Hematological Emergencies Bikalpa Khatiwada MDCM CCFP EM Sources

Hematological Emergencies Bikalpa Khatiwada MDCM CCFP (EM)

Sources Rosen’s EMRAP Pocket Medicine Upto. Date Canadian Blood Services Pepid

Cases Oncological Transfusion Hemolytic Coagulopathy Platelet Disorders Reversing Anti-platelet / Anti-coagulants

Oncologic Emergencies

Oncology Case 50 year old male PMHx: HTN, MI – stents, Colon Ca – chemo last week. Unsure about mets.
Oncology Case Scenarios 1. Fever at home >38. 5 deg. 2. Altered level of conscious without fever 3. Acute shortness of breath 4. Back pain

Case one: scenario 1 Physical: Temp 39, HR 100, BP 110/70, Sat 95% RA, Glucose 10 mmol/L Labs: • Na 135, K 3. 5, Urea 5. 5, Creat 90. • WBC: 2. 0, ANC 0. 3, hgh 100, plts 150. Diagnosis: ?

Febrile Neutropenia Clinical Features Fever. 7 -14 days post chemo. Diagnosis Absolute neutrophil count < 0. 5 x 109/L or <1. 0 x 109/L and expected to drop to less than 0. 5. Diagnositic Strategies CBC, electrolytes, ptt, U/A and culture (even without pyuria), blood culture x 2 (take one from central line) and gram stain CXR What to avoid: rectal temps and DRE, NG tubes increase sinusitis risk. What is not needed: sputum, nares, throat or stool cultures

Etiology Causes: 85% bacterial (60 -70% gram positives) Bacterial: pseudomonas aeruginosa (less with abx given during therapy) Staph. aureus, staph. epidermidis, Fungal: Candida Albicans Virals: HSV, VZV, CMV Antibiotics are given during therapy: Septra, Quinolones Management is based on low and high risk.

Management Who is low risk: • No obvious source • No SIRS criteria • ANC > 0. 1 x 109/L • Good follow up and reliable patient. Low Risk Patient: • Cipro 750 mg q 12 h, clavulin 500 mg q 8 h • Pen Allergy: Replace clavulin with clindamycin

Management (2) High Risk Patient • Pip-tazo 3. 375 g IV q 6 h • Ceftazidime 1 g IV q 8 H (cefepime – same dosing) • Pen Allergy: Cipro 400 mg IV q 12 + tobramycin 5 mg/kg IV q 24 + vancomycin 1 g IV q 12 h • Add vanco to above if worried about line sepsis, mrsa risk.
Case 1: Scenario 2 PE: T 37. 5 deg, BP 110/70, sat 95%, RR 16, glucose 10. Diagnosis: 1. Tumour Lysis Syndrome 2. Hypercalcemia 3. Brain mets with herniation

Tumour Lysis Syndrome • Clinical Features • Typically post Chemo patient (1 -5 days). • High risk: if renal disease, dehydrated, large tumour size, advanced disease. • Confusion, tetany from hypocalemia • ARF: Insufficiency from uric acid nephropathy • Dysarrythmia from hyperkalemia • Diagnosis • Hyperkalemia, Hyperphosphatemia, Hyperuricemia, Hypocalcemia.

TLS Management Admit. Hydrate following urine output (100 ml/h) Hyperuricemia (use allopurinol 300 -600 mg/d prophylactic, 600900 mg if active TLS) Avoid alkalinization if hyperkalemic or hypocalcemic (more calcium phosphate crystals in urine) Dialysis • Indications: K > 6 mmol/l, Creat>880 mmol/l, volume overload, symptomatic hypocalcemia, uric acid>580 mmol/l, phospate>3. 2 mmol/l

Hypercalcemia Clinical Features • “Moans, groans and psychic overtones” • General: itching • Neuro/psychiatric: mood changes • Renal: polyuria, polydipsia, • Gastro: abdopain constipation, • Cardiovascular: htn, dysrhythmia, digitalis sensitivity. • Causes: Bone mets, lymphomas (NHL), or from PTH hormone like agents produced by tumours. Diagnosis • Calcium high and Albumin

Hypercalcemia Management Admit Oral and IV hydration (NS 5 -6 L/day) +/- furosemide • If urine out put adequate, add furosemide (40 -80 mg U IV) to inhance calcium output if Ca>3. 5 mmol/L (check albumin) • Bisphonates: Pamidronate 90 mg iv infusion over 4 -24 hours (takes 4 days) • Calcitonin 4 -8 IU/kg IM/SC Watch for hypokalemia (q 4 hours)
Cerebral Herniation Clinical features • Increased ICP • Bleed or Mass • Uncal : Temporal lobe compresses brainstem: one eye dilated, ipsilateral paralysis. • Central: upper pons pushed caudal altered LOC, small reactive pupils, cheyne – stokes breathing. No focal signs • Tonsillar: cerebellar tonsills into foramen magnum: Altered LOC, Headache, vomiting, meningismus. Diagnosis: CT head

Central Herniation Management Transfer IV mannitol (1 gm/Kg IV q 6 -8 h) Hyperventilation (pa. CO 2 30) IV steroids (dexamethasone 10100 mg IV loading dose)

Scenario 3: With dyspnea don’t forget Tamponade Clinical Causes: Malignant effusion, radiation pericarditis Signs jvp up, muffled heart sounds, and hypotension (beck’s triad) facial and neck swelling Diagnosis EKG: Electical alternans Physical: Pulsus paradoxis EDE ULTRASOUND Before CT PE protocol. Management Pericardiocentesis (if done emergently: 4% mortality, 17% complication rate). Ultrasound guided might be useful Recollection can occur so a catheter is useful Improve RV volume. (fluids and avoid diuretics, nitrates)
Scenario 4: Spinal cord compression Clinical • Back. Pain • Weakness • Urinary retention / loss of rectal tone. • Sensory loss Diagnosis • xray (70 -90%) • MRI if any abnormality • if unclear: CT spine first step • watch out for epidural hematoma (differential Diagnosis) Management/Disposition • Dexamethasone 10 mg IV loading (start even before testing) then 4 mg IV q 6 h • Contact oncologist

Scenario 4: Hyperuricemia Clinical Features Similar to Tumour Lysis Syndrome Can get renal uric stones, obstruction, renal failure. Diagnosis: Uric Acid levels (>530 umol/l) Management If Uric Acid >530 umol/L Allopurinol (300 -600 mg/day) Fluids (urine output 2 L/day) Alkalinise urine (Na. HCO 3, acetozolamide, +/- mannitol to mantain urine flow) +/- Dialysis

Cases Oncological Transfusion Hemolytic Coagulopathy Platelet Disorders Reversing Anti-platelet / Anti-coagulants

Transfusion issues in the ER

Transfusion Complications Symptom/Sign Based: • Fever • Dyspnea • Hypotension • Uticaria

Management Even before ABCs: • STOP THE TRANSFUSION! • Notify transfusion services.

Transfusion Case 65 year old female. Lower GI Bleed but stable. Receiving 2 U p. RBCs. GI consultant to come and see. Handover patient as she is getting her second unit of blood. Nurse comes to you and says. .

Transfusion Case Scenarios 1. “Doc, that patient getting the 2 units of blood, now has a fever of 38. 5 deg. ” 2. “Doc, she is really has having a hard time breathing” 3. “Doc, she is really confused and her BP is 80/40. ”

Scenario 1: FEVER and Transfusion Clinical • If temperature increases more than 1 deg during transfusion and is >38 C within 4 hours of transfusion Diagnosis • Febrile non-hemolytic Transfusion reaction (FNHTR) • Acute Hemolytic Transfusion Reaction • Bacterial infection/contamination
Fever and Transfusion (2) Management • Stop Transfusion • Acetominophen • Benedryl if FNHTR • If Signs of SIRS Blood cultures and gram stain from patient and from blood product Check for blood type incompatibility Check urine for hemoglobinuria (seen with ABO incompatibility) Broad spectrum antibiotics (G+ve and –ve) Disposition: • Admit: bacterial sepsis or acute hemolytic rxn.

Scenario 2: Dyspnea and Transfusion Clinical: • SOB during transfusion or shortly there after Diagnosis • Transfusion Related Acute Lung Injury (TRALI) In 6 hours of transfusion. • Transfusion associated Circulatory Overload (TACO) CHF from poor cardiac history and rapid rate of transfusion. • Anaphylaxis

Dyspnea and Transfusion (2) Management • Stop the Transfusion • ABCs, IV access, O 2 and monitor and stat CXR • TRALI Supportive – mech. Ventilation when needed. 72% needed supp. Vent. 10% mortality. Lasts up to 72 h. Steriods and Diuretic use controversial • CHF (TACO) Diuretics Reduce transfusion rate (up to 4 h) if clinically able. • Anaphylaxis

Dyspnea and Transfusion (3) Disposition • TRALI: ICU • CHF: depends on clinical status. • Anaphylaxis: 4 hour observation. (Urticaria: if less than 2/3 of body can restart once benedryl is on board)

Scenario 3: Hypotension and Transfusion Clinical • >30 mg Hg drop in systolic or diastolic pressure. Diagnosis/Differential • • • Acute Hemolytic transfusion rxn. Bacterial sepsis Severe febrile non hemolytic transfusion rxn Bradykinin mediated hypotension TRALI

Hypotension and Transfusion (2) Management: Stop the transfusion IV, O 2, Monitor Manage according to differential. Bradykinin related hypotension: • Mostly with platelet transfusions • Especially on patients with an ACEi • Care supportive and don’t restart transfusion.

Transfusion Case 2 Working in small ER. MVC from local highway comes in. Your patient has a mid-shaft femur fracture and BP is labile. • You start transfusing p. RBC and hoping to transfer patient but weather is bad and Ornge is delayed. • After the nurse hangs the fifth p. RBC, you wonder what might be the issues with massive transfusion?

Massive Transfusion Definition: • Greater than 10 Units of p. RBC in 24 hours. Dilutional Coagulopathy • Avoid waiting for INR to climb (>1. 5) and plts to drop (<50 x 109/L) • Ratio is not fixed but 1: 1: 1 suggested. p. RBC: FFP: Plts. • Pediatrics: if >20 m/kg prbc/h, FFP 15 ml/kg, plts 5 ml/kg, cryoppt 2 ml/h (for the fibrinogen) Hypothermia • If giving more than 5 units of p. RBC consider warmer. Electrolyte Abnormalities • Citrate in blood products can bind Calcium and Magnesium: Parasthesia, arrythmias, hypotension, Manage with 1 gram (1 amp of 10%) of Calcium Chloride over 10 min. • Hyperkalemia If old blood products used.

Cases Oncological Transfusion Hemolytic Coagulopathy Platelet Disorders Reversing Anti-platelet / Anti-coagulants

Hemolytic Anemias

Case 1 36 year old male immigrant from Ghana Complaining of fever, abdominal and back pain No travel but two days ago treated for urethritis in clinic with Cipro. OE: T 38. 5, BP 110/80, HR 100, Sat 99% Jaundiced. Urine: Hematuria.

Hemolytic Anemia Clinical • Jaundice, Pallor • Fever, back and abdominal pain, altered LOC. Diagnosis • CBC • Reticulocyte count (>2% expected if bone marrow active) • Blood smear (schistocytes = intravascular, spherocytes = extravascular) • Haptoglobin (low if intravascular hemolysis) • LDH elevated (from rbc turnover) • Bilirubin (indirect) elevated (if hemolytic) • Direct and indirect Coombs test (if immune mediated)

G 6 PD Clinical • Signs of hemolysis • Membrane of RBC not able to handle oxidative stress due to G 6 PD deficiency • African and Mediterranean Decent Diagnosis Management Labs for Hemolysis positive Smear: Heinz Body or Bite Cells • Supportive and Transfusion as needed Drugs to Avoid • Antibiotics: Cipro, Nitrofurantoin, Sulfa • Anti malarials • Methylene blue

Case 2 25 year old male with history of Sickle Cell Disease. Presents to ER with acute chest pain.
Sickle cell cases Trait vs Disease • Single vs. Both beta gene mutation Clinical • Vaso - Occlusive crisis Acute Chest syndrome Priapism Hand foot syndrome in pediatrics • Hematological Crisis Aplastic syndrome Acute sequestration / splenic infarct • Infectious Crisis Watch for encapsulate Bacteria: S. Pneumonia, H. Influenza

Sickle Cell Disease Diagnosis • CBC and Reticulocyte count to look out for aplastic crisis (if less than 2% and drop in • • • hemoglobin) Smear: sickle cells , howell jolly bodies. Type and screen. Electrolytes LFTs UA Imaging: CXR, Abdominal US, Bone Xrays according to history. Management • Hydration (D 5 1/2 ns at 150 -200 cc/h) – watch for CHF (especially in acute chest syndrome): Need probably 2 -4 L of fluid. • Oxygen 2 -4 L/m Nasal prongs • Aggressive Anagesia: try to have protocol for these patients. • Transfuse if aplastic anemia or splenic sequestration. Watch out for iron overload antigen exposure. • Exchange transfusion if neurological symptoms or CVA in children. • Hydroxyurea (15 -35 mg/kg/day PO): long term management

Cases Oncological Transfusion Hemolytic Coagulopathy Platelet Disorders Reversing Anti-platelet / Anti-coagulants

Disorders of Hemostasis Coagulopathy Platelet Disorders

Coagulopathy

Case 35 year M Presents to ER with Epistaxis History of Hemophilia A/B/von Willebrand’s Disease. Difficulty with Controlling epistaxis using usual techniques. Any other options?

Hemophilia A/B and von willebrand’s Disease Clinical: • Hematoma, Hemarthrosis, bruising, bleeding. • Hemophilia A (x linked factor VIII defect) • Hemophilia B (factor IX defect) Diagnosis: • CBC: potential anemia from bleeding • INR normal, PTT elevated (normalises with mixing study) Management: • Hemophilia A/von Willebrand Disease: Cryoprecipitate (2 -4 bag/10 kg ) has factor VIII, FFP dd. AVP: 0. 3 mcg/kg IV in 50 ml NS over 30 min q 8 h. • Hemophilia B: Factor IX (1 st choice) and FFP (15 -20 ml/kg)

Cases Oncological Transfusion Hemolytic Coagulopathy Platelet Disorders Reversing Anti-platelet / Anti-coagulants

Platelet Disorders
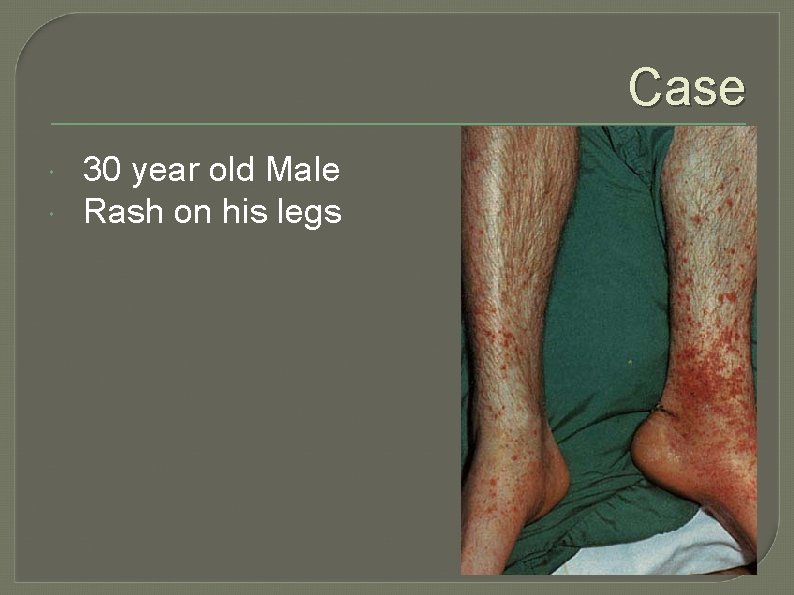
Case 30 year old Male Rash on his legs

Thrombocytopenia Case Scenarios 1: Confusion but hemodynamically stable 2: Confused and hemodynamically unstable 3: Recent viral illness, otherwise well

Thrombocytopenia Definition: less than 150 x 10 9 /L Causes: • Reduced Platelet Production: chemo, alcoholism, thiazide diuretics, leukemia, MDS. • Splenic sequestration • Destruction: Heparin Induced Lupus Clopidogrel

Thrombocytopenia (2) Diagnosis CBC and differential (just plts or more) Peripheral smear (schistocytes) If anemia: reticulocyte count, ldh, haptoglobin, bilirubin If hemolytic: INR, PTT, fibrinogen, d-dimer, coombs, ANA.

TTP: Thrombotic Thrombocytopenic Purpura Clinical: • pentad: purpura, hemolytic anemia, delerium, renal failure (hematuria, proteinurea) and fever: 40% • ADAMS 13 protease activity reduced. • Causes: idiopathic, drugs (clopidogrel, quinine), Diagnosis: • CBC: Low platelets, Anemia • Blood smear: schistocytes. • Coombs: negative • INR, PTT, Fibrinogen normal. • Liver enzymes: indirect Bili elevated. Management: • Admit (+/- ICU) • Steriods: Prednisone 1 mg/Kg PO or methylprednisolone 1 gm/kg/d IV. • Plasma exchange with FFP (aka plasmaphersis) mortality drop 90 ->17% FFP replaces ADAMTS-13 • Splenectomy • AVOID Platelet TRANSFUSION (makes clotting worse)

HUS (Hemolytic Uremic Syndrome) Clinical: • Bloody diarrhea • E. coli O 157: H 7, shigella • Shiga toxin binds to endothelial cells Diagnosis • CBC: Low platelets, Anemia, • Blood smear: schistocytes • INR, PTT, Fibrinogen normal • Thrombocytopenia, Microangiopathic hemolytic anemia, Renal failure (more so than TTP), Neurologic symptoms less than TTP. Management: • Similar to TTP

Scenario 2: DIC Clinical • Bleeding diathesis • Coagulopathy • Microangiopathic hemolytic Anemia • Look for the primary cause (sepsis, trauma, amniotic fluid emboli, transfusion) • Sick patient. Diagnosis • CBC: Anemia, low platelets. • Smear: Schistocytes. • Coagulation studies: low fibrinogen, INR and PPT elevated, D-Dimer and fibrinogen degradation products elevated. Management • Manage the Primary issue (sepsis, trauma) • If Hemorrhagic: Replace blood products: p. RBC, Platelets, FFP, cryoppt (I, V, VIII), Factor VIIa (last resort) • If Fibrin Deposition: IV Heparin (5 -10 u/kg/h) if clotting dominates the clinical picture.

Scenario 3: Idiopathic Thrombocytopenic Purpura (ITP) Clinical • A diagnosis of exclusion • Post viral infections in young children • Chronic form seen in adults (F>M) Diagnosis • Isolated low platelets and no other obvious etiology Management • Steroids (1 mg/kg/day PO Prednisone) • IVIG (1 g/kg/d IV x 2 -3 days) • Avoid platelet replacement unless active bleeding. • Disposition: Based on hemodynamic stability and follow up with hematology.
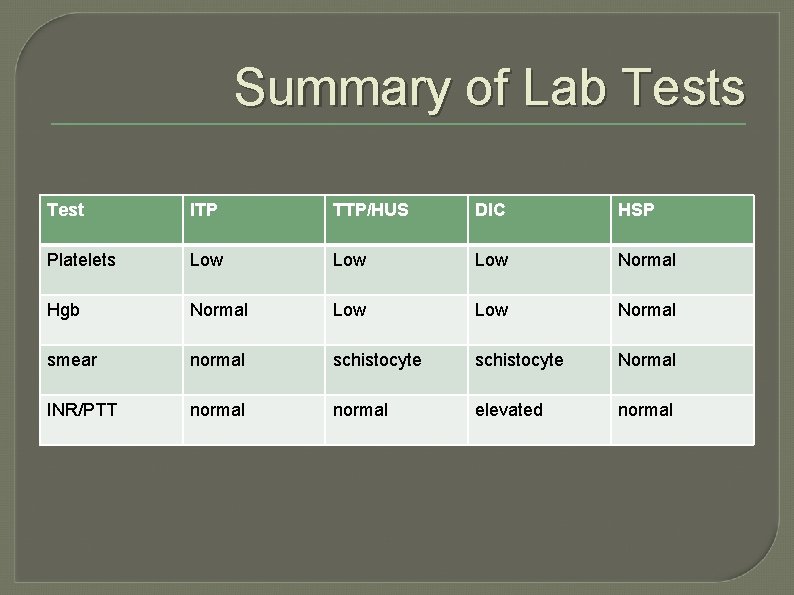
Summary of Lab Tests Test ITP TTP/HUS DIC HSP Platelets Low Low Normal Hgb Normal Low Normal smear normal schistocyte Normal INR/PTT normal elevated normal

Cases Oncological Transfusion Hemolytic Coagulopathy Platelet Disorders Reversing Anti-platelet / Anti-coagulants

Antiplatelet agents and Anticoagulation agents 70 year old male Epistaxis Not able to stop the bleeding. He is on: • Antiplatelet agent (ASA/Clopidogrel) • Anticoagulant (Warfarin, LMWH, Dabigatran)

Reversing Antiplatelet agents ASA (t 1/2 = up to 30 hours) Clopidogrel (t 1/2 = 10 hours)* Ticagrelor (t 1/2 = 7 -9 hours) Reversal: • Platelets. • DDAVP: 0. 3 ug/kg/dose in 50 ml NS over 30 min IV

Reversing Anticoagulants Heparin: • Protamine: 1 mg per 100 u Heparin used Slow Push at 5 mg/min. Watch out for side effects. Especially with fish allergy. • Low molecular weight Heparin: 1 mg per mg enoxaprin, per 100 u dalteparin. if >8 hours use half the dose (0. 5 mg/mg)

Reversing Warfarin Non Urgent: • American Association of Hematology Decreasing / Holding Reversing Testing Acute Bleed • Vitamin K: 10 mg IV • Prothrombin Concentrate Complex (Octaplex): 40 ml IV x 1 • Fresh Frozen Plasma: 10 ml/kg IV

Dabigatran (Pradax) 150 mg BID Reversal: • 60 ml Octaplex IV • 2 mg of Factor VIIa IV • ? Hemodialysis

Cases Oncological Transfusion Hemolytic Coagulopathy Platelet Disorders Reversing Anti-platelet / Anti-coagulants
- Slides: 67