Health Medical Care and Medical Spending Health Economics































- Slides: 47

Health, Medical Care, and Medical Spending Health Economics Professor Vivian Ho Fall 2007 These slides summarize material in Santerre & Neun: Health Economics, Theories Insights and Industry Studies, Thomson 2004

Ø Can we apply the tools of managerial economics to health care? 2

Outline An economic model of utility, health, and medical care l Measuring health status l Empirical evidence on health production l Health care expenditures l 3

A Basic Economic Model l Health as a consumer durable good: u Utility = U (X, Health) X represents “other goods and services” l H is a stock -- every action will affect health l On its own or combined with other goods and services, the stock of H generates a flow of services that yield satisfaction=utility l 4

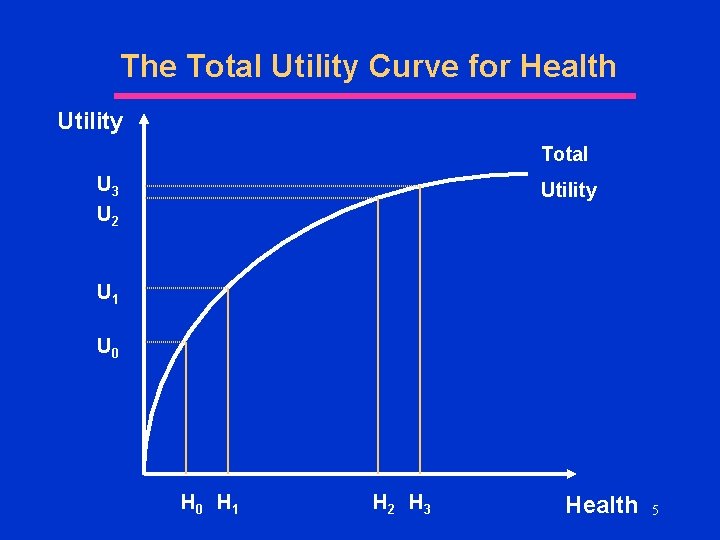
The Total Utility Curve for Health Utility Total U 3 U 2 Utility U 1 U 0 H 1 H 2 H 3 Health 5

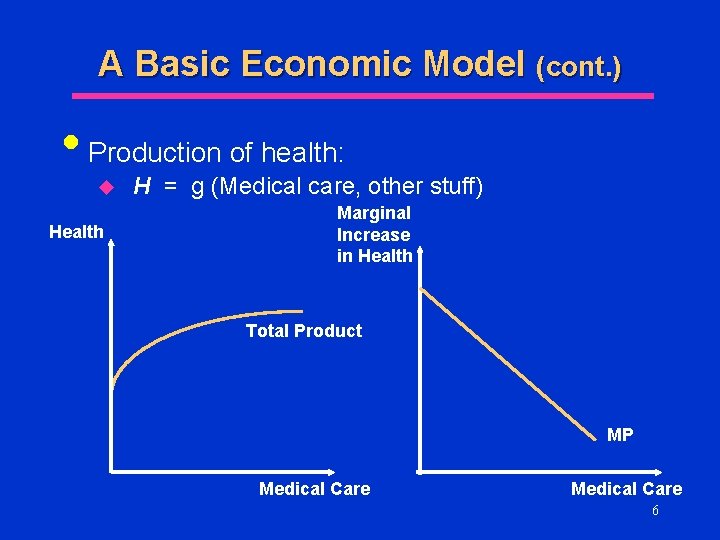
A Basic Economic Model (cont. ) • Production of health: u Health H = g (Medical care, other stuff) Marginal Increase in Health Total Product MP Medical Care 6

A Basic Economic Model (cont. ) l Medical care is not homogeneous and differs in: u Structural quality (e. g. facilities and labor) u Process quality (e. g. waiting time, case mgmt. ) u Outcome quality (e. g. patient satisfaction, mortality) l Therefore medical services are often difficult to quantify 7

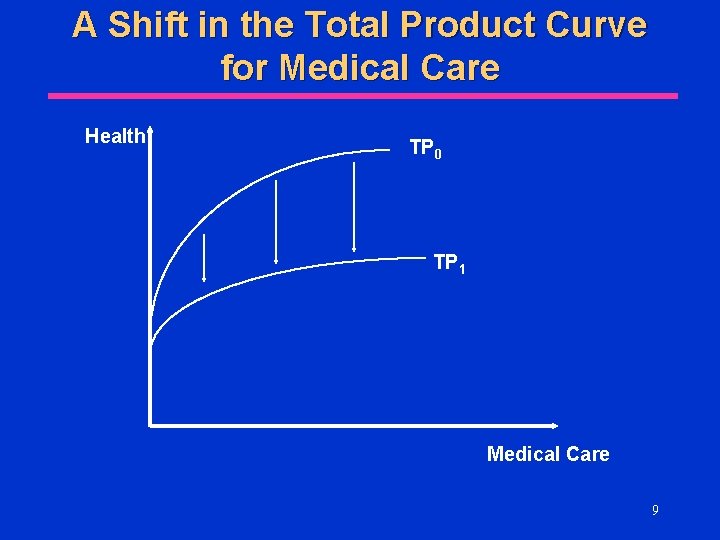
A Basic Economic Model (cont. ) l Health=H(Profile, Medical Care, Lifestyle, Socioeconomic Status, Environment) If an individual has a heart attack, then overall health decreases, regardless of the amount of medical care consumed u The total product curve for medical care shifts down l As a person ages, both health and the marginal product of medical care likely to fall u The out total product curve shifts down and flattens 8

A Shift in the Total Product Curve for Medical Care Health TP 0 TP 1 Medical Care 9

MEASURING HEALTH l Important for all health care managers today u Insurers and consumers are demanding costs AND quality 10

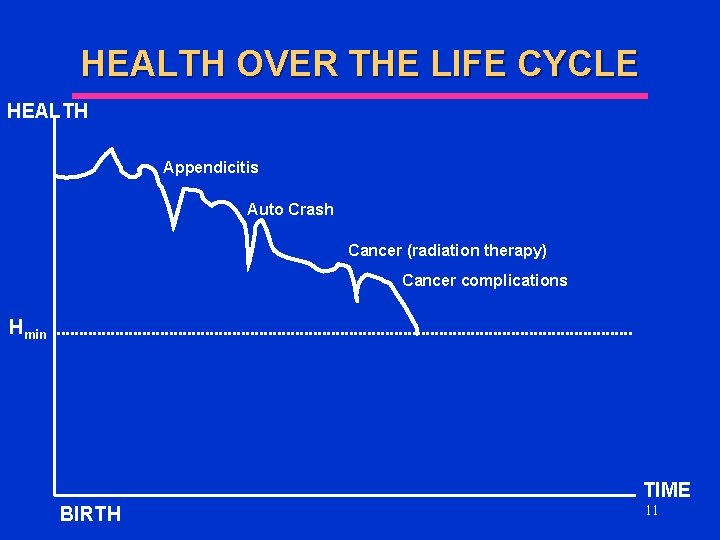
HEALTH OVER THE LIFE CYCLE HEALTH Appendicitis Auto Crash Cancer (radiation therapy) Cancer complications Hmin TIME BIRTH 11

HEALTH OVER THE LIFE CYCLE l Individuals make choices about health (make tradeoffs) which maximize U over time l Relatively high value for the future • Low discount rate l l e. g. Low-fat diet and exercise to avoid heart disease Relatively low value for the future • High discount rate l e. g. Smoking, excess drinking, drug abuse 12

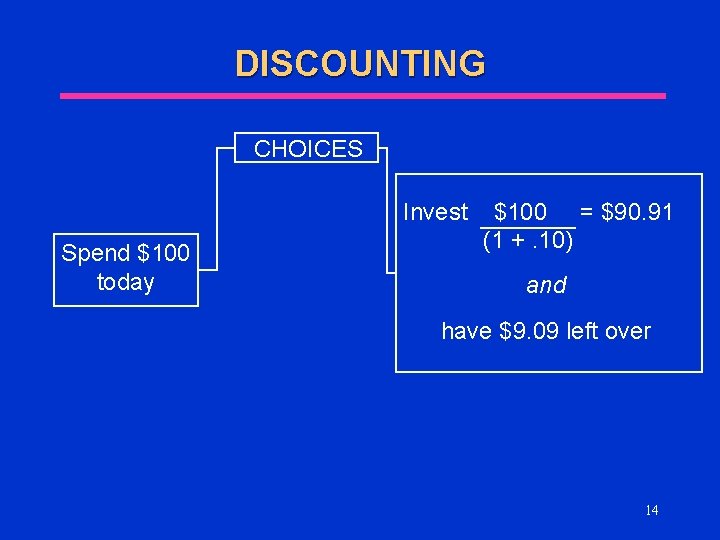
DISCOUNTING l Required when costs are incurred in the future u Why? Individuals have a positive value of time preference l l If r = 10%, then $100 invested today yields $110 next year Spending $100 one year from now is “cheaper” than spending $100 today 13

DISCOUNTING CHOICES Invest Spend $100 today $100 = $90. 91 (1 +. 10) and have $9. 09 left over 14

15

DISCOUNTING l If costs occur over multiple time periods, we must calculate the present discounted value (PDV) of these costs: T PDV = Σ t=0 • 1 COSTSt t (1 + r) Example: A project requires: $100 in year 1 $ 75 in year 2 $ 50 in year 3 PDV = $100 + $ 75 + $ 50 = $209. 50 2 (1 +. 10) 16

DISCOUNTING l If we discount costs, we must also discount benefits Assume r = 10% $990 Spend $990 to save 1 year of life today Invest $900 to save 1 year of life next year and have $90 left to spend this year 17

DISCOUNTING u Appropriate discount rate? • The medical literature has settled on 5% for comparative reasons u Discounting is not an adjustment for inflation COST YOLS 1 = Σ (1 + r)t COST Σ 1 YOLS (1 + r)t 18

Why we discount cost AND benefits l Consider an intervention which costs $100 and saves 10 years of life l Also assume r = 10% Option 1: Spend $100 today: C E = 100 = 10 10 Option 2: Invest for 1 year → $110, saves 11 YOL. If we discount costs to present value, but don’t discount YOL: C E = l 100 1 11 = 9 11 If we discount both costs and benefits: C = E 1 110 (1 +. 10) 1 (1 +. 10) = 10 11 19

MORTALITY l Alive vs. Dead u Advantages: l u Disadvantages: l 20

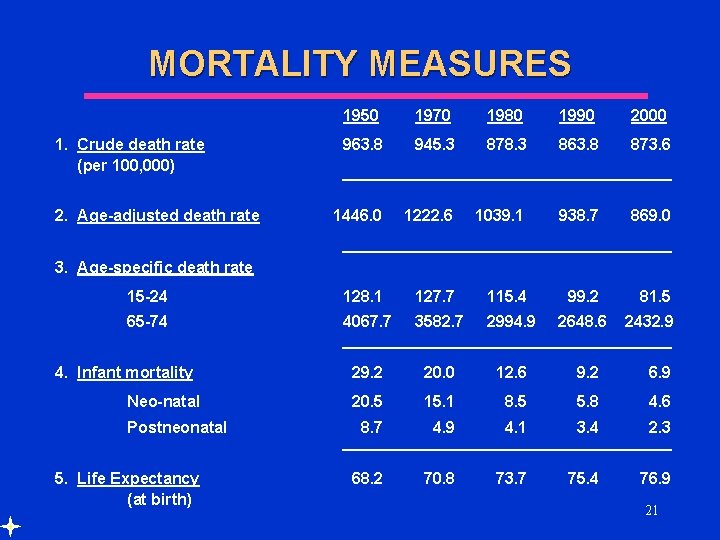
MORTALITY MEASURES 1950 1970 1980 1990 2000 963. 8 945. 3 878. 3 863. 8 873. 6 1446. 0 1222. 6 1039. 1 938. 7 869. 0 15 -24 128. 1 127. 7 115. 4 99. 2 81. 5 65 -74 4067. 7 3582. 7 2994. 9 2648. 6 29. 2 20. 0 12. 6 9. 2 6. 9 20. 5 15. 1 8. 5 5. 8 4. 6 8. 7 4. 9 4. 1 3. 4 2. 3 68. 2 70. 8 73. 7 75. 4 76. 9 1. Crude death rate (per 100, 000) 2. Age-adjusted death rate 3. Age-specific death rate 4. Infant mortality Neo-natal Postneonatal 5. Life Expectancy (at birth) 2432. 9 21

MORTALITY MEASURES l Life expectancy NOT a prediction of how long people live u 76. 9 is a summary of age-specific death rates in 2000 u “If those born in 2000 experienced agespecific death rates prevailing in 2000, on average they would live to be 76. 9 22

MORBIDITY l The relative incidence of disease u Advantages: l u Captures quality of life Disadvantages: Difficult to measure l Difficult to aggregate when patient has >1 problem l 23

MORBIDITY l Acute disease u e. g. l Chronic disease u e. g. l appendicitis, pneumonia, gun shot wounds arthritis, diabetes, asthma Incidence u occurrence l of new cases in any particular year Prevalence u new and ongoing cases in any particular year v Heart disease is more prevalent, but its incidence is declining 24

MEASURING MORBIDITY l Distinguish between symptom and disease u e. g. high blood pressure vs. stroke l Disabilities are also a sign of morbidity l Subjective measures - i. e. self-rated health u “Is your health excellent/good/fair/poor? ” u Problem: 1970 -80, # of people with high blood pressure declined. But % of people reporting restricted activity due to HTN doubled! u Depends on what you want to do - e. g. astronaut, airline pilot, or professor? 25

MEASURING MORBIDITY l How far do we go in classifying “medical” problems? l e. g. cosmetic surgery v. Beware of phrases in contracts or policy statements such as “providing all medical care” or “basic needs” 26

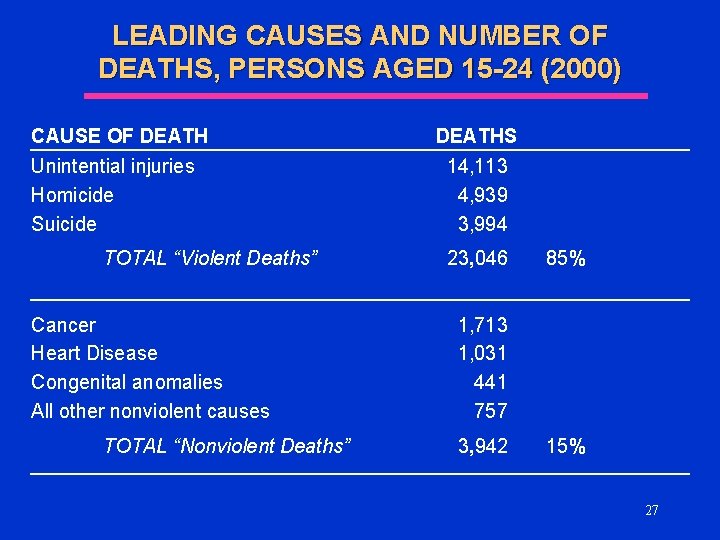
LEADING CAUSES AND NUMBER OF DEATHS, PERSONS AGED 15 -24 (2000) CAUSE OF DEATH Unintential injuries Homicide Suicide TOTAL “Violent Deaths” Cancer Heart Disease Congenital anomalies All other nonviolent causes TOTAL “Nonviolent Deaths” DEATHS 14, 113 4, 939 3, 994 23, 046 85% 1, 713 1, 031 441 757 3, 942 15% 27

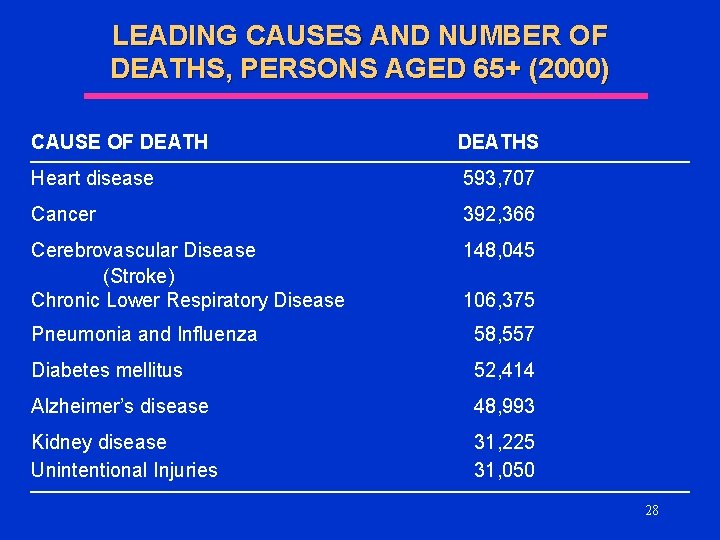
LEADING CAUSES AND NUMBER OF DEATHS, PERSONS AGED 65+ (2000) CAUSE OF DEATHS Heart disease 593, 707 Cancer 392, 366 Cerebrovascular Disease (Stroke) Chronic Lower Respiratory Disease 148, 045 106, 375 Pneumonia and Influenza 58, 557 Diabetes mellitus 52, 414 Alzheimer’s disease 48, 993 Kidney disease Unintentional Injuries 31, 225 31, 050 28

Empirical Evidence on Health Prod’n l Hadley (1982) a 10% in medical care $ per capita mortality rate by only 1. 5% l Auster et al. (1969) 10% in medical services age-adjusted mortality rate by 1% l Enthoven (1980) “flat-of-the-curve” medicine 29

LIFESTYLE l cigarette smoking 10% mortality: men 45 -64 women 45 -64 blacks 2. 3% 1. 1% whites 1. 4% 1. 1% (Hadley, 1982) l A one-pack-a-day smoker incurs 10. 9 more sick days every six months than a comparable non-smoker (Leigh and Fries, 1992) l Not smoking, regular exercise, moderate/no use of alcohol, 7 -8 hours of sleep per day, proper weight, eating breakfast, and no snacking leads to 28% lower mortality for men, 43% lower for women (Breslow and Enstrom, 1980) 30

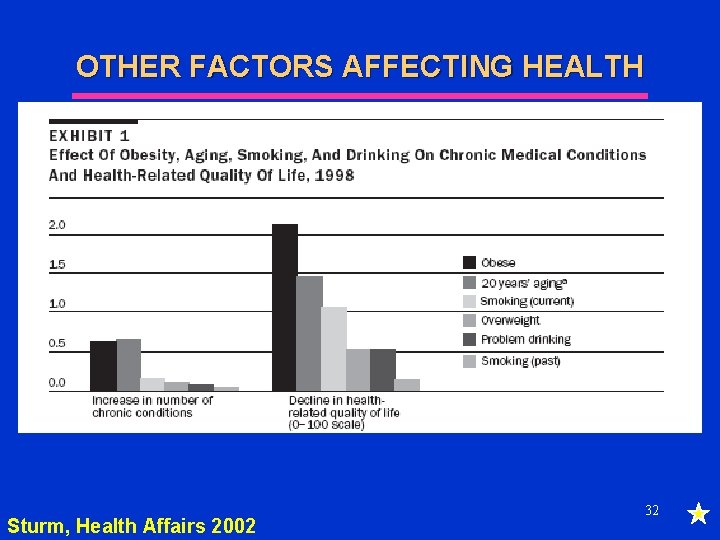
OTHER FACTORS AFFECTING HEALTH l Education u One more year of schooling prob of dying w/in 10 years by 3. 6% (Lleras-Muney 2001) l Income u People w/o high school educ & income <$10 k were 2 -3 x’s more likely to have functional limitations and poorer self-rated health 31

OTHER FACTORS AFFECTING HEALTH Sturm, Health Affairs 2002 32

Determinants of Infant Health Corman and Grossman, 1985 33

Determinants of Infant Health Selected Regression Results, Neonatal Mortality Rates Whites Blacks -0. 037 -0. 056 Newborn Intensive Care Hospitals/1000 -44. 196 -86. 196 Abortion Providers/1000 -3. 198 -16. 838 % HS Educated Corman and Grossman, 1985 34

Determinants of Infant Health l Does more schooling and the availability of more providers improve infant health? l Is the marginal productivity of more providers greater for blacks or whites? 35

Determinants of Infant Health l Why might the marginal productivities for blacks and whites differ? u The regressions have poor controls for income, health status, preferences, etc. which may be correlated with schooling and the availability of providers l If the marginal productivity for most factors is greater for blacks then whites, why isn’t the overall neonatal mortality rate lower for blacks than whites? 36

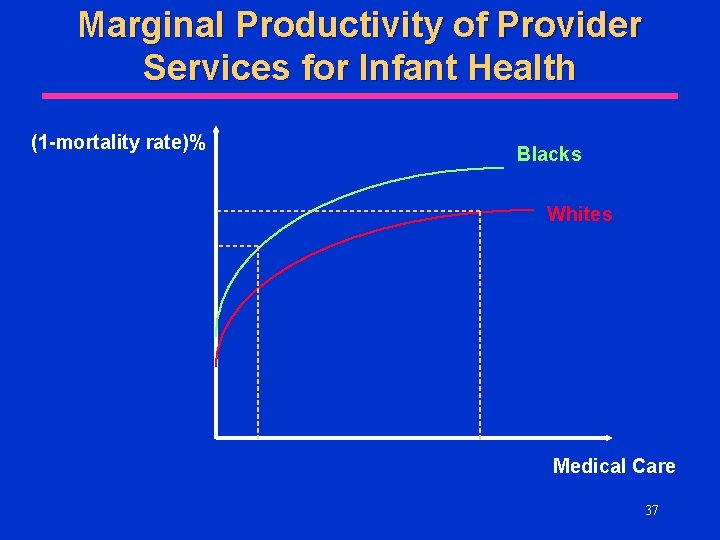
Marginal Productivity of Provider Services for Infant Health (1 -mortality rate)% Blacks Whites Medical Care 37

Marginal Productivity of Provider Services for Infant Health (cont. ) l For any given level of provider services, marginal productivity may be higher for blacks than whites l However, the level of services may be higher for whites than blacks Ø Knowing the shape of the total product curve is not enough. You must also know where you are on it 38

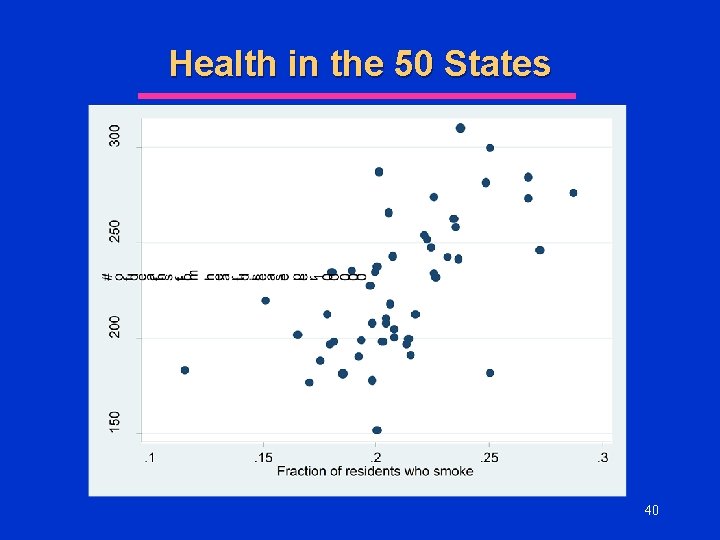
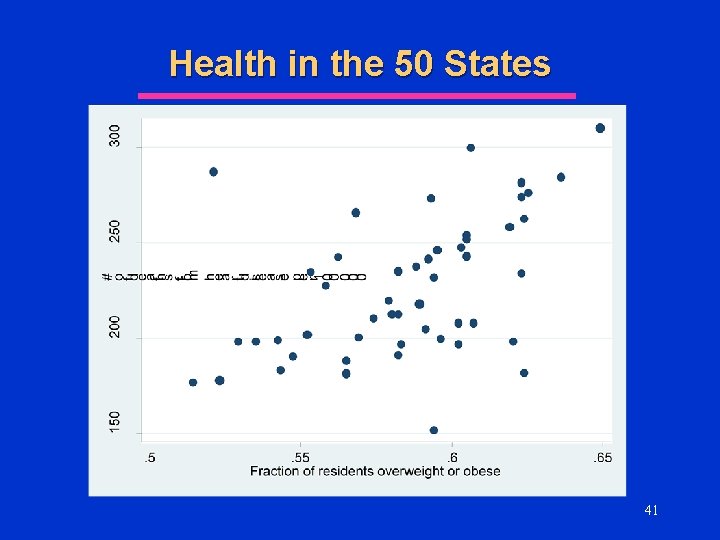
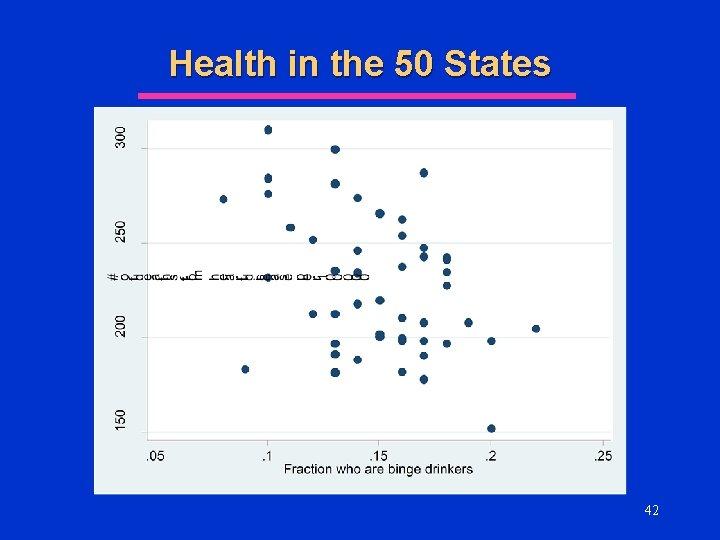
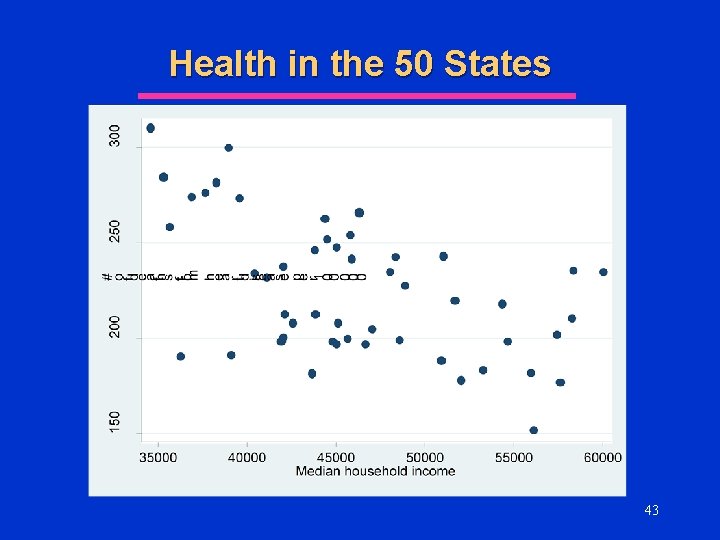
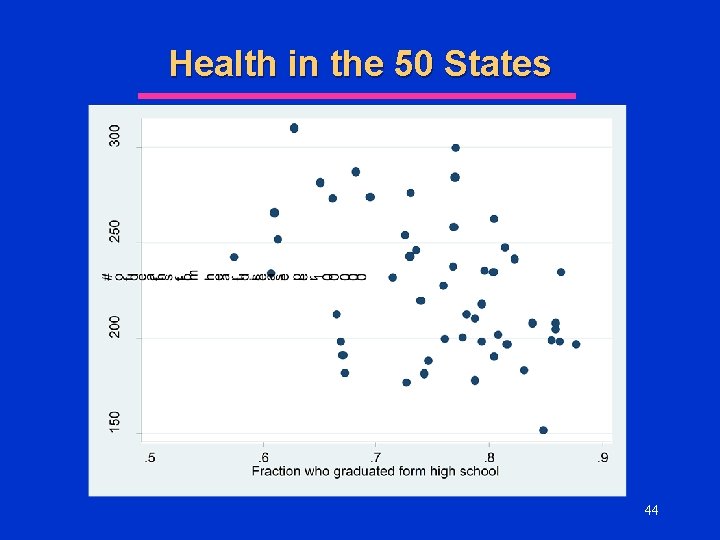
Health in the 50 States l One measure of health status in the population in the # of deaths (per 100, 000 residents) from heart disease l Suppose we have data on deaths from heart disease and other population characteristics by state u See l Excel Spreadsheet What factors might explain death from HD? u Why? 39

Health in the 50 States 40

Health in the 50 States 41

Health in the 50 States 42

Health in the 50 States 43

Health in the 50 States 44

Health in the 50 States l Which of the previous variables would you include in the multivariate regression for the determinants of death from heart disease? u Smoking? u Overweight/Obese? u Binge Drinking? u Household Income? u High School Graduation Rate? 45

Health in the 50 States l Which of the variables are statistically significant at the 95% confidence level? l Suppose the fraction of residents who are obese/overweight were reduced by 0. 10. u How fall? l much would death rates from heart disease Suppose that you could obtain data on a different variable that may explain heart disease death rates, but isn’t in this data set. u What would it be? 46

Conclusions In an economic model, medical care and other goods and services are combined to produce health, which yields utility to the consumer l The production of health can be measured in a variety of ways l Both higher health care expenditures and other factors are improving health status over time l 47
 Primary, secondary, tertiary care
Primary, secondary, tertiary care Mental health spending
Mental health spending Unit 2 equality diversity and rights
Unit 2 equality diversity and rights School of business and economics maastricht
School of business and economics maastricht Health and social component 3
Health and social component 3 State and local taxes and spending
State and local taxes and spending Mathematical vs non mathematical economics
Mathematical vs non mathematical economics Chapter 14: taxes and government spending section 1
Chapter 14: taxes and government spending section 1 Chapter 14 taxes and government spending
Chapter 14 taxes and government spending John and marcia monthly spending plan 1 answer key
John and marcia monthly spending plan 1 answer key Why is evaluating and adjusting a spending plan important
Why is evaluating and adjusting a spending plan important Chapter 14 taxes and government spending
Chapter 14 taxes and government spending Cash flow identity holds
Cash flow identity holds Benny card chard snyder
Benny card chard snyder What is spending
What is spending Moderate spending
Moderate spending Multiplier effect formula
Multiplier effect formula Tax multiplier
Tax multiplier How to calculate the tax multiplier
How to calculate the tax multiplier Government departments are accountable their spending
Government departments are accountable their spending Cash flow to creditors
Cash flow to creditors Spending plan shake up
Spending plan shake up Net fixed assets
Net fixed assets Deficit spending exists when
Deficit spending exists when Government spending multiplier formula
Government spending multiplier formula Uncontrollable spending definition ap gov
Uncontrollable spending definition ap gov Factors affecting investment spending
Factors affecting investment spending Convert spending
Convert spending Writ of certiorari ap gov example
Writ of certiorari ap gov example Ers tex flex
Ers tex flex The brown family spending plan
The brown family spending plan Ompetency
Ompetency Spending vocabulary
Spending vocabulary Spending vocabulary
Spending vocabulary Csi corporate card
Csi corporate card Opposite of spending
Opposite of spending Medicaid spending
Medicaid spending Excessive military spending in rome
Excessive military spending in rome Soup_nn
Soup_nn 24 chapter outline
24 chapter outline Deficit spending
Deficit spending Maya's spending plan answers
Maya's spending plan answers Tax multiplier
Tax multiplier Ratchet effect economics
Ratchet effect economics Gov spending multiplier
Gov spending multiplier Healthcare fsa
Healthcare fsa Mandatory spending
Mandatory spending Spending plan shake up
Spending plan shake up





































































