Hemodynamic Disorders Thromboembolic Disease and Shock Department of

Hemodynamic Disorders, Thromboembolic Disease, and Shock Department of Pathology College of Medicine Kyung. Hee University

Context Edema n Hyperemia and Congestion n Hemorrhage n Hemostasis and Thrombosis n Embolism n Infarction n Shock n

Introduction n The health of cells and organs Unbroken circulation n Normal fluid balance n n Vessel wall integrity n Intravascular pressure and osmolarity n Liquid state until time as injury to clot formation n Myocardiac infarction, pulmonary embolism, Cerebrovascular accident

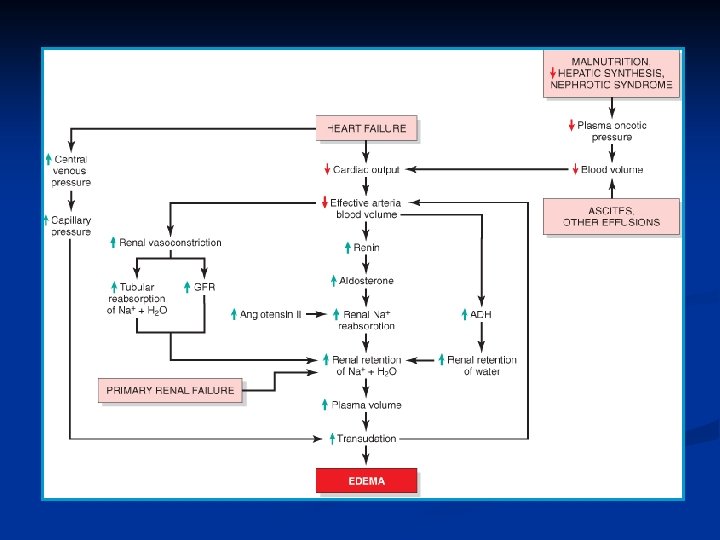
Edema n Definition n Increased fluid interstitial tissue spaces Hydrothorax, Hydropericardium, Hydroperitoneum Mechanism n n Increased hydroststic pressure: Cardiac edema Reduced plasma osmotic pressure: Nephrotic syndrome Lymphatic obstruction: parasite, irradiation, surgery Sodium and water retention
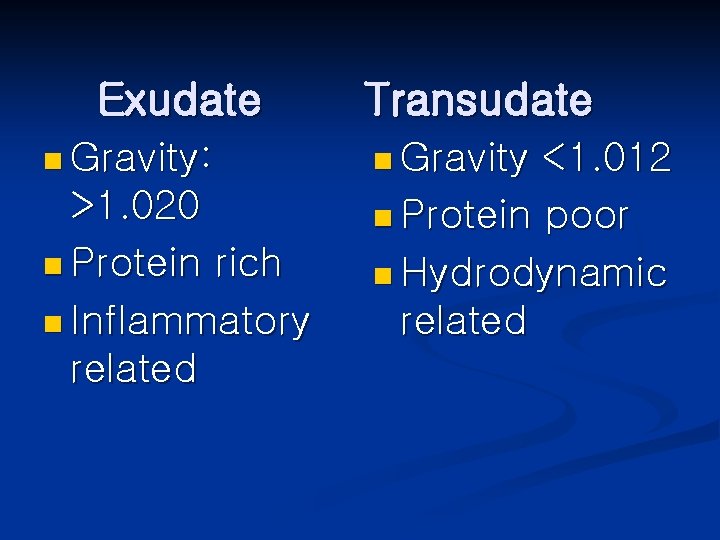
Exudate n Gravity: >1. 020 n Protein rich n Inflammatory related Transudate n Gravity <1. 012 n Protein poor n Hydrodynamic related

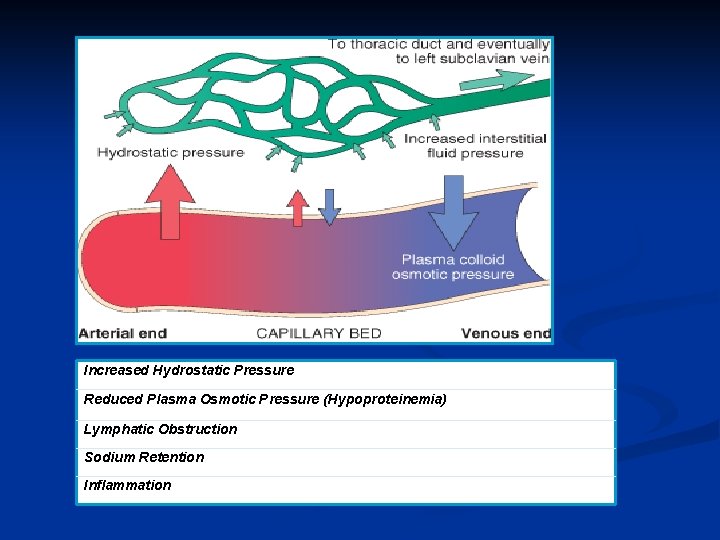
Increased Hydrostatic Pressure Reduced Plasma Osmotic Pressure (Hypoproteinemia) Lymphatic Obstruction Sodium Retention Inflammation


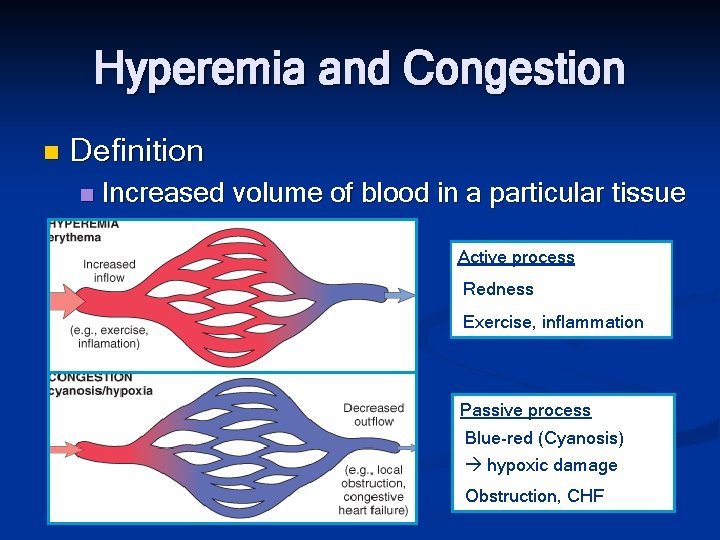
Hyperemia and Congestion n Definition n Increased volume of blood in a particular tissue Active process Redness Exercise, inflammation Passive process Blue-red (Cyanosis) hypoxic damage Obstruction, CHF




Hemorrhage n Definition n n Extravasation of blood due to vessel rupture Variety of patterns n Size n petechiae, purpura(≥ 3 mm), ecchymoses(>1~2 cm) n hemothorax, hemopericardium, hemoperitoneum, n ↑intravascular pressure, thrombocytopenia, defective PLT or clotting factor, vasculitis, trauma

Hemorrhage n Clinical significance by volume or rate of bleeding (up to 20%) hemorrhagic shock n Site of hemorrhage n n Subcutaneous n Brain: Fatal tissue: Usually OK

Hemostasis and Thrombosis n Normal hemostasis n Two important functions n n n Thrombosis n n n Maintain blood in clot-free state in normal vessels Induce rapid and localized hemostatic plug at the site of vascular injury The pathologic opposite of hemostasis Formation of blood clot in uninjured vasculature Three general component of both n Vascular wall, platelets, coagulation cascade
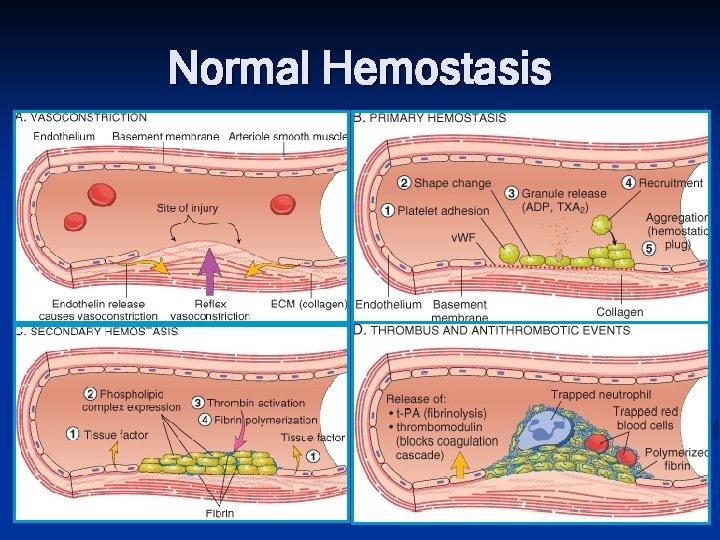
Normal Hemostasis

Endothelium • Antiplatelet activity ; PGI 2, NOx, ADP Antithrombotic Properties • Anticoagulant effects ; heparin-like molecules, thrombomodulin, tissue factor pathway inhibitor • Fibrinolytic effects ; tissue-type plasminogen activator (t-PA) Infectious agents, hemodynamic factors, plasma mediators, cytokines • Platelet effect: Prothrombotic Properties v. WF • Procoagulation effects: factor, tissue • Antifibrinolytic effects ; inhibitors of plasminogen activator (t-PA)
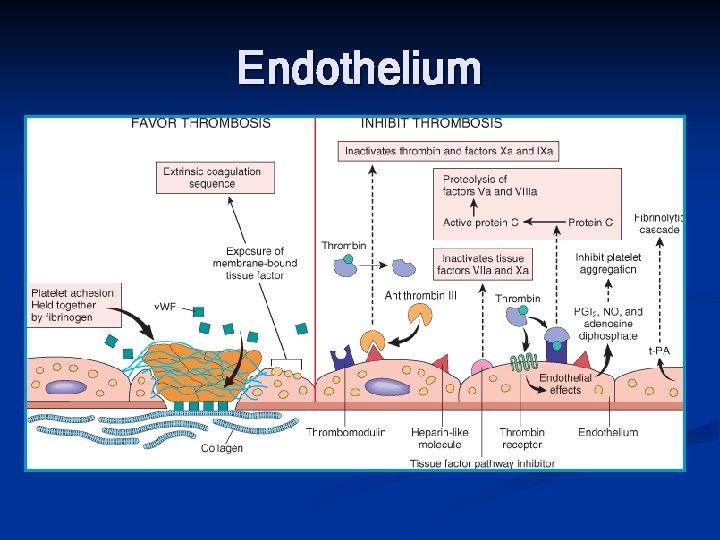
Endothelium

Platelet n Two specific types of granule Alpha granule P-selectin, fibronectin, factors V and VIII platelet factor 4, TGF-b n Dense bodies ADP, ATP, ionized calcium, histamine, serotonin, epinephrine n n Three general reactions n n n Adhesion and shape change Secretion Aggregation
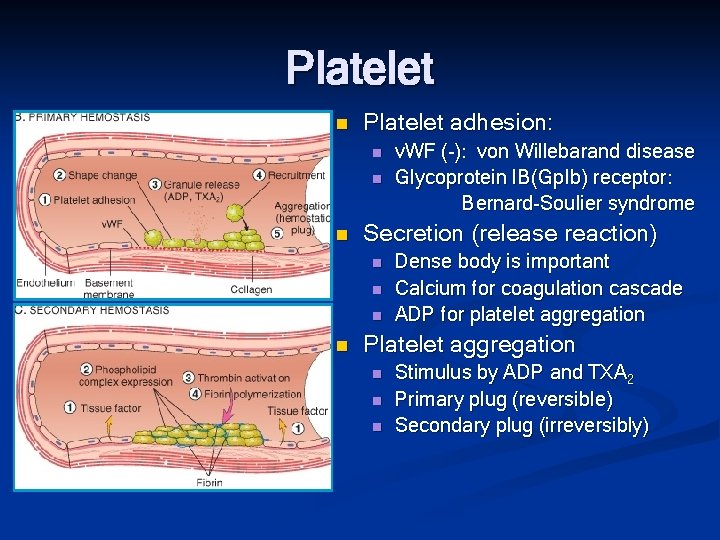
Platelet n Platelet adhesion: n n n Secretion (release reaction) n n v. WF (-): von Willebarand disease Glycoprotein IB(Gp. Ib) receptor: Bernard-Soulier syndrome Dense body is important Calcium for coagulation cascade ADP for platelet aggregation Platelet aggregation n Stimulus by ADP and TXA 2 Primary plug (reversible) Secondary plug (irreversibly)
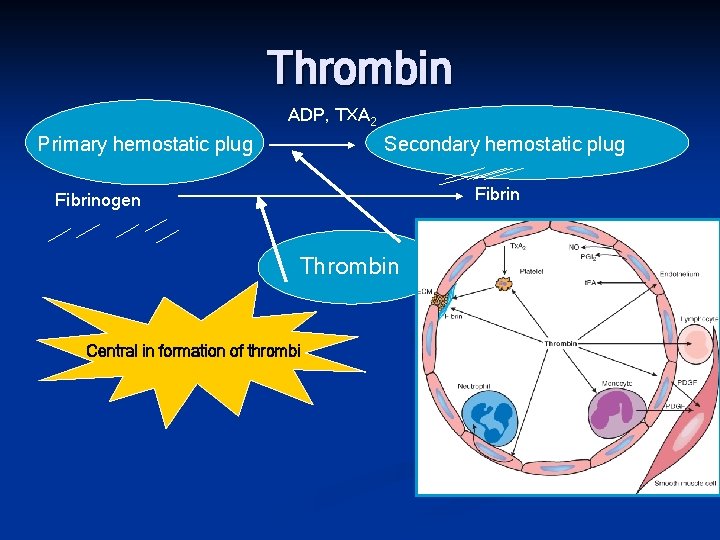
Thrombin ADP, TXA 2 Primary hemostatic plug Secondary hemostatic plug Fibrinogen Thrombin Central in formation of thrombi
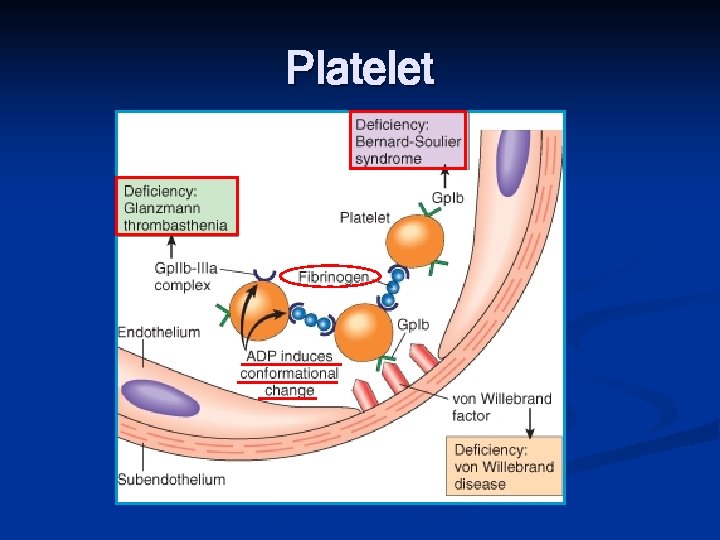
Platelet
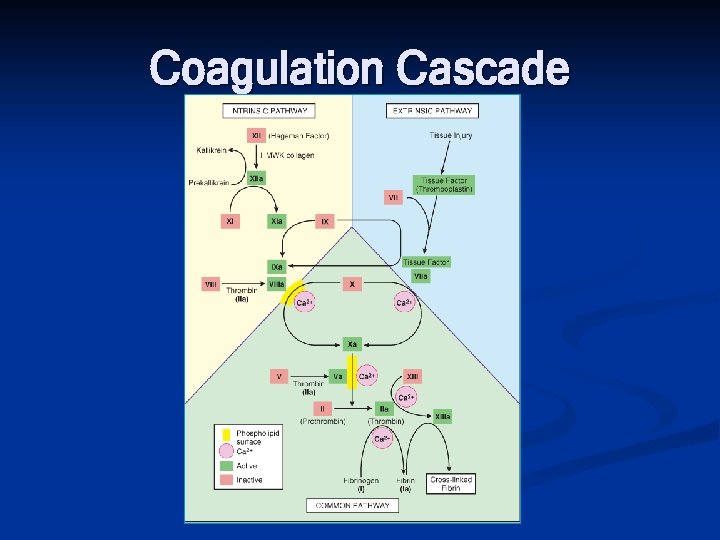
Coagulation Cascade
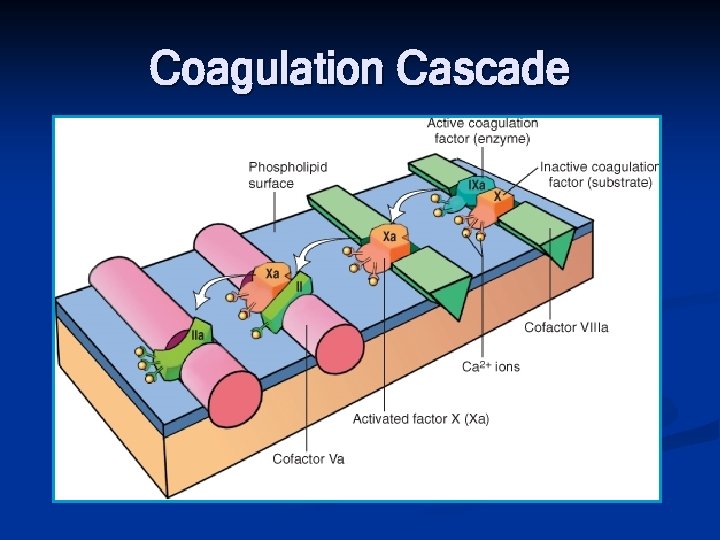
Coagulation Cascade

Coagulation Cascade n Three types of natural anticoagulants n Antithrombins (ATs) n Inhibit the activity of thrombin n Other serine proteases (Factor IXa, XIa, XIIa) n Ex) AT III, actiated by binding to heparin-like molecules n Protein C and S n Vit K-dependent proteins n Inactivate factors Va and VIIIa n Tissue factor pathway inhibitor (TFPI) n Inactivate factor Xa and VIIa
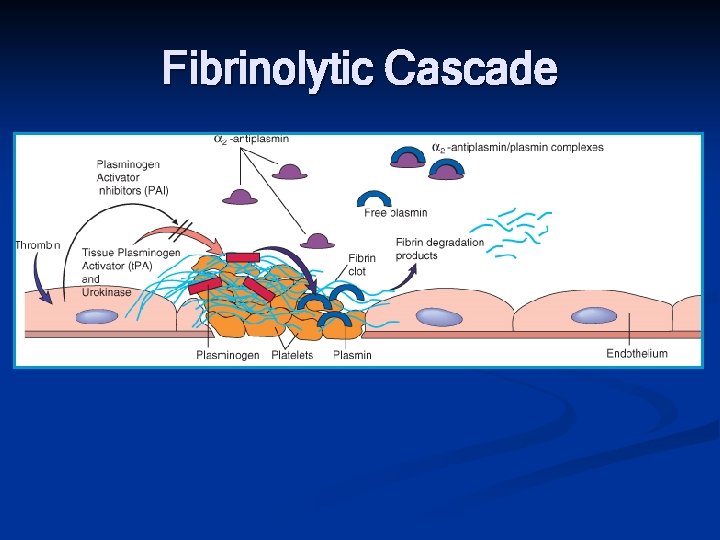
Fibrinolytic Cascade
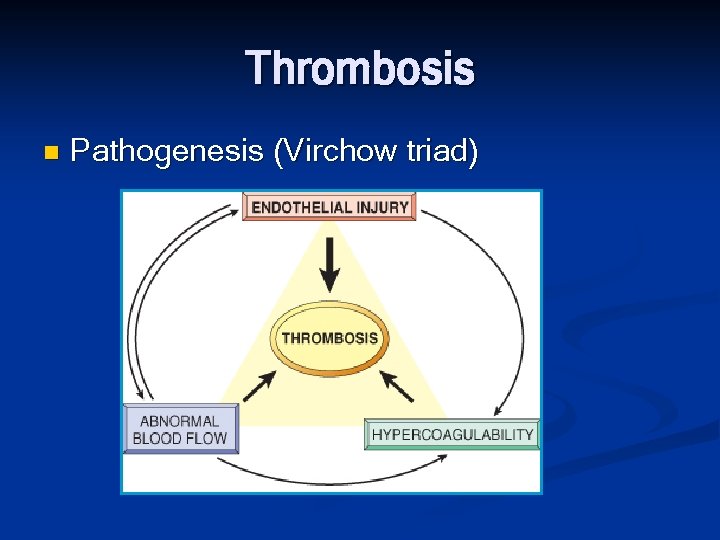
Thrombosis n Pathogenesis (Virchow triad)

Endothelial Injury However, it is important to note that endothelium need not be denuded or physically disrupted to contribute to the development of thrombosis; any perturbation in the dynamic balance of the pro- and antithrombotic effects of endothelium can influence local clotting events Significant endothelial dysfunction may occur due to 1. hemodynamic stresses of hypertension 2. turbulent flow over scarred valves 3. bacterial endotoxins
Alterations in Normal Blood Flow n Stasis and turbulence Disrupt laminar flow n Prevent dilution of activated clotting factors n Retard the inflow of clotting factor n Promote endothelial cell activation Atherosclerosis, Aneurysm, Myocardial infarction, Mitral vlave stenosis, Hyperviscosity syndromes, Sickle cell anemia n n

S t a t e s Hypercoagulability n Less frequently but important Primary (Genetic) Common Mutation in factor V gene (factor V Leiden) Mutation in prothrombin gene Mutation in methyltetrahydrofolate gene Rare Antithrombin III deficiency Protein C deficiency Protein S deficiency Very rare Fibrinolysis defects Inherited causes of hypercoagulability must be considered in patients under the age of 50 who present with thrombosis in the absence of any acquired predisposition

S t a t e s Hypercoagulability n Secondary (acquired) disorders Secondary (Acquired) High risk for thrombosis Prolonged bed rest or immobilization Myocardial infarction Atrial fibrillation Tissue damage (surgery, fracture, burns) Cancer Prosthetic cardiac valves Disseminated intravascular coagulation Heparin-induced thrombocytopenia Antiphospholipid antibody syndrome (lupus anticoagulant syndrome) Lower risk for thrombosis Cardiomyopathy Nephrotic syndrome Hyperestrogenic states (pregnancy) Oral contraceptive use Sickle cell anemia Smoking
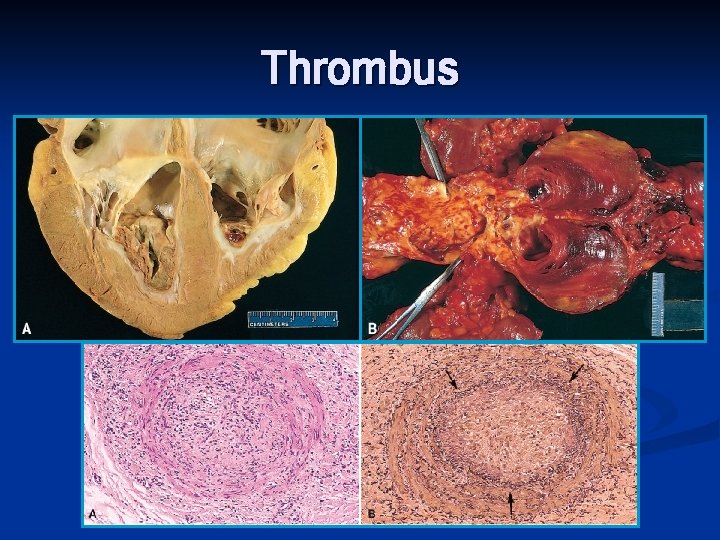
Thrombus





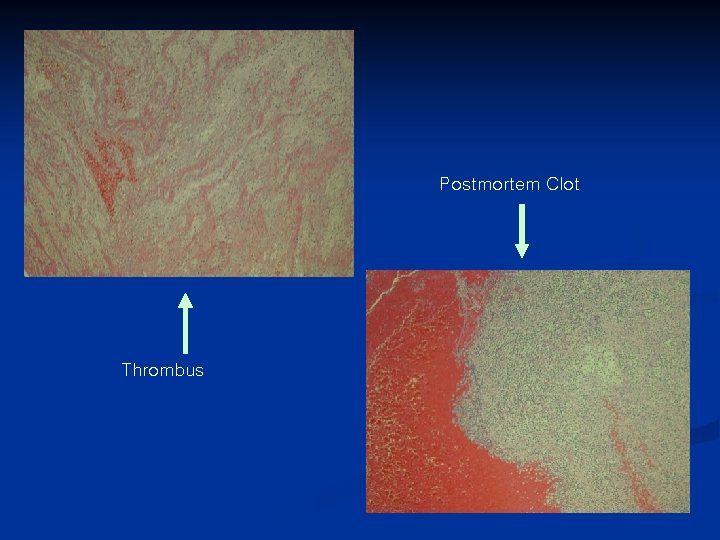
Postmortem Clot Thrombus

Fate of the thrombus 1) Propagation (증식) 2) Embolism (색전) 3) Dissolution (용해) 4) Organization & recanalization (기질화 및 재소통)
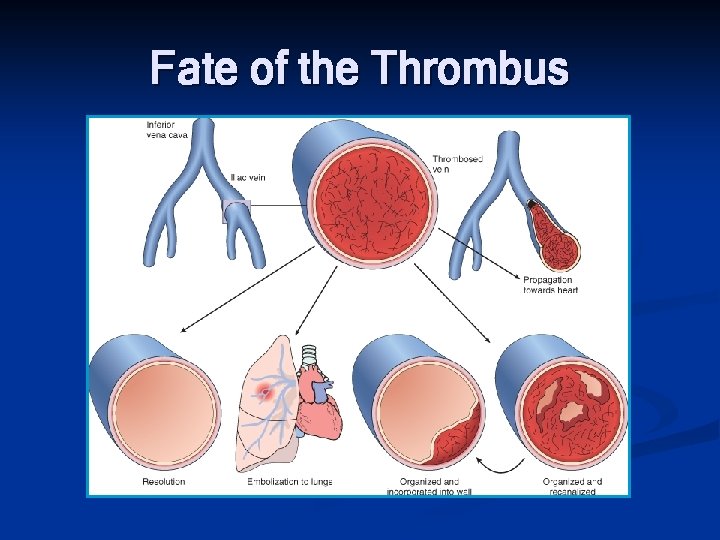
Fate of the Thrombus



Disseminated Intravascular Coagulation(DIC) Sudden or insidious onset of widespread fibrin thrombi in the microcirculation n Consumption of platelets and coagulation proteins n It should be emphasized that DIC is not a primary disease but rather a potential complication of any condition associated with widespread activation of thrombin

Embolism Embolus is a detached intravascular solid, liquid, or gaseous mass that is carried by the blood to a site distant from its point of origin. n Ischemic necrosis of distal tissue, infarction n Whether emboli lodge is important n Pulmonary thromboembolism n Systemic thromboembolism n Fat embolism n Air embolism (Decompression sickness) n Amniotic fluid embolism n






Air Emboli



Infarction n Definition n n An area of ischemic necrosis caused by occlusion of either the arterial supply or the venous drainage in a particular tissue. Etiology Arterial occlusion (99%) n Local vasospasm n Expansion of an atheroma n Extrinsic compression of a vessel (tumor) n
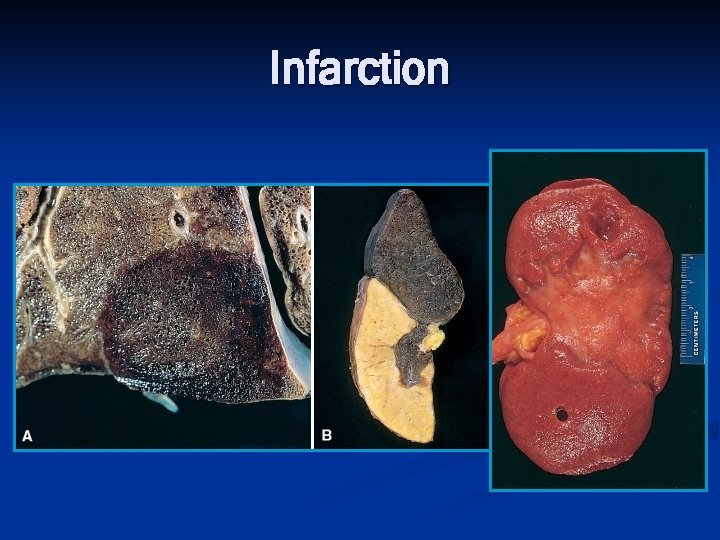
Infarction


Infarction n Major determinants of infarction n The nature of the vascular supply n Dual n supply of lung, liver, hand, forearm The rate of development of the occlusion n Collateral n The vulnerability of a given tissue to hypoxia n Neurons, n circulation myocardial cells The blood oxygen content





Shock n Final common pathway for a number of potentially lethal clinical events Reduction either in cardiac output or in the effective circulating blood volume Systemic hypoperfusion Hypotension Impaired tissue perfusion and cellular hypoxia
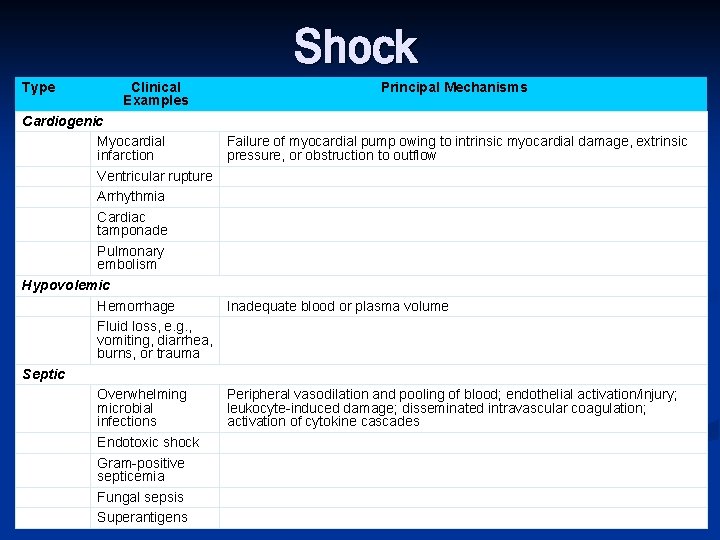
Shock Type Clinical Examples Cardiogenic Myocardial infarction Ventricular rupture Arrhythmia Cardiac tamponade Pulmonary embolism Hypovolemic Hemorrhage Fluid loss, e. g. , vomiting, diarrhea, burns, or trauma Septic Overwhelming microbial infections Endotoxic shock Gram-positive septicemia Fungal sepsis Superantigens Principal Mechanisms Failure of myocardial pump owing to intrinsic myocardial damage, extrinsic pressure, or obstruction to outflow Inadequate blood or plasma volume Peripheral vasodilation and pooling of blood; endothelial activation/injury; leukocyte-induced damage; disseminated intravascular coagulation; activation of cytokine cascades
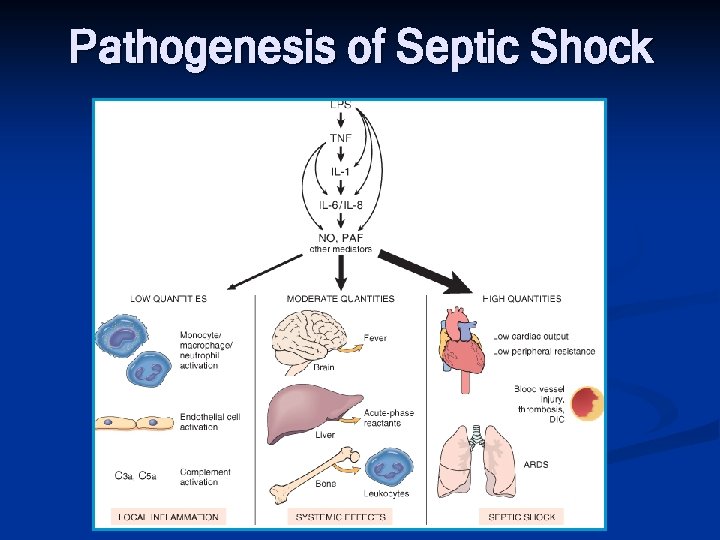
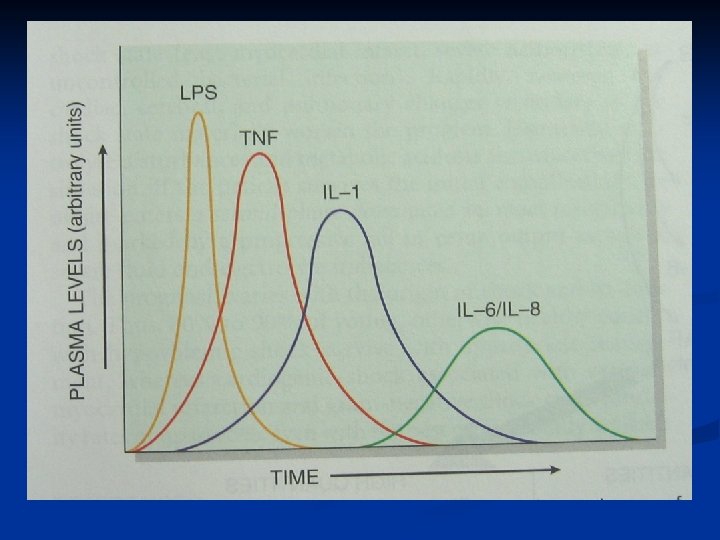
Pathogenesis of Septic Shock

Stages of Shock n Early nonprogressive phase n n Reflex compensatory mechanisms Imperceptibly o the progressive phase Widespread tissue hypoxia n Lactic acidosis (lower p. H), n Blunts the vasomotor response n Vital organs are affected and begin to fail n n Irreversible stage n Widespread cell injury (lysozomal enzyme leakage)


- Slides: 70