Hemostasis and platelets HEMOSTASIS Definition Prevention of blood

Hemostasis and platelets
HEMOSTASIS Ø Definition : Prevention of blood loss by arrest of bleeding and maintenance of blood in fluid state.

Ø v v Mechanisms of hemostasis: Vasoconstriction Formation of platelet plug Formation of blood clot ( coagulation). Fibrinolysis.
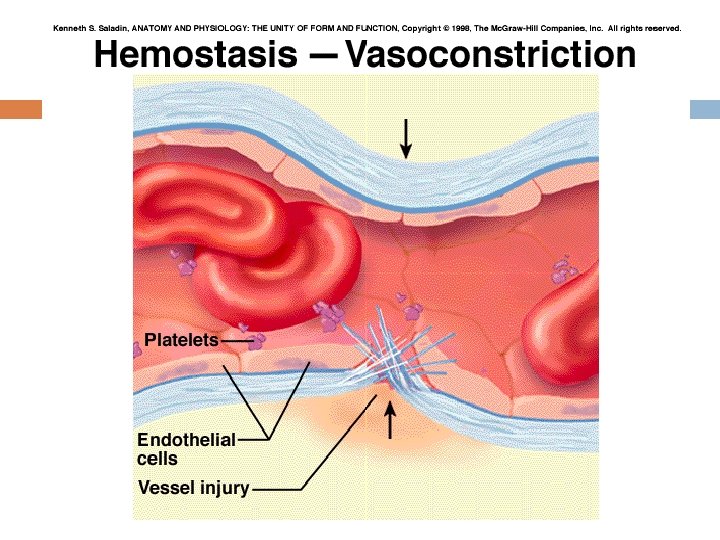
Immediately after a blood vessel is cut, the vascular smooth muscle automatically constricts. This results in a decrease in the flow of blood through the vessel that helps to limit blood loss. The vasoconstriction is caused by several factors: 1. Sympathetic nerve reflexes in response to pain 2. Local myogenic vasospasm in response to injury 3. Locally produced vasoconstrictors released from damaged tissue and from
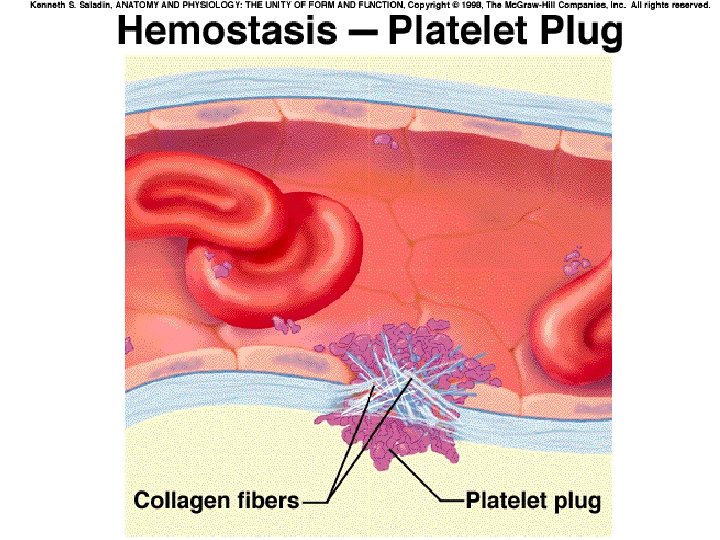
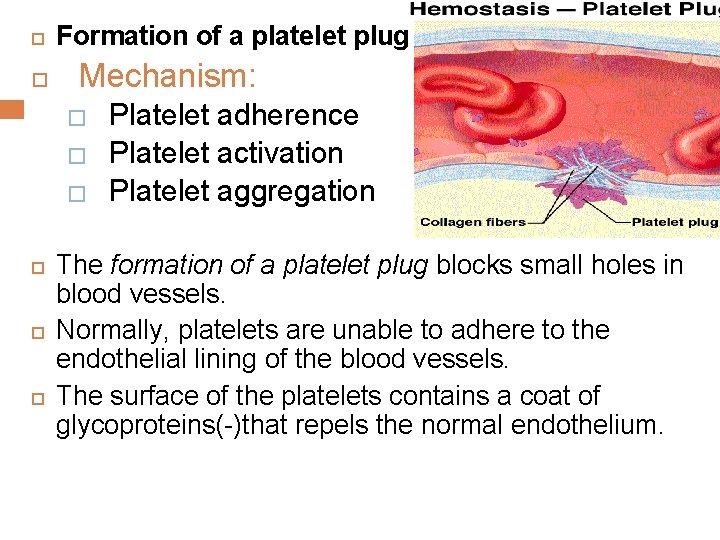
Formation of a platelet plug Mechanism: � � � Platelet adherence Platelet activation Platelet aggregation The formation of a platelet plug blocks small holes in blood vessels. Normally, platelets are unable to adhere to the endothelial lining of the blood vessels. The surface of the platelets contains a coat of glycoproteins(-)that repels the normal endothelium.

1. 2. 3. Interestingly, these same glycoproteins enable the platelets to adhere to damaged vessels. The cell membrane of platelets contains receptors for collagen, vessel wall known as von Willebrand factor. When platelets come into contact with a damaged vascular surface, in particular collagen fibers in the vessel wall or damaged endothelial cells, the platelets become activated. These activated platelets become “sticky” and adhere to the damaged tissue. They also release ADP and, a prostaglandin, which enhance the stickiness of other platelets thromboxane A 2 (aggregation of platelets to the sit of injury) serotonin(vasoconistrictor)

Pharmacy note: antiplatelet drugs Aspirin is powerful antiplatelet drug , which inhibits cyclooxygenase, an enzyme involved in arachidonic acid metabolism. Inhibition of cyclooxygenase blocks the synthesis of thromboxane. A 2 and prevent platelet aggregation. Asprin prescribed for pateints with: 1 - Thrombosis (formation of a blood clot within the vascular system) 2 -Atherosclerosis
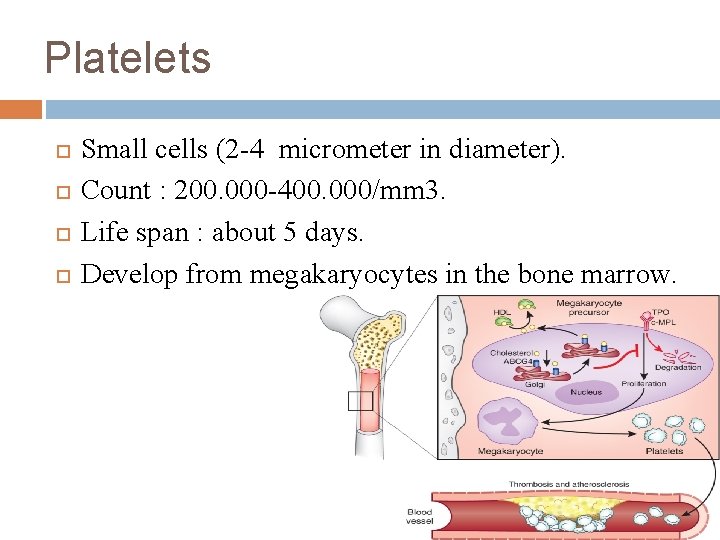
Platelets Small cells (2 -4 micrometer in diameter). Count : 200. 000 -400. 000/mm 3. Life span : about 5 days. Develop from megakaryocytes in the bone marrow.

Functions of platelets Ø ü ü Participates in hemostasis by : Vasospasm: release a vasoconstrictor (serotonin). Platelet plug formation (aggregation of platelets to close a hole in a blood vessels). Blood coagulation (release some clotting factor). Clot retraction: contraction of platelets to decrease the size of the clot.

Blood coagulation 1) 2) 3) Biochemical reactions that involve activation of clotting factors (which are proteins synthesized in the liver and present in the blood in inactive form). This complex process involves a series of reactions that result in formation of a protein fiber meshwork (fibrin)that stabilizes the platelet plug. Three essential steps lead to clotting: Activation of factor X Conversion of prothrombin into thrombin Conversion of fibrinogen into fibrin Calcium is needed for most steps of coagulation.
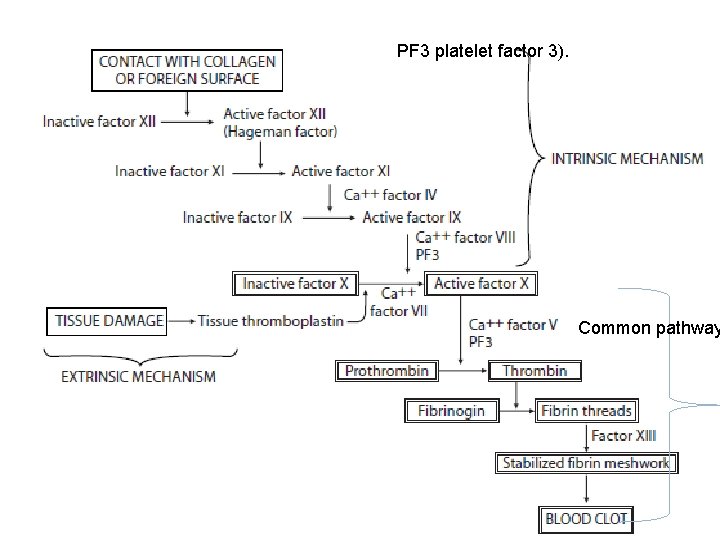
PF 3 platelet factor 3). Common pathway
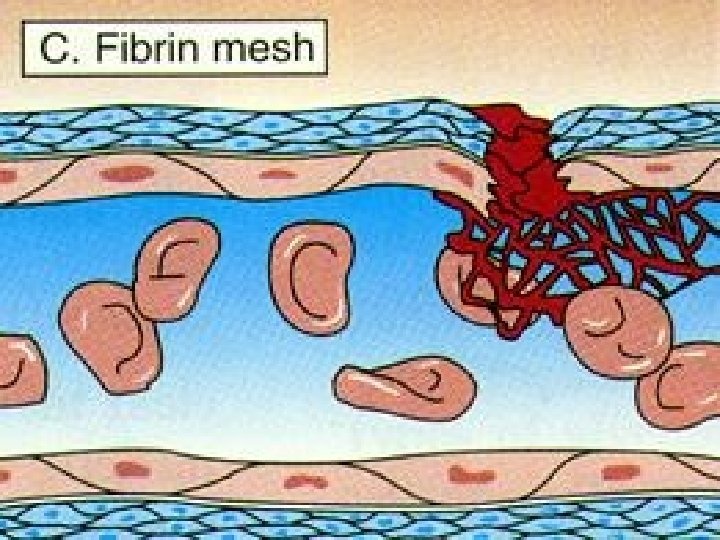

Fibrinolysis Once the blood vessel has been repaired, the clots must be removed in order to prevent permanent obstruction. Enzymatic degradation of fibrin by the enzyme plasmin. Plasmin is produced by the liver in inactive form (plasminogen). It is activated by many factors found in the blood or tissues.

Anticoagulants 1. 2. 3. 4. Prevention of blood clotting in the normal vascular system. Several factors contribute to the prevention of blood clotting in the normal vascular system: Smoothness of the endothelial lining prevents contact activation of the intrinsic mechanism. Tissue plasminogen activator activates plasmin to dissolve the fibrin continuously. The rapid blood flow. Heparin:

Pharmacy application: anticoagulant drugs o o o Warfarin (vitamin K antagonist). Prevent the synthesis of vitamin K-dependent coagulation factors in the liver (coagulation factors II, VII, IX, and X) Calcium chelating agents like oxalate, citrate and EDTA(remove the calcium ) Heparin: act directly by inhibition of thrombin and prevent the conversion of prothrombin to thrombin

Bleeding Disorders A deficiency of a clotting factor can lead to uncontrolled bleeding(Hemophilia) Examples: von Willebrand disease (the most common) hemophilia A for factor 8 deficiency hemophilia B for factor 9 deficiency. hemophilia C for factor 11 deficiency

PLASMA The fluid part of the blood. Content : Water (90%) transport medium; carries heat Electrolytes Membrane excitability; osmotic distribution of fluid between ECF and ICF; buffer p. H changes Nutrients, wastes, gases, hormones Plasma proteins

Plasma proteins In general, exert an osmotic(oncotic) effect important in the distribution of ECF between the vascular and interstitial compartments; buffer p. H changes There are three type of plasma protein: 1. Albumins Transport many substances; contribute most to colloid osmotic(oncotic) pressure 2. Globulins Alpha and beta Transport many waterinsoluble substances; clotting factors; inactive precursor molecules Gamma Antibodies (M, A, G, E & D) 3. Fibrinogen Inactive precursor for the fibrin meshwork of a clot §

Plasma proteins Ø Include : albumin, globulins & fibrinogens. Most of these are synthesized by the liver. Ø Functions of plasma proteins: Ø Oncotic pressure. Viscosity of blood. Clotting. Transport of hormones, ions …… Protection by antibodies (gamma globulins). Buffers to correct p. H in blood.

- Slides: 22