HeparinInduced Thrombocytopenia HIT HeparinInduced Thrombocytopenia HIT HIT is

Heparin-Induced Thrombocytopenia (HIT)

Heparin-Induced Thrombocytopenia (HIT) HIT is an immune-mediated adverse effect of heparin that paradoxically increases risk of thrombosis

HIT is a clinico-pathological syndrome Clinical • Thrombocytopenia and/or • Thrombosis Pathological • Heparin-dependent, platelet-activating Ig. G antibodies Warkentin TE, Chong BH, Greinacher A. Thromb Haemost 1998; 79: 1 -7. Greinacher et al. Blood 2005; 106: 2921 -2922. Greinacher et al. Thromb Haemost 2005; 94: 132 -135.

Heparin-induced thrombocytopenia (HIT) Less frequent clinical manifestations • Anaphylactoid reaction after i. v. heparin bolus • Skin lesions at s. c. heparin injection sites • Overt (decompensated) disseminated intravascular coagulation (DIC)

Approach to diagnose HIT Yes HIT Thrombocytopenia (> 50% decrease) + Possible Timing 5 -14 days after starting heparin + Thrombosis + Unusual thromboembolism; skín lesions; anaphylaxis OTher cause not apparent + + Strongly Suspected Test for HIT antibodies positive (usually strongly positive) + Confirmed when positive in context of strong clinical suspicion

Clinical events associated with HIT • Venous thrombosis (30 -70%) • • • Deep vein thrombosis (DVT) Pulmonary embolism (PE) Adrenal necrosis (adrenal vein thrombosis) Cerebral venous (sinus) thrombosis Venous limb gangrene (VKA associated) • Arterial thrombosis (“white clots”) (15 -30%) • Limb artery thrombosis • Stroke • Myocardial infarction • Skin lesions at heparin injection sites (10%) • Skin necrosis • Erythematous plaques • Acute reactions after i. v. heparin bolus (10%) • Disseminated intravascular coagulation (DIC) (10%)

Drugs associated with HIT • Unfractionated heparin • • Prophylactic dose Therapeutic dose Flushes Heparin-coated devices • Low-molecular-weight heparin • Prophylactic dose • Therapeutic dose • Other highly sulfated polysaccharides • Pentosan polysulfate • Hypersulfated chondroitin sulfate • PI-88 (anti-angiogenic drug)
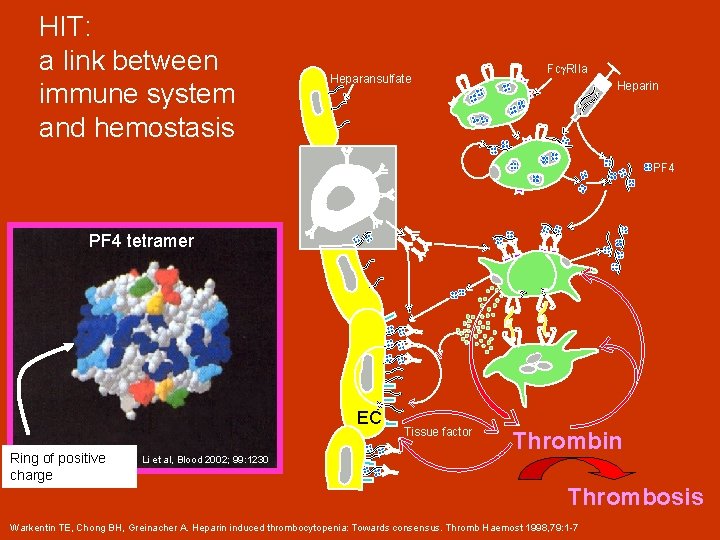
HIT: a link between immune system and hemostasis Heparansulfate Fcg. RIIa Heparin PF 4 B-L PF 4 tetramer EC Ring of positive charge Li et al, Blood 2002; 99: 1230 Tissue factor Thrombin Thrombosis Warkentin TE, Chong BH, Greinacher A. Heparin induced thrombocytopenia: Towards consensus. Thromb Haemost 1998, 79: 1 -7

Sequence of events in the development of HIT Initiation • Current or recent exposure to heparin • Immune response against platelet factor 4 (PF 4)/heparin complexes • Anti-PF 4/heparin Ig. G antibodies crosslink platelet Fc receptors and trigger platelet activation • Positive feedback for platelet activation (e. g. , adenosine diphosphate, thromboxane A 2) • Platelet activation results in shedding of procoagulant platelet microparticles

Sequence of events in the development of HIT Development of a hypercoagulable state • Platelet microparticles promote thrombin generation • Endothelial cell injury and monocyte activation further enhance thrombin generation • PF 4 release neutralizes heparin • PF 4 release leads to formation of additional PF 4/heparin complexes, exposing more antigens, and thus further amplifying platelet activation
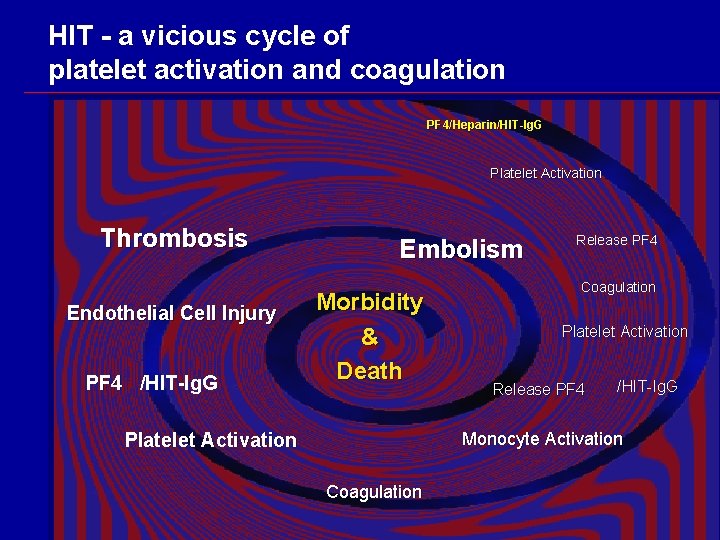
HIT - a vicious cycle of platelet activation and coagulation PF 4/Heparin/HIT-Ig. G Platelet Activation Thrombosis Endothelial Cell Injury PF 4 /HIT-Ig. G Embolism Morbidity & Death Release PF 4 Coagulation Platelet Activation Release PF 4 /HIT-Ig. G Monocyte Activation Platelet Activation Coagulation

Factors influencing frequency of HIT Factor Type of heparin Patient population Duration of heparin Influence Bovine UFH > porcine UFH > LMWH Post-surgery > medical > obstetrical 5 or more days heparin use > 1 -4 days Dose of heparin Change from low to full dose can lead abrupt platelet in immunized patient Gender Female > male Definition of thrombocytopenia Proportional platelet count fall (e. g. >50%) more sensitive than absolute platelet
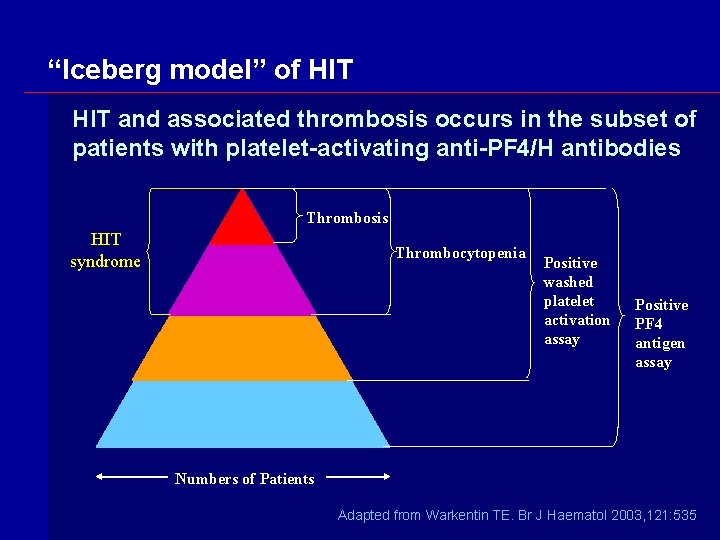
“Iceberg model” of HIT and associated thrombosis occurs in the subset of patients with platelet-activating anti-PF 4/H antibodies Thrombosis HIT syndrome Thrombocytopenia Positive washed platelet activation assay Positive PF 4 antigen assay Numbers of Patients Adapted from Warkentin TE. Br J Haematol 2003, 121: 535
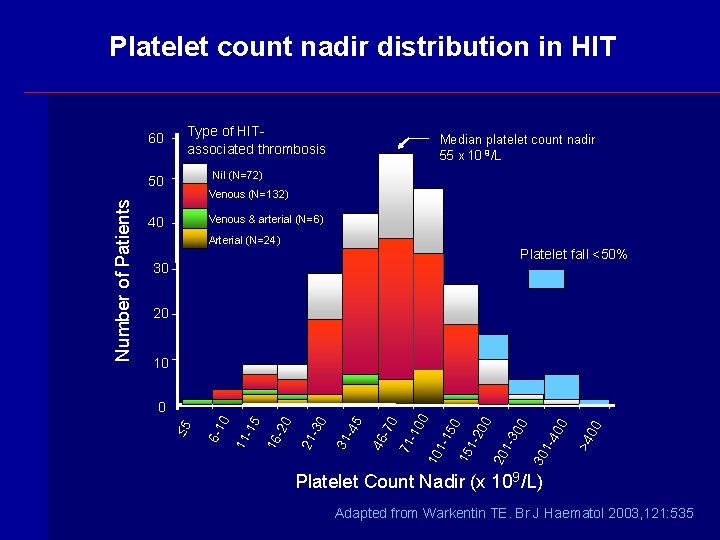
Platelet count nadir distribution in HIT 60 Type of HITassociated thrombosis Nil (N=72) 50 Venous (N=132) Venous & arterial (N=6) 40 Arterial (N=24) Platelet fall <50% 30 20 10 00 >4 30 1 -4 00 00 20 1 -3 00 1 -2 50 15 1 -1 0 10 -10 71 -70 46 -45 31 -30 21 -20 16 -15 11 6 -1 0 0 £ 5 Number of Patients Median platelet count nadir 55 x 10 9 /L Platelet Count Nadir (x 109 /L) Adapted from Warkentin TE. Br J Haematol 2003, 121: 535
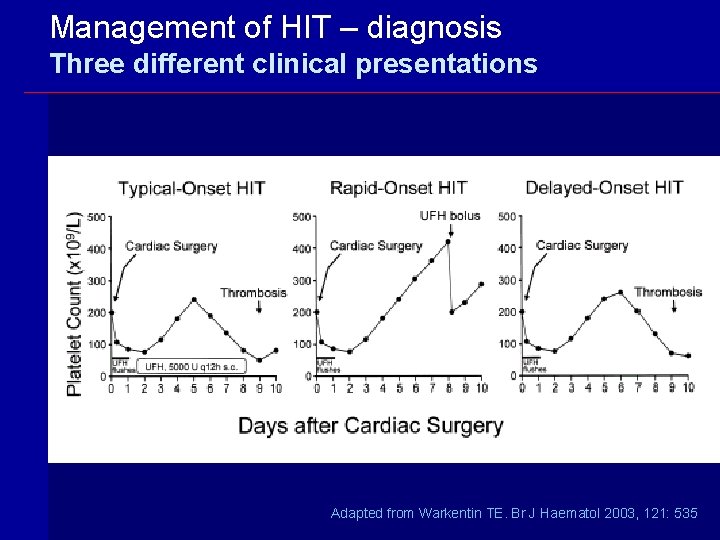
Management of HIT – diagnosis Three different clinical presentations Adapted from Warkentin TE. Br J Haematol 2003, 121: 535

Detection of HIT antibodies • Platelet activation assays • Serotonin release assay (SRA; uses “washed” platelets) • Heparin-induced platelet activation (HIPA) assay (uses “washed” platelets) • Platelet aggregation test (PAT; uses citrate-anticoagulated platelet-rich plasma) • Platelet microparticles (flow cytometry) • Antigen assays • • PF 4/heparin-enzyme immunoassay (EIA) PF 4/polyvinyl sulfonate EIA Fluid-phase EIA Particle gel immunoassay
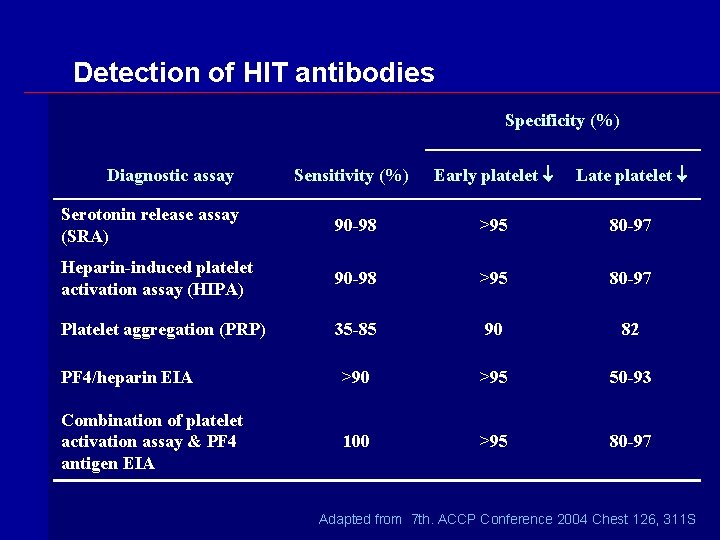
Detection of HIT antibodies Specificity (%) Sensitivity (%) Early platelet Late platelet Serotonin release assay (SRA) 90 -98 >95 80 -97 Heparin-induced platelet activation assay (HIPA) 90 -98 >95 80 -97 Platelet aggregation (PRP) 35 -85 90 82 PF 4/heparin EIA >90 >95 50 -93 Combination of platelet activation assay & PF 4 antigen EIA 100 >95 80 -97 Diagnostic assay Adapted from 7 th. ACCP Conference 2004 Chest 126, 311 S

Detection of HIT antibodies • High negative predictive value • Negative test usually rules out HIT * • Moderate positive predictive value • Stronger test result = higher chance of HIT • Routine antibody testing is NOT recommended unless: • • Thrombocytopenia or >50% in platelet count Thrombosis Heparin-induced skin necrosis Other sequelae of HIT * Applies to solid-phase EIAs and washed platelet activation assays 7 th. ACCP Conference 2004 Chest 126, 311 S
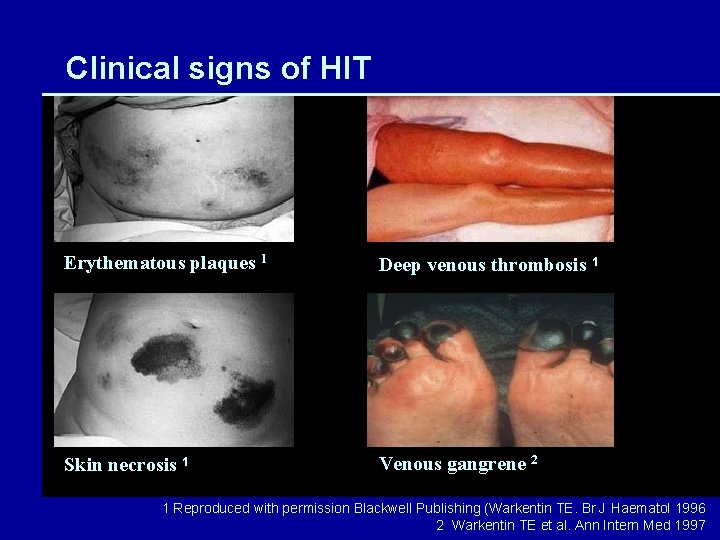
Clinical signs of HIT Erythematous plaques 1 Deep venous thrombosis 1 Skin necrosis 1 Venous gangrene 2 1 Reproduced with permission Blackwell Publishing (Warkentin TE. Br J Haematol 1996 2 Warkentin TE et al. Ann Intern Med 1997

Clinical signs of HIT Acute reactions after intravenous heparin bolus • • Fever, chills, flushing Respiratory distress Hypertension, tachycardia, chest pain Transient global amnesia, headache Venous and/or arterial thrombosis • Deep vein thrombosis • Pulmonary embolism • Limb ischemia and infarction • Thrombotic stroke and cerebral (sinus) vein thrombosis • Myocardial infarction • Adrenal necrosis

Differential diagnosis • • • • Hemodilution post-surgery Severe pulmonary embolism Sepsis DIC (multiple causes besides HIT) Cancer-associated DIC Antiphospholipid syndrome Thrombolytic therapy EDTA-induced pseudothrombocytopenia GP IIb/IIIa inhibitor-induced thrombocytopenia Drug-induced thrombocytopenia (other than heparin) Post-transfusion purpura Thrombotic thrombocytopenic purpura Non-immune heparin-associated thrombocytopenia

Platelet count monitoring is recommended in patients at risk of HIT > 0. 1%* Platelet count monitoring Patient population Yes/No Frequency Risk for HIT common (>1%) Receiving therapeutic dose UFH Yes min. alternate day 14 d Receiving post-op prophylactic dose UFH Yes min. alternate day 4 - 14 d Starting UFH/LMWH & have received UFH in last 100 d or exposure uncertain Yes baseline value-repeat in 1 d Systemic reaction after UFH bolus Yes immediate – compare with pre-bolus value Risk for HIT infrequent (0. 1 -1%). Medical/Obstetric UFH; Post -op LMWH; Post-op UFH ‘flush’; LMWH after UFH Yes every 2 -3 days, 4 - 14 d Risk HIT < 0. 1%. Medical/obstetric patients on LMWH No - * 7 th. ACCP Conference 2004 Chest, 126: 311 S
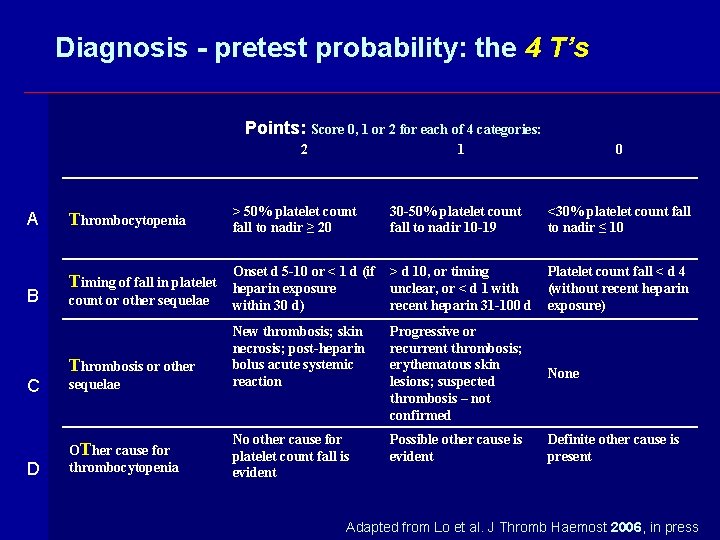

Diagnosis - pretest probability: the 4 T’s Points: Score 0, 1 or 2 for each of 4 categories: 2 A B Thrombocytopenia Timing of fall in platelet count or other sequelae 1 > 50% platelet count fall to nadir ≥ 20 30 -50% platelet count fall to nadir 10 -19 <30% platelet count fall to nadir ≤ 10 Onset d 5 -10 or < 1 d (if heparin exposure within 30 d) > d 10, or timing unclear, or < d 1 with recent heparin 31 -100 d Platelet count fall < d 4 (without recent heparin exposure) Progressive or recurrent thrombosis; erythematous skin lesions; suspected thrombosis – not confirmed None Possible other cause is evident Definite other cause is present C sequelae New thrombosis; skin necrosis; post-heparin bolus acute systemic reaction D OTher cause for thrombocytopenia No other cause for platelet count fall is evident Thrombosis or other 0 Adapted from Lo et al. J Thromb Haemost 2006, in press

Diagnosis - pretest probability Interpretation of 4 T’s score • Score 0 -3: very unlikely to be HIT (<5%) • Score 4 - 5: a minority have HIT (10 -30%) • Score 6 – 8: 20 to >80% have HIT, depending on the clinical setting and scorer´s experience: these patients usually require an alternative, non-heparin anticoagulant in therapeutic doses Adapted from Lo et al. J Thromb Haemost 2006, in press

Management of HIT – treatment When HIT is strongly-suspected: • Stop heparin (UFH/LMWH), even in patients without thrombosis • Initiate alternative non-heparin anticoagulant because of high risk of symptomatic thrombosis • Test for HIT antibodies • Duplex ultrasonography for lower-limb DVT

Management of HIT – treatment When HIT is strongly-suspected: • Do not start a vitamin K antagonist (VKA) - if started prior to diagnosis it should be reversed by vitamin K * • Do not use low-molecular-weight heparin (LMWH) • Do not give platelet transfusions unless needed to manage serious hemorrhage * Recommendation to give vitamin K applies particularly to direct thrombin inhibitors (DTIs), because prolongation of the a. PTT by warfarin can lead to underdosing of DTI therapy (in contrast, danaparoid is not monitored by a. PTT) • 7 th. ACCP Conference 2004 Chest, 126: 311 S-337 S • Warkentin TE. J Thromb Haemost 2006; in press.

Management of HIT – treatment When the diagnosis of HIT is confirmed: • Postpone starting overlapping coumarin until the platelet count has recovered to at least 100 (and preferably) 150 x 109/L • Therapeutic doses of alternative, non-heparin anticoagulants are usually required • If a sensitive test for HIT is negative, heparin therapy may be re-started with regular platelet count monitoring * 7 th. ACCP Conference 2004 Chest, 126, 311 S-337 S

Management of HIT – treatment When HIT is clinically possible but platelet count decrease is more likely caused by other reasons: • If the patient requires therapeutic dose anticoagulation for non-HIT reasons, use alternative anticoagulant in therapeutic dose. • If patient does not require therapeutic dose anticoagulation for non-HIT reasons, consider prophylactic-dose alternative anticoagulation, e. g. danaparoid 750 U b. i. d. or t. i. d. until HIT antibody test results are available. Selleng K and Greinacher A: Intensiv up-2 -date 2005; 1: 329 -341
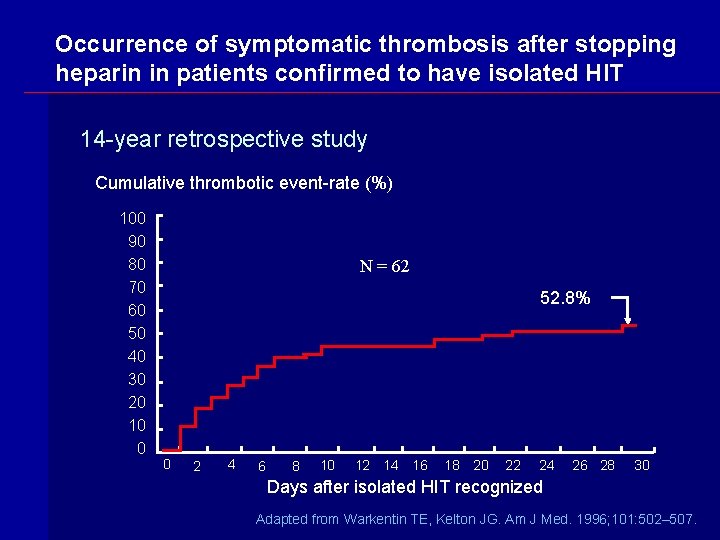
Occurrence of symptomatic thrombosis after stopping heparin in patients confirmed to have isolated HIT 14 -year retrospective study Cumulative thrombotic event-rate (%) 100 90 80 70 60 50 40 30 20 10 0 N = 62 52. 8% 0 2 4 6 8 10 12 14 16 18 20 22 24 26 28 30 Days after isolated HIT recognized Adapted from Warkentin TE, Kelton JG. Am J Med. 1996; 101: 502– 507.

Odds ratios for risk of thrombosis • • Prothrombin anomaly Lupus anticoagulant Factor V Leiden 6. 6 Protein S deficiency Dysfibrinogenaemia Protein C deficiency Antithrombin deficiency • HIT 2. 0 5. 4 10. 9 11. 3 14. 4 24. 1 20 -40 Warkentin TE. Can J Cardiol 1995; 11(Suppl. C): 29 C-34 C Warkentin TE. Thromb Res; 2003; 110: 73 -82

Management of HIT – treatment Suitable alternative non-heparin antithrombotic therapies are: • Danaparoid – Xa/IIa inhibitor (anti-Xa >> anti-IIa) • Direct thrombin inhibitor (DTI): • Lepirudin • Argatroban • Bivalirudin * 7 th. ACCP Conference 2004 Chest 126: 311 S-337 S

HIT – summary & conclusions 1. HIT is a potentially fatal side effect of heparin that is more common with UFH than LMWH 2. HIT is a clinico-pathologic syndrome: its diagnosis is based on compatible clinical features and presence of HIT antibodies 3. Antibodies against PF 4/heparin are formed commonly during heparin treatment; HIT occurs in the subset of patients with strong plateletactivating Ig. G antibodies

HIT – summary & conclusions 4. Binding of HIT antibodies to PF 4/heparin complexes on the platelet surface results in platelet activation, thrombocytopenia and increased risk of arterial thrombosis 5. Platelet, monocyte, and endothelial cell activation results in a hypercoagulable state, and increased risk of venous thrombosis 6. HIT-associated thrombosis occurs in some patients 1 – 2 days before platelet counts decrease

HIT – summary & conclusions 7. Platelet count monitoring is important to diagnose isolated HIT and thus has the potential to prevent thrombosis 8. Recognizing a relative decrease of platelet count is important since platelets do not always fall below 150 x 109/L 9. Platelet count monitoring is recommended in most patients receiving UFH and in some patients receiving LMWH.

HIT – summary & conclusions 9. Heparin should be stopped immediately in all situations where HIT is strongly suspected 10. Due to the high risk of thrombosis in patients with HIT anticoagulation with a non-heparin anticoagulant should be started even in the absence of overt thrombosis 11. Danaparoid provides an option for anticoagulation in either prophylactic or therapeutic doses

Heparin-Induced Thrombocytopenia (HIT)
- Slides: 36