HELEN HAYES HOSPITAL OUTPATIENT CARDIAC REHABILITATION PROGRAM WHAT

HELEN HAYES HOSPITAL OUTPATIENT CARDIAC REHABILITATION PROGRAM

WHAT IS CARDIAC REHABILITATION? Comprehensive Program Provided to Individuals with Cardiovascular Disease That Includes 4 Major Components: 1. Prescribed Exercise 2. Education 3. Encouragement of Healthy Eating Habits 4. Improvement of Psychological Well Being

WHAT IS CARDIAC REHABILITATION? Comprehensive Program Provided to Individuals with Cardiovascular Disease That Includes: ▪ Prescribed exercise to improve cardiovascular fitness without exceeding safe limits
WHAT IS CARDIAC REHABILITATION? Includes: ▪ Education about heart disease and ways to stabilize or reverse heart disease by improving risk factors such as: 1. Reduction/Cessation of Smoking 2. Lowering Cholesterol 3. Controlling High Blood Pressure 4. Weight Loss/Control 5. Improve/Manage Diabetes 6. Increasing Physical Activity In addition to daily videos that will be shown as you exercise, links to specific individual topics will be available on the Helen Hayes Hospital Outpatient Cardiac Rehab webpage for you to access.

WHAT IS CARDIAC REHABILITATION? Includes: ▪ Encouragement of Healthy Eating Habits – 1 on 1 consultation available with our nutritionist Carol Guarino who is also a Certified Diabetic Educator

WHAT IS CARDIAC REHABILITATION? Includes: ▪ Improvement of Psychological Well Being – 1 on 1 consultation available with our psychologist Dr. Jesse Little
GOAL OF CARDIAC REHABILITATION The primary goal of Cardiac Rehabilitation is to enable the participant to achieve his/her optimal physical, psychological, and social functioning through exercise training and lifestyle change.

BENEFITS OF CARDIAC REHABILITATION ▪ Live longer and lessen your chances for another heart attack - scientific studies have shown that people who complete a cardiac rehabilitation program can increase their life expectancy by up to five years ▪ Control heart disease symptoms such as chest pain or shortness of breath ▪ Stop or reverse damage to your blood vessels in your heart ▪ Lessen the physical and emotional effects of heart disease ▪ Improve your stamina and strength, getting you back to your usual activities, including work, hobbies, and regular exercise ▪ Improve your confidence and well-being

RISK FACTOR MANAGEMENT NON-MODIFIABLE ▪ Age ▪ Hypertension/high BP ▪ Genetic/family history ▪ Lack of physical activity/exercise ▪ Gender ▪ High cholesterol ▪ Race/ethnicity ▪ Raised blood glucose/diabetes ▪ Smoking/tobacco use ▪ Excess weight/obesity ▪ Eating Habits/Diet ▪ Depression/Stress

Non-Modifiable Risk Factors ▪ Age – As we get older our risk for cardiovascular disease increases. ▪ Genetic/family history - A positive family history involving first-degree relatives is generally associated with a twofold increase in the risk for CVD. If a close family member — a parent, brother, or sister — developed heart disease before age 55 or, in the case of female relatives, before menopause, this indicates you may be at greater risk of developing CVD. ▪ Gender - Men have a higher risk for a heart attack than women overall, but the difference narrows after women reach menopause as a result of a drop in estrogen levels, increasing the risk for women until it matches that of men. After the age of 65, the risk for heart disease is about the same between the sexes when other risk factors are similar. ▪ Race/ethnicity - The ethnic group or race that someone belongs to can have a genetic makeup and environmental influences that predispose its members to cardiovascular disease. People of the same ethnicity share many of the same genes, which is why family history and ethnicity are so closely linked. People with similar ancestry may pass down similar mutations in their genes. Native American Indian and people of African or Asian descent are at higher risk of developing heart disease.

Modifiable Risk Factors HYPERTENSION ▪ Increased force/pressure on the inner artery walls as blood passes through can create tiny micro tears that attract cholesterol, fats and calcium leading to the formation of a plaque; as the plaque grows bigger it blocks more of the artery so less blood can get through ▪ Increased force/pressure can also cause a weakening of the artery causing an aneurysm or the wall may burst bleeding into surrounding tissue ▪ At rest the goal is to have a blood pressure less than 130/80 How to Help Manage: Exercise, healthy diet, compliance with blood pressure medication, limiting excessive salt and alcohol intake all can positively affect blood pressure
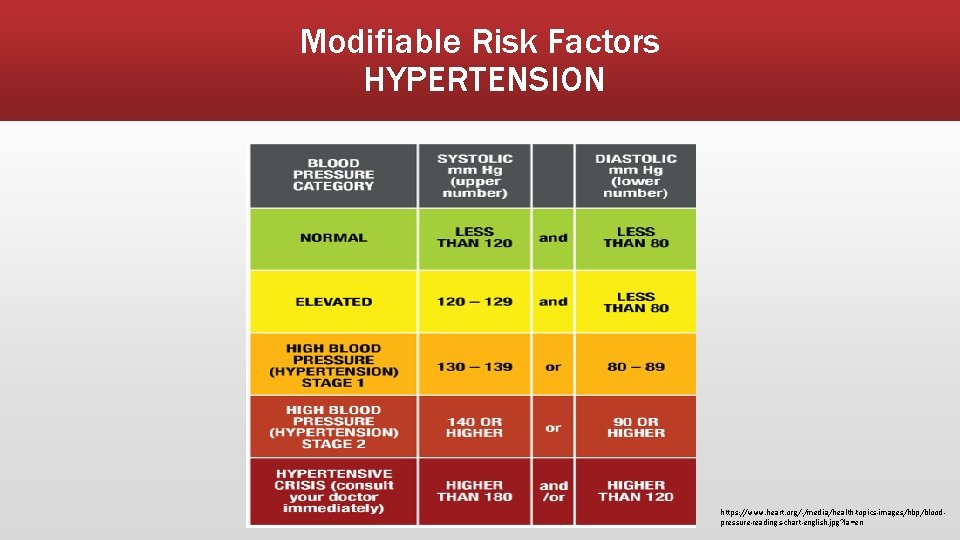
Modifiable Risk Factors HYPERTENSION https: //www. heart. org/-/media/health-topics-images/hbp/bloodpressure-readings-chart-english. jpg? la=en

Modifiable Risk Factors EXERCISE Regular aerobic exercise positively influences all the other modifiable risk factors ▪ can lower BP by 4 -6 mm. Hg ▪ can help boost “good cholesterol” and lower triglycerides ▪ improves insulin sensitivity in diabetic patients for up to 48 hours afterwards depending on the exercise ▪ helps promote weight loss and limits weight gain ▪ helps in dealing with cravings for a cigarette/reduces the urge to smoke ▪ Helps improve mood and energy levels How to help manage: Goal is to engage in at least 30 minutes of moderate intensity aerobic exercise at least 5 days a week

Modifiable Risk Factors CHOLESTEROL/LIPIDS ▪ Lipids are white, waxy fats found naturally in the body, produced mainly in the liver and also found in food sources. Excessive amounts can be damaging to the blood vessels and are an increased risk for heart attack and stroke ▪ LDL or “bad cholesterol” is most likely to clog blood vessels, increasing risk for heart disease TARGET GOAL <100 ▪ HDL or “good cholesterol” helps clear the bad LDL cholesterol out of the blood and reduces your risk for heart disease TARGET GOAL >40 MALES; >50 FEMALES ▪ Triglycerides are the chemical form in which most fat exists in food as well as in the body; avoid or limit refined grains or starchy foods which can have added sugars and are typically made from white flour which can increase triglycerides – examples include enriched or bleached white bread, pasta, sugary cereals, instant rice, bagels, pizza, pastries, pies TARGET GOAL <150

Modifiable Risk Factors CHOLESTEROL/LIPIDS How to help manage: ▪ Engage in regular exercise - Exercise helps lower triglycerides, which at high levels are linked to coronary artery disease. Exercise also raises your levels of HDL, or the “good” cholesterol which helps clear the bad cholesterol out of the body ▪ Stay compliant with statin medication – Notify your physician if you are experiencing any potential side effects such as muscle aches or pains ▪ Eat a diet high in fiber and limit saturated and trans-fats– Fiber limits the amount of cholesterol absorbed through the intestines and into the bloodstream

Both Type I (insulin deficiency) and Type II (insulin resistance) diabetes results in high concentrations of sugar in the blood that circulates through blood vessels Modifiable Risk Factors DIABETES/ RAISED BLOOD GLUCOSE https: //www. assignmentp oint. com/science/biology /about-glucose. html

EFFECTS OF HIGH BLOOD GLUCOSE: ▪ Reduces the amount of nitric oxide in the blood vessels which is a powerful vasodilator; this leads to a narrowing of the vessels and a decreased ability to expand or relax as blood flows through them which then increases the risk for hypertension ▪ With consistently high blood sugar, the vessels will remain contracted ultimately making them hard and the difficult passage of blood permanent ▪ Higher fat content in the blood is also caused by high sugar levels and accumulates in the vessels also leading to restricted blood flow Additionally, a mechanism in the cells lining our blood vessels which helps them to process glucose becomes uncontrolled in diabetes, and could be linked to the formation of blood clots and inflammation Modifiable Risk Factors DIABETES/ RAISED BLOOD GLUCOSE
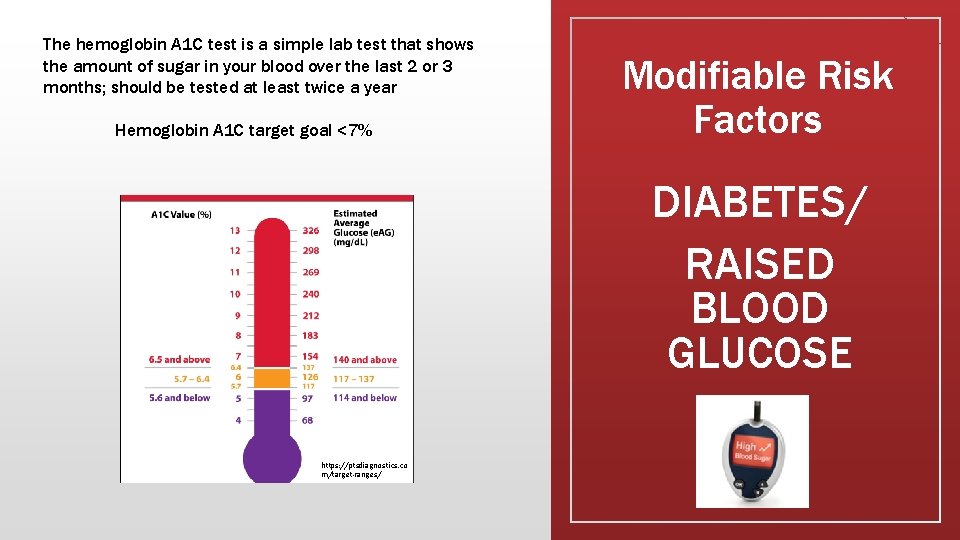
The hemoglobin A 1 C test is a simple lab test that shows the amount of sugar in your blood over the last 2 or 3 months; should be tested at least twice a year Hemoglobin A 1 C target goal <7% Modifiable Risk Factors DIABETES/ RAISED BLOOD GLUCOSE https: //ptsdiagnostics. co m/target-ranges/

How to help manage: • Stay compliant with your diabetes medications/insulin ▪ Engage in regular exercise to maintain increased insulin sensitivity ▪ Compliance with diabetic diet ▪ Weight loss Modifiable Risk Factors DIABETES/ RAISED BLOOD GLUCOSE

Modifiable Risk Factors SMOKING Smoking cigarettes affects the heart and blood vessels and remains one of the most preventable causes of heart disease. When you smoke, your arteries tighten, which makes your heart work harder. Smoking also can trigger an irregular heart rhythm and raise blood pressure, which are leading causes of stroke. According to the Centers for Disease Control and Prevention, smoking: ▪ ▪ ▪ Causes thickening and narrowing of blood vessels Raises triglycerides (a type of fat in your blood) Lowers HDL or "good" cholesterol Makes blood sticky and more likely to clot, which can block blood flow to the heart and brain Damages the cells that line the blood vessels so that the cells become swollen and inflamed Promotes the buildup of plaque (fat, cholesterol, calcium and other substances) in blood vessels and plaque rupture (resulting in an heart attack) A recent study found smoking is also associated with a thickening of the heart and lowers the heart's pumping ability—both of which are associated with heart failure. The longer and more cigarettes people without heart disease smoked, the greater the damage to their hearts' structure and function.

Modifiable Risk Factors SMOKING How to help manage: ▪ Tobacco Cessation - NY State Opt-To-Quit Program, American Lung Association Freedom From Smoking Program, Rockland County DOH “Put It Out Rockland” Program ▪ Exercise - withdrawal symptoms and cravings for cigarettes decrease during exercise and for as long as 50 minutes afterwards; also eases nicotine withdrawal symptoms when you first quit smoking

Modifiable Risk Factors EXCESS WEIGHT/OBESITY Anthropometrics BMI – Body Mass Index: Index for relating weight to height; defined as the body mass divided by the square of the body height, and is universally expressed in units of kg/m², resulting from mass in kilograms and height in meters. Underweight = < 18. 5 BMI Normal Weight = 18. 5 -24. 9 BMI Overweight = 25 -29. 9 BMI Obesity = BMI of 30 or greater

Modifiable Risk Factors EXCESS WEIGHT/OBESITY ▪ Waist Circumference: There is an increased risk for heart disease if you have a waistline of: >35 inches for women >40 inches for men

Modifiable Risk Factors EXCESS WEIGHT/OBESITY ▪ Even a modest weight loss of 5 to 10 percent of your total body weight is likely to produce health benefits, such as improvements in blood pressure, blood cholesterol, and blood sugars. ▪ For example, if you weigh 200 pounds, a 5 percent weight loss equals 10 pounds, bringing your weight down to 190 pounds. While this weight may still be in the “overweight” or “obese” range, this modest weight loss can decrease your risk factors for chronic diseases related to obesity.

Modifiable Risk Factors EXCESS WEIGHT/OBESITY How to help manage: ▪ Diet/nutrition changes ▪ Exercise ▪ Consultation with program nutritionist available ▪ Obesity Screening and Counseling – If you have Medicare Part B and have a BMI of >30 you are eligible. (Additional information available)

Modifiable Risk Factors EATING HABITS/DIET ▪ Diets high in saturated and trans-fats, cholesterol, added salt and sugar increase the risk for developing heart disease and intake should be limited

Modifiable Risk Factors EATING HABITS/DIET How to help manage: Follow a heart healthy diet Consume a diet rich in: ▪ vegetables ▪ fruit ▪ whole grain ▪ high fiber ▪ fish and lean meat Consultation with our program nutritionist, Carol Guarino, MS, RD, CDE is available (845) 786 -4811

Modifiable Risk Factors DEPRESSION/STRESS People experiencing depression, anxiety, stress, and even PTSD over a long period of time may experience certain physiologic effects on the body, such as increased cardiac reactivity (e. g. , increased heart rate and blood pressure), reduced blood flow to the heart, and heightened levels of cortisol. Over time, these physiologic effects can lead to calcium buildup in the arteries, metabolic disease, and heart disease. These effects can also arise indirectly through risky health behaviors frequently adopted by those people who experience depression, anxiety and stress such as smoking, drinking, inactive lifestyle and failure to take medications.

Modifiable Risk Factors DEPRESSION/STRESS ▪ ~20%-40% of patients after a cardiac event or diagnosis experience depression. This is 2 -4 times the number of people in the average population who experience depression. ▪ Among patients who have had a cardiac event, those who developed depression had more than two times the mortality rate of those without depression. People who have depression and a cardiac event are also two times more likely to have another cardiac event.

Modifiable Risk Factors DEPRESSION/STRESS How to help manage: ▪ Regular exercise - due to the regular release of endorphins (natural mood elevating hormones) ▪ Reach out to your physician or a mental health provider ▪ Consultation with our program’s psychologist, Jesse Little, Psy D is available (845) 786 -4165

REFERENCES 1. Burchard EG, Ziv E, Coyle N, et al. The importance of race and ethnic background in biomedical research and clinical practice. New England Journal of Medicine. 2003; 348: 1170 -1175. 2. Tishkoff S, Kidd K. Implications of biogeography of human populations for “race” and medicine. Nature Genetics. 2004; 36 (11): S 21 -S 27. 3. Jorgenson E, Tang H, Gadde M, et al. Ethnicity and human genetic linkage maps. American Journal of Human Genetics. 2005; 76 (2): 276 -290. 4. Collins F. What we do and don't know about “race, ” “ethnicity, ” genetics, and health at the dawn of the genome era. Nature Genetics. 2004; 36 (11): S 13 -S 15. 5. Statistical Fact Sheet — Populations: Hispanics/Latinos and Cardiovascular Diseases — Statistics. American Heart Association, 2004. 6. U. S Department of Health & Human Services, Revisions to the Standards for the Classification of Federal Data on Race and Ethnicity. http: //minorityhealth. hhs. gov/templates/browse. aspx? lvl=2&lvl. ID=172 The Office of Minority Health 7. Gary TL, Baptiste-Roberts K, Gregg EW, et al. Fruit, vegetable, and fat intake in a population-based sample of African Americans. Journal of the National Medical Association. 2004; 96 (12): 1599 -1605. 8. Public Health Geonomics: Family History. Centers for Disease Control and Prevention, April 2011. http: //www. cdc. gov/genomics/famhistory/resources/faq. htm#what. 9. Women and Cardiovascular Disease. World Heart Federation. http: //www. world-heart-federation. org/press/fact-sheets/women-and-cardiovascular-disease. 10. Human Aging Process. Life 123. http: //www. life 123. com/healthy-aging/age-well/human-aging-process. shtml. 11. Nucleus Medical Media. High Blood Pressure 12. AACVPR Cardiac Rehabilitation Facts Page

REFERENCES 13. High blood pressure. National Heart, Lung, and Blood Institute. https: //www. nhlbi. nih. gov/health-topics/high-blood-pressure. Accessed May 1, 2020 14. What is high blood pressure? American Heart Association. http: //www. heart. org/HEARTORG/Conditions/High. Blood. Pressure/Getthe. Facts. About. High. Blood. Pressure/What-is-High-Blood. Pressure_UCM_301759_Article. jsp#. Wrqt. Re. R 1 rcs. Accessed May 1, 2020 15. Understanding blood pressure readings. American Heart Association. http: //www. heart. org/HEARTORG/Conditions/High. Blood. Pressure/Know. Your. Numbers/Understanding-Blood-Pressure. Readings_UCM_301764_Article. jsp#. Wtn 4 hpch 3 IU. Accessed May 1, 2020. 16. Whelton PK, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APh. A/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. In press. Accessed May 1, 2020. 17. Appel LJ. Exercise in the treatment and prevention of hypertension. https: //www. uptodate. com/contents/search. Accessed May 6, 2020 18. Brook RD, Appel LJ, Rubenfire M, et al. Beyond medications and diet: alternative approaches to lowering blood pressure: a scientific statement from the A merican Heart Association. Hypertension 2013; 61: 1360. 19. Diaz KM, Shimbo D. Physical activity and the prevention of hypertension. Curr Hypertens Rep 2013; 15: 659. 20. Pescatello LS, Mac. Donald HV, Ash GI, et al. Assessing the Existing Professional Exercise Recommendations for Hypertension: A Review and Recommendations for Future Research Priorities. Mayo Clin Proc 2015; 90: 801. 21. Boutcher YN, Boutcher SH. Exercise intensity and hypertension: what's new? J Hum Hypertens 2017; 31: 157. 22. Kraus WE, Bittner V, Appel L, et al. The National Physical Activity Plan: a call to action from the American Heart Association: a science advisory from the American Heart Association. Circulation 2015; 131: 1932. 23. Eckel RH, et al. 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Journal of the American College of Cardiology. 2014; 63: 2960.

REFERENCES 24. Shaking the salt habit to lower high blood pressure. American Heart Association. http: //www. heart. org/HEARTORG/Conditions/High. Blood. Pressure/Make. Changes. That. Matter/Shaking-the-Salt-Habit-to. Lower-High-Blood-Pressure_UCM_303241_Article. jsp#. Wrq 0 Ye. R 1 rcs. Accessed Feb. 21, 2018. 25. Smoking, high blood pressure and your health. American Heart Association. http: //www. heart. org/HEARTORG/Conditions/High. Blood. Pressure/Make. Changes. That. Matter/Smoking-High-Blood-Pressureand-Your-Health_UCM_301886_Article. jsp#. Wrq 0 qu. R 1 rcs. Accessed Feb. 21, 2018. 26. Managing stress to control high blood pressure. American Heart Association. http: //www. heart. org/HEARTORG/Conditions/High. Blood. Pressure/Make. Changes. That. Matter/Managing-Stress-to-Control. High-Blood-Pressure_UCM_301883_Article. jsp#. Wrq 08 e. R 1 rcs. Accessed March 12, 2018. 27. Cholesterol Guidelines and Heart Health https: //my. clevelandclinic. org/health/articles/16866 -cholesterol-guidelines-- heart-health. Accessed April 13, 2020 28. What Your Cholesterol Levels Mean https: //www. heart. org/en/health-topics/cholesterol/about-cholesterol/what-your-cholesterol-levels-mean. Accessed April 13, 2020 29. HDL (Good), LDL (Bad) Cholesterol and Triglycerides https: //www. heart. org/en/health-topics/cholesterol/hdl-good-ldl-bad-cholesterol-and-triglycerides. Accessed April 13, 2020 30. http: //www. diabetes. org/diabetes-basics/diagnosis/ 31. http: //www. joslin. org/info/conversion_table_for_blood_glucose_monitoring. html 32. http: //www. diabetes. org/diabetes-basics/common-terms / 33. https: //www. virginiamason. org/complications 34. http: //www. diabetes. org/living-with-diabetes/treatment-and-care/blood-glucose-control/a 1 c 35. http: //www. nhlbi. nih. gov/files/docs/guidelines/atglance. pdf 36. http: //www. heart. org/HEARTORG/Conditions/Cholesterol/About-Cholesterol_ UCM_001220_Article. jsp , 37 http: //www. news-medical. net/health/Cholesterol-Physiology. aspx

REFERENCES 38. http: //www. heart. org/HEARTORG/Conditions/Cholesterol/About. Cholesterol/Good-vs-Bad-Cholesterol_UCM_305561_Article. jsp 39. . http: //www. diabetesincontrol. com/how-high-blood-sugars-damage-blood-vessels/ 40. https: //healthhearty. com/how-high-blood-sugar-damages-blood-vessels 41. https: //www. sciencedaily. com/releases/2009/05/090511140951. htm 42. How blood vessel damage from high glucose concentrations unfolds https: //www. sciencedaily. com/releases/2019/06/190605105950. htm 43. Smoking and Heart Disease https: //www. cardiosmart. org/topics/healthy-living/stop-smoking/smoking-and-heart-disease 44. Fight Cravings With Exercise https: //smokefree. gov/challenges-when-quitting/cravings-triggers/fight-cravings-exercise 45. Obesity and Heart Disease https: //www. cardiosmart. org/assets/infographic/obesity-and-heart-disease 46. https: //www. heart. org/en/healthy-living/healthy-lifestyle/my-life-check-- lifes-simple-7 47. Blackburn G. (1995). Effect of degree of weight loss on health benefits. Obesity Research 3: 211 S-216 S. 48. NIH, NHLBI Obesity Education Initiative. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults 49. https: //www. nhlbi. nih. gov/health/educational/lose_wt/BMI/bmi_dis. htm 50. https: //www. nhlbi. nih. gov/health-pro/guidelines/current/obesity-guidelines/e_textbook/txgd/4142. htm 51. https: //www. heart. org/en/healthy-living/healthy-eating/eat-smart

REFERENCES 52. https: //www. cardiosmart. org/topics/healthy-living/eat-better 53. https: //www. cardiosmart. org/topics/healthy-living/eat-better/heart-healthy-diets 54. https: //www. cardiosmart. org/topics/healthy-living/assets/infographic/heart-healthy-nutrition 55. Cardiovasc Psychiatry Neurol. 2013; 2013: 695925. Published online 2013 Apr 7. doi: 10. 1155/2013/695925 56. https: //www. heart. org/en/healthy-living/healthy-lifestyle/mental-health-and-wellbeing/how-does-depression-affect-the-heart 57. https: //www. cardiosmart. org/news/2019/2/experts-highlight-the-strong-link-between-depression-and-heart-disease 58. Loyola University Health System. "New evidence for link between depression and heart disease. " Science. Daily. 19 February 2013.
- Slides: 35