Healthier Here The Accountable Community of Health of

Healthier. Here The Accountable Community of Health of King County Partnering Organization Summit February 15, 2018

Today’s Agenda • Welcome and Updates • Overview of Healthier. Here’s portfolio of projects • King County Medicaid Population and Gap to Goal • A framework for defining roles: Partnering organizations and Healthier. Here • Partnering organization needs and ideas • Wrap Up & Next steps 2

Updates from Healthier. Here 3

Project Application & Implementation • Healthier. Here receives score of 100% on Project Plan and earns $23 M for the King County region • Transformation Committee will oversee project portfolio implementation planning • Project Workgroups will be convened to operationalize project proposals • HIE/HIT and other Domain 1 strategy development beginning

Financial Executor (FE)Update • Healthier. Here submitted an updated provider list to the FE on February 13 th • The FE will match Employee Identification Numbers (EINs) and organization names with IRS records; • Positive match: providers will receive an email from the FE to complete registration in portal (WA_FE_Financial. Services@pcgus. com) • Negative match: the FE will contact Healthier. Here who will work with providers to fix errors and create a match • The FE will host a training for providers on the registration process in March (date TBD) • Provider organizations who haven’t done so already should complete the Healthier. Here Provider Survey link: https: //www. surveymonkey. com/r/King. Provider. MTD

Provider Agreements • Healthier. Here is working on financial models for distribution of incentive funding. • A final distribution recommendation will be brought to the Governing Board for approval • Agreements finalized in May (earliest): 1. Partnering Provider Agreement – standard statewide agreement to sign when registering with the FE. Represents the basic agreement/requirements to receive payment from ACHs. 2. Healthier. Here will add an Addendum to the standard agreement to define expectations for 2018 3. Healthier. Here will additional Addenda to define expectations for 2019 and beyond

Healthier. Here Transformation Portfolio 7
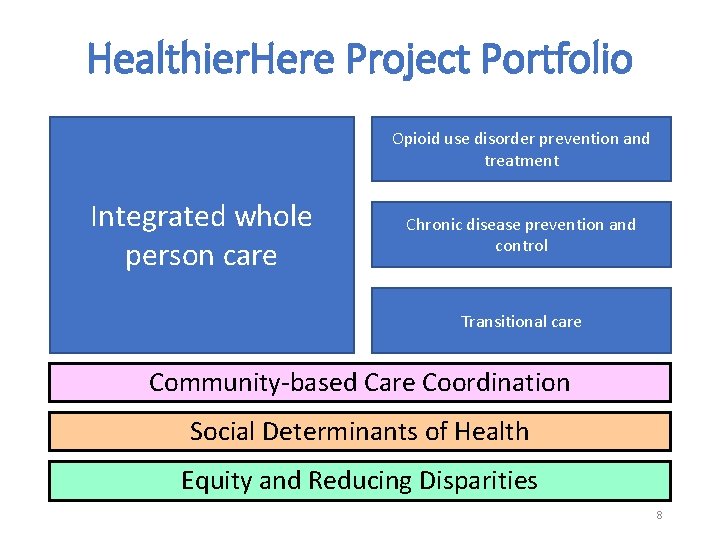
Healthier. Here Project Portfolio Opioid use disorder prevention and treatment Integrated whole person care Chronic disease prevention and control Transitional care Community-based Care Coordination Social Determinants of Health Equity and Reducing Disparities 8
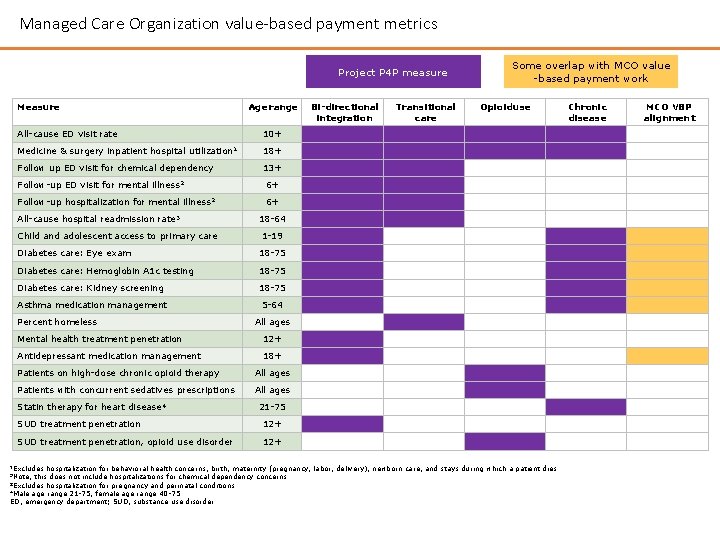
Managed Care Organization value-based payment metrics Project P 4 P measure Measure Age range All-cause ED visit rate utilization 1 Follow up ED visit for chemical dependency Follow-up ED visit for mental illness 2 Follow-up hospitalization for mental All-cause hospital readmission illness 2 rate 3 Child and adolescent access to primary care Opioiduse 18+ 13+ 6+ 6+ 18 -64 1 -19 Diabetes care: Eye exam 18 -75 Diabetes care: Hemoglobin A 1 c testing 18 -75 Diabetes care: Kidney screening 18 -75 Asthma medication management 5 -64 Percent homeless All ages Mental health treatment penetration 12+ Antidepressant medication management 18+ Patients on high-dose chronic opioid therapy All ages Patients with concurrent sedatives prescriptions All ages disease 4 21 -75 SUD treatment penetration 12+ SUD treatment penetration, opioid use disorder 12+ 1 Excludes Transitional care 10+ Medicine & surgery inpatient hospital Statin therapy for heart Bi-directional integration Some overlap with MCO value -based payment work hospitalization for behavioral health concerns, birth, maternity (pregnancy, labor, delivery), newborn care, and stays during which a patient dies this does not include hospitalizations for chemical dependency concerns 3 Excludes hospitalization for pregnancy and perinatal conditions 4 Male age range 21 -75, female age range 40 -75 ED, emergency department; SUD, substance use disorder 2 Note, Chronic disease MCO VBP alignment
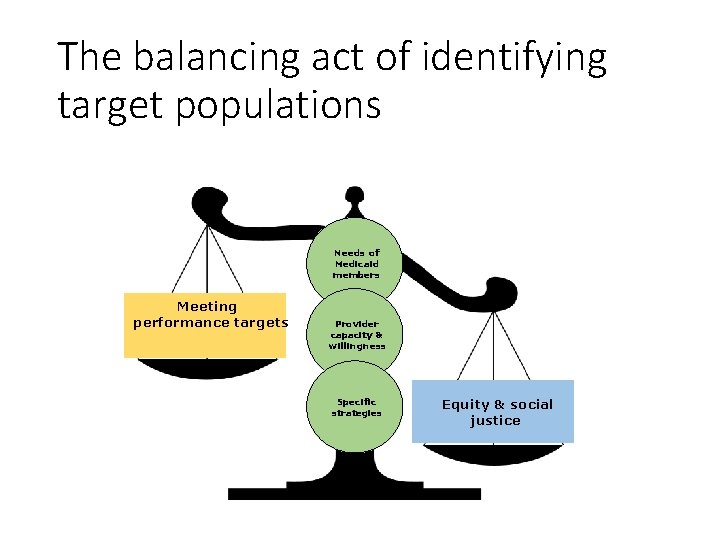
The balancing act of identifying target populations Needs of Medicaid members Meeting performance targets Provider capacity & willingness Specific strategies Equity & social justice

Transitioning to value based care Remember what this is about • Evidence based and best practices • Value base payment arrangements Population health management Providing integrated, teambased, whole person care Linking social services (SDOH) to the health care delivery system

Bi-directional Integration of Physical and Behavioral Health Project Objectives • Improve access to behavioral health through enhanced screening, identification, and treatment of behavioral health disorders in primary care settings. • Improve access to physical health services for individuals with chronic behavioral health conditions through increased screening, identification, and treatment of physical health disorders in behavioral health care settings. • Improve active coordination of care among medical and behavioral health providers and address barriers to care. • Align new bi-directional integration with successful existing community efforts, including addressing social determinants of health.
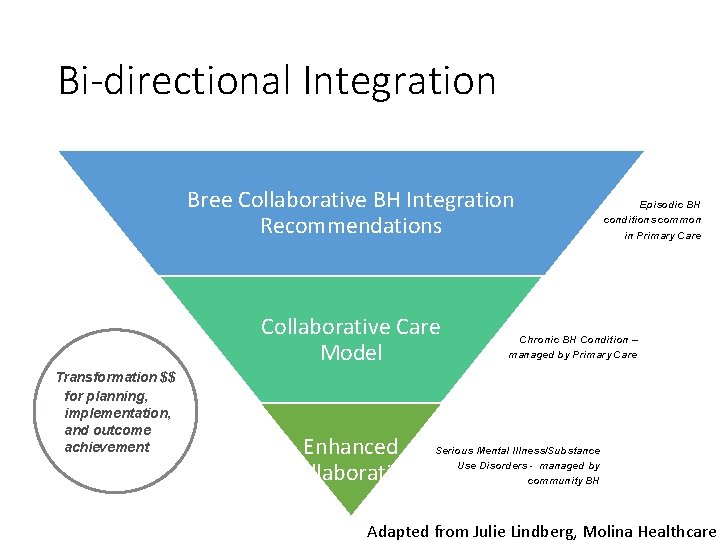
Bi-directional Integration Bree Collaborative BH Integration Recommendations Collaborative Care Model Transformation $$ for planning, implementation, and outcome achievement Enhanced Collaboration Episodic BH conditions common in Primary Care Chronic BH Condition – managed by Primary Care Serious Mental Illness/Substance Use Disorders - managed by community BH Adapted from Julie Lindberg, Molina Healthcare

Healthier. Here will focus on • Strengthening provider's ability and capacity to provide client-centered, whole-person care through training, technology, and workforce capacity leading to longterm transformation. • Building on existing efforts, rather than forcing providers to adopt one particular model. • Addressing unmet need in treating identified mental health and SUD through increased screening and access to care. • Supporting the transition to fully integrated managed care, and work with MCO partners to align VBP with models and outcomes associated with bi-directional care.

Transitional Care Project Objective • Improve transitional care services to reduce avoidable hospitalization and ensure beneficiaries are getting the right care in the right place. • Individuals transitioning from inpatient hospital settings • Individuals transitioning from inpatient psychiatric facilities • Individuals transitioning from jail

Healthier. Here will focus on • Strengthening provider's ability and capacity to provide the APIC, Coleman, and Peer Bridger models of care transition across all three target populations • Investing in evidence-based transitional care approaches to improve quality of care and building strong linkages to CBOs resulting in more stable transitions to prevent readmission. • Investing in training, technology, and workforce capacity. • Decreasing readmissions and incarcerations to resulting in cost savings • Increasing access to multidisciplinary care teams and community-based care coordination upon transition.

Addressing the Opioid Crisis Project Objective • Support the achievement of the state’s goals to reduce opioid-related morbidity and mortality through strategies that target prevention, treatment, and recovery supports.

Healthier. Here will focus on 1. Improved adherence to opioid-prescribing guidelines, including provision of non-opioid pain management resources and supports for providers 2. Expansion of low barrier access to Medication Assisted Treatment (MAT) 3. Enhanced collaboration between prescribers and community based recovery supports 4. Distribution of Naloxone Kits to prevent overdose

Chronic Disease Prevention and Control Project Objective Integrate health system and community approaches to improve chronic disease management and control. • Children and adults with chronic respiratory diseases (including asthma) • Adults with chronic cardiovascular diseases (including diabetes)

Healthier. Here will focus on • Use registries to identify and track 2 populations of Medicaid clients with chronic disease • Educate, provide care to, follow and track based on risk and family need • Redefine integrated care teams to include social workers, pharmacists, dieticians, and community health workers to strengthen linkages to social services

Community Based Care Coordination and Addressing the Social Determinants of Health • Rationalize and build off of current care coordination activities/infrastructure • Invest in mechanisms for shared care planning • Support strong two-way partnerships between health care delivery system and social service organizations • Ensure two-way referral and tracking mechanisms • Support sharing of information across provider types
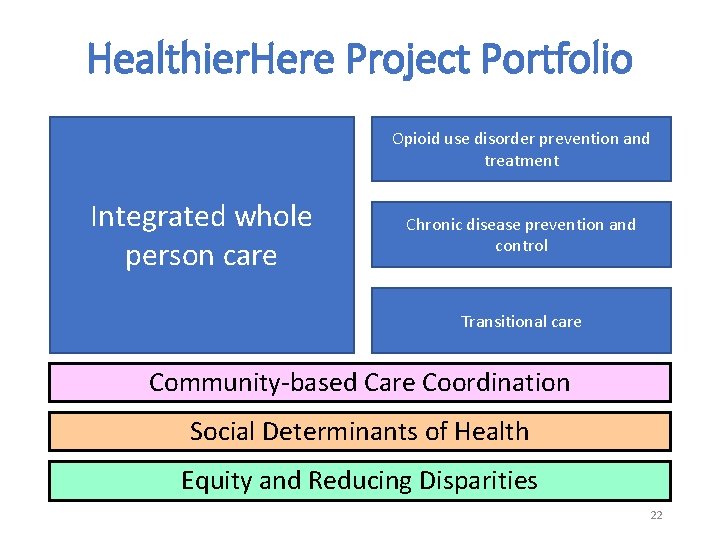
Healthier. Here Project Portfolio Opioid use disorder prevention and treatment Integrated whole person care Chronic disease prevention and control Transitional care Community-based Care Coordination Social Determinants of Health Equity and Reducing Disparities 22
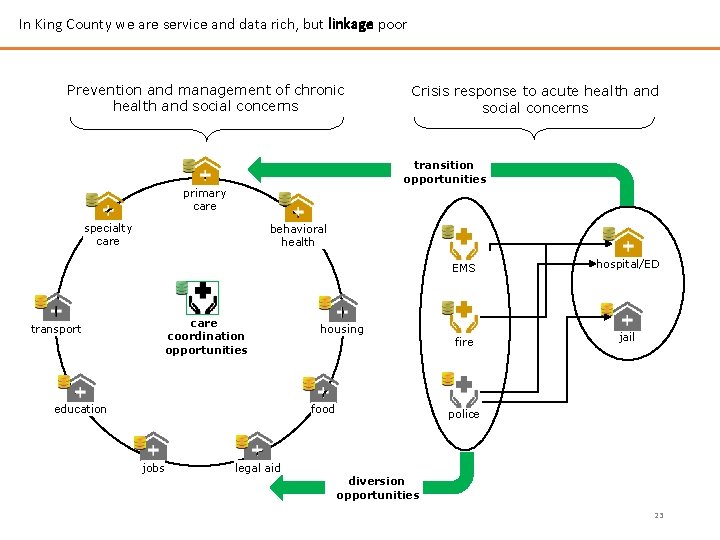
In King County we are service and data rich, but linkage poor Prevention and management of chronic health and social concerns Crisis response to acute health and social concerns transition opportunities primary care specialty care behavioral health care coordination opportunities transport education housing food jobs EMS hospital/ED fire jail police legal aid diversion opportunities 23

Key Elements of VBP Capabilities Infrastructure components required to manage VBP contracts successfully Governance and Organization Provider Engagemen t • Leadership buy-in and organizational vision • Staff education • Provider network identification and engagement • Workforce development • Referral management • Effective practice management system • Engagement with and links to nonphysician staff/ organizations • Revenue cycle management • Performance management • Co-location (if applicable) • Legal evaluation, contract management • Performance feedback and management • Change management 9 Care Coordination / Management • Single point of assessment • Coordination of care/services across specialties and sites of care Technology and Analytics • Data aggregation • Data exchange and interoperability • Development of comprehensive care plans • Evidence-based population health management systems • Patient engagement • Performance monitoring • Evidence-based case management Links to Social Determinants of Health • Patient social needs assessment • Knowledge of/ access to services and organizations • Integration into clinical and care management protocols • Development of “value case” for addressing social needs • Social services referral staff/ programs
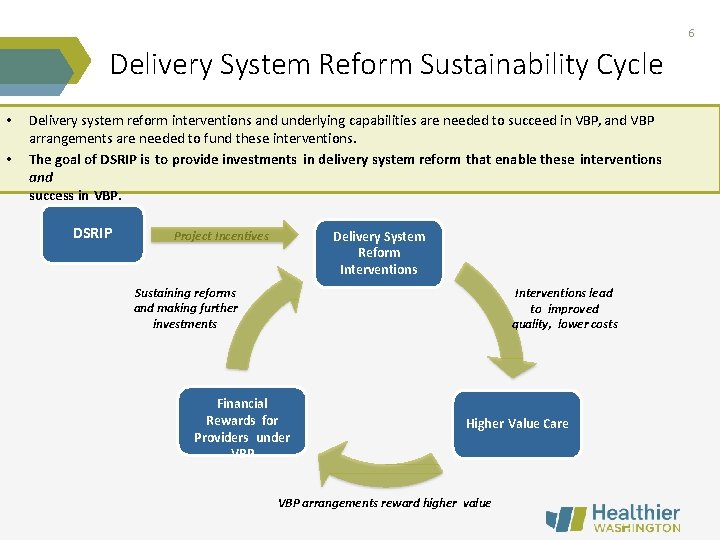
6 Delivery System Reform Sustainability Cycle • • Delivery system reform interventions and underlying capabilities are needed to succeed in VBP, and VBP arrangements are needed to fund these interventions. The goal of DSRIP is to provide investments in delivery system reform that enable these interventions and success in VBP. DSRIP Delivery System Reform Interventions Project Incentives Sustaining reforms and making further investments Interventions lead to improved quality, lower costs Financial Rewards for Providers under VBP Higher Value Care VBP arrangements reward higher value
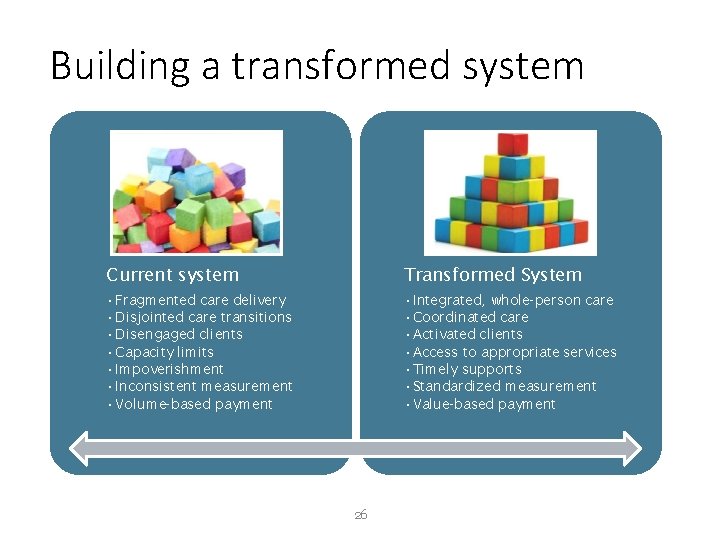
Building a transformed system Current system Transformed System • Fragmented care delivery • Disjointed care transitions • Disengaged clients • Capacity limits • Impoverishment • Inconsistent measurement • Volume-based payment • Integrated, whole-person care • Coordinated care • Activated clients • Access to appropriate services • Timely supports • Standardized measurement • Value-based payment 26


Data: Medicaid members and metrics, including “gap to goal” 28
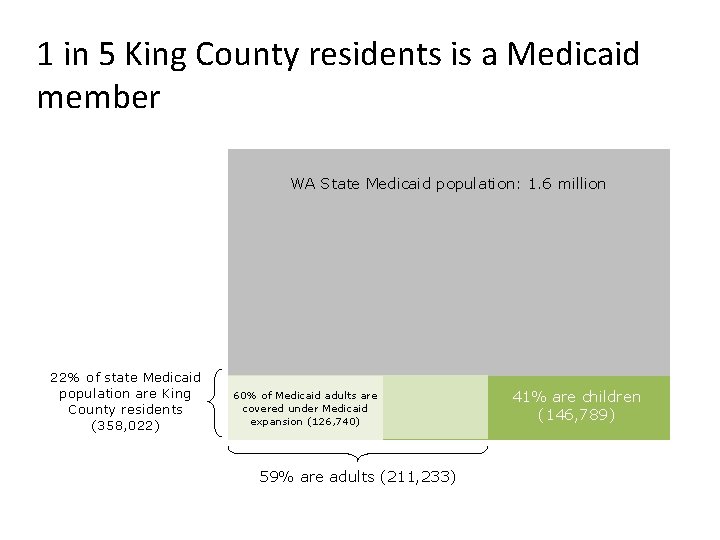
1 in 5 King County residents is a Medicaid member WA State Medicaid population: 1. 6 million 22% of state Medicaid population are King County residents (358, 022) 60% of Medicaid adults are covered under Medicaid expansion (126, 740) 59% are adults (211, 233) 41% are children (146, 789)

Where do Medicaid members live? ZIP 98001 98002 98003 98023 98030 98031 98032 98042 98058 98092 98108 98118 98133 98168 98178 98188 98198 Number of enrollees ranges from: 9, 067 Area Auburn Federal Way Kent Covington East of Renton East of Auburn Georgetown/ Beacon Hill Rainier Valley Shoreline Sea. Tac/Tukwila Renton Sea. Tac/Tukwila Des Moines 19, 361 Healthier. Here Partnering Organization Summit | 30
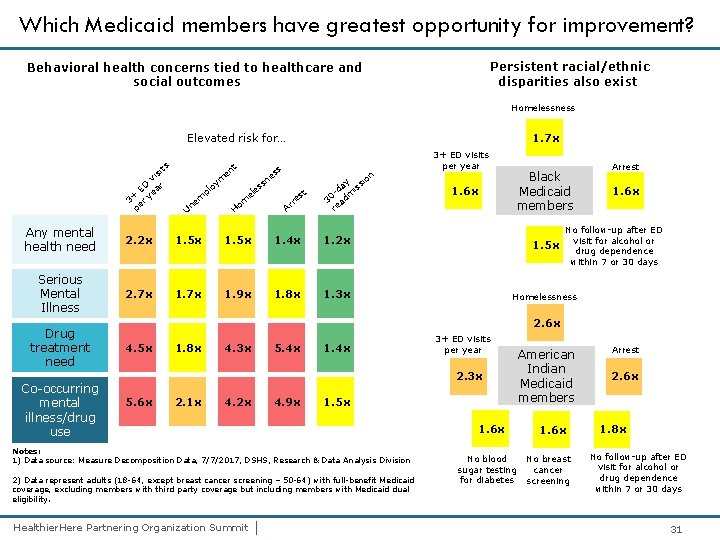
Which Medicaid members have greatest opportunity for improvement? Persistent racial/ethnic disparities also exist Behavioral health concerns tied to healthcare and social outcomes Homelessness 1. 7 x Elevated risk for… ts si vi ED ear + 3 er y p nt o pl U m ne ss e ym n io e sn es el m o H t es r Ar ay ss -d mi 0 3 ad re Any mental health need 2. 2 x 1. 5 x 1. 4 x 1. 2 x Serious Mental Illness 2. 7 x 1. 9 x 1. 8 x 1. 3 x Drug treatment need Co-occurring mental illness/drug use 3+ ED visits per year Black Medicaid members 1. 6 x 1. 5 x Arrest 1. 6 x No follow-up after ED visit for alcohol or drug dependence within 7 or 30 days Homelessness 2. 6 x 4. 5 x 1. 8 x 4. 3 x 5. 4 x 1. 4 x 3+ ED visits per year 2. 3 x 5. 6 x 2. 1 x 4. 2 x 4. 9 x 1. 5 x 1. 6 x Notes: 1) Data source: Measure Decomposition Data, 7/7/2017, DSHS, Research & Data Analysis Division 2) Data represent adults (18 -64, except breast cancer screening – 50 -64) with full-benefit Medicaid coverage, excluding members with third party coverage but including members with Medicaid dual eligibility. Healthier. Here Partnering Organization Summit | No blood sugar testing for diabetes American Indian Medicaid members 1. 6 x No breast cancer screening Arrest 2. 6 x 1. 8 x No follow-up after ED visit for alcohol or drug dependence within 7 or 30 days 31
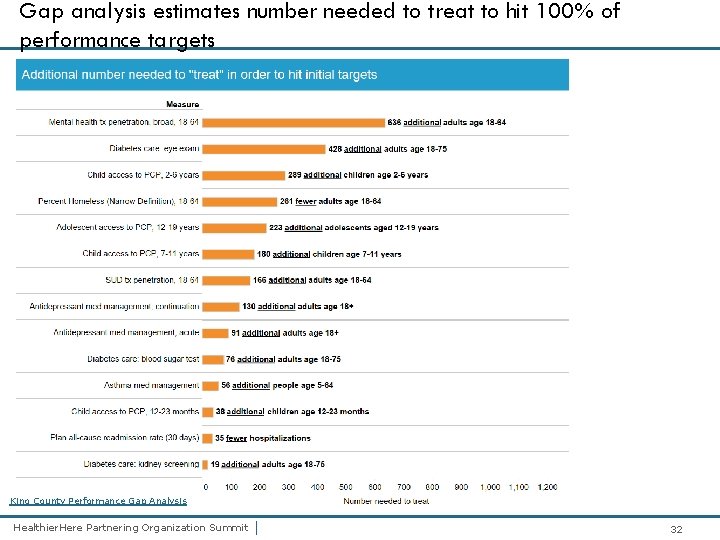
Gap analysis estimates number needed to treat to hit 100% of performance targets King County Performance Gap Analysis Healthier. Here Partnering Organization Summit | 32
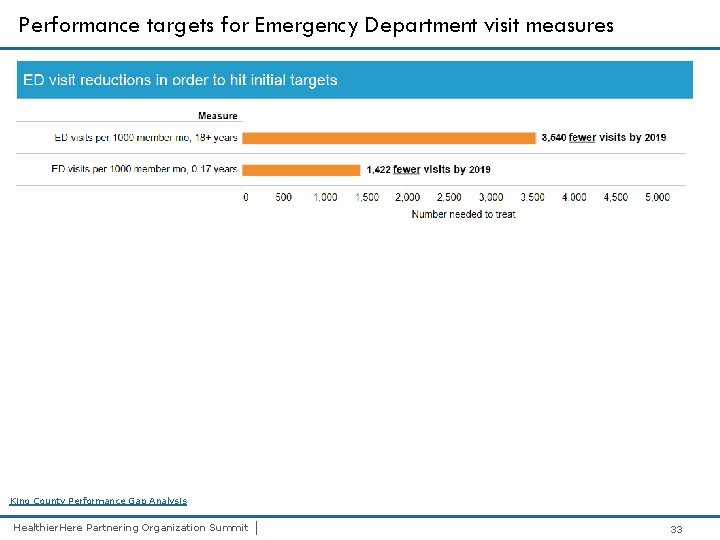
Performance targets for Emergency Department visit measures King County Performance Gap Analysis Healthier. Here Partnering Organization Summit | 33

Framework for understanding providers’ role and Healthier. Here’s role 34
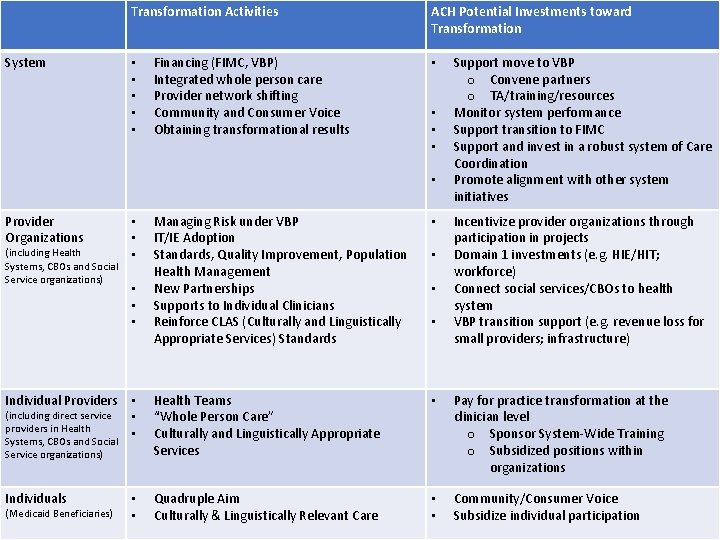
Transformation Activities System • • • Financing (FIMC, VBP) Integrated whole person care Provider network shifting Community and Consumer Voice Obtaining transformational results ACH Potential Investments toward Transformation • • • Provider Organizations Support move to VBP o Convene partners o TA/training/resources Monitor system performance Support transition to FIMC Support and invest in a robust system of Care Coordination Promote alignment with other system initiatives Managing Risk under VBP IT/IE Adoption Standards, Quality Improvement, Population Health Management New Partnerships Supports to Individual Clinicians Reinforce CLAS (Culturally and Linguistically Appropriate Services) Standards • Individual Providers • (including direct service • providers in Health • Systems, CBOs and Social Health Teams “Whole Person Care” Culturally and Linguistically Appropriate Services • Pay for practice transformation at the clinician level o Sponsor System-Wide Training o Subsidized positions within organizations Individuals Quadruple Aim Culturally & Linguistically Relevant Care • • Community/Consumer Voice Subsidize individual participation (including Health Systems, CBOs and Social Service organizations) • • • Service organizations) (Medicaid Beneficiaries) • • • Incentivize provider organizations through participation in projects Domain 1 investments (e. g. HIE/HIT; workforce) Connect social services/CBOs to health system VBP transition support (e. g. revenue loss for small providers; infrastructure)

Core Leave Behinds Collaboration between the health care system and social services, evidenced by an inter-connected HIT/HIE system connecting providers from both systems and payment models that incorporate social service providers. Access to person-centered, multi-disciplinary, culturally competent care teams -- inclusive of social services -- in health homes for everyone, regardless of where a person enters the system. An infrastructure that provides an effective mechanism for meaningful community and consumer involvement and voice in the continuous improvement of the delivery system.
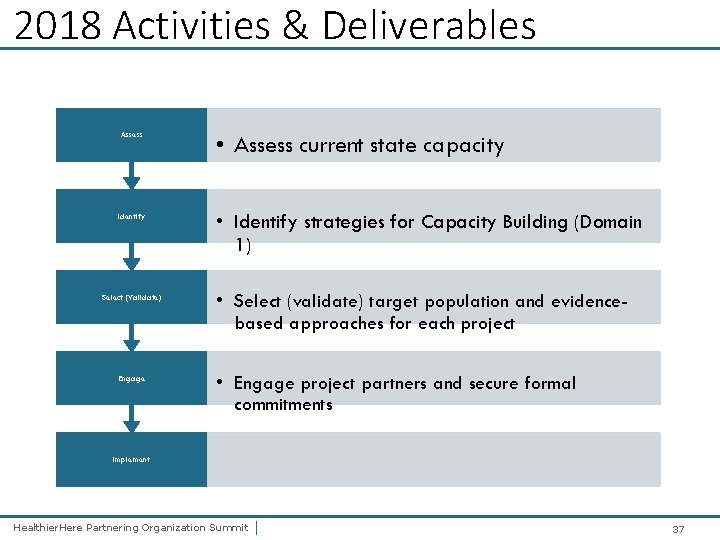
2018 Activities & Deliverables Assess Identify Select (Validate) Engage • Assess current state capacity • Identify strategies for Capacity Building (Domain 1) • Select (validate) target population and evidencebased approaches for each project • Engage project partners and secure formal commitments Implement Healthier. Here Partnering Organization Summit | 37

Stages of project implementation Healthier. Here Partnering Organization Summit |
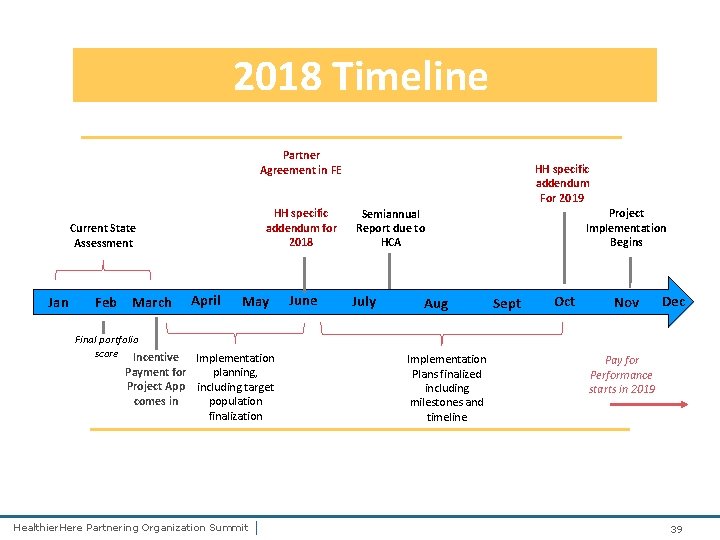
2018 Timeline Partner Agreement in FE HH specific addendum for 2018 Current State Assessment Jan Feb March April May Final portfolio score Incentive Implementation Payment for planning, Project App including target comes in population finalization Healthier. Here Partnering Organization Summit | June HH specific addendum For 2019 Project Implementation Begins Semiannual Report due to HCA July Aug Implementation Plans finalized including milestones and timeline Sept Oct Nov Dec Pay for Performance starts in 2019 39

Small Group Discussion: organizational needs and ideas 40

Small group discussion Divide into groups by provider type Hospital/Health systems Behavioral Health Community Health Centers Community-based Organizations HH staff will moderate Decide who will report out and who will scribe Discuss questions (next slides) Use flipcharts to capture your key points Be ready to report out Webinar participants will “chat” in an online small group Healthier. Here Partnering Organization Summit | 41
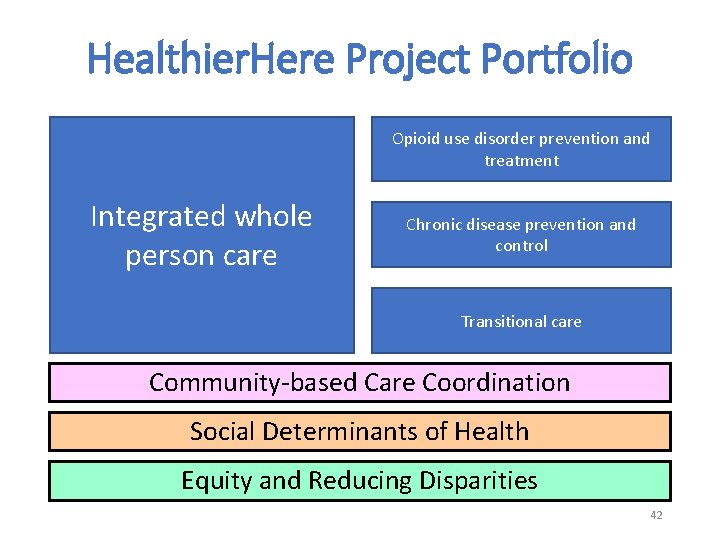
Healthier. Here Project Portfolio Opioid use disorder prevention and treatment Integrated whole person care Chronic disease prevention and control Transitional care Community-based Care Coordination Social Determinants of Health Equity and Reducing Disparities 42

Small group discussion Care Coordination Care coordination is foundational to transformation. We have heard the need for shared care planning to support care coordination. What would shared care planning look like from [your provider type] perspective? What components are/information is critical to include in a shared care plan? What does [your provider type] need to implement shared care planning? Healthier. Here Partnering Organization Summit | 43
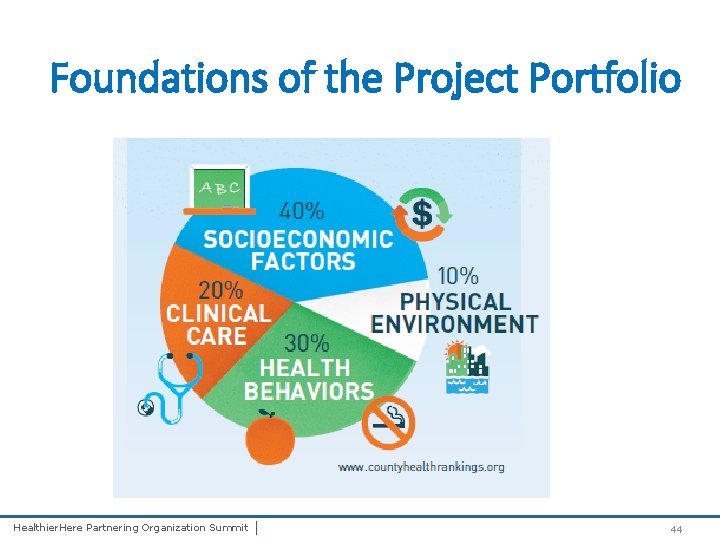
Foundations of the Project Portfolio Healthier. Here Partnering Organization Summit | 44

Small group discussion Bridging Health and Community Bridging community/social services and health systems is foundational to delivery system transformation and reducing disparities. How can we create stronger connections between health care systems and community based organizations? What are the barriers for [your provider type] to develop these partnerships? What does [your provider type] need to implement stronger two-way linkages? Healthier. Here Partnering Organization Summit | 45
What information do you need? How would you like to receive it? We welcome your feedback. Please fill out the following survey (webinar attendees): https: //www. surveymonkey. com/r/Healthier. Here 021518 This link will also be emailed to you (in-person attendees). 46

Wrap Up & Next Steps 47

Next Partnering Organization Summit: Wednesday March 14, 2018 (not a Thursday, beware!) 4: 00 – 6: 00 pm Webinar and In-person: Centilia Cultural Center 1660 S Roberto Maestas Festival St. Seattle, WA 98144 (Beacon Hill Link Station)

For more information… Susan Mc. Laughlin, Executive Director, smclaughlin@kingcountyach. org (206) 790 -3709 Gena Morgan, Director of Programs, gmorgan@kingcountyach. org (206) 849 -6262 Thuy Hua-Ly, Chief Financial Officer, thua-ly@kingcountyach. org (206) 849 -9988 Explore the Regional Health Needs Inventory: https: //goo. gl/j 5 e. Jav Healthier. Here Partnering Organization Summit | 49
- Slides: 49