Heart Failure Chapter 35 Iggy Lehne Heart Failure












































- Slides: 45

Heart Failure Chapter 35 Iggy Lehne Heart Failure Medications

Heart Failure • Also called pump failure; inability of heart to work effectively as a pump • Major types: • • • Left-sided Right-sided High-output 2

Etiology • Systemic hypertension is the cause of heart failure in most cases • About one third of patients experiencing MI also develop heart failure • Structural heart changes (e. g. , valvular dysfunction) cause pressure or volume overload on heart 3

Risk Factors • Primary risk factors • Hypertension • CAD • Contributing risk factors • • • Advanced age Diabetes Tobacco use Obesity High serum cholesterol Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Left-Sided Heart Failure • Formerly known as congestive heart failure • Typical causes • Hypertension • Coronary artery disease • Valvular disease • Not all cases involve fluid accumulation • Two types: • Systolic • Diastolic 5

Right-Sided Heart Failure • Causes • Left ventricular failure • Right ventricular MI • Pulmonary hypertension • Right ventricle cannot empty completely • Increased volume and pressure in venous system and peripheral edema 6

High-Output Failure • Cardiac output remains normal or above normal • Caused by increased metabolic needs of hyperkinetic conditions • Septicemia • Anemia • Hyperthyroidism 7

Pathophysiology Systolic HF • Inability to pump blood forward • Caused by • • Impaired contractile function Increased afterload Cardiomyopathy Mechanical abnormalities • Decreased left ventricular ejection fraction (EF) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Pathophysiology Diastolic HF • Impaired ability of the ventricles to relax and fill during diastole, resulting in decreased stroke volume and CO • Heart failure with normal EF • Result of left ventricular hypertrophy from hypertension, MI, valve disease, or cardiomyopathy Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Pathophysiology Mixed Heart Failure • Mixed systolic and diastolic failure • Seen in disease states such as dilated cardiomyopathy (DCM) • Poor EFs (<35%) • High pulmonary pressures • Biventricular failure • Both ventricles may be dilated and have poor filling and emptying capacity Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Compensatory Mechanisms • When cardiac output is insufficient to meet body’s demands, these mechanisms operate to increase cardiac output: • • Sympathetic nervous system stimulation Other renin-angiotensin system activation Chemical responses (BNP) Myocardial hypertrophy 11

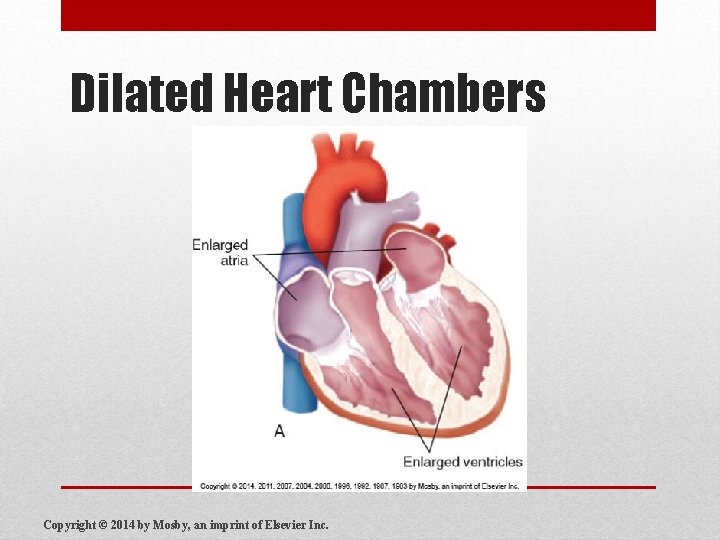
Dilated Heart Chambers Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Left-Sided Heart Failure • Clinical manifestations • • Weakness Fatigue Dizziness Acute confusion (low flow) Pulmonary congestion Breathlessness Oliguria 13

Right-Sided Heart Failure • Clinical manifestations • • Jugular vein distention Increased abdominal girth Dependent edema Hepatomegaly Hepatojugular reflux Ascites Weight most reliable indicator of fluid gain/loss 14

Chronic Heart Failure Clinical Manifestations • Dependent on age, underlying type and extent of heart disease, and which ventricle is affected • FACES • • • Fatigue Limitation of Activities Chest congestion/cough Edema Shortness of breath Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Assessment of Right-Sided Heart Failure • Laboratory • • • Electrolytes Hemoglobin and hematocrit BNP Urinalysis (proteinuria/high specific gravity) ABGs • Imaging • CXR • Echocardiography (best diagnostic tool) • ECG • Pulmonary artery catheter 16

Heart Failure Complications • • • Pleural effusion Dysrhythmias – atrial and ventricular Left ventricular thrombus Hepatomegaly Renal failure Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Diagnostic Studies • • Determine and treat underlying cause Endomyocardial biopsy (EMB) Echocardiography and/or nuclear imaging Chest x-ray ECG, stress test Cardiac catheterization BNP (NT-pro. BNP), ABGs Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Collaborative Management • Main treatment goals • • Treat the underlying cause and contributing factors Maximize CO Provide treatment to alleviate symptoms Improve ventricular function Improve quality of life Preserve target organ function Improve mortality and morbidity Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Collaborative Management • Oxygen therapy • Relieves dyspnea and fatigue • Physical and emotional rest • Conserve energy and decrease oxygen needs • Dependent on severity of HF • Structured exercise program Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Collaborative Management • Biventricular pacing/cardiac resynchronization therapy (CRT) • With implantable cardioverter-defibrillator (ICD) • IABP and VADs as bridge or destination therapy for stage IV HF Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Drug Therapy • Diuretics • Reduce edema, pulmonary venous pressure, and preload • Promote sodium and water excretion • Loop diuretics • Thiazide diuretics • Monitor potassium levels (hypokalemia) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Drug Therapy • RAAS inhibitors • • ACE inhibitors Angiotensin II receptor blockers Aldosterone antagonists Monitor potassium levels (hyperkalemia) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Drug Therapy • β-adrenergic blockers • Vasodilators • Nitrates • Bi. Dil • Positive inotropic agents • Digitalis Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nutritional Therapy • Low sodium diet • Individualize recommendations and consider cultural background (www. nhlbi. nih. gov/health/index. htm#recipes) • Recommend Dietary Approaches to Stop Hypertension (DASH) diet • Sodium is usually restricted to 2 g/day Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nutritional Therapy • Fluid restriction not generally required • If required, < 2 L/day. • Ice chips, gum, hard candy, ice pops to help thirst • Daily weights important • Same time, same clothing each day • Weight gain of 3 lb (1. 4 kg) over 2 days or a 3 - to 5 -lb (2. 3 kg) gain over a week should be reported to health care provider Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Assessment • Subjective data • Past health history • Any cardiac history or diseases that increase risk for cardiac dysfunction • Drugs • Any cardiac drugs, estrogens, steroids, NSAIDs, OTC drugs, herbs Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Assessment • Subjective data • Fatigue, depression, anxiety • Usual sodium intake • Nausea/vomiting/anorexia • Stomach bloating • Weight gain • Ankle swelling Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Assessment • Subjective data • Nocturia • Decreased daytime urine output • Constipation • Dyspnea, orthopnea, cough • Palpitations • Dizziness, fainting Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Assessment • Subjective data • • Number of pillows used for sleeping Paroxysmal nocturnal dyspnea Insomnia Chest pain or heaviness RUQ pain, abdominal discomfort Behavioral changes Visual changes Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Assessment • Objective data • • Skin color and temperature Edema Respiratory rate and sounds Frothy, blood-tinged sputum Heart rate and sounds Abdominal distention Changes in LOC Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Assessment • Objective data • • Serum electrolytes BUN, creatinine Liver function tests NT-pro. BNP or BNP • • Chest x-ray Echocardiogram ECG O 2 saturation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Diagnosis • Impaired gas exchange • Decreased cardiac output • Excess fluid volume • Activity intolerance Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Planning • Overall goals • Decrease in symptoms • Decrease in peripheral edema • Increase in exercise tolerance • Compliance with the medical regimen • No complications related to HF Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Implementation • Health promotion • Identify and treat risk factors for HF to prevent or slow progression • Flu and pneumonia vaccinations for patients with HF Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Intervention • Basic principles of care • HF is a progressive disease: establish treatment plans and quality -of-life goals • Use of self-management tools for symptom management • Restrict salt (and water at times) • Conserve energy • Maintain support systems Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Intervention • • Monitor respiratory status Administer oxygen therapy Semi-Fowler’s position Monitor hemodynamic status Daily weights I&O Administer prescribed drugs Monitor edema Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Nursing Intervention • • Alternate rest with activity Provide diversionary activities Monitor response to activity Collaborate with OT/PT Reduce anxiety Evaluate support system Patient teaching Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Ambulatory and Home Care • Explain to patient and caregiver physiologic changes that have occurred • Assist patient to adapt to both the physiologic and psychologic changes • Integrate patient and caregiver(s) into the overall care plan Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Patient Teaching • Signs and symptoms of HF exacerbations – what to do/report • Importance of early detection • Can have positive outlook with chronic health problem if treatment plan is followed Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Patient Teaching • Drug therapy • • • Expected actions Signs of drug toxicity How to take pulse and what to report Signs and symptoms of hypokalemia and hyperkalemia BP monitoring as needed Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Patient Teaching • Dietary therapy • • • Written plan Reading labels for sodium No added salt Daily weights Smaller, more frequent meals Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Patient Teaching • Activity/rest • • • Energy-conserving and energy-efficient behaviors Exercise training (cardiac rehab) Increase gradually Avoid heat and cold extremes Rest after exertion Avoid emotional upsets Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Patient Teaching • Ongoing monitoring • • • Know FACES Reappearance of symptoms What to report Regular follow-up Support group • Health promotion • Vaccinations • Reduce risk factors Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Chronic HF Evaluation • Monitoring to assess outcomes and prevent/ limit future hospitalizations • • Vital signs Weight Pulse oximetry Dyspnea • Home health nurses can be essential • Can use electronic monitoring Copyright © 2014 by Mosby, an imprint of Elsevier Inc.