HealthRelated Quality of Life HRQOL Working Group Brad

Health-Related Quality of Life (HRQOL)

Working Group Brad Zebrack, Ph. D, MSW, MPH, Co-Chair • University of Michigan School of Social Work Lynne Wagner, Ph. D, Co-Chair • Northwestern University, Robert H. Lurie Comprehensive Cancer Center Barbara Jones, Ph. D, MSW • University of Texas School of Social Work Sheila Santacroce, Ph. D, RN, APRN • UNC School of Nursing and Lineberger Comprehensive Cancer Center Anne Kirchhoff, Ph. D, MPH • Huntsman Cancer Institute, University of Utah Nina Kadan-Lottick, MD, MSPH • Yale University School of Medicine Erin Kent, Ph. D • NCI Ashley Wilder Smith, Ph. D, MPH • NCI Kelly Trevino, Ph. D • Rowan University Sarah R. Arvey, Ph. D • LIVESTRONG Foundation

Objectives and Strategy • To identify gaps and recommendations via a systematic review of HRQOL literature (since 2000) • Define search terms ‘Adolescent, ’ ‘Young adult, ’ + (PHYSICAL, PSYCHOLOGICAL, SOCIAL, SPIRITUAL/EXISTENTIAL, MEASUREMENT, METHODOLOGICAL) – Google Scholar, Psych. Info, CINHAL • Define parameters for inclusion – Inclusion (Liberal): aged 15 -39 years; younger and older also included; patients, survivors of childhood cancer – Inclusion (Conservative): diagnosis at age 15 -39 years – Exclusion: sample includes subjects aged <12/13 years or >40 years
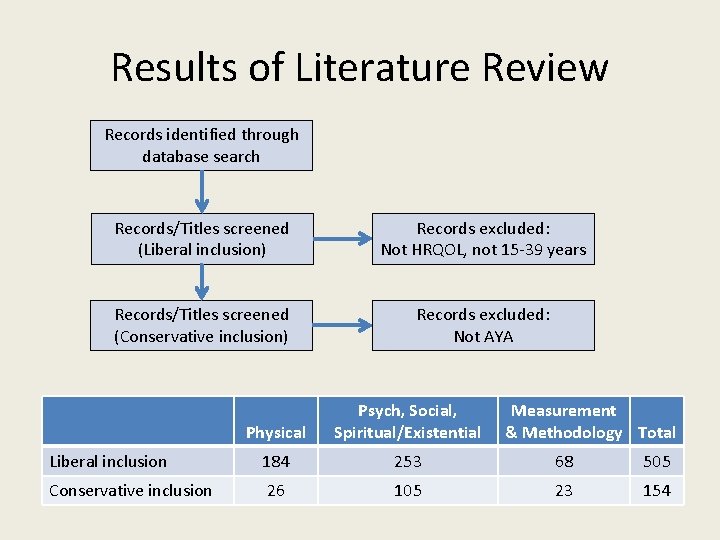
Results of Literature Review Records identified through database search Records/Titles screened (Liberal inclusion) Records excluded: Not HRQOL, not 15 -39 years Records/Titles screened (Conservative inclusion) Records excluded: Not AYA Physical Psych, Social, Spiritual/Existential Measurement & Methodology Total Liberal inclusion 184 253 68 505 Conservative inclusion 26 105 23 154
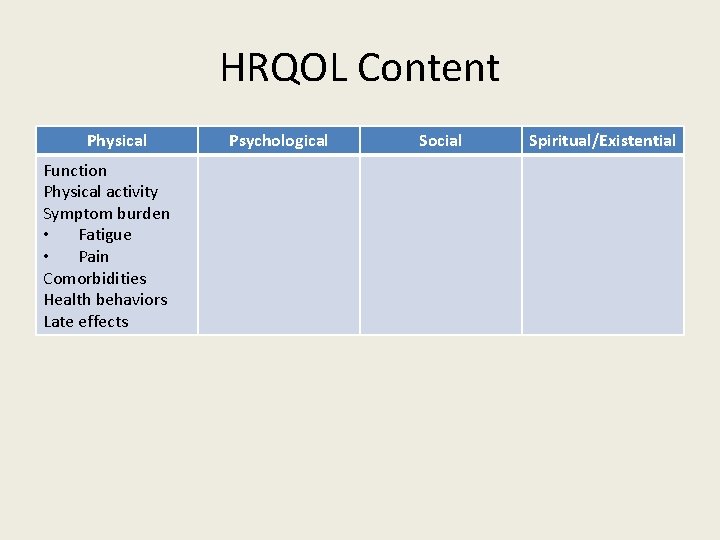

HRQOL Content Physical Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects Psychological Social Spiritual/Existential

Physical Well-Being • AYAs report: – Poorer physical functioning than healthy peers or siblings (CCSS) – Better physical functioning compared to older survivors • YAs reported greater symptom burden compared to older adults with the same cancer type – Breast: Moderate/severe drowsiness, hair loss, sx interference in relationships – Colorectal: Moderate/severe pain, fatigue, nausea, distress, drowsiness, shortness of breath, rash, and greater interference in general activity, mood, work, relationships and life enjoyment • Diagnosis, type of treatment, age at treatment completion and time since treatment completion not correlated with HRQL

Physical Well-Being • AYAs on treatment have greater symptom burden than those post-treatment, though fatigue persists for years • Fatigue and pain negatively affect HRQL • AYAs report higher rate of comorbidities (24%) than non-cancer controls (14%), including cardiovascular disease, hypertension, asthma, and disability

Physical Well-Being • AYAs report levels of physical activity comparable to controls, below recommended guidelines • High proportion of AYAs report being overweight (20%) or obese (15%) with higher rate of obesity among AYAs (31%) than controls (27%) • Rates of cigarette use among AYAs estimated at 16% and 26% – One study estimated use higher than non-cancer controls (18%) – One study found higher rate among age-related peers (25%) and lower rate among older cancer survivors (4%)
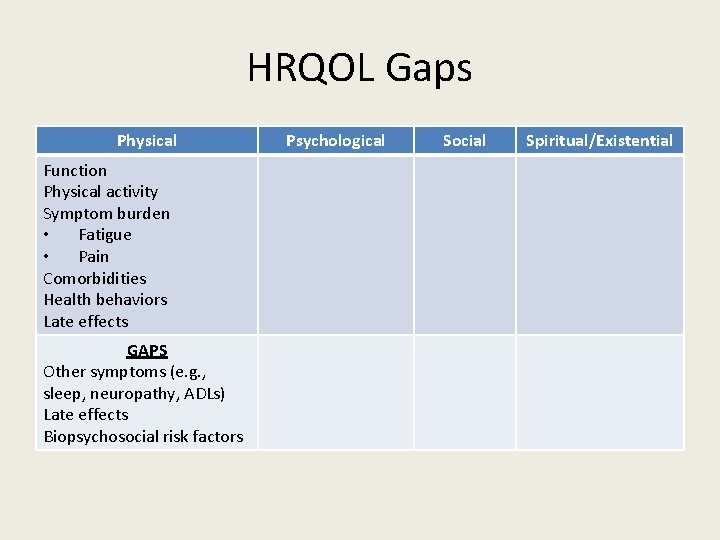
HRQOL Gaps Physical Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects GAPS Other symptoms (e. g. , sleep, neuropathy, ADLs) Late effects Biopsychosocial risk factors Psychological Social Spiritual/Existential
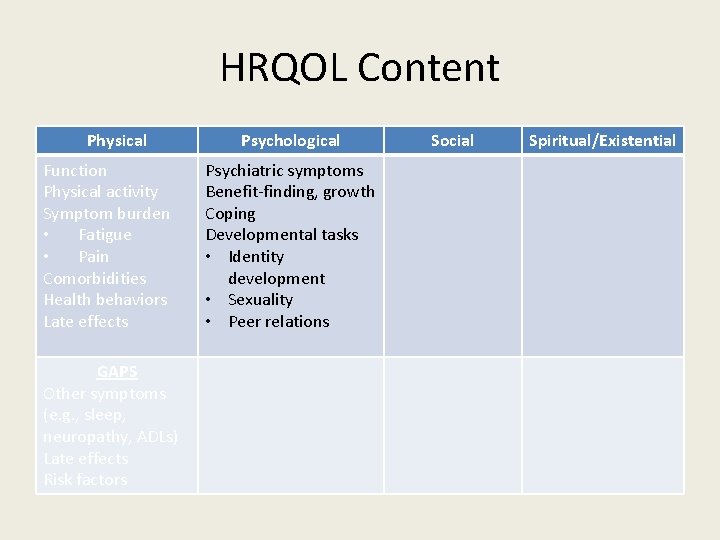
HRQOL Content Physical Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects GAPS Other symptoms (e. g. , sleep, neuropathy, ADLs) Late effects Risk factors Psychological Psychiatric symptoms Benefit-finding, growth Coping Developmental tasks • Identity development • Sexuality • Peer relations Social Spiritual/Existential

Psychological Well-Being • AYAs report higher prevalence of psychiatric symptoms (compared to normative data, noncancer controls, older cancer patients) – 6%-41% distress – Study findings mixed with regard to identifiable risk factors • age, time since diagnosis, education, employment status, relationship status, cancer type/severity, treatment type, symptom burden, needs of daily living, fertility concerns, information needs, insurance status, health system characteristics

Psychological Well-Being • Coping strategies employed – Acceptance, problem-solving – Support seeking – Emotional expression (through writing, blogs) – Seeking normalcy – Physical activity • Benefit finding, meaning-making associated with positive outcomes • Evidence of low levels of receipt/use of psychosocial care

Psychological Well-Being • Existing interventions: promote achievement of developmental tasks – Identity development, sexuality, peer relationships • Intervention modalities reported – Expressive therapy through arts, music, videomaking, writing, physical activity
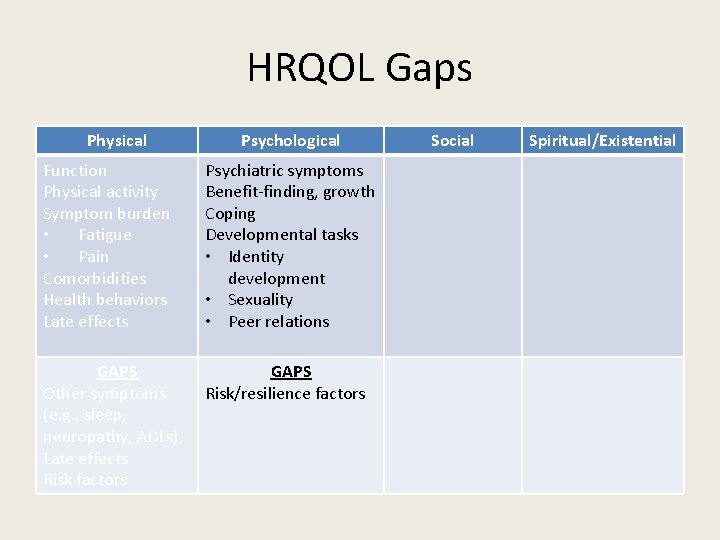
HRQOL Gaps Physical Psychological Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects Psychiatric symptoms Benefit-finding, growth Coping Developmental tasks • Identity development • Sexuality • Peer relations GAPS Other symptoms (e. g. , sleep, neuropathy, ADLs) Late effects Risk factors GAPS Risk/resilience factors Social Spiritual/Existential
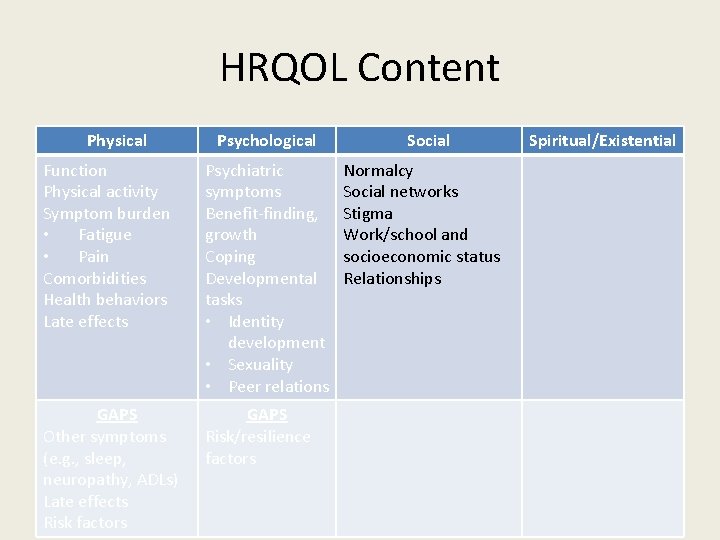
HRQOL Content Physical Psychological Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects Psychiatric symptoms Benefit-finding, growth Coping Developmental tasks • Identity development • Sexuality • Peer relations GAPS Other symptoms (e. g. , sleep, neuropathy, ADLs) Late effects Risk factors GAPS Risk/resilience factors Social Normalcy Social networks Stigma Work/school and socioeconomic status Relationships Spiritual/Existential

Social Well-Being • AYAs compare selves to peers – Fertility concerns compromise sense of normalcy • Social networks – Friends help – …but offer few opportunities to ask questions, receive information, process feelings, develop coping strategies

Social Well-Being • Stigma and unfair treatment – From peers, employers, government agencies • Challenges in returning to work/school • Low SES contributes to poor HRQOL • AYAs less likely to be married/partnered; more likely to divorce.
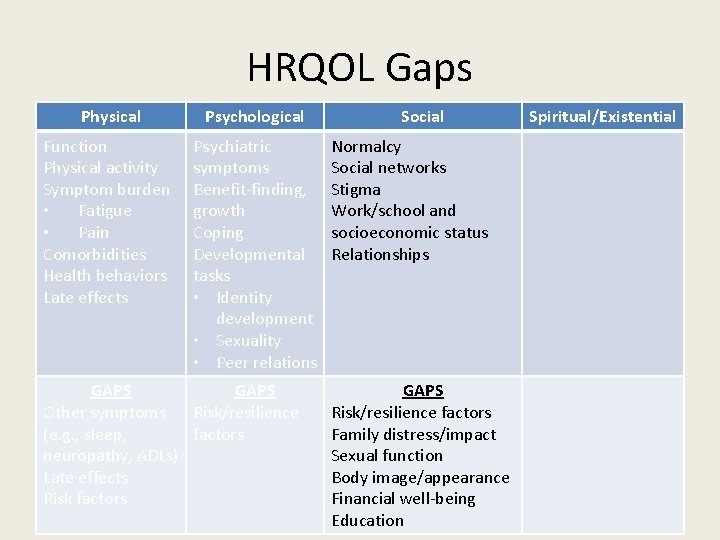
HRQOL Gaps Physical Psychological Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects Psychiatric symptoms Benefit-finding, growth Coping Developmental tasks • Identity development • Sexuality • Peer relations GAPS Other symptoms Risk/resilience (e. g. , sleep, factors neuropathy, ADLs) Late effects Risk factors Social Normalcy Social networks Stigma Work/school and socioeconomic status Relationships GAPS Risk/resilience factors Family distress/impact Sexual function Body image/appearance Financial well-being Education Spiritual/Existential
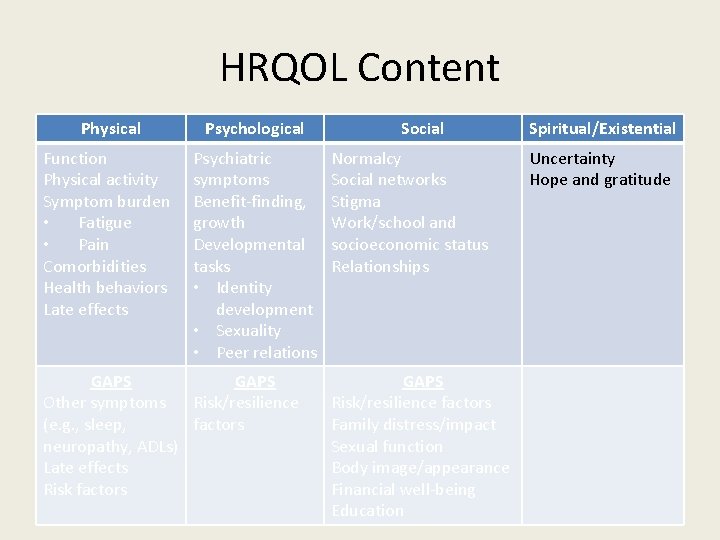
HRQOL Content Physical Psychological Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects Psychiatric symptoms Benefit-finding, growth Developmental tasks • Identity development • Sexuality • Peer relations GAPS Other symptoms Risk/resilience (e. g. , sleep, factors neuropathy, ADLs) Late effects Risk factors Social Normalcy Social networks Stigma Work/school and socioeconomic status Relationships GAPS Risk/resilience factors Family distress/impact Sexual function Body image/appearance Financial well-being Education Spiritual/Existential Uncertainty Hope and gratitude

Spiritual/Existential Well-Being • Coping with Uncertainty • Expressions of Hope and Gratitude
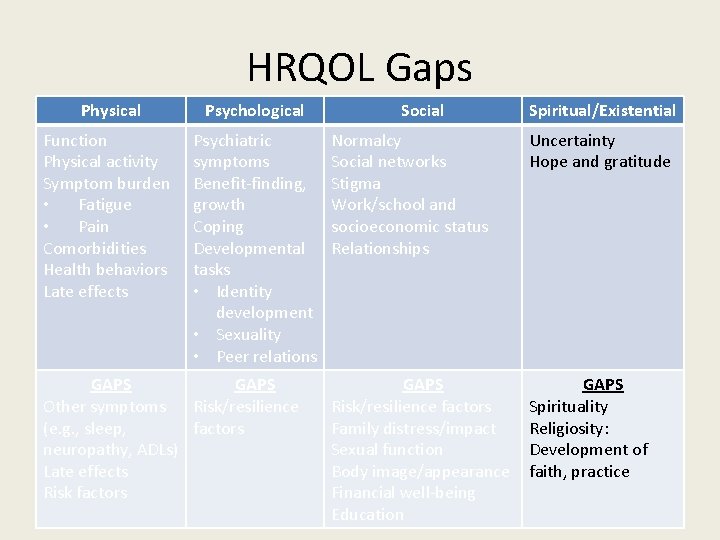
HRQOL Gaps Physical Psychological Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects Psychiatric symptoms Benefit-finding, growth Coping Developmental tasks • Identity development • Sexuality • Peer relations GAPS Other symptoms Risk/resilience (e. g. , sleep, factors neuropathy, ADLs) Late effects Risk factors Social Spiritual/Existential Normalcy Social networks Stigma Work/school and socioeconomic status Relationships Uncertainty Hope and gratitude GAPS Risk/resilience factors Family distress/impact Sexual function Body image/appearance Financial well-being Education GAPS Spirituality Religiosity: Development of faith, practice

Methodology and Measurement • Lower rates of AYA study participation and retention as compared to older survivors • Recruitment strategies vary in effectiveness (as per response rate) – Clinic-based recruitment, mailings, social media, population-based (SEER) – Online approaches and registries for study recruitment have mixed results re study accrual • Study retention increased with use of peer participants, collateral contacts, and parental awareness of participation

Methodology and Measurement • Peer outreach (peer-to-peer recruitment) increased retention in health care • Online technology effective for intervention delivery – Use of social media outlets (e. g. , Facebook) for collecting PROs • Evidence of higher response bias in reporting inflated levels of socio-emotional functioning

Methodology and Measurement • Few HRQOL-specific measures with reported psychometric data – Minneapolis-Manchester QOL – Peds. QOL – Cancer Needs Questionnaire • Few specific content areas covered by use of standardized measures – Fatigue, Pain, Sleep – Depression, Distress, Neurocognitive function
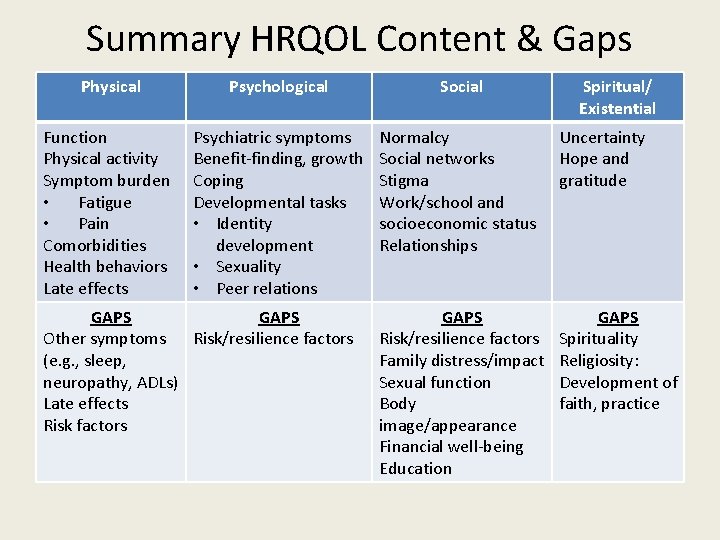
Summary HRQOL Content & Gaps Physical Psychological Social Function Physical activity Symptom burden • Fatigue • Pain Comorbidities Health behaviors Late effects Psychiatric symptoms Benefit-finding, growth Coping Developmental tasks • Identity development • Sexuality • Peer relations Normalcy Social networks Stigma Work/school and socioeconomic status Relationships Uncertainty Hope and gratitude GAPS Risk/resilience factors Family distress/impact Sexual function Body image/appearance Financial well-being Education GAPS Spirituality Religiosity: Development of faith, practice GAPS Other symptoms Risk/resilience factors (e. g. , sleep, neuropathy, ADLs) Late effects Risk factors Spiritual/ Existential

Recommendations • Rigorous designs – Comparison groups, disease- and treatment-specific sub-groups – Longitudinal studies w/repeated measures -- Important given relatively rapid psychosocial & cognitive development – Comparative effectiveness evaluations of non-traditional interventions (e. g. , videogames, movies, creative arts, social networking) compared to conventional interventions (e. g. , psychotherapy, support groups) • Instrumentation – Deeper evaluation of function, performance, coverage of content, validity, reliability – Use of standardized measures and – Biomarkers with established AYA reference ranges or community norms • Health disparities – Identify disparities in symptom burden (physical and psychosocial), and access to supportive care services • By AYA characteristics: race/ethnicity, age sub-group, SES, language

Recommendations • Intervention studies – Reduce symptom burden – Promote positive adaptation and coping – Target self-efficacy/self-management (symptoms, surveillance of late effects & 2 nd malignancies) – Involve friends, family, peers – Better understanding of role and potential of social networking/social media
- Slides: 27