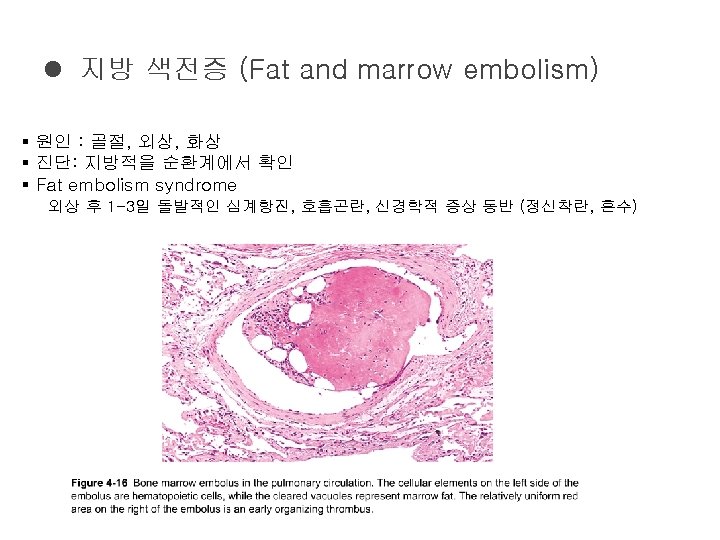
Hemodynamic Disorders Thromboembolic Disease and Shock Edema l

Hemodynamic Disorders, Thromboembolic Disease, and Shock 상계백병원 병리과 김정연
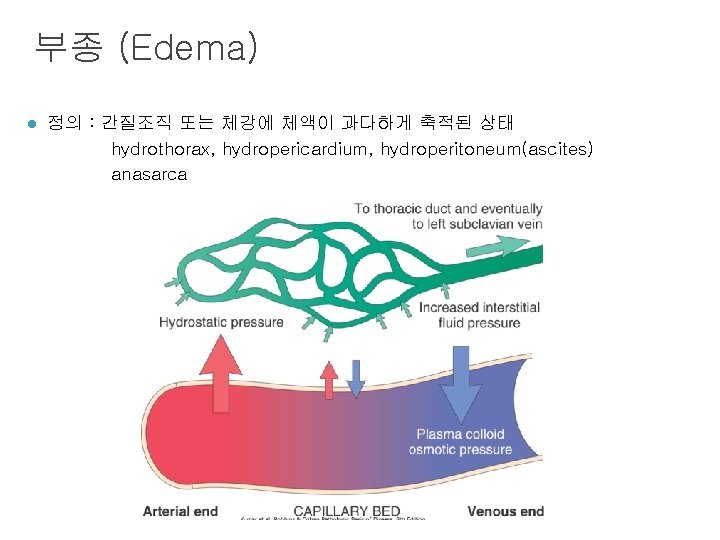
부종 (Edema) l 정의 : 간질조직 또는 체강에 체액이 과다하게 축적된 상태 hydrothorax, hydropericardium, hydroperitoneum(ascites) anasarca


Pathophysiologic Categories of Edema Increased hydrostatic pressure Impaired venous return Congestive heart failure Constrictive pericarditis Ascites venous obstruction or compression Thrombosis external pressure lower extremity inactivity with prolonged dependency Arteriolar dilation Heat Nuerohumoral dysregulation Reduced plasma osmotic pressure (hypoproteinemia) Protein-losing glomerulonephritis (nephrotic syndrome) Liver cirrhosis (ascites) Malnutrition Protein-losing gastroenteropathy

Pathophysiologic Categories of Edema Lymphatic obstruction Inflammatory Neoplastic Postsurgical Postirradiation Sodium retention Excessive salt intake with renal insufficiency Increased tubular reabsorption of sodium Renal hypoperfusion Increased renin-angiotensin-aldosterone secretion Inflammation Acute inflammation Chronic inflammation Angiogenesis
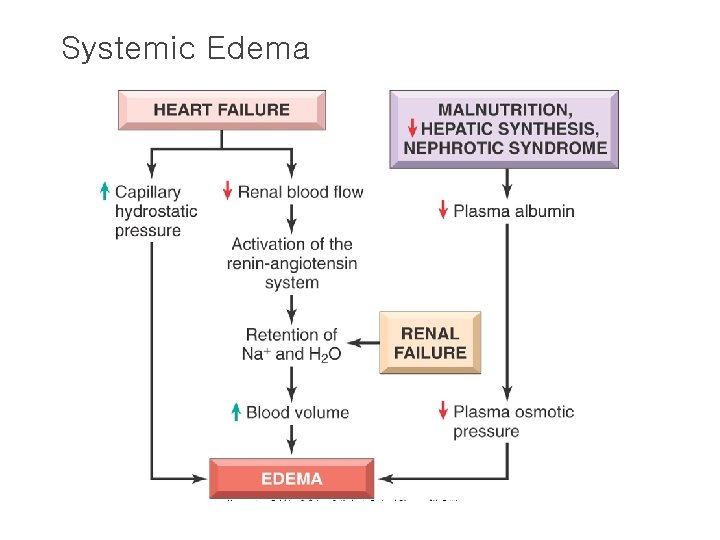
Systemic Edema


충혈(Hyperemia) vs. 울혈(Congestion) l 정의: 특정 조직 내 국소적인 혈류량의 증가 충혈: 능동적 과정, 동맥의 확장, 붉은 색 울혈: 수동적 과정, 정맥의 배류 장애로 발생, 암적색 형태학적 소견 (1) 폐울혈 급성 : capillary engorgement, septal edema, intra-alveolar hemorrhage 만성 : thickened and fibrotic septa, hemosiderin laden macrophage in alveoli (heart failure cell) l
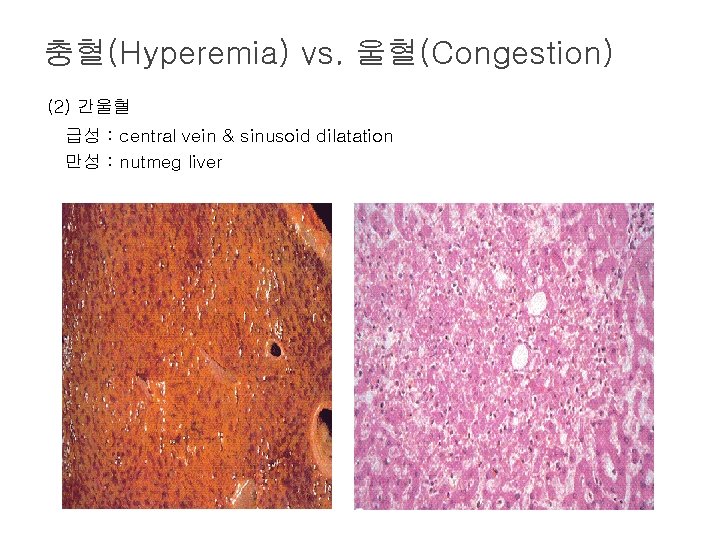
충혈(Hyperemia) vs. 울혈(Congestion) (2) 간울혈 급성 : central vein & sinusoid dilatation 만성 : nutmeg liver
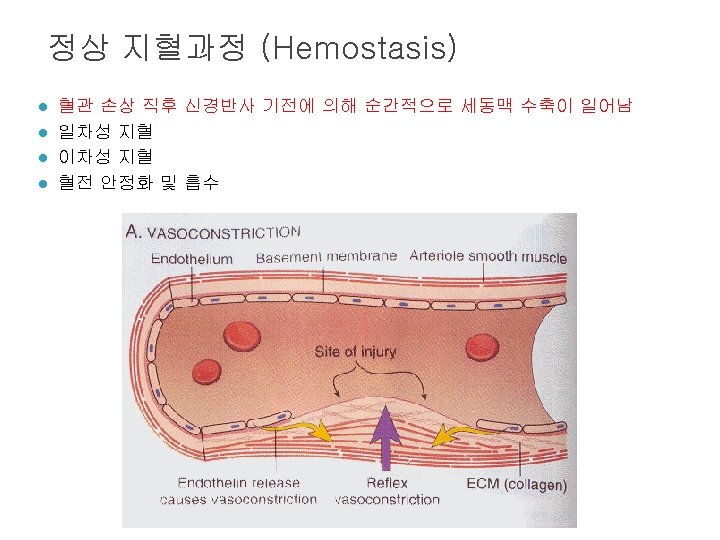
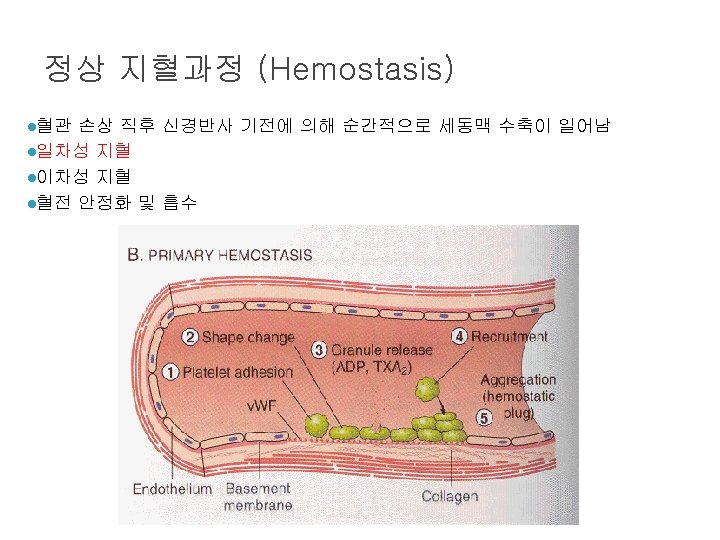
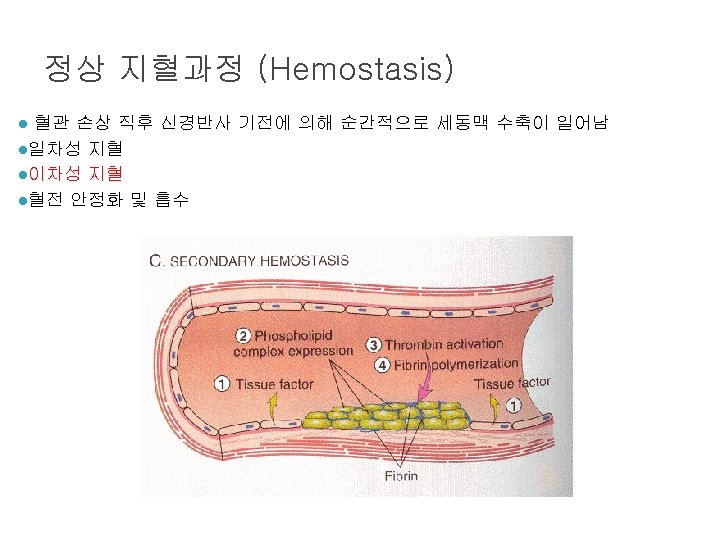
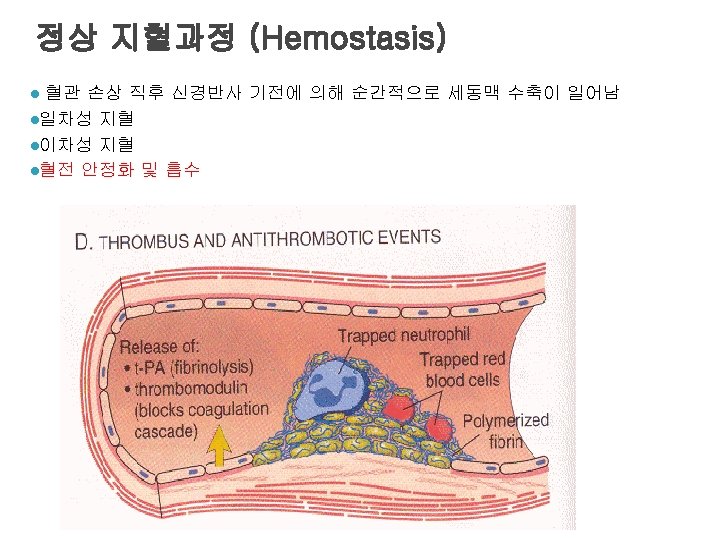

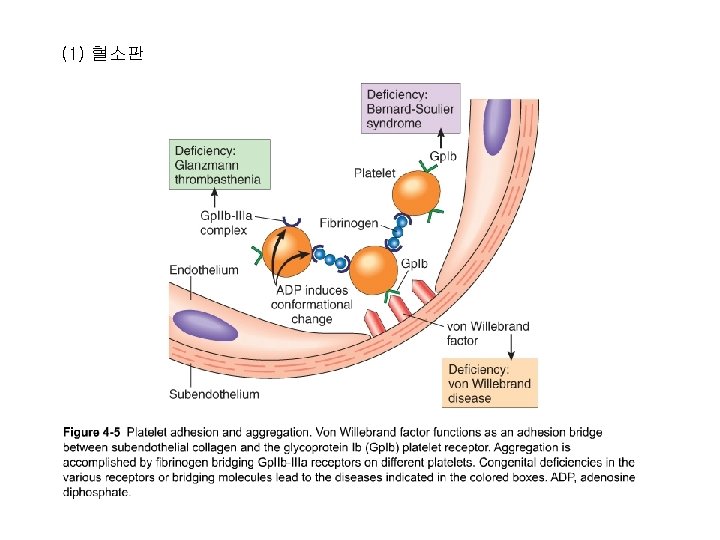

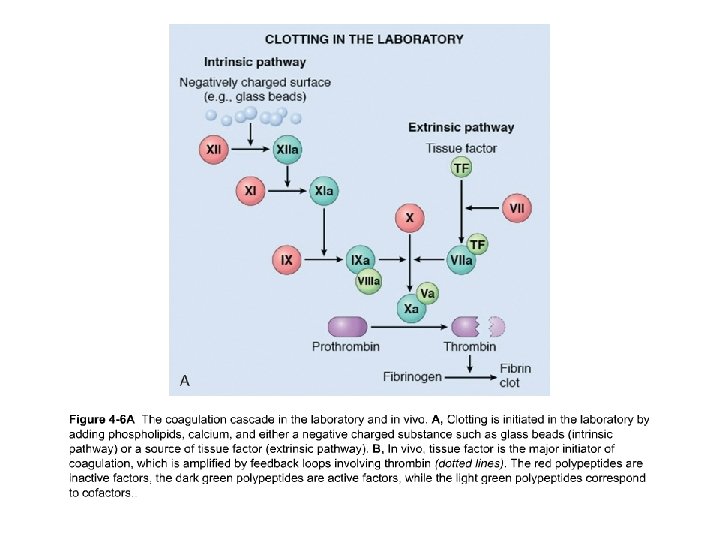
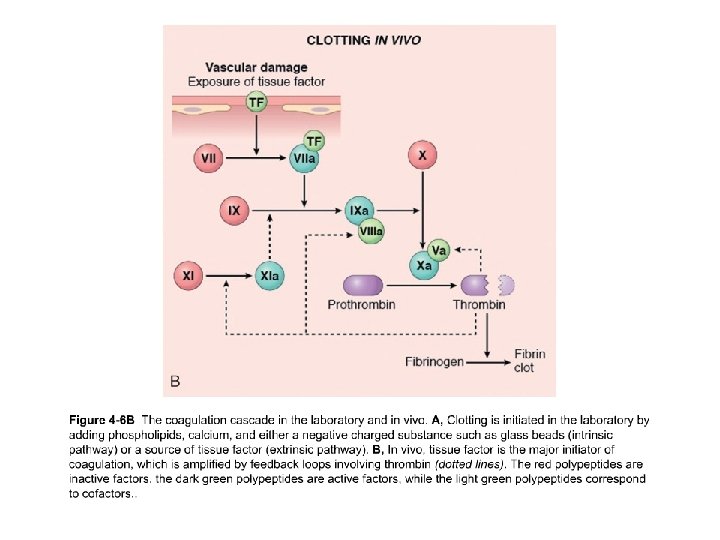
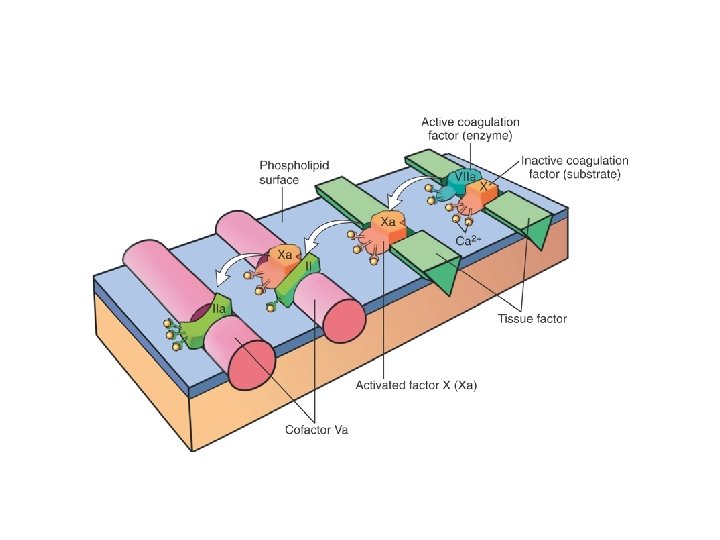
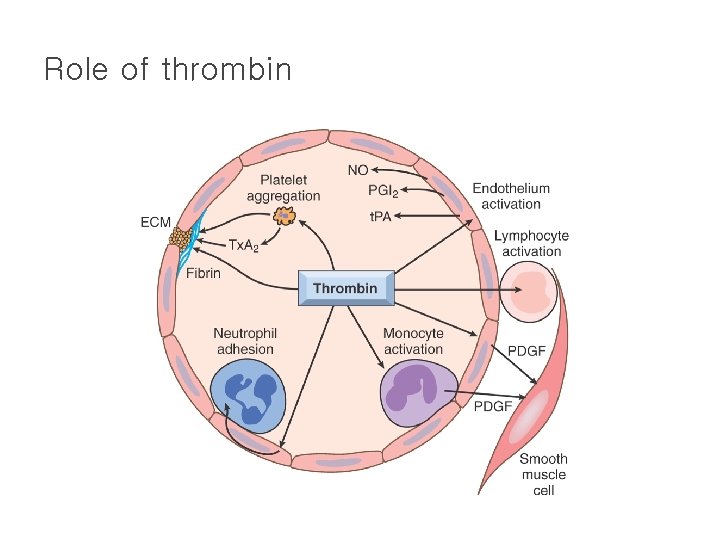
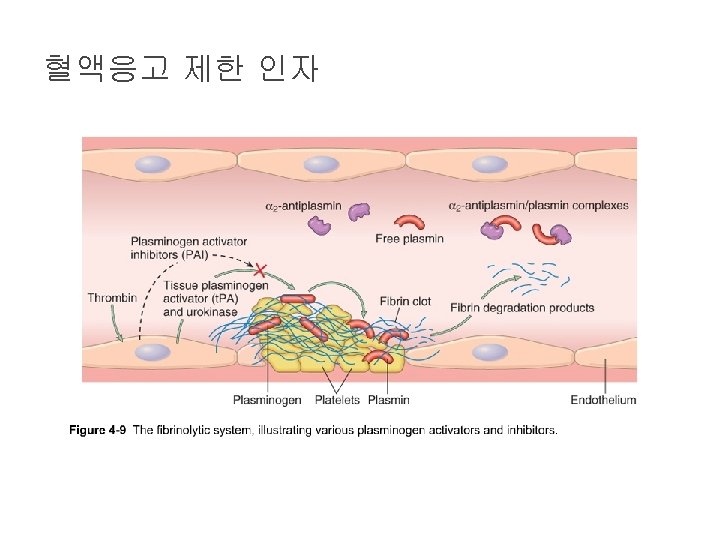
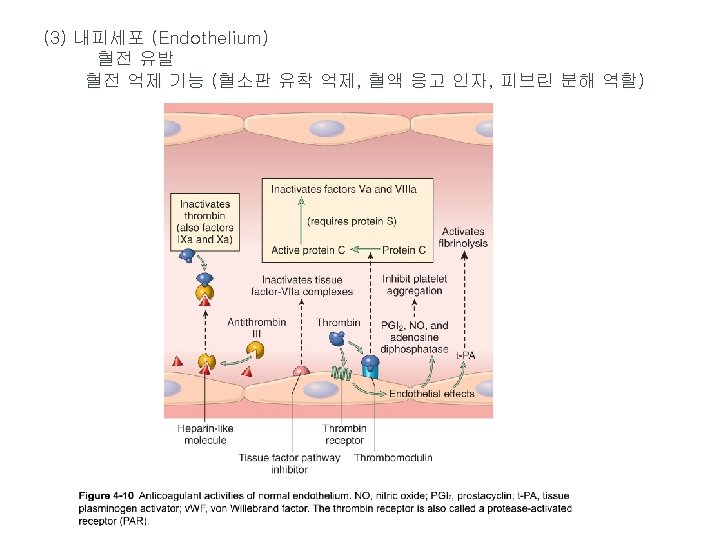
Role of thrombin

Hypercoagulable States Primary (genetic) Common Factor V mutation Prothrombin mutation Increased levels of factor VIII, IX, XI, or fibrinogen (genetics unknown) Rare Antithrombin III deficiency Protein S deficiency Protein C deficiency Very rare Fibrinolysis defects Homozygous homocystinuria Secondary (acquired) High risk for thrombosis Prolonged bed rest or immobilization Myocardial infarction Atrial fibrillation Tissue damage (surgery, fracture, burns) Cancer Prosthetic cardiac valves Disseminated intravascular coagulation Heparin-induced thrombocytopenia Antiphospholipid antibody syndrome Lower risk for thrombosis Cardiomyopathy Nephrotic syndrome Hyperestrogenic states (pregnancy) Oral contraceptive use Sickle cell anemia Smoking
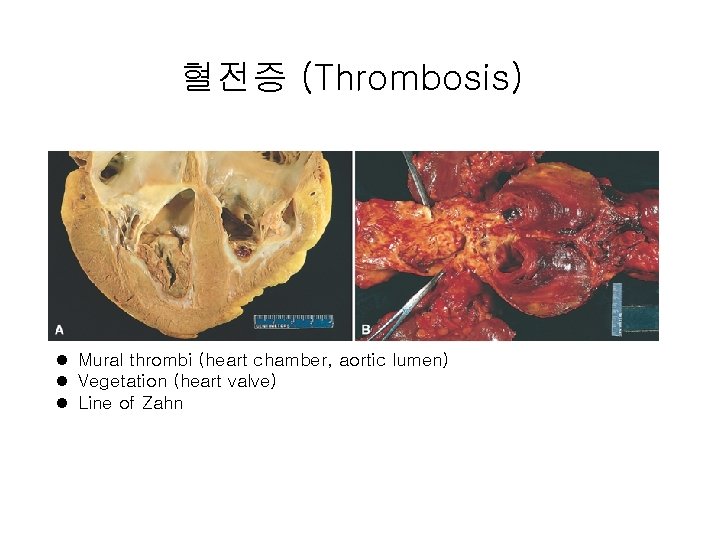
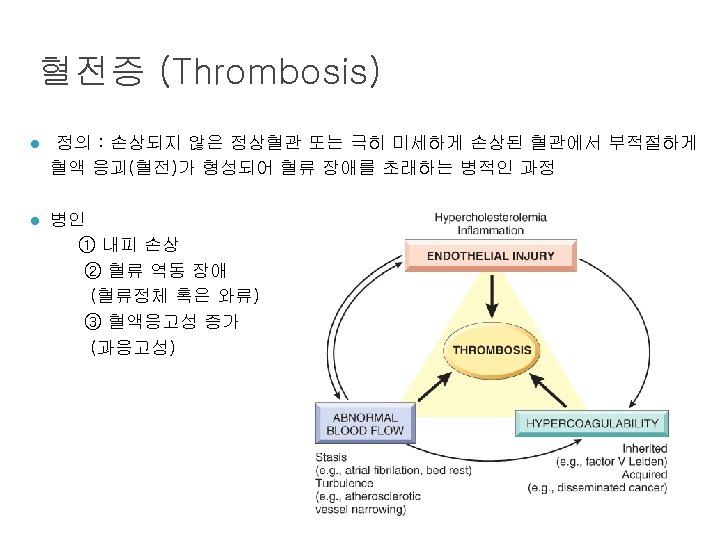
혈전증 (Thrombosis) l Mural thrombi (heart chamber, aortic lumen) l Vegetation (heart valve) l Line of Zahn
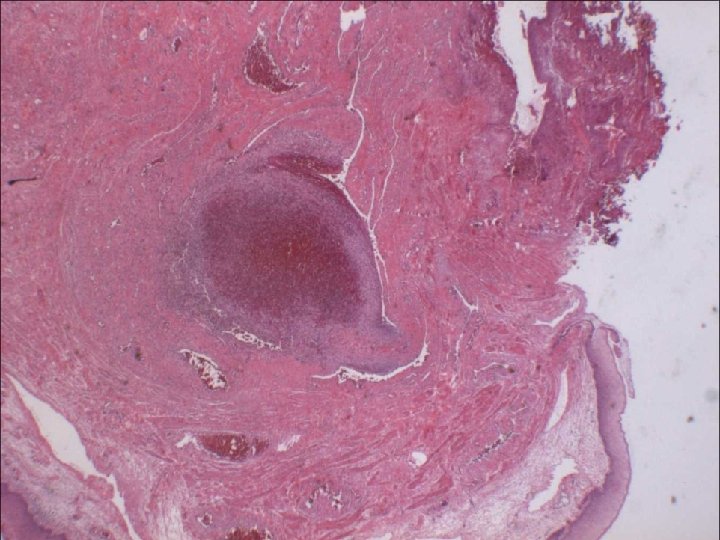
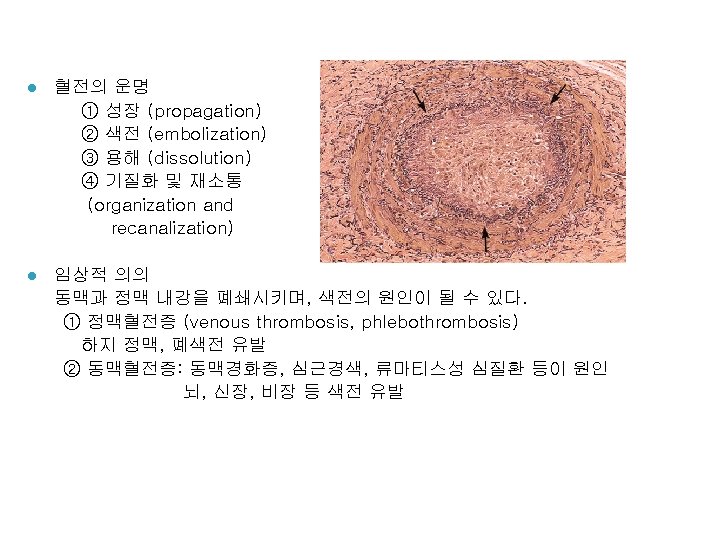


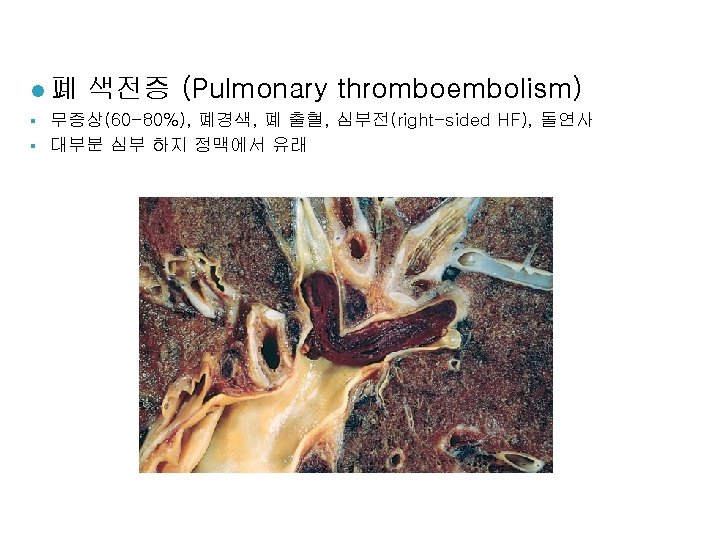


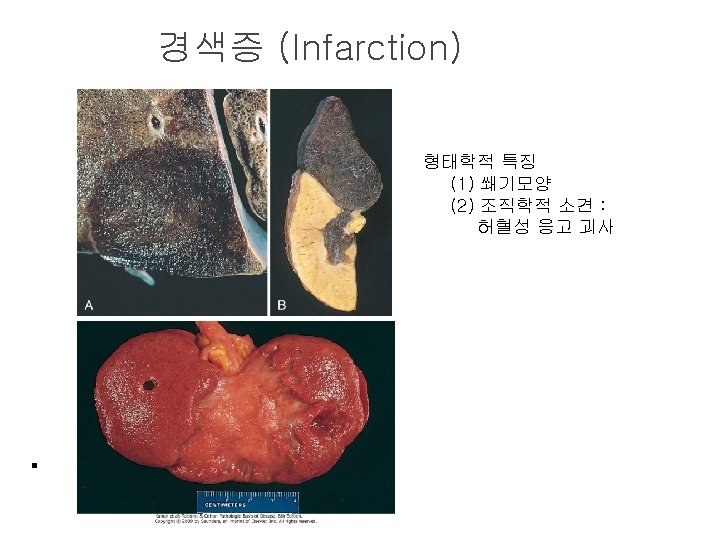

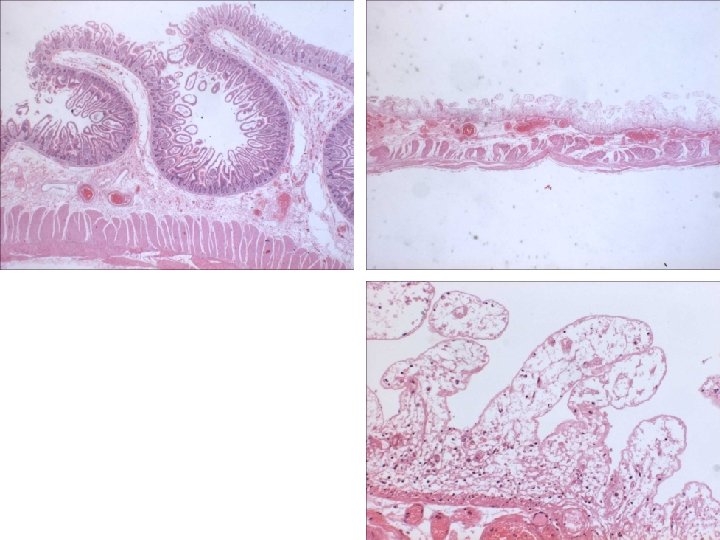
경색증 (Infarction) l 경색증 유발인자 (1) 혈류 공급의 양상 dual blood supply: lung, liver, forearm end artery: kidney, spleen (2) 동맥폐쇄가 일어나는 속도 collateral 발달 정도 (3) 저산소증에 대한 조직의 취약성 neuron, myocardial cell vs. fibroblast (4) 혈중 산소분압 (저산소증)
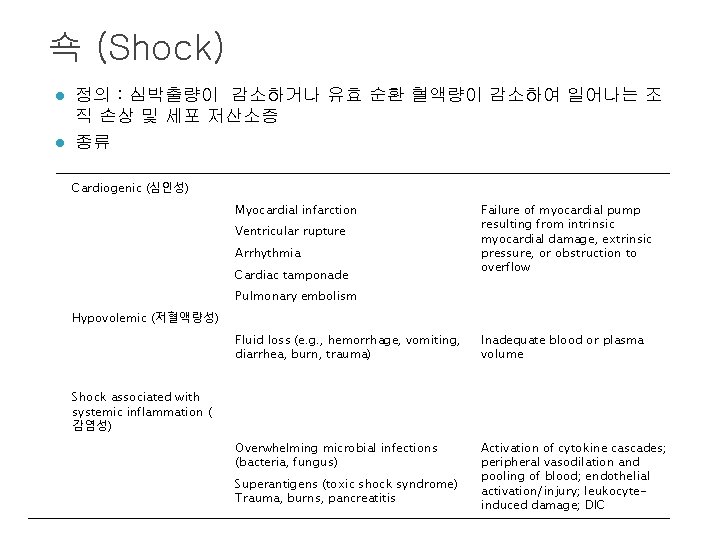
쇽 (Shock) l l 정의 : 심박출량이 감소하거나 유효 순환 혈액량이 감소하여 일어나는 조 직 손상 및 세포 저산소증 종류 of Shock Clinical Examples Principal Mechanisms Myocardial infarction Failure of myocardial pump resulting from intrinsic myocardial damage, extrinsic pressure, or obstruction to overflow Cardiogenic (심인성) Ventricular rupture Arrhythmia Cardiac tamponade Pulmonary embolism Hypovolemic (저혈액량성) Fluid loss (e. g. , hemorrhage, vomiting, diarrhea, burn, trauma) Inadequate blood or plasma volume Overwhelming microbial infections (bacteria, fungus) Activation of cytokine cascades; peripheral vasodilation and pooling of blood; endothelial activation/injury; leukocyteinduced damage; DIC Shock associated with systemic inflammation ( 감염성) Superantigens (toxic shock syndrome) Trauma, burns, pancreatitis
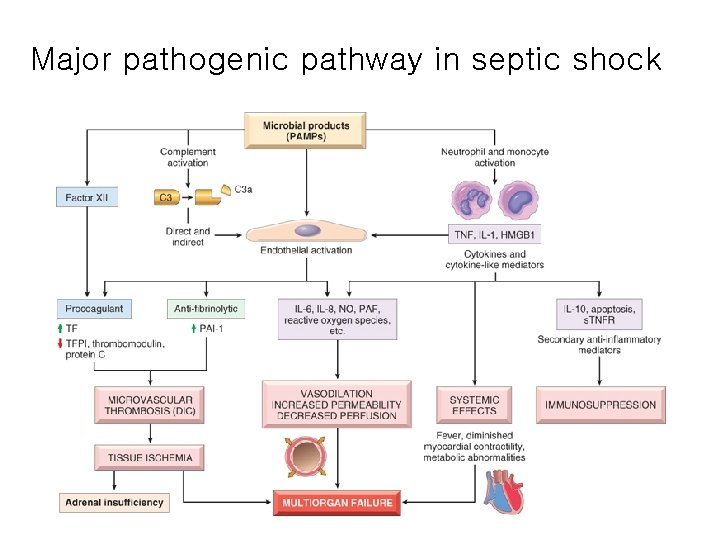
Major pathogenic pathway in septic shock

- Slides: 41