Health systems for UHC a global perspective Presented

Health systems for UHC: a global perspective Presented by: Dr. Naeema H. Al Gasseer & Dr. Denis Porignon WHO Khartoum, January 2017 1|

I. Health Systems, UHC, SDGs 2|

Critical to have the right policies in place Universal entitlement to (essential) health services Adequate funding for health (in particular public) Better use of available funds (efficient, equitable) 3|

What is the health care policy? l Health policy refers to decisions, plans, and actions that are undertaken to achieve specific health care goals within a society. An explicit health policy can achieve several things: it defines a vision for the future which in turn helps to establish targets and points of reference for the short and medium term. l Healthy Public Policy is one of the key health promotion actions. Advancement of Healthy Public Policy requires that the health consequences of policy should be correctly foreseen and that the policy process should be influenced so that those health consequences are considered. 4|

WHO World Health Report 08 – Health System Development – – Revitalisation PHC Universal Access Equity Strengthen Public Health – WHO - Halfdan Mahler – 1978 – WHO - Margret Chan – 2008 5| The Lancet 2008

Health Systems Strengthening and UHC: towards conceptual clarity l HSS is about Instruments l UHC is about Goals (what we do) (what we want) – Equity in service use relative to need, for equity in health goal – Quality improvement, for improving health – Universal financial protection – (and intermediate objectives like equity and efficiency in resource use) 6| – Better mix, distribution and capability of HRH – Investment in effective public health services – Reducing fragmentation – Benefit package specification linked to service delivery strengthening, provider payment incentives, and actions to address demand -side barriers – - systems that is resilient and can respond - IHR

WHO, 2016 A new WHO Framework for UHC as part of the SDGs 7|

Timely - renewed interest for HSS Multi & Bi-laterals WHO G 7 a him S e Is tion a r a 6 cl De y 201 a M 8| Ger m any Hea Sys lthy t Hea ems lthy Li Roa ves dm ap UHC 2030

Health Systems Strengthening is about leveraging domestic resources l The minimum additional investment required in the health sector for countries to attain the SDGs by 2030 amounts US$55 billion per year l Between US$35 -40 billion of these US$ 55 Billion per year must be spent on HSS efforts l In 2013, ODA for funding HSS reached US$ 2. 3 Billion or only 6% of total ODA for health, whereas funding for disease-specific programs (e. g. fighting HIV/AIDS or malaria) amounted to US$34 billion l Even in fragile states, about 75% of total health spending come from domestic sources (95% in middle income countries) l However, in most fragile and low income countries OOP is unacceptably high (50% of THE): domestic resources are not optimally distributed Source: Based on WHO’s work as part of the Lancet Commission Global Health 2035; WHO analyses prepared for the 3 rd Ff. D Conference and HSS roadmap; Institute for Health Metrics and Evaluation (IHME) estimates for 2013 http: //vizhub. healthdata. org/fgh/; WHO Global Health Expenditure Database (GHED) 2013 (http: //apps. who. int/nha/database, accessed 15 February 2016) 9|

Therefore. . l A critical issue is about channelling funding in the right direction l There is a need to bring back governance in the domestic space l There is a need to build or strengthen institutions that will allow this l But one size doesn't fit all. . . => there is a need for a tailored approach 10 |

FIT for purpose… country contexts matters 3 HSS Support Strategies l Strategy 1: Building Health system Foundations in least developed and fragile countries l Strategy 2: Strengthening health system Institutions in least developed countries where foundations are already in place l Strategy 3: Supporting health system Transformation in countries with mature health systems A right combination of “essential investments” (strategy 1) 11 |
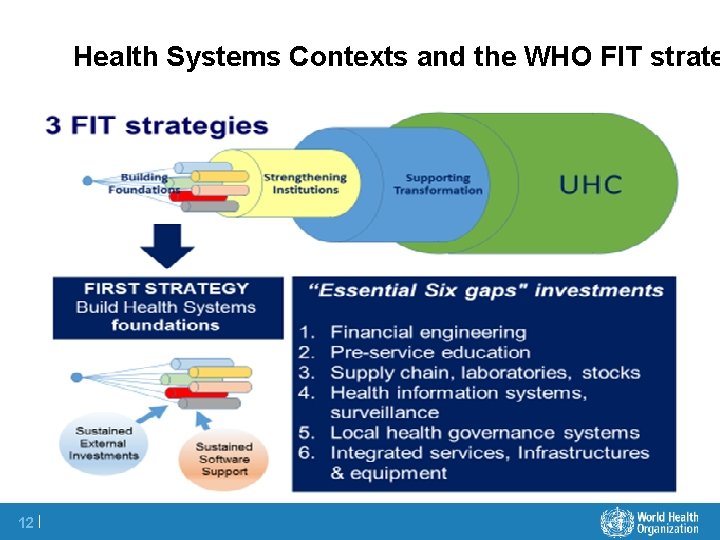
Health Systems Contexts and the WHO FIT strate 12 |
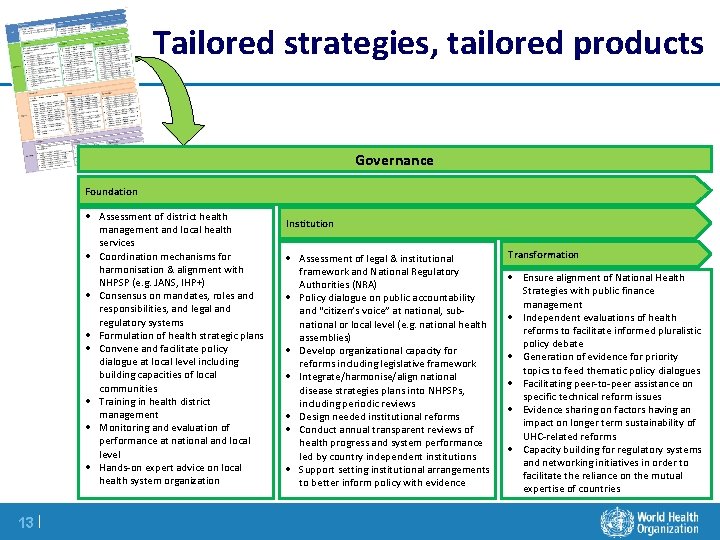
Tailored strategies, tailored products Governance Foundation Assessment of district health management and local health services Coordination mechanisms for harmonisation & alignment with NHPSP (e. g. JANS, IHP+) Consensus on mandates, roles and responsibilities, and legal and regulatory systems Formulation of health strategic plans Convene and facilitate policy dialogue at local level including building capacities of local communities Training in health district management Monitoring and evaluation of performance at national and local level Hands-on expert advice on local health system organization 13 | Institution Assessment of legal & institutional framework and National Regulatory Authorities (NRA) Policy dialogue on public accountability and “citizen’s voice” at national, subnational or local level (e. g. national health assemblies) Develop organizational capacity for reforms including legislative framework Integrate/harmonise/align national disease strategies plans into NHPSPs, including periodic reviews Design needed institutional reforms Conduct annual transparent reviews of health progress and system performance led by country independent institutions Support setting institutional arrangements to better inform policy with evidence Transformation Ensure alignment of National Health Strategies with public finance management Independent evaluations of health reforms to facilitate informed pluralistic policy debate Generation of evidence for priority topics to feed thematic policy dialogues Facilitating peer-to-peer assistance on specific technical reform issues Evidence sharing on factors having an impact on longer term sustainability of UHC-related reforms Capacity building for regulatory systems and networking initiatives in order to facilitate the reliance on the mutual expertise of countries

II. More concretely? 14 |

The EU-Lux/WHO UHC partnership Supporting Policy Dialogue on National Health Policies, Strategies and Plans For Universal Health Coverage 27 countries 2012 -2018 www. uhcpartnership. net 15 |
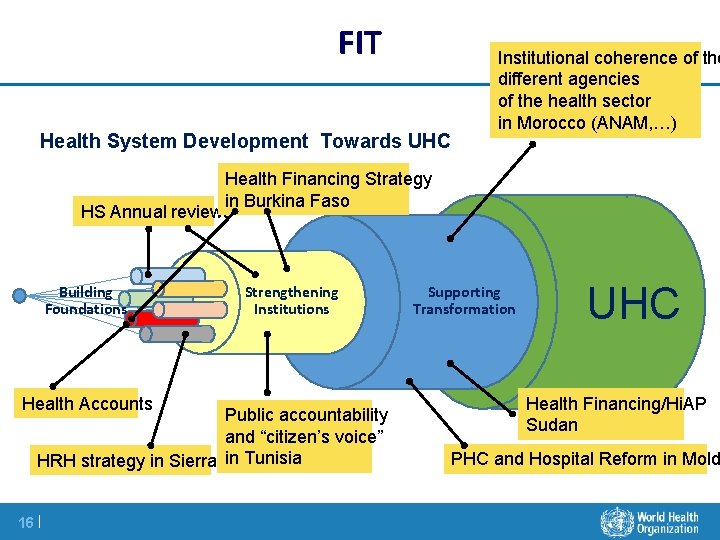
FIT Health System Development Towards UHC Institutional coherence of the different agencies of the health sector in Morocco (ANAM, …) Health Financing Strategy in Burkina Faso HS Annual reviews Building Foundations Health Accounts Strengthening Institutions Public accountability and “citizen’s voice” in Tunisia HRH strategy in Sierra L. 16 | Supporting Transformation UHC Health Financing/Hi. AP Sudan PHC and Hospital Reform in Mold
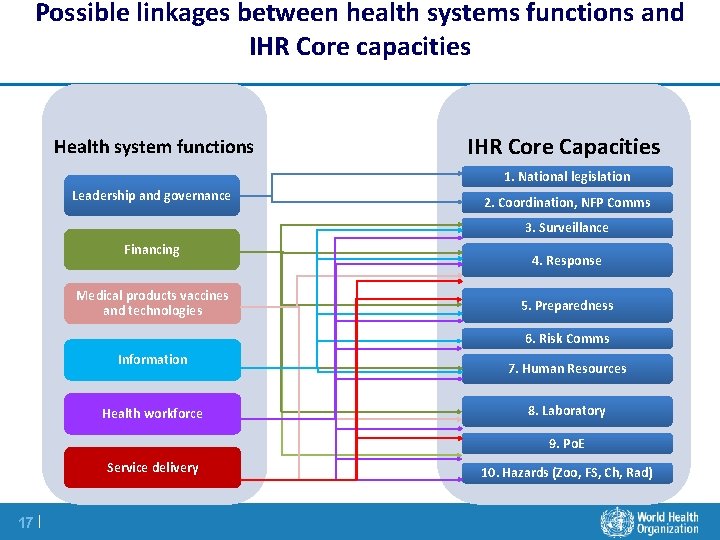
Possible linkages between health systems functions and IHR Core capacities Health system functions IHR Core Capacities 1. National legislation Leadership and governance 2. Coordination, NFP Comms 3. Surveillance Financing Medical products vaccines and technologies 4. Response 5. Preparedness 6. Risk Comms Information Health workforce 7. Human Resources 8. Laboratory 9. Po. E Service delivery 17 | 10. Hazards (Zoo, FS, Ch, Rad)

Beyond UHC : additional objectives for health system (Transformation /not a parallel agenda) l Health security – Individual: protection of individuals against the risk health threats and vulnerabilities; confidence that the services will be available, and of good quality, if needed (UHC as a goal in itself – “can I sleep well at night…” – and not merely instrumental) – Collective: reducing vulnerability of societies to health threats that spread across national borders (beyond UHC) l Health system resilience/ transformation – ability to absorb disturbance, adapt and respond with the provision of needed services – a dynamic objective that cannot be observed at one point in time 18 |
Monitoring and measuring health determinants/barriers to improve health and access to health services Monitoring Health in All Policies Social determinants impacts on health equity What factors in broader society are impacting health equity, and what is being done to address this? | 1919 | Monitoring intersectoral factors influencing univeral health coverage Social determinants impact on coverage inequalities What factors in broader society are contributing to incomplete coverage of health services, and what is being done to address this? Monitoring health status and coverage Health outcomes for health status or coverage by socioeconomic position How large are health inequalities between social groups?

A National Health Service… National Institute for Health “…to secure equal access to comprehensive health and healthcare for every individual across the country regardless of their ability to pay” N Bevan, 1946 [Largest Social Engineering of its time] Professor S Rawaf 21 | © WHO C Centre, Imperial College London
- Slides: 20