Hearing Dr B Kalpana At the end of

Hearing Dr B. Kalpana

At the end of class students should be able to: 1. Explain the structure and functions of external, middle and inner ear 2. Explain the role of external, middle and inner ear in mechanism of hearing. 3. Trace auditory pathway 4. List theories of hearing. 5. List the types of deafness and its causes.
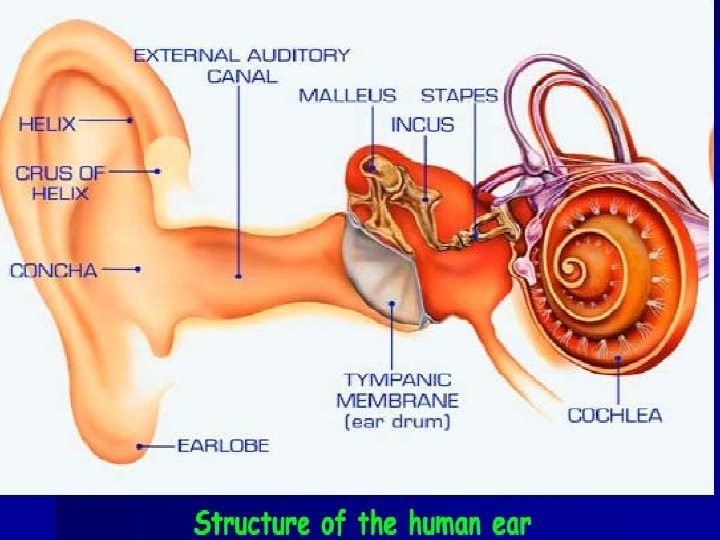

External Ear:

Structures – Auricle or Pinna • elastic cartilage covered with skin – External Auditory canal • curved 1” tube of cartilage & bone • Ear wax
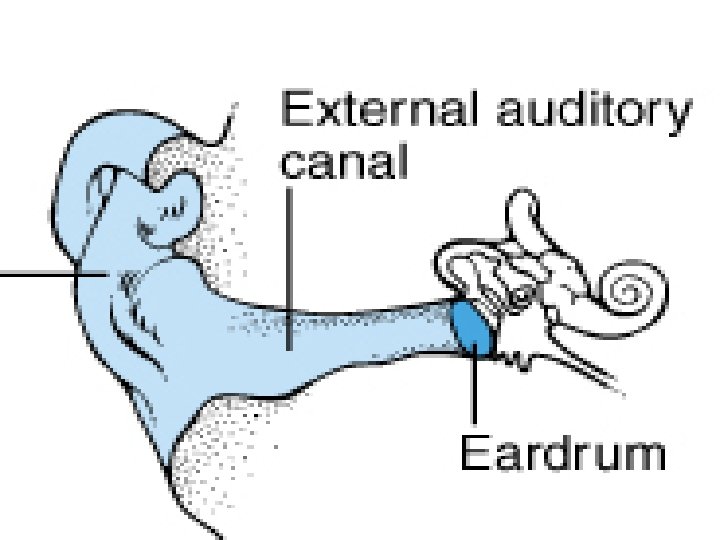

Function: • Establish direction of sound waves • Conducts sound waves to middle ear • Help in increasing the sound pressure at the tympanic membrane by about 10 -15 db. • Aid in sound localization. • Provides warm humid environment which is essential for proper vibration of the tympanic membrane.

• Various chemicals present in the wax kills the bacteria and fungi • It limits the frequency that reaches the tympanic membrane • Help in sound collection.

Middle ear
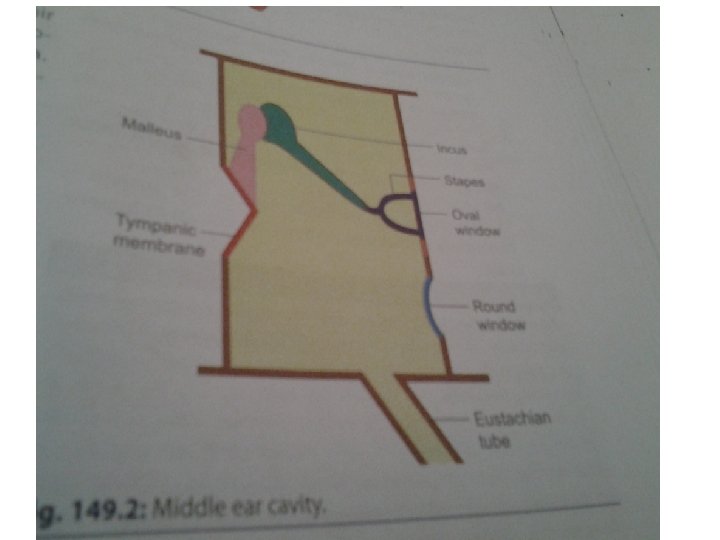

• Air filled cavity. • Epithelial cells-four walls • Anterior -opens to exterior via Eustachian tube • Posterior-communicates with mastoid air cells. • Medial-separates middle from internal ear. • Lateral wall-tympanic membrane

Tympanic membrane • Thin elastic semitransparent conical membrane-5090 mm 2 in surface area. • Collagen and elastic fibers. Functions • Acts as a resonator Sensitive to pressure changes • Critically dampens sound waves • Mechanical barrier-prevents entry of foreign bodies.
OSSICLES

Ossicular muscles: Tensor tympani: • • Attached to the malleus. In the tympanic membrane increases the tension. More responsive to sound waves. Helps open Eustachian tube. Stapedius • Attached to the stapes. • Pulls footplate of stapes out from oval window • Contracts in Response to Loud sounds, chewing, speaking. • Dampens the vibration transmitted to inner ear.

• Tympanic reflex • Protective reflex • Checks the overstimulation of hair cells in inner ear. • Prevents damage to cochlea

• Function: • Support ossicular chain. • Protect the inner ear from high intensity sounds. • Prevents damage of cochlea • Improves sound transmission to cochlea • Supress self-generated sounds.

Eustachian tube • Middle ear cavity with the pharynx. • Normally kept closed, opened while swallowing, chewing, yawning and sneezing. • Equalizes the pressure on the two sides of the ear drum. • Closure of the tube results in conduction deafness.

Functions of middle ear: 1. Impedance matching: The resistance offered by the fluid is overcome by the process of impedance matching. It is brought about by • The difference in the surface area of the tympanic membrane and the oval window (50 sqmm: 3 sqmm)which increase the pressure acting on the oval window by about 17 times.
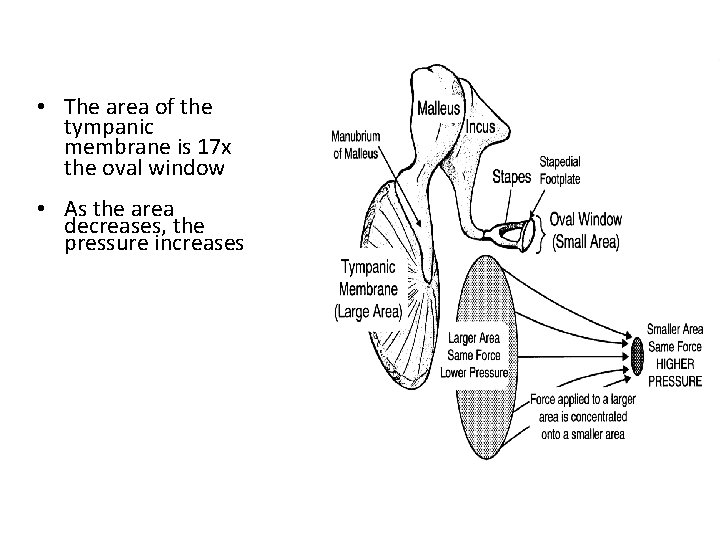
• The area of the tympanic membrane is 17 x the oval window • As the area decreases, the pressure increases


• The lever action provided by the special arrangement of the ear ossicles which further increase the pressure by 1. 3 times.

• Total amplification of sound waves -22 times

2. Pressure equilibrium on the either side of the tympanic membrane. 3. Protection from the loud sounds(Tympanic reflex) Tensor tympaneae pulls malleus inwards and stapedius pulls stapes outwards. Two forces oppose each other and develop a high degree of rigidity. 4. Acts as a biological filter.

Inner Ear---Bony Labyrinth

• Labyrinth-complicated series of canals. • Outer bony labyrinth-fluid –perilymph • surrounds membranous labyrinth • Inner membranous labyrinth –series of fluid- filled -endolymph. It consists of auditory apparatus and vestibular apparatus.

Auditory apparatus • Cochlea • Transduction of sound energy into Aps in cochlear nerve fiber. Vestibular apparatus • saccule, utricle and semicircular canals • Maintenance of posture and balance of body.
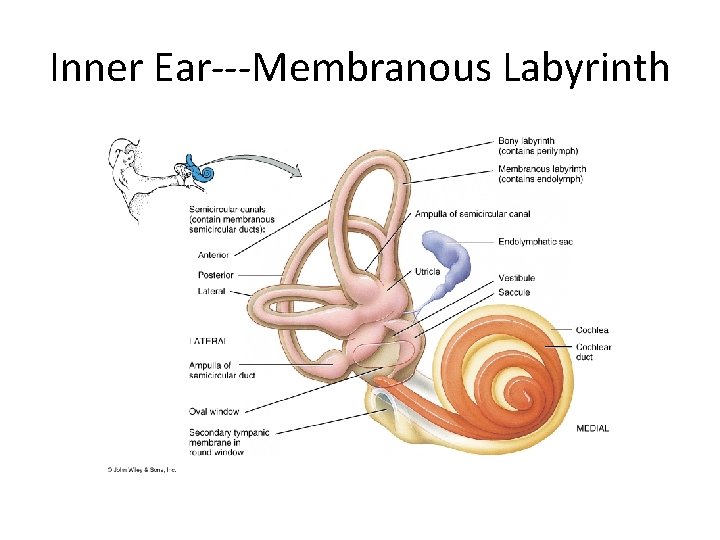
Inner Ear---Membranous Labyrinth

COCHLEA

• Fluid filled coiled tube • Its lumen is divided by Reissner`s and basilar membranes into : • Scala vestibula - Perilymph. • Scala media – Endolymph • Scala Tympani - Perilymph
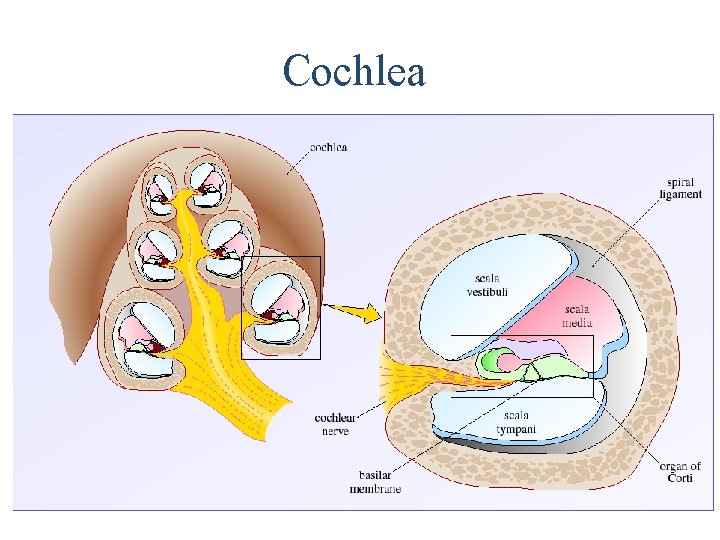
Cochlea
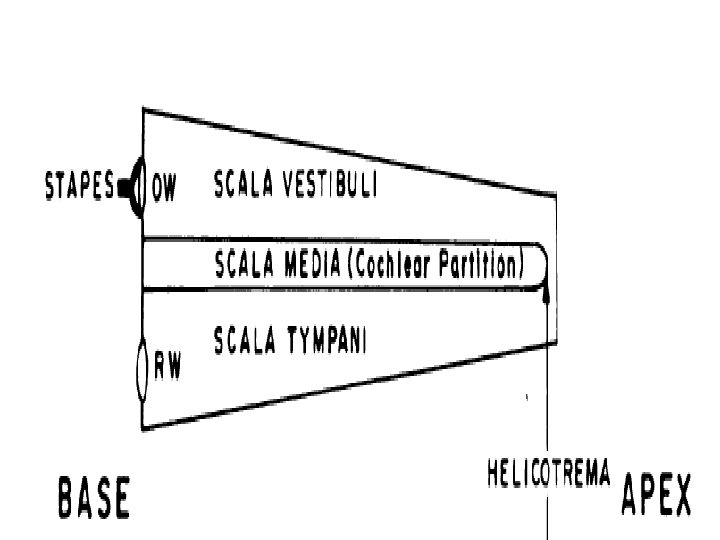

• Scala vestibuli-gap above Reissner`s membrane. • Base of cochlea-scala vestibuli ends at oval window-enclosed by foot plate of stapes. • Scala tympani and scala vestibuli communicate – helicotrema • Scala media –Reissner`s and basilar membrane. • Filled with endolymph-secreted – stria vascularis. • Scala tympani ends at round window. -enclosed by secondary tympanic membrane.

Healthy Cochlea The cilia ( sensory hairs) appear normal
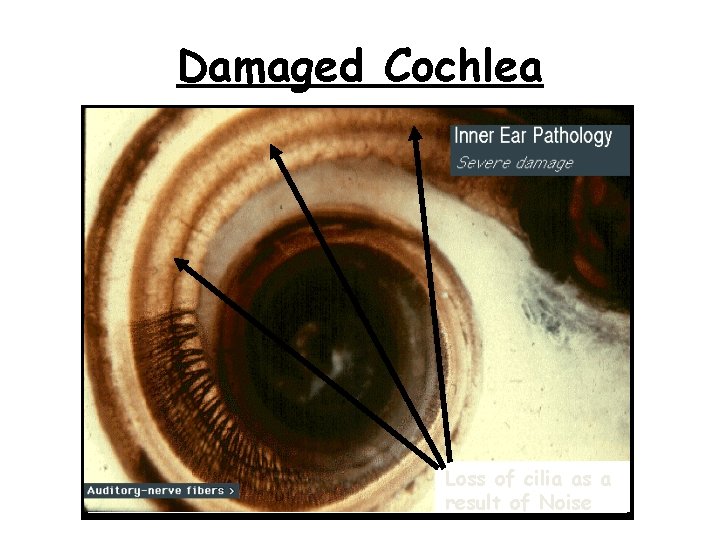
Damaged Cochlea Loss of cilia as a result of Noise

Structure concerned with hearing. It contain the auditory receptors – organ of corti.
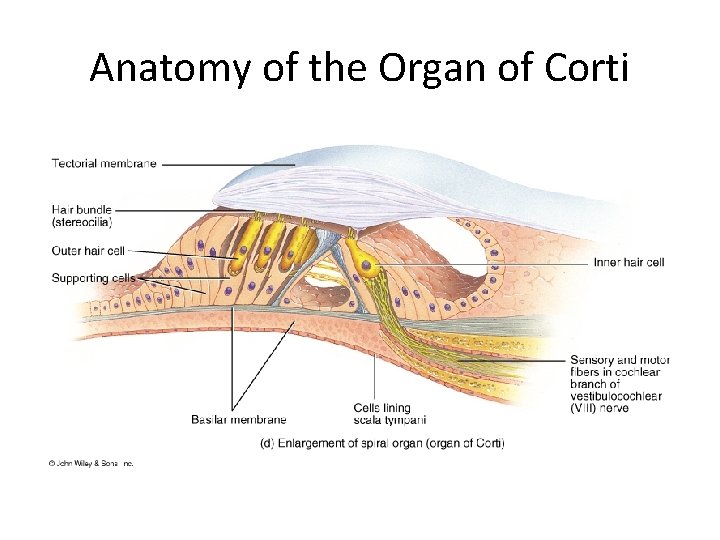
Anatomy of the Organ of Corti

• • Spiral organ Basilar membrane Receptors for hearing-hair cells Sound waves –reach organ of corti-transducer -converts mechanical form of energy into Aps in cochlear nerve.
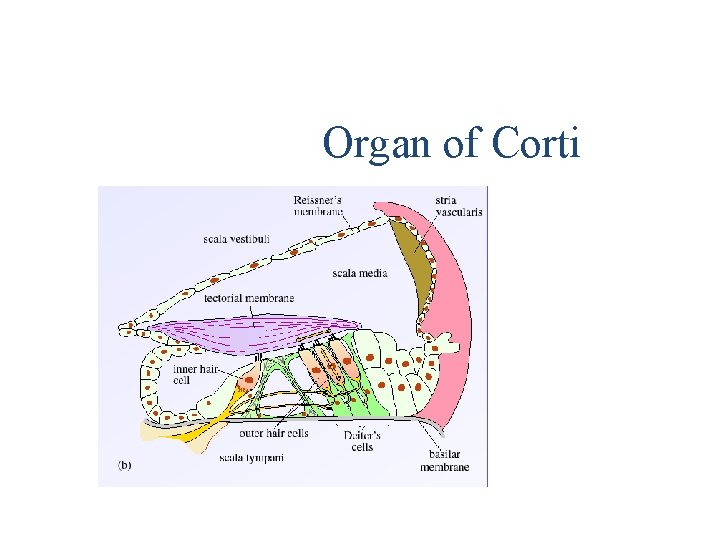
Organ of Corti

Hair cell • There are two different rows of hair cellsouter and inner hair cells. • Outer cell is longer than inner cell. • fine cilia at apical surface-basal end-synaptic connection. • Stereocilia-apical part of hair cell

• • Surrounded by supporting cells. Separated by rods of corti. Tunnel of corti 3500 inner hair cells and 20, 000 outer hair cells in each cochlea.

• Apical ends of hair cells-cilia-reticular lamina. • Tectorial membrane-covers the reticular lamina and processes of hair cells. • Cilia of outer hair cell –embedded in the tectorial membrane - inner one do not touch it.
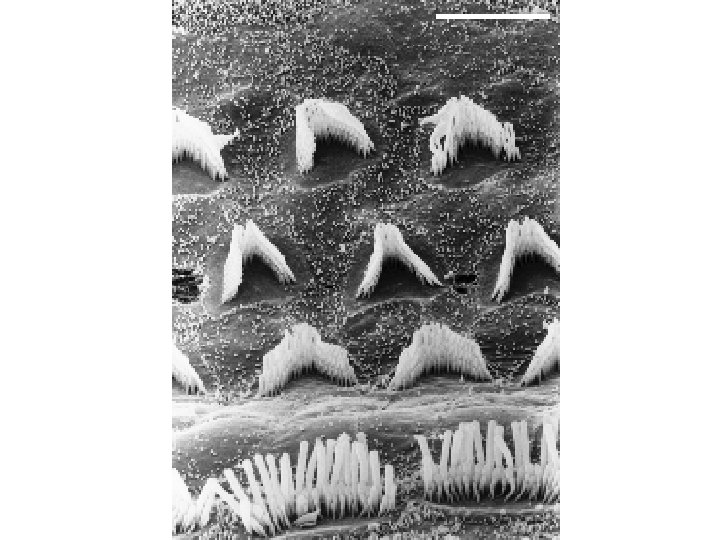

Ø Height of stereocilia-stria vascularis-tallest.
Functions of the hair cells: Act as a transducer and converts sound waves into electrical potentials Inner hair cells-primary sensory cells Responsible for the production of action potential in the auditory nerve. Outer hair cells: Improves the perceptibility of low intensity sounds. Discrimination of pitch/frequency and intensity/loudness of the sound is the most important function of the organ of corti

Mechanism of hearing

• • Sound waves compression and rarefaction –moleculesstrike tympanic membrane-sensation of sound. Properties Speed Frequency Pitch, wavelength and intensity.

Sound travels in waves as does light • 1. Pitch: determined by “frequency, ” the number of cycles per second of a sound wave, measured in hertz (Hz) • 2. Loudness: determined by “amplitude” (height) of the sound wave, measured in decibels (d. B)

• Audible range is 20 to 20, 000 Hz • Ear is more senstive-1000 -4000 Hz • Frequency of a sound vibration is pitch – higher frequency is higher pitch • Greater intensity (size) of vibration, the louder the sound measured in decibels (d. B)

Hearing threshold • 0 d. B at 1000 Hz-normal adult. • Human ear is sensitive to intensity about 60 d. B. • About 80 d. B-shouting • 140 d. B-pain and damage to ear.

Transmission of sound waves
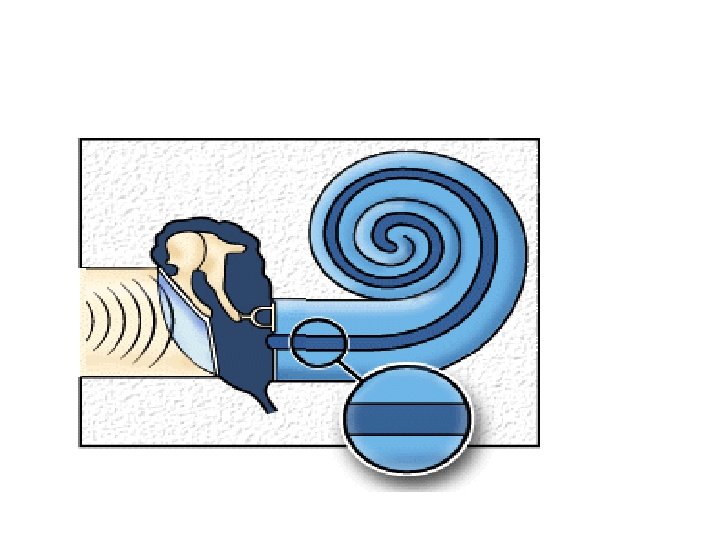

Transmission through outer and middle ear: • Sound waves-external canal-tympanic membrane-middle ear-chain of ossicular bones-amplified –foot plate of stapes • Ossicular conduction • Air conduction • Bone conduction

Transmission through inner ear: Travelling wave • Sound waves-foot plate of stapes-fluid of inner ear. • stapes move inward-Pressure-perilymph increases. • Depresses Reissners and basilar membrane • Scala tympani-outward movement of round window. • Stapes move outward- upward bulging of basilar membrane -inward movement of round window.

• Up and down movement of basilar membrane -moves organ of corti in same way.

Stimulation of hair cells • Basilar membrane move-sharp motion between tectorial and reticular membranebends the processes of hair cells • Leads to generation of AP in auditory (VIII) nerve.
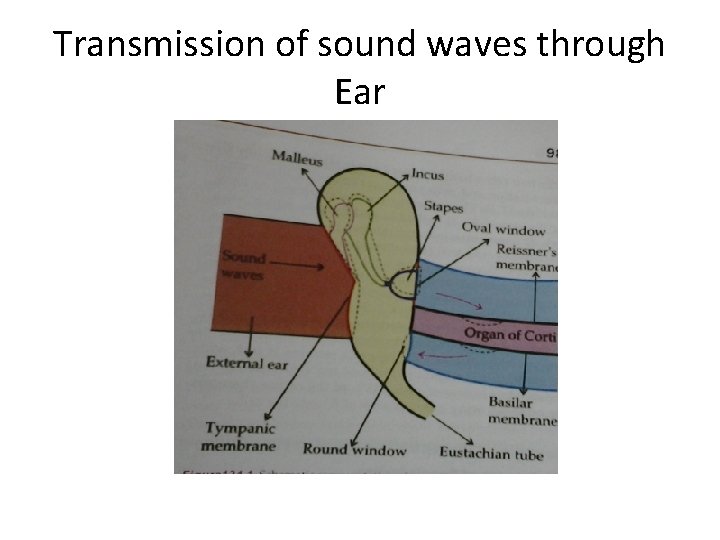
Transmission of sound waves through Ear
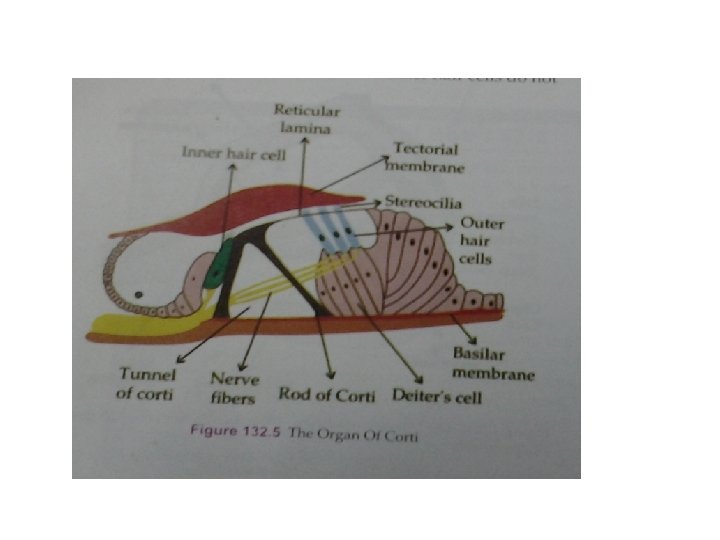
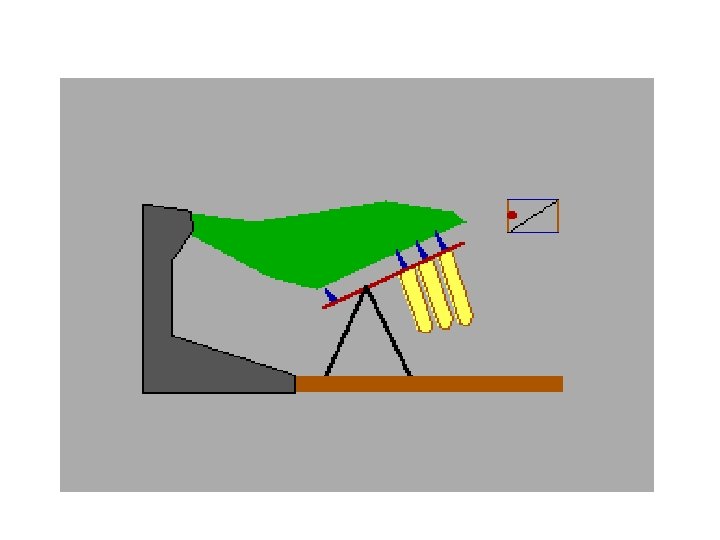

Excitation of hair cells • Stereocilia-embedded in tectorial membrane. travelling wave-vibration of basilar membrane -excitement of hair cells and generation of receptor potential.

Transduction of sound waves

Mechanical energy of sound-receptor potential-Aps-auditory pathway

Mechano-transduction process • Hair cell stereocilia are the site of mechanotransduction, i. e. , the translation of the sound vibration into a nervous (bio-electrical) message which the brain can interpret.

Resting state of hair cell • Resting membrane potential • Basolateral RMP-hair cell—-60 mv • Endocochlear potential
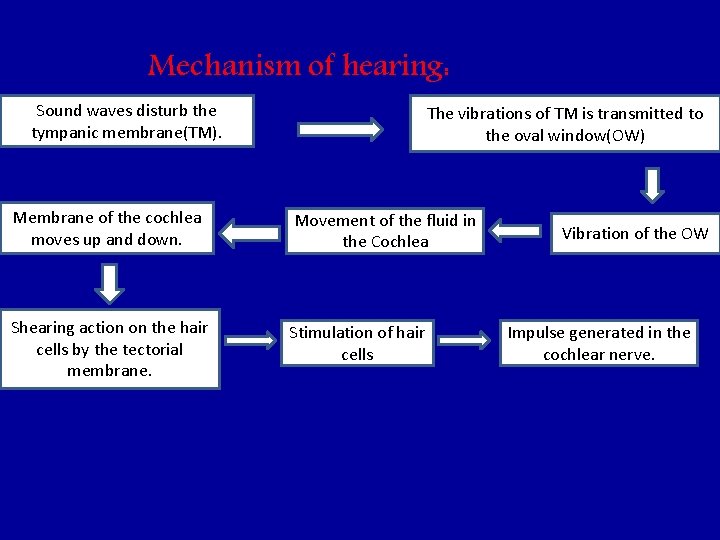
Mechanism of hearing: Sound waves disturb the tympanic membrane(TM). The vibrations of TM is transmitted to the oval window(OW) Membrane of the cochlea moves up and down. Movement of the fluid in the Cochlea Shearing action on the hair cells by the tectorial membrane. Stimulation of hair cells Vibration of the OW Impulse generated in the cochlear nerve.

Auditory pathway
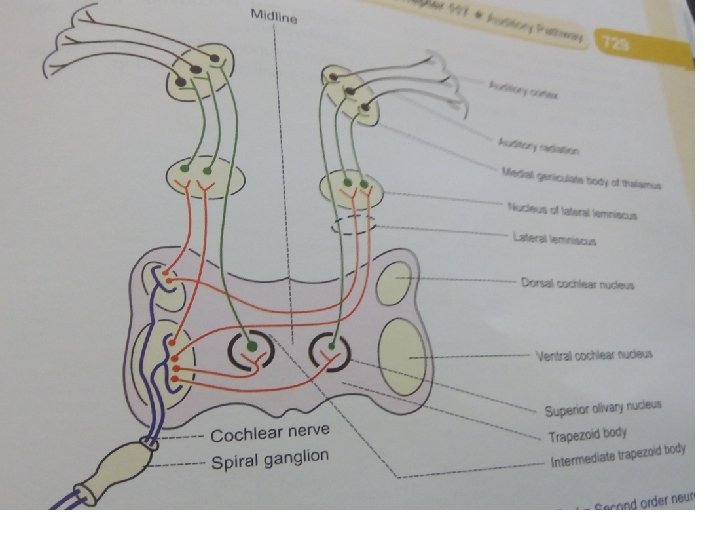

First order neurons • Cochlear division -8 th cranial nerve –projects to dorsal and ventral cochlear nuclei of medulla oblongata. Second order neurons • Starts from cochlear nuclei end in superior olivary nuclei and trapezoid body.

Third order neuron • Ascend via lateral lemniscus –inferior colliculi • From inferior colliculi many fibers relay in MGB –project to primary auditory cortex(area 41)

Auditory association area Area 22, 21 and 20 Area 22: superior temporal gyrus-processing of auditory signals Area 21 and 20 -middle and inferior temporal gyrus.

Theories Of Hearing

• Place theory • Different portions of organ of corti-respond to sounds of different frequency. • Travelling wave theory
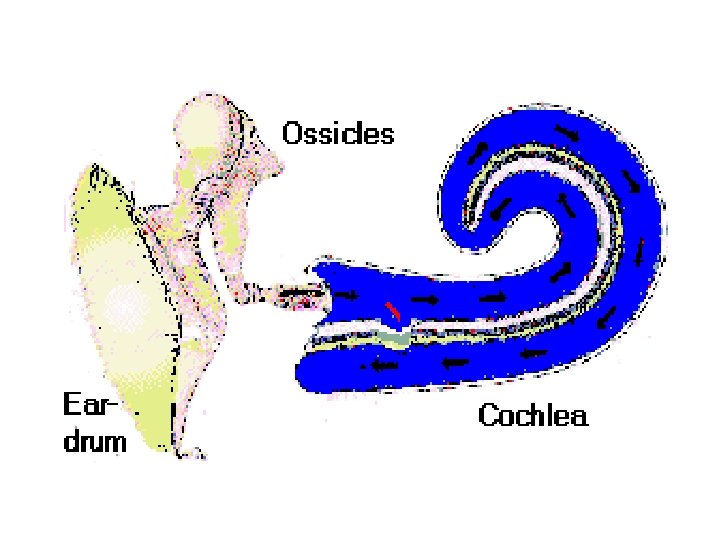

Localization of sound waves Ability to locate the direction of sound.

Deafness Types Ø Conductive Deafness ØNerve Deafness

• Nerve deafness – damage to organ of corti or anywhere along the auditory pathway. – Air conduction will be better than bone conduction.

• Conduction deafness Damage to the tympanic membrane /inflammation in the inner ear/ accumulation of wax in the auditory meatus Eustachian obstruction Bone conduction is better than air conduction. Nerve Disease of cochlea tumors

References • Textbook of medical physiology for dental students Prof G K Pal • Essentials of physiology for dental students ( 2 nd edition) K Sembulingam Prema Sembulingam AEJ 77
- Slides: 77