Hemodynamic pathology BY DR MAYS IBRAHEEM Hemodynamic is
Hemodynamic pathology BY DR. MAYS IBRAHEEM
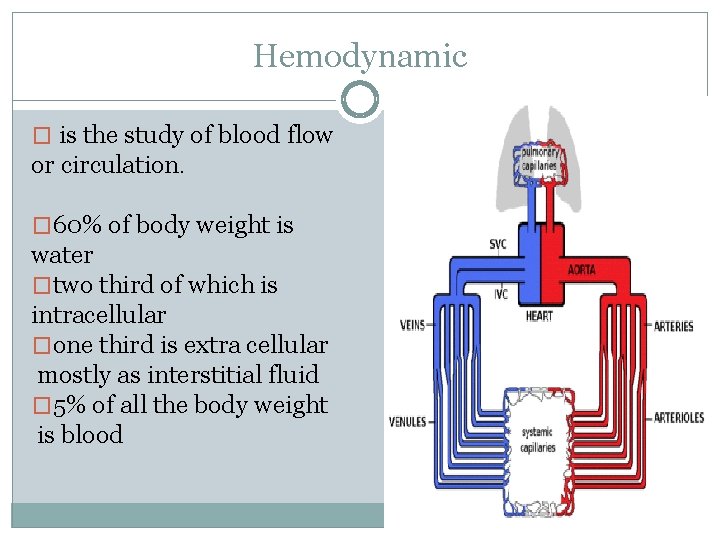
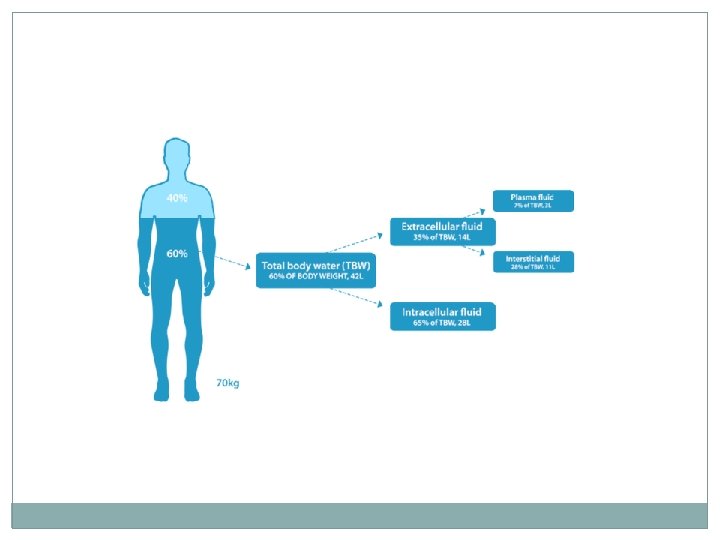
Hemodynamic � is the study of blood flow or circulation. � 60% of body weight is water �two third of which is intracellular �one third is extra cellular mostly as interstitial fluid � 5% of all the body weight is blood
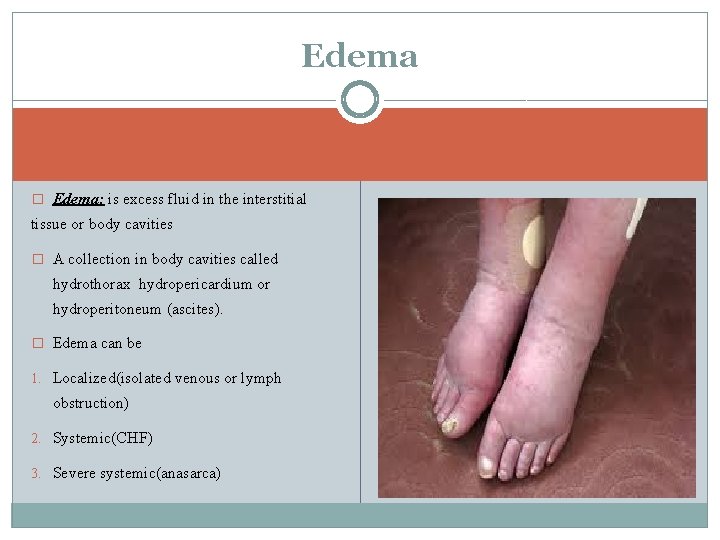
Edema � Edema: is excess fluid in the interstitial tissue or body cavities � A collection in body cavities called hydrothorax hydropericardium or hydroperitoneum (ascites). � Edema can be 1. Localized(isolated venous or lymph obstruction) 2. Systemic(CHF) 3. Severe systemic(anasarca)
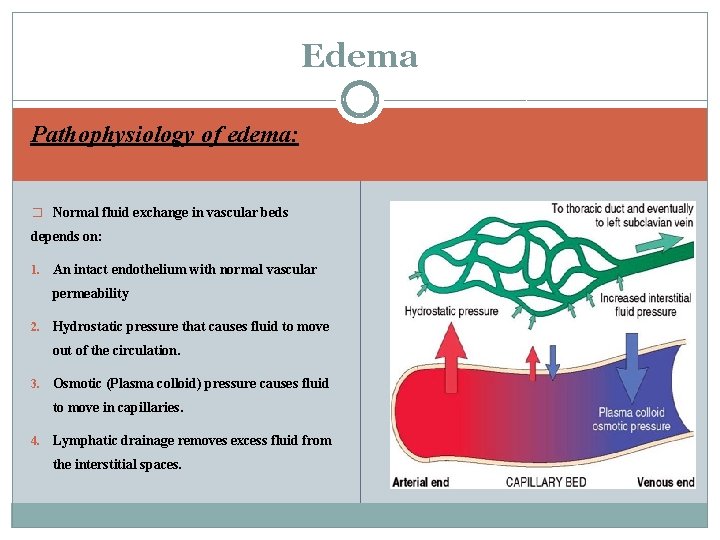
Edema Pathophysiology of edema: � Normal fluid exchange in vascular beds depends on: 1. An intact endothelium with normal vascular permeability 2. Hydrostatic pressure that causes fluid to move out of the circulation. 3. Osmotic (Plasma colloid) pressure causes fluid to move in capillaries. 4. Lymphatic drainage removes excess fluid from the interstitial spaces.
Factors leads to edema formation are Increased vascular permeability by the effect of inflammatory mediators 2. Increase hydrostatic pressure 3. Decrease osmotic pressure 4. Lymphatic obstruction. 1.

Increased hydrostatic pressure 1. Localized: example (deep venous thrombosis DVT) with edema of the affected limb. 2. Generalized: such in congestive heart failure � CHF →reduced cardiac output → reduced renal perfusion →activation of rennin angiotensin aldosterone axis → sodium & water retention by kidney. � This extrafluid load only increased venous pressure and no increase in cardiac output → edema. � Unless cardiac output restored or renal fluid retention reduced (e. g salt restriction , diuretics &/or aldosteron antagonists), vicious cycle of renal fluid retention & worsening edema result.

Reduced plasma osmotic pressure: (reduced plasma proteins) �Result from: Increased loss of albumin in nephrotic syndrome. Decrease protein synthesis as in cirrhosis, malnutrition.

Lymphatic obstruction � Usually localized and caused by: 1. Tumors a) Breast cancer treated by irradiation or surgery with resection of lymphatic drainage of upper limb lead to edema of the arm. a) Breast CA, infiltration & obstruction of superficial lymphatics will cause edema of breast skin and accentuation of depression in the skin at site of hair follicles giving what is called (peau-de-orange) 2. Parasitic infestation (filariasis→elephantiasis).

Definitions: � Exudate is an inflammatory, extravascular fluid contains high protein concentration (specific gravity ≥ 1. 020), with cellular debris � Transudate is excess, extravascular fluid with low protein content (specific gravity ≤ 1. 012; no cellular debris. � Pus is a purulent inflammatory exudate rich in neutrophils and cell debris. � Anasarca: is a severe generalized edema

Morphology of edema: �Microscopically: Clearing & separation of extra cellular matrix.
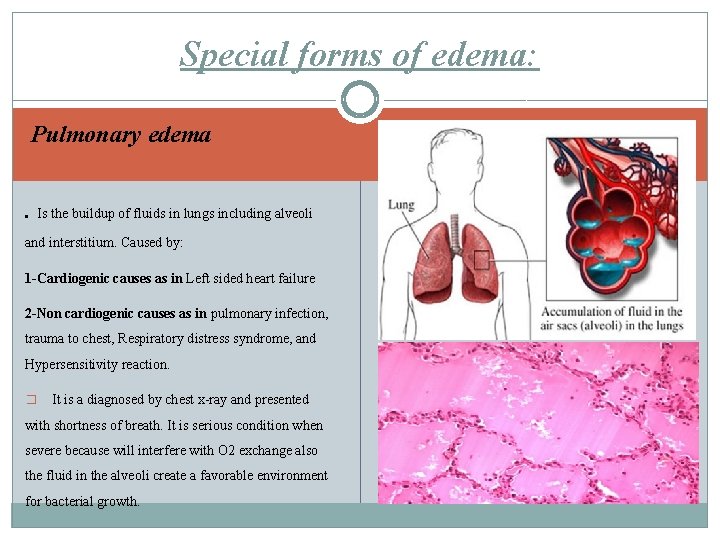
Special forms of edema: Pulmonary edema. Is the buildup of fluids in lungs including alveoli and interstitium. Caused by: 1 -Cardiogenic causes as in Left sided heart failure 2 -Non cardiogenic causes as in pulmonary infection, trauma to chest, Respiratory distress syndrome, and Hypersensitivity reaction. � It is a diagnosed by chest x-ray and presented with shortness of breath. It is serious condition when severe because will interfere with O 2 exchange also the fluid in the alveoli create a favorable environment for bacterial growth.

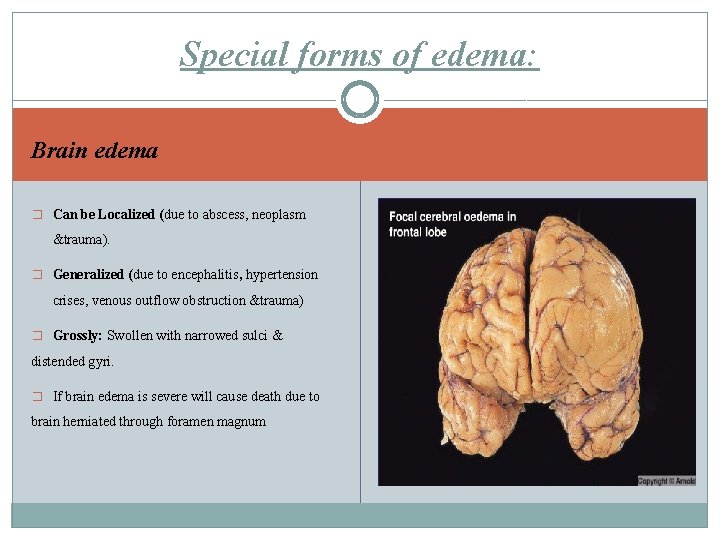
Special forms of edema: Brain edema � Can be Localized (due to abscess, neoplasm &trauma). � Generalized (due to encephalitis, hypertension crises, venous outflow obstruction &trauma) � Grossly: Swollen with narrowed sulci & distended gyri. � If brain edema is severe will cause death due to brain herniated through foramen magnum

Hyperemia & Congestion �*Hyperemia: is an active process of increase amount of blood in organ or tissue resulted from augmented blood flow due to arteriolar dilatation; the affected tissue is redder than normal. Eg: at site of inflammation, exercise, and flushing. �*Congestion: is passive process of increase amount of blood resulted from impair venous outflow from tissue (venous obstruction). The affected tissue is blue red color (cyanosis). 1. Localized venous congestion: e. g DVT of leg. 2. Generalized systemic congestion e. g. right ventricular failure in which there is decrease venous return to the heart with accumulation of blood in the venous side.

Morphology of generalized congestion: examples Liver congestion: 1. Acute congestion: distension of the central vein with occasional Necrosis of the hepatocytes surrounding the central vein because of pressure & hypoxia. The peripheral liver cells are normal or show fatty change. 2. Chronic congestion: Grossly: central hepatocyte are grossly red brown and slightly depressed (loss of cells) relative to surrounding uncongested tan liver (nut meg liver) Micro: centrilobular necrosis with hepatocyte drop out and hemosiderin laden macrophage � In long standing severe hepatic congestion (most commonly with heart failure), hepatic fibrosis (cardiac cirrhosis) develops.

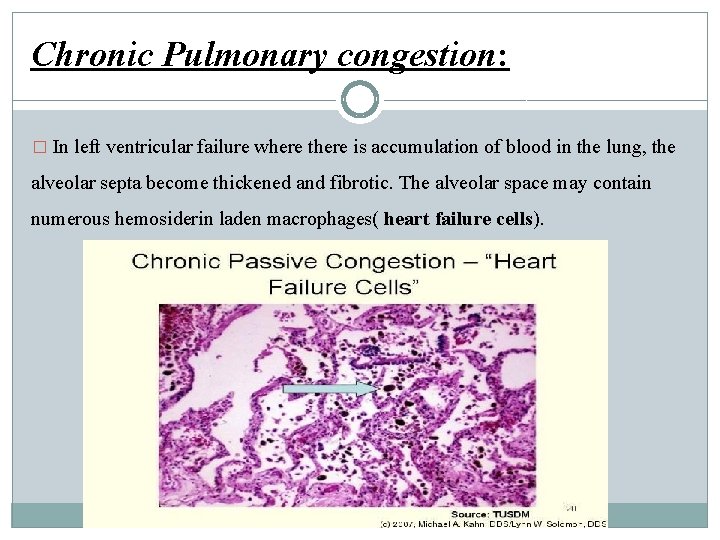
Chronic Pulmonary congestion: � In left ventricular failure where there is accumulation of blood in the lung, the alveolar septa become thickened and fibrotic. The alveolar space may contain numerous hemosiderin laden macrophages( heart failure cells).
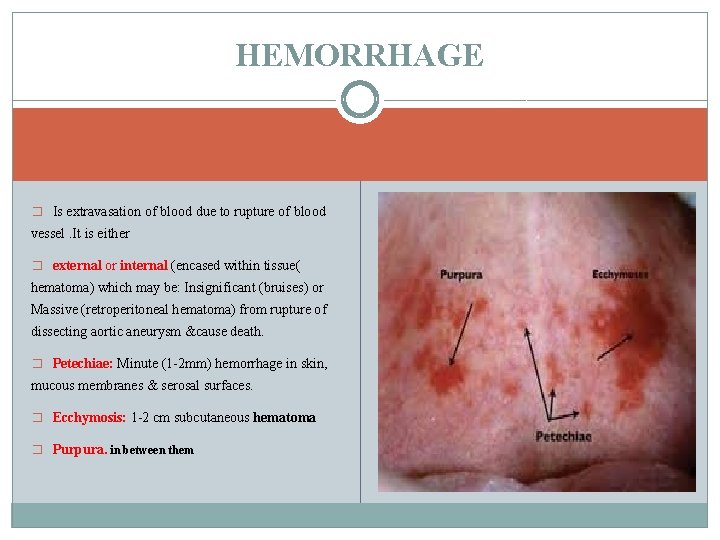
HEMORRHAGE � Is extravasation of blood due to rupture of blood vessel. It is either � external or internal (encased within tissue( hematoma) which may be: Insignificant (bruises) or Massive (retroperitoneal hematoma) from rupture of dissecting aortic aneurysm &cause death. � Petechiae: Minute (1 -2 mm) hemorrhage in skin, mucous membranes & serosal surfaces. � Ecchymosis: 1 -2 cm subcutaneous hematoma � Purpura. in between them

- Slides: 21