Health Plan Enrollment Rules and Strategies Presented by

Health Plan Enrollment – Rules and Strategies Presented by Benefit Administration Company, LLC.

Introduction

Today’s Agenda Open enrollment is a good time to review: • Enrollment periods • Election methods • Plan design changes • Notices to plan participants
Enrollment Periods

Enrollment Periods Initial Enrollment Period Newly eligible employees enroll in coverage Open Enrollment Period Eligible employees may enroll in coverage for the upcoming plan year Mid-year Enrollment Periods Employees enroll for coverage during the plan year (often triggered by major life events, such as marriage or having a baby)
Initial Enrollment

Initial Enrollment Period (IEP) The period of time when newly eligible employees can enroll in the health plan Enrollment Opportunities • If employees do not enroll during the IEP, they usually must wait until the next open enrollment period • Unless they experience a mid-year enrollment event Timing • Timing of the IEP is flexible • Subject to legal restrictions and terms of insurance policy or collective bargaining agreements

IEP – ACA Rules Waiting Period Limits • Affordable Care Act (ACA) imposes a 90 -day limit on waiting periods • Cannot require eligible employees to wait until open enrollment to enroll Applicable Large Employers (ALEs) • To avoid penalties, generally must offer coverage to full-time employees after the first three full calendar months of employment • Under look-back measurement method, must offer coverage to new variable hour and seasonal employees (determined to be fulltime) for stability period following initial measurement period

IEP – Section 125 Rules • Many employees pay health premiums on a pre-tax basis through a Section 125 plan (cafeteria plan) • Section 125 elections generally must be prospective only • Limited exception – Elections that new employees make within 30 days of hire date can be retroactive Eligible employee is hired on July 1 IEP begins on date of hire and lasts 30 days Employee elects coverage on July 26, retroactively effective July 1

Initial Enrollment Notices

Notices for New Participants Exchange Notice • Must provide all new hires with a written notice about the Exchanges SPD • Must be provided within 90 days of when group health coverage begins Summary of Benefits and Coverage (SBC) Grandfathered Plan Notice • Must be provided with enrollment materials (issuer typically provides for fully insured plans) • Must be included in enrollment materials (only applies to grandfathered plans)

COBRA Notice – General Notice • Provides information to plan participants regarding COBRA and plan procedures • Must be provided within 90 days after plan coverage begins • May be included in plan’s SPD

Medicare Part D Notice • Employers with group health plans that provide prescription drug coverage must notify Medicare Part D eligible individuals whether that coverage is creditable • Notice must be provided prior to the effective date of coverage (and before Oct. 15 each year)
Open Enrollment

Open Enrollment Period Time period each year when an eligible employee may: – Enroll for coverage, even if coverage was previously declined – Change coverage elections (if employer offers more than one benefit package option) – Change enrollment for dependents (drop or add coverage for eligible dependents)

Open Enrollment Period Is an open enrollment period required? ACA Section 125 Other • To avoid penalties, ALEs must provide full -time employees with an annual opportunity to accept or decline coverage • If health plan does not meet affordability or minimum value standards, employees must be able to decline coverage at least once per year • If employees can pay premiums on a pre-tax basis, Section 125 rules generally require that they have a period of time to make their elections each year • Open enrollment periods may be required by health insurance contracts or collective bargaining agreements

Open Enrollment Period – Timing Rules • Takes place prior to beginning of plan year for which elections are made • Elections for pre-tax benefits must be effective on a prospective basis • Ends well in advance of upcoming plan year to provide time for: – Confirming elections – Administering enrollment – Preliminary nondiscrimination testing
Mid-year Enrollment
Mid-year Enrollment Periods Special enrollment periods Other enrollment periods • Employers must allow employees to enroll during a plan year if they experience a HIPAA special enrollment event • Other mid-year enrollment opportunities may be permitted, depending on plan design • For fully insured plans, check with carrier • Section 125 rules only allow mid-year changes for certain events (called “mid-year election change events”)

HIPAA Special Enrollment Event Enrollment Period Length Employee (or dependent) loses eligibility for other health coverage Employee acquires new dependent through marriage, birth, adoption or placement for adoption Coverage Effective Date No later than the first day of the calendar month beginning after the plan receives the special enrollment request At least 30 days However, when a new dependent is acquired through birth/adoption, coverage must be retroactively effective to the date of birth/adoption
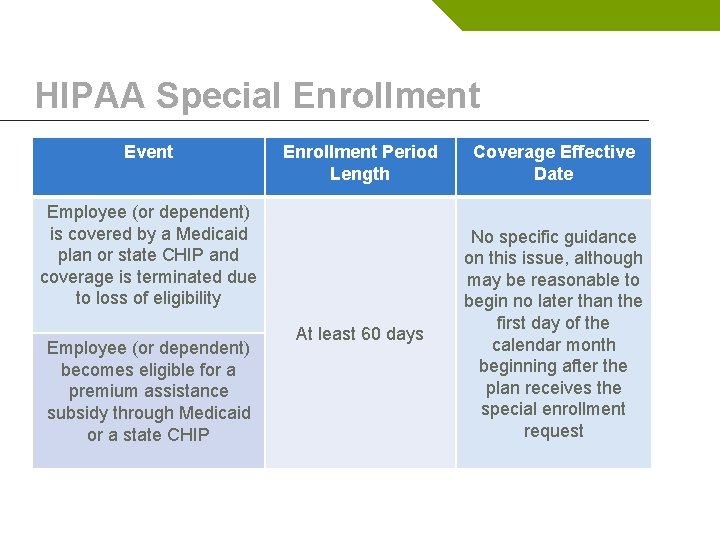

HIPAA Special Enrollment Event Enrollment Period Length Coverage Effective Date At least 60 days No specific guidance on this issue, although may be reasonable to begin no later than the first day of the calendar month beginning after the plan receives the special enrollment request Employee (or dependent) is covered by a Medicaid plan or state CHIP and coverage is terminated due to loss of eligibility Employee (or dependent) becomes eligible for a premium assistance subsidy through Medicaid or a state CHIP

Mid-year Election Change Events General Section 125 Rule: Participants’ elections are irrevocable during the plan year Subject to certain limited exceptions IRS recognizes certain events as permitting mid-year election changes Plan design option—not required to allow participants to change elections Most employers design their Section 125 plans to allow the midyear election change events permitted by IRS
Mid-Year Election Change Events The IRS recognizes three broad categories of mid-year election change events Change in status • Major life events (marriage, birth, adoption, employment changes) Cost or coverage changes • Changes to qualified benefits under cafeteria plan Other laws or court orders • Coordinate cafeteria plan rules with other laws (for example, FMLA and COBRA)

Election Methods
Three Main Election Methods Employers have three main options for how employees will make their elections at enrollment time Affirmative elections Default (or automatic) elections Rolling (or evergreen) elections

Election Methods Affirmative Elections • At each enrollment period, employees complete a written (or electronic) agreement to participate in the plan • Works well with all types of welfare benefits • Most common and straightforward method

Election Methods Default Elections • Each employee is automatically enrolled in health coverage, unless the employee affirmatively waives coverage • Employers must provide adequate notice to employees, describing how process works and how to waive coverage • Sometimes used with rolling elections for reenrollment • Confirm compliance with state wage withholding law

Election Methods Rolling Elections • Current elections continue to next plan year unless employee makes an election to change coverage • Process should be described in open enrollment materials • As a best practice, remind employees of current elections at open enrollment • Does not work well with all benefits (for example, health FSA) • Confirm compliance with wage withholding laws

Electronic Enrollment More employers are using online enrollment and posting health plan notices electronically ERISA requirements for electronic disclosure • • Must notify employees when documents are posted Must follow ERISA’s style and content requirements Participants have a right to paper copies Employees who do not have work-related computer access must consent to electronic delivery

Open Enrollment 2018

Plan Design Changes Group health plan sponsors should be aware of changes for the 2018 plan year ü Review plan documents ü Make any necessary updates ü Communicate changes to participants with an updated SPD or a summary of material modifications (SMM)

Grandfathered Status A grandfathered (GF) plan is one that was in existence when the ACA was enacted and has not had certain prohibited changes made to it since then Review GF Status • Determine whether plan will maintain GF status for upcoming plan year • GF plans must provide a special notice • Non-GF plans must comply with additional ACA mandates Additional Mandates • Preventive care without cost-sharing • Out-of-pocket maximum for essential health benefits (EHB) • Nondiscrimination rules for fully insured plans (not currently effective)

Out-of-Pocket Maximum (OOPM) Non-GF plans must comply with an annual limit on cost-sharing for coverage of EHB 2017 • $7, 150 for self-only • $14, 300 for family 2018 • $7, 350 for self-only • $14, 700 for family

Administering the OOPM Multiple service providers • If a plan uses different service providers for EHB, must coordinate claims or divide up the OOPM Embedded OOPM • Self-only OOPM must apply to all individuals, even those with family coverage • If family OOPM is higher than self-only limit, must embed individual OOPM in family coverage IMPORTANT: If you have a high deductible health plan (HDHP), your plan’s OOPM must be lower than the ACA limit

Health FSA Limit The health FSA limit increases to $2, 650 for 2018 • ACA imposes dollar limit on employees’ pre-tax contributions to a health FSA – $2, 550 for 2015/2016 – $2, 600 for 2017 – $2, 650 for 2018 • Employers can impose their own limits that are lower than the ACA’s limit Communicate the plan’s limit on health FSA contributions as part of enrollment process
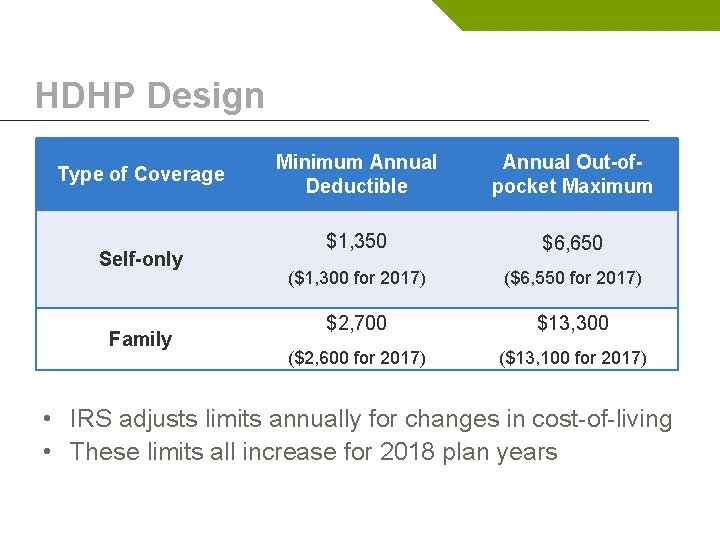
HDHP Design Type of Coverage Self-only Family Minimum Annual Deductible Annual Out-ofpocket Maximum $1, 350 $6, 650 ($1, 300 for 2017) ($6, 550 for 2017) $2, 700 $13, 300 ($2, 600 for 2017) ($13, 100 for 2017) • IRS adjusts limits annually for changes in cost-of-living • These limits all increase for 2018 plan years
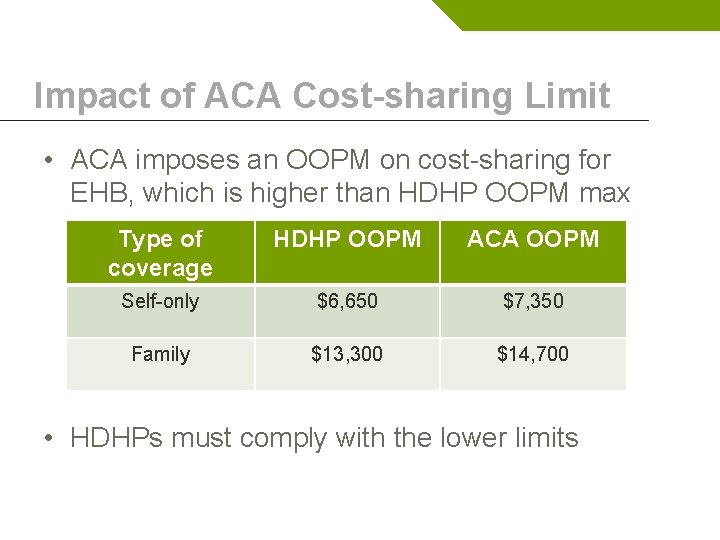
Impact of ACA Cost-sharing Limit • ACA imposes an OOPM on cost-sharing for EHB, which is higher than HDHP OOPM max Type of coverage HDHP OOPM ACA OOPM Self-only $6, 650 $7, 350 Family $13, 300 $14, 700 • HDHPs must comply with the lower limits

HDHP – Plan Design Issues Embedded deductibles for family coverage Deductible carryovers • Claims paid if individual deductible is met, even if family has not met family deductible • Expenses incurred below deductible in last few months of prior plan year are applied to current year deductible • Only allowed if embedded deductible is not lower than HDHP family deductible • Only allowed if current year deductible is proportionately increased
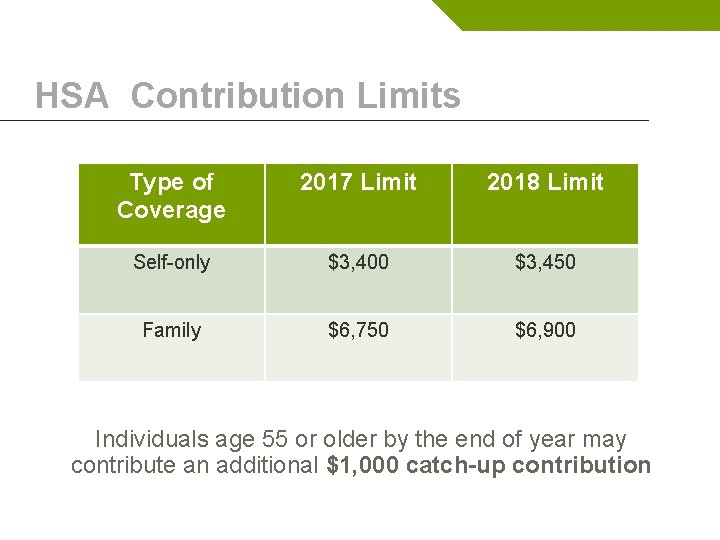
HSA Contribution Limits Type of Coverage 2017 Limit 2018 Limit Self-only $3, 400 $3, 450 Family $6, 750 $6, 900 Individuals age 55 or older by the end of year may contribute an additional $1, 000 catch-up contribution
Open Enrollment Notices

Open Enrollment Notices Annual CHIP Notice • Group health plans that cover residents in a state that provides a premium subsidy to low-income residents to pay for employersponsored coverage must provide this notice. WHCRA Notice • Must provide an annual notice regarding participants’ rights to mastectomy-related benefits under the Women’s Health and Cancer Rights Act (WHCRA) Medicare Part D Notice • Must provide notice of creditable (or noncreditable) coverage each year before Oct. 15

Summary of Benefits and Coverage (SBC) • Short summary of benefits and coverage under the plan required by the ACA • Must be provided by Plan Administrator and insurer – Non-duplication rule allows one party to distribute SBC – At enrollment, re-enrollment and upon request IMPORTANT: There is a new SBC template that must be used for open enrollment periods or plan years that begin on or after April 1, 2017
Questions?

Thank you! This presentation is current as of the date presented and is for informational purposes only. It is not intended to be exhaustive nor should any discussion or opinions be construed as legal advice. Please contact legal counsel for legal advice on specific situations. This presentation may not be duplicated or redistributed without permission. © 2016 -2018 Zywave, Inc. All rights reserved.
- Slides: 44