HEMOPHILIA A HEMOPHILIA B BY BRITTNI MCCLELLAN CLASSIFICATIONS

HEMOPHILIA A HEMOPHILIA B BY: BRITTNI MCCLELLAN

CLASSIFICATIONS Hemophilia A Hemophilia B Factor VIII Deficiency Factor IX Deficiency X-Linked Recessive 80 -85% of Cases 1: 5000 Male Births 10 -15% of Cases 1: 30, 000 Male Births
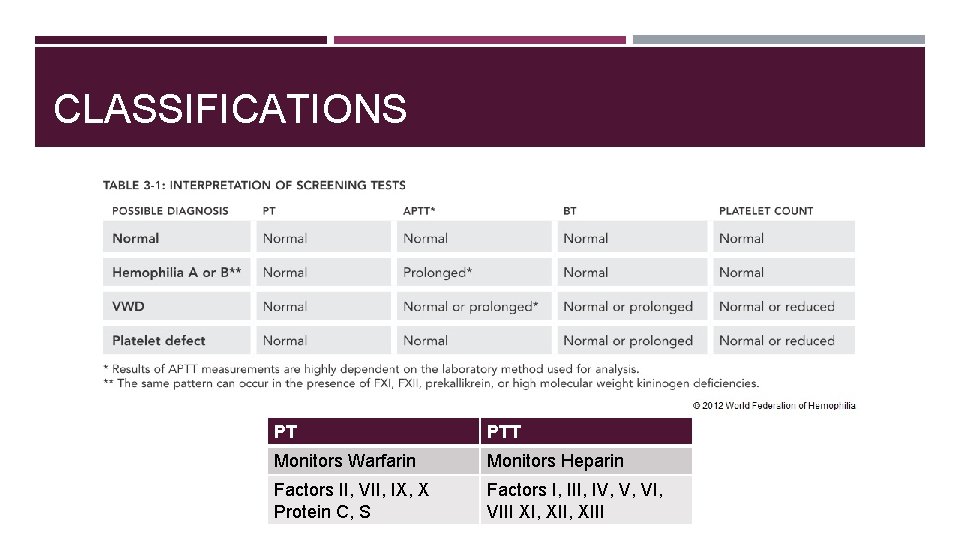

CLASSIFICATIONS PT PTT Monitors Warfarin Monitors Heparin Factors II, VII, IX, X Protein C, S Factors I, III, IV, V, VIII XI, XIII
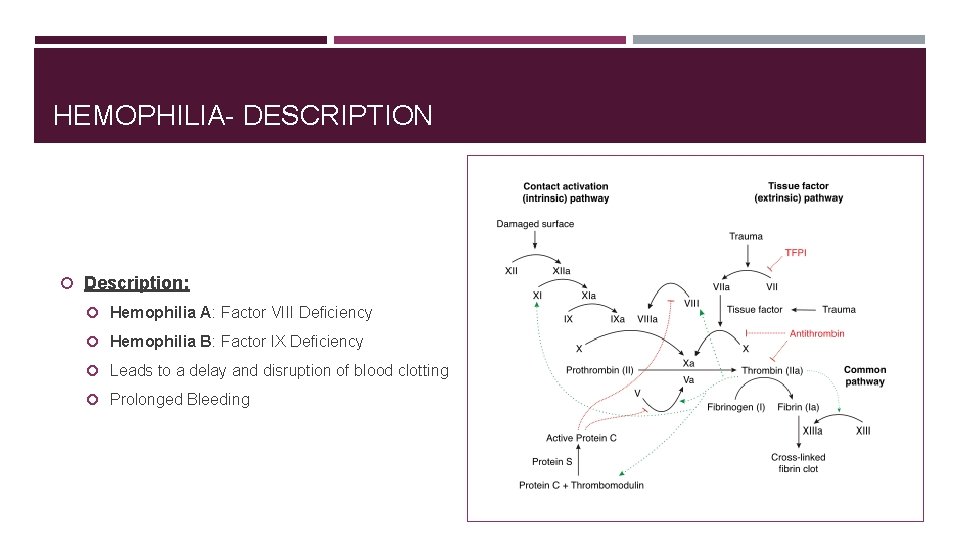
HEMOPHILIA- DESCRIPTION Description: Hemophilia A: Factor VIII Deficiency Hemophilia B: Factor IX Deficiency Leads to a delay and disruption of blood clotting Prolonged Bleeding
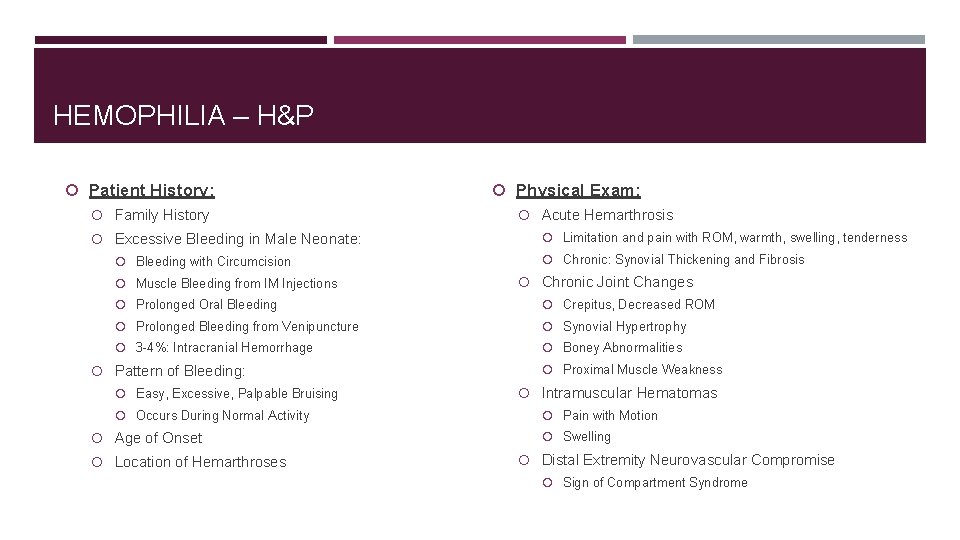

HEMOPHILIA – H&P Patient History: Family History Excessive Bleeding in Male Neonate: Bleeding with Circumcision Muscle Bleeding from IM Injections Physical Exam: Acute Hemarthrosis Limitation and pain with ROM, warmth, swelling, tenderness Chronic: Synovial Thickening and Fibrosis Chronic Joint Changes Prolonged Oral Bleeding Crepitus, Decreased ROM Prolonged Bleeding from Venipuncture Synovial Hypertrophy 3 -4%: Intracranial Hemorrhage Boney Abnormalities Pattern of Bleeding: Easy, Excessive, Palpable Bruising Occurs During Normal Activity Age of Onset Location of Hemarthroses Proximal Muscle Weakness Intramuscular Hematomas Pain with Motion Swelling Distal Extremity Neurovascular Compromise Sign of Compartment Syndrome
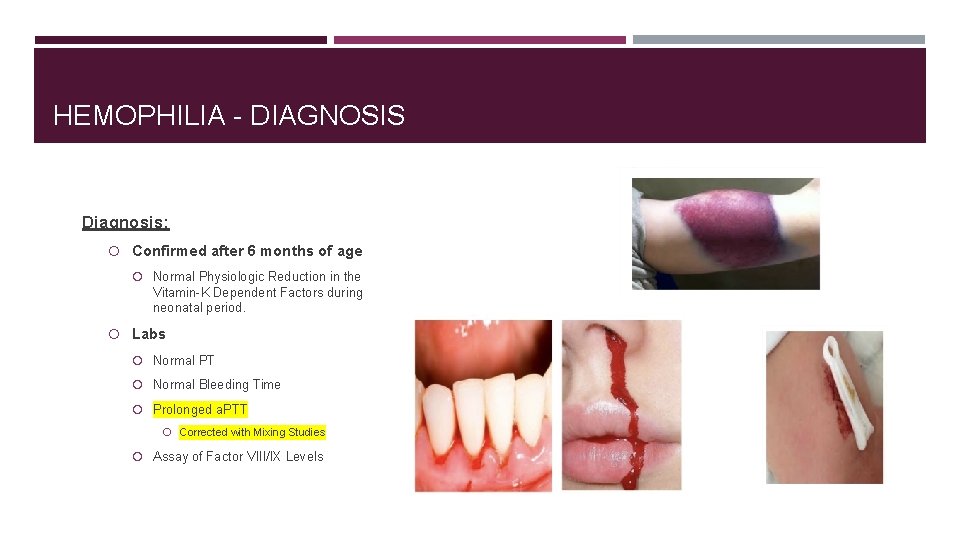
HEMOPHILIA - DIAGNOSIS Diagnosis: Confirmed after 6 months of age Normal Physiologic Reduction in the Vitamin-K Dependent Factors during neonatal period. Labs Normal PT Normal Bleeding Time Prolonged a. PTT Corrected with Mixing Studies Assay of Factor VIII/IX Levels

HEMOPHILIA – TREATMENT Medication Factor Replacement: Factor VII %Rise in Factor VIII x Body Weight (kg) x 0. 5 Factor IX Prothrombin Complex Concentrate (PCC) %Rise in Factor IX x Body Weight (kg) x 1. 4 Desmopressin Stimulates Release of Endogenous Factor VIII Contraindications Avoid Aspirin/NSAIDs Use Acetaminophen
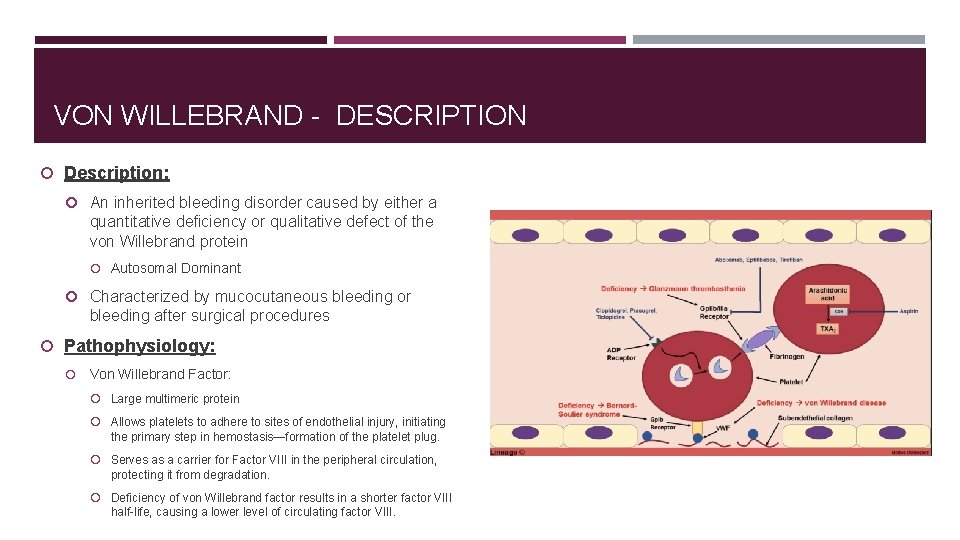
VON WILLEBRAND - DESCRIPTION Description: An inherited bleeding disorder caused by either a quantitative deficiency or qualitative defect of the von Willebrand protein Autosomal Dominant Characterized by mucocutaneous bleeding or bleeding after surgical procedures Pathophysiology: Von Willebrand Factor: Large multimeric protein Allows platelets to adhere to sites of endothelial injury, initiating the primary step in hemostasis—formation of the platelet plug. Serves as a carrier for Factor VIII in the peripheral circulation, protecting it from degradation. Deficiency of von Willebrand factor results in a shorter factor VIII half-life, causing a lower level of circulating factor VIII.
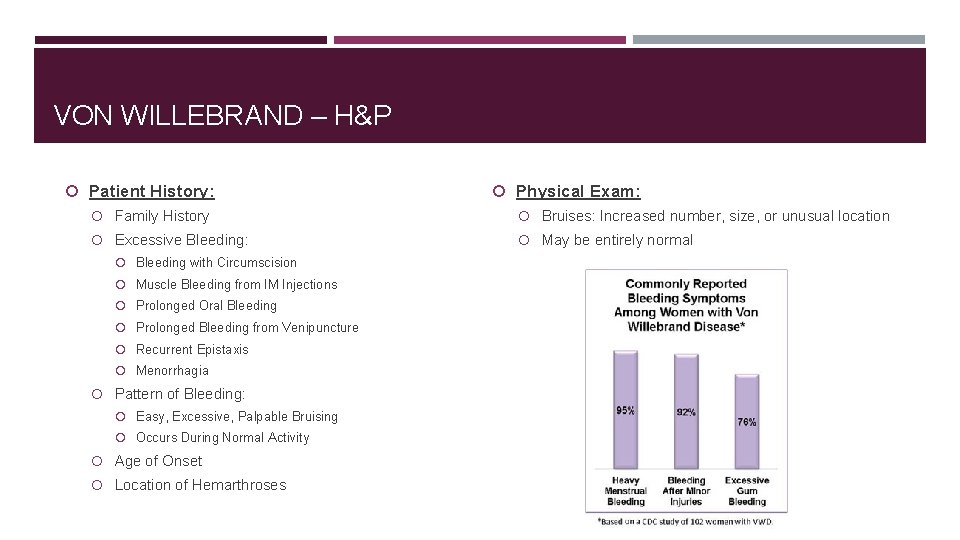

VON WILLEBRAND – H&P Patient History: Physical Exam: Family History Bruises: Increased number, size, or unusual location Excessive Bleeding: May be entirely normal Bleeding with Circumscision Muscle Bleeding from IM Injections Prolonged Oral Bleeding Prolonged Bleeding from Venipuncture Recurrent Epistaxis Menorrhagia Pattern of Bleeding: Easy, Excessive, Palpable Bruising Occurs During Normal Activity Age of Onset Location of Hemarthroses
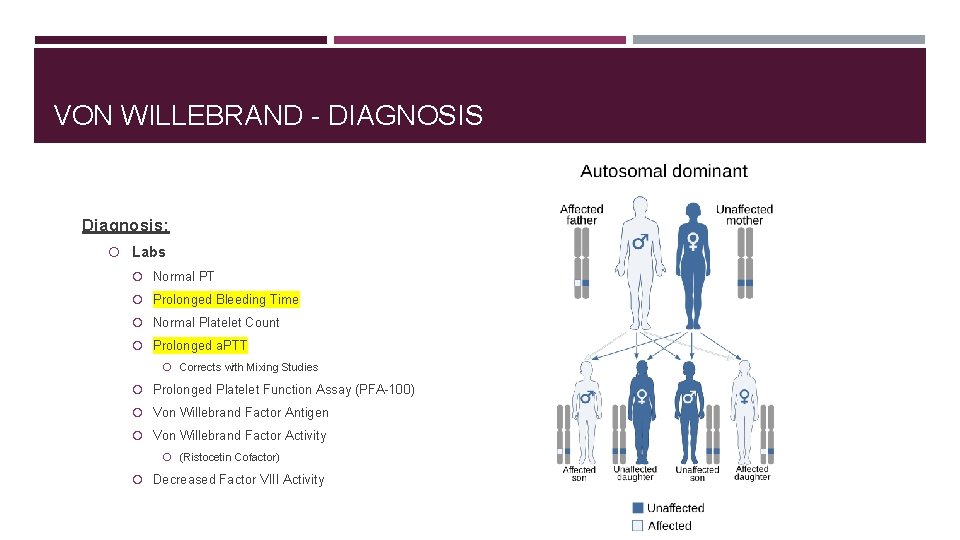
VON WILLEBRAND - DIAGNOSIS Diagnosis: Labs Normal PT Prolonged Bleeding Time Normal Platelet Count Prolonged a. PTT Corrects with Mixing Studies Prolonged Platelet Function Assay (PFA-100) Von Willebrand Factor Antigen Von Willebrand Factor Activity (Ristocetin Cofactor) Decreased Factor VIII Activity

VON WILLEBRAND – TREATMENT Medication Desmopressin (DDAVP): Synthetic analog of vasopressin that stimulates endothelial cell release of von Willebrand factor. Humate-P or Alphanate: Factor VIII concentrate products with adequate levels of von Willebrand factor Aminocaproic acid or tranexamic acid: Antifibrinolytics Stabilize the fibrin clot by inhibiting the physiologic process of clot lysis Best for oral mucosal bleeding Aspirin Increases Bleeding - C/I

QUESTION 1 A 16 -year-old male presents to the emergency department with a hematoma after falling during gym class. He claims that he has a history of prolonged nosebleeds and bruising/bleeding a) Decreased platelet count after minor injuries. Physical exam is b) Decreased levels of factor VIII unrevealing other than the hematoma. Labs are obtained showing an increased bleeding time c) Decreased levels of factor IX and an abnormal ristocetin cofactor assay. d) Decreased activity of ADAMTS 13 Coagulation assays reveal an increased partial thromboplastin time (PTT) and but a normal e) Decreased plasma fibrinogen prothrombin time (PT). The patient is given desmopressin and is asked to avoid aspirin. Which of the following findings is most likely to also be present in this patient? b) Decreased levels of factor VIII

QUESTION 2 A 5 -year-old boy accompanied by his mother presents to the pediatrician for his yearly exam. His medical history is notable for a mutation in the gene for clotting factor VIII, for which he is followed by a hematologist. His mother reports that the boy has required hospitalization for administration of factor VIII concentrate following minor trauma twice in the last year. The patient reports no current complaints and wants to return to kindergarten for the day. Which of the following would be consistent with the boy's diagnosis? Synovial thickening with fibrosis within the joints Prolonged bleeding time Elevated prothrombin time Mucosal bleeding Bleeding worse with aspirin a) Synovial thickening with fibrosis within the joints.
- Slides: 13