Health Services Delivery Framework Focus Area 1 Adults



















- Slides: 24

Health Services Delivery Framework Focus Area 1: Adults Receiving Care in Community Settings For Information Only

Presentation Objectives • Discuss the key recommendations in the Palliative Care Health Services Delivery Framework (Delivery Framework) Focus Area 1: Adults Receiving Care in Community Settings. • Describe the starting point for implementation, and how available Ontario Palliative Care Network tools can support change. 2

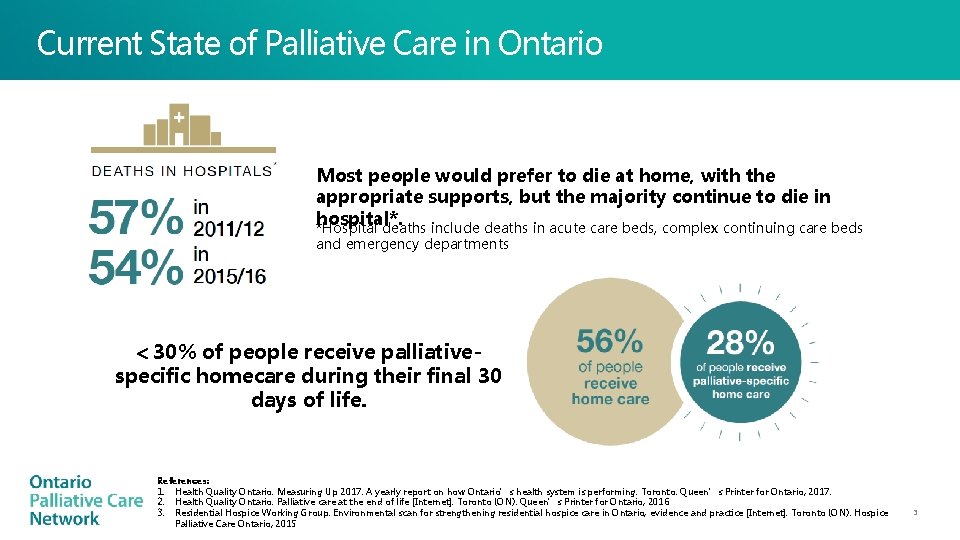
Current State of Palliative Care in Ontario Most people would prefer to die at home, with the appropriate supports, but the majority continue to die in hospital*. *Hospital deaths include deaths in acute care beds, complex continuing care beds and emergency departments 30% of people receive palliativespecific homecare during their final 30 days of life. References: 1. Health Quality Ontario. Measuring Up 2017: A yearly report on how Ontario’s health system is performing. Toronto: Queen’s Printer for Ontario; 2017. 2. Health Quality Ontario. Palliative care at the end of life [Internet]. Toronto (ON): Queen’s Printer for Ontario; 2016 3. Residential Hospice Working Group. Environmental scan for strengthening residential hospice care in Ontario, evidence and practice [Internet]. Toronto (ON): Hospice Palliative Care Ontario; 2015 3

Why Ontario Needs Palliative Models of Care For patients with a life-limiting illness and their family/caregivers : • They are not receiving palliative care where and when they need it. • They have uncontrolled pain and symptoms, distress, and poor quality of life. For Health Care Providers : • There are gaps in palliative care education and training for health care providers. • The palliative care competencies needed by different types of care providers are not clear. For the Health System : • There is no roadmap to guide the scale and spread of models that deliver good palliative care. • There are too many avoidable hospitalizations and emergency department visits. The Goal: To create a model of care with a first focus on care for adults with a progressive, life-limiting illness who live in the community. 4

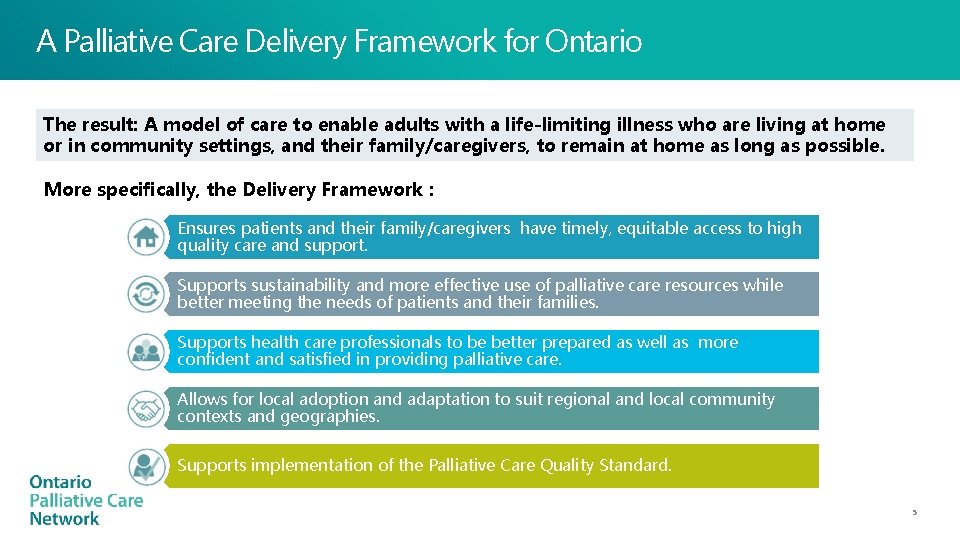
A Palliative Care Delivery Framework for Ontario The result: A model of care to enable adults with a life-limiting illness who are living at home or in community settings, and their family/caregivers, to remain at home as long as possible. More specifically, the Delivery Framework : Ensures patients and their family/caregivers have timely, equitable access to high quality care and support. Supports sustainability and more effective use of palliative care resources while better meeting the needs of patients and their families. Supports health care professionals to be better prepared as well as more confident and satisfied in providing palliative care. Allows for local adoption and adaptation to suit regional and local community contexts and geographies. Supports implementation of the Palliative Care Quality Standard. 5

Process for the Delivery Framework Recommendations Development Established a Provincial Working Group • Healthcare providers and administrators, patient & family caregiver representatives • 18 month effort Examined Best Practice and Research System-Wide Engagement • An achievement of the whole system, not just OPCN Unanimous endorsement by OPCN partners • CCO, LHINs, Health Quality Ontario, Quality Hospice Palliative Care Coalition of Ontario 6

This model will enable patients to remain at home as long as possible through: • Seamless 24/7 access to high quality person-centred care and supports. • An Interdisciplinary Care Team having access to relevant and up -to-date patient information. Patient and Family/Caregiver • Engaging patients/caregivers as active members of the care team, with care decisions aligned to the patient’s specific goals and wishes. • Tailored recommendations for Francophones, First Nation, Inuit, Métis and urban Indigenous peoples, homeless and vulnerably housed populations, and people living in long-term care homes. 7

Enabling Access to an Interdisciplinary Palliative Care Team The model of care describes “team” from a patient (or family/ caregiver) perspective and matches how they want to receive care from an Interdisciplinary Palliative Care Team Patient and Family/Caregiver The interdisciplinary palliative care team: • Includes a core team of a physician or nurse practitioner and a designated care coordinator and, often, a nurse • Often includes other interdisciplinary providers (extended services) • Have an established connection with palliative care specialist(s) for consult with team members and providing direct patient care as needed The Delivery Framework also recommends that providers have access to palliative care expertise 24/7 to support decision-making and clinical practice. 8

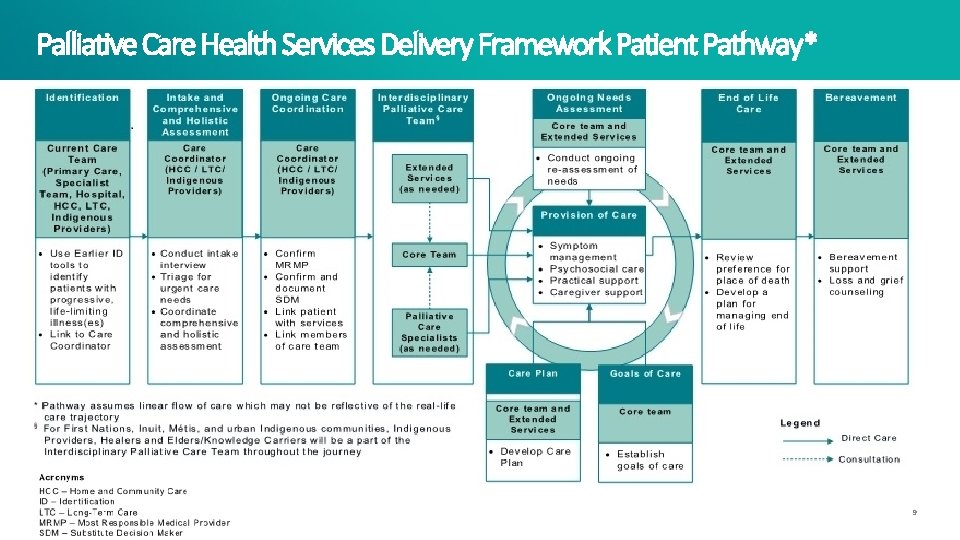
Palliative Care Health Services Delivery Framework Patient Pathway* 9

Prioritized Recommendations for Implementation With input from the 14 Regional Palliative Care Networks/LHINs, the following recommendations have been prioritized as a starting point for teams to implement the Delivery Framework recommendations. Recommendation 1: The patient who would benefit from palliative care will be identified early in their illness. 2 Foundational Elements Recommendation 2: At any point from when the patient’s illness is identified through end-oflife and bereavement, there will always be a designated care coordinator. Recommendation 3: All patients and family/caregivers will have 24/7 access to an interdisciplinary palliative care team. 6 System Gaps Recommendation 6: The patient and their family will have access to emotional, psychological and spiritual care to address their needs in a culturally safe manner. Recommendation 7: The patient and their family/caregivers will have access to practical and social supports that addresses their needs in a culturally safe manner. To provide more clarity on these broad recommendation areas, selected subrecommendations accompany each prioritized recommendation (see Appendix). 10

New Tools to Implement Delivery Framework and Improve Palliative Care In parallel with the Delivery Framework, OPCN has created ready-to-use tools and resources to enable implementation. • These tools address known gaps in palliative care (identified by palliative care providers, patients and families/caregivers) and support implementation of the Delivery Framework. 1. Better Conversations Four resources to enable better provider-patient conversations about goals of care. 2. Early Identification Tools to support earlier identification of patients who would benefit from a palliative approach to care. 3. Competencies for Providers A comprehensive guide to palliative care competencies required for every type of care provider, from specialists to volunteers. 11

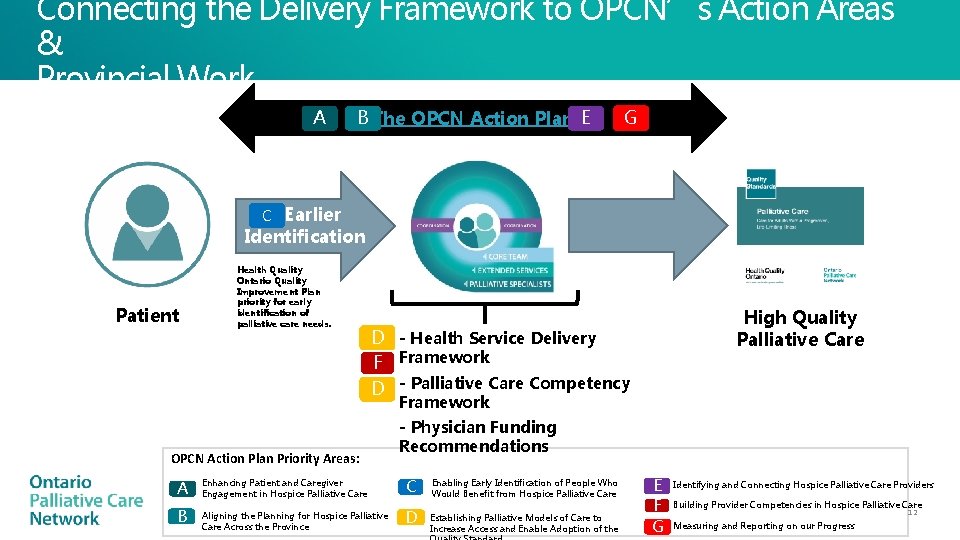
Connecting the Delivery Framework to OPCN’s Action Areas & Provincial Work A B The OPCN Action Plan E G C Earlier Identification Patient Health Quality Ontario Quality Improvement Plan priority for early identification of palliative care needs. High Quality Palliative Care D - Health Service Delivery F Framework D - Palliative Care Competency Framework OPCN Action Plan Priority Areas: A B - Physician Funding Recommendations Enhancing Patient and Caregiver Engagement in Hospice Palliative Care C Aligning the Planning for Hospice Palliative Care Across the Province D Enabling Early Identification of People Who Would Benefit from Hospice Palliative Care Establishing Palliative Models of Care to Increase Access and Enable Adoption of the E F G Identifying and Connecting Hospice Palliative Care Providers Building Provider Competencies in Hospice Palliative Care 12 Measuring and Reporting on our Progress

Working Together to Make the Delivery Framework a Reality in Ontario Provincial implementation will be flexible to allow for adaptation, and adoption based on local priorities and resource availability. • The model is not a new start, rather a framework to guide ongoing palliative care system improvements and alignment at provincial, regional and local geography. 13

OPCN Next Steps In collaboration with Regional Palliative Care Networks and other key stakeholders: • Determine the plans for a current state and readiness assessment against the 5 priority areas. • Determine an evaluation strategy to measure the impact of the Delivery Framework on the health system, participating organizations and patients/families/caregivers. • Understand available levers, funding requirements, and areas where legislation/policy changes are needed based on the data collected. • Work with provincial partners and identify opportunities and existing initiatives to implement OPCN recommendations. 14

Thank you!

Appendix

Priority Sub-Recommendations Recommendation 1: The patient who would benefit from palliative care will be identified early on in the trajectory of their illness. 1. 1 All members of the patient’s current care team (primary care, hospital team, home and community care providers, etc. ) will use the approaches and tools as recommended by the OPCN Working Group on Early Identification to identify patients and families’ need for palliative care. 1. 2 The current care team will connect the patient and the family/caregiver with a Care Coordinator for intake. This will be communicated with the patient’s family physician when someone other than the family physician has identified that the patient would benefit from palliative care. 17

Priority Sub-Recommendations Recommendation 2: At any point during the patient and family/caregiver journey, from identification to end-of-life and bereavement, there will always be a designated Care Coordinator. 2. 1. After the referral from the patient’s current care team, a Care Coordinator will be assigned to each patient and their family/caregiver. This designated Care Coordinator will be the central point of contact with services and resources and the patient and family/caregiver’s advocate. 2. 2. The Care Coordinator will conduct an intake interview to triage for any palliative care needs that require urgent interventions (e. g. uncontrolled physical symptoms or urgent needs for personal care services or social work services) and will connect the patient and family/caregiver with the appropriate service (e. g. family physician, ambulatory symptom management clinic, community nursing, personal support worker (PSW)). 2. 4. Following the intake interview, the Care Coordinator will ensure that a comprehensive and holistic assessment of the health, social, and emotional needs of the patient and family/caregiver is completed collaboratively between the members of the team. 2. 6. If day-to-day care and practical supports are not required at the time of comprehensive assessment, the patient will remain on the coordinator’s caseload for case management only. The patient and family/caregiver will be contacted by the Care Coordinator at regular intervals to identify whether the patient and/or family’s needs have changed. 18

Priority Sub-Recommendations Recommendation 3: All patients and family will have 24/7 access to an inter-disciplinary palliative care team. 3. 1 All patients will have a Core Team of health care providers. The Core Team is responsible for providing direct, day-to-day support for the patient and family/caregiver, identifying their care needs and connecting them with appropriate services. This Core Team will include, a designated Care Coordinator and a most responsible medical professional (MRMP). In cases when the patient has day-to-day needs, the Core Team may also include a nurse (registered nurse (RN) or registered practical nurse (RPN)). All members of the Core Team will have at least primary level competency in palliative care. 3. 2 The Care Coordinator, after having conversations with the patient’s primary care provider and or/the specialist currently involved in care, and after considering the patient’s needs and preferences, identifies the MRMP. The MRMP may be: an NP or an MD (e. g. family physician/NP, disease specific specialist physician/NP, palliative care specialist). 3. 3 As patient and family/caregiver needs increase and/or change overtime, the Core Team will engage Extended Services to address these changing needs. 3. 9 The patient and family will have access to the Core Team or on-call system for the Core Team 24/7. While during the daytime, the central point of contact may be the Care Coordinator, after hours and on weekends, if the Core Team has a designated nurse, they will be the first point of contact. The nurse will assess the urgency of needs of the patient and family/caregiver, will address the needs or will connect the patient and family/caregiver with the MRMP or the individual oncall for the MRMP. Virtual and other technologies will be used to improve access to care particularly in in rural and remote locations. 3. 10 Every Core Team will be supported by Palliative Care Specialists who will be available 24/7 to provide support and consultation to the MRMP in-person or via telephone or other technologies (e. g. telemedicine, virtual care, secure electronic communication). 19

Priority Sub-Recommendations Recommendation 6: Patients and the family will have access to emotional, psychological and spiritual care that addresses their needs in a culturally safe manner. 6. 1 The core team will regularly assess psychological and emotional needs of the patient (e. g. fear, anxiety, and depression) in a culturally safe manner. The core team may need support from other providers to effectively manage the needs of the patient/family’, and may engage social work, spiritual care, and hospice providers. 6. 3 The Core Team may need support from other providers to effectively manage the needs of the patient/family. This may include members of the Extended Team (e. g. social work, trained volunteers, Indigenous Providers, and hospice) or when the patient or family’s needs are more extensive or complex, the Care Coordinator will ensure referrals are made to providers with expertise in psychosocial care (e. g. social work with expertise in palliative care, grief counsellors, mental health professionals, Recommendation 7: Members of the Core Team will regularly assess and identify the practical and social needs of the patient and family/caregiver. 7. 1. The Core Team and providers of Extended Services will regularly assess the activities of daily living (ADL) and instrumental activities of daily living (IADL) of the patient and communicate with the Care Coordinator. Extended Service providers such as PSW, PT, OT, social worker and others will be engaged as needed to provide practical support. 20

Mandate of the Ontario Palliative Care Network (OPCN) An organized partnership of community stakeholders, health service providers and health systems planners. Be a principal advisor to government for quality, coordinated, hospice palliative care in Ontario Be accountable for quality improvement initiatives, data and performance measurement and system level coordination of hospice palliative care in Ontario Support regional implementation of high-quality, high-value hospice palliative care 21

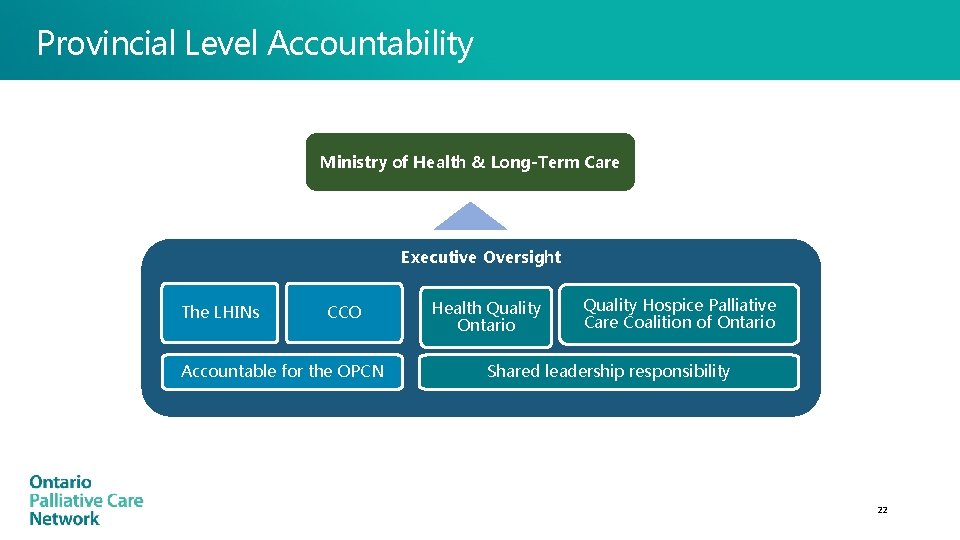
Provincial Level Accountability Ministry of Health & Long-Term Care Executive Oversight The LHINs CCO Accountable for the OPCN Health Quality Ontario Quality Hospice Palliative Care Coalition of Ontario Shared leadership responsibility 22

Development of the OPCN Action Plan 1: 2017 – 2020 Improving System Level Measures and Targets by focusing on patients remaining at home with the appropriate supports and reducing acute care utilization. 1 % of caregivers of decedents who received palliative care services who were invited to respond to a Caregiver. Voice survey 2 % of community dwelling decedents who received physician home visit(s) and/or palliative home care in the last 90 days of life 3 % of decedents who had a) 1 or more ED visits or b) 2 or more ED visits in the last 30 days of life 4 % of decedents who died in hospital* * Other locations of death will continue be reported, but are not system level measures 23

Specific action areas identified in the Action Plan A • Enhancing Patient and Caregiver Engagement in Hospice Palliative Care B • Aligning the Planning for Hospice Palliative Care Across the Province C • Enabling Early Identification of People Who Would Benefit from Hospice Palliative Care D • Establishing Palliative Models of Care to Increase Access and Enable Adoption of the Quality Standard E • Identifying and Connecting Hospice Palliative Care Providers F • Building Provider Competencies in Hospice Palliative Care G • Measuring and Reporting on our Progress 24