HEMOSTASIS The ability of the body to control
HEMOSTASIS The ability of the body to control the flow of blood following vascular injury is paramount to continued survival. - prevention of blood loss - to close the hole in the vessel permanently - the process of blood clotting and then the subsequent dissolution of the clot, following repair of the injured tissue

• normal haemostasis complicated relations between the vessel wall, trombocytes and coagulation and fibrinolytic system • the balanced system = the mutual proportions are not impaired - is continuously maintained the systems supporting the local haemostasis • the systems inhibiting the disseminated thrombosis ENDOTHELIUM- the inner surface of vessels initiated) - a nontrombogenic barrier- its primary function - inhibiting the interaction of blood components with subendothelial structures (the thrombus formation - no tissue factor (strong activator of coagulation)
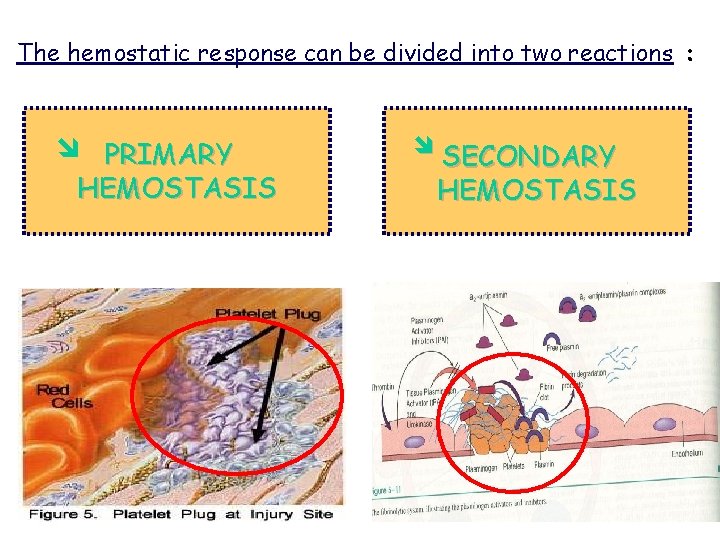
The hemostatic response can be divided into two reactions : PRIMARY HEMOSTASIS SECONDARY HEMOSTASIS

Primary hemostasis vascular constriction -the initial phase of the process -this limits the flow of blood to the area of injury - stimulus of the traumatized vessel nervous reflexes (pain) local myogenic spasm (direct damage) - many minutes or even hours adhesion, activation and ggregation of platelets, formation of platelets plug platelets - circulate in an inactive form -are activated, if the endothelium is damaged

a) Vascular wall - active role , mainly endotel a subendotel - function „ mechanical „ VAZOCONSTRICTION „ synthetic „ formation and accumulation of substantions involved in hemostasis Important physiological anticoagulant instrument endothelium intact , watter-repellent Endothelium – no tissue factor - nontrombrogenic barrierinhibits interaction between components of blood a subendothelial structures - expression of trombodulin , heparin (natural inhibitors of coagulation)
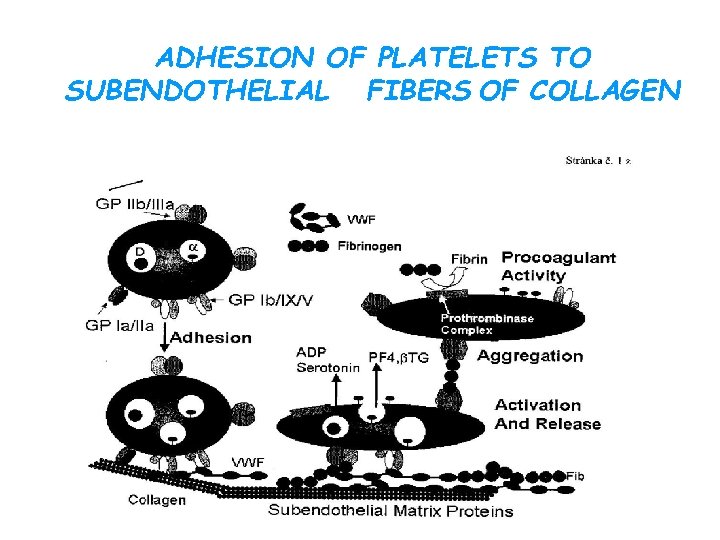
ADHESION OF PLATELETS TO SUBENDOTHELIAL FIBERS OF COLLAGEN

ACTIVATION OF PLATELETS -the initial activation is induced by binding to collagenous fibrils -activation evoke also several agonists especially ADP, adrenaline , serotonin, some arachidonic acid metabolites -triggers the action of thrombocyte contractile system. ----change their shape -- to accommodate the formation of the plug - upon activation, platelets release large quanties of adenosine-5'-diphosphate, ADP and TXA 2, serotonin, phospholipids, lipoproteins and other proteins important for the coagulation cascade
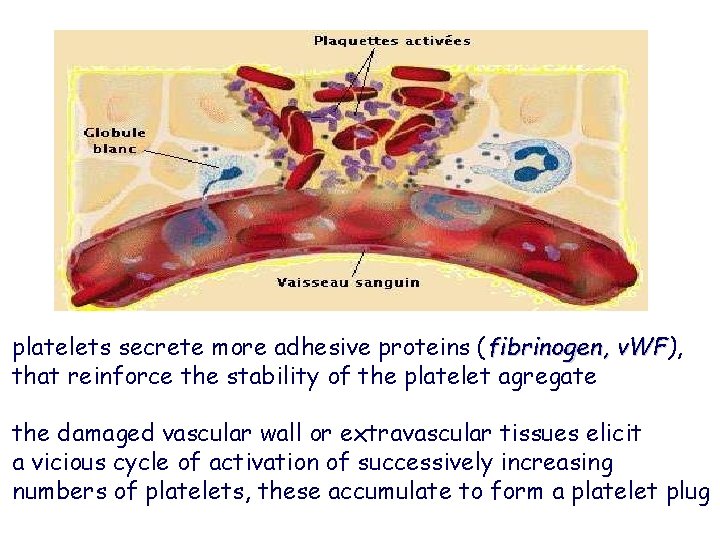
platelets secrete more adhesive proteins (fibrinogen, v. WF), v. WF that reinforce the stability of the platelet agregate the damaged vascular wall or extravascular tissues elicit a vicious cycle of activation of successively increasing numbers of platelets, these accumulate to form a platelet plug

SECONDARY HEMOSTASIS • over 40 different substances • balance between promoting coagulation …. procoagulants inhibiting coagulation. . . anticoagulants - the activation of plasma coagulation factors resulting in the formation of fibrin - fibrin reinforcement of the initial platelet aggregate is essential to prevent bleeding from larger lesions


1. 2. 3.
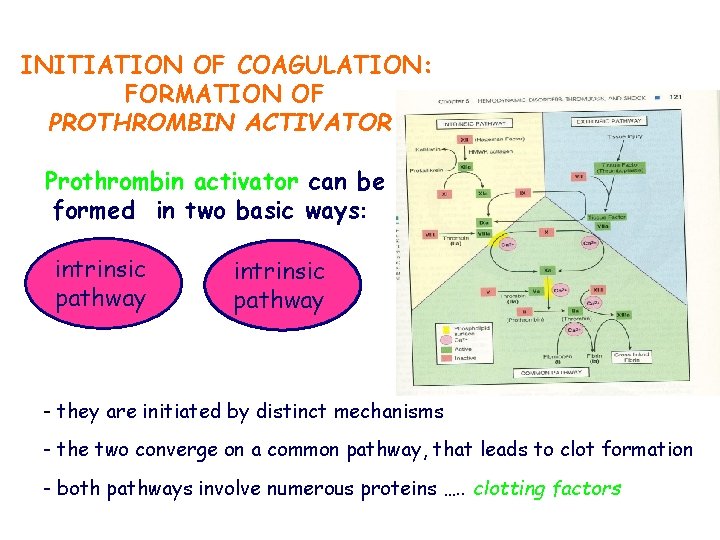
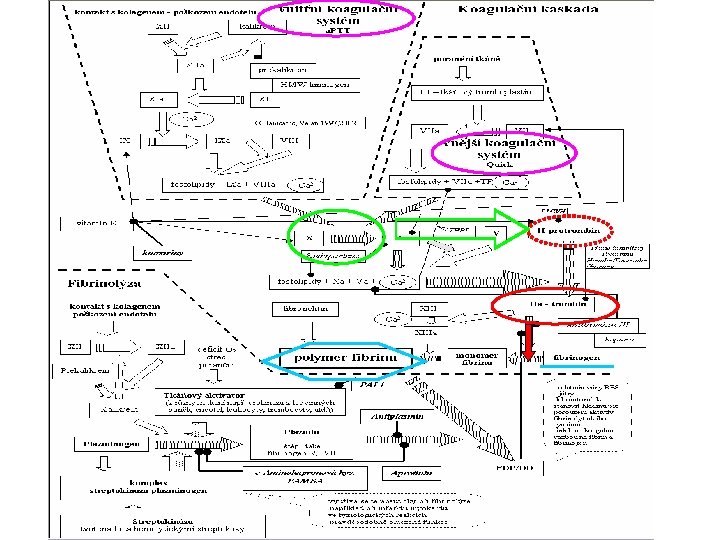
INITIATION OF COAGULATION: FORMATION OF PROTHROMBIN ACTIVATOR Prothrombin activator can be formed in two basic ways: intrinsic pathway - they are initiated by distinct mechanisms - the two converge on a common pathway, that leads to clot formation - both pathways involve numerous proteins …. . clotting factors
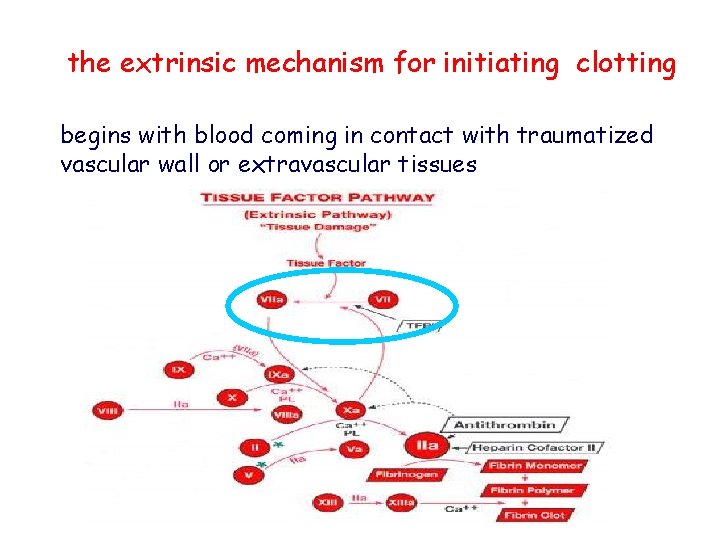
the extrinsic mechanism for initiating clotting begins with blood coming in contact with traumatized vascular wall or extravascular tissues

the intrinsic mechanism for initiating clotting 1, activation of factor XII, release of platelet phospholipids by blood trauma to the blood alters two important factors factor XII and the platelets -contact with collagen or with a wettable surface „activated factor XII” release of the platelets platelet phospholipid 2. activation of factor XI XIIa acts enzymatically on factor XI to activate this as well 3. activation of factor IX by activated factor XI XIa then acts enzymatically on factor IX to activate this factor 4. activation of factor X – role of factor VIII IXa + VIII + platelet phospholipids activates factor X
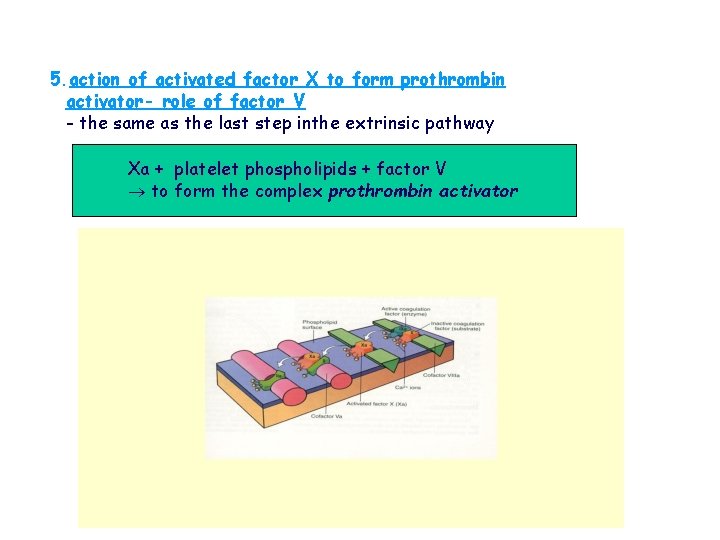
5. action of activated factor X to form prothrombin activator- role of factor V - the same as the last step inthe extrinsic pathway Xa + platelet phospholipids + factor V to form the complex prothrombin activator
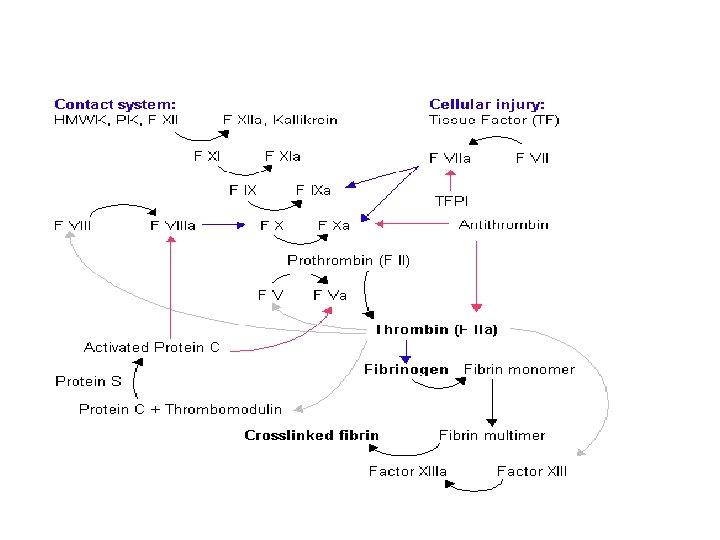
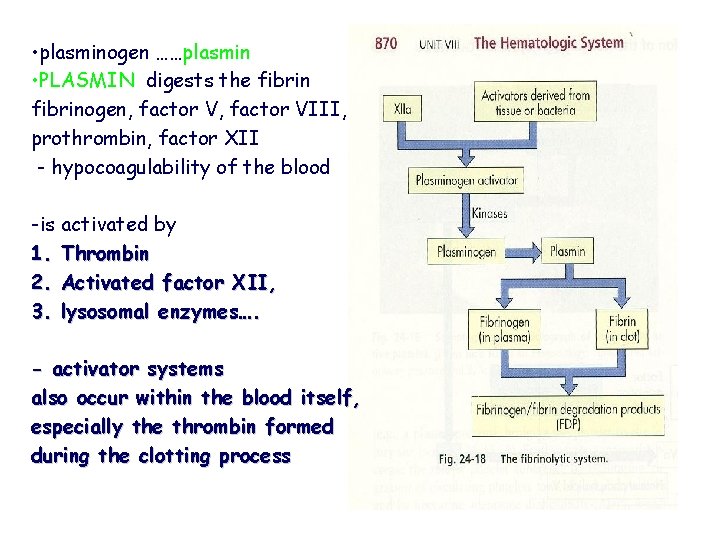
• plasminogen ……plasmin • PLASMIN digests the fibrinogen, factor VIII, prothrombin, factor XII - hypocoagulability of the blood -is activated by 1. Thrombin 2. Activated factor XII, 3. lysosomal enzymes…. - activator systems also occur within the blood itself, especially the thrombin formed during the clotting process

DISSEMINATED INTRAVASCULAR COAGULATION • pathophysiological process and not a disease • inappropriate excessive and uncontrolled activation of haemostatic process • systemic circulation of thrombin and plasmin • characterised by consumption of clotting factors and platelets within circulation resulting in varying degrees of microvascular obstruction due to fibrin deposition

is a syndrome arising as a complication of many different serious and life-threatening illnesses in its acute form, form DIC is usually an explosive, often lifethreatening disorder when it is relatively mild or subclinical, subclinical DIC may not be so easy to spot. • clinical manifestation of DIC relate to occlusion of the microvessels during the obstructive phase of the syndrome and hemorrhage secondary to consumption of plasma and cellular components in the hemorhagic phase • the perpetuation of the process may be due to continuation of the stimulus and/or consumption of the natural inhibitors of hemostasis

in initiation ……. . may be adequate compensation ……. . . defects only in the laboratory tests severe the initiating disorder…. . . uncontrolled acute DIC. . . systemic bleeding state …. . . end organ failure ACUTE (OVERT) FORM a hemorrhagic disorder…. multiple ecchymoses, mucosal disorder bleeding, and depletion of platelets and clotting factors CHRONIC (NONOVERT) FORM - involves thromboembolism accompanied by evidence of activation of the coagulation system - coagulation factors may be normal, increased, or moderately decreased, as may the platelet counts
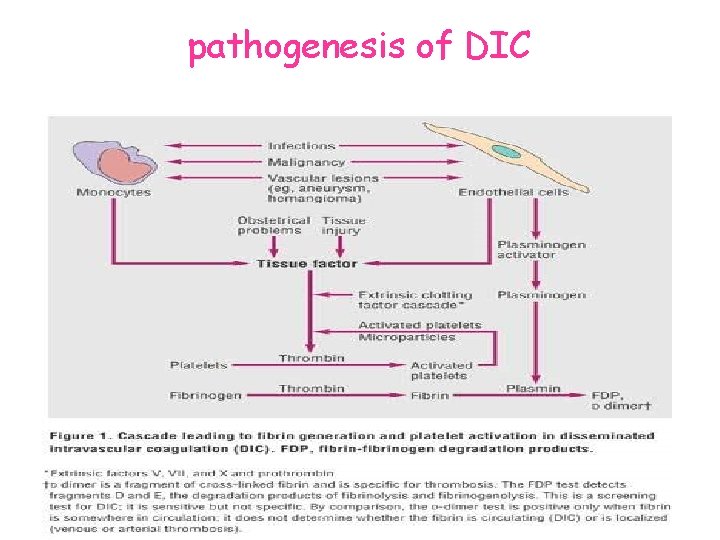
pathogenesis of DIC
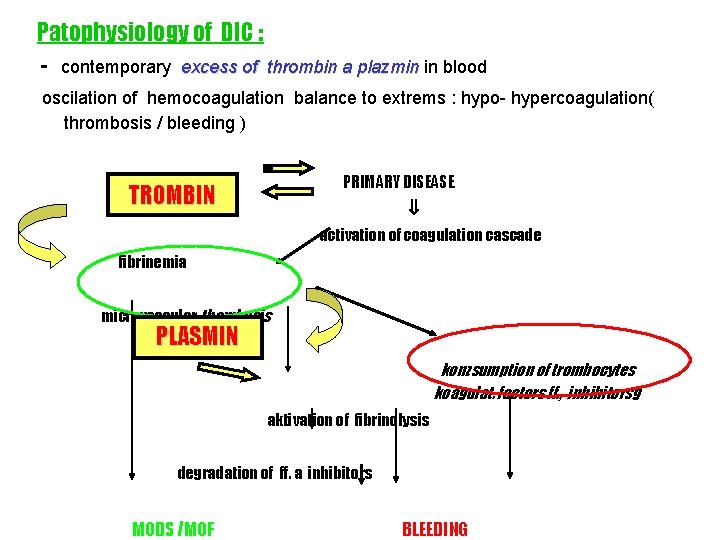
Patophysiology of DIC : - contemporary excess of thrombin a plazmin in blood oscilation of hemocoagulation balance to extrems : hypo- hypercoagulation( thrombosis / bleeding ) PRIMARY DISEASE TROMBIN activation of coagulation cascade fibrinemia microvascular thombosis PLASMIN konzsumption of trombocytes koagulat. factors ff. , inhibitorsg aktivation of fibrinolysis degradation of ff. a inhibitors MODS /MOF BLEEDING

mechanisms which may inappropriately activate haemostatic system: 1. activation of coagulation sequence by release of tissue thromboplastins into systemic circulation (eg extensive trauma, surgery, malignancy , intravascular haemolysis) 2. induction of platelet activation (eg septicaemia, viraemia, immune complexes) 3. vessel wall endothelial injury causing platelet activation followed by activation of the haemostatic systém(. e. g Gram-negative sepsis, extensive burns, prolonged hypotension, hypoxia or acidosis)

pathogenesis of DIC occurs when monocytes and endothelial cells are activated or injured in certain diseases monocytes and endothelial cells generate tissue factor on the cell surface activating the coagulation cascade acute DIC…. . . explosive generation of thrombin depletes clotting factors and platelets activates the fibrinolytic system

BLEEDING into the subcutaneous tissues, skin, and mucous membranes OCCLUSION of blood vessels caused by fibrin in the microcirculation significant platelet and coagulation factor consumption BLEEDING may become a major feature chronic DIC…. . . less explosive, compensatory responses the likelihood of bleeding hypercoagulable state - changes can be detected by testing the coagulation system - thromboembolism

clinical features presentation varies mixture of thrombotic, haemorrhagic or mixed manifestations in various organ systems major problem and presenting feature of acute DIC is bleeding when occurs in patients with MOF prognosis is poor in some patients, Dic may be an agonal event and should not be treated presentation in pregnancy may be more sudden and unexpected

CONDITIONS ASSOCIATED WITH DIC • INFECTION bacterial viral: CMV, hepatitis viruses, HZV • OBSTETRIC amniotic fluid embolism placental abruption eclampsia retained dead fetus septic abortion

INTRAVASCULAR HAEMOLYSIS haemolytic transfusion reaction massive transfusion minor haemolysis • TRAUMA OR BURNS • VENOMS AND TOXINS • HEPATIC DISEASE • PROSTHETIC DEVICES intra-aortic balloon pump Leveen shunt cardiopulmonary bypass

• VASCULAR DISORDERS hereditary telangiectasia thrombotic thrombocytopaenic purpura vasculitis AV fistula angiosarcoma malignant hypertension • MALIGNANCY adenocarcinoma: prostate, lung, breast, pancreas haematological: acute promyelocytic leukaemia, myeloproliferative disease, myeloma

laboratory findings • results may be variable and difficult to interpret • significant DIC can be present despite normal PT, APTT and TT but conversely patients may have laboratory features of DIC without any clinical sequelae • the key tests in diagnosis are those that provide evidence for excesseve conversion of fibrinogen to fibrin within the circulation and its subsequent lysis • platelet- fibrin clots create a mesh in the microcirculation in which passing red cells may be traumatized, resulting in haemolysis

diagnosis combination of the clinical picture with supportive pattern of laboratory tests of the haemostatic systém evidence for the diagnosis thrombocytopenia, hypofibrinogenaemia, prolongation of the APTT, PT, TCT, elevation of fibrin degradation products ( D- Dimer test) - in chronic DIC, the laboratory findings are different from acute DIC - many of the usual tests of haemostasis are normal or near normal

diagnosis of acute DIC • clinical findings multiple bleeding sites, ecchymoses of skin, mucous membranes visceral hemorrhage, ischemic tissue • laboratory abnormalities • coagulation abnormalities: prolonged prothrombin time, activated partial thromboplastin time, thrombin time; decreased fibrinogen levels; increased levels of FDP (eg, on testing for FDP, D dimer) platelet count decreased, schistocytes on peripheral smear

diagnosis of chronic DIC • clinical findings - signs of deep venous or arterial thrombosis or embolism - superficial venous thrombosis, thrombosis without varicose veins - multiple thrombotic sites at the same time - serial thrombotic episodes • laboratory abnormalities - modestly increased prothrombin time - shortened or lengthened partial thromboplastin time - normal thrombin time - high, normal, or low fibrinogen level - high, normal, or low platelet count - increased levels of FDP (eg, on testing for FDP, D dimer)

therapy Blood component in haemorrhaging patient !!!! the use of heparin only in selected causes !!! FFP …. contains all the coagulation factors, main inhibitors, antithrombin III, protein C, in near normal quantities and should be used if haemorrhage is occurring. Cryoprecipitate…. . contains VIII complex as well as fibrinogen , factor XIII in concentrated form Platelet transfusion …. . in the presence of life-threatening haemorrhage

TREATMENT - treatment of the underlying disease is the mainstay of management of either acute or chronic DIC ! - additionally, acute DIC is treated with blood products TREAT THE UNDERLYING DISEASE - avoid delay - treat vigorously (eg, shock, sepsis, obstetrical problems)

manage the acute DIC without bleeding !!! No treatment !!! with ischemia with bleeding blood components as needed fresh frozen plasma cryoprecipitate platelet transfusions anticoagulants (see "with thromboembolism" below) after bleeding risk is corrected with blood products

manage the chronic DIC without thromboembolism no specific therapy needed but prophylactic drugs (eg, low-dose heparin, low-molecular-weight heparin) may be used for patients at high risk of thrombosis with thromboembolism heparin or low-molecular-weight heparin, trial of warfarin sodium (Coumadin).

management of sudden massive obstetric haemorrhage is similar to other cases of DIC except!!! the onset is more likely to be fulminant and unexpected is associated with greater depletion of coagulation factors, especially fibrinogen ( marked fibrinolysis) fresh blood is possibly warranted !once the uterus has been emptied and contracted, the haemostatic failure quickly resolves!
- Slides: 39