Hematopoiesis Blood cell formation Occurs in red bone
Hematopoiesis • Blood cell formation • Occurs in red bone marrow

Hematopoiesis • Hemocytoblast differentiation: • Lymphoid stem • Myeloid stem c
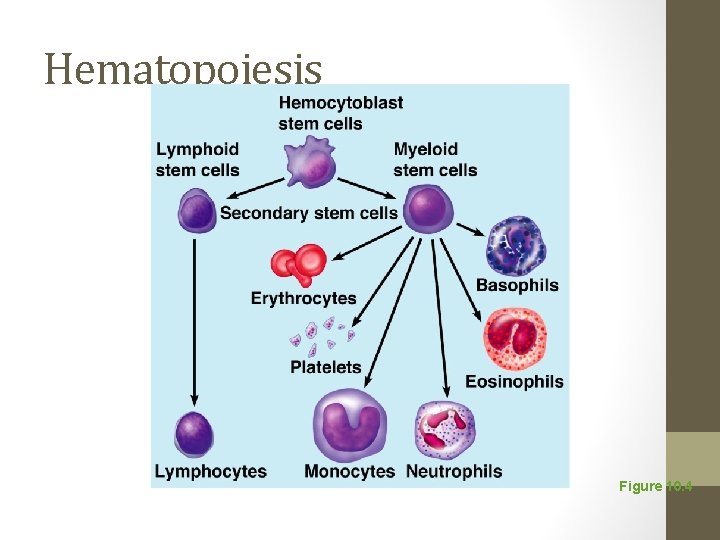
Hematopoiesis Figure 10. 4

Formation of Erythrocytes • Unable to divide, grow, or synthesize proteins • Wear out in 100 to 120 days • When worn out, RBCs are eliminated by phagocytes in the spleen or liver • Lost cells are replaced by division of hemocytoblasts in the red bone marrow

Control of Erythrocyte Production • Erythropoietin • Kidneys produce most erythropoietin as a response to reduced oxygen levels in the blood
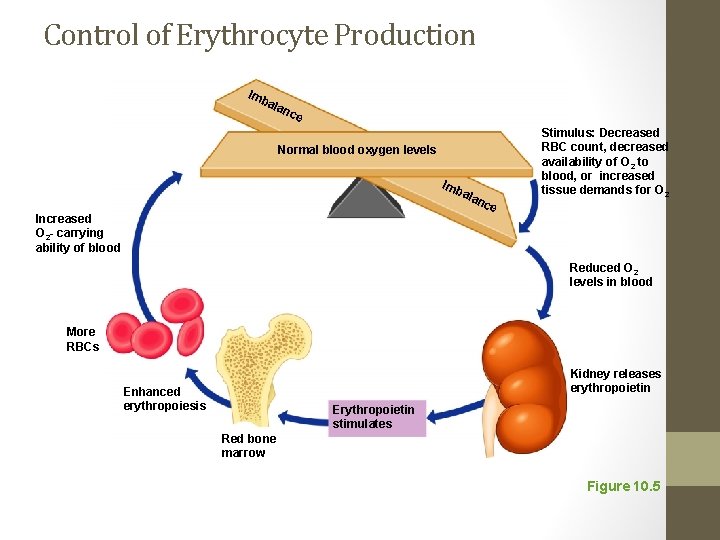
Control of Erythrocyte Production Imb ala nce Normal blood oxygen levels Imb ala Increased O 2 - carrying ability of blood nce Stimulus: Decreased RBC count, decreased availability of O 2 to blood, or increased tissue demands for O 2 Reduced O 2 levels in blood More RBCs Kidney releases erythropoietin Enhanced erythropoiesis Erythropoietin stimulates Red bone marrow Figure 10. 5
Formation of White Blood Cells and Platelets • Controlled by hormones • Colony stimulating factors (CSFs) and interleukins prompt bone marrow to generate leukocytes • Thrombopoietin

Hemostasis • Stoppage of bleeding resulting from a break in a blood vessel • Hemostasis involves three phases • Vascular spasms • Platelet plug formation • Coagulation (blood clotting)
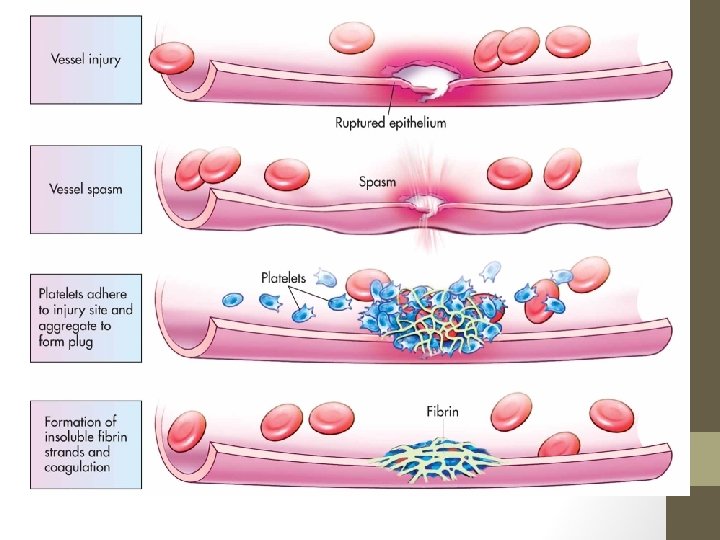

Hemostasis • Vascular spasms • Vasoconstriction – spasms

Hemostasis • Platelet plug formation • Collagen fibers are exposed • Platelets become “sticky” and cling to fibers
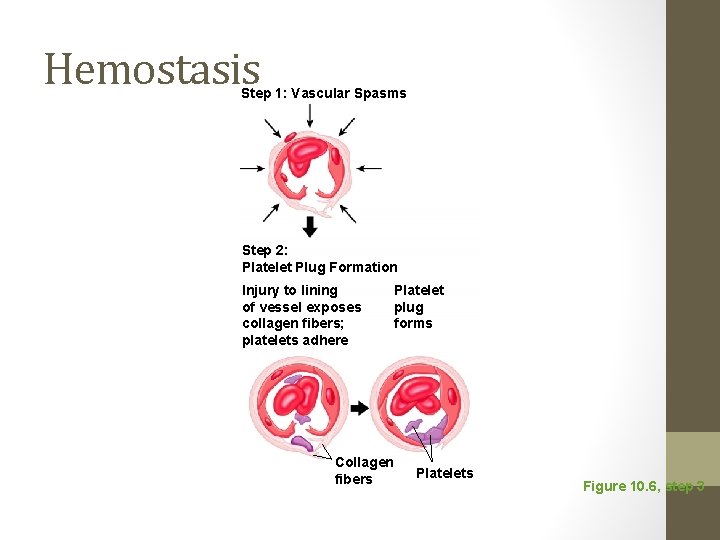
Hemostasis Step 1: Vascular Spasms Step 2: Platelet Plug Formation Injury to lining of vessel exposes collagen fibers; platelets adhere Collagen fibers Platelet plug forms Platelets Figure 10. 6, step 3
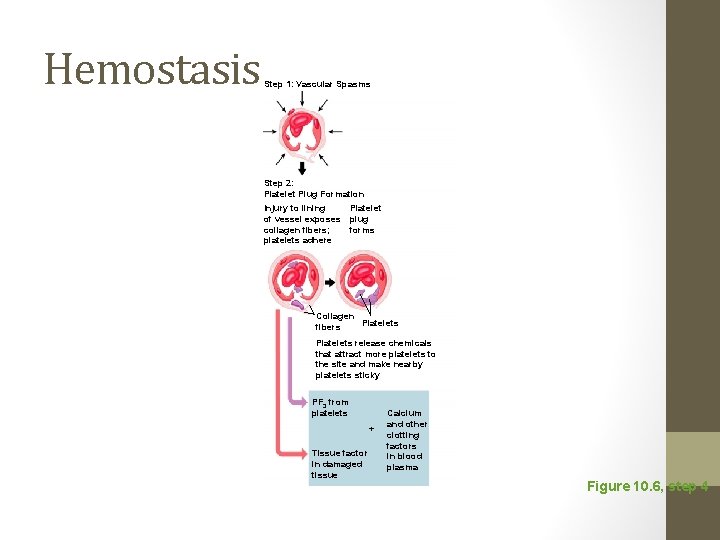
Hemostasis Step 1: Vascular Spasms Step 2: Platelet Plug Formation Injury to lining Platelet of vessel exposes plug collagen fibers; forms platelets adhere Collagen Platelets fibers Platelets release chemicals that attract more platelets to the site and make nearby platelets sticky PF 3 from platelets + Tissue factor in damaged tissue Calcium and other clotting factors in blood plasma Figure 10. 6, step 4
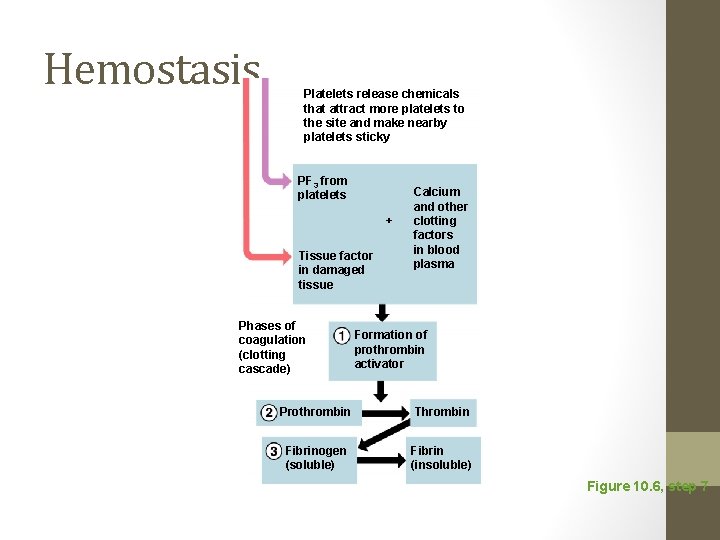
Hemostasis Platelets release chemicals that attract more platelets to the site and make nearby platelets sticky PF 3 from platelets + Tissue factor in damaged tissue Phases of coagulation (clotting cascade) Calcium and other clotting factors in blood plasma Formation of prothrombin activator Prothrombin Thrombin Fibrinogen (soluble) Fibrin (insoluble) Figure 10. 6, step 7

Hemostasis • Coagulation • Injured tissues release tissue factor (TF) • PF 3 (a phospholipid) interacts with TF • Prothrombin activator converts prothrombin to thrombin (an enzyme)

Hemostasis • Coagulation (continued)
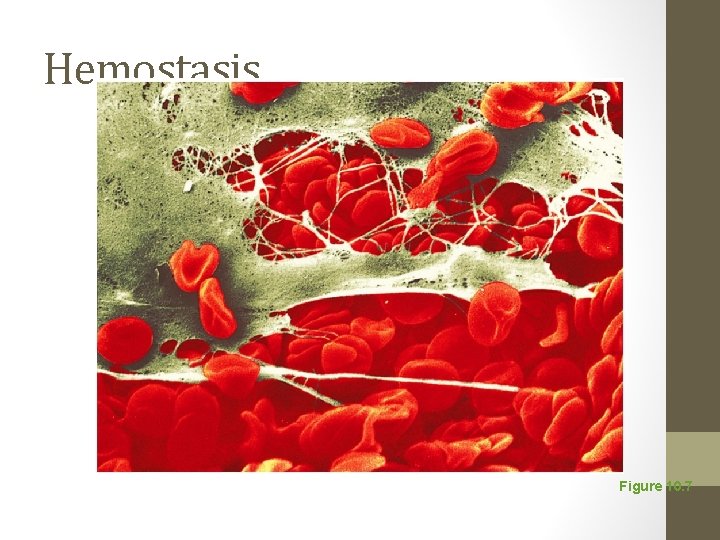
Hemostasis Figure 10. 7

Hemostasis • Blood usually clots within 3 to 6 minutes • The clot remains as endothelium regenerates • The clot is broken down after tissue repair
- Slides: 18