Healthcare for trans and nonbinary Australians comparing primary
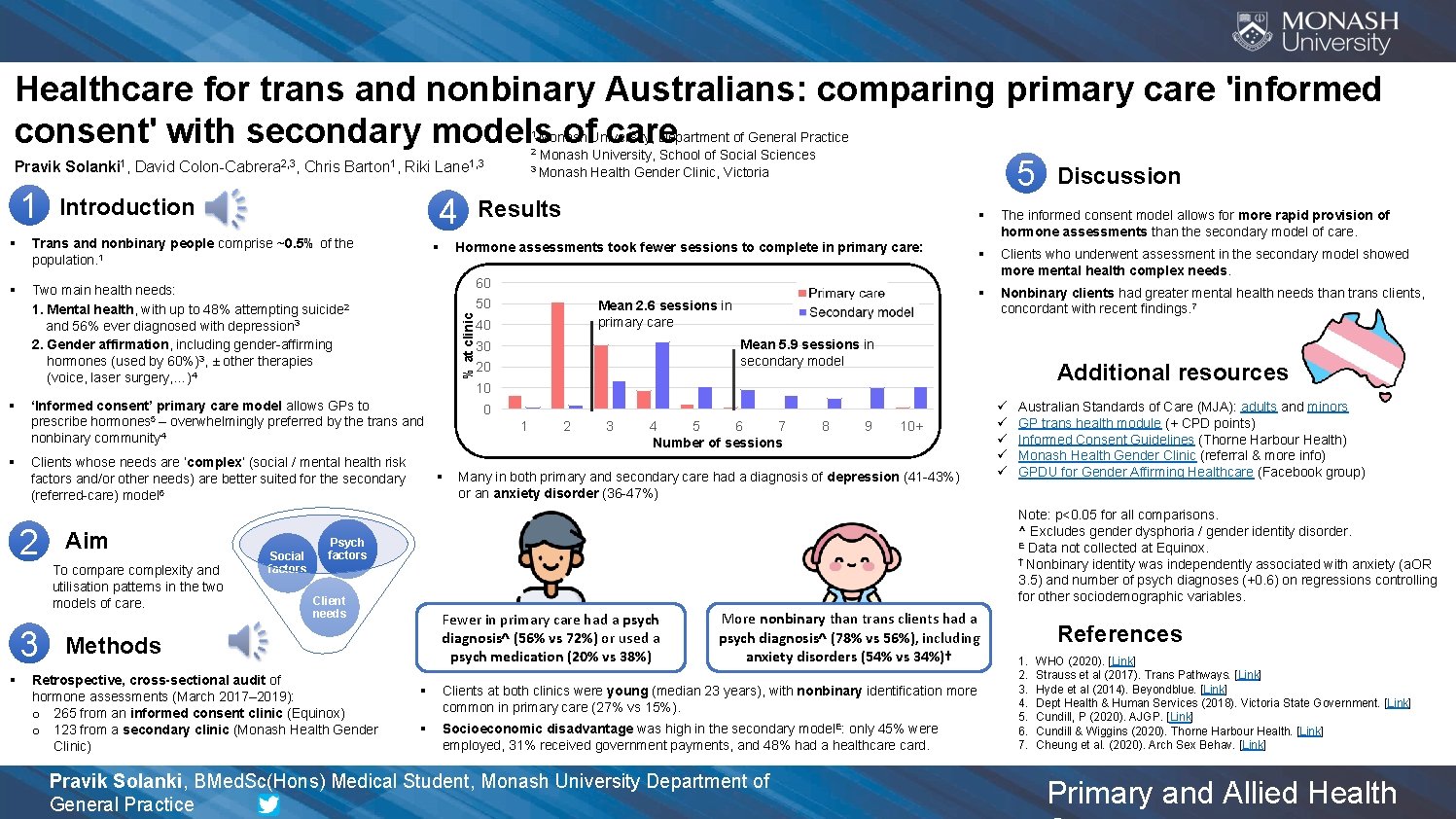
Healthcare for trans and nonbinary Australians: comparing primary care 'informed consent' with secondary models of care Pravik Solanki , David Colon-Cabrera , Chris Barton , Riki Lane 5 Discussion 1 Introduction § 4 Results 1 Monash University, Department of General Practice Monash University, School of Social Sciences 3 Monash Health Gender Clinic, Victoria 2 2, 3 1 § Trans and nonbinary people comprise ~0. 5% of the population. 1 § Two main health needs: 1. Mental health, with up to 48% attempting suicide 2 and 56% ever diagnosed with depression 3 2. Gender affirmation, including gender-affirming hormones (used by 60%)3, ± otherapies (voice, laser surgery, …)4 § § The informed consent model allows for more rapid provision of hormone assessments than the secondary model of care. § Hormone assessments took fewer sessions to complete in primary care: 60 50 Clients whose needs are ‘complex’ (social / mental health risk factors and/or other needs) are better suited for the secondary (referred-care) model 6 Aim To compare complexity and utilisation patterns in the two models of care. 3 Social factors Mean 2. 6 sessions in primary care 40 § Clients who underwent assessment in the secondary model showed more mental health complex needs. § Nonbinary clients had greater mental health needs than trans clients, concordant with recent findings. 7 Mean 5. 9 sessions in secondary model 30 20 Additional resources 10 ‘Informed consent’ primary care model allows GPs to prescribe hormones 5 – overwhelmingly preferred by the trans and nonbinary community 4 2 § 1, 3 % at clinic 1 0 1 § 2 3 4 5 6 7 Number of sessions 8 9 10+ Many in both primary and secondary care had a diagnosis of depression (41 -43%) or an anxiety disorder (36 -47%) Australian Standards of Care (MJA): adults and minors GP trans health module (+ CPD points) Informed Consent Guidelines (Thorne Harbour Health) Monash Health Gender Clinic (referral & more info) GPDU for Gender Affirming Healthcare (Facebook group) Note: p<0. 05 for all comparisons. ^ Excludes gender dysphoria / gender identity disorder. E Data not collected at Equinox. † Nonbinary identity was independently associated with anxiety (a. OR 3. 5) and number of psych diagnoses (+0. 6) on regressions controlling for other sociodemographic variables. Psych factors Client needs Fewer in primary care had a psych diagnosis^ (56% vs 72%) or used a psych medication (20% vs 38%) Methods Retrospective, cross-sectional audit of hormone assessments (March 2017– 2019): o 265 from an informed consent clinic (Equinox) o 123 from a secondary clinic (Monash Health Gender Clinic) ü ü ü More nonbinary than trans clients had a psych diagnosis^ (78% vs 56%), including anxiety disorders (54% vs 34%)† § Clients at both clinics were young (median 23 years), with nonbinary identification more common in primary care (27% vs 15%). § Socioeconomic disadvantage was high in the secondary model. E: only 45% were employed, 31% received government payments, and 48% had a healthcare card. Pravik Solanki, BMed. Sc(Hons) Medical Student, Monash University Department of General Practice References 1. 2. 3. 4. 5. 6. 7. WHO (2020). [Link] Strauss et al (2017). Trans Pathways. [Link] Hyde et al (2014). Beyondblue. [Link] Dept Health & Human Services (2018). Victoria State Government. [Link] Cundill, P (2020). AJGP. [Link] Cundill & Wiggins (2020). Thorne Harbour Health. [Link] Cheung et al. (2020). Arch Sex Behav. [Link] Primary and Allied Health
- Slides: 1