HEME CATABOLISM Prof Dr Arzu SEVEN HEME CATABOLISM

HEME CATABOLISM Prof. Dr. Arzu SEVEN

HEME CATABOLISM • In one day, 70 kg human turns over ~= 6 gr of Hb • Hb heme globulin iron_free porphyrin iron (reuse) amino acid (reuse)

• Heme is the source of bile pigments. • Iron free porphrin of heme is degraded in RES (liver, spleen bone_marrow) by microsomal heme oxygenase system. • Humans have at least 3 izoenzyems of heme oxygenase (HO).

• HO-1 highyl regulated, induced by a wide range of stress conditions (shear stress, angiogenesis, hypoxia, heat shock, UV light, H 2 O 2) • HO-2 MAİNLY İN BRAİN γ TESTES • HO-3 NOT WELL CHARACTERİZED • Iron is oxidized to ferric form HEMIN
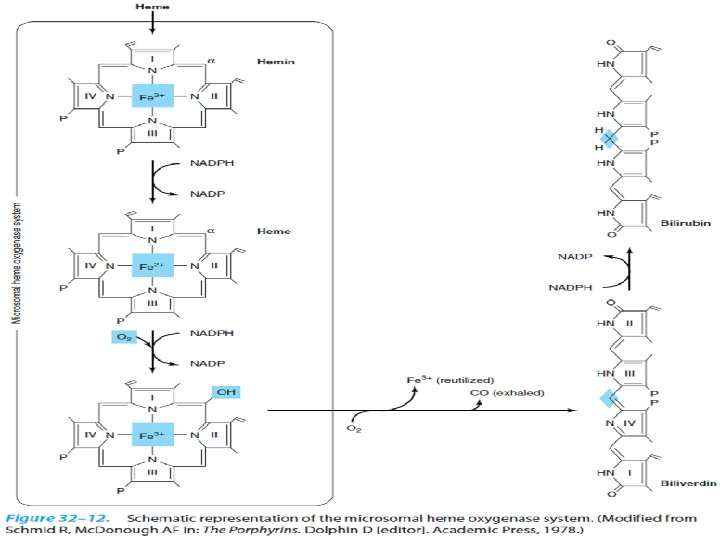

• Hemin is reduced to heme by NADPH. • O 2 is added to α_methenyl bridge between pyroles I and II of the porphyrin. • Ferrous iron is again oxidized to ferric form. • O 2 is added, Fe is released, CO is +3 produced, tetrapyrole ring is split to form biliverdin (green).

• In animals biliverdin reductase reduces the methenly bridge between pyrole III and IV to a methylene group to produce bilirubin. (yellow pigment) • 1 gr Hb 35 mg biliburin • Daily bilirubin formation in human adults = 250 -350 mg (from Hb +ineffective erytropoiesis+cyt P 450)

• The CO produced by heme oxygenase is toxic at high concentrations, however at very low concentrations generated during heme degradation, it has regulatory and/or signalling functions, it acts as a vasodilatator, less potent than NO. • Low levels of CO have regulatory effects on neurotransmission.

• Bilirubin is the most abundant antioxidant in mammalian tissues and is responsible for the most of the antioxidant activity in serum. • İts protective effects are important in the developing brain of newborn infants

• Bilirubin formed in peripheral tissues is transported to liver by albumin • IN LIVER: 1)Uptake of bilirubin by liver paranchmal cells 2)conjugation of bilirubin with glucuronate in endoplasmic reticulum 3)secretion of conjugated bilirubin into bile
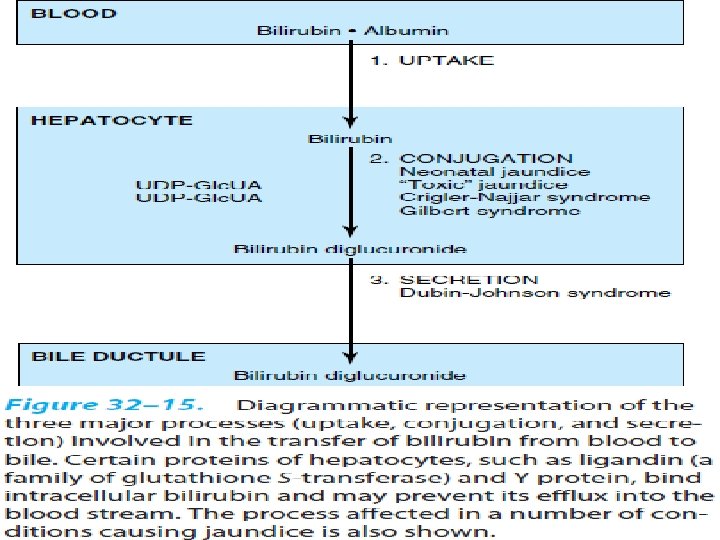

• Uptake of bilirubin by liver • Bilirubin is only sparingly soluble in water • İts solubility in plasma is increased by noncovalent binding to albumin • Albumin has one high affinity site and one low affinity site for bilirubin • In 100 ml plasma = 25 mg bilirubin can be tightly bound to albumin at high affinity site

• Antibiotics and other drugs compete with bilirubin to bind to high_affinity site of albumin. • In liver, bilirubin is removed from albumin and taken up at the sinusoidal surface of hepatocytes by a facilated transport system. • In the hepatocytes bilirubin binds to cytosolic proteins : ligandin (a family of glutathione s-transferases) and protein γ_to be kept solubilized prior to conjugation.

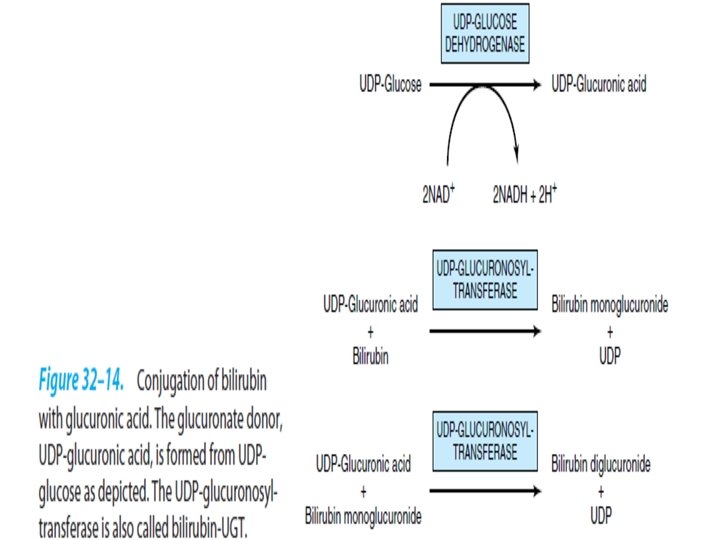
Conjugation of bilirubin with glucuronic acid • Bilirubin is non_polar. • Hepatocytes convert bilirubin to a polar form by adding glucuronic acid to it (conjugation) • Enzyme: glucuronosyl transferase • Location: endoplasmic reticulum • Glucuronosyl donor: UDP_GLUCURONİC ACİD

• Bilirubin monoglucuronide is an intermediate, subsequently converted to diglucuronide. • Phenobarbital induces UDP_glucuronosyl_transferase activity

Secretion of conjugated bilirubin into bile • Active transport mechanism • Rate-limiting for the entire hepatic bilirubin metabolism • MRP_2 (multidrug resistance like protein 2) = MOAT(multi specific organic anion transporter) Location: plasma membrane of the bile canalicular membrane

• A member of the family of ATP_binding cassette (ABC) transporters • Inducible by phenobarbital • Conjugation γ excretion systems behave as a coordinated functional unit. • Conjugated bilirubin reaches the terminal ileum and large intestine. • The glucuronides are removed by β_glucuronidases (specific bacterial enzymes)

• The pigment is reduced by intestinal bacteria (fecal flora) to urobilinogen (colorless tetrapyrolic compound) • A small portion of urobilinogen is reabsorbed and reexcreted through the liver: ENTEROHEPATİC UROBİLİNOGEN CYCLE

• Some urobilinogen is reabsorbed into the blood and transported to the kidney, where it is oxidized to urobilin(the compound that gives urine its yellow color). • Urobilinogen remaining in the intestine is converted to stercobilin, which gives the red_brown color to feces.
- Slides: 20