HEALTHCARE REFORM 101 The basics and beyond Presented

HEALTHCARE REFORM 101 The basics and beyond Presented by Amy Fossum, SVP Alliant Employee Benefits June 12, 2013

AGENDA § Healthcare Reform § Why – What – Who § Overview § Strategy § Interactive Timeline § Grandfathered plans § Dependent coverage through age 25 § Preventive coverage § No rescission § Essential health benefits § Pre-existing condition exclusions § Medical loss ratio § Summary of benefits and coverage (SBC) § Taxes & Fees § W-2 reporting § Flexible spending account Limits § Notice of exchange § Automatic enrollment § Non-discrimination testing 2 § Individual mandate § Exchanges § Pay or Play § Coverage by 91 st day § Coverage for clinical trials § Wellness incentives § Cadillac Tax
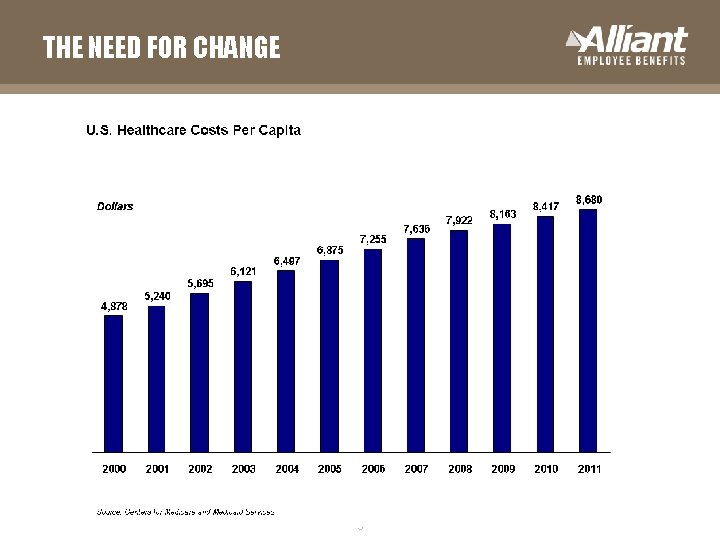
THE NEED FOR CHANGE 3

WHAT IS DRIVING HEALTH CARE SPENDING? What is driving health care spending? § While there is broad agreement that the rise in costs must be controlled, there is disagreement over the driving factors. Some of the major factors that have been discussed in cost growth are: § Technology and prescription drugs–Some analysts state that the availability of more expensive, state-of-the-art medical technologies and drugs fuels health care spending for development costs and because they generate demand for more intense, costly services even if they are not necessarily cost-effective. [2] § Rise in chronic diseases – It is estimated that health care costs for chronic disease treatment account for over 75% of national health expenditures. [3] In particular, there has been tremendous focus on the rise in rates of overweight and obesity and their contribution to chronic illnesses and health care spending. § Administrative costs – At least 7% of health care expenditures are estimated to go toward for the administrative costs of government health care programs and the net cost of private insurance (e. g. administrative costs, reserves, taxes, profits/losses). [1] Some argue that the mixed public-private system creates overhead costs and large profits that are fueling health care spending. [4] 1 Centers for Medicare and Medicaid Services, Office of the Actuary, National Health Statistics Group, National Health Care Expenditures Data , January 2012. 2 Congress of the United States, Congressional Budget Office. Technological Change and the Growth of Health Care Spending , January 2008. 3 Centers for Disease Control and Prevention. Rising Health Care Costs Are Unsustainable. April 2011. 4 Recent opinions/ reports have focused on the viability of a single-payer system in the U. S. W. C. Hsiao’s article “ State-based single-payer health care- as solution for the United States? ” explores potential adoption among states, and R. Feldman explores unregulated markets vs. single-payer systems in “ Quality of care in single-payer and multipayer health systems. ” 4
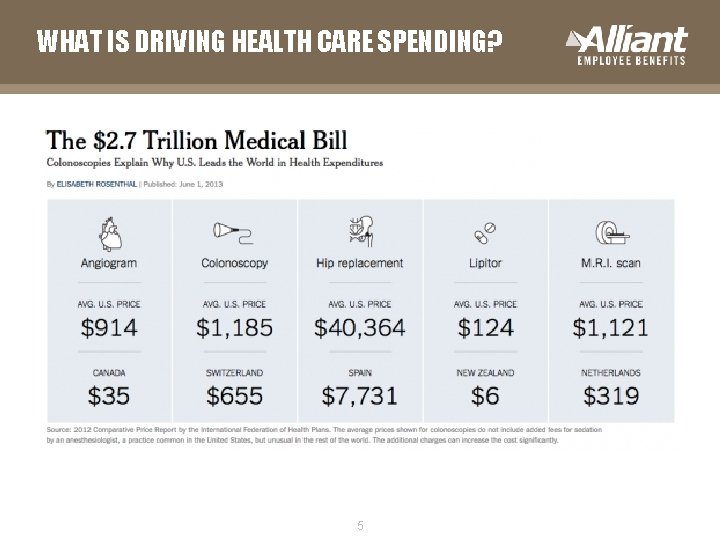
WHAT IS DRIVING HEALTH CARE SPENDING? 5

WHAT IS DRIVING HEALTH CARE SPENDING? 6

THE BILL AND AMENDMENTS I’m Just a Bill 7

IMPACT ON EMPLOYERS § Very small groups under 25 lives § Small groups under 50 lives § Large group 50+ 8

SMALL GROUP MARKET 9

SMALL GROUP MARKET § On average, small businesses pay about 18% more than large firms for the same health insurance policy. And small businesses lack the purchasing power that larger employers have § If you have fewer than 25 employees, pay average annual wages below $50, 000, and provide health insurance, you may qualify for a small business tax credit of up to 35% (up to 25% for non-profits) to offset the cost of your insurance. This credit will increase in 2014 to 50% (35% for non-profits) § In 2014, small businesses with generally fewer than 100 employees can shop in the Health Insurance Marketplace. This is meant to give better choices and lower prices. Open enrollment begins on October 1, 2013 § The Marketplace will offer a choice of plans that meet certain benefits and cost standards. Starting in 2014, members of Congress will be getting their health care insurance through the Marketplace § Employers with fewer than 50 employees are exempt from new employer responsibility policies. Don’t have to pay an assessment if their employees get tax credits through an Exchange 10

SMALL GROUP MARKET What You Need to Know about the Small Business Health Care Tax Credit § To be eligible, you must cover at least 50 percent of the cost of single (not family) health care coverage for each of your employees. You must also have fewer than 25 full-time equivalent employees (FTEs). Those employees must have average wages of less than $50, 000 a year. § For tax years 2010 through 2013, the maximum credit is 35 percent for small business employers and 25 percent for small tax-exempt employers such as charities. An enhanced version of the credit will be effective beginning Jan. 1, 2014. Additional information about the enhanced version will be added to IRS. gov as it becomes available. In general, on Jan. 1, 2014, the rate will increase to 50 percent and 35 percent, respectively. § Even if you are a small business employer who did not owe tax during the year, you can carry the credit back or forward to other tax years. Also, since the amount of the health insurance premium payments are more than the total credit, eligible small businesses can still claim a business expense deduction for the premiums in excess of the credit. That’s both a credit and a deduction for employee premium payments. § If you can benefit from the credit this year but forgot to claim it on your tax return there’s still time to file an amended return. 11

HEALTHCARE REFORM - WHY q Require health insurance q Larger employers must offer comprehensive, affordable coverage q Create healthcare Exchanges q No pre-existing conditions q Coverage becomes guarantee issue q Dependent coverage through age 25 q No cost preventive care Improve access to healthcare q Federal subsidies for lower income families q Caps on employee contributions q Expanded access to Medicaid q Caps on non-claims costs q Minimize cost-shifting for uninsured care q Pilot programs to address healthcare cost, quality and transparency Make coverage more affordable 12

HEALTHCARE REFORM- WHAT q Healthcare Exchanges q No pre-existing conditions Cost & quality initiatives q Guaranteed issue coverage q No rescission of coverage q Dependent coverage through age 25 q No limits on Essential Health Benefits generation q Coverage must be. Revenue Minimum Value (60%) q Improved preventive/women’s healthcare q Limit waiting periods – benefits begin by 91 st day q Medical Loss Ratio (MLR) Rebates Employer q 80 -85% of premiums must be used for claims Affordability administration q Wellness program premium differential (up to 50%) q Pilot quality of care programs q Subsidies for lower income families q Caps on employee cost for single coverage q Automatic enrollment q Monitor status changes q Proof of coverage offering q Pay or Play penalties q FSA Employee limits communication q Cadillac tax q Various taxes & fees q Summary of Benefit Coverage (SBC) q Notice of Exchange q W-2 reporting Coverage required - Individual Mandate 13
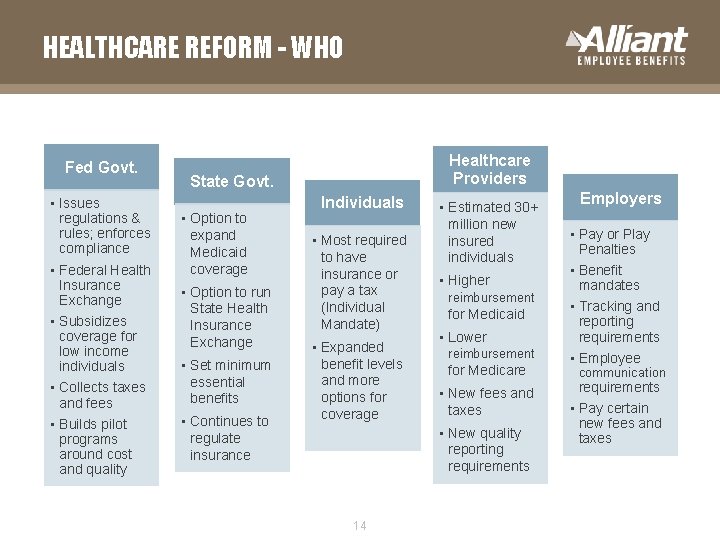

HEALTHCARE REFORM - WHO Fed Govt. • Issues regulations & rules; enforces compliance • Federal Health Insurance Exchange • Subsidizes coverage for low income individuals • Collects taxes and fees • Builds pilot programs around cost and quality Healthcare Providers State Govt. • Option to expand Medicaid coverage • Option to run State Health Insurance Exchange • Set minimum essential benefits • Continues to regulate insurance Individuals • Most required to have insurance or pay a tax (Individual Mandate) • Expanded benefit levels and more options for coverage • Estimated 30+ million new insured individuals • Higher reimbursement for Medicaid • Lower reimbursement for Medicare • New fees and taxes • New quality reporting requirements 14 Employers • Pay or Play Penalties • Benefit mandates • Tracking and reporting requirements • Employee communication requirements • Pay certain new fees and taxes

HEALTHCARE REFORM - OVERVIEW 2010 § § 2010, cont. § Young adult (through age 25) Affordable Care Act passed on March 23, 2010 Coverage expansion begins almost immediately: § Grandfathered plans GF § limit plan changes, avoid or delay some ACA mandates § Many preventive care services covered at no cost to member § No rescission (retroactive cancel) in most cases § Direct access to OBGYNs § Access to out-of-network emergency care § No lifetime dollar limits on Essential Health Benefits allowed to stay on parent’s plan § Grandfathered not req’d to offer if access to other group coverage § No pre-existing conditions for members age 18 and younger § Temporary ERRP subsidy program established to encourage early retiree benefits programs § New claims appeals processes 2011 § 15 Medical Loss Ratio (MLR) levels § 80%-85% of premiums must be paid out in claims costs § Any balance reimbursed

HEALTHCARE REFORM - OVERVIEW 2012 § § § 2013, cont. Accountable Care Organizations (ACOs) introduced First MLR rebates issued Plans must provide Summary of Benefit Coverage (SBC) § § 2013 § § § W-2 s include value of healthcare plan (for 250+ W-2 s issued) Healthcare flexible spending accounts limited to $2, 500/individual/employer Employer notice to employees regarding State Exchanges § Notice must be provided by 10/1/13 for current ee’s § For new ee’s hired on or after 10/1/13 Notice must be provided within 14 days of start date § § § 16 Medicare Tax increase from 1. 45% to 2. 35% (higher wage earners) Comparative Effectiveness Fee (PCORI) due 7/31/13 § $1 PMPY 1 st year § $2 PMPY thereafter Annual Insurance Carrier Fee § Some carriers will begin collecting in 2013 § Very little information available Medicare Part D subsidy is taxable to employer State Exchanges must begin enrolling members October 1 st

HEALTHCARE REFORM - OVERVIEW 2014 § Individual Mandate § Most required to have health § 2014, cont. § Pay or Play § Large Employers (50+) must offer Minimum Essential Coverage that is Affordable and provides a Minimum Value to all full-time employees and their dependents or risk penalties of: § $2, 000/employee (less 1 st 30 employees) OR § $3, 000 for each employee that qualifies for subsidized Exchange coverage § Penalties triggered if ONE employee enrolled in subsidized exchange coverage § Reinsurance Fee § $63 PMPY § Appears to end in 2017 insurance or penalty is: § 2014: greater of up to $285/family or 1% of family income § 2015: greater of up to $975/family or 2% of family income § 2016: greater of up to $2, 085/family or 2. 5% of family income State Exchanges begin offering coverage (individual/small group) § Federal Exchanges provides coverage if no state Exchange § Unclear if Exchanges will be ready – as of 11/29/12 only 17 states + DC stated intent 17
HEALTHCARE REFORM - OVERVIEW 2014, cont. § § § § 2018 No pre-existing conditions Coverage for clinical trials § Specific criteria will apply § Details pending Update SBC § Include statement about Affordable, Minimum Essential Coverage No limits on Essential Health Benefits § Remove annual dollar limits, if needed All non-grandfathered plans $6, 250 outof-pocket max for employee only coverage Fully-insured, small group plans $2, 000 deductible max for employee only coverage Limit waiting periods § Benefits begin by 91 st day 6055/6056 reporting to IRS § Includes plan coverage details and information on individuals coverage § Cadillac tax § 40% tax on plan premiums >$10, 200/individual or $27, 500/family § Higher limits for high risk jobs or older workforces Delayed § § 18 Automatic enrollment (200+) § Enroll full-time employees that don’t elect or waive in single, base-plan coverage Non-discrimination § Fully-insured plans offer consistent plans, contributions and waiting periods § Self-insured rules should be updated as well
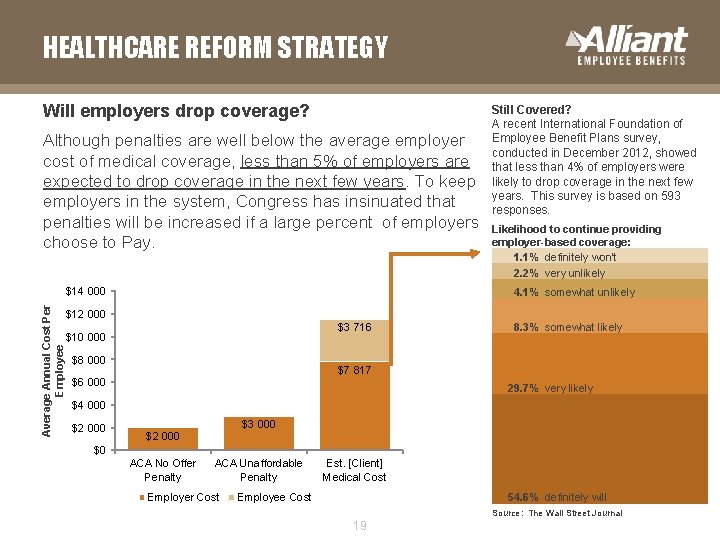
HEALTHCARE REFORM STRATEGY Will employers drop coverage? Although penalties are well below the average employer cost of medical coverage, less than 5% of employers are expected to drop coverage in the next few years. To keep employers in the system, Congress has insinuated that penalties will be increased if a large percent of employers choose to Pay. Average Annual Cost Per Employee $14 000 Still Covered? A recent International Foundation of Employee Benefit Plans survey, conducted in December 2012, showed that less than 4% of employers were likely to drop coverage in the next few years. This survey is based on 593 responses. Likelihood to continue providing employer-based coverage: 1. 1% definitely won't 2. 2% very unlikely 4. 1% somewhat unlikely $12 000 $3 716 $10 000 $8 000 8. 3% somewhat likely $7 817 $6 000 29. 7% very likely $4 000 $2 000 $3 000 $2 000 $0 ACA No Offer Penalty ACA Unaffordable Penalty Employer Cost Est. [Client] Medical Cost Employee Cost 54. 6% definitely will Source: The Wall Street Journal 19

HEALTHCARE REFORM STRATEGY Why will most employers choose to play? Dropping coverage competitive disadvantage increase pay to offset Soft dollar Hard dollar Cost challenges: § Comparable Exchange based coverage more costly § Adverse selection § Higher cost of admin for individual policies § Age-bands for older workers § Tax Issues § Penalties not deductible to employer; unlike healthcare premiums § Additional payroll taxes (FICA) owed by employer/employee § Cost of Exchange coverage generally not deductible for employees § Gross up pay further to offset employee tax increases § Only those ≤ 400% of poverty level eligible for premium subsidies § § § Loss of ability to manage health and productivity of workforce Productivity Loss – time spent procuring coverage Employees lose HR as advocate 20

HEALTHCARE REFORM STRATEGY Cost containment approaches Conservative • Leaner benefit levels (i. e. deductibles, copays, coinsurance, out of pocket, etc…) • Increase employee contributions • Increase dependent contributions • Incent enrollment in lower cost plans (i. e. CDHP or other) • Educate workforce on Exchange coverage options Moderate Aggressive • Add new “compliant” lower cost plan as default plan • Use permissible wellness surcharges to increase employee contributions (pending guidance) • Design plans or contributions to incent subsidy eligible employees to seek Exchange coverage • Lever wellness campaigns to reduce health risk related costs • Revise hourly schedules to limit benefit eligibility • Evaluate employee leasing • Self-insure to limit exposure to state and federal health premium taxes • Discontinue medical plans in favor of Exchange strategy • Ensure members have transparent access to cost and quality detail • Establish defined contribution approach 21

HEALTHCARE REFORM STRATEGY Reform Review Tool § Tool to review your plans and administrative procedures against the major ACA employer requirements including: § Pay or Play § Plan coverage levels § Administrative processes § Taxes and fees § Tool to document § Administrative elections (e. g. , Measuring Period and MLR rebates) § Action plan 22
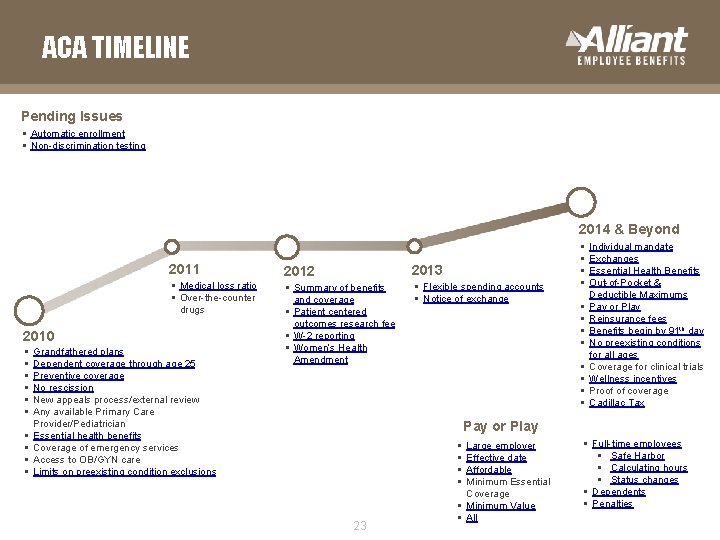
ACA TIMELINE Pending Issues § Automatic enrollment § Non-discrimination testing 2014 & Beyond 2011 2012 2013 § Medical loss ratio § Over-the-counter drugs § Summary of benefits and coverage § Patient centered outcomes research fee § W-2 reporting § Women’s Health Amendment § Flexible spending accounts § Notice of exchange 2010 § § § § § Grandfathered plans Dependent coverage through age 25 Preventive coverage No rescission New appeals process/external review Any available Primary Care Provider/Pediatrician Essential health benefits Coverage of emergency services Access to OB/GYN care Limits on preexisting condition exclusions § § § Individual mandate Exchanges Essential Health Benefits Out-of-Pocket & Deductible Maximums Pay or Play Reinsurance fees Benefits begin by 91 th day No preexisting conditions for all ages Coverage for clinical trials Wellness incentives Proof of coverage Cadillac Tax Pay or Play § § 23 Large employer Effective date Affordable Minimum Essential Coverage § Minimum Value § All § Full-time employees § Safe Harbor § Calculating hours § Status changes § Dependents § Penalties

GRANDFATHERED HEALTH PLANS What Grandfathered health plans are not required to comply with all ACA mandates Who Plans that established and have maintained grandfather status since March 23, 2010 How When Penalty GF § Must have continuously covered someone since March 23, 2010. § Make limited, allowed plan changes only § Annually notify plan members of grandfathered status Ongoing $100 per day per affected individual 24 Timeline

GRANDFATHERED PLANS How can a grandfathered health plan lose its status? q Significantly cut benefits q Increase out-of pocket costs q Reduce employer contribution towards the cost of the plan q Change insurance carriers before 11/07/10 A plan may enhance its coverage or add options without jeopardizing its status. Employer Action! To maintain grandfathered status, a plan must : § Provide a statement that the plan is a grandfathered plan (at least annually) along with contact information for questions or complaints; § Document the terms of existence on March 23, 2010. 25 Timeline

GRANDFATHERED PLANS ACA Mandates that do not apply to Grandfathered Plans: q Any provider designated as PCP q Direct access to OB/GYN q Access to out-of-network emergency services q Coverage for clinical trials q 100% preventive care coverage q Including women’s preventive q Non-discrimination for fully-insured plans q New claims appeals processes q Cover children through age 25 if they are eligible for their own employer’s health plan (until 1/1/2014) 26 Timeline

DEPENDENT COVERAGE THROUGH AGE 25 What Plans must cover children through age 25 Who Any group health plan that covers dependent children How When Penalty § Only requirement is relationship between child and subscriber § Marital, student, residency or tax dependency doesn’t matter § Plan years starting September 23, 2010 and after § Grandfathered health plans can exclude children that are eligible for their own employer’s plan until the first plan year on or after January 1, 2014 $100 per day per affected individual 27 Timeline
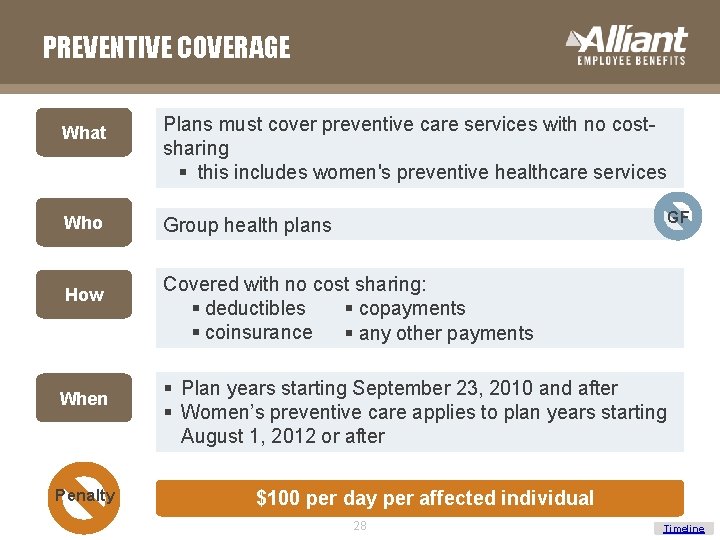
PREVENTIVE COVERAGE What Who How When Penalty Plans must cover preventive care services with no costsharing § this includes women's preventive healthcare services GF Group health plans Covered with no cost sharing: § deductibles § copayments § coinsurance § any other payments § Plan years starting September 23, 2010 and after § Women’s preventive care applies to plan years starting August 1, 2012 or after $100 per day per affected individual 28 Timeline

PREVENTIVE COVERAGE What is included under preventive care? q Evidence-informed preventive q Immunizations care q Well-woman visits q Contraception* q Support for breastfeeding q Domestic violence screening* equipment* * Women’s preventive care is effective for plan years on or after August 1, 2012. Additional guidance is still pending around religious employers and how the contraceptive coverage applies to them. Employer Action! Religious employers are required to distribute a notice to employees if delaying contraceptive services. 29 Timeline
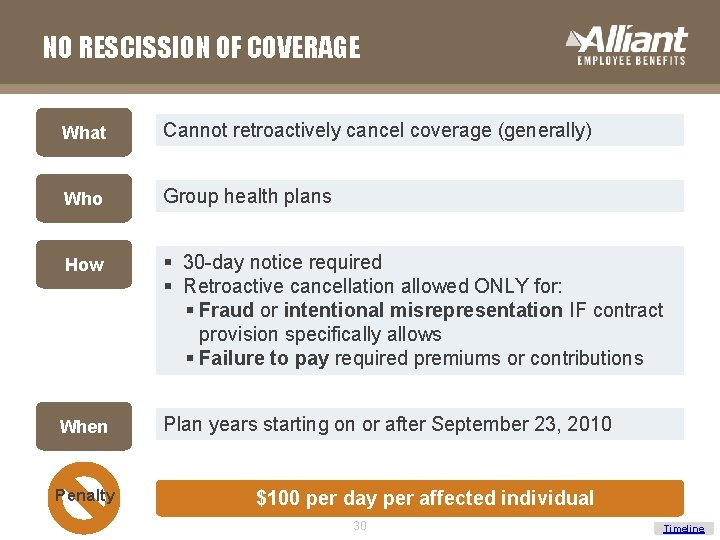

NO RESCISSION OF COVERAGE What Cannot retroactively cancel coverage (generally) Who Group health plans How § 30 -day notice required § Retroactive cancellation allowed ONLY for: § Fraud or intentional misrepresentation IF contract provision specifically allows § Failure to pay required premiums or contributions When Penalty Plan years starting on or after September 23, 2010 $100 per day per affected individual 30 Timeline
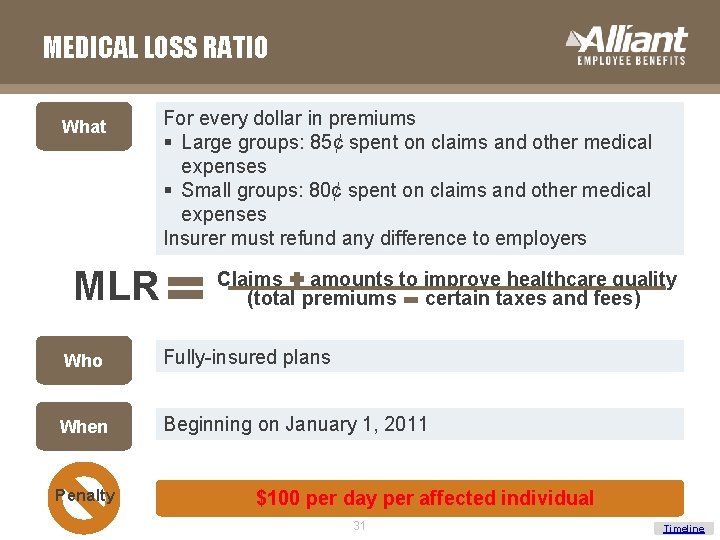

MEDICAL LOSS RATIO What MLR For every dollar in premiums § Large groups: 85¢ spent on claims and other medical expenses § Small groups: 80¢ spent on claims and other medical expenses Insurer must refund any difference to employers Claims amounts to improve healthcare quality (total premiums certain taxes and fees) Who Fully-insured plans When Beginning on January 1, 2011 Penalty $100 per day per affected individual 31 Timeline

MEDICAL LOSS RATIO Example: Giant Insurance Co. has $900 MM in claims and $100 MM in health quality expenses. § Total premiums were $1. 2 B; no taxes or fees § Giant’s MLR = $900 MM+$100 MM)/ $1. 2 B = 83. 33% § Giant owes the difference between the 85% and the 83. 33% they actually spent Rebates must be provided to employers by August 1 of the following year by premium credit or lump-sum check Employer Action! What can employer do with funds? Three basic choices: 1) Reduce participant premiums 2) Provide benefit enhancements 3) Return in cash to participants § Each choice carries considerations, the plan document should be checked first § All three choices not available to all plans 32 Timeline
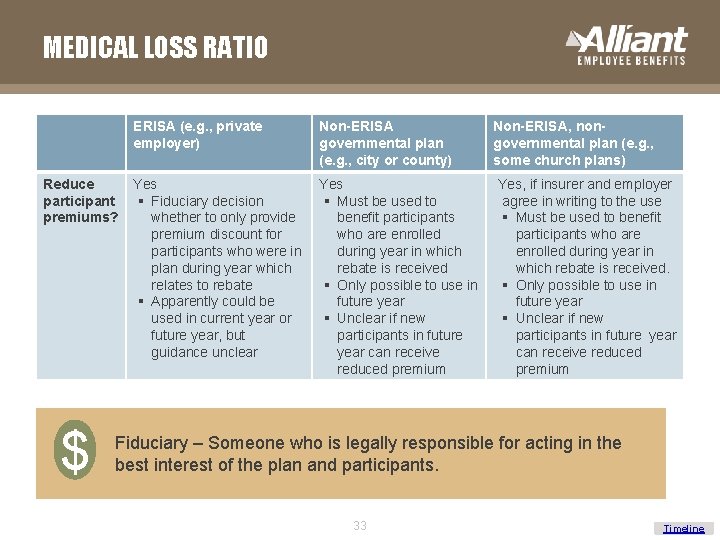
MEDICAL LOSS RATIO Reduce participant premiums? $ ERISA (e. g. , private employer) Non-ERISA governmental plan (e. g. , city or county) Yes § Fiduciary decision whether to only provide premium discount for participants who were in plan during year which relates to rebate § Apparently could be used in current year or future year, but guidance unclear Yes § Must be used to benefit participants who are enrolled during year in which rebate is received § Only possible to use in future year § Unclear if new participants in future year can receive reduced premium Non-ERISA, nongovernmental plan (e. g. , some church plans) Yes, if insurer and employer agree in writing to the use § Must be used to benefit participants who are enrolled during year in which rebate is received. § Only possible to use in future year § Unclear if new participants in future year can receive reduced premium Fiduciary – Someone who is legally responsible for acting in the best interest of the plan and participants. 33 Timeline
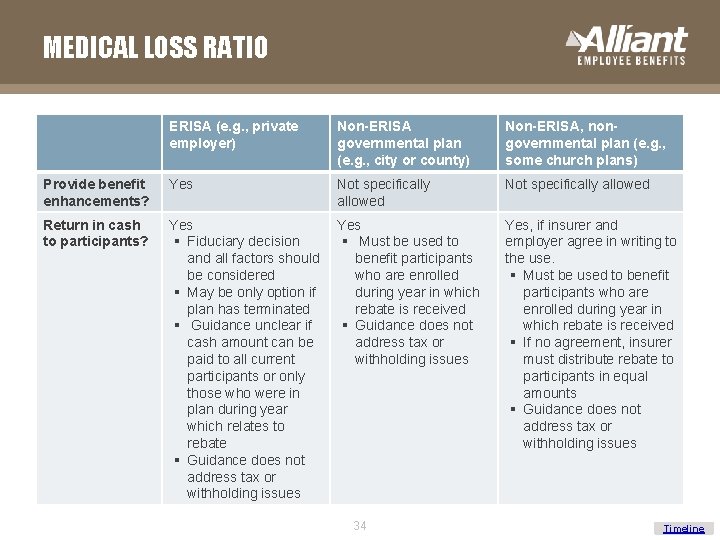
MEDICAL LOSS RATIO ERISA (e. g. , private employer) Non-ERISA governmental plan (e. g. , city or county) Non-ERISA, nongovernmental plan (e. g. , some church plans) Provide benefit enhancements? Yes Not specifically allowed Return in cash to participants? Yes § Fiduciary decision and all factors should be considered § May be only option if plan has terminated § Guidance unclear if cash amount can be paid to all current participants or only those who were in plan during year which relates to rebate § Guidance does not address tax or withholding issues Yes § Must be used to benefit participants who are enrolled during year in which rebate is received § Guidance does not address tax or withholding issues Yes, if insurer and employer agree in writing to the use. § Must be used to benefit participants who are enrolled during year in which rebate is received § If no agreement, insurer must distribute rebate to participants in equal amounts § Guidance does not address tax or withholding issues 34 Timeline

SUMMARY OF BENEFITS AND COVERAGE (SBC) What Who How When Penalty Health insurers and self-insured group health plans are required to provide a SBC to all individuals eligible to enroll in a group health plan including: § Mid-year enrollees § Qualifying event enrollees § Upon request § Open enrollment Fully-insured and self-funded health plans. The SBC must be distributed to: § Participants § Prospective enrollees § Beneficiaries § Special enrollees Either print or electronic delivery allowed First open enrollment period on or after September 23, 2012 $1, 000 per enrollee 35 Timeline

SUMMARY OF BENEFITS AND COVERAGE (SBC) SBC Requirements q Be printed in 12 -point font q Include consumer costs examples based on the specific plan’s benefits q List customer service phone number and a web site q Contain renewability and continuation of coverage provisions (COBRA) q Be no more than four double-sided pages q Use terms most people understand (including a glossary) q Include description of coverage including cost sharing and limitations q Be written in culturally respectful language Employer Action! ! Employers must distribute the SBC with initial enrollment materials. If renewal is automatic, the SBC must be provided at least 30 days before the first day of the new plan year. An SBC must be provided within seven business days when requested. SBCs may be distributed electronically if certain requirements are met. 36 Timeline

SUMMARY OF BENEFITS AND COVERAGE (SBC) What plans require an SBC? § Generally required for any group health plan, some exceptions exist § Excepted benefits do not need an SBC ? A group health plan is any employer-sponsored plan that provides medical care to employees directly or through insurance, reimbursement, or otherwise 37 Timeline

SUMMARY OF BENEFITS AND COVERAGE Benefit Type Do SBC Rules Apply? Comments Dental Plan Usually not — Many dental plans are an excepted benefit under HIPAA § Coverage must be limited to treatment of the mouth Health FSA Usually not — Most Health FSAs are excepted benefits under HIPAA § Excepted benefits test for Health FSAs usually satisfied if no employer contributions (or employer contributions are capped at $500) § Test for SBC purposes identical to test for other purposes. HSA Usually not — Most HSAs are not a group health plan or "employee welfare benefit plan ! Remember, excepted benefits do not need an SBC 38 Timeline
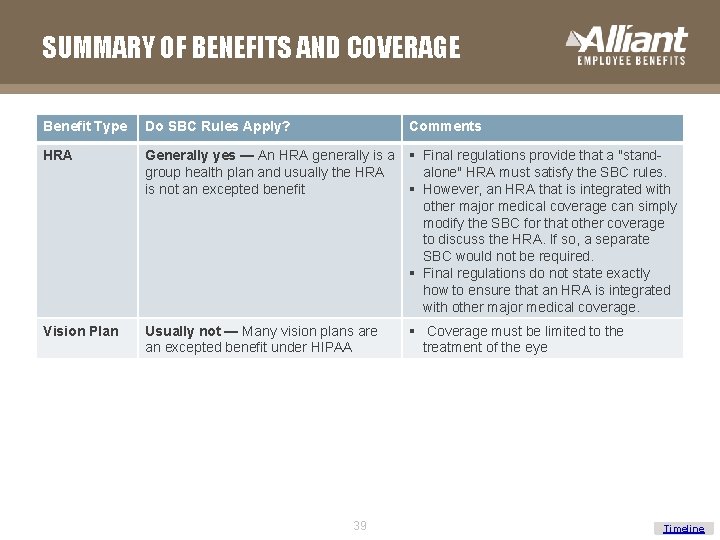
SUMMARY OF BENEFITS AND COVERAGE Benefit Type Do SBC Rules Apply? Comments HRA Generally yes — An HRA generally is a group health plan and usually the HRA is not an excepted benefit § Final regulations provide that a "standalone" HRA must satisfy the SBC rules. § However, an HRA that is integrated with other major medical coverage can simply modify the SBC for that other coverage to discuss the HRA. If so, a separate SBC would not be required. § Final regulations do not state exactly how to ensure that an HRA is integrated with other major medical coverage. Vision Plan Usually not — Many vision plans are an excepted benefit under HIPAA § Coverage must be limited to the treatment of the eye 39 Timeline

PATIENT CENTERED OUTCOMES RESEARCH FEE What Who How When Also known as the Comparative Effectiveness Fee, will fund a private, non-profit corporation is to assist providers, payers and policy makers in making informed health decisions. Both self-funded medical plans and health insurance carriers § $1 multiplied by the average number of covered lives under the plan § $1 fee doubles to $2 the following year § Covered lives is defined as the average number of lives covered under a plan – this includes employees and dependents. The first plan year ending after September 30, 2012. 40 Timeline

REINSURANCE FEES What Who How When TPAs of group health plans and insurers are required to contribute to a temporary reinsurance program for the individual market to offset risk of high-cost claims (in effect shifting risk from insurers to reinsurers) TPAs and insurance carriers are likely to pass these fees along to employers. § Fee based on the number of covered lives and applies to major medical coverage. § For benefit year 2014, HHS expects the per capita contribution rate to be $5. 25 per month ($63 per year). Effective no later than 1/1/14. This fee only lasts for three benefit years — 2014, 2015 and 2016. (A benefit year = calendar year and is not based on a health plan‘s specific plan year. ) 41 Timeline

ANNUAL FEES FOR INSURANCE CARRIERS What Annual fee on covered entities that provide health insurance Who § Fully-insured plans How When § No guidance yet on how fee is calculated or collected § Insurance carriers likely to pass it along to policyholders § Likely significant variation in how fees applied — in some cases, fee may be included in rates or charged as a separate line item § Payable to the government sometime in 2014 § Some insurance carriers may begin collecting fee from policyholders in 2013 42 Timeline

MEDICARE PART D SUBSIDY TAXABLE What Previously employers could subtract the cost of providing retiree prescription drug benefits, plus collect a subsidy (in effect, getting a deduction for expenses they did not actually pay) Who Employers receiving Medicare Part D subsidy How Starting in 2013, employers will be taxed on subsidies (can still deduct cost of prescription drug program) When Tax years beginning January 1, 2013 43 Timeline

W-2 REPORTING What Who When How Penalty Value of applicable employer-sponsored group health plan coverage is reported on employee's W-2 Form Employers that distribute ≥ 250 W-2 s for the previous tax year including: § Private employers § Federal, state and local government entities § Churches and other religious organizations 2012 tax year (provided to employees in January 2013) Value printed on W-2; delivered to employee by mail, online or other standard delivery method $100 for each reporting failure 44 Timeline

W-2 REPORTING ? How does this rule apply to control groups? In a controlled group, each employer is considered separately (i. e. , aggregation rules don’t apply). ? Will employees get taxed on the amount reported? No. W-2 reporting is done for informational purposes only. An amount is not taxable simply because it is reported on the Form W-2. ? What coverage is reported? Employer-sponsored coverage provided to an employee and his/her family, including coverage under a group health plan, such as major medical coverage. 45 Timeline

W-2 REPORTING – COST OF COVERAGE $ Employee contribution Employer contribution Cost of coverage is determined on a month by month, employee-by-employee basis Employer Action! Employer can select between three methods to calculate cost of coverage: 1) COBRA Applicable Premium – Reportable cost = COBRA premium under traditional COBRA rules 2) Premium Charged – Fully-insured plans only. Employer uses premium charged by insurer for employee’s coverage. 3) Modified COBRA Premium – Only available for employers that subsidize cost of COBRA coverage or that set cost of COBRA coverage by applying COBRA premium from prior year. Employers subsidizing COBRA coverage use good faith estimate of COBRA premium. Employers using prior year's COBRA premium for current year report that COBRA premium. 46 Timeline

W-2 REPORTING – COVERAGE EXCEPTIONS Coverage Discussion of exception Archer MSA with employer contributions COBRA coverage Employer has option to report cost of COBRA coverage. However, employer must be consistent under that plan (either including or not including the cost of such COBRA coverage). Dental plan If an excepted benefit Dental or vision plan not integrated into another medical or health plan X Dental or vision plan which gives the choice of declining or electing and paying an additional premium X 47 Timeline

W-2 REPORTING – COVERAGE EXCEPTIONS Coverage Discussion of exception EAP (employee assistance program) – in some circumstances Excepted benefits § Excluded if not a group health plan or § if a group health plan but no premium charged under COBRA Includes: § Coverage only for accident, or disability income insurance § Coverage issued as a supplement to liability insurance § Liability insurance, including general liability insurance and automobile liability insurance § Workers' compensation or similar insurance § Automobile medical payment insurance § Credit-only insurance. 48 Timeline

W-2 REPORTING – COVERAGE EXCEPTIONS Coverage Discussion of exception Health FSA – with employer Rule applies if benefit under Health FSA > contributions or flex credits employee's contribution for the year. If so W-2 reportable amount Health FSA – with only employee contributions HSA with employer or employee contributions Health FSA benefit Employee contribution Usually excluded if benefit is ≤ to employee's salary reduction election (e. g. , no employer matching or seed contributions) Not subject to the rules. However, still have to report employer contributions (and pre-tax employee contributions through a cafeteria plan). 49 Timeline
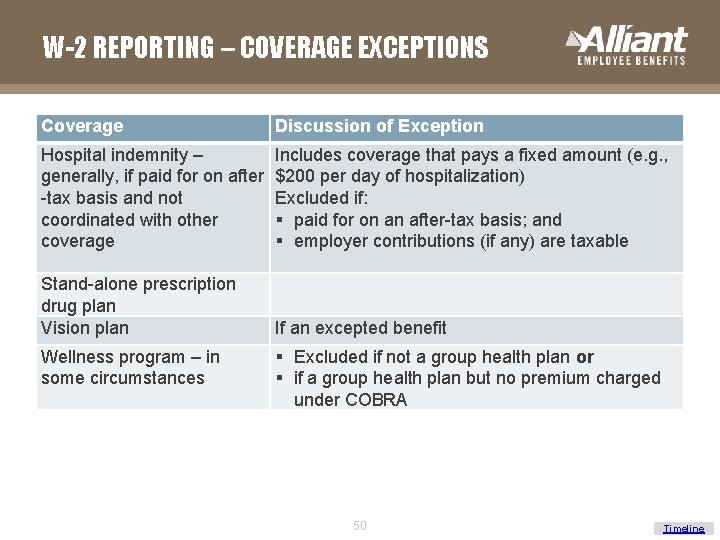

W-2 REPORTING – COVERAGE EXCEPTIONS Coverage Discussion of Exception Hospital indemnity – generally, if paid for on after -tax basis and not coordinated with other coverage Includes coverage that pays a fixed amount (e. g. , $200 per day of hospitalization) Excluded if: § paid for on an after-tax basis; and § employer contributions (if any) are taxable Stand-alone prescription drug plan Vision plan If an excepted benefit Wellness program – in some circumstances § Excluded if not a group health plan or § if a group health plan but no premium charged under COBRA 50 Timeline
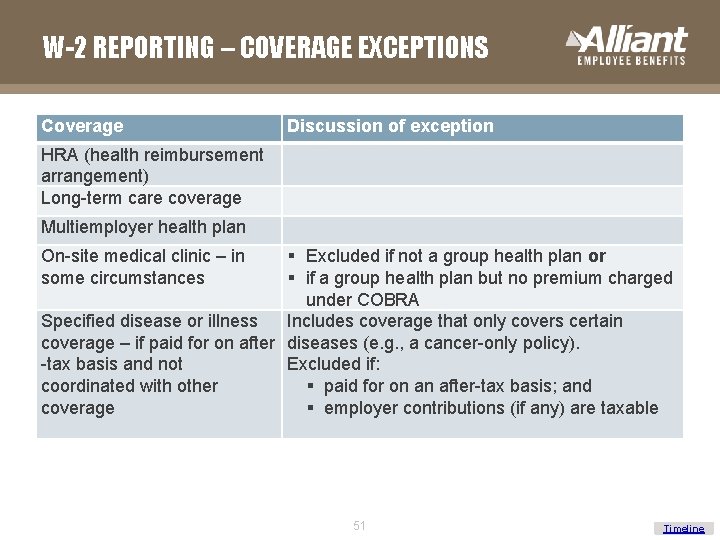
W-2 REPORTING – COVERAGE EXCEPTIONS Coverage Discussion of exception HRA (health reimbursement arrangement) Long-term care coverage Multiemployer health plan § Excluded if not a group health plan or § if a group health plan but no premium charged under COBRA Specified disease or illness Includes coverage that only covers certain coverage – if paid for on after diseases (e. g. , a cancer-only policy). -tax basis and not Excluded if: coordinated with other § paid for on an after-tax basis; and coverage § employer contributions (if any) are taxable On-site medical clinic – in some circumstances 51 Timeline
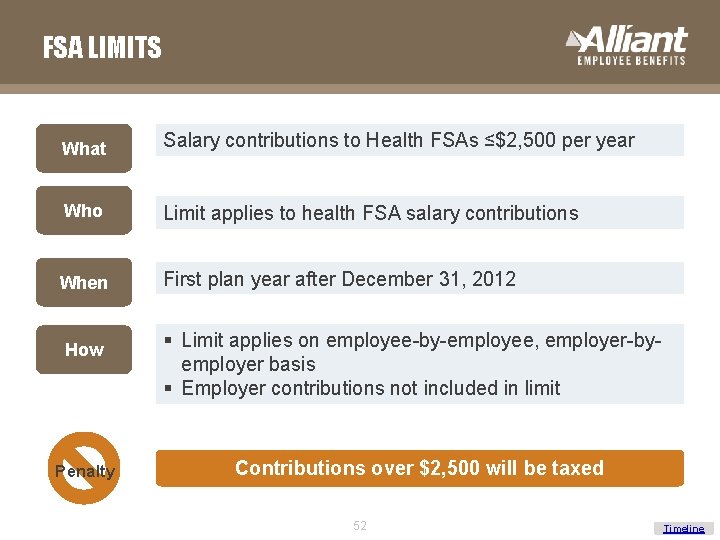

FSA LIMITS What Salary contributions to Health FSAs ≤$2, 500 per year Who Limit applies to health FSA salary contributions When First plan year after December 31, 2012 How Penalty § Limit applies on employee-by-employee, employer-byemployer basis § Employer contributions not included in limit Contributions over $2, 500 will be taxed 52 Timeline

FSA LIMITS $2, 500 limit applies to each employee. § Example: Employer employs two individuals who are married to each other, each of the employees may contribute $2, 500 and receive a total family benefit of $5, 000 ! An individual eligible for benefits at two separate employers can elect up to $2, 500 in each Health FSA as long as the employers are not part of the same controlled group $2, 500 annual limit will be indexed for inflation for tax years beginning after December 31, 2013 53 Timeline

MARKETPLACE NOTICE (NOTICE OF EXCHANGE) What Who When How Provide information about the Marketplace and outline some differences between purchasing a health plan through the Marketplace and choosing group-sponsored coverage All employers § For new employees hired on or after 10/1/13, the Notice must be provided within 14 days of the employee’s start date. § For employees employed before 10/1/13, the Notice must be provided no later than 10/1/13. Can be provided by first-class mail or can be provided electronically if the DOL's electronic disclosure safe harbor requirements are met 54 Timeline

INDIVIDUAL MANDATE What Individuals must have Minimum Essential Coverage Who All U. S. citizens and legal residents When Beginning in 2014 How Penalty If individual or individual’s spouse or dependent does not have Minimum Essential Coverage, penalty will be assessed against that individual Penalty is charged for each individual without coverage: § 2014: $95/individual, $47. 50/child, capped at greater of $285/family or 1% of family income § 2015: $325/individual, $162. 50/child, capped at greater of $975/family or 2% of family income § 2016: $695/individual, $347. 50/child, capped at greater of $2, 085/family or 2. 5% of family income 55 Timeline
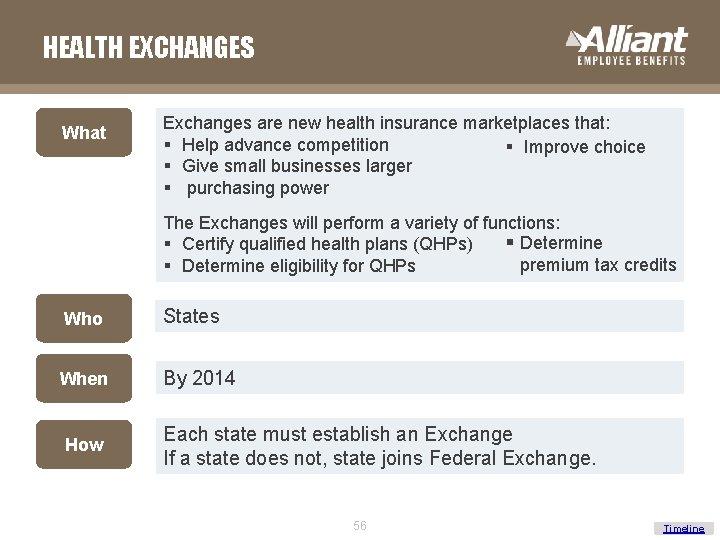
HEALTH EXCHANGES What Exchanges are new health insurance marketplaces that: § Help advance competition § Improve choice § Give small businesses larger § purchasing power The Exchanges will perform a variety of functions: § Determine § Certify qualified health plans (QHPs) premium tax credits § Determine eligibility for QHPs Who States When By 2014 How Each state must establish an Exchange If a state does not, state joins Federal Exchange. 56 Timeline

ESSENTIAL HEALTH BENEFITS What Fully-insured small group and individual health plans must cover essential health benefits with no annual dollar limits or lifetime maximums. Large group health plans and self funded plans are not required to cover EHB. However, if they do cover a EHB the plan must cover it with no annual dollar limits or lifetime maximums. Who Group health plans and insurers, but not to certain excepted benefits When Plan years beginning on or after January 1, 2014 How Essential health benefits include minimum benefits in ten categories § Prescription drugs § Ambulatory patient services § Emergency services § Rehabilitative services and § Laboratory services devices § Preventive and wellness § Hospitalization services; chronic disease § Maternity and newborn care management § Mental health and substance § Pediatric services use disorder services 57 Timeline
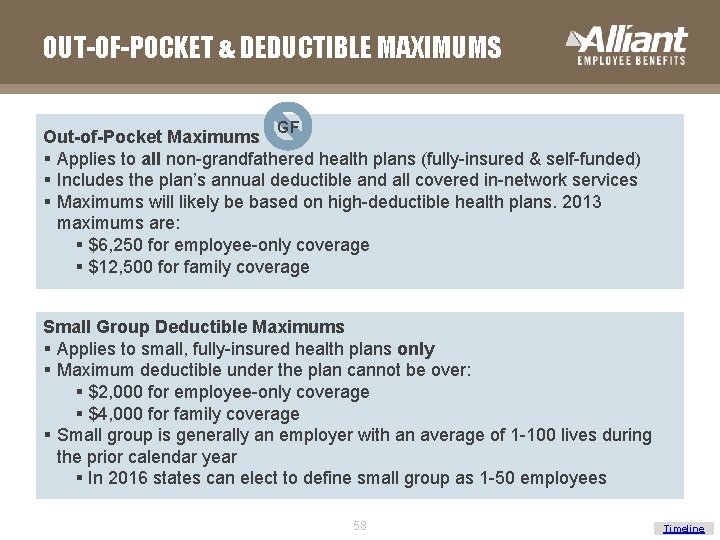

OUT-OF-POCKET & DEDUCTIBLE MAXIMUMS GF Out-of-Pocket Maximums § Applies to all non-grandfathered health plans (fully-insured & self-funded) § Includes the plan’s annual deductible and all covered in-network services § Maximums will likely be based on high-deductible health plans. 2013 maximums are: § $6, 250 for employee-only coverage § $12, 500 for family coverage Small Group Deductible Maximums § Applies to small, fully-insured health plans only § Maximum deductible under the plan cannot be over: § $2, 000 for employee-only coverage § $4, 000 for family coverage § Small group is generally an employer with an average of 1 -100 lives during the prior calendar year § In 2016 states can elect to define small group as 1 -50 employees 58 Timeline

PAY OR PLAY What Health plan offers Minimum Essential Coverage that is Affordable and provides Minimum Value (60% actuarial) Who Large employers (50+ full-time + FTEs) How Provided coverage to full-time employees (130+ hrs/mo) and their dependents. When January 1, 2014 (non-calendar year plans may qualify for delay to first day of 2014 plan year) = $2, 000 x (# full-time employees - 30) Penalty Coverage not offered at all OR fail to offer Minimum Essential Coverage to all full-time employees. = $3, 000 per employee that enrolls in subsidized exchange coverage if Affordable, Minimum Value coverage not offered 59 Timeline
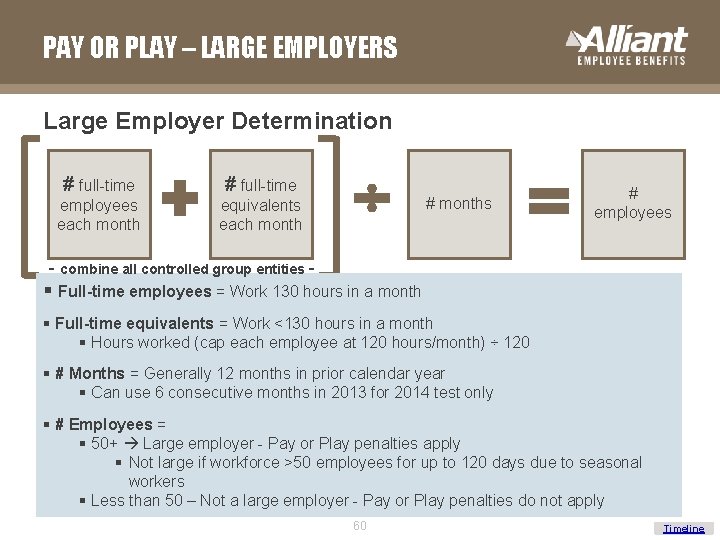
PAY OR PLAY – LARGE EMPLOYERS Large Employer Determination # full-time employees each month equivalents each month # months # employees - combine all controlled group entities - § Full-time employees = Work 130 hours in a month § Full-time equivalents = Work <130 hours in a month § Hours worked (cap each employee at 120 hours/month) ÷ 120 § # Months = Generally 12 months in prior calendar year § Can use 6 consecutive months in 2013 for 2014 test only § # Employees = § 50+ Large employer - Pay or Play penalties apply § Not large if workforce >50 employees for up to 120 days due to seasonal workers § Less than 50 – Not a large employer - Pay or Play penalties do not apply 60 Timeline

PAY OR PLAY – EFFECTIVE DATE Effective date Pay or Play penalties generally effective January 1, 2014 Big Deal! ! Non-calendar year plans effective date may be delayed to 1 st day of 2014 plan year if: § They offer Affordable, Minimum Value Coverage to full-time employees by the 1 st day of the 2014 plan year, and § Plan was in place on December 27, 2012, and § Coverage offered to 1/3 of employees during 2012 open enrollment, or § 25% of employees enrolled at 2012 open enrollment or on any date between October 31, 2012 – December 27, 2012 Note: Employee is not defined. Assume includes all employees including part-time, seasonal, on unpaid leave (e. g. , FMLA), etc. 61 Timeline

PAY OR PLAY – EFFECTIVE DATE Example 1 ABCco has a plan year that starts on June 1 st. ABCco does not offer coverage to employees that work less than 35 hours per week. At the end of their most recent open enrollment period (June 1, 2012) they offered coverage to 30 of their 100 employees. Of the 30 employees offered coverage, 26 chose to enroll during the 2012 open enrollment. Effective Date Evaluation Percent Eligible Calculation: 30/100 = 30% Fail (less than 33. 33%) Percent Coverage Calculation: 26/100 = 26% Pass (at least 25%) Overall Results: Pass – Delayed effective date is available Because ABCco passed one of the tests, they will avoid all penalties as long as they offer Affordable, Minimum Value Coverage to full-time employees by June 1, 2014. 62 Timeline

PAY OR PLAY – EFFECTIVE DATE Example 2 XYZco has a plan year that starts on December 1 st. XYZco offers coverage to salaried full-time employees, but not hourly full-time employees. At the end of their most recent open enrollment period (November 15, 2012), XYZco had offered coverage to 64 of its 200 employees. Of the 64 employees offered coverage, 48 were enrolled on December 1, 2012. Effective Date Evaluation Percent Eligible Calculation: 64/200 = 32% Fail (less than 33. 33%) Percent Coverage Calculation: 48/200 = 24% Fail (less than 25%) Overall Results: Fail – Delayed effective date is not available. Because XYZco did not pass one of the tests, they may have to pay penalties if they don’t offer Minimum Essential Coverage which is Affordable and provides Minimum Value to all full-time employees by January 1, 2014. 63 Timeline

PAY OR PLAY– EFFECTIVE DATE Identifying your plan year § Ideally plan year is identified in plan document (e. g. , SPD) § May not be the same as the policy (renewal) year § In the absence of plan documents, defer to: 1) The deductible or limit year used under the plan 2) If the plan does not impose deductibles or limits on a yearly basis, then the plan year is the policy year 3) If the plan does not impose deductibles or limits on a yearly basis, and either the plan is not insured or the insurance policy is not renewed on an annual basis, then the plan year is the employer's taxable year, or 4) In any other case, the plan year is the calendar year Note: The rules listed above are not based on IRS guidance. They are based on guidance from a different federal agency. This is the best information available at this time. 64 Timeline

PAY OR PLAY - AFFORDABILITY Affordable Coverage must be Affordable for those with household incomes of 100 -400% of Federal Poverty level § Federal Poverty Level Annual single coverage costs ≤ 9. 5% of Federal Poverty Level for single household § Employer uses same base contribution for all employees § § Safe Harbor Rate of Pay Method § § Monthly single coverage costs ≤ 9. 5% of hourly wage x 130 W-2 Method § Annual single coverage costs ≤ 9. 5% of year end W-2 (box 1) = $3, 000 per employee Penalty that enrolls in subsidized exchange coverage if coverage is not Affordable 65 Timeline

PAY OR PLAY - AFFORDABILITY Federal Poverty Level Safe Harbor Single coverage employee cost is ≤ 9. 5% of single household Federal Poverty Level Continental US $11, 490 x 9. 5% = $1, 091. 55 Affordable base plan employee contribution ≤ $1, 091. 55/year or $90. 96/month Alaska $14, 350 x 9. 5% = $1, 363. 25 Affordable base plan employee contribution ≤ $1, 363. 25/year or $113. 60/month Hawaii $13, 230 x 9. 5% = $1, 256. 85 Affordable base plan employee contribution ≤ $1, 256. 85/year or $104. 73/month EASY Calculations based on 2013 Federal Poverty Levels 66 Timeline

PAY OR PLAY - AFFORDABILITY Rate of Pay Safe Harbor Single coverage employee cost is ≤ 9. 5% employee’s hourly wage x 130 Calculation § Each employee evaluated separately § Employee earning $8. 50/hr $8. 50 x 130 = $1, 105 x 9. 5% = $104. 97 Affordable base plan employee contribution ≤ $104. 97/mo W-2 Safe Harbor Single coverage employee cost is ≤ 9. 5% employee’s W-2 earnings (box 1) Calculation § Each employee evaluated separately § Employee that earned $14, 000/yr $14, 000 x 9. 5% = $1, 330 Affordable base plan employee contribution ≤ $1, 330/yr or $110. 83/mo WARNING! W-2 income is final at end of year, but no retroactive changes 67 Timeline
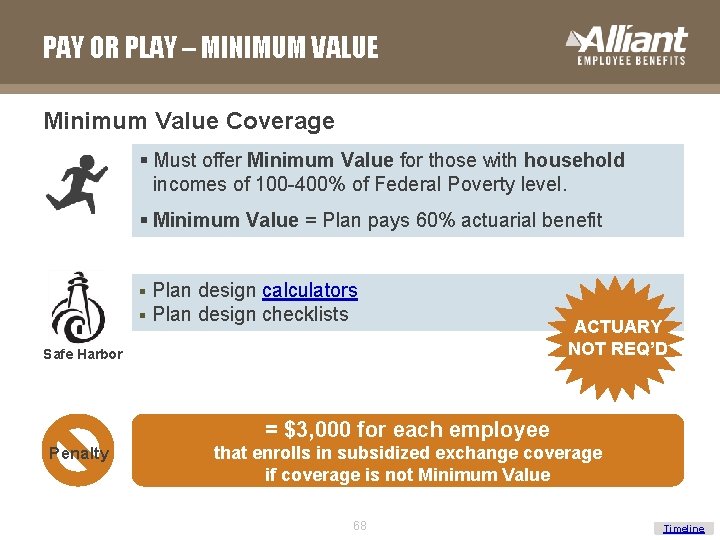

PAY OR PLAY – MINIMUM VALUE Minimum Value Coverage § Must offer Minimum Value for those with household incomes of 100 -400% of Federal Poverty level. § Minimum Value = Plan pays 60% actuarial benefit § § Plan design calculators Plan design checklists Safe Harbor ACTUARY NOT REQ’D = $3, 000 for each employee Penalty that enrolls in subsidized exchange coverage if coverage is not Minimum Value 68 Timeline

PAY OR PLAY – MINIMUM VALUE Minimum Value Safe Harbor Plan Designs § $3, 500 integrated medical and drug deductible, 80% plan costsharing and a $6, 000 maximum out-of-pocket limit for employee cost-sharing Safe Harbor § $4, 500 integrated medical and drug deductible, 70% plan costsharing, a $6, 400 maximum out-of-pocket limit and a $500 employer contribution to a HSA § $3, 500 medical deductible, $0 drug deductible, 60% plan medical expense cost-sharing, 75% plan drug cost-sharing, a $6, 400 maximum out-of-pocket limit and drug co-pays of $10 / $20 / $50 for the first, second and third prescription drug tiers, with 75% coinsurance for specialty drugs. 69 Timeline

PAY OR PLAY – ALL All clarified § Must offer coverage to all full-time employees Big Deal! ! Penalty § De Minimus Exception § All = at least 95% of full-time employees WARNING! Offering coverage to 95% of employees does not eliminate potential for other penalties (e. g. , if coverage is not Affordable) = $2, 000 x (# full-time employees - 30) Coverage not offered at all OR fail to offer Minimum Essential Coverage to full-time employees and dependents if ONE employee enrolls in subsidized exchange coverage 70 Timeline

PAY OR PLAY – FULL-TIME EMPLOYEES Full-time § Must offer coverage to full-time employees (130+ hrs/mo) ? § Monitor status on monthly basis § Stable workforce with full-time/part-time only § Assume retroactive changes req’d based on hours worked § Safe Harbor Establish Measurement/Stability Periods § Workforce includes variable hour, temporary and/or seasonal employees § Movement between full-time and part-time status = $2, 000 x (# full-time employees -ACTUARY 30) Penalty NOT REQ’D Coverage not offered at all OR fail to offer Minimum Essential Coverage to full-time employees and dependents if ONE employee enrolls in subsidized exchange coverage 71 Timeline
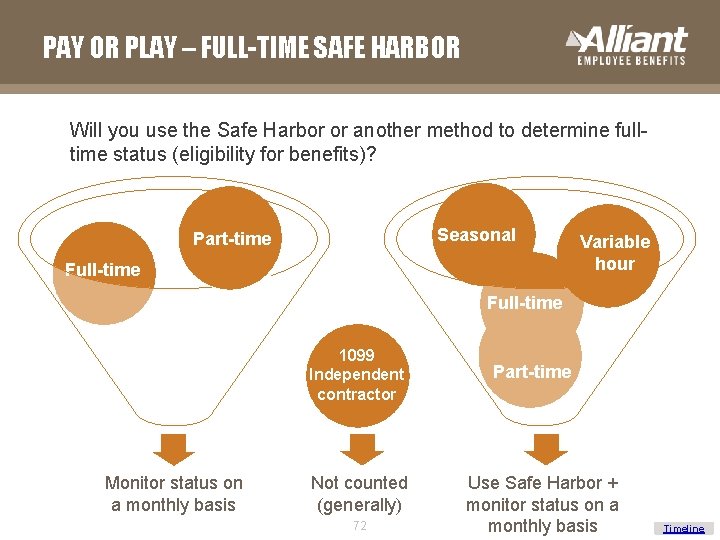
PAY OR PLAY – FULL-TIME SAFE HARBOR Will you use the Safe Harbor or another method to determine fulltime status (eligibility for benefits)? Seasonal Part-time Full-time Variable hour Full-time Part-time 1099 Independent contractor Monitor status on a monthly basis Not counted (generally) 72 Part-time Use Safe Harbor + monitor status on a monthly basis Timeline
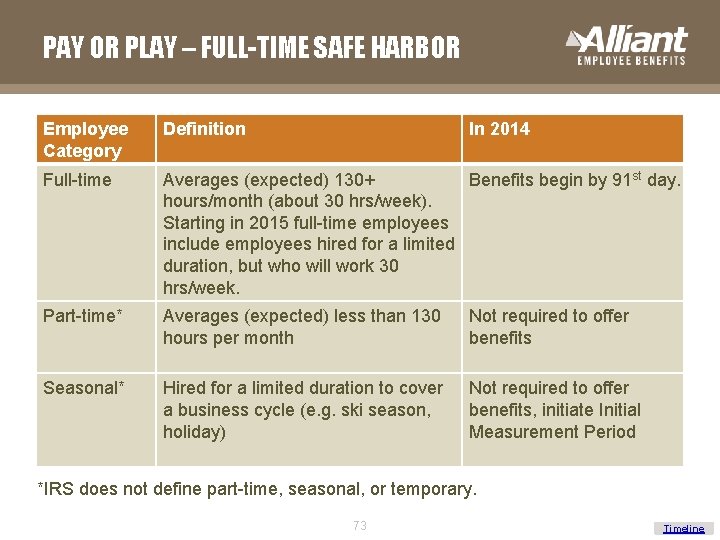
PAY OR PLAY – FULL-TIME SAFE HARBOR Employee Category Definition In 2014 Full-time Averages (expected) 130+ Benefits begin by 91 st day. hours/month (about 30 hrs/week). Starting in 2015 full-time employees include employees hired for a limited duration, but who will work 30 hrs/week. Part-time* Averages (expected) less than 130 hours per month Not required to offer benefits Seasonal* Hired for a limited duration to cover a business cycle (e. g. ski season, holiday) Not required to offer benefits, initiate Initial Measurement Period *IRS does not define part-time, seasonal, or temporary. 73 Timeline
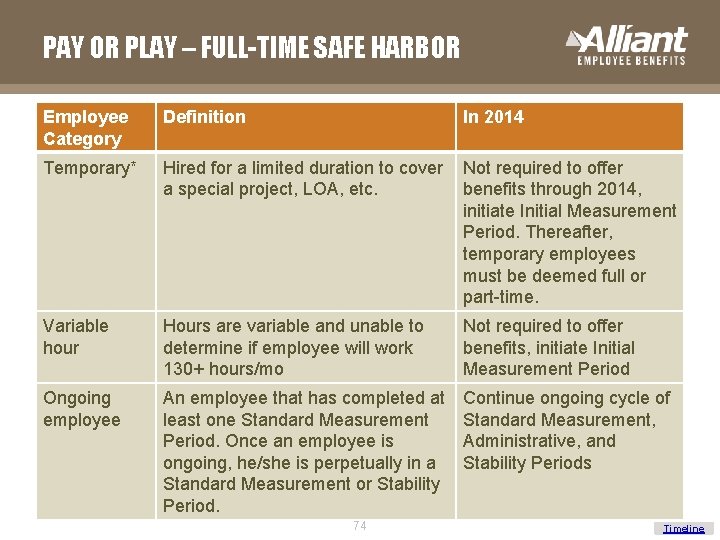
PAY OR PLAY – FULL-TIME SAFE HARBOR Employee Category Definition In 2014 Temporary* Hired for a limited duration to cover a special project, LOA, etc. Not required to offer benefits through 2014, initiate Initial Measurement Period. Thereafter, temporary employees must be deemed full or part-time. Variable hour Hours are variable and unable to determine if employee will work 130+ hours/mo Not required to offer benefits, initiate Initial Measurement Period Ongoing employee An employee that has completed at least one Standard Measurement Period. Once an employee is ongoing, he/she is perpetually in a Standard Measurement or Stability Period. Continue ongoing cycle of Standard Measurement, Administrative, and Stability Periods 74 Timeline
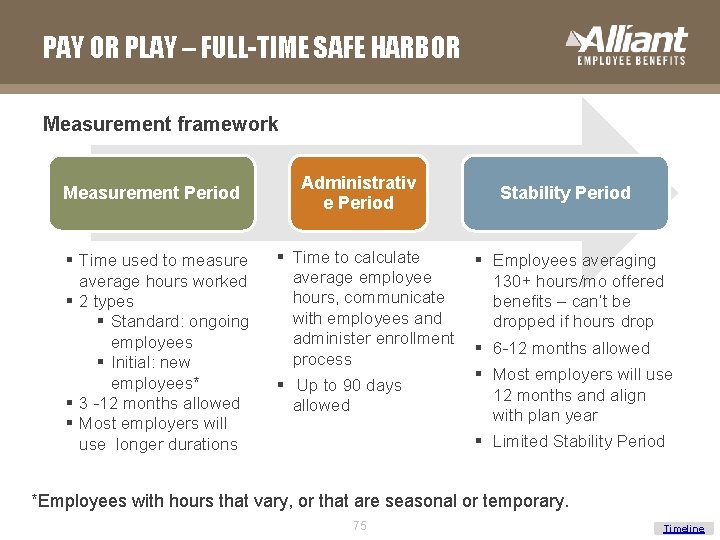

PAY OR PLAY – FULL-TIME SAFE HARBOR Measurement framework Measurement Period § Time used to measure average hours worked § 2 types § Standard: ongoing employees § Initial: new employees* § 3 -12 months allowed § Most employers will use longer durations Administrativ e Period § Time to calculate average employee hours, communicate with employees and administer enrollment process § Up to 90 days allowed Stability Period § Employees averaging 130+ hours/mo offered benefits – can’t be dropped if hours drop § 6 -12 months allowed § Most employers will use 12 months and align with plan year § Limited Stability Period *Employees with hours that vary, or that are seasonal or temporary. 75 Timeline
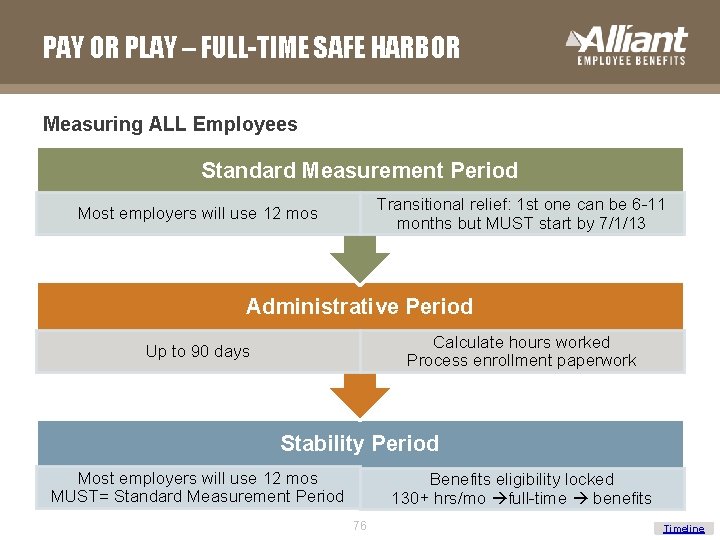
PAY OR PLAY – FULL-TIME SAFE HARBOR Measuring ALL Employees Standard Measurement Period Transitional relief: 1 st one can be 6 -11 months but MUST start by 7/1/13 Most employers will use 12 mos Administrative Period Calculate hours worked Process enrollment paperwork Up to 90 days Stability Period Most employers will use 12 mos MUST= Standard Measurement Period Benefits eligibility locked 130+ hrs/mo full-time benefits 76 Timeline

PAY OR PLAY – FULL-TIME SAFE HARBOR Measuring NEW Variable Hour (<30)/Seasonal Employees Initial Measurement Period (IMP) May start on DOH or 1 st of the Month following/coincident with DOH Most employers will use 11 or 12 mos Initial Measurement Period + Admin Period cannot extend beyond the end of the 13 th month following or coincident with date of hire. Administrative Period Up to 90 days TOTAL May be split before and after IMP or a single period following IMP Calculate hours worked Process enrollment paperwork Stability Period Limited Stability Period Employee is full-time Benefits offered Most employers will use 12 mos MUST= Standard Measurement Period Employee is part-time No benefits Duration = remainder of Stability Period for Ongoing Employees 77 Timeline
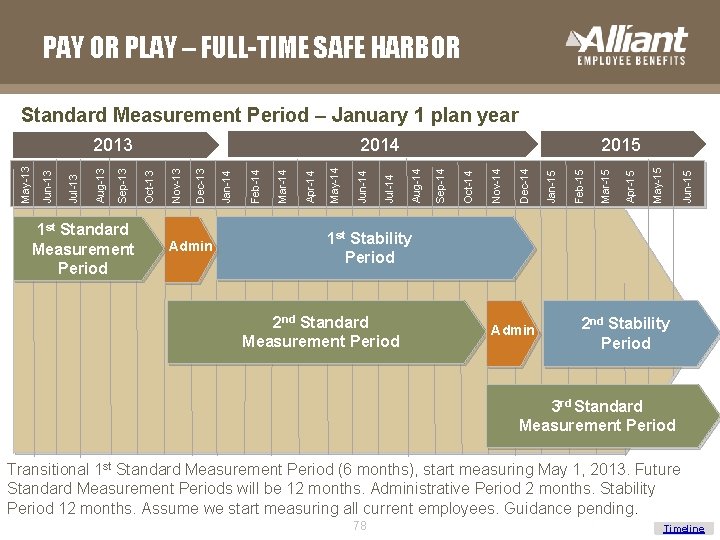
PAY OR PLAY – FULL-TIME SAFE HARBOR Standard Measurement Period – January 1 plan year Admin Jun-15 May-15 Apr-15 Mar-15 Feb-15 Jan-15 Dec-14 Nov-14 Oct-14 Sep-14 Aug-14 Jul-14 Jun-14 May-14 Apr-14 Mar-14 Feb-14 Jan-14 Dec-13 Nov-13 Oct-13 Sep-13 Aug-13 Jul-13 Jun-13 May-13 1 st Standard Measurement Period 2015 2014 2013 1 st Stability Period 2 nd Standard Measurement Period Admin 2 nd Stability Period 3 rd Standard Measurement Period Transitional 1 st Standard Measurement Period (6 months), start measuring May 1, 2013. Future Standard Measurement Periods will be 12 months. Administrative Period 2 months. Stability Period 12 months. Assume we start measuring all current employees. Guidance pending. 78 Timeline
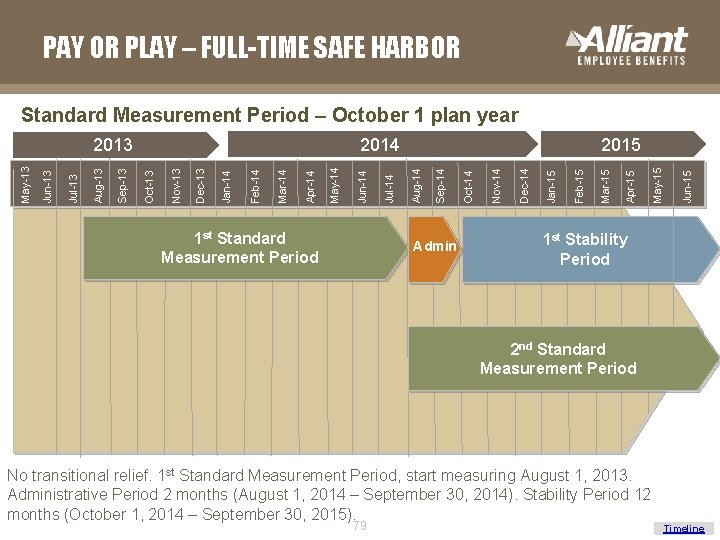
PAY OR PLAY – FULL-TIME SAFE HARBOR Standard Measurement Period – October 1 plan year 1 st Standard Measurement Period Admin Jun-15 May-15 Apr-15 Mar-15 Feb-15 Jan-15 Dec-14 Nov-14 Oct-14 Sep-14 Aug-14 Jul-14 Jun-14 May-14 Apr-14 Mar-14 Feb-14 Jan-14 Dec-13 Nov-13 Oct-13 Sep-13 Aug-13 Jul-13 Jun-13 May-13 2015 2014 2013 1 st Stability Period 2 nd Standard Measurement Period No transitional relief. 1 st Standard Measurement Period, start measuring August 1, 2013. Administrative Period 2 months (August 1, 2014 – September 30, 2014). Stability Period 12 months (October 1, 2014 – September 30, 2015). 79 Timeline
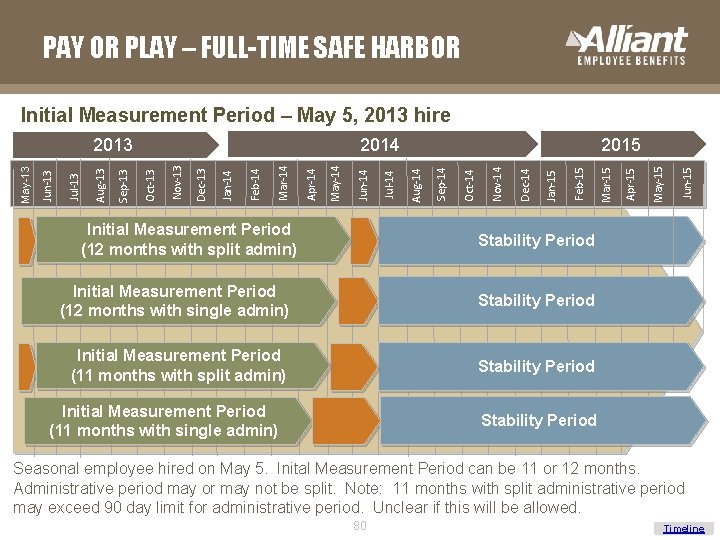
PAY OR PLAY – FULL-TIME SAFE HARBOR Initial Measurement Period – May 5, 2013 hire Initial Measurement Period (12 months with split admin) Jun-15 May-15 Apr-15 Mar-15 Feb-15 Jan-15 Dec-14 Nov-14 Oct-14 Sep-14 Aug-14 Jul-14 Jun-14 May-14 Apr-14 Mar-14 Feb-14 Jan-14 Dec-13 Nov-13 Oct-13 Sep-13 Aug-13 Jul-13 Jun-13 May-13 2015 2014 2013 Stability Period Initial Measurement Period (12 months with single admin) Stability Period Initial Measurement Period (11 months with split admin) Stability Period Initial Measurement Period (11 months with single admin) Stability Period Seasonal employee hired on May 5. Inital Measurement Period can be 11 or 12 months. Administrative period may or may not be split. Note: 11 months with split administrative period may exceed 90 day limit for administrative period. Unclear if this will be allowed. 80 Timeline
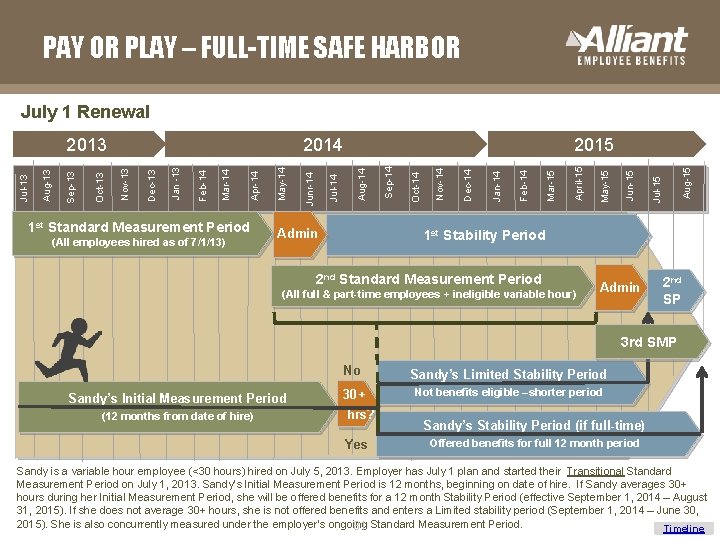
PAY OR PLAY – FULL-TIME SAFE HARBOR July 1 Renewal 1 st Standard Measurement Period (All employees hired as of 7/1/13) Admin Aug-15 Jul-15 Jun-15 May-15 April-15 Mar-15 Feb-14 Jan-14 Dec-14 Nov-14 Oct-14 Sep-14 2015 Aug-14 Jul-14 Junr-14 May-14 Apr-14 Mar-14 Feb-14 Jan -13 Dec-13 2014 Nov-13 Oct-13 Sep-13 Aug-13 Jul-13 2013 1 st Stability Period 2 nd Standard Measurement Period (All full & part-time employees + ineligible variable hour) Admin 2 nd SP 3 rd SMP No Sandy’s Initial Measurement Period (12 months from date of hire) 30+ hrs? Yes Sandy’s Limited Stability Period Not benefits eligible –shorter period Sandy’s Stability Period (if full-time) Offered benefits for full 12 month period Sandy is a variable hour employee (<30 hours) hired on July 5, 2013. Employer has July 1 plan and started their Transitional Standard Measurement Period on July 1, 2013. Sandy‘s Initial Measurement Period is 12 months, beginning on date of hire. If Sandy averages 30+ hours during her Initial Measurement Period, she will be offered benefits for a 12 month Stability Period (effective September 1, 2014 – August 31, 2015). If she does not average 30+ hours, she is not offered benefits and enters a Limited stability period (September 1, 2014 – June 30, 2015). She is also concurrently measured under the employer‘s ongoing 81 Standard Measurement Period. Timeline

PAY OR PLAY – FULL-TIME SAFE HARBOR MNOco Case Study MNOco has a calendar year plan. Like most employers, they are choosing to align their Stability Period with their plan year. We will look at how they measure four different employees during their 1 st Standard Measurement Period. Here are the key dates: § Standard Measurement Period § 2013 Standard Measurement Period: April 16, 2013 – October 15, 2013 (6 months) § Administrative Period: October 16, 2013 – December 31, 2013 § Stability Period: January 1, 2014 – December 31, 2014 § Initial Measurement Period: 11 months from date of hire § Administrative Period: Any portion of month remaining after Initial Measurement Period ends + 2 months § Stability Period: 12 months 82 Timeline
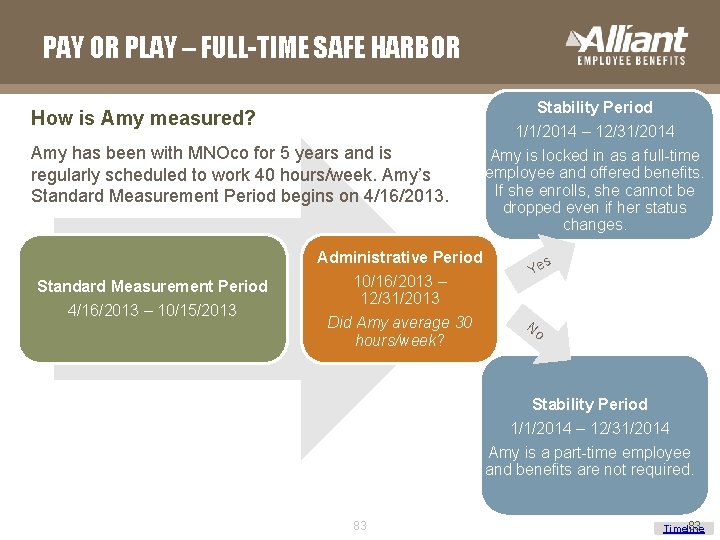
PAY OR PLAY – FULL-TIME SAFE HARBOR Stability Period How is Amy measured? 1/1/2014 – 12/31/2014 Amy has been with MNOco for 5 years and is regularly scheduled to work 40 hours/week. Amy’s Standard Measurement Period begins on 4/16/2013. Standard Measurement Period 4/16/2013 – 10/15/2013 Administrative Period 10/16/2013 – 12/31/2013 Did Amy average 30 hours/week? Amy is locked in as a full-time employee and offered benefits. If she enrolls, she cannot be dropped even if her status changes. s Ye No Stability Period 1/1/2014 – 12/31/2014 Amy is a part-time employee and benefits are not required. 83 83 83 Timeline
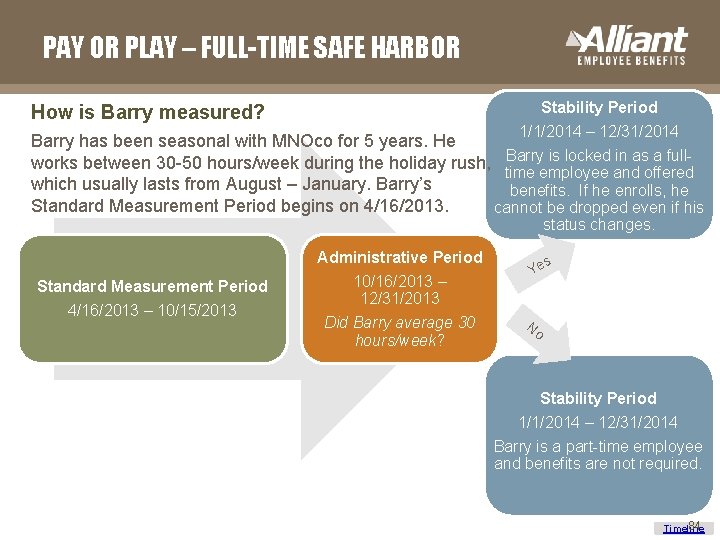
PAY OR PLAY – FULL-TIME SAFE HARBOR Stability Period How is Barry measured? 1/1/2014 – 12/31/2014 Barry has been seasonal with MNOco for 5 years. He works between 30 -50 hours/week during the holiday rush, Barry is locked in as a fulltime employee and offered which usually lasts from August – January. Barry’s benefits. If he enrolls, he Standard Measurement Period begins on 4/16/2013. cannot be dropped even if his status changes. Standard Measurement Period 4/16/2013 – 10/15/2013 Administrative Period 10/16/2013 – 12/31/2013 Did Barry average 30 hours/week? s Ye No Stability Period 1/1/2014 – 12/31/2014 Barry is a part-time employee and benefits are not required. 84 84 Timeline

PAY OR PLAY – FULL-TIME SAFE HARBOR Stability Period How is Chris measured? Chris is a new variable employee hired as of 4/10/2013. He is scheduled to work 32 hours per week. Chris’ Standard Measurement Period begins on 4/16/2013. Standard Measurement Period 4/16/2013 – 10/15/2013 1/1/2014 – 12/31/2014 Chris is locked in as full-time employee and offered benefits. If he enrolls, he cannot be dropped even if his status changes. Administrative Period 10/16/2013 – 12/31/2013 Did Chris average 30 hours/week? s Ye No Stability Period 1/1/2014 – 12/31/2014 Chris is a part-time employee and benefits are not required. This is less clear. We assume that Chris goes through same measurement period as Amy and Barry. 85 Timeline

PAY OR PLAY – FULL-TIME SAFE HARBOR Stability Period How is Debra measured? Debra is a new, variable hour employee who is hired on June 15, 2013, after the Standard Measurement Period begins. Debra’s Initial Measurement Period begins on 6/15/2013. Initial Measurement Period 6/15/2013 – 5/14/2014 Administrative Period 5/15/14 – 7/31/14 Did Debra average 30 hours/week? 8/1/2014 – 7/31/15 Debra is locked in as full-time employee and offered benefits. If she enrolls, she cannot be dropped even if her status changes. s Ye No Stability Period 8/1/2014 – 7/31/15 Debra is a part-time employee and benefits are not required. 86 Timeline
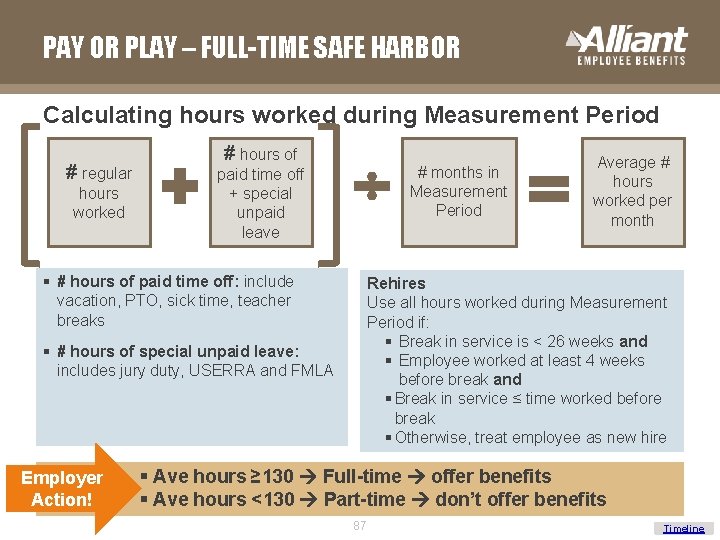
PAY OR PLAY – FULL-TIME SAFE HARBOR Calculating hours worked during Measurement Period # regular hours worked # hours of # months in Measurement Period paid time off + special unpaid leave § # hours of paid time off: include vacation, PTO, sick time, teacher breaks Rehires Use all hours worked during Measurement Period if: § Break in service is < 26 weeks and § Employee worked at least 4 weeks before break and § Break in service ≤ time worked before break § Otherwise, treat employee as new hire § # hours of special unpaid leave: includes jury duty, USERRA and FMLA Employer Action! Average # hours worked per month § Ave hours ≥ 130 Full-time offer benefits § Ave hours <130 Part-time don’t offer benefits 87 Timeline

PAY OR PLAY – FULL-TIME SAFE HARBOR Status change: Measurement Period not completed § Part-time et al. full-time Employees in Initial Measurement Period: Offer benefits by 1 st day of 4 th month (e. g. , change occurs 4/15/14, offer benefits by 8/1/14) § Employees not in Initial Measurement Period: Unclear - Appears no requirement to offer benefits but likely employer would choose to offer § § Full-time part-time et al. § Unclear - likely able to drop benefits and offer COBRA Status change: Measurement Period completed § Part-time et al. full-time § § Employee locked into part-time status for Stability Period. No requirement to offer benefits but likely employer would choose to offer. Full-time part-time et al. § Employee locked into full-time status for Stability Period. Employer cannot drop employee from benefits (unless employment ends. ) 88 Timeline

PAY OR PLAY - DEPENDENTS Dependents Coverage must be offered to dependents ? Penalty Children § Dependents include children under age 26 § Child does not need to be a tax-dependent of the employee § Child coverage does not need to be offered in 2014 as long as employer is taking steps to offer it in 2015 § Grandfathered plans can’t exclude children with access to their own employee sponsored group coverage starting 1 st plan year of 2014 Spouses/domestic partners § Coverage is not required to be offered = $2, 000 x (# full-time employees - 30) Coverage not offered at all OR fail to offer Minimum Essential Coverage to full-time employees and dependents if ONE employee enrolls in subsidized exchange coverage 89 Timeline

PAY OR PLAY - PENALTIES Penalties = $2, 000 x (# full-time employees - 30) Penalty Coverage not offered at all OR fail to offer Minimum Essential Coverage to full-time employees and dependents if ONE employee enrolls in subsidized exchange coverage* = $3, 000 for each employee that enrolls in subsidized exchange coverage if coverage is not Minimum Value or Affordable *This is the maximum combined Pay or Play penalty ? Controlled group entities treated separately for penalties 90 Timeline

WAITING PERIOD – THE 90 DAY RULE What Who When How Penalty Benefits must begin by the 91 st day Applies to group health plans and insurers Plan years beginning on or after January 1, 2014 If an employee is expected to be full-time (130 hrs/month), he/she must be eligible to enroll within 90 days of his/her start date. Note that this 90 -day standard appears to be a true "days passed" standard. § Guidance does not appear to allow an employer to wait until the first of the month after 90 days have passed – seems to require employers to allow mid-month enrollments $100 per day per affected individual 91 Timeline

NO PRE-EXISTING CONDITIONS FOR ALL AGES What Cannot deny coverage based on a pre-existing condition Who Group health plans and insurers When Plan years beginning on or after January 1, 2014 How Penalty No restrictions on plan enrollment or coverage based on a preexisting condition $100 per day per affected individual 92 Timeline

WELLNESS INCENTIVES What Increase premium discount for rewards-based wellness program from 20% to 30% or 50% Who Employers with rewards-based wellness programs When Plan years beginning on or after January 1, 2014 How ? § 30% premium discount allowed for wellness participants § 50% if nicotine cessation included § Reasonable alternative required to qualify for reward where individual did not meet standard § Allow family premium differential IF wellness program allows family participation § Unclear how Affordability factors into premium discount § External review may be required to determine reasonable standard 93 Timeline

CADILLAC TAX What 40% tax on excess premiums Who Insurers and TPAs (assume costs passed onto employers) When 2018 How Penalty § Healthcare premiums >$10, 200/individual and $27, 500/ family are “excessive” § Higher limits for high risk jobs or workforces with older populations Tax = [(Individual premium – premium cap) x 40%] x # singles enrolled + [(Family premium – premium cap) x 40%] x # families enrolled 94 Timeline

NON-DISCRIMINATION TESTING What Plans may not discriminate by giving highly-compensated employees better benefits or premium contributions Who Fully‐insured group health plans When Delayed (until 2014? ) How Penalty GF § Fully‐insured group health plans cannot discriminate in favor of highly compensated individuals - Code Section 105(h)(2) § Assume plans must offer consistent plans, contributions and waiting periods to all eligible employees § Can discriminate in favor of lower paid employees § In effect for self-funded plans – updated guidance expected $100 per day per affected individual 95 Timeline

AUTOMATIC ENROLLMENT What Automatically enroll new full-time employees in group health coverage Who Employers with > 200 full-time employees that a group health plan When Delayed (effective 2015? ) How Penalty § Offer coverage to new full-time employees § Provide ample time for employee to make election § If employee does not enroll or waive coverage § Enroll employee for single coverage in base plan Details pending 96 Timeline

EXCEPTED BENEFITS – DENTAL & VISION There are two separate tests that an employer can use to determine if a dental or vision benefit is an excepted benefit. The tests apply based on the funding arrangement of the plan (i. e. fully-insured or self funded). Fully-insured test To determine if a fully-insured dental or vision plan is an excepted benefit, the plan just needs to meet one test – it needs to be provided by a separate fully-insured contract. EASY Examples: ABCco has medical and vision coverage through Aetna. The vision coverage is imbedded in the medical contract. It is a single contract document. ABCco’s vision plan IS NOT an Excepted Benefit. MNOco has medical and dental coverage through CIGNA. The medical and dental plans have two separate contract documents. MNOco’s dental plan IS an Excepted Benefit. 97 Timeline

EXCEPTED BENEFITS – DENTAL & VISION Self-funded Test To determine if a self-funded dental or vision plan is an excepted benefit the plan must meet two criteria: § Employees must be able to elect the benefit separately (I. e. it is not bundled with another plan such as medical) AND § Employees must contribute to the cost of the coverage. Examples: § DEFco has medical and dental coverage through UMR. The employees medical and dental elections are separate (e. g. the employee can waive medical coverage and enroll in dental coverage). DEFco pays 100% of the employee only dental premium. DEFco’s dental plan IS NOT an Excepted Benefit. § PQRco has medical and dental coverage through HMA. . The employees medical and dental elections are separate (e. g. the employee can waive medical coverage and enroll in dental coverage). Employees contribute $1 per month for employee only dental coverage. PQRco’s dental plan IS an Excepted Benefit. 98 Timeline

AFFORDABLE? 99 Timeline
- Slides: 99