HEMOSTASIS NENITA CUAABUEVA MD STAGES OF HEMOSTASIS 4

HEMOSTASIS NENITA CUA-ABUEVA, MD

STAGES OF HEMOSTASIS (4) (1). Vascular spasm (2). Platelet plug (3). Blood coagulation or clotting (4). Growth of fibrous tissue to close hole in the vessel


I. Vascular spasm : a). Nervous reflexes initiated by pain b). Local myogenic spasm initiated by direct damage to vessel wall

PLATELETS : Functional Characteristics of Platelets : (1). Non-nucleated (2). Have actin , myosin and thrombosthenin molecules (3). Have residual ER and Golgi apparatus , synthesize enzymes & store Ca⁺⁺ (4). Have mitochondria &enzyme system to synthesize ATP & ADP (5). Have enzyme system to synthesize prostaglandins (6). Have fibrin-stabilizing factor (7). Have growth factor that promote growth & multiplication of vascular endothelial cells, vascular smooth muscle cells & fibroblasts ---repair (8). Its surface has a glycoprotein coat that adheres to injured endothelial cells (9). Its membrane has phospholipids that activates intrinsic system of blood clotting (10). Half-life in the blood 8 to 12 days

II Platelet Plug Formation : Mechanism > when platelets come in contact with collagen fibers in the vascular wall – they swell & form radiating processes and become sticky and adhere to collagen in the tissues & to a protein( von Willebrand factor). They secrete ADP and form thromboxane A₂. – Activate nearby platelets ---- form loose plug. ** Platelet plugging is extremely important for closing minute holes in small blood vessels. > Fibrin threads formation & attaches to platelets = tight plug *

COAGULATION : > When blood is shed it loses its fluidity and becomes semi-solid. ( coagulation or clotting) ➢Clot begins to develop in 15 to 20 seconds ➢ After 20 minutes- an hour clot retracts


MECHANISM OF BLOOD COAGULATION 3 Essential Steps: I. Prothrombin activator formation II. Prothrombin activator in the presence of suff. amount of Calcium, causes conversion pf prothrombin to thrombin III. Thrombin causes polymerization of fibrinogen molecules to fibrin
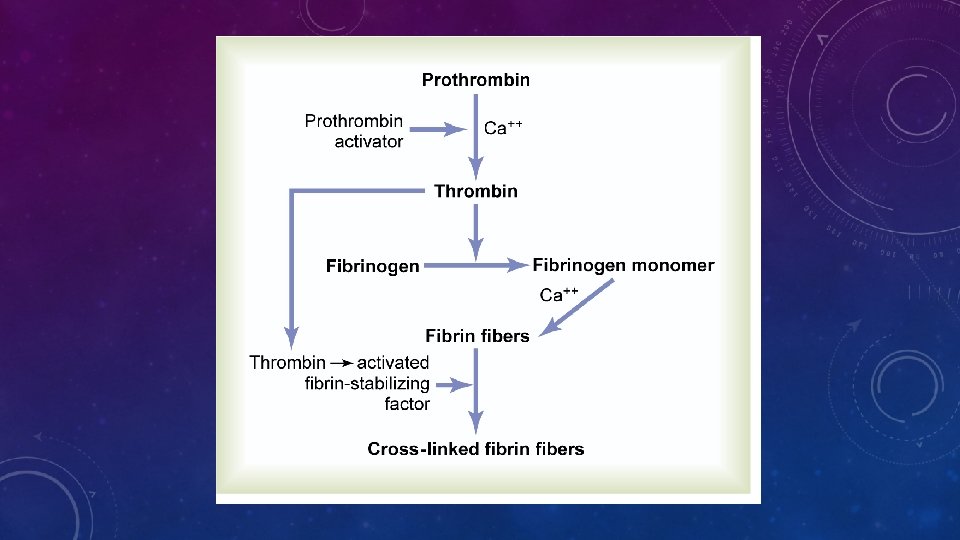

• PROTHROMBIN : > FORMED CONTINOUSLY IN THE LIVER > Ptothrombin --- thrombin > VITAMIN K required by the liver for normal activation of prothrombin > Plasma protein; mol. wt- =68, 700 ( alpha 2 -globulin ) THROMBIN : > protein enzyme with weak proteolytic activity > acts on fibrinogen to remove 4 low mol. wt peptides ---fibrin monomer. > polymerization of fibrin monomer

III. BLOOD CLOT : 1. Clot invaded by fibroblasts 2. Clot dissolution

• Positive Feedback on Clot Formation: • > Clot initiates a positive feedback to promote more clotting

FORMATION OF PROTHROMBIN ACTIVATOR: • 1. Extrinsic pathway -- Tissue factor. • 2. Intrinsic pathway -- Contact of Factor XII & platelets with collagen in the
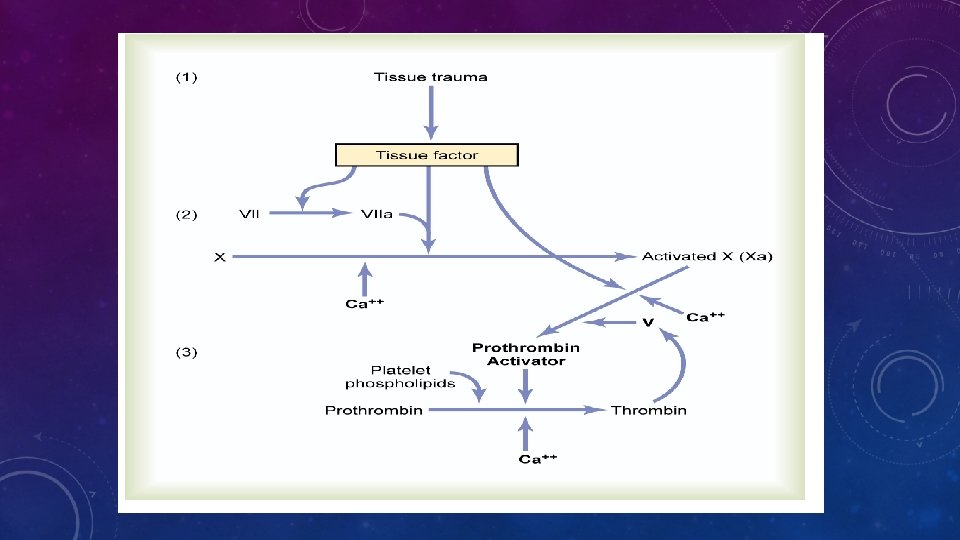
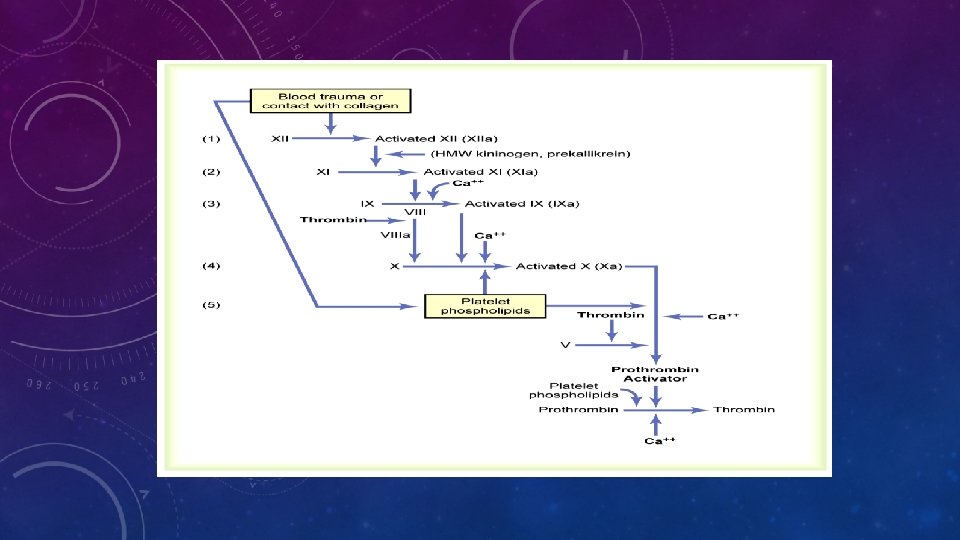

• Role of Calcium Ions in the Extrinsic and Intrinsic Pathways: > Except for the 1 st two steps in the intrinsic pathway , Ca++ are required for promotion or acceleration of all blood clotting reactions. > Absence of Ca++, blood-clotting by either pathway does not occur.

INTRAVASCULAR ANTICOAGULANTS : 1. Smoothness of the endothelial cell surface- contact activation of the intrinsic system 2, Glycocalyx on the endothelium factors & platelets prevents repels clotting 3. Thrombomodulin binds with thrombin ( thrombomodulin-thrombin complex) slows clotting process activates protein C ( acts as anticoagulant by inactivating Factors V & VIII

• IMPORTANT ANTICOAGULANTS IN THE BLOOD : • 1. Fibrin fibers -- formed during the process of clotting • 2. Antithrombin III or anti-heparin cofactor -- alpha globulin • 3. Heparin – conc. In the blood is normally low. ( Mast cells)

Lysis of Blood Clots: Activated profibrinolysin or plasminogen Plasmin (fibrinolysin ) PLASMIN: proteolytic enzyme ( trypsin) digest fibrin fibers and some other protein coagulants ( fibrinogen, Factors V, VIII, XII and prothrombin )

• CONDITIONS THAT CAUSE EXCESSIVE BLEEDING IN HUMANS : • 1. Vitamin K deficiency • 2. Hemophilia • 3. Thrombocytopenia ( platelet def)

• HEMOPHILIA : • • > Bleeding disease almost exclusively in males (TRAUMA) > 85% cases due to abnormality or deficiency of Factor VIII, (classic hemophilia, hemophilia A) • > 15% cases due to Factor IX def. • > Genetic transmission by way of the female chromosome (XX) • Hemophilia carrier ( XXd) transmitting the disease to half of male offspring, & the carrier state to half of female offspring. • > Injection of purified Factor VIII

• THROMBOCYTOPENIA: • > bleeding from small venules and capillaries. ( larger vessels in hemophilia ) • > small purple blotches on the skin- thrombocytopenic purpura • > bleeding occurs when platelet falls below 50, 000/ᵤl • > idiopathic thrombocytopenia

• PREVENTION OF BLOOD COAGULATION OUTSIDE THE BODY : • • HEPARIN Substances that decrease calcium ions in the blood ; (oxalate, citrates )

BLOOD COAGULATION TESTS: • BLEEDING TIME : 1 – 6 minutes • CLOTTING TIME : 6 – 10 minutes PROTHROMBIN TIME : 12 seconds

THANK YOU Nenita cua-abueva, md
- Slides: 26