Heart to Heart A Discussion about Nutrition in

Heart to Heart: A Discussion about Nutrition in Pediatric Patients Undergoing Heart Transplant Melissa Froh, MS, RD, CNSC

Objectives • Understand the impact of malnutrition in patients waiting for transplant • Understand the nutrition needs of patients during the transplant process
Statistics • Based on UNOS data for 2018, there were 1895 pediatric solid organ transplant recipients (less than 18 year of age). – Of those, 25% received heart transplants • Recipients less than 1 year of age accounted for 25% • Ages 1 -5 accounted for another 25% • Ages 6 -10 accounted for 14% • Ages 11 -17 accounted for 36%

Defining Malnutrition • Malnutrition: “an imbalance between nutrient requirement and intake, resulting in cumulative deficits of energy, protein, or micronutrients that may negatively affect growth, development, and other relevant outcomes 2, 3. ”

Causes of Malnutrition in Heart Failure • Decrease energy intake 2, 3 – Fatigue – Intolerance – Anorexia – Intermittent NPO/feeding interruptions – Malabsorption • Increased energy requirements 2, 3 – Hypermetabolism – Inflammation
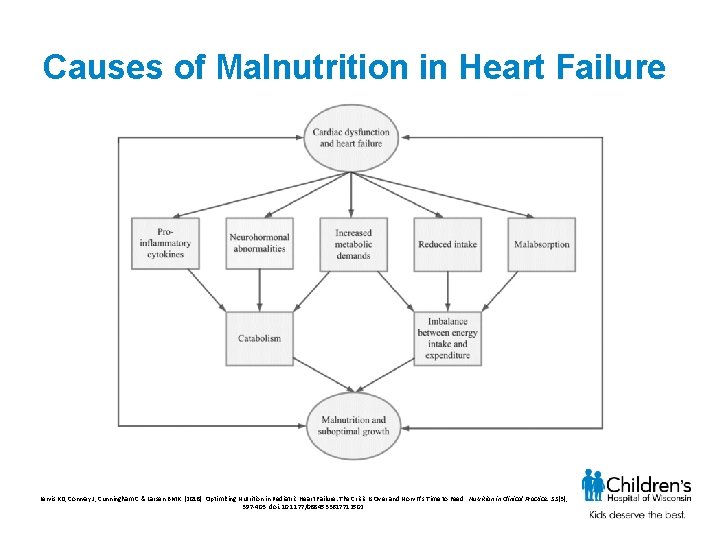
Causes of Malnutrition in Heart Failure Lewis KD, Conway J, Cunningham C & Larsen BMK. (2018). Optimizing Nutrition in Pediatric Heart Failure: The Crisis Is Over and Now It’s Time to Feed. Nutrition in Clinical Practice. 33(3), 397 -403. doi: 10. 1177/0884533617712502.

Prevalence of Malnutrition in Pediatric Heart Failure • Malnutrition is a significant problem in children with heart failure 2, 3, 4 – Prevalence of wasting in patients with heart failure has been reported to be as high as 86% (defined by z-score of weight-for-height < -2) • According to the Pediatric Cardiomyopathy Registry, 24% of children with dilated cardiomyopathy were malnourished • Studies have shown that between 14 -18% of children on the transplant waitlist are malnourished

Impact of Malnutrition • Malnutrition has been shown to increase risk of waitlist mortality – In a 2014 study of 1653 infants less than 2 years old, moderate or severe wasting was shown to be in an independent risk factor for waitlist mortality 5 • Of the patients included, 29% died on the waitlist – 52% had normal nutrition status, 24% had mild wasting, and 15% had moderate or severe wasting – Nutrition remained an independent risk factor of waitlist mortality even after adjusting for other predictors of heart failure: listing status, inotrope use, ECMO or VAD support, and ventilator use

Impact of Malnutrition • Same authors assessed the BMI of 2712 patients 2 -18 years of age 6 – BMI below the 1 st percentile was a risk factor for both waitlist and post-transplant mortality in patients with cardiomyopathy. – It was noted that in this study, there were differing risk factors based on disease etiology

Impact of Malnutrition • Another study published in 2014 looked at both poor growth and hypoalbuminemia 7 – 27% of the patients had poor growth at the time of transplant – Patients with z-score less than -2 at time of listing and time of transplant had decreased survival

Challenges of Assessing Malnutrition in Pediatric Heart Failure • Historically, there have not been standard definitions of malnutrition severity 2, 5 • American Society of Parenteral and Enteral Nutrition definitions allow for improved studies on malnutrition • Wasting and malnutrition in heart failure patients can be masked by fluid overload – Important to use weight at a time when patient was euvolemic

Nutrition Goals for Transplant • Overall goal is to optimize nutrition status in order to improve outcomes and quality of life 8 – Improve energy intake – Improve micronutrient deficiencies – Early intervention
Nutrition Goals for Transplant: Estimated Energy Needs • Children in heart failure often require 1050% more calories 3, 4 – Increased BMR from increased work of the heart – Increased work of breathing – Infectious and inflammatory processes – Cyanosis • Leads to a greater dependence on anaerobic metabolism, which is less energy efficient

Nutrition Goals for Transplant: Estimated Energy Needs • Pre-transplant needs, using predictive equations 3, 4, 8: – 110 -125% of the EER – REE x 1. 6 -2 – Up to 120 -150 kcals/day for infants • Post-transplant needs may decrease – In the short-term post-op period, may continue to need increased energy intake, but often can return to similar needs as healthy patients

Nutrition Goals for Transplant: Protein • Protein needs are higher given critical illness and surgical recovery 3, 4 – Wound healing support – Preserve skeletal muscle mass – Support inflammatory responses – Account for losses from possible malabsorption due to impaired perfusion

Nutrition Goals for Transplant: Protein • Estimated needs 3, 4 – 50 -100% higher than healthy patients – RDA x 1. 5 -2

Nutrition Goals for Transplant: Micronutrients • Micronutrient deficiencies may be worsened by medications 3, 4, 8, 9 – Interfere with metabolism – Increase excretion • Key micronutrients: – Vitamin D – Sodium

Nutrition and Mechanical Support • Children requiring VAD support had greater improvement in nutrition status while waiting for heart transplant and a lower prevalence of malnutrition at time of transplant 10

Conclusion • Malnutrition is highly prevalent in pediatric heart failure and can have a negative effect on transplant outcomes • Goals of nutrition support during the transplant process are to correct deficiencies and support growth and development as best as possible

References 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. UNOS Data Report: Transplants in the U. S. by Recipient Age. https: //optn. transplant. hrsa. gov/data/view-datareports/national-data/ Hollander SA. (2019). Malnutrition in Pediatric Heart Failure. American College of Cardiology. Retrieved from https: //www. acc. org/latest-in-cardiology/articles/2019/02/04/06/39/malnutrition-in-pediatric-heart-failure Lewis KD, Conway J, Cunningham C & Larsen BMK. (2018). Optimizing Nutrition in Pediatric Heart Failure: The Crisis Is Over and Now It’s Time to Feed. Nutrition in Clinical Practice. 33(3), 397 -403. doi: 10. 1177/0884533617712502. Miller TL, Neri D, Extein J, et al. (2007. Nutrition in pediatric cardiomyopathy. Progress in Pediatric Cardiology. 24(2007), 59 -71. doi: 10. 1016/j. ppedcard. 2007. 08. 007 Godown J, Friedland-Little JM, Gajarski, RJ, et al. (2014). Abnormal nutrition affects waitlist mortality in infants awaiting heart transplant. International Society for Heart and Lung Transplantation. 33(3), 235 -240. Retrieved from https: //www. sciencedirect. com/science/article/pii/S 1053249813015350? via%3 Dihub Godown J, Donohue JE, Yu S, et al (2014). Differential effect of body mass index on pediatric heart transplant outcomes based on diagnosis. Pediatric Transplantation. 18(7), 771 -776. doi: 10. 1111/petr. 12352 Castleberry C, White-Williams C, Naftel D, et al. (2014). Hypoalbuminemia and poor growth predict worse outcomes in pediatric heart transplant recipients. Pediatric Transplantation. 18(3), 280 -287. doi: 10. 1111/petr. 12239. Benzecry SG, Leite HP, Oliveira FC, et al. (2008). Interdisciplinary approach improves nutritional status of children with heart diseases. Nutrition. 24(7 -8), 669 -674. doi: 10. 1016/j. nut. 2008. 03. 016. Bailer, J. , & Kaufman, B. D. (2010). Nutrition Implications of Heart Failure and Heart Transplantation in Children With Dilated Cardiomyopathy: A Case Series. ICAN: Infant, Child, & Adolescent Nutrition, 2(6), 377– 384. https: //doi. org/10. 1177/1941406410390937 Hollander SA, Schultz LM, Dennis K, et al. (2019). Impact of ventricular assist device implantation on the nutritional status of children awaiting heart transplantation. Pediatric Transplantation. 23(2), e 13351. doi: 10. 1111/petr. 13351.

Questions?
- Slides: 21