Health Benefit Consultants HBC Independent Third Party Administrator

Health Benefit Consultants (HBC( Independent Third Party Administrator Found in 1993 Address 849 Vorawat Building, Floor 19 th Silom Road, Bangrak Bangkok 10500 1

HBC’s Services Design MEI and PA products Establish hospital network Claim assessment services Concurrent review Case management 2

HBC’s Competencies Full-time Nurses, experienced claim assessors, and Medical Consultants 303 Hospital Network throughout Thailand Specifically designed computer software We have 3 relevant data bases 3

HBC have been performing claim administration more than 1, 000 claims since 1993 4

HBC’s Competencies Full-time Nurses, experienced claim assessors, and Medical Consultants 303 Hospital Network throughout Thailand Specifically designed computer software We have 3 relevant data bases 5

Main contents in the hospital contract To ensure that HBC can proceed the claims efficiently and accurately To provide best service to the patient (the claimant) To gather essential information/profile – Hospital’s specialists and medical equipments – Drug and medical supplies’ price lists and discount structures – Doctor profile To cooperate with HBC i. e. , supplying all relevant medical information and documents, coordinating the claim to ensure timely and accurately communication 6

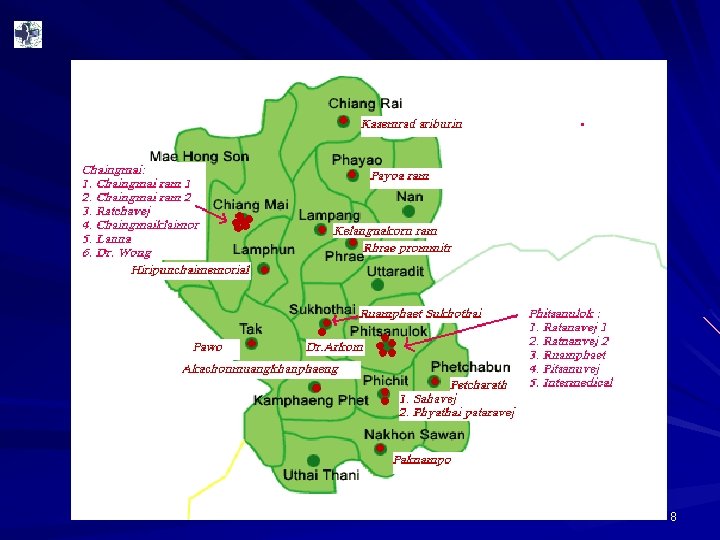
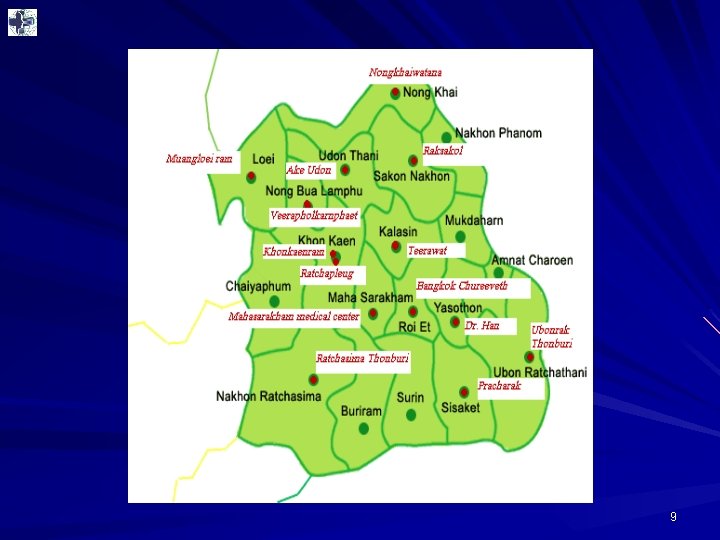
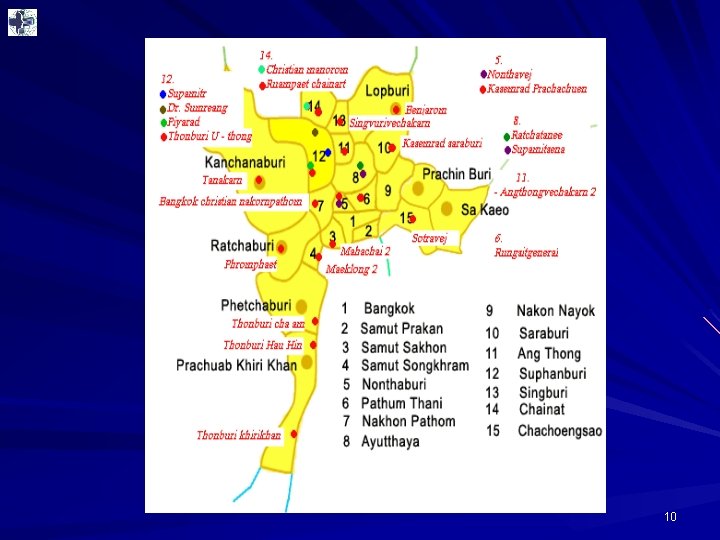
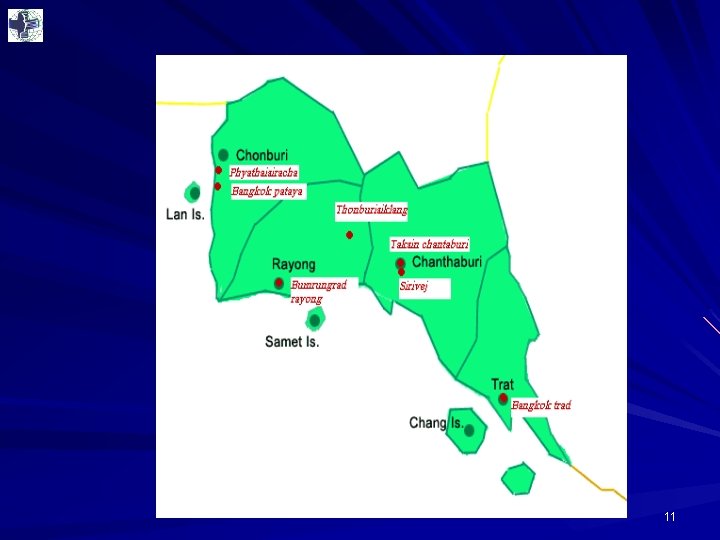
Hospital network location 7
8
9
10
11
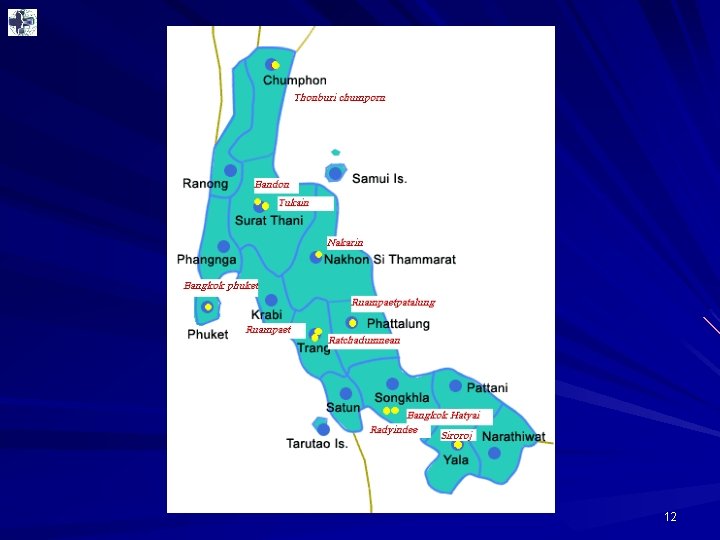
12

HBC’s Competencies Full-time Nurses, experienced claim assessors, and Medical Consultants 303 Hospital Network throughout Thailand Specifically designed computer software We have 3 relevant data bases 13

Major characteristics-Computer software Open platform system Data Security – Data back up system – Data control system HBC-Link 14

HBC’s Competencies Full-time Nurses, experienced claim assessors, and Medical Consultants 303 Hospital Network throughout Thailand Specifically designed computer software We have 3 relevant data bases 15
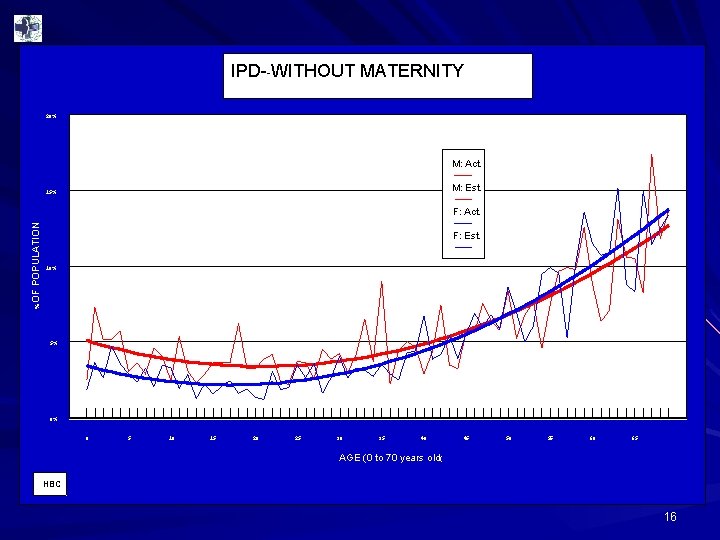
IPD--WITHOUT MATERNITY 20% M: Act. M: Est. 15% %OF POPULATION F: Act. F: Est. 10% 5% 0% 0 5 10 15 20 25 30 35 40 45 50 55 60 65 AGE (0 to 70 years old( HBC 16

Changes in Health Continuum of Managed Care 17
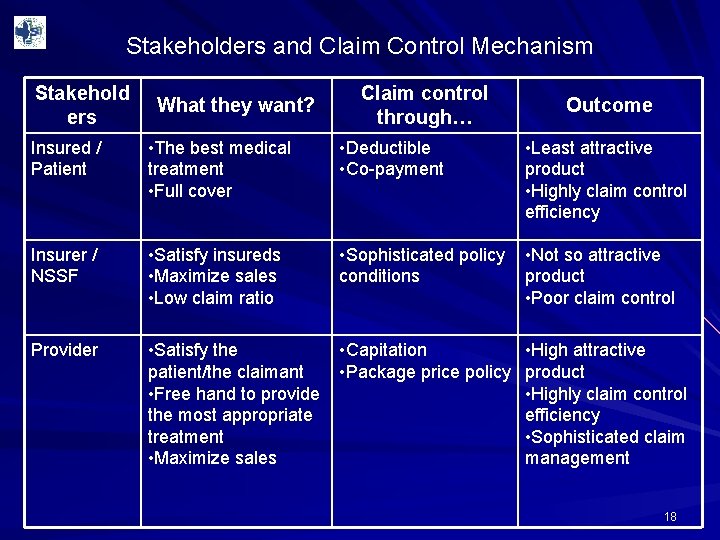

Stakeholders and Claim Control Mechanism Stakehold ers What they want? Claim control through… Outcome Insured / Patient • The best medical treatment • Full cover • Deductible • Co-payment • Least attractive product • Highly claim control efficiency Insurer / NSSF • Satisfy insureds • Maximize sales • Low claim ratio • Sophisticated policy conditions • Not so attractive product • Poor claim control Provider • Satisfy the • Capitation patient/the claimant • Package price policy • Free hand to provide the most appropriate treatment • Maximize sales • High attractive product • Highly claim control efficiency • Sophisticated claim management 18

Kurnia-HBC Common Objectives Accurate To reflex the accurate Loss Ratio, Drawing Rate etc. To maximize clients’ satisfaction – Clear 80% of the reimbursement claims will done within 6 working days – Clean All claim assessments must be able to explain to claimants – Convenience Claimants can access 24 hours a day, 7 days a week 19

Our services offer 20

Free-of-charge product development services 1. Analyze and comment NSSF’s existing scheme 2. Initiate / create new schemes 21

Claim processing 1. Provide claim pre-certification 2. Concurrent review 3. Provide fax-claim services 4. Q & A claim form insured members 22
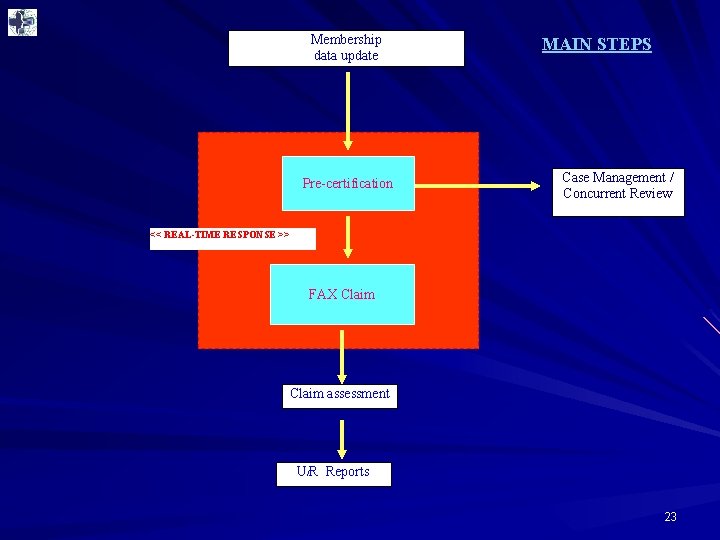
Membership data update Pre-certification MAIN STEPS Case Management / Concurrent Review << REAL-TIME RESPONSE >> FAX Claim assessment U/R Reports 23
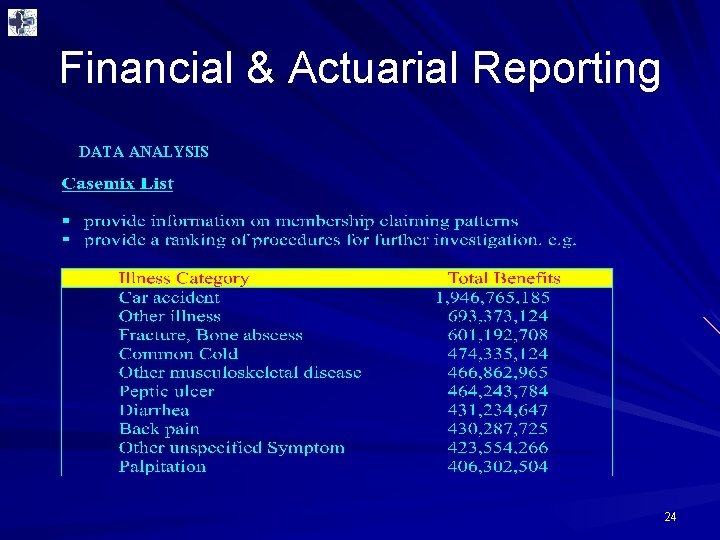

Financial & Actuarial Reporting DATA ANALYSIS 24
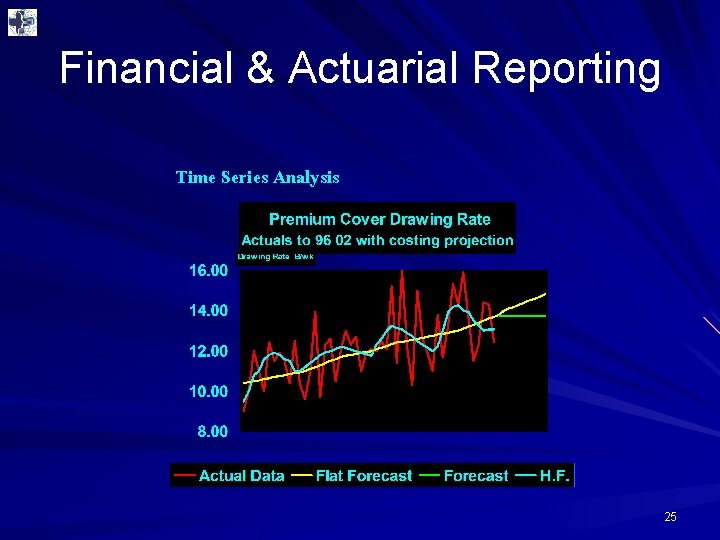
Financial & Actuarial Reporting Time Series Analysis 25

Thank you 26
- Slides: 26