Hemostasis Platelets or thrombocytes Fragments of megakaryocytes a


Hemostasis

Platelets or thrombocytes • Fragments of megakaryocytes, a large cell in the bone marrow- 60 micrometer in diameter • One megakaryocyte gives about 1000 platelets • 1 -4 micrometer diameter • 150, 000 – 300, 000 per cmm of blood • No nuclei • Actin & myosin molecules for contraction • Special contractile protein Thrombosthenin • Thrombopoietin→↑ Megakaryocytes & Platelets production in the bone marrow
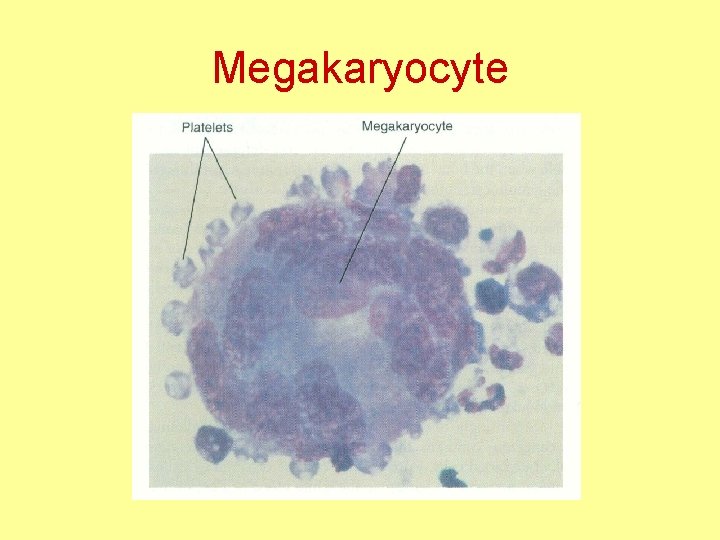
Megakaryocyte
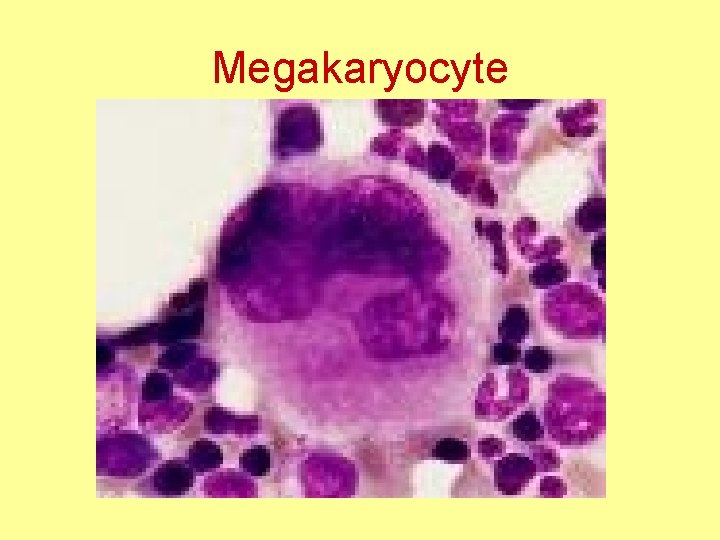
Megakaryocyte

Platelets or thrombocytes • Residual ER and Golgi complex synthesize enzymes and store Ca++ • Fibrin stabilizing factor (FSF) production • Mitochondria form ADP & ATP • Prostaglandin, Thromboxane A 2 -local hormones produced • ADP and Thromboxane A 2 activate Platelets • Growth factor for growth & multiplication of – Endothelial cells – Vascular smooth muscle cells – Fibroblasts

Platelets or thrombocytes • Glycocalyx on the cell membrane – Repulsive for normal endothelium – Adhesive to damaged endothelial cells and collagen fibers • Cell membrane contains Phospholipid involved in blood coagulation • Half life = 8 - 12 days • Removed from circulation by macrophages mostly in spleen and liver
Hemostasis • Prevention of blood loss • Four processes – Vascular constriction – Formation of platelets plug – Formation of blood clot – Fibrous organization of clot

Vascular constriction • Local myogenic spasm – due to direct trauma to smooth muscles of the vessels • Local vasoconstrictors – From the traumatized tissue and platelets e. g. thromboxane A 2 and Serotinin • Nervous reflexes – Due to pain & other sensory signals from the traumatized tissue – Vascular constriction is very strong when the vessel is severely damaged • Most effective in smaller vessels • Can significantly reduce blood loss for 20 -30 minutes

Formation of platelets plug • Contact with damaged vascular cells or Collagen • Swelling • Form spiked processes, Irregular shape Many pseudopodia • Release of sticky substances by contraction • Stick to each other, Collagen, von Willebrand factor etc.

Formation of platelets plug • Contraction and release of active substances • Secretion of ADP & thromboxane A 2 (TXA 2) • Both activate more and more platelets • A positive feedback cycle is initiated that forms a platelet plug and seals the hole within 1 minute
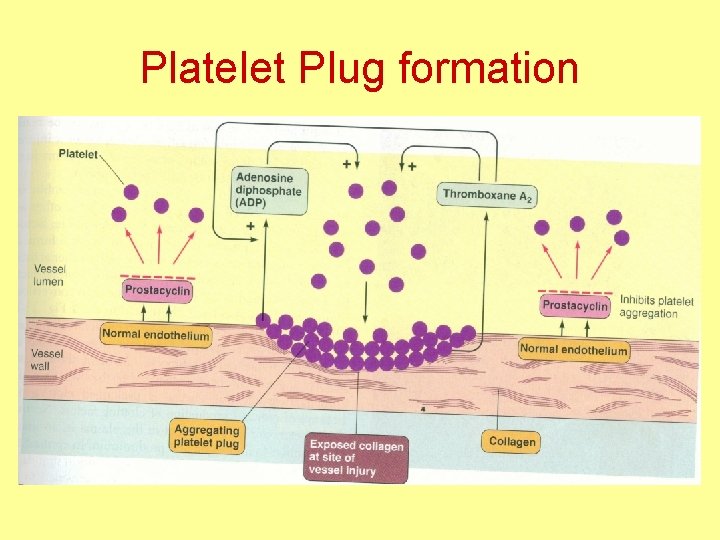
Platelet Plug formation

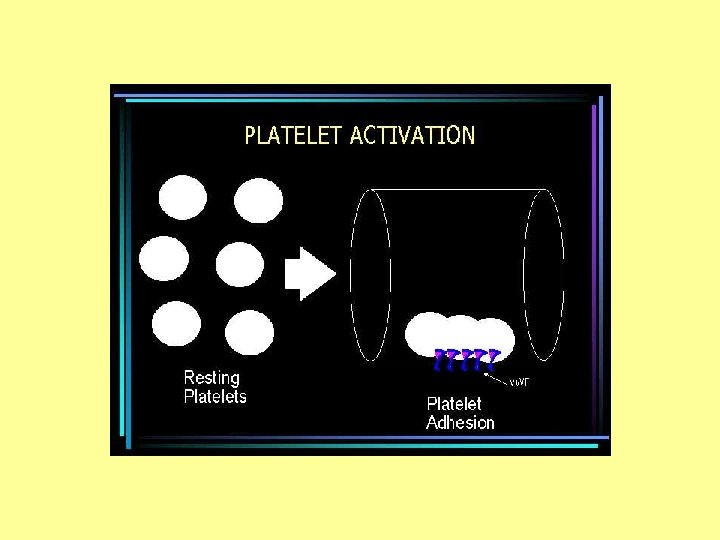



Formation of platelets plug • The platelet plug must be limited in size and extent • Plug should be limited to the damaged area only • Prevention of blocking the whole vessel • Prostacyclin, produced by endothelial cells is a strong inhibitor of platelet plug formation • It stops the +ve feed back cycle of plug formation

Formation of platelets plug • Initially loose plug but successfully blocks small openings in the capillary wall • Later on plug is invaded by fibrin meshwork in the clotting process for permanent repair • Important in day to day small damages in the capillary walls • Process may actually result in formation of additional endothelial cell membrane due to fusion of platelets and endothelial cells thereby closing the small holes in endothelial cells. • Failure of plug formation in thrombocytopenia causes Purpura

Thrombocytopenic purpura • • • Very low platelets count Tendency to bleed more Many small purplish blotches in the skin Count may be as low as 50, 000/cmm Count below 10, 000/cmm is lethal Idiopathetic thrombocytopenia – Antibodies formed against platelets • Treatment – Platelets transfusion from a fresh blood – Fresh whole blood

Blood coagulation • Conversion of fluid state of blood into semisolid state by activation and interaction of procoagulants in the blood • Set in motion with formation of the platelet plug • Many steps involving > 30 plasma factors – Proteins (made in the liver), – Vitamin K necessary for the synthesis of the liver proteins – Ca++
Formation of blood clot • Starts earlier (15 -20 seconds) if trauma is severe and late (1 -2 minutes) if trauma is trivial • The activating factors are – Traumatized vessel wall or surrounding tissue – Platelets – Plasma proteins • Clotting completes in 3 -6 minutes • Clot retracts after 20 minutes

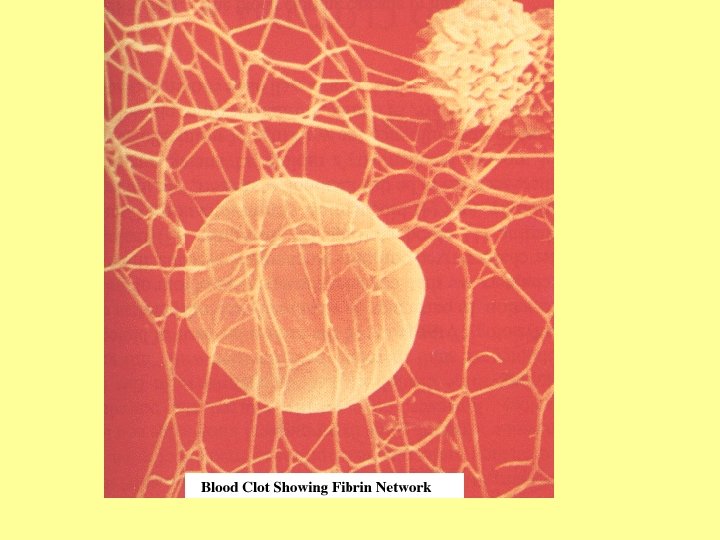
Blood coagulation • Last three phases of critical importance I. Prothrombin activator is formed II. Which converts prothrombin III. Which converts fibrinogen fibrin – Fibrin threads form a meshwork which traps blood cells and seals the hole until permanent repair

RBCs Trapped in Clot

Fibrous organization of clot • Within a few hours clot is invaded by fibroblasts which form connective tissue all through the clot. • The process is promoted by growth factor secreted by platelets. • Complete fibrous organization of the clot within about 1 -2 weeks.
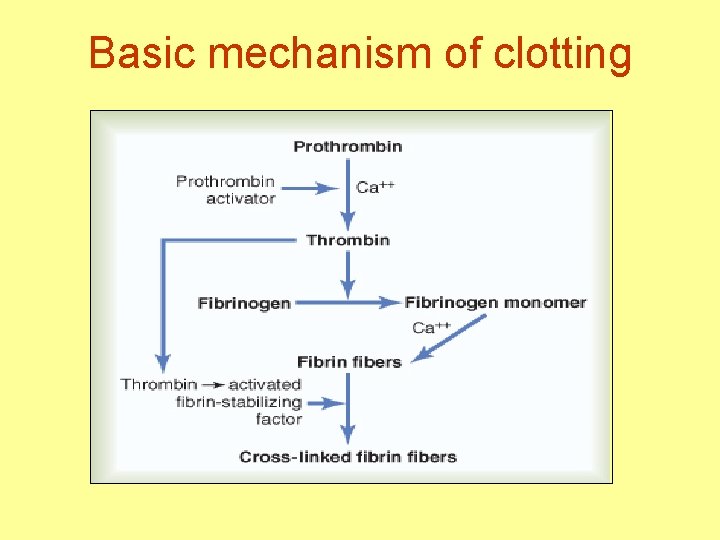
Basic mechanism of clotting

Prothrombin • • A plasma protein α 2 globulin M. W. 68700 15 mg/dl Broken to thrombin MW 33700 Synthesized in liver Vit K required for synthesis ↓ Vit K or liver disease → ↓ prothrombin →↑Bleeding tendency

Fibrinogen • • • Plasma protein 100 – 700 mg/dl M. W. 340, 000 Formed in liver Liver diseases →↓fibrinogen → bleeding tendency • Large molecule, does not leak into interstitial fluid which has very poor clotting property • When it leaks into interstitial space in pathological conditions. Interstitial fluid clots

Thrombin & clot formation • Thrombin → Breakdown of fibrinogen into fibrin monomer (4 small peptides removed) • Fibrin molecules polymerize to fibrin threads • Network of these fibers formed • Thrombin → Activation of Fibrin stabilizing factor (FSF) → Covalent bond between fibrin molecules and cross linkages → more stable meshwork of fibrin threads • FSF also formed from platelets entrapped in clot

Action of thrombin & clot formation • Formed elements entrapped in fibrin meshwork • Fibrin threads attached to damaged surface of blood vessels → rent sealed

Clot retraction • The platelets attached to fibrin threads and bond different threads • The platelet produce FSF which further strengthens the fibrin network • Platelets activate thrombosthenin, actin and myosin → contraction of platelets → retraction of clot to smaller mass → extraction of serum • The contraction is helped by Ca++ released from mitochondria, ER and Golgi complex of platelets • Clot retraction → damaged ends of blood vessels closer to each other • Serum extracted out of the clot • Serum = Defibrinated plasma

Thank-you Questions ? ?
- Slides: 36