Hematopoiesis and development of B and T lymphocytes

Hematopoiesis and development of B and T lymphocytes
• The B cells develop from Haemotopoitic Stem cells of Bone marrow. • Some of the stem cells are Pro-B cells ( Progenitor B-cells). • Pro B cells enter the bursa of fabricius and develop into B Lymbhoblast (Immature lymphocyte) • In mammals this occur in the bone marrow it self • The immature B lymphoblast change into Immature B cell which has Ig M molecule on the surface • The immature B cell change into mature B Cell which has Ig D and Ig M molecules on the surface. • The immature B Lymphocyte move into Lymph node and Spleen from Bone marrow / bursa of fabricius • Here the B lymphocyte is put into action when exposed to Ag
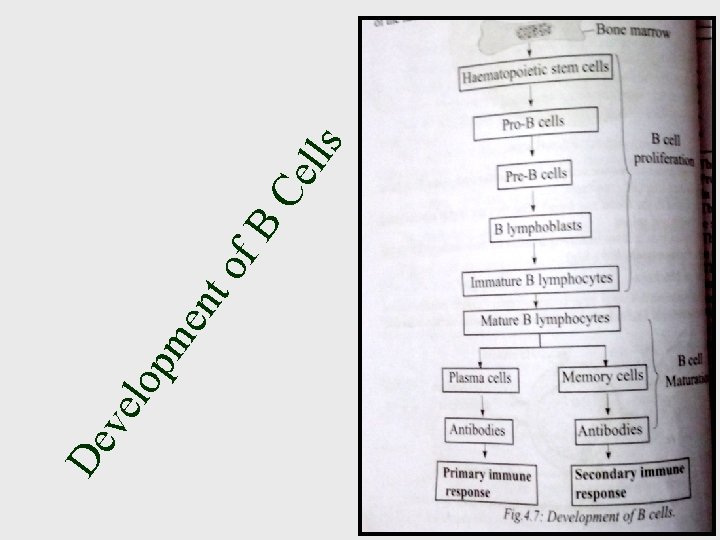
ve De nt me lop of B s Ce ll
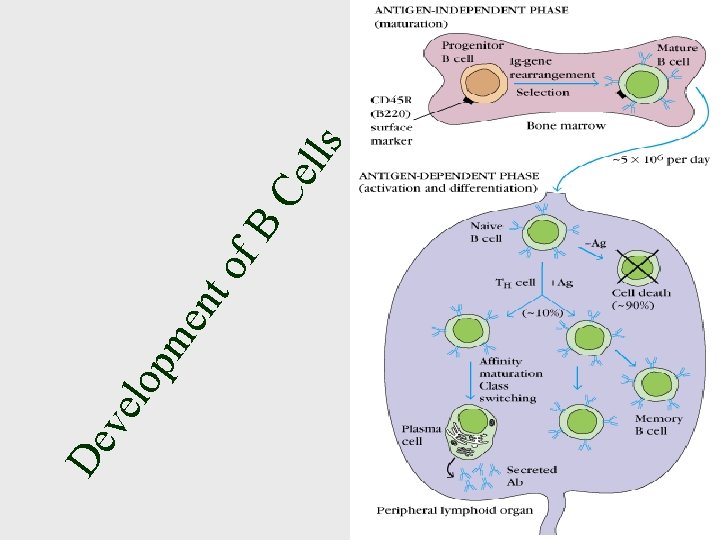
ve De nt me lop of B s Ce ll
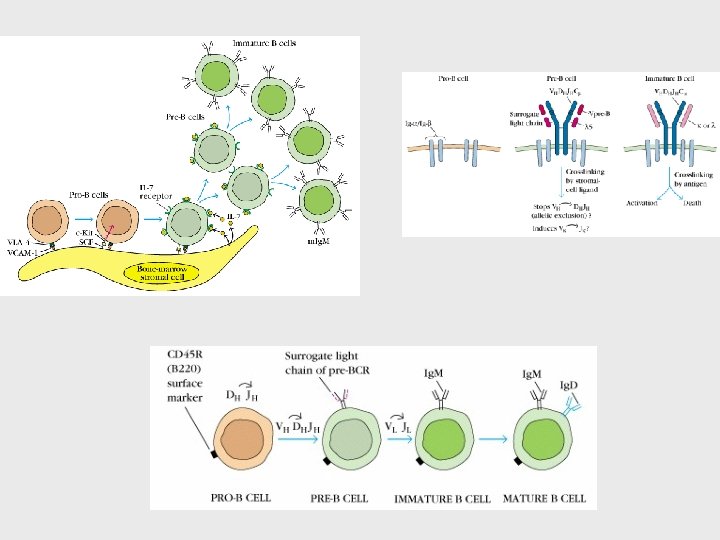

B and T cell Activation

Mechanism of B Cell maturation • 3 Important process • Clonal Selection • Affinity maturation • Class switching

Clonal Selection • The selection of single lymphocyte (B or T) out of the thousands of lymphocyte by an Ag • And its proliferation into a population of similar cells to fight against that Ag

Mechanism of clonal selection • 1000 of lymphocyte circulate in the Blood and Lymph • Each lymphocyte has a single type of receptor eith Unique specificity • When a Ag binds to the receptor--- the lymphocyte is activate. • The activation cells undergoes proliferation, producing a population of similar cells, a clone. • This clones of cells bear Identical Receptors similar to parental cells • When a Bcells is selected , its proliferate in to many Plasma cells and Few Memory cells • Plasma cells produce enormous amount of Ab
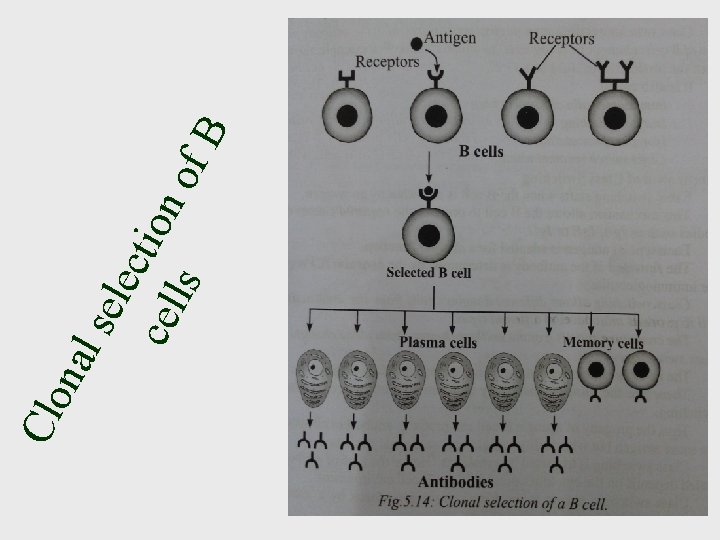
sel ect cel ion ls of B nal Clo

Affinity maturation • Affinity maturation is the process of producing Ab by B cells with Increased affinity for Ag.

Class switching • This is the immunological process by which the Ab production of B cells from one class to another class • Eg. Change from the production of Ig M to Ig. G. • Its also called • Immunoglobulin class switching • Isotype switching • Class switch recombination

Mechanism of Class switching • Class switching starts when the Bcell is activate by the Ag • This mechanism allow the B cells produce the require class of Ab (Ig A, Ig E or Ig. G) • Each type of Ag is adapted for a distinct function • Function of the AB determined by Constant Region of Immunoglobulin • Constant region of the Ab heavy chain alone changes duration of class switching. • Variable region remain Unchanged • Therefore the Ag specificity also remain Unchanged • New class of Ab include Ig. G, Ig. A and Ig. E with respective heavy chain • In this process VDJ gene segment recombine with C region

• Class switching triggered by Cytokines • Hence the type of Ab generated depends up on the cytokines present in the B cell environment • Class switching occur in the heavy chain LOCUS by a mechanisms called Class switching recombinant (CSR) • The CSR mechanism relies on the conserved nucleotide motifs called SWITCH (s) Regions found in the DNA upstream of each constant region. • The DNA Strand is broken by the activity of serious of ENZYME at TWO selected S region • The variable domain exon is rejoined through a process called NON HOMOLOCUS END JOINING (NHEJ) to the desired Constant region • This process result in an immunoglobulin gene that encodes AB of different type.

Mechanism of B-cell Activation • • • Recognition of Ag Colonal selection T cell dependent Activation T cell Independent activation Proliferation Affinity maturation (Fine tuning of the shape of Ab) Class switching Production of Plasma and Memory cells Secretion of immunoglobulins

B cell activation • The process of stimulating the B cells to produce Ab and Humoral immune response called B cell activation. • B cells are bursal or Bone marrow derived Lymphocyte. • They attack extracellular Ag (Bacteria, virus) by secreting Ab. • B cells are activated by Infection or Vaccine • Bcells activated in two ways • Thymus independent activation (Polysaccharides or Lipopolysaccharides canactivate the B cells directly) • Thymus dependent activation (Need a of TH cells

Development of T Lymphocyte • The lymphocyte matures in Thymus and that brings about Cell mediated immunity • The T Lymphocytes are Thymus dependent cells. They mature under influence of thymic hormones. • T Lymphocytes have large Nucleus • They highly concentrate in the Blood and Spleen. • T Lymphocytes contains certain unique proteins called T cell surface markers. (Erythrocyte receptor, T cell Receptor (TCR), Ia Protein receptor, Interlukein receptor
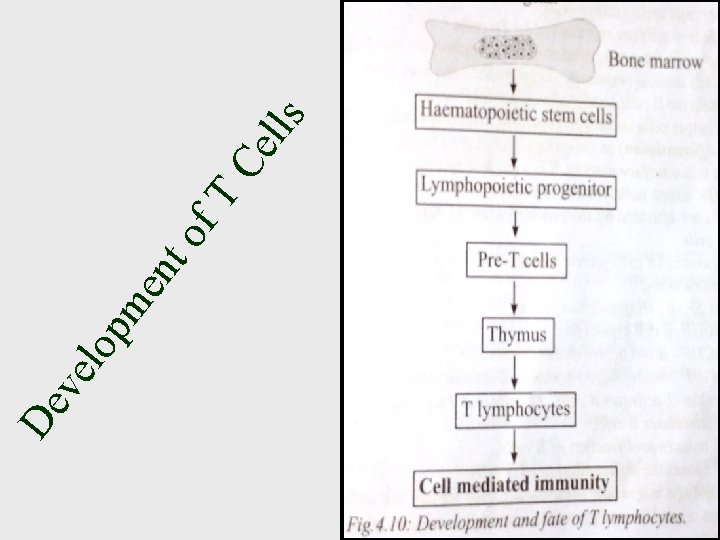
De pm e ve lo f. T nt o Ce lls

Activation of T cells • The process of making T cells into functional T cells is called T cell activation • T cells are thymus dependent lymphocytes • They bring about cell mediated immunity • Pathogens are the Ag to Activate the T cells • The Ag has identify by APC such Macrophages, dentric cells • APC sallow the Ag , degrades it into peptide fragment • A piece of peptide fragment of Ag loaded on the MHC to form Peptide – MHC complex. This complex deposited on the surface of APC this called Antigen presentation

• This complex indicates that the pathogen is inside APC • Now the APC tells to the Th cells (I found dangerous enemy , , , ) • The warning received by a T helper cells and a cytotoxic T cells • Th cells receiving the signal, proliferates into a clone of Th cells and Tc cells. • Th clones produce two type of cells , 1. Effectors Th cells 2. Memory Th cells • Effector Th cells activate Macrophages and B cells • Macrophages march towards Ag (pathogens), surround it and kill the pathogens by phgocytosis

Mechanisms of T cell activation 1. Reorganization of Ag (recognize Ag deposited on the surface of APC - recognized only processed Ag) 2. Processing of Ag (“ “ “ they neutralize the Ag into the cytoplasm, the Ag processed and degraded in to peptide fragment) 3. Presentation of Ag § A piece of peptide fragment of Ag loaded on the MHC to form Peptide – MHC complex I or II. This complex deposited on the surface of APC this called Antigen presentation 4. Binding of T cells with Ag (T cell recognize the Ag deposited on the MHC molecules of APCs. § The MHC molecules function as markers which inform the T cells that Culprit Ag. § Th cell recognize Ag deposited on MHC II, TC cell recognize Ag deposited on MHC I § This binding provides first signal for T cell activation

6. Co-stimulation of T cells § The T cell has another surface molecule called CD 28. It binds with a surface molecule called B 7 present on the surface of APC 7. Secretion of cytokine § The APC secretes a cytokine called IL-1. § It binds to the IL 1 receptor Present on the T cell, § It stimulates the T cell to go on its differentiation 8. Colonal proliferation § The activated T cell is called sensitized T Cells § The sensitized T cell undergoes proliferation (clone of T cell produced) 9. Triggering of activation § Tc cell activation is caused by two Factors, namely § Binding of Tc Cell with Peptide class I MHC complex of APC § Binding of CD 28 of T cell and B 7 of APC

10. Tc cell activation § The activated Tc cell binds with the target cell (Ag) to form a conjugate § The binding occur between the Tc cell receptor and Ag-class I MHC complex of target cells. • Destruction of Ag by Tc cells • Activation of Th cells • Changes in activated Th cells
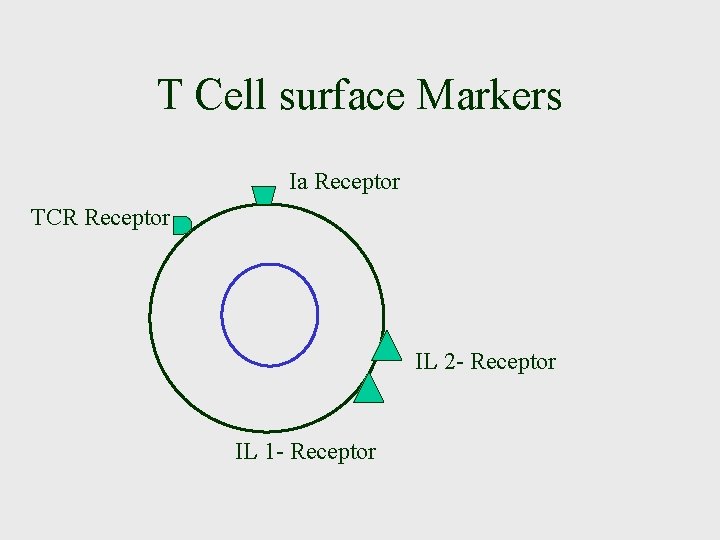
T Cell surface Markers Ia Receptor TCR Receptor IL 2 - Receptor IL 1 - Receptor

on ati tiv Ac of T ce ll

B-CELLS… • • Origin… Development… Selection. S Activation. S • Progenitor B cells (pro-B-cells) bearing a CD 45 R marker develop – in the bone marrow – into immature and then mature B cells. • Then, they migrate to peripheral lymph nodes. • Those developmental events are physically and physiologically distinct; the former are antigen independent; the latter are antigen dependent.

NEGATIVE selection: • crosslinkage of m. Ig. M on immature B cells can cause cells to die within the bone marrow • aka: CLONAL DELETION

Nota bene: • Prior to clonal deletion, development is antigen independent. • Negative selection and positive selection are antigen dependent. • Recognition of the ANTIGEN in the periphery leads to positive selection… • aka CLONAL EXPANSION

SELECTION does not equal ACTIVATION… Recall that a B-CELL needs a signal from a T-HELPER CELL

SELECTION does not equal ACTIVATION… Recall that a B-CELL needs a signal from a T-HELPER CELL
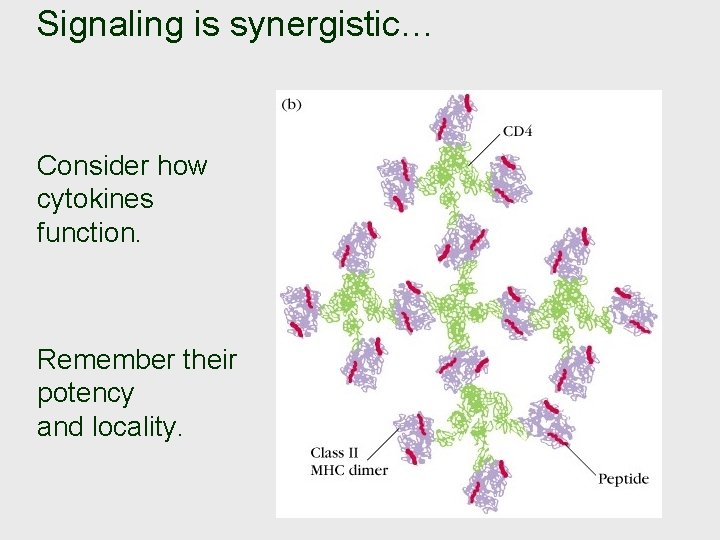
Signaling is synergistic… Consider how cytokines function. Remember their potency and locality.
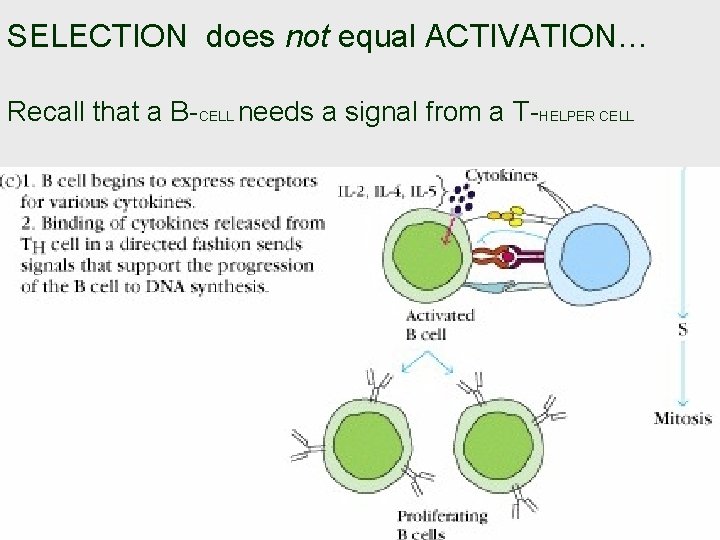
SELECTION does not equal ACTIVATION… Recall that a B-CELL needs a signal from a T-HELPER CELL

Activation…. • Activation occurs when a B-cell associates with a T-helper cell through a ternary complex; this association establishes specificity (the B-cell will have processed the antigen and presented it through MHC-II, thus selecting a specific T-helper cell lineage). • Pairing between B 7 on the B-cell and CD 28 on the T-helper cell constitutes a co-stimulatory signal which will activate the Thelper cell. (The identities of the co-stimulatory proteins are “specific”; but these same proteins are involved regardless of the identity of the antigen). • The T-helper cell , once activated, synthesizes CD 40 L. Now, pairing occurs between CD 40 on the B-cell and CD 40 L on the T -helper cell. This association constitutes a co-stimulatory signal which activates the B-cell. • Thus, there is “mutuality” between the B-cell activating the Thelper cell and the activated T-helper cell, in turn, activating the B-cell. • (This “mutuality” should not obscure that the process is “antigen-driven. ”)
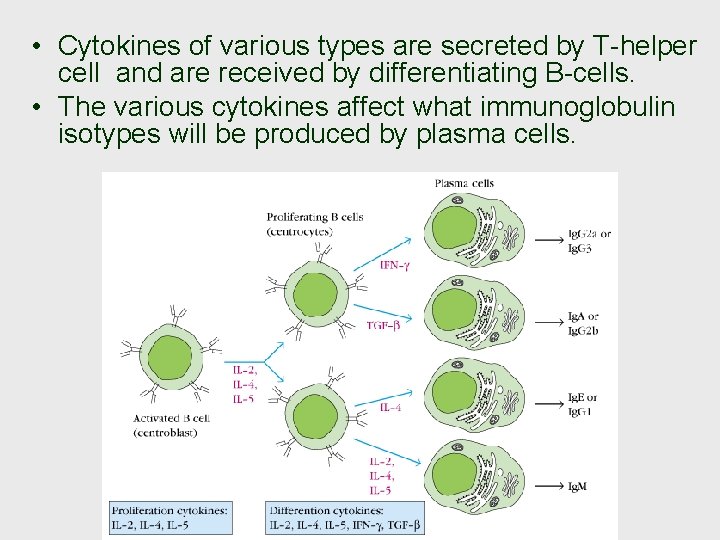
• Cytokines of various types are secreted by T-helper cell and are received by differentiating B-cells. • The various cytokines affect what immunoglobulin isotypes will be produced by plasma cells.

Where is activation happening? And what is happening? The primary response is initiated in the paracortex. T-cells respond to processed antigen that is typically delivered from a site of origin by dendritic cells. B-cells see the same antigen in an unprocessed form in the lymph. The T-cells and B-cells, now both activated, form associations which allow proper signaling. The B-cells migrate to the periphery of the paracortex and form foci where they mature into plasma cells which secrete, first, Ig. M and then Ig. G. Some B-cells – along with some Thelper cell’s – migrate to primary follicles in the cortex.
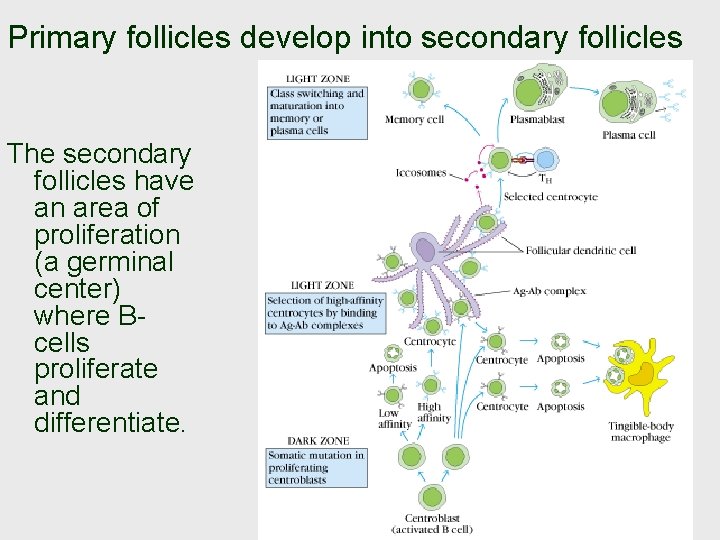
Primary follicles develop into secondary follicles The secondary follicles have an area of proliferation (a germinal center) where Bcells proliferate and differentiate.

Follicular dendritic cells… not an APC! The follicular dendritic cells do not originate in the bone marrow and do not have MHC-II. Rather, the follicular dendritic cell contains Fc receptors, receptors which can capture immunoglobulins through their constant region. Thus, the follicular dendritic cells become decorated with Ab complexed to whole (unprocessed) antigen. Stated another way, these follicles have a rich supply of the filtered antigen The dendrites are fragile and can break in to (non-nucleated) beads (about 0. 3 -0. 4 µm in diameter); these beads are called “iccosomes” (immune-complex coated bodies); they can persist for several months.
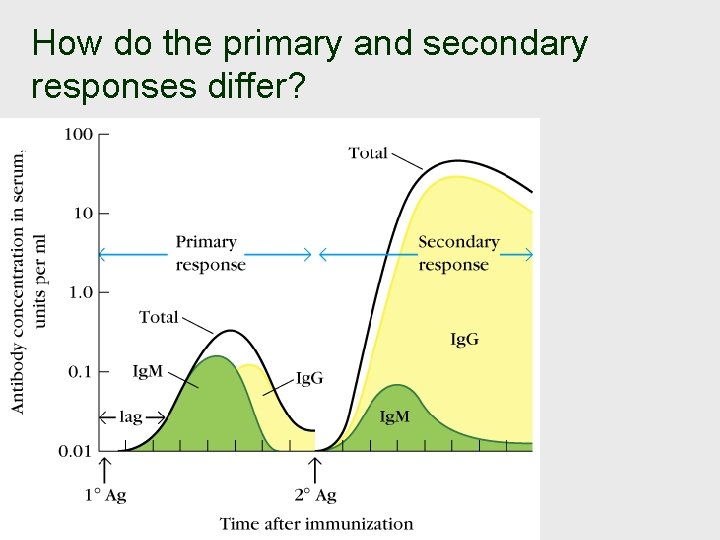
How do the primary and secondary responses differ?
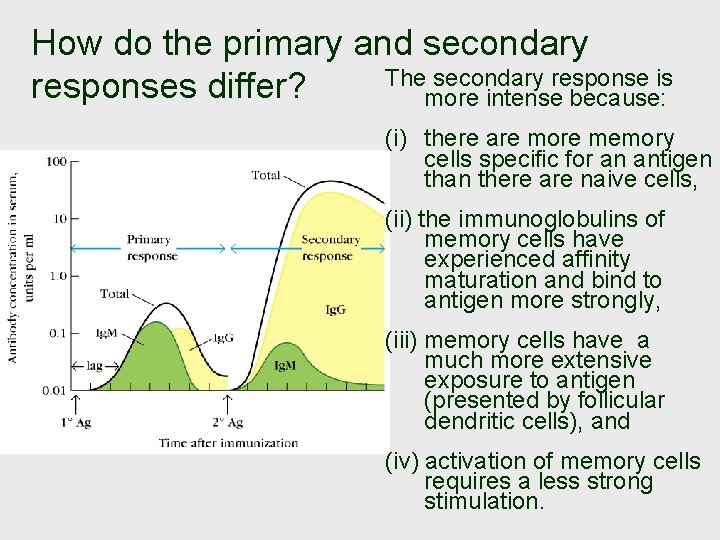
How do the primary and secondary The secondary response is responses differ? more intense because: (i) there are more memory cells specific for an antigen than there are naive cells, (ii) the immunoglobulins of memory cells have experienced affinity maturation and bind to antigen more strongly, (iii) memory cells have a much more extensive exposure to antigen (presented by follicular dendritic cells), and (iv) activation of memory cells requires a less strong stimulation.
- Slides: 39