HEMATOLOGY Bone marrow function Hematopoiesis n Antibody producing
HEMATOLOGY
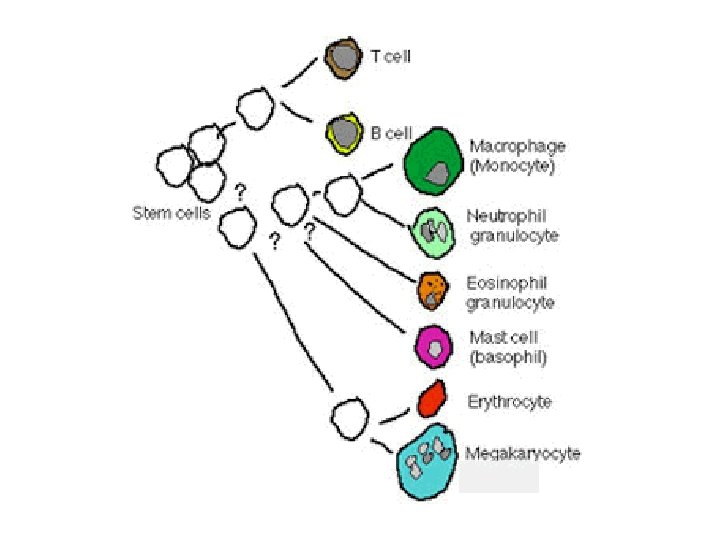
Bone marrow function Hematopoiesis n Antibody producing plasma cell differentiation n Monitoring hematopoietic cell quality n Important key nutrients: iron n folic acid vitamin B 12 regulatory hormones (EPO, CSF-s) interleukins
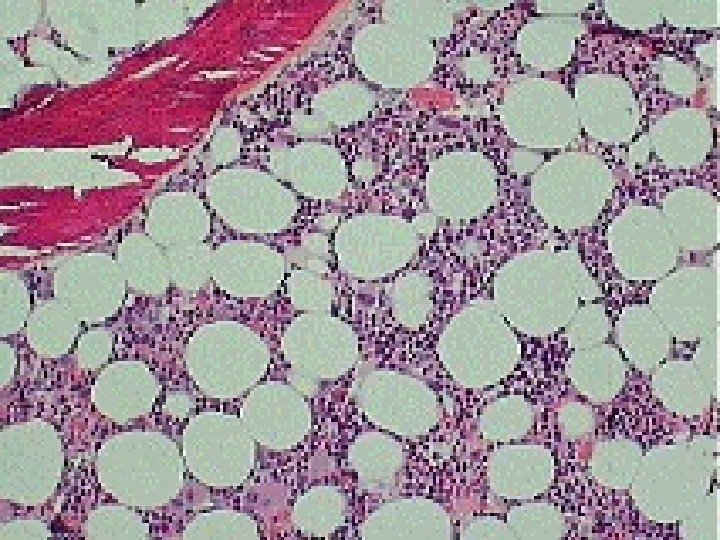
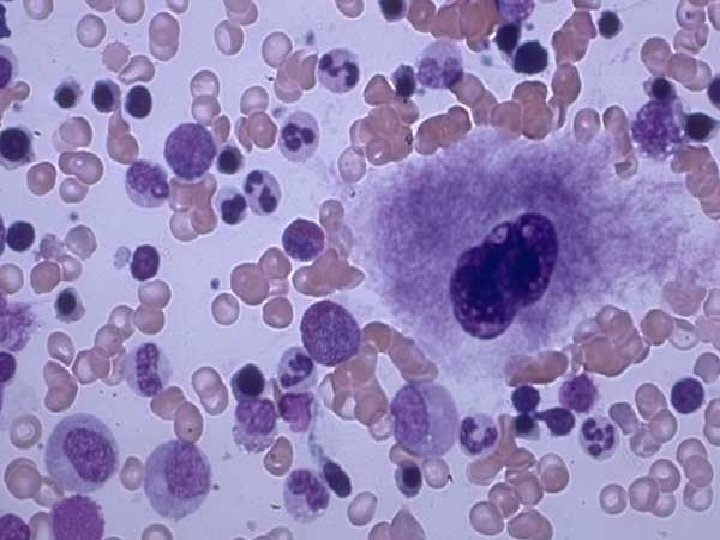

Signs and symptoms of hematological diseases n Factors – – – n Red blood cells Leukocytes Coagulation system Alterations – – Change of the amount Change in the function

Anemia n Decrease in red cell mass or hemoglobin content of blood below the physiologic need n Not n a disease itself! A clinical sign! Analysis of anaemia – Background mechanisms n loss of red blood cell - bleeding n lack of red blood cell production n excessive red blood cell damage

History n n n n Family history: anemia, splenomegaly, jaundice splenectomy Bleeding tendency in the family Diet, alcohol intake Pregnancy, menorrhagia Drugs Chronic diseases Malnutrition, malabsorption Transfusion, iron or otherapy against anemia

Anemia n Signs and symptoms vary with the rapidity of onset: n Rapid (bleeding or brisk hemolysis) cardiovascular compensatory reactions: tachycardia, postural hypotension, vasoconstriction in the skin and extremities, dyspnea on exertion, faintness, even shock n Slowly developing anemias (ie. nutritional deficiency, chr. bleeding, hemolysis etc. ) – there is time for compensation – the patient remains asymptomatic for a long time –

Anemia Mild: often asymptomatic n Moderate: symptoms on exertion n Severe: symptoms on rest heart failure n

Anemia – non cause-specific symptoms – – – – fatigue dizziness, vertigo, headache, tinnitus increased irritability, difficult concentration sleeping disturbancies cold intolerance exertional intolerance: Hb<75 g/l : resting heart rate, stroke volume dyspnea complaints of local vascular diseases (angina pectoris, cerebral ischaemia, intermittent claudication)

Anemia - physical findings Non cause-specific n Pallor of skin and mucous membranes – – causes: Hb and blood redistribution from the skin colors n greyish: malignancy n lemon-like: hemolysis, B 12 deficiency Tachycardia n Hyperkinetic precordium n Systolic murmur (reversible) n

Anemia - physical findings Cause-related n Jaundice hemolysis n Hepatosplenomegaly - e. g. hemolysis n Lymphadenopathy - lymphomas, autoimmune diseases n Cheilosis (fissura) iron deficiency n Koilonychia (spoon-shaped nails) iron def. n Beefy red smooth tongue (Hunterglossitis) - pernicious anemia n Neuropathy - pernicious anemia n Rectal digital examination - bleeding
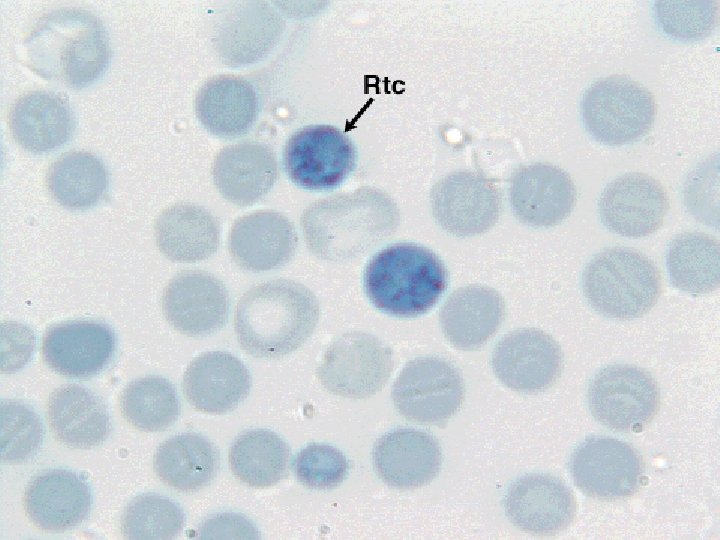
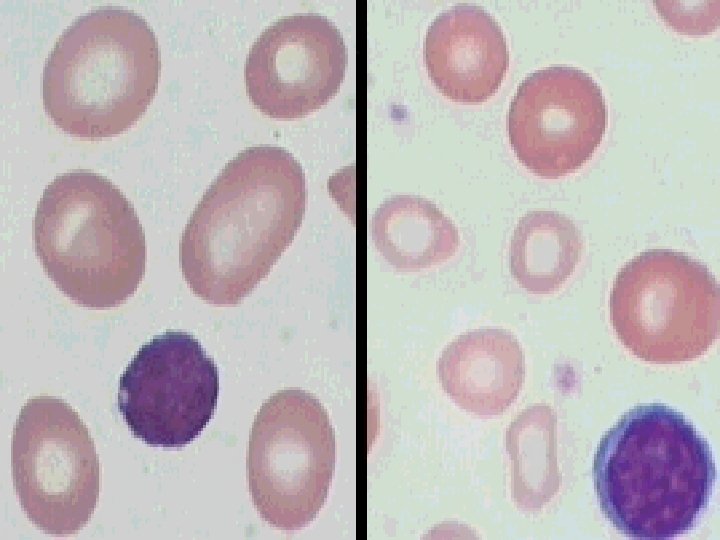
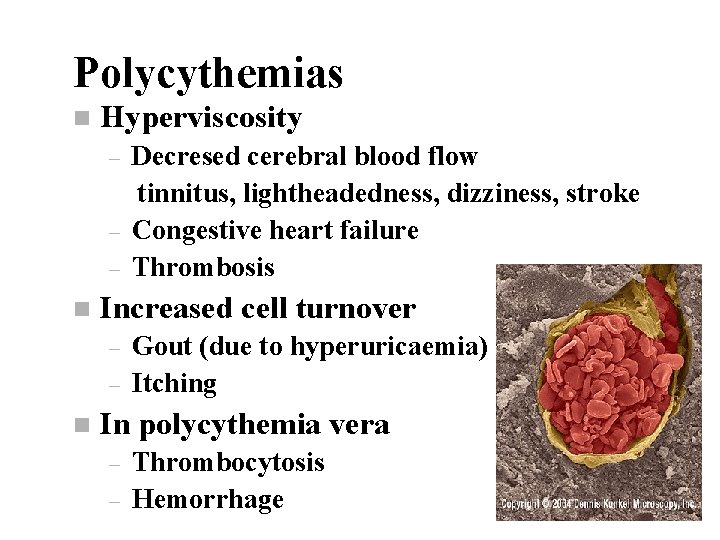
Polycythemias n Hyperviscosity – – – n Increased cell turnover – – n Decresed cerebral blood flow tinnitus, lightheadedness, dizziness, stroke Congestive heart failure Thrombosis Gout (due to hyperuricaemia) Itching In polycythemia vera – – Thrombocytosis Hemorrhage

Polycythemias n Primary: polycythemia vera myeloproliferative disorder – – – n other cell lines are affected (leukocytosis, thrombocytosis) hepatosplenomegaly EPO level: low Secondary: – hypoxia EPO production n chr. pulmonary diseases n morbid obesitiy (Pickwick’s syndrome) n high altitude – EPO overproduction: tumors

Leukocyte disorders Granulocytes (neutrophil, eosinophil basophil) n Monocytes and tissue macrophages n Lymphocytes n
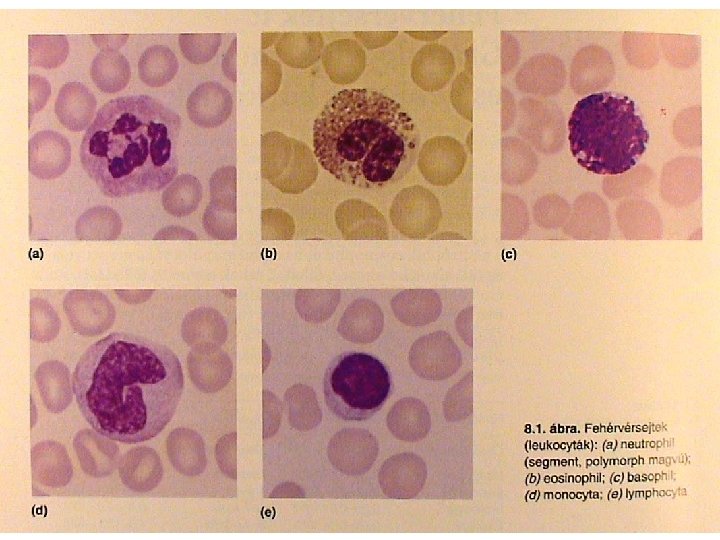

Functions of leukocytes Maintaining host defences against disease n Killing microorganisms n Digestion of tissue debris n Releasing cytokines and mediators n Activation of the immune system n

Leukocyte diseases n Benign – – – Leukocytosis > 10 G/L Leukocytopenia < 4 G/L Agranulocytosis absolute granulocyte count < 1 G/L n Malignant – – Leukemias Lymphomas
Acute leukemias n Agressive immature hemopoietic cell proliferation, without differentiation – (hiatus leucemicus in the blood smear) Subtypes: n ALL (acute lymphoblastic leukemia) n ANLL (acute non lymphoblastic leukemia) or AML (acute myeloblastic leukemia)

Acute leukemia syndrome Susceptibility to infections - serious infections n Anemia due to bone marrow infiltration and bleeding n Thrombocytopenia - bleeding tendency purpuras, petechiae, mucosal bleeding n Organ infiltration n In ALL: lymphadenopathy, splenomegaly n
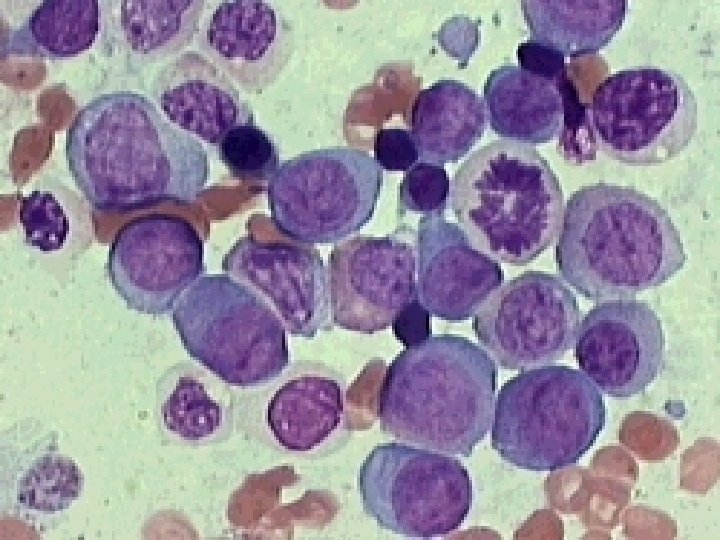
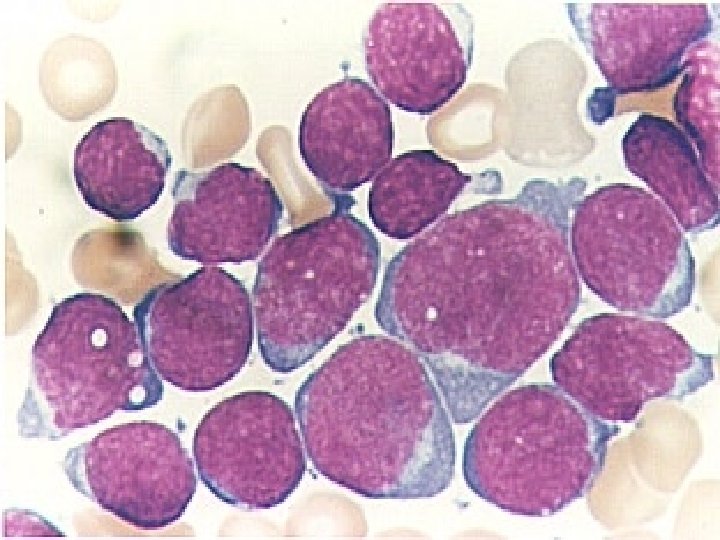

Chronic leukemias Uncontrolled expansion of premature hemopoietic cells which are able to differentiate n Subtypes: n – – Chronic myelogenous leukemia (CML or CGL) a myeloproliferative disorder Chronic lymphocytic leukemia (CLL) a malignant lymphoma

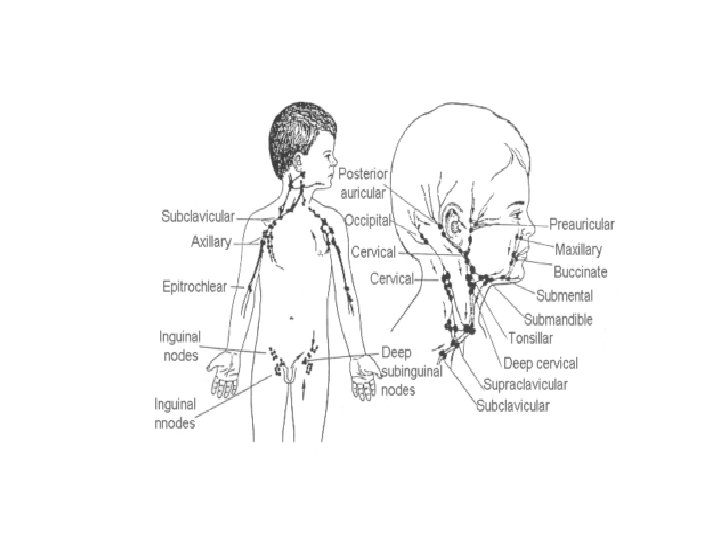
Diseases of the lymphoid system n Normal lymph nodes – – n Non palpable or <1 cm, except in the inguinal region where can be 0, 5 -2 cm sized lymph nodes normally Small lymph nodes can be remain after infection Significant: one or more new nodes >1 cm (which can’t explain by a previously recognised cause) – New lymph nodes in older age more significant n children more likely respond with lymphoid hyperplasia n lymphyadenopathy under 30 years: 80% beningn over 50 years: 40% beningn

Lymph node characteristics Location n Number (single, multiple, matted together) n Size n Tenderness n Consistency (hard, rubbery, soft) n Mobility n Skin reactions above the lymph node n

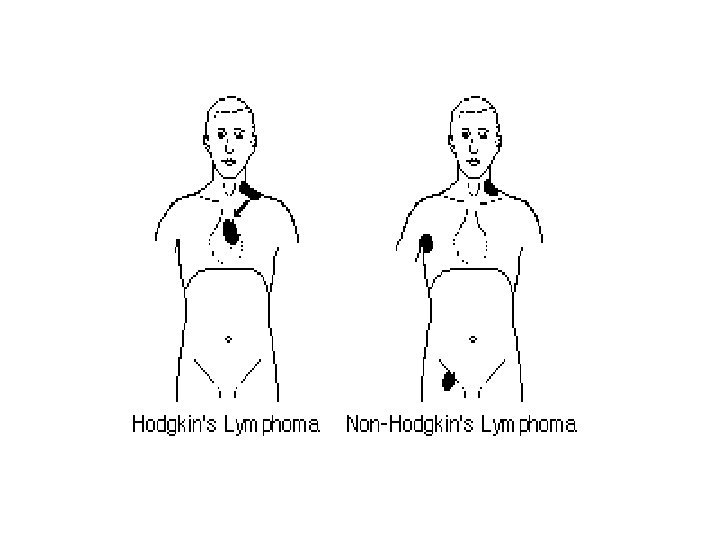
Malignant lymphomas Arise in lymph nodes or extranodal lymphoid tissue n Subtypes: n – – Hodgkin’s disease Non Hodgkin’s lymphomas

Hodgkin’s disease Mostly young adults n Asymptomatic lymphadenopathy n – – often cervical sometimes mediastinal or abdominal Hepatomegaly, splenomegaly n Fever, night sweats, loss of weight n Diagnosis: lymph node histology (Reed-Sternberg cells) Staging n

Non Hodgkin’s lymphomas Older patients n More diffuse lymph node involvement n General symptoms: fever, weight loss, night sweat n Frequent extralymphatic involvement (50%: bone marrow anemia, tct-penia) n Special forms: CLL Skin infiltration (T-cells) MALT-lymphoma Multiple myeloma n

Coagulation disorders Bleeding tendency, thrombosis, embolism Factors n platelets (number, function) n coagulation factors (amount, function) n surface of the blood vessels, circulation

Bleeding - history n History of common hemostatic stresses: n gum extraction, minor surgeries n menstruation, childbirth n injuries n Family history of bleeding tendency

Bleeding n Primary hemostatic defect (platelets) n occurs immediately after trauma n from superficial sites (skin, mucous membranes, nose, rarely from gastrointestinal, genitourinary tract) – – purpuras, petechiae ecchymoses n bleeding n time Secondary hemostatic defect (coagulation) n delayed occurence (hours, days) n from deep sites (joints, subcutaneous tissues, muscles, retroperitoneum, body cavities, cerebrum) – – hematomas hemarthroses n coagulation time

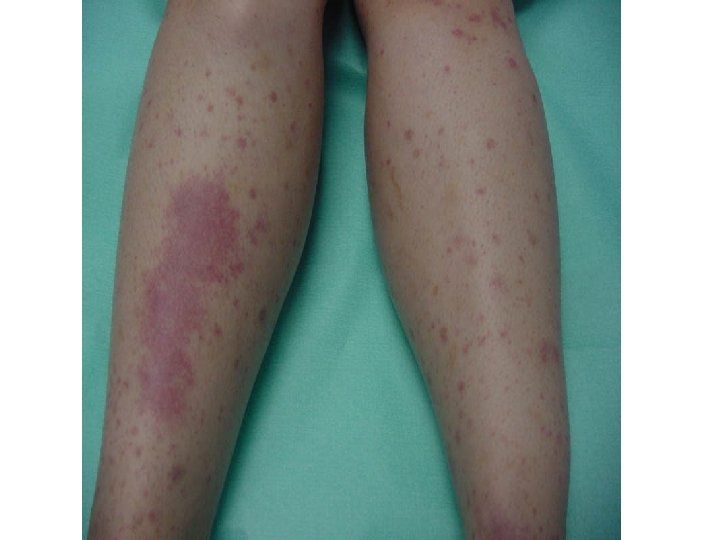
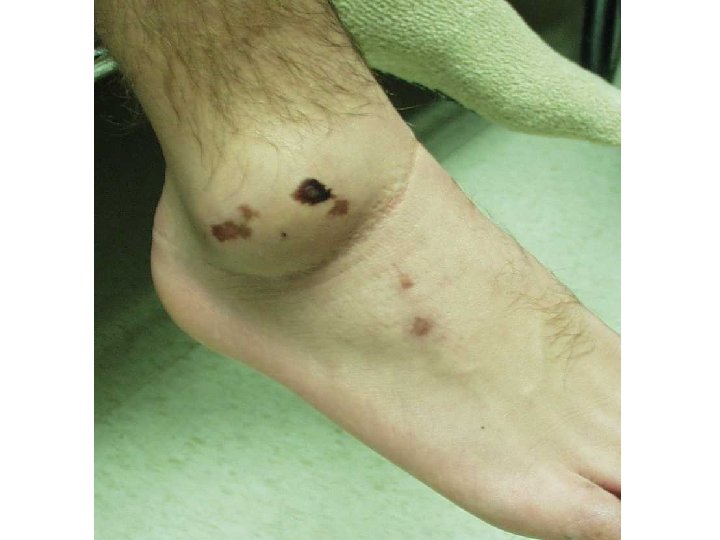
Bleeding - physical findings n From capillaries: purpuras, petechiae small, superficial, dermal or mucosal pinpoint hemorrhages characteristic for platelet disorders n From small arterioles and venules: – – – n ecchymoses subcutaneous blood collections- bruises hematomas deeper, palpable in platelet and coagulation disorders Hemarthros - bleeding into joints characteristic for coagulation disorders (mostly hemophilia) leads to chronic joint deformity
Thrombosis and embolism n Virchow’s triad – – – Hypercoagulability Circulation disturbance- congestion Pathological endothelial surface
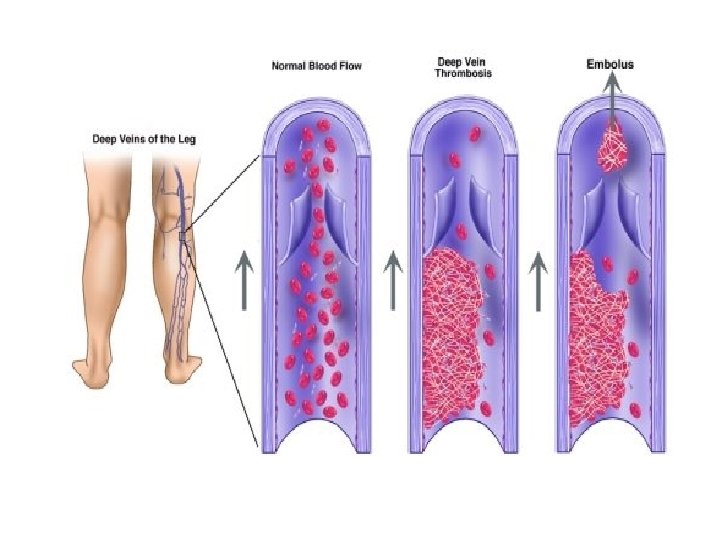
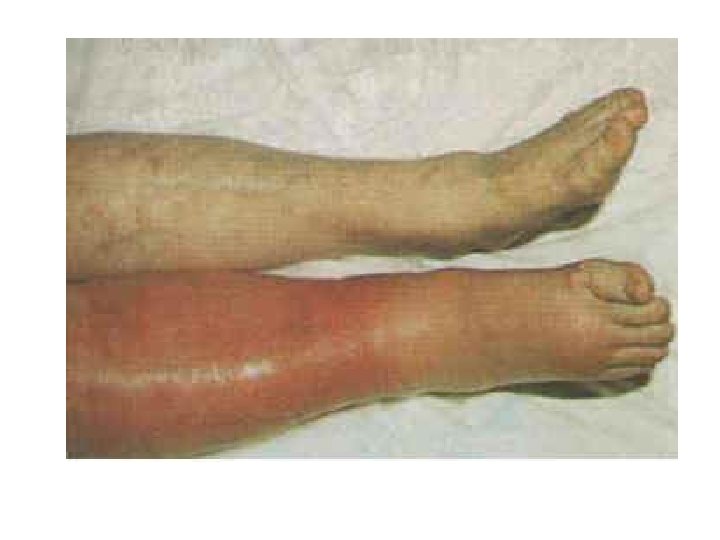
- Slides: 42