Health Care Transformation Bogot Colombia 28 July 2016

: Health Care Transformation Bogotá, Colombia 28 July 2016 Professor Elizabeth Teisberg The Dell Medical School, University of Texas at Austin and The Institute for Strategy and Competitiveness, Harvard Business School Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Every person has a story. Colombia has a great story…coverage for all! Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Health Care The goal is to help patients and families improve health. Quality of life and dignity of death are at stake. Smart, caring, hard-working professionals are working in a difficult context. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Why hasn’t competition worked better? How can we redefine care delivery for dramatic and ongoing improvement in results? Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Competition Bad Competition is over • shifting costs or capturing a bigger share of revenue • increasing bargaining power • capturing patients and limiting choice • restricting services Good Competition is over • increasing value for patients and families Zero or Negative Sum Positive Sum Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Competition Bad Competition is over • shifting costs or capturing a bigger share of revenue • increasing bargaining power e • capturing patients and limiting u l choice va g • restricting services in order to n i maximize revenue per visit or d i to reduce costs iv W O L N I E S d Zero or Negative Sum Volume based Good Competition is over • increasing value for patients IN ue W val IN g W in t a e r c Positive Sum Value based Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

How to change the dynamic? Get everyone IN the system. Then… Spend more? or Limit more? or Improve Health Care Value Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Value in health care Value = Health Outcomes that matter to patients Cost of delivering the outcomes Higher value enables better health results for more people for the money spent. Value is created one person at at time. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Strategic Shift to Value Health care Patients and families want more health, not more treatment. Treatment is an intermediate good. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Value in health care Value = Health Outcomes that matter to patients Cost of delivering the outcomes Outcomes are multidimensional and occur during and after treatment. Costs are for the full continuum of care. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
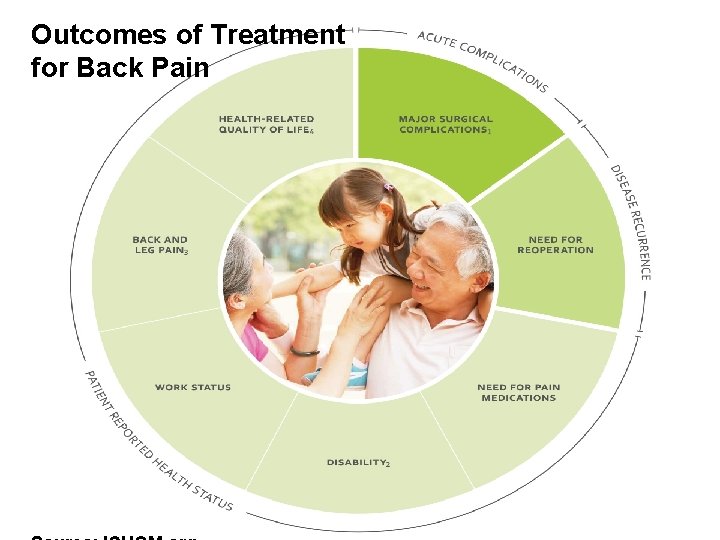
Outcomes of Treatment for Back Pain Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Can we afford better health? The most powerful way to increase value is to improve outcomes in ways that reduce costs. More health, success, efficiency; fewer problems and treatments. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Can we afford poor health? Poor health drives spending. Living in good health is inherently less expensive than living in poor health. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Keys to accelerate dramatic improvement in value • Define services from patients’ perspectives-by condition or segment. • Organize care delivery around solutions. • Create integrated, interdisciplinary teams. • Measure results to accelerate improvement. • Align financial success with medical success. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Innovation in Structure for High-Value Care Delivery In health care, value is created at the level of the individual patient. Organize to deliver solutions for patient segments with similar needs or shared medical conditions… even in primary care. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
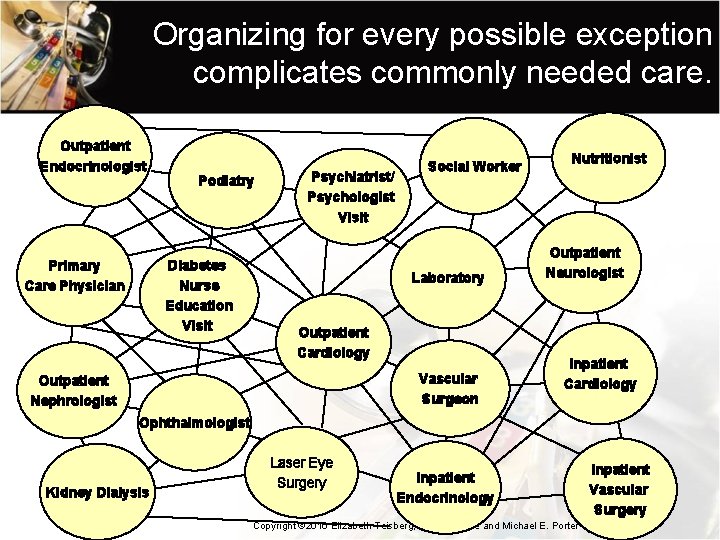
Organizing for every possible exception complicates commonly needed care. Outpatient Endocrinologist Podiatry Diabetes Nurse Education Visit Primary Care Physician Psychiatrist/ Psychologist Visit Social Worker Laboratory Outpatient Cardiology Vascular Surgeon Outpatient Nephrologist Nutritionist Outpatient Neurologist Inpatient Cardiology Ophthalmologist Kidney Dialysis Laser Eye Surgery Inpatient Endocrinology Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter Inpatient Vascular Surgery

Beyond Coordinating: Experience Group research led to new care solution in Type 2 diabetes Ongoing classes Chronic health self-management Peer coaching Group discussions & Shared appointments Home assessment Patients/ Families Care Solutions Chronic Health facility visits Web-based, telephonic reporting of core metrics (BS, weight, BP) Regular clinical team meetings Worksite assessment Pre-hospital consults Coordinated appointments based on need, not calendar Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
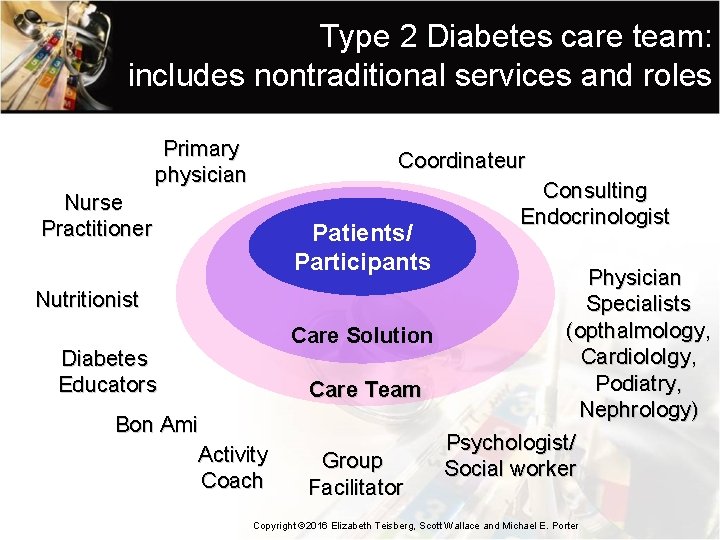
Type 2 Diabetes care team: includes nontraditional services and roles Primary physician Coordinateur Nurse Practitioner Patients/ Participants Nutritionist Diabetes Educators Bon Ami Activity Coach Consulting Endocrinologist Physician Specialists (opthalmology, Care Solution Cardiololgy, Podiatry, Care Team Nephrology) Psychologist/ Group Social worker Facilitator Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Remote team members • Enable designed primary care for some medicallydefined patient segments (frail elderly, people with diabetes…) • Ask how to bring expertise to the location of need, not just how to move patients • Use technology to build relationships • Use coaches, accompaniateurs, behavioral health Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Measure results that clinicians and patients can affect • Clinicians need to measure results for each patient. • Drive value improvement and learning. • Adjust outcomes for initial patient conditions. • Don’t wait for perfection: When used, measures and risk adjustment methods improve rapidly. Failure to measure outcomes spurs the wrong competition, slows improvement and invites costly micromanagement Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
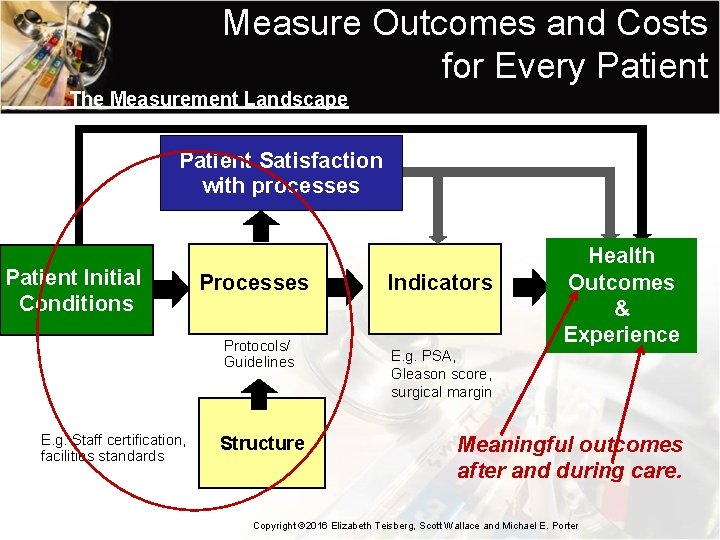
Measure Outcomes and Costs for Every Patient The Measurement Landscape Patient Satisfaction with processes Patient Initial Conditions Processes Protocols/ Guidelines E. g. Staff certification, facilities standards Structure Indicators Health Outcomes & Experience E. g. PSA, Gleason score, surgical margin Meaningful outcomes after and during care. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Not asking the critical questions How were we? How are you? Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

What matters most to patients? Quality of life and Dignity of death Specifically… • Capability – better functional outcomes • Comfort – less burden of disease – Less physical suffering; less emotional angst • Calm – less burden of treatment – Less time spent; less hassle endured Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
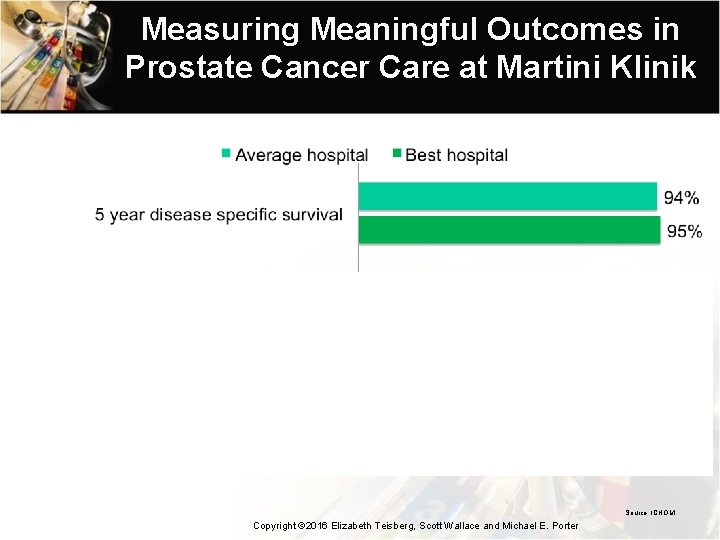
Measuring Meaningful Outcomes in Prostate Cancer Care at Martini Klinik Source: ICHOM Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
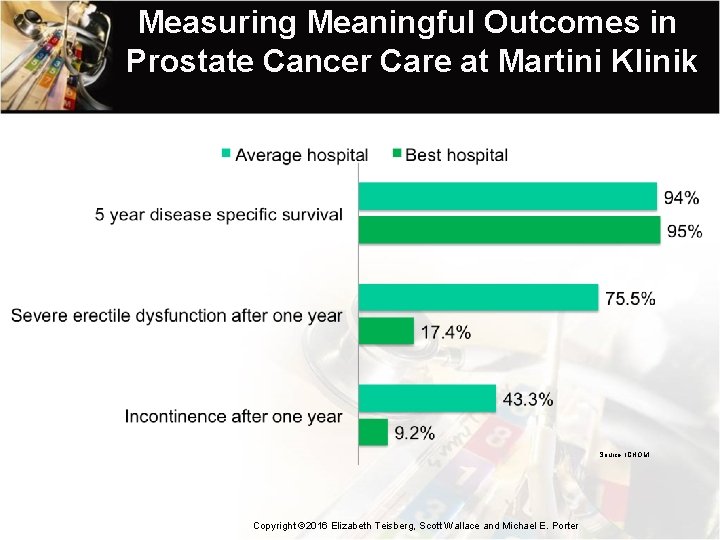
Measuring Meaningful Outcomes in Prostate Cancer Care at Martini Klinik Source: ICHOM Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Migraine Care in Germany Old model: components, not solutions Organized by specialty in discrete, fragmented services. Most patients were not getting effective or appropriate care for migraines. Outpatient Physical Therapist Imaging Unit Outpatient Neurology Primary Care Physician Inpatient Treatment and Detox Outpatient Psychologist Source: KKH, Westdeutsches Kopfschmerzzentrum Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
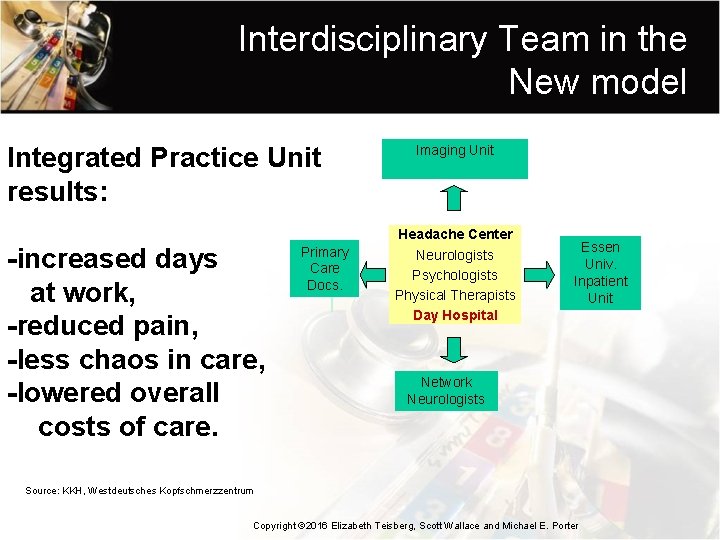
Interdisciplinary Team in the New model Integrated Practice Unit results: -increased days at work, -reduced pain, -less chaos in care, -lowered overall costs of care. Primary Care Docs. Imaging Unit Headache Center Neurologists Psychologists Physical Therapists Day Hospital Essen Univ. Inpatient Unit Network Neurologists Source: KKH, Westdeutsches Kopfschmerzzentrum Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
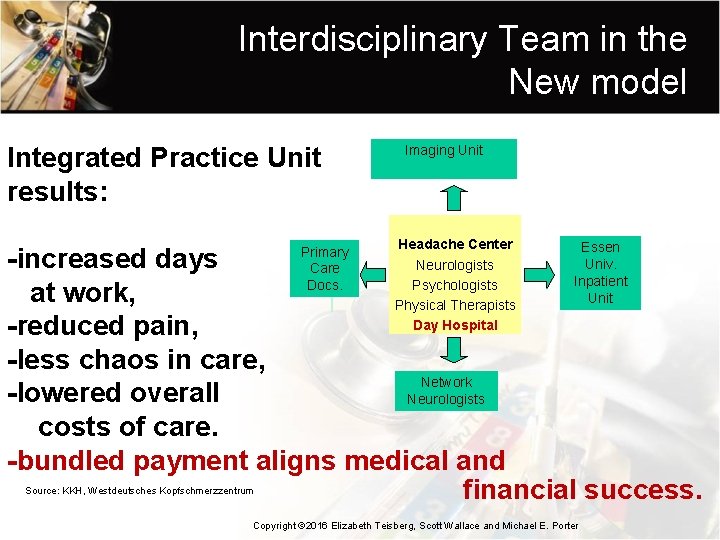
Interdisciplinary Team in the New model Integrated Practice Unit results: Imaging Unit Headache Center Neurologists Psychologists Physical Therapists Day Hospital Essen Univ. Inpatient Unit -increased days at work, -reduced pain, -less chaos in care, Network -lowered overall Neurologists costs of care. -bundled payment aligns medical and financial success. Primary Care Docs. Source: KKH, Westdeutsches Kopfschmerzzentrum Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Transformation to High Value is a Journey • It’s about individual and family health… • Recognize medically meaningful population segments. • Set the compass with specific outcome measures. • Create solutions including (nonmedical) services and remote team members. • Demonstrate early wins. Celebrate…and keep going. • Don’t worry yet about last leg of the journey. Make a huge improvement now. Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Health is Capability, Comfort and Calm …cómo estás? Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

gracias Elizabeth Teisberg Professor The Dell Medical School University of Texas at Austin Teisberg@austin. utexas. edu Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Health care supports economic strength • Health enables presence and productivity • Health care disparities undermine stability • Health-focused services support local economic strength • Technology to take expertise to local communities can benefit more than health care • Leadership in particular services (e. g. eye treatments…) attract customers, clinicians and supporting businesses Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
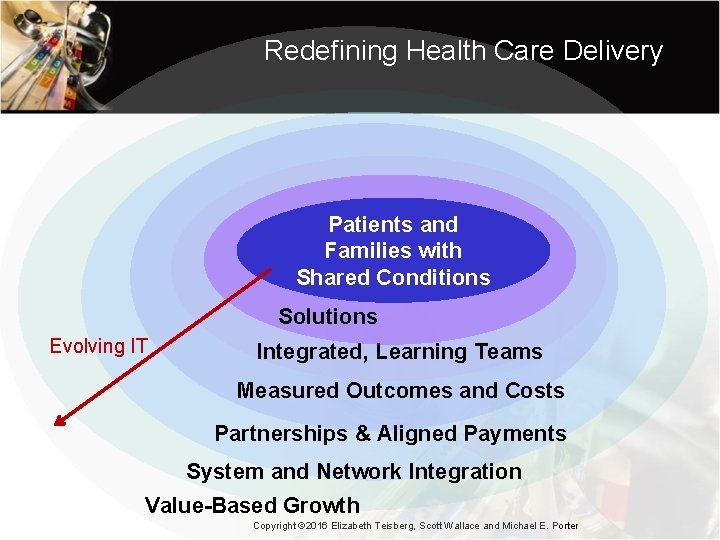
Redefining Health Care Delivery Patients and Families with Shared Conditions Solutions Evolving IT Integrated, Learning Teams Measured Outcomes and Costs Partnerships & Aligned Payments System and Network Integration Value-Based Growth Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter

Prepayment reforms alone are not enough. Prepayment (per member per month) Bundled payment within organizations Multidisciplinary teams (care bundles) Improving care solutions Measured results (outcomes and costs) Patient segments Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
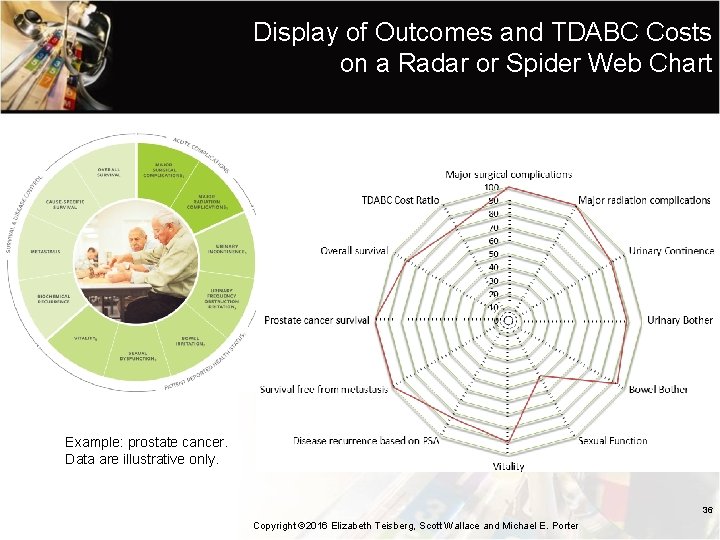
Display of Outcomes and TDABC Costs on a Radar or Spider Web Chart Example: prostate cancer. Data are illustrative only. 36 Copyright © 2016 Elizabeth Teisberg, Scott Wallace and Michael E. Porter
- Slides: 36