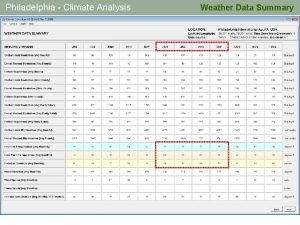
Health Promotion Council Philadelphia Department of Public Health

Health Promotion Council Philadelphia Department of Public Health Department of Family and Community Medicine Office to Advance Population Health Department of Medicine – Division of Genetic and Preventive Medicine Thomas Jefferson University and Hospital SHAPE IT is a joint project with Thomas Jefferson University Hospital, Health Promotion Council and The Philadelphia Department of Public Health. This project is funded, in part, under a contract with the Pennsylvania Department of Health. Basic data for use in this study were supplied by the Pennsylvania Department of Health, Harrisburg, Pennsylvania. The Department specially disclaims responsibility for any analyses, interpretations or conclusions.

n OAPH n – James Plumb MD, MPH – Rickie Brawer MPH, Ph. D – David Madison M. Ed n – – DFCM – – – Michael Rosenthal MD James Diamond Ph. D Fiona Choury BS Health Promotion Council n Vanessaa Briggs MBA Tineesha Peterson MPH Sterlen Barr BS Joseph Woodlock BA Behavioral Medicine – Ron Meyers Ph. D – Audrey Berry MSN n PDPH – Joan Beckwith MD Thanks to Bob Groves MPH

Objectives n Identify – factors related to planning, developing and implementing a comprehensive Community Action Plan designed to increase knowledge, change attitudes, modify behaviors and support a social change process related to hypertension, stroke and prostate cancer prevention in African American men n Describe – individual attitudes, beliefs, behaviors and barriers/opportunities/ assets related to education, prevention, and compliance with treatment and screening recommendations.

Background n n Pennsylvania State Disparities Project Philadelphia and Pittsburgh 2. 5 years Focus – AA men age 35+ - mortality from stroke and prostate cancer – RFP n – Utilization of State Health Improvement Partnerships – Emphasis on Community Engagement and Planning in all project aspects In Philadelphia n Zip codes – 19104, 19121, 19122, 19123, 19132, 19133, 19139, 19143, 10140 (West and North Philadelphia) n 25% of ~ 27, 000 men
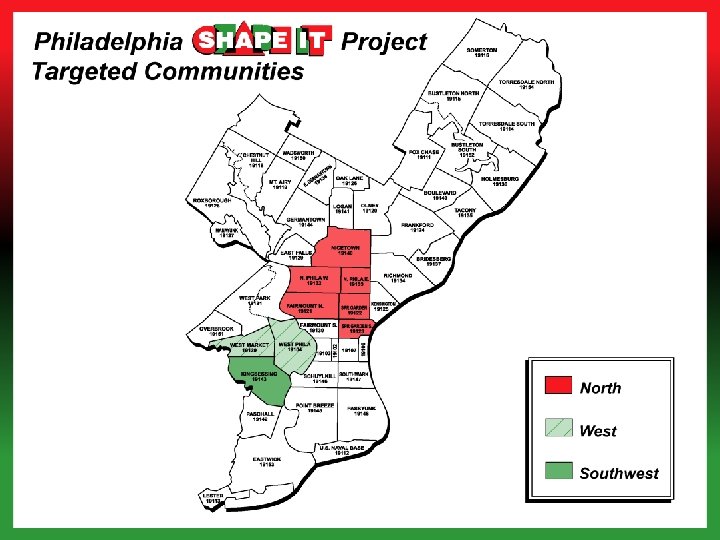

Project Goal and SHAPEIT Aims n State - Reduce the incidence of stroke and mortality from prostate cancer n Philadelphia – Aims – Reach 25% of target population of 27, 000 African American men age 35+ – Use shared responsibility model of community health planning – Develop multiple strategies that are seen by target population as relevant – Direct these strategies towards 2 different health conditions that require different types of decision-making and behavior change

Partners n n Health Promotion Council of Southeastern PA Philadelphia Department of Public Health Office to Advance Population Health and Department of Family and Community Medicine Department of Medicine - Division of Genetic and Preventive Medicine n n n Nicetown-Tioga and Haddington Community Health Initiatives The Village of the Arts and Humanities Project H. O. M. E. American Cancer Society Multiple community outreach sites in West and North Philadelphia

Prostate Cancer - Rates n n In Pennsylvania (2001)– AA – Incidence 252. 2; Whites – 158. 0/100, 000; Mortality – 63. 9 AA; 27. 8/100, 000 (HP 2010 – 28. 8) In Philadelphia – – Age adjusted incidence rate for AA men 481. 4/100, 000 compared to State rate of 252. 2 for AA men and 158 for White men – (1997 -2001) death rates – AA – 71/100, 000 (132/year); White – 27. 7/100, 000 (106/year)
Stroke - Rates In US – Risk for Stroke Mortality – AA vs. White by ages – 35 -44 (4. 0), 45 -54 (3. 9), 55 -64 (3. 0), 65 -74 (1. 9), 75 -84 (1. 2), 85+ (0. 9) n Stroke Death rates (age 35+ and older) n – Pennsylvania – AA – 161; White 118/100, 000 – Philadelphia – AA – 166; White 122/100, 000 – Not broken down by age

Characteristics of Black Men Living in Target Areas n n n More likely to be unemployed, live in poverty and have less formal education More likely to have regular source of care and have seen PCP in last year Men aged 40 -49 twice as likely not to fill prescription due to cost Men aged 40 -59 more likely to have a stroke More likely to report extreme stress Philadelphia Health Management Corporation Household Health Survey, 2004
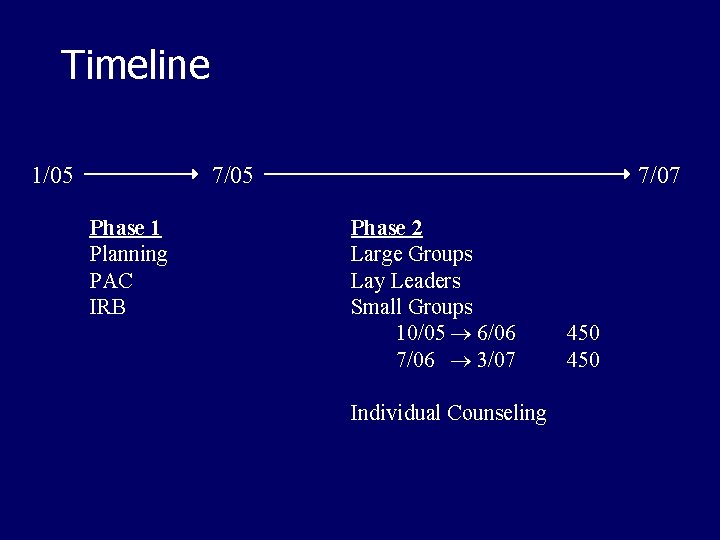

Timeline 1/05 7/05 Phase 1 Planning PAC IRB 7/07 Phase 2 Large Groups Lay Leaders Small Groups 10/05 6/06 7/06 3/07 Individual Counseling 450

Goals of Project Year 1 Establish Project Advisory Council n Conduct Focus Groups and Key Informant Interviews n Develop a Community Action Plan and tools for implementation n

Project Advisory Council n Consists of 25 members n Two Co-Chairs (one woman) act as liaisons between the PAC and the Project Team Monthly meetings + calls with Co-Chairs Provide guidance to the Project Team during program development, implementation and evaluation 17 meetings n n n – community and organizational representatives, men with hypertension and prostate cancer survivors

Program Planning Methodology Literature Review n PHMC Household Health Survey Data 2004 n Focus Groups n Key Informant Surveys n

Assessment of Community and Individual Beliefs, Assets and Needs n n 5 focus groups (57 participants) with men with and without hypertension, men with prostate cancer, men from the general population, and social support networks of men 15 key informant interviews representing 11 disciplines (Family Medicine, Internal Medicine, Neurology, Health Educators, Cancer Patient Educator, ACS, Philadelphia Stroke Council, Stroke Educator, Drug and Alcohol Counselor, Registered Dietitian, Cancer Survivor and ACS volunteer)

Hypertension/Stroke Risk Factors: Focus groups and Key Informant Surveys n n n n “ Being Black in White America” Diet – salt (internal stress due to racism over time) Overweight “I know high blood pressure runs in Lack of knowledge my family, but I eat what I Heredity (being African want…I just hope I’ll be the one American) that it skips”. Stress (where you live, job, “Men don’t associate obesity, smoking, lipids, or lack of relationships- women, exercise with preventing racism) hypertension. They do not Elevated cholesterol see relationship of Age hypertension and its risk factors to stroke prevention. “Lack information about how it occurs – if you don’t know you can’t prevent it”

High Blood Pressure Symptoms and Stroke Causes and Symptoms n n n High BP symptoms: red “High blood pressure can be finger tips, sweating, prevented…I don’t know about irritability/ mood changes, stroke”. facial tics, headaches, “Numbness went away, so I never blurred vision, nose bleeds, went back” (don’t link symptom no symptoms to stroke). Stroke Symptoms: “For many of my young (under 40) numbness, cramp up, African American stroke patients tingling in finger tips, the first time they find out they slurred speech , muscle have hypertension is when they weakness, sweating have a stroke. Or they know Stroke causes: lack of they have hypertension and it’s oxygen to brain, high not controlled (can’t afford meds cholesterol, heredity, stress, or are not taking). Major blood clot, drinking, nervous reasons for stroke are related to system out of wack, uncontrolled BP and cocaine clogged arteries use. ”

Attitudes and Beliefs about Hypertension and Stroke “My grandfather was n n n Strokes happen to older people not younger people Believe high blood pressure is serious but don’t take seriously due to lack of symptoms. Don’t link to stroke Fear stroke – paralysis Can’t prevent stroke (fatalism); or to prevent stroke don’t drink alcohol or take drugs No need to make changes – doctors/medicines can cure you healthy…he walked 8 miles a day and he was hit with a stroke out of the blue – If it’s gonna come , it’s gonna come”. “If you take medications then you don’t have to worry, nothing will happen – you don’t need to make (lifestyle) changes or get checked” “If someone has a stroke they don’t talk about it…fear of stigma at work…people who have minor stroke blend into community”.

Attitudes and Beliefs about Hypertension and Stroke n n BP medications cause impotence, make you tired May not understand concept of chronic disease “ Men need to know other treatment options. Need to promote that impotence can be treated with Viagra and other drugs, but if you have a heart attack or stroke then you can no longer take Viagra” “If meds make the patient tired then he may not take if he has multiple jobs…” “Patients may stop taking meds when the prescription runs out –may not realize that he needs to take them the rest of of his life. ” “I make changes when the doctor suggest it, but when I feel better I go back to the old ways”.

Prostate Cancer n Men and women know little about prostate and prostate cancer (where prostate gland is, how it works, etc) n Some young men more worried about prostate cancer than about elevated blood pressure (over anxious) while other men who have witnessed a family member or friend with prostate cancer may deny symptoms n Prostate cancer feared more than stroke or heart attack n Confusion about screening criteria and what the PSA numbers mean

Prostate Cancer Risk Factors n n n n n Lack of circumcision Heavy work/ construction/lifting straining Tight clothing; too much pressure causes it to swell Sex (too much; too little) Age Diet Stress Heredity Hemorrhoids Smoking n “Many men don’t know family history or believe that if it doesn’t run in family then they are not at risk. Some men only consider hereditary risk from their father’s family only; don’t consider mother’s side of family in terms of hereditary prostate cancer risk. ”

Prevention of Prostate Cancer n n n n n Can’t prevent – early detection is best Castor oil and tea Vitamins (bottle says vitamins can reduce prostate cancer risk) Fasting Regular bowel movement Rest Exercise Keep system clean; drink lots of water Don’t smoke Regular check-ups

Prostate Cancer Attitudes and Beliefs n n n “Those not exposed to prostate cancer information have Fatalism - cancer is a knowledge couched in death sentence; superstition. Some men believe therefore, why get that if you have surgery then the cancer is exposed to air and screened will spread”. Some men not sure if “Some men believe prostate checked for prostate or cancer can be sexually transmitted to wife” colon cancer “I don’t know if I’m at risk but cancer Denial- “What I don’t to me is scary and I pray to God I don’t have it. I think I’m at risk know won’t hurt me”. because I’m a black man…and you Fear digital rectal exam should get it checked at age 40. And my father and grandfather died Fear erectile from it…I would like to be tested dysfunction but I fear doctors and I don’t want anything going in there…” Fear of screening

Barriers to Prostate Cancer Screening n n n Lack of insurance Lack of knowledge Digital rectal exam concerns Male pride Fear of screening outcome and treatment (impotence; incontinen ce) Lack of family communication about health history “I was afraid of the outcome, a lot of men are too macho to get this thing done and feel that they will come out of the doctor’s office and be called gay. My son feels that this is his space and if anyone touches you there that they are violating him. I had to tell my son that there are certain procedures that doctors have to do that are good for you” “Backside territory is mine, raised not to let folks go there…” “It’s hard to let a man get behind me and ring the doorbell…” “Men fear treatment – see as mutilation/ castration. Black men are not aware of new treatments. They need to know their treatment options (at the time of screening)”.

Other Barriers to Care and Treatment n Trust Issues: lack of trust of health care providers, information and medical system – Historically African Americans treated in the ER for acute conditions - inconsistent relationships with doctors. n n n “You only make changes for doctor that you know – if you don’t know the doctor then you won’t change”. “if the provider has been in the family for years (generations) then trust is increased. Also if provider and patient have similar values then trust is increased and compliance with screening increases”. Some patients believe that you “go into hospital and come out worse”.

Other Barriers to Care and Treatment n Denial: “Men won’t see doctor unless they are in pain; they use home remedies first”. “If it ain’t broke don’t fix it”. “Depends on the consequences…will still smoke cause I know I won’t die then and there…if the doctor told me that the next cigarette would kill me, then I would stop”. “Men will tell other men they need to see the doctor even if they don’t go themselves”.

Other Barriers to Care and Treatment n Age: – Younger men (less than 50) don’t see themselves as at risk (invincible) and don’t think about health until sick and then go to the ER. – Older men more likely to see a doctor “Wait until you have a problem to make changes…(therefore) older people more likely to make changes” n Insurance – “Some insurance is better than others…type of insurance depends on what tests you get done – doctors may not tell you need a test if they think you can’t pay for it”. – (Providers) “ always need to let patients know all the options even if you think they can’t afford. Sometimes people just find the money”.

Other Barriers to Care and Treatment n Life Priorities – Time n Working/family responsibilities – can’t take off from work. Will go to the doctor when I have time. Need to pay the bills and take care of family. May have multiple jobs or searching for job. – Money n n Insurance, co-pay, cost of prescriptions vs. food, rent, entertainment Spend money on things that provide a visual perception of success. “You can’t see good health, like you can a car, jewelry and clothes (material possessions) or a trip to Disney World. Health is competing with bragging rights of how people spend money and time”. – Don’t want to make lifestyle changes

Other Barriers to Care and Treatment n Lack of Education n “If you want to hide something from a Black man put it in a book” n “a lot of guys can’t read or write – need to educate verbally – don’t ask them to fill our papers”. n “I was never a good reader so my wife was the one who spoke to the doctor and then explained it to me” n Men may be embarrassed at not understanding health related information. Doctors need to “talk in plain terms so it’s easy to understand”

Communication/ Information Needs n Women and family members provide support: n “Wives should go to the doctor with men to make sure the right questions are asked. My wife always asks primary care questions – she makes sure I have the information…I’m not embarrassed. When I was younger my mom took all the information about what would happen during surgery… Men aren’t good listeners…don’t have patience to listen. As men get older they listen better. ” “ It take 10 people to get one male to see the doctor and they come from different states” – Women may be impediment: Men don’t want to be led. “You’re not my mama” “Women can push men to make changes, but men don’t like to be told what to do”.

Communication/ Information Needs n n n Families, particularly men, may not discuss health until there is a crisis. Mothers discuss health with daughters, but not with sons. If no male in household sons will learn about health issues from friends and information may be wrong. Need older male input. Need person to person messages “Brothers talking to brothers… breaking it down” n n Trust/credibility – believe someone who has been through it (testing/treatment) Misconceptions are passed on also

Communication/ Information Needs n Patient-Provider communication n Lack of time to discuss complex issues such as sexuality issues n Doctors may be intimidating or talk down to patients limiting patient willingness to ask questions n Need to develop on-going consistent relationship with doctor where “there’s some sharing going on”.

Communication/ Information Needs – Providers need to give “real messages” n “Need to communicate reality and not super sanitize health. We have insulated people from outcomes of disease. If something happens we (medical science) can fix it (medication/ transplants)” n “Strokes, cancer and high blood pressure torture you slowly and cause prolonged misery (dialysis, disability, nursing home) – worse than death. One does not have a merciful death” n “If you get sick who will care for you? Someone will have to put their lives on hold for you if you keep smoking and get cancer”. n Easier to take medications than recover from stroke. If you have a heart attack or stroke you can’t take Viagra.

Program Ideas n n n Churches/Mosques (prayer meetings, train clergy, develop messages for clergy, church bulletins, choir, parish nurse education) Fraternal organizations (Masons – earn points for healthy behaviors; Kappa Alpha Phi; Omega Psi Theta; Phi Beta Sigma) Barbershops Family mapping projects Sporting events, workplace, health clubs, Auto Zone Music video; cable TV; WDAS, Power 99, Q 102 n n n n n Community centers, schools Billboards/buses Testimonials Health fairs; screening programs in community Events such as Men’s Health Night Out Programs for women Newspapers (Daily Bread) Movie trailers; posters in pharmacy Prisons; probation officers; rehab facilities

Strategies n n n Intergenerational Use “real people” who have survived, been screened, had treatment, etc; peer education Interpersonal (man to man; friend to friend) Use multiple strategies Need consistent and sustainable programs/messages, not one -shot programs/messages (need to address throughout year – not just in September) n n n n Hypertension, stroke and prostate should be addresses as part of a comprehensive program Verbal communication best Provide follow-up to screening Focus on real messages, long term consequences Promote taking personal responsibility for health Theme: strong individuals, strong family, strong community = health Tie community message to PCP messages

Community Action Plan Strategies: – Train the trainer – Large group programs – Small group programs – One-on-One counseling Programs should: n n n n Provide resource information (i. e. access to care information) and health education materials Include re-education about myths Build on existing programs Link men to community resources Include intergenerational opportunities Include testimonials Utilize plays/videos (visual/ oral vs written materials)

Community Action Plan Model Train the Trainer programs Recruit change agents such as: clergy, barbers, rehab staff, day care staff, probation officers Large Group Programs (Lectures/ Plays/ Videos/ Men’s Health Night Out / Health Fairs (1 session) ·Faith based ·Day care Centers ·Health Centers ·Fraternal Organizations Pre-intervention survey (telephone/survey) ·Knowledge, attitudes, beliefs, behaviors, access (insurance, PCP) Small Group Programs (2 sessions) ·Barbershops ·Faith based ·Halfway houses ·Daycare centers ·Fraternal organizations ·Support person/women ·Health Centers One-on-one counseling ·Health Centers ·Community sites Post Intervention Survey (telephone/survey; 2 months post program conducted with assistance from trained lay leaders ·Changes in knowledge, attitudes, beliefs, behaviors, access (insurance, PCP)

Large Groups n Venues – – n Churches Day Care Centers Health Centers Fraternal Organizations Strategies – – Lectures Plays Videos Men’s Health Night Out n Activities – Blood Pressure Screens – Distribution of educational pamphlets – Recruitment of men into SHAPE-IT small group programs

Small Interactive Groups n n n 25 men per site 450 men recruited during each of the two 9 -month periods (totaling 900 men) Locations – 18 locations n n n 5 city health centers, 4 churches, 5 barbershops, 2 fraternal organizations, 2 recovery homes n 2 sessions; 2 hours each Condensed into one 3 hour session

Small Interactive Groups n Session I – What is High Blood Pressure/Stroke – Identify/Define Symptoms – Managing High Blood Pressure – Untreated High Blood Pressure Screens n Session II – Review of Session I – What is the Prostate and its function – Reasons to have the Prostate checked – Cause of Prostate Cancer – Diagnosis – Attitudes/Beliefs about Prostate Cancer/Screening – Talk to your Health Care Provider

One-on-One Counseling n Shared Decision Making Process on Prostate Cancer Screening – – Recruit from Small Groups Provide individual counseling Review : Let’s talk about prostate cancer screening Refer to Primary Care Physician Decision Counseling is a method of facilitating informed, value- based decision making about behavioral alternatives through a process of preference clarification. It uses Analytic Hierarchy Processing and Self-Regulation Theory for its theoretical basis.

Number Reached n Total- 7, 019 – 18 month period - divided into two 9 month cycles; – 450 men per cycle; – provided the subset of 900 men - extensive assessment of the perceptions, beliefs and reactions to SHAPE-IT small group programs – Pre and 2 month post-test (by phone)

Key Recruiting Supermarkets n Automotive Repair Shops n Public Transportation n Polling Stations n

Special Events n Men’s Wellness Dinner – Father’s Day n Tribute Event – “Own Their Health” – African Libation n Creating a Healthier Village – Men’s Health Movement





Blood Pressure n Hypertensive – 140+/90+ – 145/619 = 23% n Pre- Hypertensive – 120 -139/80 -89 – 249/619 = 40% n Normal – 120 -/80– 225/619 = 36%

Knowledge n n eight of eleven knowledge questions showed improvement from pre-test to 2 month follow-up, the other three (questions 1, 2, and 4) were stable. This finding indicates that key knowledge was improved and maintained two months after the program. on several questions, men demonstrated a highlevel of knowledge at pretest, indicating that issues about obtaining care may be often more about attitudes and behaviors than knowledge, itself. For example: 94% of men at pretest agreed that African American men should be tested for high blood pressure, and that controlling blood pressure reduces the chances of having a stroke. 92% of men at pretest agreed that it is important to detect prostate cancer in the early stages.

Attitudes – – – – increased reliance on family for health advice (28% to 52%) comfort talking to other men about health issues (79% to 94%) easy to talk with partner about my health (77% to 88%) communicate well with my doctor (80% to 94%) my doctor and I work together (84% to 94%) comfortable talking to others about prostate problems (78% to 83%) if I get prostate cancer, there is nothing I can do (more disagreed, 80% to 91%)

Attitudes n n n 94% of men felt their ability to control their health had improved, 49% a lot. 83% of men felt their quality of life had improved, 39% a lot. 90% of men felt their state of health had improved, 60% a lot

Behavior n n n n Blood pressure measured (87%), Talked to a doctor about prostate cancer (64%) Screened for prostate cancer (41%) Scheduling appointments (86%) Seeing a provider (76%) Getting a health care provider (for those who didn’t have one, 59%). Note: all these actions were done in 2 months time!

Behavior n n n n n (68%) exercised more often (73%) ate more fruits and vegetable (81%) cut back on salt (92%) take blood pressure medicine as recommended (20%) stopped smoking 44 men (68% of the other 65 smokers) cut (73%) reduced fat in their diet (52%) used stress management techniques more often (45%) reduced the amount of alcohol they drink in a week (37%) lost 5 lbs. or more weight

Program Replication Staff training and qualifications n n Make sure educators are well-trained. Trained educators equal an effective program (PAC) Make sure you find health educators who are invested in and passionate about the program (leadership/staff) The Lay leader component was not as effective we had hoped. (This may have been due to recruitment strategies as well as leadership commitment to the lay health strategy. ) Consider training PAC members as community champions rather than using lay leaders (leadership) Provide cultural competence training for all project staff, leadership/ PAC leadership in the beginning of the project (leadership

Program Replication Project Advisory Council n n Diversity of PAC is key Involve PAC to even a greater degree - involvement should be active, not just advisory. PAC incentives are important. Consider signing MOU with members of what they agree to do as a PAC member Increase PAC membership on a continual basis. Choosing PAC members from focus group participants, and people known to be active in the community worked, but need to continually recruit interested people. As PAC members became inactive - particularly those from the community - members should be replaced. Recruit from men who attend programs PAC recognition is important - Provide stipend, ask to do catering (creates employment opportunities, appreciation/celebration dinners)

Program Replication Program Curriculum n n n Provide single session programs only Review group decision-making process for applicability and validity. Develop strategies to capture voting preferences. Expand to other health issues Provide other health resources. Have a table with information about where they can go to be tested. Help men to set up an appointment to get tested. . Need more assistance/training in how to talk with their doctor in general (participants) Would like slide presentation (more visual). Show stages of cancer. Include testimonials (film or inperson) (participants) Use simple visual aids (staff)

Program Replication Outreach Strategies n n n n Consider evening hours to bring out other men Include women/significant others in programmatic efforts (programs for women and/or attend with men) Need flexibility in program to ensure it meets AA men needs and is able to reach the desired population Refreshments (staff/participants). Don't limit geographic areas, age groups or topics that can be covered. Younger men need to be included. Men of all ages have poor habits (colon cancer, smoking cessation, diabetes. Bring sons Include more health care providers in program.

Program Replication Communication n n n Reinforce motto "Own your own health" - use this in follow-up calls - remind men of importance of speaking up for themselves (PAC) More media exposure (PAC/staff) Simplify and clarify initial PAC recruitment letter (PAC) Increase consumer input - include more consumers in the PAC (PAC) Create resource guide to promote empowerment of men in accessing existing community resources (leadership) Build strong relationships based on trust, transparency, really listening to all partners (leadership) Consider copying everyone on all e-mails to improve communication (leadership)

Program Replication Communication n n Make sure leadership is willing to listen to the educators (leadership) Allow men to be active participants, not just listeners (staff) Men need to be loved/appreciated. Let men know they are the backbone of the family. And community. Empower men, you mean so much to so many people, their contributions are important to family and community. Message is it starts with good health. (staff) Provide telephone number of educators so participants can call with follow-up questions (participants) Use simple visual aids (staff)

Program Replication Program Evaluation n Shorten survey instruments. Revise instruments to reflect appropriate skip patterns. n Make sure all program participants sign in so that contact information is available for follow-up. n Consider having evaluation meetings with comanagers outside of regular monthly meetings with staff. Monthly meeting should focus on quality not quantity. n More fully integrate evaluators into all program components. Share evaluation/outcomes with PAC on a regular basis including changes in knowledge/attitudes and behaviors of participants as well as number of programs and number reached.

Program Replication Next Steps n n n n Provide individual counseling for men with hypertension (leadership) Expand to Latino community (PAC) Create resource guide to promote empowerment of men in accessing existing community resources (leadership, staff, participants) Replicate the "process" and have educators that mirror the community (PAC/leadership/staff) Bolster program with best practices as they are identified in national/state initiatives (leadership) Consider chronic care model for future research on hypertension/ or method for follow-up (leadership) Expand program to include other diseases/conditions or men's health in general

Program Replication n n Include more health care providers in program. Provide cultural competence training for all project staff, leadership/ PAC leadership in the beginning of the project Need more connection between decision-making piece and evaluation team. Apply for additional funding (CEED grant; other funders. Combine health issues or do a men's health overall program

Program Replication n n Presentations - write articles. Share what we have learned. Expand to other communities and age groups Explore group decision making further. After a 3 hour program the men were still connected - group decision-making allows for discussion, sharing, creates connections through shared experience.

Program Replication n Consider providing refresher sessions - do program semi annually. Have additional programs at the same site so men who missed program can attend. Create a web site/e-mail system so participants can follow-up with educators if they have questions/concerns or want to schedule future programs Complete video that can be played in recovery homes, barber shops, and health centers

Program Replication n n Identify and train people so program is replicated in every part of the city. Develop strategy to recognize achievement of program participants and raise awareness of their accomplishments Further explore "medical outcomes" – Do a longitudinal follow-up of shape-it cohort. For example "booster session" over the years
- Slides: 67