HEALTH PROBLEMS During Infancy I DDH Cleft Lip

HEALTH PROBLEMS During Infancy I • DDH • Cleft Lip and Palate • Club foot • Tay Sachs Disease • Down Syndrome • Feeding Difficulties • GERD • Omphalocele & Gastroschisis • Failure to Thrive • Skin abnormalities • SIDS

Developmental Dysplasia of the Hip (DDH) Spectrum of disorders of the hip that may develop any time: fetal life, infant, child Predisposing factors: Physiologic: maternal hormones & intrauterine posture Mechanical factors: breech and C sections Genetic: positive family hx Tests: Ortolani and Barlow (birth – 3 m) Shortening of limb on that side Asymmetric thigh and gluteal folds Broadening of perineum: √ when diapering Problems when begins to walk

Management of DDH Tx: Pavlik harness, hip spica cast, surgery Link with great pictures and tx with Pavlik harness Nursing care focuses on safe and careful assessment of circulation and skin care both with spica cast and the harness. Color~ capillary refill <3 sec. Mobility~ able to move toes easily Temperature~ warm to touch Sensation~ no numbness or tingling
![Care Skin care with Pavlik harness [pg 1593 (10 th ed. )] Put undershirt Care Skin care with Pavlik harness [pg 1593 (10 th ed. )] Put undershirt](http://slidetodoc.com/presentation_image/51506821fe25e61e62b4090757638002/image-4.jpg)
Care Skin care with Pavlik harness [pg 1593 (10 th ed. )] Put undershirt under chest straps and knee socks under foot and leg pieces Check under straps for redness 2 -3 x/day Gently massage under straps once a day Avoid lotions or powders Place diaper under straps Monitor for Growth and Development Parents need to be aware baby grows and if difficulty applying harness, angle of leg changes, increased fussiness/pain when harness applied

Cleft Lip and Cleft Palate Maxillary & nasal tissue fail to fuse during embryonic development (6 -12 wks) Result: abnormal opening in lip, palate, and/or nose Cleft Lip with or without Cleft Palate is the most common craniofacial malformation Cleft lip more common in males Cleft palate more common in females Etiology unknown – may occur as part of genetic or environmental factors, medications such as a retinoid, steroid, anticonsulvies
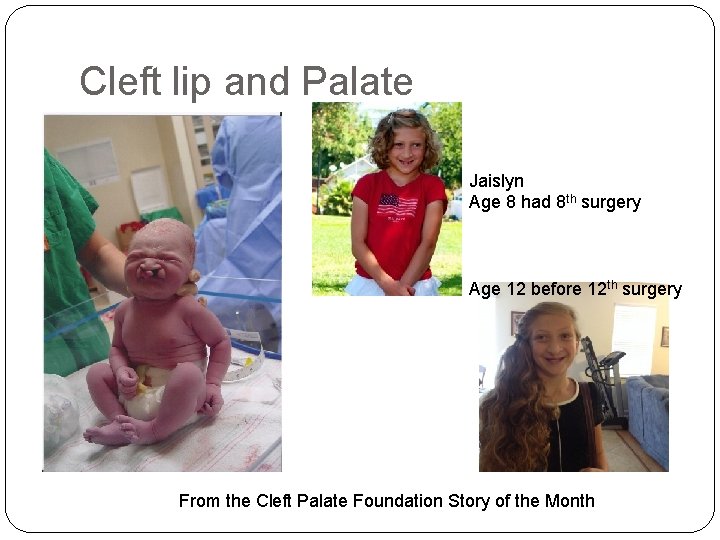
Cleft lip and Palate Jaislyn Age 8 had 8 th surgery Age 12 before 12 th surgery From the Cleft Palate Foundation Story of the Month

Clinical Manifestations Cleft Lip: may be unilateral or bilateral Simple notching of lip to deep cleft extending thru lip or into nose Cleft Palate: midline fissure or opening in hard &/or soft palate areas (may have absence of nasal septum) Difficulty forming seal for sucking Coughing & choking w/feeding Nasal distortion & congestion Failure to thrive if unrepaired Excellent sites: http: //emedicine. medscape. com/article/1280866 -overview http: //kidshealth. org/parent/medical/ears/cleft_lip_palate. html Cleft Palate Foundation: http: //www. cleftline. org/

Management Team approach (teams in Champaign, Rockford, Chicago) Emotionally difficult for families Feeding before surgery: feeding video Breastfeeding possible and encouraged If Bottle fed specialty bottles needed Baby’s head must be upright Frequent burping needed Patience and support needed Surgical correction: CL before CP Cleft Lip repair between 2 and 3 months of age as soon as stable Surgery for CP usually later typically between 6 and 12 months of age but before speech develops

Post Operative Care CL repair (Cheiloplasty); CP (Palatoplasty) Meticulous care of suture line(s) Restraints frequently needed Pain management Monitor for signs of infection or bleeding Avoid placing anything hard in mouth Position in semi-Fowler or partial side-lying to prevent aspiration and maintain open airway

Read stories of children with Cleft Lip and Palate and their outcomes

Congenital Clubfoot Talipes Equinovarus (TEV) Deformity of ankle & foot (pp 424 -425, 9 th ed. 10 th ed. pp 1596 -97) Bone deformity and malposition w/soft tissue contracture 3 categories: positional, syndromic, congenital or idiopathic (most common 95%) Readily apparent at birth; they are at an increased risk Developmental Dysplasia of the Hip (DDH)

Treatment- Correction, maintenance, follow-up Casting soon after birth; serial casting common; possible surgery Nursing care: Assess distal extremities for Color, Mobility, Temperature, and Sensitivity (CMTS). Teach parents. See cast care instructions ( 9 th ed. pp 16431645, 10 th ed. pp 1556 -59).

Tay-Sachs Disease Autosomal recessive genetic disorder Leads to progressive destruction of the CNS Fatty substance accumulates in brain nerve cells Normal development at first (~ 6 months) until nerve cells become distended w/fatty material Blindness, deaf, unable to swallow, atrophy of muscles leading to paralysis Most die by age 5 Occurrence higher in persons of eastern European (Ashkenazi) Jewish descent National Tay-Sachs & Allied Diseases Assoc. : Resource for parents https: //www. youtube. com/watch? v=SZor 2_WJmk. M

Down Syndrome Most common chromosome abnormality 1 in 800 to 1000 births Also known as trisomy 21 Extra chromosome 21 in 92% to 95% Mosaicism in 1% to 3% Translocation of chromosome 21 in 3% to 6% Not related to maternal age Could be a carrier so higher risk w/another PG

Syndrome-see handout in course calendar for specific characteristics Wide variations physically and mentally Effects entire body with variations in the head, eyes, nose, ears, mouth, teeth, chest, neck, abdomen, genitalia, hands, feet, skin, and musculoskeletal functions 40% to 45% heart defects Renal, Hirschsprung, TE fistula Altered immune function Skeletal defects Atlantoaxial instability

Nursing Considerations Down Syndrome LOTS of parental support, especially at birth Encourage bonding; promote acceptance Provide contact information to a support group Encourage expressions of grief and loss Teach prevention of physical problems Safe handling due to hypotonicity Prevention of respiratory problems Bulb syringe use, humidification, position changes Good handwashing Skin care Help with feeding difficulties

Parental Support Down Syndrome Referrals to support groups and appropriate web sites www. ndss. org National Down Syndrome www. nads. org Nat. Assoc. for Down Syndrome click on FAQ Photos of siblings—one with and one without Information on early intervention programs Refer for genetic counseling

FEEDING DIFFICULTIES All Newborns and Infants Regurgitation-return of undigested food with burping Spitting up-dribbling of un-swallowed formula from mouth after feeding Encourage frequent burping, minimum handling during and after, position child on right side with head up after eating Avoid skin breakdown – keep skin dry; apply ointment If regurgitation is persistent – Provider evaluation for GERD

Childhood Food Sensitivity Food allergy = immunologic Most common: eggs, cow’s milk, peanuts, soy, wheat, corn, tree nuts, shell fish, fish Allergy w/hereditary tendency – atopy 1 parent 50% greater risk; 2 parents up to 100% risk of developing allergy Milk allergy: no definitive test, best is to eliminate followed by challenge test Change to casein hydrolysate formula where protein is broken down(Nutramigen) – NOT soy

Food Intolerance: non immunologic Lactose deficiency Congenital lactase deficiency: rare Late-onset/primary-most common, 3 -7 yrs. Asians, southern Europeans, Arabs, Israelis, and African-Americans Secondary – from damage to intestinal lumen, cystic fibrosis, sprue, infections, etc. S/S: abd. pain, bloating, gas, diarrhea within 30 min. to hrs. after ingestion Enzyme tablets, pretreated milk, yogurt, soy

Colic Paroxysmal abd. pain or cramping with loud crying and drawing legs up to the abdomen More common < 3 mos Usually resolves around 12 to 16 months. Several theories – Carb malabsorption most common and accepted Assess for cow’s milk allergy Tx: medication, variety of approaches (pp. 532 -534, 9 th ed. ; pp. 470 -472, 10 th ed. ), assess daily routine & home environment Provide emotional support for parents

Vegetarian Diets Lacto-ovovegetarian – fewest problems Lactovegetarians – no meat or eggs Vegans (purists) – no milk or eggs or meat Zen macrobiotics – fruits, vegies, legumes Semi-vegetarian – some fish & poultry Encourage Fe supplementation – educate on factors that affect iron absorption

PICA Disorder characterized by the compulsive and excessive ingestion of both food and NONFOOD substances Differing theories on cause: psychologic, nutritional deficiency (lead or zinc) Complications: parasites, lead poisoning, intestinal obstruction, inflammation

Gastroesophageal Reflux (GER) Def: regurgitation of gastric contents into the esophagus; results of relaxation or incompetence of the lower esophageal (cardiac) sphincter. Etiology: Inappropriate LES relaxation. Delayed emptying. Pathophysiology: Repeated reflux damages the esophageal mucosa Severe cases require surgery: Nissen fundoplication; the gastric fundus is wrapped around the distal esophagus.

Gastroesophageal Reflux Symptoms: Effortless spitting up 1 -2 mouthfuls (under age one) Irritability Failure to thrive, weight-loss Aspiration - recurrent respiratory infections Anemia Apnea, worsening asthma Esophagitis

Gastroesophageal Reflux Diagnosis: Barium swallow or ultrasound: √ for: Hiatal hernia Pyloric Stenosis Malrotation Esophageal Manometry: √ control of lower esophageal sphincter Endoscopy & p. H probe - 24 hours/Gold Standard; p. H is placed down to the distal esophagus - if p. H is below 4. 0 suggests reflux. Endoscopy is the most sensitive test for esophagitis & also gastric outlet syndrome; biopsies obtained at same time.

Gastroesophageal Reflux Management Maintained child in the upright position during feedings & 30 min. pc Provide frequent small feedings; frequent burping w/infants Add rice cereal to formula to thicken feedings Avoid fatty foods, citrus juices, chocolate, carbonated drinks Avoid vigorous play after feedings & feeding b/4 bedtime Prone vs supine sleeping position for infants; ↑ SIDS risk Assess respiratory status before and after feedings Monitor hydration status, I & O, & frequency of emesis Meds: Antacids- Histamine blockers-, Cimetidine (Tagamet), Ranitidine (Zantac) Dopamine antagonist increases muscle contractions in the upper digestive tract: Metoclopramide (Reglan)

Failure to Thrive Inadequate growth from inability to obtain and/or use calories needed Wt. falls below the 5 th percentile Persistent deviation from growth curve most important Organic – physical, i. e. heart defect Nonorganic (NFTT)– unrelated to disease; poor care; psychosocial factors; attachment problems, child may not make eye contact Idiopathic – Unexplained by the above but often classified as NFTT

Factors of Nonorganic Failure To Thrive Poverty – uninsured, homeless, insufficient food Health beliefs – fad diets; obsess about weight Inadequate nutrition knowledge Family Stress Feeding Resistance – non oral nutritional therapy early due to medical problem Insufficient breast milk Most Difficult – parent/child disturbance

Failure to Thrive Multidisciplinary team approach needed May be multiple psychosocial problems Prognosis related to the cause Prognosis poor with: severe feeding resistance, lack of cooperation or awareness from parents, low income, low ed. level, teen Mom, early onset Takes time and patience (see guidelines pp. 534 -538, 9 th ed; pp. 462 -465 10 th ed. ) for feeding the infant with NFTT

Diaper Dermatitis Peak age: 9 -12 months Prolonged contact with urine, feces, friction of wet diaper; soap, detergent, wipes Change diaper ASAP, expose skin to air, use ointment/zinc oxide, breast milk, corn starch not talc Candida infection: bright red, confluent lesions w/raised borders; satellite lesions; painful; may need antifungal cream

Seborrheic Dermatitis “Cradle Cap” – chronic, recurrent, inflammatory reaction of the skin Eyelids, ears, nose, inguinal area Over growth of yeast Thick, yellow, adherent, scaly, oily patches NOT associated w/family hx for allergy Infants and also after puberty Daily shampoo, let soak to soften crusts, rinse & use fine tooth comb to remove or can use mineral oil; reassure no harm to fontanel

Atopic Dermatitis Pruritic eczema associated with allergy Hereditary tendency – atopy Usually begins in infancy (2 -6 m); Infantile eczema w/remission by 3 yrs. Childhood – may follow infantile or begin at 2 -3 yrs; 90% by 5 yrs Preadolescent – begins abt. 12 yrs and cont. indefinitely

Major Goals of Management Hydrate the skin: tepid bath w/no soap or mild (Dove, Neutrogena) w/immediate application of emollient (Eucerin) Relieve pruritus: antihistamine drugs, colloid baths, topical steroids Prevent/control secondary infection: antibiotics, keep fingernails/toenails cut short, teach to look for signs of infections Eliminate rough fabrics, wool, irritants in soaps, detergents, wipes. Avoid latex. Keep cool – avoid excess perspiration & heat. Provide support to family – very difficult situation
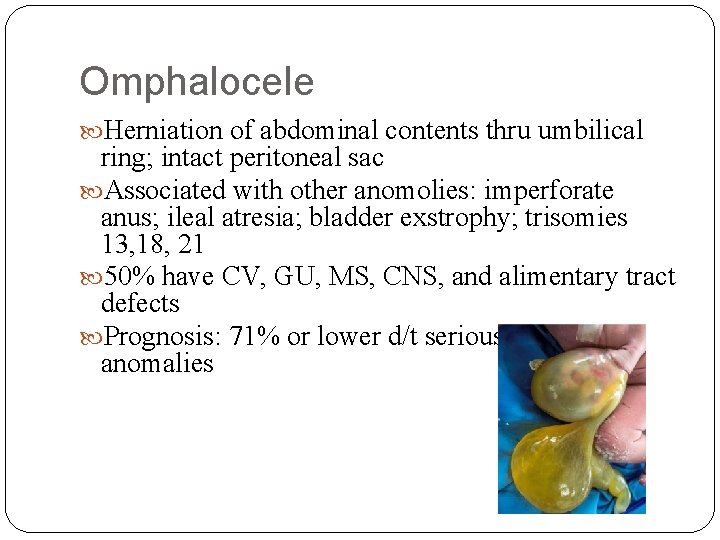
Omphalocele Herniation of abdominal contents thru umbilical ring; intact peritoneal sac Associated with other anomolies: imperforate anus; ileal atresia; bladder exstrophy; trisomies 13, 18, 21 50% have CV, GU, MS, CNS, and alimentary tract defects Prognosis: 71% or lower d/t serious associated anomalies
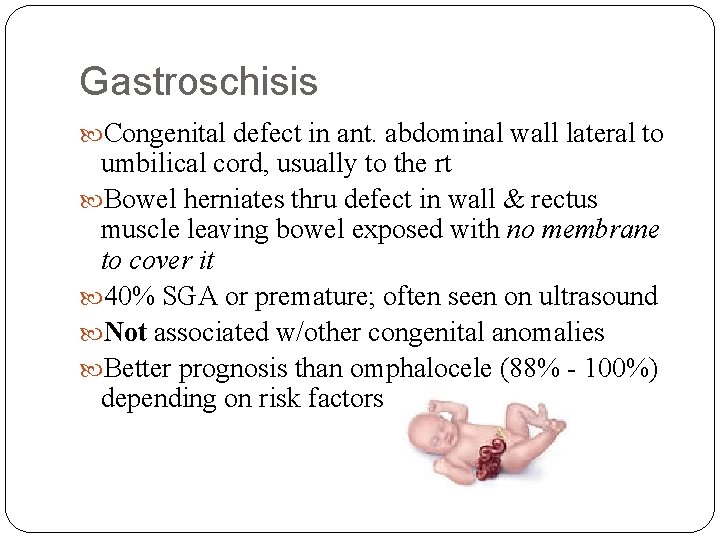
Gastroschisis Congenital defect in ant. abdominal wall lateral to umbilical cord, usually to the rt Bowel herniates thru defect in wall & rectus muscle leaving bowel exposed with no membrane to cover it 40% SGA or premature; often seen on ultrasound Not associated w/other congenital anomalies Better prognosis than omphalocele (88% - 100%) depending on risk factors

Nursing Management for Omphalocele or Gastroschisis Immediately cover contents w/warm, moist sterile saline-soaked dressing to keep moist and maintain heat Sterile technique imperative NG tube for decompression IV fluid d/t high fluid losses Positioning & handling to prevent rupture Cardiac & apnea monitor with oximetry; monitor VS Thermoregulation critical w/fluid losses Antibiotics started ASAP Assess fluid/electrolyte status May need TPN Surgery always

Sudden Infant Death Syndrome SIDS Sudden death of an infant under 1 year of age after complete postmortem exam, investigation of death scene & review of case history 3 rd leading cause of death bet. 1 m – 1 yr Dramatic 40% decrease since 1992 since “Back to Sleep” campaign Hypothesis: brainstem abnormality in neurologic regulation of cardiorespiratory control. Maternal smoking– major factor in SIDS

SIDS Other risk factors: co-sleeping or bed sharing, prone position, soft bedding, overheating during sleep (thermal stress) Plagiocephaly – alter head position during sleep; place prone or side when awake Autopsy findings: pulmonary edema, intrathoracic hemorrhages – similar to those found with suffocation

SIDS Family Care In ER, ask only factual questions Autopsy needed to find cause If breastfeeding, mom needs info Allow family to say goodby; make sure room and baby are cleaned up; allow quiet time and encourage them to hold baby Make sure referral is made for follow up home visit Primary nursing responsibility is emotional support of the family and referral for follow up
That’s it, folks!!
- Slides: 41