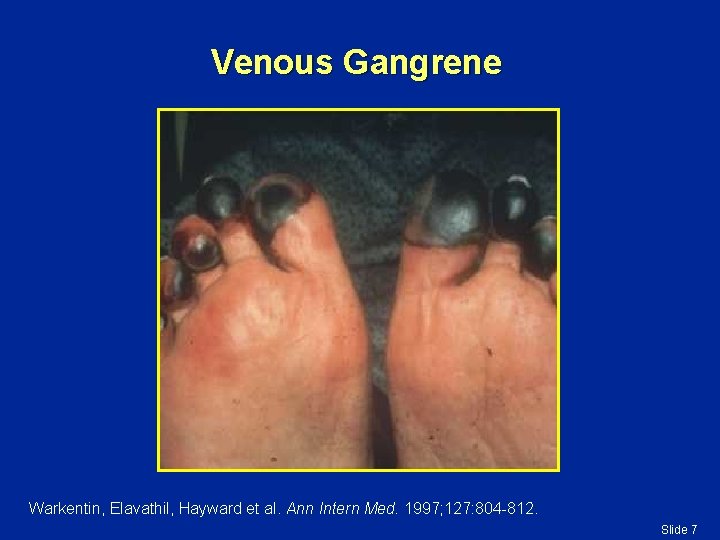
Venous Gangrene Warkentin, Elavathil, Hayward et al. Ann Intern Med. 1997; 127: 804 -812. Slide 7
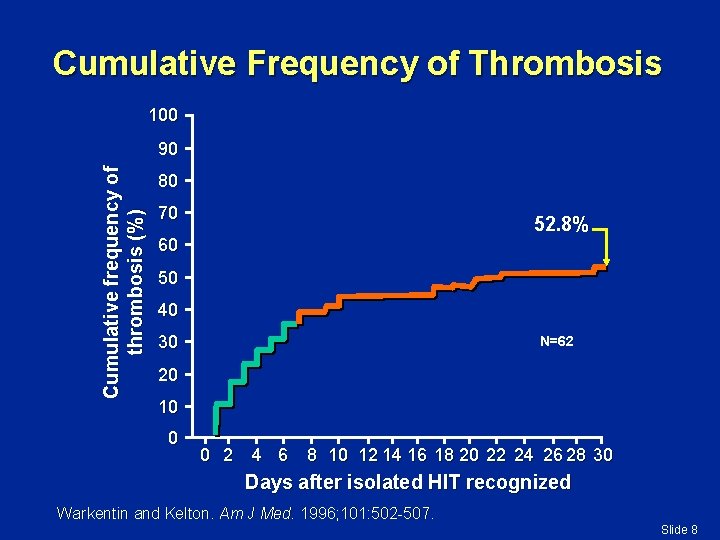
Cumulative Frequency of Thrombosis 100 Cumulative frequency of thrombosis (%) 90 80 70 52. 8% 60 50 40 30 N=62 20 10 0 0 2 4 6 8 10 12 14 16 18 20 22 24 26 28 30 Days after isolated HIT recognized Warkentin and Kelton. Am J Med. 1996; 101: 502 -507. Slide 8

Consequences of HIT w 38% to 52% of HIT patients managed by heparin cessation alone developed thrombotic complications, including DVT, PE, stroke, or MI within 1 month w Since thrombotic events have been observed even after cessation of heparin exposure, early recognition and initiation of appropriate therapy are essential steps in management Levine et al. Ann Emer Med. 2004; 44: 511 -515. Adapted from Parker. J Crit Ill. 2005’ 20(3): 64 -71. Slide 9

Consequences of HIT w Mortality rate of 22% to 28% has been reported in patients with HIT associated with thrombosis not treated with alternative anticoagulation. Levine et al. Ann Emer Med. 2004; 44: 511 -515. Slide 10

HIT Patients Presenting with Thrombosis w Deep venous thrombosis (50%) w Pulmonary embolism (25%) w Skin lesions at injection site (10% to 20%) w Acute limb ischemia (5% to 10%) w Warfarin-associated venous limb gangrene (5% to 10%) w Acute thrombotic stroke or myocardial infarction (3% to 5%) w Acute systemic reactions following IV bolus (~25%) Warkentin. Thromb Haemost. 1999; 82: 439 -447; Warkentin. J Crit Illness. 2005; 20(1): 6 -13. Slide 11
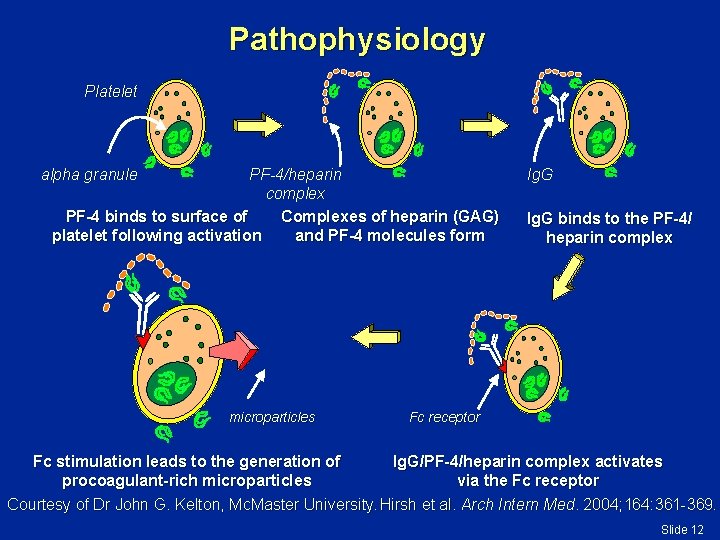
Pathophysiology Platelet alpha granule PF-4/heparin complex PF-4 binds to surface of Complexes of heparin (GAG) platelet following activation and PF-4 molecules form microparticles Ig. G binds to the PF-4/ heparin complex Fc receptor Fc stimulation leads to the generation of Ig. G/PF-4/heparin complex activates procoagulant-rich microparticles via the Fc receptor Courtesy of Dr John G. Kelton, Mc. Master University. Hirsh et al. Arch Intern Med. 2004; 164: 361 -369. Slide 12

Clinical Diagnosis of HIT w Timing of thrombocytopenia – 5 to 14 days after initiation of heparin, except in patients with recent heparin exposure – Earlier onset of thrombocytopenia with heparin re-exposure – Onset may be delayed and may can occur weeks to months after heparin discontinuation w Degree of thrombocytopenia – Decrease from baseline of 30% to 50% – 10% to 15% of HIT patients will have platelet count WNL w Other causes of thrombocytopenia excluded Rice et al. Ann Intern Med. 2002: 136(3): 210 -215; Warkentin. Thromb Haemost. 1999; 82: 439 -44 Warkentin. Semin Hematol. 1998; 35(suppl 5): 9 -16. Slide 13
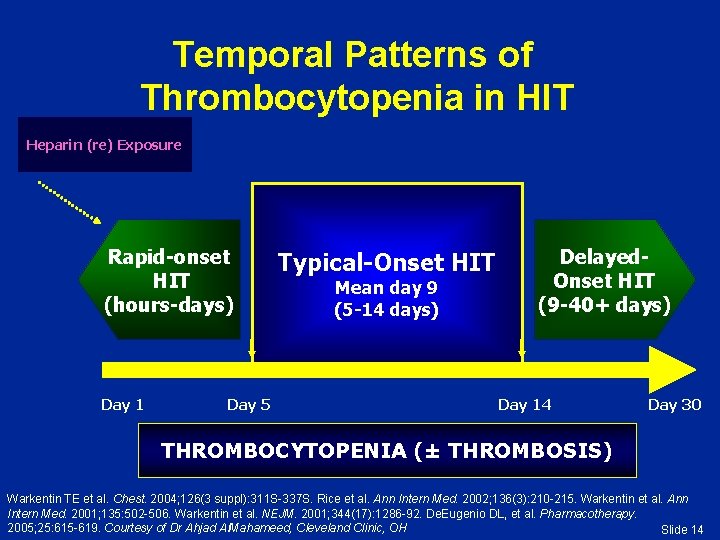
Temporal Patterns of Thrombocytopenia in HIT Heparin (re) Exposure Rapid-onset HIT (hours-days) Day 1 Day 5 Typical-Onset HIT Mean day 9 (5 -14 days) Delayed. Onset HIT (9 -40+ days) Day 14 Day 30 THROMBOCYTOPENIA (± THROMBOSIS) Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Rice et al. Ann Intern Med. 2002; 136(3): 210 -215. Warkentin et al. Ann Intern Med. 2001; 135: 502 -506. Warkentin et al. NEJM. 2001; 344(17): 1286 -92. De. Eugenio DL, et al. Pharmacotherapy. 2005; 25: 615 -619. Courtesy of Dr Ahjad Al. Mahameed, Cleveland Clinic, OH Slide 14
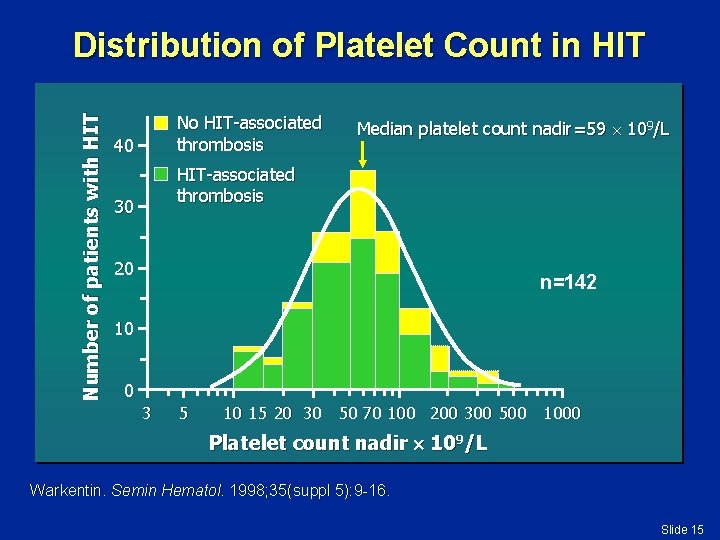
Number of patients with HIT Distribution of Platelet Count in HIT No HIT-associated thrombosis 40 Median platelet count nadir=59 109/L HIT-associated thrombosis 30 20 n=142 10 0 3 5 10 15 20 30 50 70 100 200 300 500 1000 Platelet count nadir 109/L Warkentin. Semin Hematol. 1998; 35(suppl 5): 9 -16. Slide 15

Differential Diagnosis of Thrombocytopenia Clinical Setting – Outpatient w Pregnancy w Myelodysplastic syndrome w Hypersplenism w Antiphospholipid syndrome w Immune thrombocytopenia purpura (ITP) Aird AC, Mark EJ. N Engl J Med. 2002; 346: 1562 -1570. Slide 16

Differential Diagnosis of Thrombocytopenia Clinical Setting – Inpatients w Drug Induced w Sepsis w Disseminated intravascular coagulation (DIC) w Dilutional thrombocytopenia w Posttransfusion purpura Aird AC, Mark EJ. N Engl J Med. 2002; 346: 1562 -1570. Slide 17

Differential Diagnosis of Thrombocytopenia Clinical Setting – Cardiac Inpatients w HIT w Use of platelet GP IIb/IIIa-receptor antagonists w Use of adenosine diphosphatereceptor antagonists w Coronary-artery bypass grafting w Use of intra-aortic ballon pump Aird AC, Mark EJ. N Engl J Med. 2002; 346: 1562 -1570. Slide 18

Test Laboratory Testing for HIT Advantages Disadvantages SRA Sensitivity: high Specificity: high (false positives rare) Technically demanding (radioisotopes) Not readily available Platelet (HIPA) aggregation Specificity: high Sensitivity: low Technique-dependent Immunoassay (ELISA) Sensitivity: high Technically easy Rapid turnaround time Specificity: low (false positives common for some populations) PIFA® Sensitivity: high Specificity: high Technically easy Rapid turnaround time Limited clinical history Positive & Negative controls not provided with assay HIT Requires a Clinical Diagnosis SRA=serotonin-release assay; ELISA=enzyme-linked immunosorbent assay. Fabris et al. Arch Pathol Lab Med. 2000; 124: 1657 -1666; Kelton. Semin Hematol. 1999; 36(suppl 1): 17 -21. PIFA® Heparin/Platelet Factor 4 Rapid Assay [package insert]. Thorofare, NJ: Akers Biosciences, Inc. ; 2005. Slide 19

Diagnosis and Management Decisions for HIT w Current or recent heparin exposure with thrombocytopenia w Presence of thrombosis or other characteristic sequelae w If HIT is suspected, discontinue all forms of heparin IMMEDIATELY: Initiate alternative anticoagulant, as indicated Hirsh et al. Arch Intern Med. 2004; 164: 361 -369; Warkentin. Thromb Haemost. 1999; 82: 439447; Warkentin. Semin Hematol. 1998; 35(suppl 5): 9 -16. Slide 20

Prophylaxis and Treatment of HIT: Patient Risk Factors w HIT with/without thrombosis should be suspected in patients with a 30% to 50% drop in platelets and – – Heparin use History of HIT Recent exposure to heparin Surgery § § Venous thrombosis: more common in orthopedic surgery Arterial thrombosis: more common in cardiac procedures Boshkov et al. Br J Haematol. 1993; 84: 322 -328; Hirsh et al. Arch Intern Med. 2004; 164: 361369; Spencer. J Thrombolysis. 2000; 10(suppl 1): 21 -25; Warkentin and Kelton. Am J Med. 1996; 101: 502 -507; Warkentin et al. N Engl J Med. 1995; 332: 1330 -1335. Slide 21

Treatment Goals Based on Pathophysiology and Clinical Studies w Interrupt the immune response – Discontinue heparin w Inhibit thrombin generation – Treat active thrombosis – Prevent new thrombosis w Minimize complications of HIT – Thromboses, limb amputation, death Slide 22
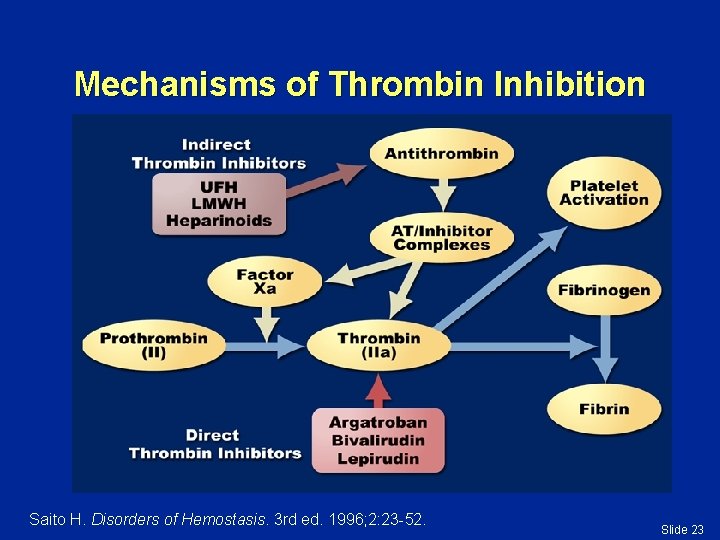
Mechanisms of Thrombin Inhibition Saito H. Disorders of Hemostasis. 3 rd ed. 1996; 2: 23 -52. Slide 23

Direct Thrombin Inhibitors: Mechanism of Action w Directly inhibit procoagulant and prothrombotic actions of thrombin w Do not require a cofactor to inhibit thrombin w Active against both free and clot-bound thrombin w Do not interact with or produce heparindependent antibodies Angiomax® (bivalirudin) for Injection [package insert]. The Medicines Company; 2004; Argatroban Injection [package insert]. Glaxo. Smith. Kline; 2005; Chen. Heart Dis. 2001; 3: 189198; Refludan® [lepirudin (r. DNA) for injection] [package insert]. Berlex Laboratories; 2004. Slide 24

Potential Benefits of Direct Thrombin Inhibitors w Predictable anticoagulant response w Inhibition of clot-bound and circulating thrombin w Direct binding to thrombin (no cofactor required) w Lack of heparin/PF 4 antibody formation Weitz JI, Buller HR. Circulation. 2002; 105: 1004 -1011. Slide 25

Direct Thrombin Inhibitors Argatroban Synthetic L-arginine derivative Half-life in healthy subjects Lepirudin Bivalirudin Recombinant Semisynthetic hirudin hirulog 39 -51 min 1. 3 hours 25 minutes Hepatic Renal 80% Enzymatic 20% Renal Monitoring needed a. PTT, ACT Thrombin binding Reversible Irreversible Partially reversible None Elimination Antidote a. PTT = activated partial thromboplastin time; ACT = activated clotting time. Adapted from Chen JL. Heart Dis. 2001; 3: 189 -198. Warkentin, TE, Greinacher A. Heparin-Induced Thrombocytopenia. 3 rd ed. Revised and Expanded. 2004; : 339 -479. Warkentin TE, Greinacher A. Chest 2004; 126: 311 s– 337 s. Slide 26

Direct Thrombin Inhibitors: FDA Indications and Usage w Argatroban – Indicated as an anticoagulant for prophylaxis or treatment of thrombosis in patients with HIT – Indicated as an anticoagulant in patients with or at risk for HIT undergoing PCI w Lepirudin – Indicated for anticoagulation in patients with HIT and associated thromboembolic disease to prevent further thromboembolic complications w Bivalirudin* – Indicated as an anticoagulant in patients undergoing percutaneous transluminal coronary angioplasty (PTCA) *Recently approved for with or at risk HIT patients undergoing PCI. (Dec. 2005) Angiomax® (bivalirudin) for injection [package insert]. Parsippany, NJ: The Medicines Company; 2005; Argatroban Injection [package insert]. Research Triangle Park, NC: Glaxo. Smith. Kline; 2005; Refludan ® [lepirudin (r. DNA) for Injection] [package insert]. Montvale, NJ: Berlex Laboratories, Inc. ; 2004. Slide 27

The Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy: Evidence-Based Guidelines CHEST: HIT Recommendations Warkentin TE, Greinacher A, Chest 2004; 126: 311 s– 337 s. Slide 28

ACCP Guidelines: Strongly Suspected or Confirmed HIT ACCP recommends use of an alternative nonheparin anticoagulant in therapeutic doses over further UFH, LMWH, or no anticoagulation Grade 1 C: Intermediate recommendation § Danaparoid (Grade 1 B) § Lepirudin (Grade 1 C+) § Argatroban (Grade 1 C) Grade 2 C: Very weak recommendation ▪ Bivalirudin (Grade 2 C) Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 29

ACCP Guidelines: Strongly Suspected or Confirmed HIT Grade 1 C: Intermediate recommendation § Routine ultrasonography of lower limb veins should be performed to evaluate thrombosis Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 30

ACCP Guidelines: HIT Grade 1 C+ : Do not use ACCP recommends strongly AGAINST use of vitamin K antagonists Coumadin® until after platelet count has recovered (100, 000150, 000/mc. L) w Vitamin K antagonists should be administered only during overlap with alternative anticoagulation w Begin with low, maintenance doses (maximum 5 mg warfarin; 6 mg phenprocoumon) w Alternative anticoagulants should not be STOPPED until platelet count has reached a stable plateau and with at least the last 2 days of INR within target therapeutic range Coumadin® (Warfarin Sodium for Injection, USP) [package insert]. Princeton, NJ: Bristol-Myers Squibb Company; 2005. Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 31

ACCP Guidelines: HIT Grade 2 C: Very weak recommendation w ACCP recommends for patients receiving vitamin K antagonist therapy at the time of diagnosis, reversal of vitamin K antagonism by use of oral or IV vitamin K Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 32

ACCP Guidelines: Acute or Previous HIT in Patients Who Require Catheterization or PCI Grade 1 C: Intermediate recommendation Argatroban § Bivalirudin § Lepirudin § Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 33

ACCP Guidelines: HIT Grade 1 C+: Do not use w ACCP recommends strongly AGAINST use of low–molecular-weight heparins in HIT patients Grade 2 C: Do not use w ACCP recommends AGAINST prophylactic platelet transfusions for patients who do not have active bleeding Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 34
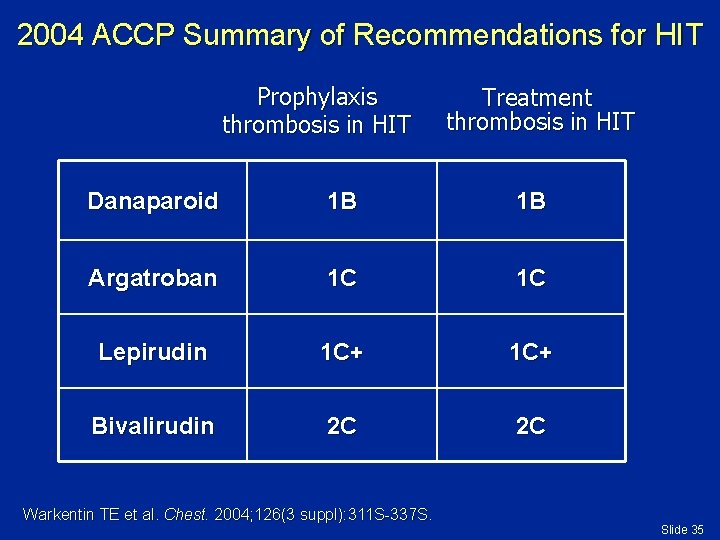

2004 ACCP Summary of Recommendations for HIT Prophylaxis thrombosis in HIT Treatment thrombosis in HIT Danaparoid 1 B 1 B Argatroban 1 C 1 C Lepirudin 1 C+ Bivalirudin 2 C 2 C Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 35

2004 ACCP Summary of Recommendations for HIT Acute HIT LMWH Do not use 1 C+ VKA Do not use 1 C Platelet transfusion Do not use 2 C LMWH = low–molecular-weight heparin; VKA = vitamin K antagonists. Warkentin TE et al. Chest. 2004; 126(3 suppl): 311 S-337 S. Slide 36

HIT CASE STUDIES

HIT CASE STUDY - Patient #1 w w w 45 yo F Stage IB Endometrial Carcinoma w w Post-op Day 9 - sudden PLT drop 238, 000 to 39, 000 mc. L TAH, BSO, LND Received prophylactic post op IV heparin x 4 days Post-op Day 6 - chest pain and SOB, collapsed, cyanotic VQ scan (+) for PE & 5 mm thrombosis @ tip of CVC IV Heparin re-initiated + urokinase given for thrombolysis with initial improvement in signs and symptoms HIT suspected, heparin d/c'd Aida H, Aoki Y, Ohki I, & Tanaka K. Anticoagulation with a selective thrombin inhibitor in a woman with heparin-induced thrombocytopenia. Obstet Gynecol. 2001; 98: 952 -954. Slide 38

HIT CASE STUDY - Patient #1 (cont'd) w POD 10, CVC thrombus larger. Underwent successful thrombectomy w w w Argatroban was administered intra- and postoperatively PLT post-op Day 1 - 104, 000/mc. L Oral warfarin and ASA initiated PLT post-op Day 4 - 236, 000/mc. L Patient was discharged home without further complications on hospital Day 32 Case based on an actual patient. Individual results may vary. Aida H, Aoki Y, Ohki I, & Tanaka K. Anticoagulation with a selective thrombin inhibitor in a woman with heparin-induced thrombocytopenia. Obstet Gynecol. 2000; 98: 952 -954. Slide 39

HIT DIAGNOSIS - Patient #1 w. Potential Causes w. Drug therapy – anesthesia, pain meds, heparin, urokinase w. Timing of PLT drop – re-exposure of heparin – day 3 w. Degree of PLT fall – 238, 000 to 39, 000 mc. L w. Patient Factors – obese, carcinoma w. Events – surgery w. Concurrent events – CVC thrombosis – PE w. Lab findings – elevated Ig. G antibody by immunoassay Aida H, Aoki Y, Ohki I, & Tanaka K. (2001). Anticoagulation with a selective thrombin inhibitor in a woman with heparin-induced thrombocytopenia. Obstet Gynecol. 2001; 98: 952 -954. Slide 40

HIT CASE STUDY - Patient #2 w 60 yo female underwent repair of aortic aneurysm with aortic valve replacement. w She received LMWH 30 mg SQ bid from POD 1 through 6 followed by warfarin therapy upon D/C w POD 4 she experienced transient amnesia that was attributed to medications w Re-presented to ED 33 days later after initial heparin exposure with proximal-thigh DVT despite a INR of 4. 2 w Patient admitted and IV heparin initiated in ED Rice L, Attisha WK, Drexler, AD, Francis JL. Delayed-onset heparin-induced thrombocytopenia. Ann Intern Med. 2002; 136(3): 210 -215. Slide 41

HIT CASE STUDY - Patient #2 (cont'd) w Immediately after receiving IV heparin bolus, she developed dyspnea, tachycardia & hypotension which required intubation and mechanical ventilation w w An inferior vena cava filter was placed for suspected PE w w VQ scan low probability for PE PLT count was 420, 000/mc. L on readmission, but dropped to 47, 000/mc. L after the heparin bolus ELISA (+) for heparin antibodies Started on danaparoid* Patient D/C without further sequelae, PLT’s 343, 000/mc. L Case based on an actual patient. Individual results may vary. *No longer available in the US. Rice L, Attisha WK, Drexler, AD, Francis JL. Delayed-onset heparin-induced thrombocytopenia. Ann Intern Med. 2002; 136(3): 210 -215. Slide 42

HIT DIAGNOSIS - Patient #2 w Onset of HIT – HIT has been documented to occur up to 40 days after heparin discontinuation – Patient presented to the ED with a DVT 33 days after initial exposure w Thrombotic complications – venous vs arterial – Suspect transient amnesia during first hospitalization was related to HIT – New onset DVT w Degree of PLT fall – 10% to 15% of patients with HIT, PLT nadir is above 150, 000/mc. L – Upon heparin re-exposure, dramatic drop in PLT count 420, 000/mc. L to 47, 000/mc. L after bolus w Delayed-onset HIT should be a primary diagnostic consideration whenever a recently hospitalized patient presents with thromboembolism Rice L, Attisha WK, Drexler, AD, Francis JL. Delayed-onset heparin-induced thrombocytopenia. Ann Intern Med. 2002; 136(3): 210 -215. Slide 43

HIT CASE STUDY - Patient #3 w w w 63 yo F w/ metastatic Ovarian Carcinoma w w Received Cisplatin, Taxol, CTX Presented to clinic c/o (R) arm swelling Hickman catheter placement 2 1/2 weeks prior to chemo Daily heparin saline flushes for 3 wks Day 10 after chemo PLT drop 329, 000 to 73, 000/mc. L At clinic visit, day 18, PLT continued to fall to 20, 000/mc. L with R subclavian vein thrombosis documented Kadidal VV, Mayo DJ, Horne MK. Heparin-induced thrombocytopenia (HIT) due to heparin flushes: a report of three cases. J Int Med. 1999; 246: 325 -329. Slide 44

HIT CASE STUDY - Patient #3 (cont'd) w w w w PLT transfusion given IV heparin initiated Due to failure of PLT to rise, HIT was suspected Heparin was d/c'd Danaparoid* was initiated Pre-heparin ELISA and SRA assays were (+) PLT count rose >100, 000 mc. L within 3 days while on danaparoid* Case based on an actual patient. Individual results may vary. *No longer available in the US. Kadidal VV, Mayo DJ, Horne MK. Heparin-induced thrombocytopenia (HIT) due to heparin flushes: a report of three cases. J Int Med. 1999; 246: 325 -329. Slide 45

HIT DIAGNOSIS - Patient #3 w. Potential Causes w. Drugs – chemotherapy, heparin flush, IV heparin, platelet transfusion w. Patient factors – cancer, Hickman line w. Timing of PLT fall – initial fall suspected to be chemo nadir Day 10 – continuation of fall Day 18 w. Delayed onset HIT? ? w. Degree of PLT fall – 329, 000 to 73, 000 to 20, 000/mc. L – lack of response to transfusion and IV heparin w. Development of Thrombosis – subclavian vein thrombosis w. Laboratory findings – (+) ELISA and SRA Kadidal VV, Mayo DJ, Horne MK. Heparin-induced thrombocytopenia (HIT) due to heparin flushes: a report of three cases. J Int Med. 1999; 246: 325 -329. Slide 46

HIT CASE STUDY - Patient #4 w w 75 yo male had infected knee prosthesis removed w w Venography showed subclavian thrombosis Received LMWH 30 mg SQ BID POD 1 -9 Discharge Day 9 Readmitted Day 12 with swollen, dusky left arm, the site of subclavian catheter Day 12 Platelet count 145, 000/mc. L Initiated LMWH 80 mg SQ BID Day 13 platelet count 85, 000/mc. L Rice L, Attisha WK, Drexler, AD, Francis JL. Delayed-onset heparin-induced thrombocytopenia. Ann Intern Med. 2002; 136(3): 210 -215. Slide 47

HIT CASE STUDY - Patient #4 (cont'd) w w w w Arm worsened with impending gangrene Day 15 hematology consult Due to failure of PLT to rise, HIT was suspected Tissue plasminogen activator given Hirudin was initiated Arm improved dramatically within 2 days Result of ELISA was (+) Discharged on warfarin with PLT 240, 000/mc. L Case based on an actual patient. Individual results may vary. Rice L, Attisha WK, Drexler, AD, Francis JL. Delayed-onset heparin-induced thrombocytopenia. Ann Intern Med. 2002; 136(3): 210 -215. Slide 48

HIT DIAGNOSIS - Patient #4 w. Potential Causes w. Drugs – Low molecular weight heparin, anesthesia, pain meds w. Patient factors – orthopedic patient, subclavian catheter w. Timing of PLT fall – initial documented fall day 12 w. Typical onset HIT w. Degree of PLT fall – 145, 000 to 85, 000/mc. L – Question platelet count on initiation of enoxaparin and prior to discharge w. Development Thrombosis – subclavian vein thrombosis w. Laboratory findings – (+) ELISA Rice L, Attisha WK, Drexler, AD, Francis JL. Delayed-onset heparin-induced thrombocytopenia. Ann Intern Med. 2002; 136(3): 210 -215. Slide 49

HIT CASE STUDY - Patient #5 w w w 67 y/o male had undergone coronary artery bypass surgery w w POD 7 PLT 233, 000/mc. L POD 7 presented to ED with sudden onset of confusion CT scan revealed no intracranial hemorrhage Diagnosed with left-sided cerebrovascular accident Intravenous heparin initiated in ED for possible thromboembolic stroke POD 9 PLT 84, 000/mc. L Heparin d/c’d due to suspicion of HIT antibody testing (+) Levine et al. Annals of Emergency Medicine. 2004; 44: 511 -515. Slide 50

HIT CASE STUDY - Patient #5 (cont'd) w w w w Neurologic status deteriorated w Withdrawal of life support and patient expired Repeat CT scan showed large area of ischemia w/o bleeding IV Argatroban initiated but d/c’d after 2 hours Concerns of possible intracranial bleeding Serial CT scans revealed no bleeding No further anticoagulant administered During next 3 days patient remained unresponsive, developed multiple bilateral cerebral infarcts with clinical deterioration Case based on an actual patient. Individual results may vary. Levine et al. Annals of Emergency Medicine. 2004; 44: 511 -515. Slide 51

HIT DIAGNOSIS - Patient #5 w. Potential Causes w. Drugs – Anesthesia, cardiac meds w. Patient factors - cardiac surgery patient w. Timing of PLT fall – initial documented fall day 9 w. Typical onset HIT w. Degree of PLT fall – 233, 000/mc. L to 84, 000/mc. L – Question platelet count post cardiac surgery and prior to discharge w. Development Thrombosis – ? Thromboembolic stroke w. Laboratory findings – (+) antibody test Levine et al. Annals of Emergency Medicine. 2004; 44: 511 -515. Slide 52

Management of HIT w Identify HIT early with diligent PLT monitoring w D/C all heparin sources – IV, SC, flushes, coated lines w Avoid platelet transfusions – Exception: major bleeding w Initiate alternative anticoagulation as indicated Warkentin, TE. Arch Pathol Lab Med. 2000; 126: 1415 -1423. Slide 53

Nursing & Pharmacy Role w Key to limiting early morbidity and mortality from HIT is – – – Rapid recognition of signs & symptoms Early identification with diligent PLT monitoring Avoid platelet transfusions except in major bleeding Immediate cessation of all heparin sources Initiation of alternate therapy w Nurses & pharmacists play a vital role in the early recognition of HIT by monitoring vigilantly for drops in platelet counts & new thrombotic events while patients are on heparin Miller, P. AORN. 2003; 78(1): 79 -89. Warkentin, TE. Arch Pathol Lab Med. 2000; 126: 1415 -1423. Slide 54

Monitor Platelet Counts w. For adjusted- and full-dose therapy, perform platelet counts pre-treatment and at least on alternate days – Begin on day 4 for heparin-naïve patients – Begin on day 1 for patents with prior heparin exposure w. For high-risk patients: – Obtain baseline – Monitor regularly – Monitor frequently College of American Pathologists Consensus Arch Pathol Lab Med 1998; 122: 782– 798. Slide 55

Summary of HIT w HIT is a life- and limb-threatening medical emergency w HIT is a relatively common and often under- recognized devastating complication of heparin therapy w However the consequences of HIT are largely preventable with early recognition and proper treatment w Awareness of the clinical presentation of HIT and the ability to distinguish it from other causes of platelet count reduction are keys to avoiding serious sequelae Greinacher et al. Thrombosis Research. 2005 In Press. Warkentin. J Crit Ill. 2005 ; 20(1): 6 -13. Slide 56

Summary of HIT w Diagnosis of HIT is based upon clinical suspicion w Treatment of HIT should not be delayed while awaiting laboratory confirmation w Untreated patients with HIT are at a high risk of having thromboembolic complications w Management of HIT – Discontinue all types of heparin – Assess risk of thrombosis – Initiate alternative anticoagulant therapy, as indicated Greinacher et al. Thrombosis Research. 2005 In Press. Warkentin. J Crit Ill. 2005; 20(1): 6 -13. Slide 57
- Slides: 57